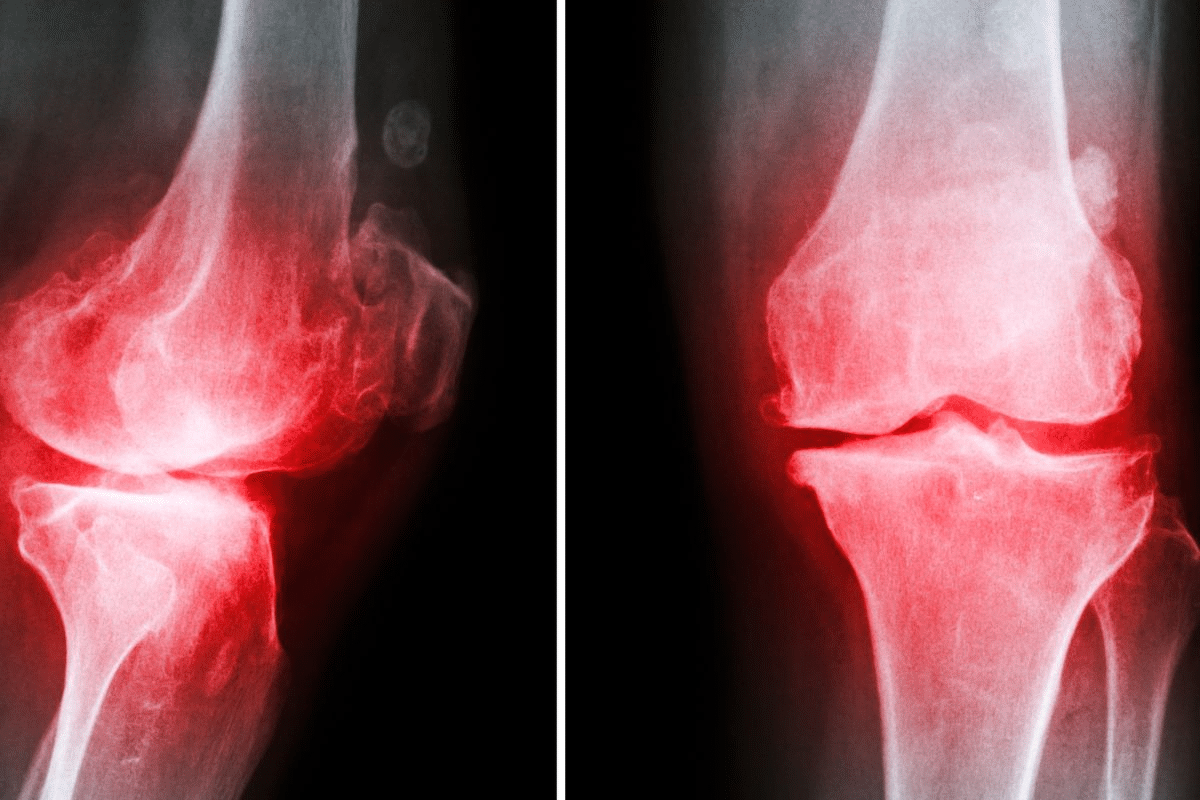
Inflammatory joint disease affects millions worldwide. Nearly 1 in 5 American adults have arthritis, says the Centers for Disease Control and Prevention.
AtLiv Hospital, we understand the impact of joint pain, swelling, or stiffness on your life. Early diagnosis and treatment can stop long-term disability. We are committed to giving you the best care.
Our goal is to help you manage inflammatory conditions well. We want to help you feel better with top medical care and care that focuses on you.
Key Takeaways
- Inflammatory joint disease is a big health problem worldwide.
- Early diagnosis is key to avoiding long-term disability.
- Liv Hospital offers full care for managing inflammatory conditions.
- Personalized treatment plans are made for each patient’s needs.
- Advanced medical treatments and support services are available.
Understanding Joint Inflammation
It’s important to know what causes joint inflammation to manage it well. This condition can make simple tasks hard. Let’s explore the causes and symptoms to understand it better.
What Causes Inflammation in Joints
Many things can cause joint inflammation. Autoimmune diseases, like rheumatoid arthritis, are a big reason. In these diseases, the body attacks the joints. Wear and tear, seen in osteoarthritis, is another major factor. Infections, injuries, and some medicines can also cause it.
Autoimmune diseases play a big role in joint inflammation. In cases like rheumatoid arthritis, the immune system attacks the joints. This leads to pain, swelling, and can damage the joints. Knowing the causes helps doctors find the right treatment.
|
Cause |
Description |
Common Symptoms |
|---|---|---|
|
Autoimmune Conditions |
Rheumatoid arthritis, where the immune system attacks the joints. |
Pain, swelling, stiffness |
|
Wear and Tear |
Osteoarthritis, resulting from joint cartilage breakdown. |
Pain, limited mobility |
|
Infections |
Bacterial or viral infections that cause joint inflammation. |
Redness, warmth, swelling |
Signs and Symptoms to Recognize
It’s key to know the signs of joint inflammation for early treatment. Look out for pain, swelling, redness, and warmth. Stiffness, mainly after rest, is also common.
Watching for these signs and seeing a doctor if they don’t go away is important. Early treatment can greatly help manage joint inflammation.
Types of Inflammatory Joint Disease
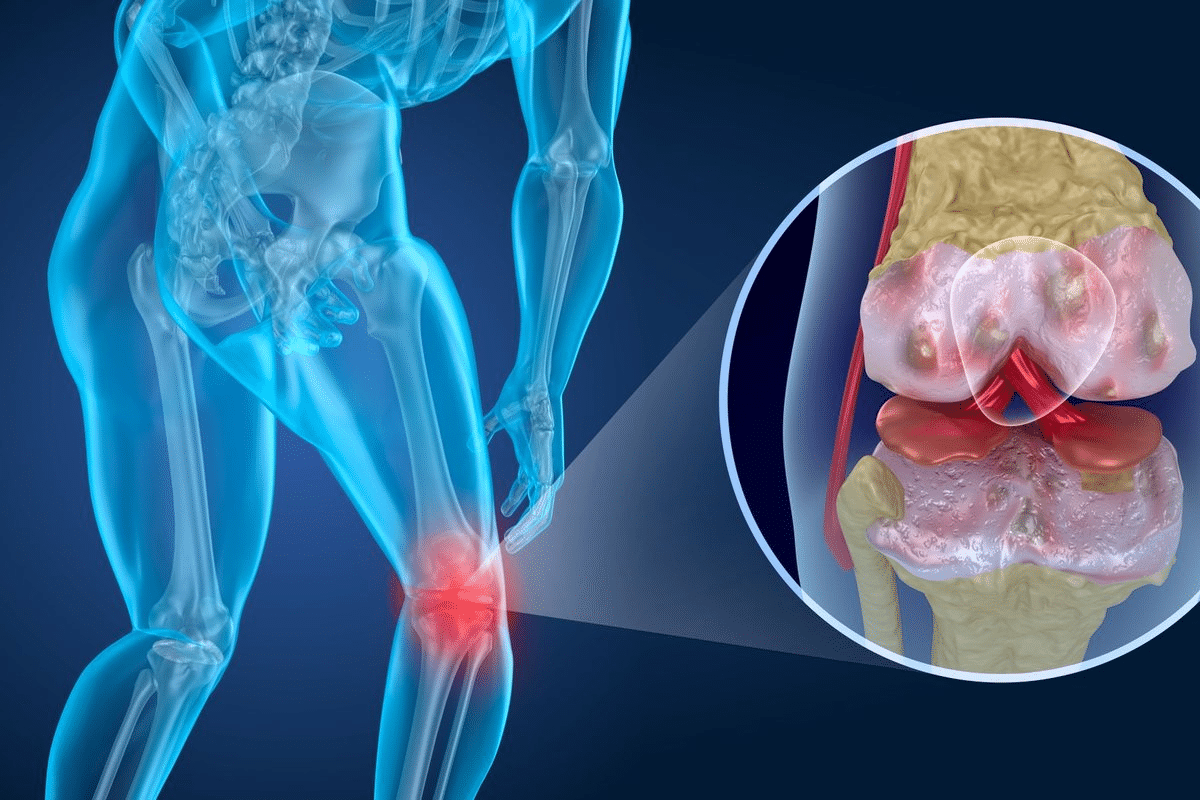
It’s important to know about the different types of inflammatory joint diseases. These conditions can really hurt your quality of life. They cause pain, stiffness, and make it hard to move.
Rheumatoid Arthritis
Rheumatoid arthritis (RA) is a chronic condition that mainly affects the joints. It causes inflammation, pain, and can damage the joints over time. If one hand is affected, the other hand usually is too.
Key characteristics of RA include:
- Mornings stiffness lasting more than an hour
- Symmetrical joint involvement
- Rheumatoid nodules
- Positive rheumatoid factor or anti-CCP antibodies in the blood
Osteoarthritis
Osteoarthritis (OA) is the most common arthritis. It’s often called “wear and tear” arthritis. It happens when cartilage in joints breaks down, causing pain. Unlike RA, OA is not an autoimmune disease but a degenerative condition.
|
Characteristics |
Rheumatoid Arthritis |
Osteoarthritis |
|---|---|---|
|
Nature of Disease |
Autoimmune |
Degenerative |
|
Joint Involvement |
Symmetrical |
Asymmetrical |
|
Primary Symptoms |
Pain, stiffness, swelling |
Pain, stiffness, limited mobility |
Gout and Pseudogout
Gout is a type of inflammatory arthritis. It causes sudden, severe pain, redness, and tenderness in the joints. It often happens at the base of the big toe.
Pseudogout, or calcium pyrophosphate deposition disease (CPPD), is similar to gout. But it’s caused by calcium pyrophosphate dihydrate crystals instead of urate crystals.
“Gout is a very painful condition that can significantly impact a person’s quality of life. Managing it requires a complete approach that includes medication, lifestyle changes, and dietary adjustments.” – Medical Expert
Psoriatic Arthritis and Other Forms
Psoriatic arthritis (PsA) is a type of arthritis that happens in some people with psoriasis. It causes joint pain, stiffness, and swelling. It can also lead to eye inflammation.
Other types of inflammatory joint disease include juvenile idiopathic arthritis, ankylosing spondylitis, and reactive arthritis. Each has its own characteristics and treatment methods.
We know that everyone’s experience with inflammatory joint disease is different. Knowing the specific type and its characteristics is key to finding the right treatment.
Diagnosing Joint Inflammation
Getting a correct diagnosis for joint inflammation is key to managing it well. Knowing the cause helps doctors create a treatment plan that works.
Medical Tests and Examinations
Doctors use tests and exams to find out about joint inflammation. They might do:
- A physical check to see how joints move and feel
- Blood tests to look for signs of inflammation or specific antibodies
- Imaging like X-rays, ultrasound, or MRI to see joint damage
- Joint aspiration to check for infection or certain types of arthritis
These steps help doctors tell if it’s rheumatoid arthritis, osteoarthritis, or gout.
Working with Healthcare Providers
It’s important to work closely with doctors for a correct diagnosis. Be ready to talk about your symptoms in detail. Share when they started, how long they last, and what makes them better or worse.
Keeping a symptom journal is a good idea. It helps doctors understand your condition better.
Tracking Your Symptoms
Tracking your symptoms is a big part of getting diagnosed. By paying close attention, you can give doctors the info they need.
Consider using a symptom tracking app or a simple log. Record:
- The pain and stiffness levels
- How symptoms affect your daily life
- Any changes in symptoms over time
This helps not just in diagnosing but also in making a treatment plan that fits you.
Pharmaceutical Approaches to Reduce Joint Inflammation
Pharmaceutical methods are key in fighting joint inflammation. They help ease symptoms, slow disease growth, and boost life quality. We’ll look at the different medicines, both over-the-counter and prescription, and how to handle side effects.
Over-the-Counter Options
Over-the-counter (OTC) drugs are often the first choice for joint inflammation. Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and naproxen are used to lessen pain and swelling. They block enzymes that cause inflammation, helping many people feel better.
But, it’s important to use OTC drugs wisely. Taking too much or for too long can cause stomach problems. Always talk to a doctor before starting any OTC treatment.
Prescription Medications
For serious joint inflammation, prescription drugs are needed. Disease-modifying antirheumatic drugs (DMARDs) and biologics are used for conditions like rheumatoid arthritis. These medicines target specific inflammation pathways, bringing significant relief.
Biologics have changed how we treat inflammatory joint diseases. They aim at specific molecules in the inflammation process, giving a more precise treatment than traditional DMARDs.
Managing Medication Side Effects
While medicines are effective, dealing with side effects is key. NSAIDs can cause stomach problems and increase bleeding risk. DMARDs and biologics may raise infection risk and affect liver health.
To lessen these risks, regular check-ups with doctors are vital. Changing doses or switching medicines can help manage side effects while keeping benefits.
By knowing the different medicines and working with doctors, people can manage joint inflammation well. This improves their life quality greatly.
Nutritional Strategies for Fighting Joint Inflammation
The food we eat is key in fighting joint inflammation. Making smart food choices can greatly improve joint health. Understanding nutritional strategies is important.
Anti-Inflammatory Diet Principles
An anti-inflammatory diet includes foods rich in antioxidants, omega-3s, and fiber. Eating a variety of fruits, vegetables, whole grains, and lean proteins is vital. Drinking plenty of water is also important.
It’s best to cut down on processed foods, sugars, and saturated fats. These can make inflammation worse. Eating whole, unprocessed foods is a good way to follow an anti-inflammatory diet.
Foods That Combat Inflammation
Some foods are known to fight inflammation. These include:
- Fatty fish like salmon and sardines, rich in omega-3 fatty acids
- Berries, which are high in antioxidants
- Green leafy vegetables, rich in various vitamins and minerals
- Nuts and seeds, good sources of healthy fats and antioxidants
- Olive oil, a key component of the Mediterranean diet, known for its anti-inflammatory effects
Foods to Limit or Avoid
Some foods can make inflammation worse. Foods to limit or avoid include:
- Processed meats, which are high in advanced glycation end (AGE) products that stimulate inflammation
- Refined carbohydrates and sugars, which can lead to increased inflammation
- Foods high in saturated and trans fats, such as fried foods and certain processed snacks
Being mindful of portion sizes and overall dietary patterns is key. Avoiding these foods can help manage joint inflammation.
Supplements for Joint Health
Some supplements can also support joint health. These include:
- Omega-3 fatty acid supplements, for their anti-inflammatory effects
- Glucosamine and chondroitin, often used to support cartilage health
- Turmeric/Curcumin, known for its potent anti-inflammatory properties
- Vitamin D, important for overall bone health
Always talk to a healthcare provider before starting any new supplements. This ensures they are safe and effective.
Physical Approaches to Managing Inflammatory Joint Disease
Physical methods are key to managing inflammatory joint disease and improving life quality. We will look at different ways to ease symptoms and boost mobility.
Appropriate Exercise Types
Exercise is vital for managing inflammatory joint disease. Gentle activities like yoga, swimming, and cycling keep joints moving without too much stress.
These activities also make joints more flexible. They strengthen the muscles around the joints, giving better support and less pain.
Physical Therapy Techniques
Physical therapy is a powerful tool for managing inflammatory joint disease. Methods like manual therapy, therapeutic exercises, and modalities like heat or cold therapy are customized for each person.
Physical therapists help create special exercise plans. These plans aim to improve joint function and lessen discomfort.
Rest and Activity Balance
It’s important to balance rest and activity for managing inflammatory joint disease. Rest helps lower inflammation, while the right amount of activity keeps joints moving.
Listening to your body and adjusting your activity levels based on symptoms is key. This prevents overdoing it.
Assistive Devices and Supports
Assistive devices can greatly help daily life for those with inflammatory joint disease. Items like canes, walkers, and orthotic supports reduce strain on affected joints.
|
Device |
Purpose |
Benefit |
|---|---|---|
|
Canes |
Reduce weight-bearing stress on joints |
Improved mobility and reduced pain |
|
Walkers |
Provide additional support and stability |
Enhanced safety and confidence |
|
Orthotic Supports |
Support and stabilize joints |
Reduced strain and improved function |
Lifestyle Modifications for Long-Term Joint Health
Improving joint health for the long term needs a few key changes in lifestyle. By making these changes, people can greatly enhance their joint health and overall well-being.
Weight Management Strategies
Keeping a healthy weight is key to reducing joint strain, mainly in hips, knees, and ankles. Extra weight can make joint inflammation worse, so managing weight is vital. A balanced diet and regular exercise are good ways to manage weight.
It’s best to lose 1-2 pounds a week for a healthy pace. This can be done by eating better and being more active. Talking to a healthcare provider or nutritionist can help make a weight loss plan that fits you.
Stress Reduction Techniques
Stress can harm joint health by causing more inflammation. Techniques like meditation, deep breathing, and yoga can help reduce stress. These activities also boost mental and physical health.
Doing stress-reducing activities regularly can lower inflammation and improve joint health. It’s important to find activities you enjoy and do them often.
Sleep Optimization
Good sleep is essential for joint health. Poor sleep or not enough sleep can make inflammation and pain worse. A consistent sleep schedule and a comfortable sleep environment can help improve sleep.
Ways to better sleep include avoiding caffeine and screens before bed, keeping a cool room, and getting a good mattress. Improving sleep habits can greatly benefit joint health.
Ergonomic Adjustments
Making ergonomic changes in daily life can help reduce joint strain. Using ergonomic furniture and tools designed to reduce body stress is important. Simple changes, like adjusting a computer monitor or using a supportive chair, can help a lot.
Also, being aware of how you sit and taking breaks to stretch can help. Using ergonomic practices at work and home can help keep joints healthy for a long time.
Alternative and Complementary Therapies
Many people are looking for new ways to manage joint inflammation. They are exploring alternative and complementary therapies. These methods can add extra benefits when used with traditional treatments.
Acupuncture and Acupressure
Acupuncture and acupressure are ancient healing methods. They involve stimulating certain points on the body. This helps with healing and pain relief.
Acupuncture uses thin needles, while acupressure uses fingers or tools to apply pressure.
Benefits: Both can lessen pain and swelling. They also improve joint function and overall health.
Massage and Manual Therapies
Massage therapy works by manipulating soft tissues. It aims to relax muscles, reduce tension, and boost circulation. Manual therapies, like chiropractic care and osteopathy, focus on aligning the body’s structure.
Benefits: These therapies can ease pain, soften stiffness, and enhance joint movement.
Heat and Cold Applications
Using heat or cold on joints can offer quick relief from pain and stiffness. Heat therapy, like warm baths or heating pads, relaxes muscles and increases blood flow. Cold therapy, with ice packs or cold compresses, cuts down inflammation and dulls pain.
|
Therapy Type |
Benefits |
Application |
|---|---|---|
|
Heat Therapy |
Relaxes muscles, increases blood flow |
Warm baths, heating pads |
|
Cold Therapy |
Reduces inflammation, numbs pain |
Ice packs, cold compresses |
Mind-Body Approaches
Mind-body therapies, like meditation, yoga, and tai chi, connect mental and physical health. These practices help lower stress, improve mood, and boost coping skills.
Benefits: Regular practice can manage chronic pain and inflammation better. It also improves overall health.
Conclusion: Creating Your Comprehensive Joint Inflammation Management Plan
We’ve looked at many ways to handle inflammatory joint disease. This includes medicines, diet, exercise, and lifestyle changes. Now, let’s put these together into a plan that fits you.
A good plan mixes all these strategies to fight joint inflammation. By using medicine, eating right, exercising, and changing your lifestyle, you can feel better. It’s smart to work with your doctor to make a plan that’s just for you.
To make your plan, first look at where you are now and what works best for you. Think about what you eat, how you move, and your lifestyle. A whole-body approach to fighting joint disease can lead to better results and fewer problems.
By using this complete method, you’re on the path to a plan that meets your needs. This will help improve your health and well-being.
FAQ
What is inflammatory joint disease?
Inflammatory joint disease is when joints get inflamed. This leads to pain, stiffness, and less mobility. Conditions like rheumatoid arthritis and osteoarthritis fall under this category.
How can I identify if I have joint inflammation?
Signs of joint inflammation include pain, swelling, and redness. You might also feel warmth and stiffness. If you notice these, see a doctor for help.
What are the causes of joint inflammation?
Many things can cause joint inflammation. Autoimmune diseases, wear and tear, infections, and metabolic disorders are some examples. Knowing the cause helps in managing it better.
What are the different types of inflammatory joint disease?
There are several types, like rheumatoid arthritis and osteoarthritis. Gout, pseudogout, and psoriatic arthritis are others. Each affects joints differently.
How is joint inflammation diagnosed?
Doctors use several methods to diagnose. They look at your medical history and do physical exams. They might also use X-rays or MRI and blood tests.
What are the treatment options for reducing joint inflammation?
There are many ways to treat joint inflammation. Medications like NSAIDs and biologics can help. Diet and exercise are also important. So is managing your weight and stress.
Can diet help manage inflammatory joint disease?
Yes, diet is key. Eating anti-inflammatory foods like fruits and whole grains helps. Avoiding processed foods is also good.
Are there any alternative therapies that can help with joint inflammation?
Yes, therapies like acupuncture and massage can help. Heat and cold treatments and mind-body approaches also offer relief. Always talk to a doctor first.
How can I manage my symptoms and prevent flare-ups?
Work with your doctor to manage symptoms. Keep track of your feelings and stick to your treatment plan. Making lifestyle changes and trying alternative therapies can also help.
Can exercise help with inflammatory joint disease?
Yes, exercise is beneficial. It improves mobility and strengthens muscles. Choose low-impact activities and get advice from a doctor or physical therapist.
How can I reduce inflammation in my joints naturally?
To reduce inflammation naturally, eat right and stay active. Follow an anti-inflammatory diet and manage your weight. Stress reduction and good sleep are also important.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://pubmed.ncbi.nlm.nih.gov/27156434/

































