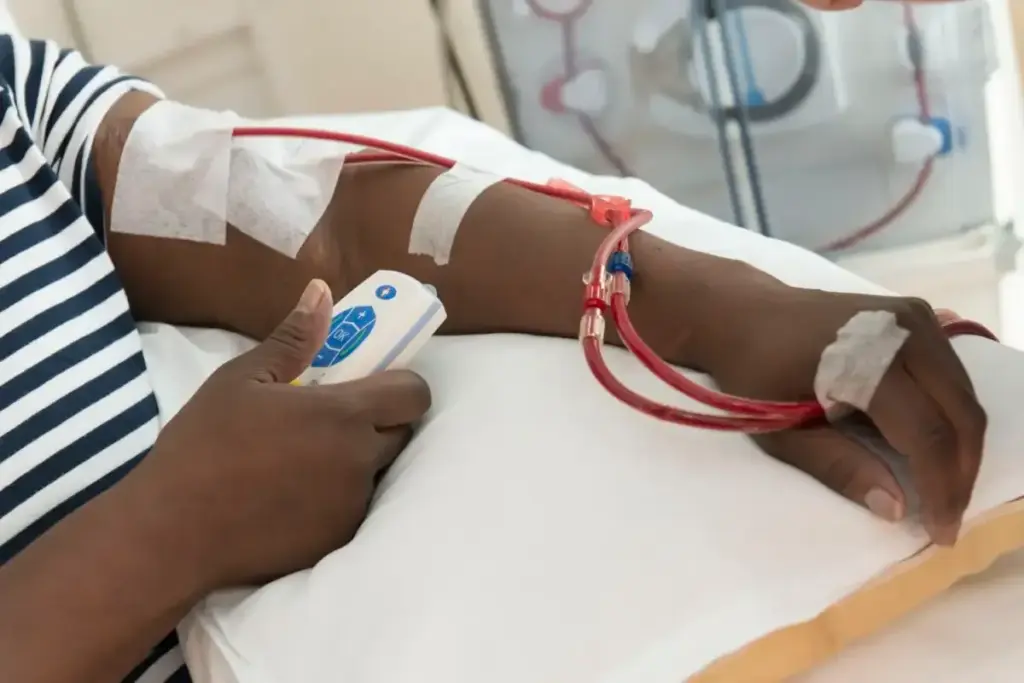
Stopping bleeding after dialysis is a big worry for many patients. Those on hemodialysis (HD) face a higher risk. HD patients bleed at a rate of 60.8/1000 person-years, which is almost double the risk of those on peritoneal dialysis (PD) at 34.6/1000 person-years. Managing a graft for dialysis? Discover amazing safety tips and vital, powerful ways to stop bleeding for a successful recovery.
It’s important to know the difference between HD and PD to manage bleeding risks. An arteriovenous fistula or a graft is used for HD. Knowing how to take care of these access points is key.
We will look at proven ways to lower bleeding risks and improve patient results.
Key Takeaways
- Bleeding risks are significantly higher in hemodialysis patients compared to peritoneal dialysis patients.
- Understanding the type of dialysis access, such as an arteriovenous fistula or graft, is important.
- Evidence-based interventions can help minimize bleeding risks.
- Proper care and management of dialysis access points are vital.
- Patient outcomes can be significantly improved with the right care and interventions.
Understanding Bleeding Risks in Dialysis Patients
Bleeding risks are a big worry for dialysis patients. It’s key to know about these risks to care for them well. Dialysis is a life-saving treatment for those with kidney failure. But, it can lead to bleeding problems.
There are many reasons why dialysis patients might bleed. The dialysis process itself, medicines to prevent blood clots, and health issues can all play a part. The type of dialysis a patient gets can also affect their risk of bleeding.
Comparative Bleeding Risks: Hemodialysis vs. Peritoneal Dialysis
Hemodialysis (HD) and peritoneal dialysis (PD) are the main dialysis types. Studies show HD patients face a higher risk of bleeding than PD patients. This is because HD needs anticoagulation to stop the dialysis circuit from clotting.
PD, on the other hand, doesn’t need anticoagulation. It uses the peritoneum in the abdomen to filter waste from the blood. This makes PD patients less likely to bleed compared to HD patients.
“The risk of bleeding is a major consideration for healthcare providers when treating patients who are on dialysis.”
Statistical Evidence on Bleeding Complications
Studies back up the idea that HD patients face a higher risk of bleeding. Some research shows up to 30% of HD patients experience bleeding issues.
A study compared HD and PD patients. It found PD patients had fewer bleeding episodes. The study said PD patients’ bleeding risk is more tied to their health conditions than the dialysis itself.
- Bleeding risks vary significantly between HD and PD patients.
- HD patients are at a higher risk due to anticoagulation therapy.
- PD patients have fewer bleeding episodes, mainly due to the absence of anticoagulation.
It’s vital for healthcare providers to understand these risks. This knowledge helps them manage patient care better and lower the chance of bleeding problems.
Causes of Post-Dialysis Bleeding
Many things can cause bleeding after dialysis. Knowing what these are helps us manage and lower this risk.
Anticoagulation Factors
Anticoagulation therapy is used to stop clots in the dialysis circuit. But, it can also increase bleeding risk. Heparin, a common anticoagulant, can make bleeding more likely, mainly in those at higher risk.
Managing anticoagulation therapy is key. We need to watch patients closely for any signs of bleeding.
|
Anticoagulant |
Mechanism of Action |
Bleeding Risk |
|---|---|---|
|
Heparin |
Activates antithrombin, inhibiting thrombin and factor Xa |
High |
|
Citrate |
Cheates calcium ions, preventing clot formation |
Moderate |
Needle Site Complications
Problems at the needle site are a big cause of bleeding after dialysis. Issues like hematoma formation or aneurysm development can cause bleeding. It’s important to use the right techniques and care for the needle site to reduce these risks.
For those with a dialysis arm port, managing the access site well is critical. This means placing the needle correctly and securing it to avoid dislodgment.
Patient-Specific Risk Factors
Each patient’s risk of bleeding after dialysis is different. Factors like age, underlying health conditions (like diabetes or hypertension), and medication use (such as antiplatelet agents or anticoagulants) can affect this risk.
For example, those with bleeding disorders or on long-term anticoagulation therapy are at higher risk. Knowing these factors helps us tailor our approach to reduce bleeding risks.
|
Risk Factor |
Description |
Impact on Bleeding Risk |
|---|---|---|
|
Age |
Older patients may have more comorbidities and fragile tissues |
Increased |
|
Underlying Health Conditions |
Conditions like diabetes and hypertension can affect vascular health |
Variable |
|
Medication Use |
Use of antiplatelet agents or anticoagulants |
Increased |
By understanding and addressing these causes, we can better manage post-dialysis bleeding. This helps improve patient outcomes and ensures proper treatment for fistula arm swelling when needed.
Immediate Steps to Stop Bleeding After Dialysis
Managing bleeding after dialysis needs a mix of manual pressure and the right patient position. After dialysis, bleeding from the access site is a big worry. It needs quick action.
Proper Application of Manual Pressure
Using manual pressure is key to stop bleeding after dialysis. Here’s how to do it right:
- Use clean gauze to press on the needle site.
- Apply firm, steady pressure for a while.
- Don’t lift the pressure too fast, or it might not stick.
Correct Positioning of the Access Site
Where you place the access site is very important. We suggest:
- Put the access limb up, above the heart, to slow blood flow.
- Make sure the patient is comfy and the site is easy to watch.
Time Considerations for Pressure Application
How long to keep pressure on can change based on the patient and the access type. Usually:
- Keep pressure on for at least 5-10 minutes.
- Watch the site for any bleeding or swelling.
Here’s a quick guide on how to stop bleeding after dialysis:
|
Step |
Description |
Considerations |
|---|---|---|
|
1. Manual Pressure |
Apply firm pressure using clean gauze. |
Ensure consistent pressure; avoid releasing too quickly. |
|
2. Access Site Positioning |
Elevate the limb above heart level. |
Monitor for comfort and accessibility. |
|
3. Time Considerations |
Maintain pressure for 5-10 minutes. |
Adjust based on patient factors and access type. |
Advanced Methods for Controlling Post-Dialysis Bleeding
Keeping patients safe from post-dialysis bleeding is key. New methods are now available to help. These include special dressings and advanced bandage systems.
Specialized Hemostatic Dressings
Specialized dressings are now a big help in managing bleeding after dialysis. Chitosan-based bandages are showing great promise. Studies show they can cut down bleeding times, helping patients a lot.
These dressings work by helping blood to clot faster. Using them right after dialysis can greatly lower bleeding risks. They should be part of a full plan to manage bleeding.
IRIS and Other Advanced Bandage Systems
IRIS and other bandage systems are also helping with bleeding control. The IRIS system applies pressure and supports the access site, cutting down on bleeding. It’s great for arteriovenous fistulas and grafts.
IRIS and similar systems are easy to use and very effective. They help healthcare providers give better care and lower bleeding risks for patients.
As dialysis care gets better, using these new dressings and bandages will be more important. They help us care for dialysis patients better and reduce bleeding problems.
Graft for Dialysis: Understanding Your Vascular Access
An arteriovenous graft is a surgically implanted vascular access for dialysis. It’s key for patients with end-stage renal disease. This graft connects an artery to a vein, making dialysis efficient.
What is an Arteriovenous Graft?
An arteriovenous graft is a synthetic tube that connects an artery to a vein in the forearm. It allows for high blood flow, essential for dialysis. It’s used when a patient’s blood vessels can’t support a fistula.
Using an arteriovenous graft for dialysis has many benefits. These include:
- Lower risk of complications compared to other vascular access types
- Quicker maturation time
- Works well for patients with certain vascular conditions
Placement and Maturation Process
The graft is placed through surgery, usually in the arm. The surgery is done under local anesthesia. The graft is then connected to an artery and a vein.
After surgery, the graft needs time to mature. This means it must become ready for dialysis. Proper care during this time is vital to avoid problems.
Bleeding Management Specific to Grafts
Managing bleeding in arteriovenous graft patients is critical. Bleeding can happen for many reasons, like needle dislodgment or graft damage. To manage bleeding, you can apply manual pressure, use hemostatic agents, or sometimes, surgery is needed.
It’s important for patients and caregivers to know the signs of bleeding. They should also know how to react. Regular graft checks and quick reporting of any issues to the healthcare team can prevent serious problems.
“Proper care and monitoring of the arteriovenous graft can significantly reduce the risk of bleeding and other complications, ensuring a safer dialysis experience.”
— Dialysis Care Expert
Understanding arteriovenous grafts and managing complications can help patients. It improves their treatment options and overall care.
Arteriovenous Fistula vs. Graft: Comparing Dialysis Access Options
Arteriovenous fistulas and grafts are key for dialysis. Each has its own benefits and drawbacks. We’ll look at their differences to help you choose wisely.
Differences in Structure and Function
An arteriovenous fistula connects an artery to a vein in the forearm. It’s made for dialysis and allows more blood flow. A graft, on the other hand, is a synthetic tube that connects an artery to a vein.
Fistulas are often chosen because they offer natural blood flow and fewer problems. But, they need time to mature before use. Grafts are quicker to use but face more risks like clotting and infection.
Bleeding Risk Comparison
Bleeding risks differ between fistulas and grafts. Mature fistulas have lower bleeding risks than grafts. Grafts, being synthetic, might bleed more due to mechanical issues.
|
Access Type |
Bleeding Risk |
Complications |
|---|---|---|
|
Arteriovenous Fistula |
Lower |
Maturation failure, stenosis |
|
Graft |
Higher |
Clotting, infection, mechanical failure |
Longevity and Maintenance Requirements
The lifespan of fistulas and grafts depends on many factors. Patient health, access care, and cannulation techniques play a big role. Fistulas usually last longer than grafts if well cared for.
Regular check-ups with your healthcare provider are key. They help keep your vascular access healthy, whether it’s a fistula or a graft. Proper care and timely action can greatly extend your dialysis access’s life and function.
Managing Bleeding Fistula Emergencies
A bleeding fistula crisis needs quick action to avoid serious problems. For those on dialysis, knowing how to handle these emergencies is key for their safety.
Recognizing a Bleeding Fistula Crisis
Spotting the signs of a bleeding fistula is the first step. Signs include fast bleeding, swelling, or pain at the fistula site. Knowing these signs helps you act fast.
It’s smart for patients and caregivers to know what a normal fistula looks and acts like. This way, they can spot any oddities right away.
Immediate Response Protocols
When you see a bleeding fistula, you must act quickly. Apply manual pressure to the bleeding spot to stop it. Also, raising the affected limb can cut down blood flow.
- Apply firm and steady pressure to the bleeding site.
- Elevate the limb above heart level to reduce blood flow.
- Monitor the patient’s vital signs and overall condition.
Stay calm and follow these steps to control the bleeding well.
Hospital vs. Home Management
First steps for a bleeding fistula can be taken at home. But, knowing when to go to the hospital is key. Severe bleeding, big swelling, or signs of infection mean you need to see a doctor right away.
We suggest patients have a plan for emergencies. Keep your dialysis team’s contact info and emergency services handy.
Handling bleeding fistula emergencies well means quick action, knowing what to do first, and when to get medical help. Being ready and informed can lower the risks of fistula bleeding.
Ways to Prevent Aneurysms in Fistulas and Grafts
To prevent aneurysms in dialysis access sites, we need regular checks, proper cannulation, and quick action. Let’s dive into these methods to keep dialysis patients’ fistulas and grafts safe.
Regular Monitoring Techniques
Keeping an eye on your access site is key to spotting problems early. This means:
- Looking for swelling or dilation in the access site.
- Using ultrasound or other imaging to check the fistula or graft’s structure.
- Watching the blood flow and pressure in the access site.
Table: Monitoring Techniques for Fistulas and Grafts
|
Monitoring Technique |
Description |
Frequency |
|---|---|---|
|
Visual Inspection |
Checking for visible signs of aneurysm or damage. |
Daily |
|
Ultrasound Imaging |
Assessing the internal structure of the fistula or graft. |
Monthly |
|
Blood Flow Monitoring |
Measuring the flow rate and pressure within the access site. |
Weekly |
Proper Cannulation Practices
Using the right needle size and type is important to avoid damage. This also means:
- Rotating cannulation sites to avoid repetitive trauma to the same area.
- Ensuring proper needle placement and securement.
Early Intervention Strategies
Acting fast is key to stopping aneurysms from getting worse. This includes:
- Surgical revision of the affected area.
- Endovascular interventions, such as angioplasty or stenting.
- Close monitoring and follow-up to assess the effectiveness of the intervention.
By using these methods, dialysis patients can lower their risk of aneurysms. This makes dialysis safer and more effective.
Managing Fistula Arm Swelling and Related Complications
Managing fistula arm swelling is key in dialysis care. It needs careful attention and the right treatment. Swelling can happen due to dialysis access issues. Knowing how to handle it is vital for patient care.
Normal vs. Problematic Swelling
It’s important to tell normal swelling from problematic swelling after a fistula is made. Normal swelling usually goes away in a few weeks. But, if it doesn’t or gets worse, it might mean there’s a problem.
Identifying Problematic Swelling: Look for signs like more pain, redness, or warmth around the fistula. These could mean an infection or serious issues.
Treatment Options for Fistula Arm Swelling
There are many ways to manage fistula arm swelling. These range from simple steps to more serious procedures.
- Conservative Management: Raising the affected arm and using cold compresses can help lessen swelling.
- Compression Therapy: Wearing compression garments or bandages can help by improving blood flow.
- Medical Intervention: Sometimes, medicine is needed to treat issues like infection or blood clots.
|
Treatment Option |
Description |
Benefits |
|---|---|---|
|
Conservative Management |
Elevation and cold compresses |
Reduces swelling, easy to implement |
|
Compression Therapy |
Compression garments or bandages |
Improves circulation, reduces swelling |
|
Medical Intervention |
Medication for infection or thrombosis |
Addresses underlying causes, effective for serious conditions |
Prevention Strategies for Recurring Swelling
To stop swelling from coming back, proper fistula care, watching for signs, and teaching patients are key.
“Proper cannulation techniques and regular monitoring can significantly reduce the risk of complications such as swelling.”
Expert Opinion
Important prevention steps include:
- Checking the fistula site often for early signs of problems.
- Using the right way to put in needles to avoid hurting the fistula.
- Telling patients how to take care of their fistula and spot issues early.
By knowing why fistula arm swelling happens and using good management and prevention, we can make patients’ lives better.
When to Seek Medical Help for Post-Dialysis Bleeding
Dialysis patients should know when to seek medical help for bleeding after dialysis. Knowing these signs can prevent serious problems.
Warning Signs of Serious Bleeding Complications
There are warning signs for serious bleeding after dialysis. These include:
- Prolonged bleeding that doesn’t stop with manual pressure
- Swelling or hematoma at the access site
- Signs of infection such as redness, warmth, or fever
Spotting these signs early is key to acting fast.
Emergency Response Protocols
If there’s serious bleeding, apply manual pressure and elevate the limb. It’s also important to have a plan for emergencies. Keep your dialysis team’s contact info handy.
Communication with Your Dialysis Team
Keeping in touch with your dialysis team is essential. Tell them about any bleeding after dialysis. This helps them manage your care and avoid future issues.
|
Warning Signs |
Emergency Response |
Communication Tips |
|---|---|---|
|
Prolonged bleeding |
Apply manual pressure |
Inform your dialysis team about bleeding incidents |
|
Swelling or hematoma |
Elevate the affected limb |
Report any signs of infection |
|
Signs of infection |
Seek immediate medical help |
Keep contact information for your dialysis team handy |
Home Care Tips for Dialysis Access Sites
Caring for your dialysis access site at home is very important. It helps keep it working well. Good home care is key to your dialysis treatment’s success.
Daily Maintenance Practices
Keeping your dialysis access site clean is essential. Wash the area gently with mild soap and water. It’s important to keep it clean and dry to avoid infections.
Check your access site daily for redness, swelling, or drainage. If you see anything unusual, call your healthcare provider right away.
Infection Prevention
Stopping infections is a big part of caring for your dialysis access site at home. Always wash your hands before touching it. Use an antiseptic solution as your healthcare provider tells you to.
- Keep your access site clean and dry.
- Avoid tight clothing that may rub against or put pressure on your access site.
- Monitor your access site regularly for signs of infection.
Activity Restrictions and Precautions
It’s good to stay active, but some activities are not safe for your dialysis access site.
|
Activity |
Precaution |
|---|---|
|
Lifting Heavy Objects |
Avoid lifting heavy objects to prevent strain on your access site. |
|
Tight Clothing |
Avoid wearing tight clothing that may constrict your access site. |
|
Contact Sports |
Refrain from participating in contact sports that could potentially damage your access site. |
By following these home care tips, you can help keep your dialysis access site working well. If you have any concerns or questions, always talk to your healthcare provider.
Latest Advancements in Dialysis Access Management
New materials and techniques are changing dialysis access care. Managing dialysis access sites is key to patient care. Ongoing research aims to better patient outcomes.
New Materials and Technologies
New materials and technologies are making dialysis access sites better. For example, advanced graft materials help lower risks of problems like thrombosis and infection.
Also, 3D printing is being used to make custom vascular access grafts. This could lead to better graft success rates and fewer surgeries.
Improved Cannulation Techniques
Cannulation techniques are vital in dialysis access care. New methods aim to reduce damage to the access site. This lowers the chance of complications.
- Buttonhole cannulation
- Rope-ladder cannulation
- Area puncture technique
Using these techniques right can make dialysis access sites last longer.
Future Directions in Dialysis Access Care
Looking ahead, research is promising. It includes making biocompatible materials that work better with the body. This could lower the risk of bad reactions.
Regenerative medicine is also being studied. It might help fix or replace damaged tissues. This offers hope for patients with tough dialysis access problems.
By using these new advancements, we can keep improving care for dialysis patients.
Conclusion
We’ve talked about how to handle bleeding risks in dialysis patients. We looked at grafts for dialysis and arteriovenous fistulas. Knowing the difference between arteriovenous fistula vs graft is key to picking the right dialysis access for each patient.
Handling bleeding risks involves several steps. These include applying manual pressure, placing the access site correctly, and using advanced dressings. It’s also important to keep an eye on the dialysis access site and maintain it well.
Healthcare providers can lower bleeding risks by using proven methods and staying up-to-date with new dialysis access management. This not only helps patients but also improves their quality of life.
As we learn more about dialysis access, we must focus on patient care. We should use new technologies and methods to manage grafts for dialysis. This helps patients overall.
FAQ
What is the difference between a graft and a fistula for dialysis?
A graft is a synthetic tube that connects an artery and vein. A fistula is a direct connection between an artery and vein made surgically. Both are used for dialysis, but they differ in characteristics and risks.
How can I prevent bleeding after dialysis?
To prevent bleeding, apply manual pressure correctly and position the access site right. Use specialized dressings or advanced bandage systems like IRIS.
What are the risks associated with hemodialysis compared to peritoneal dialysis?
Hemodialysis has a higher risk of bleeding due to anticoagulation and vascular access. Peritoneal dialysis is safer in this regard.
How do I manage bleeding from a dialysis fistula or graft?
Manage bleeding by applying manual pressure and elevating the limb. Seek medical help if bleeding doesn’t stop or is heavy.
What are the signs of a bleeding crisis with a dialysis access site?
Signs include heavy or uncontrollable bleeding, swelling, or pain. Seek immediate medical help if you see these symptoms.
How can I prevent aneurysms in my dialysis access site?
Prevent aneurysms with regular monitoring and proper cannulation. Early intervention is key if issues arise.
What are the treatment options for fistula arm swelling?
Treatment options include elevation, compression, and monitoring. Medical intervention may be needed for underlying causes.
When should I seek medical help after dialysis?
Seek medical help for heavy or uncontrollable bleeding, severe pain, swelling, or other concerning symptoms after dialysis.
How do I care for my dialysis access site at home?
Follow a daily maintenance routine and prevent infection. Adhere to activity restrictions to ensure the access site’s longevity.
What are the latest advancements in dialysis access management?
New materials and technologies, improved cannulation techniques, and personalized care are recent advancements. They aim to optimize dialysis access site management.
How do arteriovenous fistulas and grafts compare in terms of bleeding risk?
Arteriovenous fistulas have a lower bleeding risk than grafts. Both need proper care and monitoring to minimize risks.
What is the role of anticoagulation in post-dialysis bleeding?
Anticoagulation increases the risk of bleeding after dialysis. Careful management of anticoagulation therapy is essential.
Can I manage a bleeding fistula emergency at home?
Initial steps like applying manual pressure can be done at home. But, it’s best to seek medical attention for a bleeding fistula emergency to ensure proper care and minimize risks.
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from
References
https://my.clevelandclinic.org/health/treatments/14618-dialysis
































