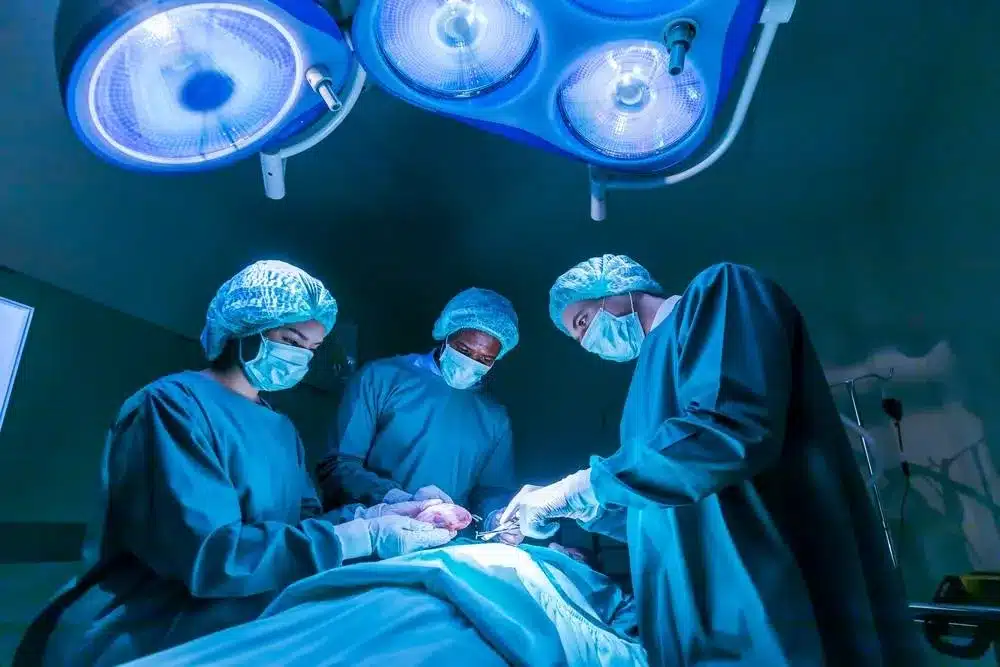
Becoming a surgeon is a tough goal. Some specialties are even harder. It takes dedication, perseverance, and a strong passion for medicine to get there.
Surgery has many specialties, each with its own hurdles. Neurosurgery is very detailed, while cardiothoracic surgery is very stressful. Becoming a skilled surgeon is a long and hard journey.
Key Takeaways
- The journey to becoming a surgeon is long and demanding.
- Different surgical specialties have unique challenges.
- Residency training is a critical component of a surgeon’s education.
- Certification is a high-stakes process that requires significant preparation.
- A strong passion for medicine is essential for success in surgery.
The Path to Becoming a Surgeon: An Overview
Becoming a surgeon is a long and challenging journey. It involves years of education and training. Aspiring surgeons must go through medical school, residency, and sometimes fellowship programs. Each step requires dedication, hard work, and a strong passion for surgery.
Medical School Requirements and Preparation
Medical school is the first step, lasting four years. Students learn a wide range of subjects, including clinical skills. Clinical rotations in the final years give them hands-on experience in various specialties, including surgery.
To stand out for surgical residencies, students need to do well in surgery rotations. Getting involved in research projects and surgical interest groups can also boost their applications.
“The art of surgery is long to learn, and life is short.” – Hippocrates
Residency Training Structure in the United States
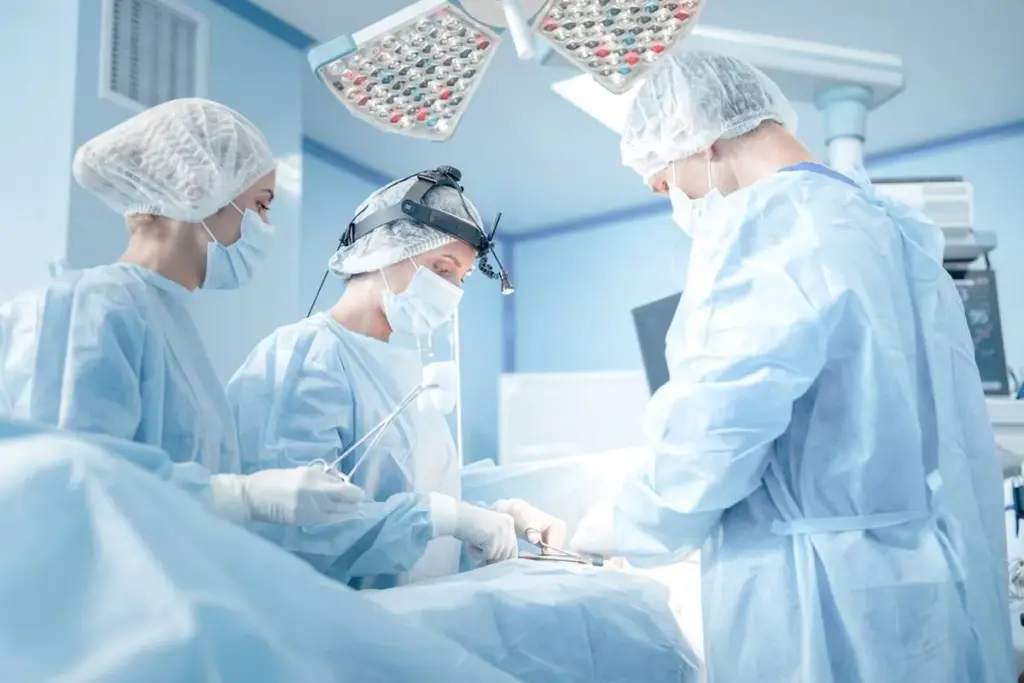
Residency training is a key part of a surgeon’s education. It provides hands-on experience under experienced surgeons. In the United States, these programs are accredited by the Accreditation Council for Graduate Medical Education (ACGME). They usually last:
- General Surgery Residency: 5-7 years
- Specialized Surgical Residencies: Variable lengths, often longer than general surgery
Residents learn surgical techniques, patient care, and decision-making. The training is intense, with long hours, to prepare them for surgical practice.
|
Type of Residency |
Duration (Years) |
|---|---|
|
General Surgery |
5-7 |
|
Orthopedic Surgery |
5 |
|
Neurosurgery |
7 |
Fellowship and Subspecialization Options
After residency, many surgeons pursue fellowship programs for specialized training. These programs focus on specific areas of surgery, such as:
- Pediatric Surgery
- Surgical Oncology
- Cardiothoracic Surgery
Fellowships last one to three years. They give surgeons the expertise to excel in their chosen subspecialty. The choice to pursue a fellowship is often driven by the desire to provide specialized care.
Factors That Determine the Difficulty of Surgical Specialties
Several key factors make some surgical specialties harder than others. It’s important for those thinking about a career in surgery to know these factors.
Competitiveness in Matching
The match rate shows how competitive a surgical specialty is. Specialties with low match rates are more competitive because there are fewer spots than applicants. For example, some specialties have a match rate under 80%, showing a tough environment.
Competitiveness in surgery depends on the program’s reputation, applicant quality, and available spots.
Length and Intensity of Training
The length and intensity of training greatly affect a specialty’s difficulty. Longer, more demanding programs are harder.
Some specialties need at least seven years of residency after medical school. Some even require more years for fellowship training.
Technical Complexity and Skill Requirements
The technical skills needed for a specialty also play a big role in its difficulty. Complex procedures and precise skills make some specialties tougher.
Surgeons in these areas need great hand-eye coordination, fine motor skills, and quick decision-making under pressure.
Work-Life Balance Challenges
Finding a good work-life balance is hard in many surgical fields. Long hours, night shifts, and being on call can harm a surgeon’s personal life.
Some specialties, like trauma or cardiothoracic surgery, are even harder. They require quick decisions and are high-stakes, making work-life balance even more challenging.
Ranking the Hardest Surgical Specialty: Methodology
To figure out which surgical specialties are the toughest, we looked at lots of data and talked to experts. We checked things like how many people match into each specialty, how many leave training early, and how hard the training is.
Match Rate Statistics and Trends
The match rate shows how competitive a specialty is. A low match rate means it’s really hard to get into. For example, neurosurgery and orthopedic surgery are very competitive because fewer people get in.
“The match rate is a key sign of how tough it is to get into a surgical field,” says a top expert in surgical education.
Looking at match rate trends helps us see how competitive specialties are changing. If match rates go down, it means it’s getting even harder to get in.
Attrition Rates and Training Difficulty
Attrition rates during training are very important. A high attrition rate means a specialty is really tough. This could be because the work is intense, the procedures are complex, or the training environment is challenging.
Surveys and feedback from residents and program directors also help us understand how hard a specialty is. They share what they find most challenging during training. a program director, says, “It’s not just about the technical skills. It’s also about the mental and physical stamina to handle long hours and high-pressure decisions.”
By looking at match rates, attrition rates, and how hard training is, we get a full picture of what makes a surgical specialty tough. This way, our ranking is based on a detailed analysis of all the factors that make a specialty challenging.
Neurosurgery: The Summit of Surgical Complexity
Neurosurgery is at the top of surgical challenges. It deals with brain, spinal cord, and nervous system disorders. It needs deep anatomy knowledge and precise surgery skills.
Seven-Year Training Pathway
Becoming a neurosurgeon takes at least seven years after medical school. This long training prepares them for complex surgeries.
Neurosurgeons learn a lot during their training. They get both theory and hands-on experience in neurosurgery. This ensures they can handle all kinds of cases.
Match Statistics and Applicant Profiles
Getting into neurosurgery residency is tough. The competition is high, with fewer spots than applicants. This makes it harder to match into a program.
|
Year |
Applicants |
Positions Available |
Match Rate (%) |
|---|---|---|---|
|
2022 |
243 |
117 |
48.1 |
|
2021 |
235 |
114 |
48.5 |
|
2020 |
228 |
109 |
47.8 |
Technical Challenges and Subspecialties
Neurosurgery has many subspecialties like spine and brain cancer surgery. Each has its own challenges. Neurosurgeons use advanced tools like radiosurgery and endovascular techniques.
Neurosurgery is very precise and demanding. It requires constant learning to keep up with new technologies. This ensures the best care for patients.
Pediatric Cardiovascular Surgery: Precision Under Pressure
Pediatric cardiovascular surgeons face high pressure. They need both technical skill and emotional strength. This field involves complex surgeries for children’s heart issues.
Extended Training Pathway
Training to be a pediatric cardiovascular surgeon is tough. It starts with medical school, then a cardiothoracic surgery residency. Often, there’s a fellowship in pediatric cardiovascular surgery next. This extended training pathway prepares surgeons well.
The typical training includes:
- A minimum of 4 years of medical school
- 5-7 years of residency training in cardiothoracic surgery
- 1-2 years of fellowship training in pediatric cardiovascular surgery
Technical Demands and Anatomical Challenges
Pediatric cardiovascular surgery is very technical. Surgeons must work with delicate tissues and fix complex heart defects. The small size and variability of children’s hearts add to the challenge.
|
Technical Skill |
Anatomical Consideration |
Challenge Level |
|---|---|---|
|
Microvascular surgery |
Small vessel size |
High |
|
Congenital defect repair |
Variability in defect type |
High |
|
Heart transplantation |
Matching donor and recipient |
Very High |
Emotional and Psychological Resilience
The emotional side of pediatric cardiovascular surgery is huge. Surgeons make critical decisions and deal with the emotional toll on families. Emotional resilience is key to handling these pressures.
Surgeons need ways to manage stress, like:
- Seeking support from colleagues and mentors
- Engaging in stress-reducing activities outside of work
- Maintaining a healthy work-life balance
Orthopedic Surgery: Highly Competitive and Physically Demanding
Orthopedic surgery is one of the most challenging fields in medicine. It needs a mix of technical skill, physical strength, and a competitive spirit.
Match Rate and Application Competitiveness
The competition in orthopedic surgery is high. Many qualified applicants compete for a few spots. To stand out, they must show exceptional academic achievement, research experience, and clinical skills.
Recent data shows the match rate for orthopedic surgery has stayed steady. There’s a slight increase in available positions. But, the competition is tough, with many needing to apply several times.
Physical Requirements and Technical Skills
Orthopedic surgery is both competitive and physically demanding. Surgeons need physical stamina for long, complex operations. They must also have precise technical skills.
Surgeons use various techniques and instruments. They must keep up with new advancements in orthopedic surgery. The challenges make it rewarding for those who excel.
Subspecialty Options and Additional Training
After residency, orthopedic surgeons can pursue fellowships. These programs focus on areas like sports medicine or joint reconstruction.
Subspecialty options let surgeons tailor their careers. This enhances their job satisfaction and helps advance the field.
Plastic Surgery: Artistry Meets Technical Precision
Plastic surgery is where art and science meet. It needs both skill and an eye for beauty. This mix makes it both tough and rewarding.
Integrated vs. Independent Pathways
There are two ways to become a plastic surgeon. The integrated pathway mixes plastic surgery with general surgery training for six years. The independent pathway needs a general surgery residency first, then a plastic surgery fellowship.
Choosing depends on what you want and your goals. The integrated way starts with plastic surgery right away. But, it’s very competitive with few spots.
Competitive Landscape and Match Statistics
Getting into plastic surgery is tough. Many skilled people apply. High USMLE scores and lots of research show how competitive it is.
To get noticed, you need to be top in school and show you’re serious about plastic surgery. A strong application is key in this competitive field.
Aesthetic and Reconstructive Challenges
Plastic surgeons face many challenges. They deal with the beauty of cosmetic surgery and the complex fixes after injuries or tumors. Aesthetic surgery requires understanding beauty and being skilled in surgeries like facelifts.
Reconstructive surgery is about fixing damage and restoring function. It’s complex and high-pressure. It needs great technical skills and the ability to handle tough situations.
Cardiothoracic Surgery: High Stakes and Demanding Training
Cardiothoracic surgery is known for its high-stakes environment and tough training. These surgeons are among the most skilled, handling complex heart, lung, and thoracic organ issues.
Traditional vs. Integrated Pathways
There are two main ways to train in cardiothoracic surgery. The traditional path involves a general surgery residency followed by cardiothoracic surgery training. Integrated programs, on the other hand, start right after medical school, blending both into a six-year program.
Key differences between traditional and integrated pathways include:
- Duration of training
- Curriculum structure
- Research opportunities
- Clinical exposure
|
Pathway |
Duration |
Structure |
|---|---|---|
|
Traditional |
Typically 7-8 years |
General surgery residency + cardiothoracic surgery fellowship |
|
Integrated |
6 years |
Combined general and cardiothoracic surgery training |
Technical Complexity and Evolving Technologies
Cardiothoracic surgery is very technical, with complex procedures on vital organs. The field keeps evolving with new tech, like minimally invasive and robotic-assisted surgeries. Surgeons must keep up with these advancements.
The technical challenges in cardiothoracic surgery include:
- Precision in delicate procedures
- Adaptation to new technologies
- Management of complex patient cases
Lifestyle Considerations and Burnout Rates
The demanding nature of cardiothoracic surgery affects lifestyle, with long hours and high stress. Surgeons must find a balance between work and personal life to avoid burnout.
Lifestyle considerations for cardiothoracic surgeons include:
- Work-life balance
- Stress management
- Support systems
Vascular Surgery: Complex Procedures and Evolving Techniques
Vascular surgery is a precise and adaptable field. It deals with complex procedures and new methods.
This surgery treats vascular diseases, excluding heart issues. Surgeons must know both old and new techniques.
Training Pathways and Duration
In the U.S., vascular surgery training takes at least seven years. It starts with five years of general surgery residency. Then, there’s a two-year fellowship in vascular surgery.
Training is tough to prepare surgeons for complex cases. They learn both open and endovascular methods.
Endovascular Skills and Traditional Techniques
Vascular surgeons use many techniques. They do open repairs and bypass grafting. They also do advanced endovascular procedures like angioplasty and stenting.
Endovascular skills have changed patient care. They make recovery faster and interventions more successful.
|
Technique |
Description |
Benefits |
|---|---|---|
|
Open Repair |
Traditional surgical method involving direct access to the affected vessel. |
Effective for complex cases, allows for direct repair. |
|
Endovascular Repair |
Minimally invasive technique using catheters and stents to repair vessels. |
Reduced recovery time, less invasive. |
Future Outlook and Technological Advances
The future of vascular surgery depends on new technology. This includes better imaging, devices, and materials. These will make surgeries more precise and successful.
As vascular surgery grows, new tech and methods are key. Surgeons must keep up with these changes to care for patients well.
Trauma Surgery: High Pressure and Unpredictability
Trauma surgery is known for its high-stakes environment. Surgeons must make quick decisions that can greatly affect patient outcomes. This field requires not just technical skill but also the ability to work under intense pressure.
Training Pathway and Critical Care Integration
The training for trauma surgeons is tough and includes critical care. This training prepares them to handle complex trauma cases and make fast decisions under pressure.
- Completion of a surgical residency program
- Fellowship training in trauma surgery
- Integration with critical care teams to manage complex patient care
Trauma surgeons must quickly assess situations and make life-saving decisions. Their training helps them deal with the unpredictability of trauma cases, where being able to adapt is key.
Lifestyle Impact and Call Schedules
The job of a trauma surgeon greatly affects their lifestyle. They often work irregular hours, including nights, and have to be ready to respond at any time.
Key lifestyle considerations include:
- Irregular working hours and night shifts
- Frequent on-call duties
- High levels of stress and the risk of burnout
Despite the challenges, many trauma surgeons find their work rewarding. They have the chance to save lives immediately.
Psychological Demands and Burnout Prevention
The psychological demands of trauma surgery are high. Surgeons face intense stress and traumatic cases. It’s important to prevent burnout to keep them well.
Effective strategies include:
- Mental health support services
- Peer support groups
- Regular breaks and time off to manage stress
By recognizing the psychological demands and using support systems, trauma surgeons can handle the job’s stresses better.
International Medical Graduates and Competitive Surgical Fields
For international medical graduates, the journey to become a surgeon is tough. They face extra hurdles like visa issues, cultural changes, and different medical education systems. These challenges make their path to surgery very hard.
Additional Challenges and Requirements
IMGs have unique hurdles in competitive surgical fields. These include:
- Visa and licensure rules that change by state and school
- Potential language barriers and cultural changes
- Different medical education and training standards
- More competition for limited spots in residency
To beat these challenges, IMGs need to be proactive. They must understand the U.S. surgical residency program requirements. This means getting the right visas, passing the USMLE series, and getting strong letters of recommendation.
Success Strategies for IMGs
Many IMGs succeed in getting into top surgical fields. Key strategies include:
- Looking for programs that accept IMGs
- Building a strong application with good USMLE scores and research
- Getting strong letters of recommendation from U.S. doctors
- Networking and making connections in the surgical field
The table below shows important stats and strategies for IMGs in competitive surgical fields:
|
Specialty |
Match Rate for IMGs |
Average USMLE Step 1 Score |
Recommended Strategies |
|---|---|---|---|
|
Neurosurgery |
20% |
240+ |
Research, strong recommendations |
|
Orthopedic Surgery |
25% |
245+ |
Away rotations, research |
|
Cardiothoracic Surgery |
15% |
250+ |
Research, networking |
By knowing the challenges and using smart strategies, IMGs can improve their chances in competitive surgical fields.
Strategies for Success in the Most Competitive Surgical Fields
To succeed in top surgical fields, you need a mix of academic success, research, and networking. Aspiring surgeons must put in a lot of time and effort. This builds a strong base for their careers.
Academic Excellence and Board Scores
Doing well in medical school is key. Focus on clinical rotations and board exams. High scores on these exams help you get into top residencies.
- Maintain a high GPA throughout medical school
- Excel in clinical rotations, specially in surgery
- Prepare well for board exams to get high scores
Research, Publications, and Presentations
Research and publishing are essential for a successful surgical career. They improve your skills and show your dedication to the field.
Key aspects of a successful research strategy include:
- Find areas you’re interested in and where research is needed
- Work with experienced researchers and mentors
- Get your work published in top journals
- Present your research at big conferences
Networking, Mentorship, and Away Rotations
Networking and finding good mentors are vital. Away rotations offer chances to try new places and meet people in your field.
Strategies for effective networking and mentorship include:
- Find mentors who can guide and support you
- Join professional groups and go to conferences
- Do away rotations at famous hospitals to learn and connect
By focusing on academic success, research, and networking, you can stand out in tough surgical fields.
Conclusion: Choosing Your Surgical Path
Starting a surgical career is a big decision. It involves looking at the challenges and benefits of different fields. Specialties like neurosurgery, pediatric cardiovascular surgery, and cardiothoracic surgery are very complex and competitive.
When picking a surgical path, think about what you’re interested in and what you’re good at. Knowing the training needed, the lifestyle, and the technical skills required for each field is key. Whether you’re into the detail of orthopedic surgery or the creativity of plastic surgery, choosing a field that fits your strengths and goals is important.
Being a surgeon takes hard work, determination, and a love for learning. By understanding the unique aspects of each specialty, you can make the most of your surgical career. This way, you can reach your goals in your chosen field.
FAQ
What is the most challenging surgical specialty to become?
Neurosurgery is the most challenging. It has a long training period, is very competitive, and is technically complex.
How long does it take to become a neurosurgeon?
It takes at least 7 years of residency after medical school. This makes the total training time about 11-12 years after college.
What are the key factors that determine the difficulty of a surgical specialty?
Difficulty depends on how competitive it is, the length and intensity of training, technical complexity, and work-life balance.
How competitive is cardiothoracic surgery?
It’s very competitive. It focuses on technical skills, research, and clinical experience. The match rate for these programs is low.
What are the challenges faced by international medical graduates in competitive surgical fields?
International medical graduates face visa issues, ECFMG certification, and fewer residency spots.
How can one succeed in highly competitive surgical specialties?
Focus on academic success, research, and networking. Gain clinical experience and build a strong professional network.
What is the role of fellowship training in surgical specialties?
Fellowship training offers advanced training in a specific area. It helps surgeons develop expertise and stay updated with new techniques.
How do surgical specialties impact work-life balance?
Some specialties require long hours, night shifts, and weekend work. This can affect personal and family life.
What are the technical demands of pediatric cardiovascular surgery?
It requires specialized skills to operate on small children with complex heart defects. It demands precision and delicacy.
How is plastic surgery both an art and a science?
Plastic surgery combines technical skill with artistic talent. Surgeons need to understand anatomy, aesthetics, and reconstructive techniques, and have an artistic eye.
What is the future outlook for vascular surgery?
Vascular surgery’s future will be shaped by new technologies. Advances in endovascular techniques and imaging will improve patient outcomes.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/37456122/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























