Interventional radiology has changed the medical world. It offers new ways to treat patients without the need for big surgeries. Every year, over 2 million of these procedures are done worldwide. They help patients heal faster and do better.
Some procedures are really tough because they need a lot of skill and knowledge. Doctors must know a lot about the body’s structure and what’s wrong with it. This knowledge is key to doing these hard procedures right.
We’re going to look at the toughest interventional radiology procedures. We’ll see what makes them so hard and what skills are needed to get them done.
Key Takeaways
- Interventional radiology offers minimally invasive alternatives to traditional surgery.
- Complex procedures require advanced technical expertise and a deep understanding of anatomy and pathology.
- The hardest procedures demand precision and skill to achieve optimal patient outcomes.
- Understanding these challenges is key to moving the field forward.
- Expertise in interventional radiology is vital for handling complex cases.
Understanding Interventional Radiology: A Brief Overview
Interventional radiology is a medical field that uses imaging and therapy together. It offers a new way to diagnose and treat many health issues.
Definition and Scope of Interventional Radiology
Interventional radiology uses imaging to guide minimally invasive procedures. It has changed how we treat many conditions, making surgery less common.
This field covers a wide range of treatments. It includes vascular and non-vascular interventions, like biopsies and tumor treatments.
Evolution of Minimally Invasive Techniques
Minimally invasive methods have grown a lot over time. This is thanks to better imaging and tool design.
New materials and devices help interventional radiologists do complex tasks safely and accurately.
|
Technique |
Description |
Benefits |
|---|---|---|
|
Angioplasty |
Procedure to widen narrowed or obstructed arteries |
Restores blood flow, reduces symptoms |
|
Embolization |
Procedure to block blood flow to a specific area |
Controls bleeding, reduces tumor size |
|
Ablation |
Procedure to destroy diseased tissue |
Minimally invasive treatment for tumors |
The Interventional Radiologist’s Skillset
Interventional radiologists need special skills. They must know vascular anatomy well and be good with imaging. They also need to be skilled with catheters and other tools.
They can handle complex cases, make fast decisions, and work well under pressure.
Factors That Determine Procedure Difficulty in Interventional Radiology
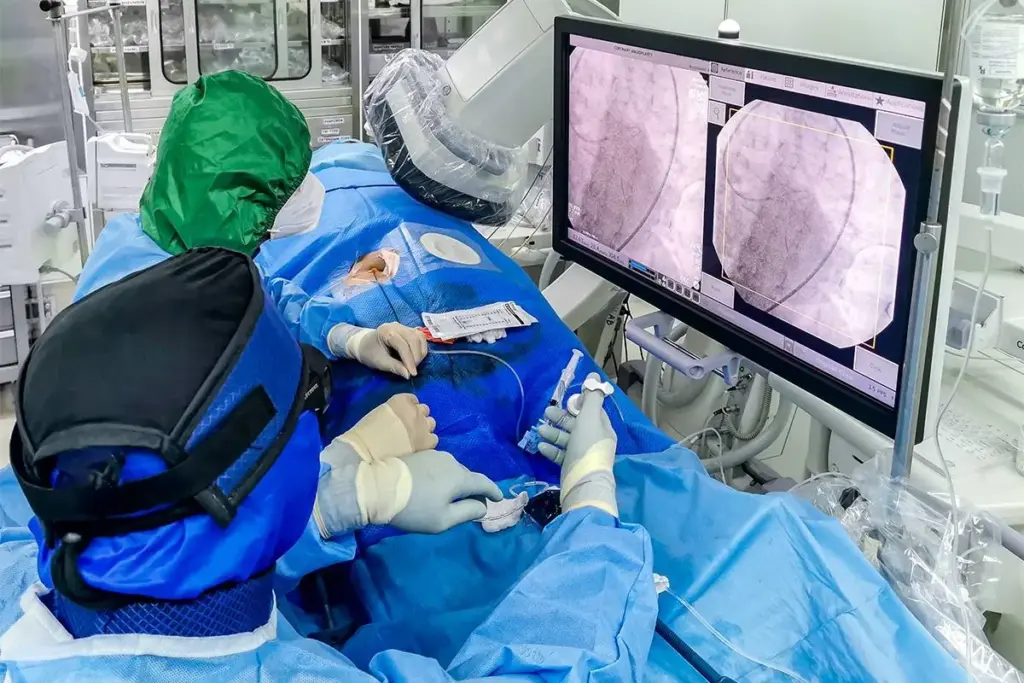
It’s key for interventional radiologists to know what makes procedures hard. They do many minimally invasive procedures, each with its own challenges.
Technical Complexity and Equipment Requirements
The technical part of interventional radiology is a big factor in how hard a procedure is. It needs advanced tools and skills. For example, transjugular intrahepatic portosystemic shunt (TIPS) creation is very technical.
New technology, like 3D roadmapping and fusion imaging, makes procedures more complex. But it also makes them more accurate and successful. Radiologists need to keep up with new tech to handle tough procedures well.
Anatomical Challenges and Variations
Every patient’s body is different, which can make procedures harder. Knowing each patient’s body is key to success. For example, different blood vessel layouts can make embolization or angioplasty harder.
Patient-Specific Risk Factors
Things like health problems, allergies, and past surgeries can make procedures harder. For example, patients with serious health issues might need special care. Radiologists must consider these factors to make the procedure right for each patient.
Time Constraints and Emergency Situations
Doing procedures quickly, like in emergencies, adds to the challenge. Situations like acute hemorrhage or stroke require fast decisions. Radiologists must be ready to act fast while keeping the patient safe.
Transjugular Intrahepatic Portosystemic Shunt (TIPS): The Technical Challenge
The Transjugular Intrahepatic Portosystemic Shunt (TIPS) is a complex procedure in interventional radiology. It’s used to handle issues like variceal bleeding and refractory ascites due to portal hypertension.
Procedure Overview and Indications
The TIPS procedure creates a shunt between the hepatic and portal veins to lower portal pressure. It’s done by accessing the hepatic vein through the jugular vein. It’s used for variceal bleeding that doesn’t respond to endoscopy and for refractory ascites.
Why TIPS is Considered Technically Demanding
TIPS faces several technical challenges. These include precise navigation of the portal venous anatomy and the risk of complications. It also requires careful post-procedure care. The procedure needs a skilled and experienced interventional radiologist.
Navigating Portal Venous Anatomy
Understanding the portal venous anatomy is key in TIPS. It involves knowing the portal vein and its branches. Advanced imaging helps in this process.
|
Anatomical Consideration |
Challenge |
Solution |
|---|---|---|
|
Portal Vein Location |
Difficulty in accessing the portal vein |
Use of advanced imaging techniques |
|
Variations in Portal Venous Anatomy |
Increased risk of procedural complications |
Pre-procedure planning and anatomical understanding |
Complication Rates and Management
Despite challenges, TIPS is effective in managing portal hypertension complications. Complications include shunt dysfunction and hepatic encephalopathy. Managing these is key to the procedure’s success.
Choosing the right patients, using precise techniques, and providing thorough care after the procedure are vital. They help reduce the risk of complications with TIPS.
Neurointerventional Procedures: Navigating the Brain’s Vascular Maze
Neurointerventional procedures are a key area in modern medicine. They offer hope to those with complex brain vascular conditions. These procedures involve complex brain anatomy, making them technically challenging.
Techniques like cerebral aneurysm coiling, AVM embolization, and mechanical thrombectomy treat serious conditions. They are used to save lives.
Cerebral Aneurysm Coiling Techniques
Cerebral aneurysm coiling is a minimally invasive method to treat brain aneurysms. It involves placing coils in the aneurysm to stop bleeding. The challenge is navigating the delicate brain structures around the aneurysm.
Arteriovenous Malformation (AVM) Embolization Challenges
AVM embolization is a complex procedure that blocks abnormal brain blood vessels. The main challenges are navigating through twisted vessels and ensuring the embolic material reaches the AVM without harming the brain.
- Understanding the AVM’s angioarchitecture
- Choosing the right embolic agent
- Navigating through complex vascular anatomy
Mechanical Thrombectomy for Acute Stroke
Mechanical thrombectomy has changed acute ischemic stroke treatment. It quickly removes blood clots. This procedure needs quick action and precise technique to restore brain blood flow.
The success of mechanical thrombectomy depends on several factors. These include how long it takes to start the procedure, the clot’s location, and the patient’s health.
Complex Biliary Interventions: When Standard Approaches Fail
Complex biliary interventions are key when usual methods don’t work. They tackle tough biliary blockages and other issues that simple methods can’t handle.
Percutaneous Transhepatic Biliary Drainage
Percutaneous transhepatic biliary drainage (PTBD) helps with biliary blockages. It uses a catheter to drain bile from the liver. PTBD is great when other methods don’t work.
Doing PTBD is tricky. It involves going through the liver to reach the bile ducts. It’s important to avoid bleeding or infection and place the catheter right. Advanced imaging helps a lot.
Biliary Reconstruction Procedures
Biliary reconstruction is needed for serious damage or blockages. It makes new paths for bile or fixes damaged ducts. The aim is to keep bile flowing and protect the liver.
- Biliary-enteric anastomosis: Makes a connection between the biliary system and the intestine.
- Bile duct repair: Fixes or rebuilds damaged bile ducts.
Managing Complications in Biliary Interventions
Handling complications is vital in complex biliary work. Issues like infection, bile leaks, and damage to nearby areas can happen. Quickly spotting and fixing these problems is key.
Managing complications includes:
- Antibiotics for infections.
- Drainage or stenting for bile leaks.
- Embolization to stop bleeding.
Case Studies of Challenging Biliary Procedures
Looking at tough biliary procedure cases helps us understand the challenges. For example, a case with a complex blockage might show the use of both percutaneous and endoscopic methods for success.
Complex biliary interventions need skill, planning, and a focus on the patient. Knowing the challenges helps healthcare teams improve care and results for patients.
Pulmonary Arteriovenous Malformation Embolization: Precision Required
Precision is key in PAVM embolization. This procedure closes abnormal connections between pulmonary arteries and veins. It needs a deep understanding of the patient’s anatomy and advanced technical skills.
Anatomical Considerations and Imaging
Accurate imaging is vital for PAVM embolization success. We use CT angiography and angiography to see the malformation. Knowing the malformation’s size, location, and blood supply helps plan the embolization.
Technical Approach and Device Selection
Choosing the right devices is key in PAVM embolization. We often use coils or Amplatzer plugs. The device choice depends on the malformation’s size and location, and the patient’s vascular anatomy.
Preventing Non-Target Embolization
Preventing non-target embolization is a big challenge. We use careful device selection and precise deployment to reduce this risk. Advanced imaging helps ensure the embolization material goes to the right place.
Outcomes and Possible Complications
PAVM embolization is usually safe, but complications can happen. These include recurrence of the malformation, pleuritic chest pain, and device migration. Knowing these risks and how to manage them is key to providing top-notch care.
With careful planning, advanced technical skills, and a deep understanding of anatomy, we can improve our patients’ lives through PAVM embolization.
The Most Challenging Interventional Radiology Procedures in Oncology
Interventional oncology is key in cancer treatment. It uses minimally invasive methods to help patients. Cancer is complex, and radiologists face many challenges in treating it.
Radioembolization (Y-90) for Complex Liver Malignancies
Radioembolization, or Y-90 therapy, treats liver cancers. It uses radioactive microspheres to target tumors. This method is precise, aiming to harm tumors while sparing healthy tissue.
It’s complex because of the need for accurate dosing and navigating the liver’s blood vessels. Challenges include managing liver disease, dealing with liver anatomy, and avoiding side effects.
Difficult Tumor Ablations in Critical Locations
Tumor ablation destroys cancer cells. Tumors in hard-to-reach places make this procedure tough. Radiologists must plan carefully to avoid harming nearby tissues.
Technologies like microwave and cryoablation help. But, they need precise imaging and technique to work well.
Irreversible Electroporation (IRE) for Pancreatic Cancer
Irreversible electroporation (IRE) treats pancreatic cancer. It uses electrical pulses to kill cells. The pancreas’s location makes this procedure complex.
IRE requires general anesthesia and careful planning. It demands precision and teamwork among specialists.
Combination Therapies and Their Complexities
Combination therapies use different treatments together. This approach is complex but can be effective. It requires teamwork among specialists.
Managing interactions between treatments and monitoring side effects are challenges. Despite these, combination therapies can lead to better outcomes for complex cancers.
Vascular Access in Challenging Patient Populations
Getting reliable vascular access is key for many interventional radiology procedures. It’s even more important for patients who are hard to access. The right vascular access can greatly affect the success of these treatments.
Central Venous Occlusions and Recanalization
Central venous occlusions make it hard to get vascular access. Recanalization techniques help by opening up the blockage. We use advanced imaging and guidewires to get through.
Planning and doing the procedure carefully is vital. Knowing the venous anatomy well and using the right tools are essential for success.
|
Technique |
Description |
Success Rate |
|---|---|---|
|
Guidewire Recanalization |
Using a guidewire to traverse the occluded segment |
80% |
|
Rheolytic Thrombectomy |
Employing a device to break down the thrombus |
75% |
Pediatric Vascular Access Considerations
Pediatric patients need special care because of their small size and growing bodies. We adjust our methods to fit their needs, making sure access is safe and works well.
We often use micro-access techniques and smaller tools for kids. It’s also important to watch out for too much radiation.
Approaches for Patients with Anatomical Variations
Patients with unique anatomy need custom vascular access plans. Knowing their specific anatomy helps us come up with the best strategy.
Tools like 3D reconstruction imaging are very helpful in planning access for these patients. We also use flexible tools to handle complex anatomy.
Solutions for Difficult Access Scenarios
When usual vascular access methods don’t work, we find new ways. This might include using ultrasound guidance or other advanced tech to help access.
Working with other specialists is also key in complex cases. It helps us give our patients the best care possible.
Endovascular Aneurysm Repair (EVAR) Complexities
EVAR is a groundbreaking procedure but comes with its own set of challenges. It’s important to understand these complexities to improve patient care and the success of the procedure.
Fenestrated and Branched Endografts
Fenestrated and branched endografts have made EVAR more effective for complex aneurysms. They allow for blood flow to vital organs, treating patients who were once unsuitable for EVAR. But, these devices require precise planning and execution.
Key considerations include detailed imaging, customizing the endograft, and the technical skill needed. We also have to watch out for endoleaks and other complications.
Hostile Neck Anatomy Management
Managing patients with hostile neck anatomy is a big challenge in EVAR. This means the anatomy makes it hard to seal the endograft to the aortic wall. Techniques like extension cuffs and balloon molding can help, but careful planning is key.
We use advanced imaging to understand the anatomy and plan the best approach. This includes 3D reconstruction and fusion imaging.
Dealing with Tortuous Iliac Arteries
Tortuous iliac arteries are another challenge in EVAR. They can make it hard to deliver the endograft and increase the risk of injury. Techniques like pre-dilation and stiff wires can help, but we must avoid causing harm.
In some cases, using iliac conduits or external iliac artery stenting is necessary. Careful planning and the right techniques are essential.
Managing Endoleaks and Long-term Complications
Endoleaks and long-term complications are a big worry in EVAR. Endoleak surveillance is key to catching and managing these issues early. We use regular imaging to monitor for signs of endoleak or graft migration and act quickly if needed.
Managing endoleaks might involve additional procedures like embolization or cuff placement. Long-term follow-up is vital for early detection and management of these complications, ensuring the best outcomes for our patients.
Pediatric Interventional Radiology: Small Vessels, Big Challenges
Pediatric interventional radiology faces unique challenges. The small size and developing anatomy of patients require special techniques. We must adapt our methods to ensure effective treatment.
Technical Adaptations for Pediatric Patients
For pediatric patients, technical adaptations are key. We use smaller instruments and catheters. Techniques are also modified to fit the patient’s size and anatomy.
Advanced imaging technologies, like fusion imaging and 3D roadmapping, are vital. They help us see the complex anatomy of children. This allows for more precise interventions.
Sedation and Radiation Considerations
Sedation is critical for pediatric interventional radiology. It ensures the patient’s comfort and cooperation. We use various sedation techniques, from conscious sedation to general anesthesia, based on the patient’s needs.
Reducing radiation exposure is also important. We use low-dose radiation protocols and plan our imaging carefully. This is essential for pediatric patients, as they are more sensitive to radiation.
Challenging Pediatric Vascular Malformations
Vascular malformations in children are challenging to treat. We use embolization techniques and sclerotherapy to manage them. Our approach is tailored to the malformation and the patient’s health.
Managing vascular malformations requires collaborative care. We work with pediatric specialists to develop treatment plans. This ensures we address each patient’s unique needs.
Collaborative Approaches with Pediatric Specialists
Collaboration is vital in pediatric interventional radiology. It allows us to use the expertise of various specialists. We work as a team to plan and execute procedures, considering all aspects of the patient’s health.
- Regular multidisciplinary meetings to discuss complex cases
- Close communication with pediatricians and other specialists
- Tailoring treatment plans to the individual needs of each patient
By adapting our techniques and working together, we can achieve successful outcomes. This improves the quality of life for young patients.
Recanalization of Chronic Total Occlusions (CTOs)
Recanalizing CTOs is a big challenge in vascular medicine today. It needs skill, advanced tech, and knowledge of blood vessel anatomy. This is to open up blocked vessels after a long time.
Techniques for Peripheral Arterial CTOs
Peripheral arterial CTOs are tough because of their complex nature and varied anatomy. To tackle these, we use:
- Advanced wire and catheter systems for navigating tough lesions.
- Subintimal angioplasty for very hard cases.
- Re-entry devices to help in successful recanalization.
Venous Recanalization Challenges
Venous recanalization is also a big challenge. The main hurdles are:
- Going through blocked parts without harming the vein wall.
- Reducing the risk of blood clots going to the lungs.
- Handling the different shapes of veins and the presence of side veins.
Advanced Wire and Catheter Techniques
Using the latest in wire and catheter tech is key for CTO recanalization. This includes:
- Hydrophilic wires and catheters for better navigation.
- Catheter-directed therapies to manage issues and boost success.
New Technologies for CTO Crossing
New tech has made CTO recanalization better. Some new tools are:
- Special crossing devices for better handling of complex blocks.
- 3D roadmapping and fusion imaging for better vision and accuracy.
As we keep improving in interventional radiology, new tech and methods will help us more. This will lead to better results for patients and a better life for them.
Interventional Radiology Procedures in Trauma Settings
In trauma settings, interventional radiology is key. It helps manage life-threatening injuries. We use small techniques to stabilize patients and stop bleeding, improving care.
Embolization for Major Hemorrhage Control
Embolization is a main tool in trauma care. This method blocks blood flow to certain areas to stop bleeding. We choose the right agent based on the injury.
Success in embolization needs quick and accurate imaging. Our team works with trauma surgeons to pick the best treatment.
Challenges in the Hemodynamically Unstable Patient
Stabilizing unstable patients is tough. They need fast and effective care. We face issues with keeping them stable and dealing with complex blood vessels.
We use advanced imaging and top-notch equipment. Our skills in interventional radiology help us adapt to trauma care, improving outcomes.
Damage Control Interventional Radiology
Damage control interventional radiology uses small techniques to stabilize patients. It’s great when surgery is risky. This method helps control bleeding and keeps vital organs working.
By doing this, we improve patient care. Our team works together to find the best treatment, combining radiology with other care.
Multidisciplinary Approach to Trauma Interventions
Working together is key in trauma care. We team up with surgeons, intensivists, and others to plan care. This includes using interventional radiology.
This teamwork ensures patients get the right care. By combining our skills with others, we can save more lives.
The Role of Advanced Technology in Complex Interventional Radiology
Advanced technology is changing interventional radiology, making procedures more precise and safe. It’s helping us do more with less invasive treatments. New tech is key to pushing what’s possible in our field.
3D Roadmapping and Fusion Imaging Applications
3D roadmapping and fusion imaging are big steps forward. They give us real-time, detailed images for better guidance. Fusion imaging combines old images with live views, helping us avoid mistakes and improve results.
Robotic-Assisted Interventional Procedures
Robotic-assisted systems are a big leap. They give us more control and precision, making tough procedures easier. This tech is great for detailed work, like in neuro or vascular treatments.
Artificial Intelligence in Procedure Planning
Artificial intelligence (AI) is starting to help with planning. AI looks at lots of data to find the best treatments and predict issues. It’s early, but AI could make procedures safer and more successful.
Future Technological Developments
Looking ahead, technological advancements will keep improving interventional radiology. New tech like augmented reality and advanced biometrics will help us even more. Keeping up with these changes is essential for top-notch patient care.
Training and Expertise Required for Difficult Interventional Radiology Procedures
Interventional radiologists need a lot of education and training to handle complex procedures. The field is always changing, with new methods and tools coming out. So, they must have a wide range of skills to do these tough procedures.
Fellowship Training and Subspecialization Pathways
Fellowship programs give radiologists more education in interventional radiology. They get to practice with complex procedures. Subspecialization lets them focus on certain areas, making them even more expert.
Volume-Outcome Relationship in Complex Cases
The volume-outcome relationship is key in interventional radiology. Doing more procedures leads to better results. This shows how important experience is in handling tough cases.
The table below shows what training for interventional radiologists includes:
|
Training Component |
Description |
Importance |
|---|---|---|
|
Fellowship Training |
Advanced education in interventional radiology |
High |
|
Subspecialization |
Specialized training in specific areas of interventional radiology |
High |
|
Simulation Training |
Practicing rare or complex procedures in a simulated environment |
Medium |
|
Continuous Learning |
Ongoing education to stay updated with the latest techniques and technologies |
High |
Simulation Training for Rare Procedures
Simulation training is great for radiologists. It lets them practice rare procedures safely, without risking patients.
Maintaining Competency and Continuous Learning
Keeping up with the field is vital for radiologists. They must always learn new things to improve patient care.
As interventional radiology keeps growing, the need for good training and learning never stops.
Conclusion: Balancing Risk, Benefit, and Technical Feasibility in Complex Interventions
Complex interventional radiology procedures need a careful balance. We’ve looked at many procedures, like TIPS and neurointerventional procedures. We also talked about complex biliary interventions.
Each procedure has its own challenges. These include technical complexity, anatomical variations, and patient-specific risk factors. A detailed risk-benefit analysis is key to deciding if a procedure is feasible.
Interventional radiologists can improve patient care by understanding each procedure’s technical feasibility. They must consider the risks and benefits. This way, they can make sure patients get the best results and help the field grow.
FAQ
What is interventional radiology?
Interventional radiology is a medical field. It uses imaging to guide procedures. This is a less invasive option compared to surgery.
What makes an interventional radiology procedure difficult?
Several factors make a procedure hard. These include technical complexity and anatomical challenges. Patient-specific risk factors and time constraints also play a role.
What is the TIPS procedure, and why is it considered challenging?
The TIPS procedure creates a shunt to manage portal hypertension. It’s tricky because of the need for precise navigation in the portal vein.
What are some of the challenges associated with neurointerventional procedures?
Neurointerventional procedures, like cerebral aneurysm coiling, are complex. They require navigating the brain’s vascular anatomy. This poses significant technical challenges and risks.
How do interventional radiologists manage complications during complex procedures?
Radiologists get extensive training to handle complications. They learn to adapt to unexpected anatomy and patient-specific risks.
What is the role of advanced technology in interventional radiology?
Advanced technologies improve precision and safety. Tools like 3D roadmapping and fusion imaging are key. Robotic assistance and artificial intelligence also play a role.
What kind of training is required for interventional radiologists to perform complex procedures?
Radiologists need fellowship training and subspecialization. This is to gain the skills and expertise for complex procedures.
How do interventional radiologists stay updated with the latest techniques and technologies?
Radiologists keep up through continuous learning. They stay current with new techniques, technologies, and research.
What are some of the most challenging interventional radiology procedures in oncology?
Procedures like radioembolization for liver cancer are challenging. Tumor ablation in critical areas and irreversible electroporation for pancreatic cancer also pose difficulties.
How do interventional radiologists address vascular access challenges in patients?
Radiologists use various techniques to overcome vascular access issues. This includes recanalization and adapted approaches for patients with central venous occlusions or anatomical variations.
References
National Center for Biotechnology Information. Dealing with complications in interventional radiology. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC10957835/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News




























