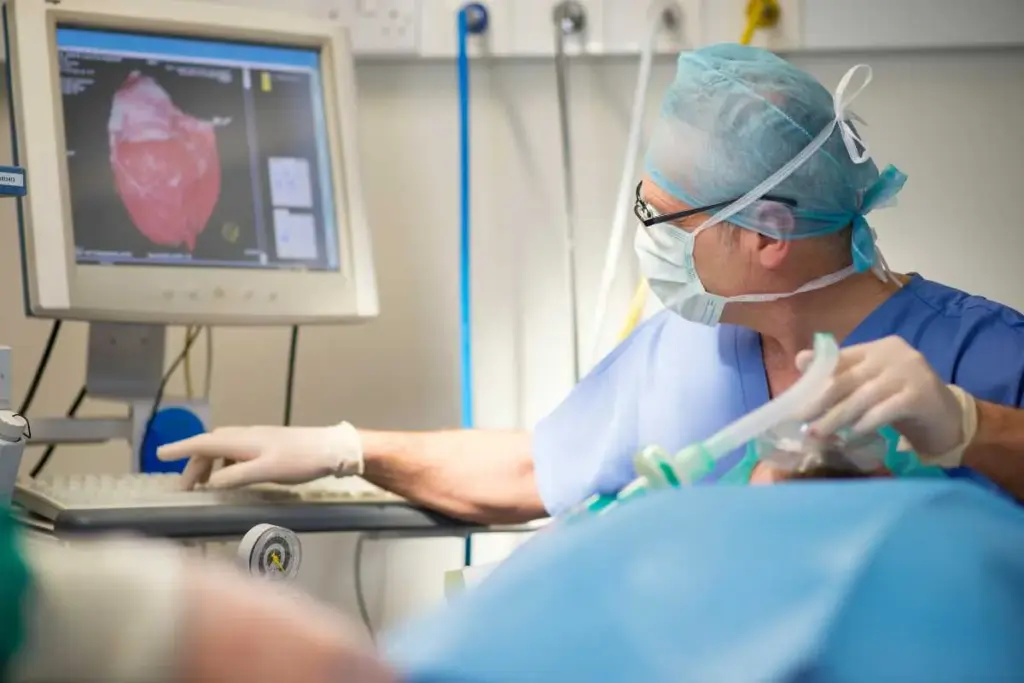
Nearly 6.2 million adults in the United States live with heart failure. This is when the heart doesn’t pump blood as effectively as it should. Accurate diagnosis is key to better care and outcomes.
Getting a serious diagnosis can be scary. Blood tests help spot heart failure and how severe it is. Doctors look at blood biomarkers to understand the condition and plan treatment.
Key Takeaways
- Heart failure is a serious condition affecting millions worldwide.
- Blood tests are key for diagnosing and understanding heart failure’s severity.
- Cardiac rehabilitation is vital for many patients’ recovery.
- Early diagnosis and treatment can greatly improve patient outcomes.
- Understanding the diagnosis is the first step towards effective management and recovery.
Understanding Heart Failure: An Overview
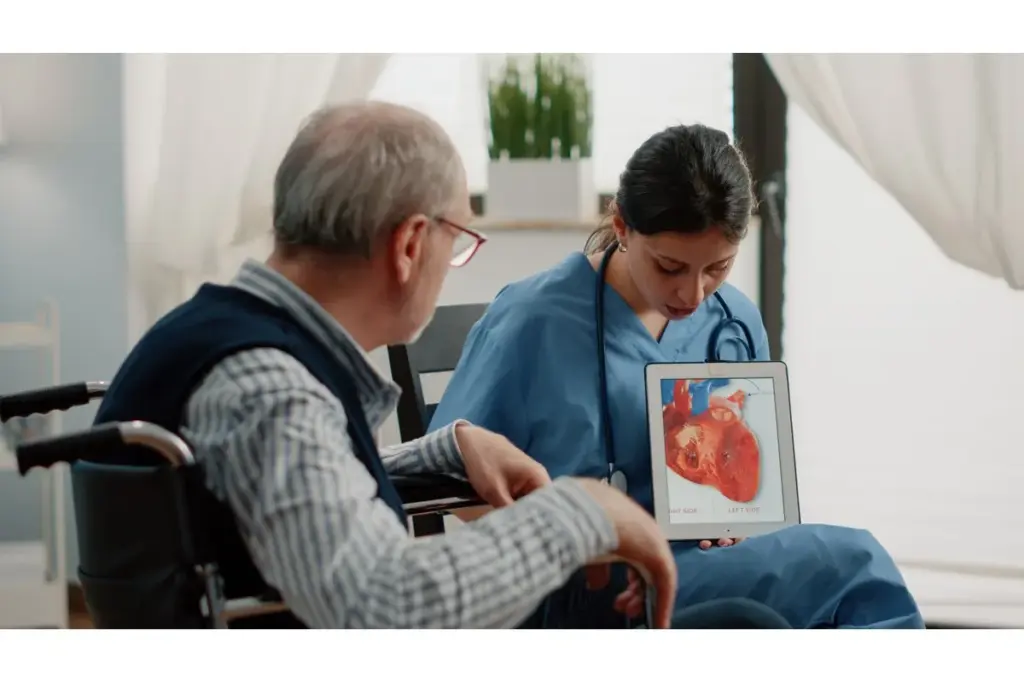
Heart failure is a big health problem worldwide. It’s expected to get worse as more people get older and have more health issues. This condition makes it hard for the heart to pump enough blood for the body’s needs.
What is Heart Failure?
Heart failure is when the heart can’t pump enough blood. This leads to tiredness, swelling, and trouble breathing. It really affects how well someone can live their life. It’s not the same as a heart attack, but a heart attack can cause heart failure.
Common Causes of Heart Failure
There are many reasons why heart failure happens. Damage to the heart muscle, like from heart attacks or cardiomyopathy, is one. High blood pressure, diabetes, and heart valve problems also play a part. Knowing these causes helps in preventing and managing heart failure.
Prevalence and Risk Factors
Heart failure affects millions globally, and it gets more common with age. Risk factors include high blood pressure, diabetes, being overweight, and a history of heart disease. Early identification and management of these risk factors are key to preventing or slowing heart failure. Cardiac rehab programs help manage heart failure and improve patient outcomes.
Understanding heart failure’s causes, risk factors, and how common it is helps us tackle it better. This way, we can improve the lives of those dealing with it.
The Role of Blood Tests in Heart Failure Diagnosis
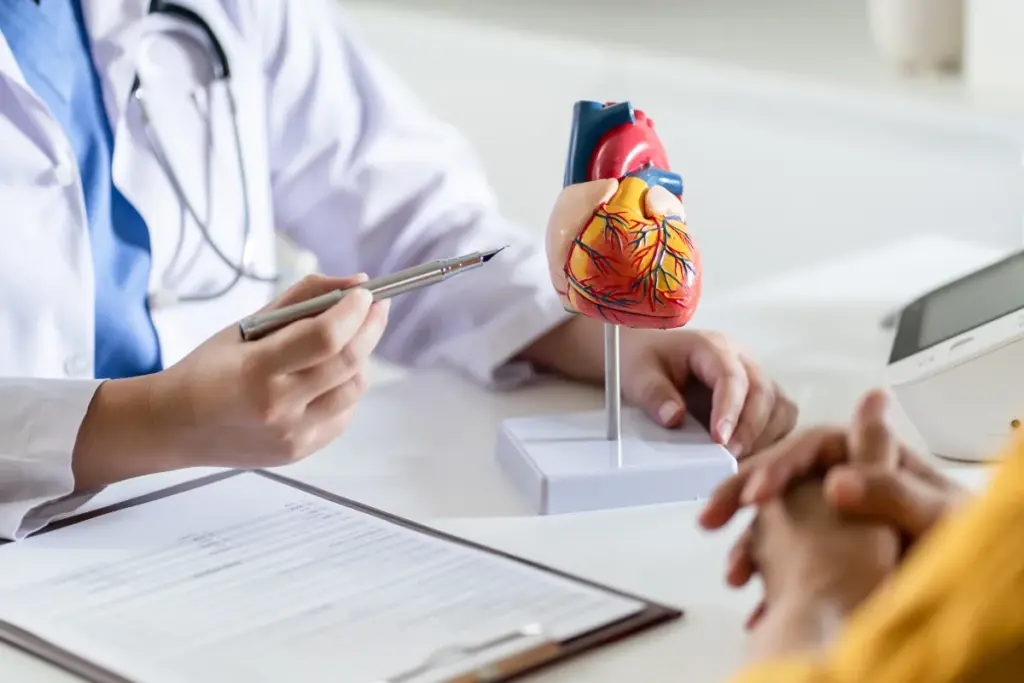
Blood tests are key in diagnosing heart failure. They measure cardiac biomarkers that show heart stress or damage. This gives us important insights into heart function.
Why Blood Tests Are Important
Blood tests are essential for diagnosing heart failure. They help find biomarkers linked to heart health. Cardiac biomarkers like B-type Natriuretic Peptide (BNP) and N-terminal pro-B-type Natriuretic Peptide (NT-proBNP) are critical. They show heart stress and damage.
Healthcare providers use these biomarkers to understand the heart’s state. They decide the best treatment. Early detection through blood tests can greatly improve patient outcomes by allowing for timely treatments.
|
Biomarker |
Significance |
Normal/Abnormal Levels |
|---|---|---|
|
BNP |
Indicates heart stress |
<100 pg/mL (normal) |
|
NT-proBNP |
Associated with heart failure severity |
<300 pg/mL (normal for <50 years) |
|
Troponin |
Indicates heart muscle damage |
<0.04 ng/mL (normal) |
Limitations of Blood Work in Heart Failure
Even though blood tests are vital, they have their limits. Dependence on blood work alone can result in incomplete diagnoses. Heart failure is complex and needs a full assessment.
Other tools like imaging tests and physical exams are also needed. A complete approach ensures accurate diagnosis and effective treatment planning.
Key Biomarkers for Heart Failure in Blood Tests
Diagnosing heart failure is complex, with blood tests playing a big role. These tests help find important biomarkers. These biomarkers show how well the heart is working and guide treatment.
Three biomarkers are key in diagnosing heart failure: BNP, NT-proBNP, and Troponin. They are important because they are reliable and show the heart’s health.
B-type Natriuretic Peptide (BNP)
BNP is a hormone made by the heart when it’s under stress. High BNP levels mean heart failure. A top cardiologist says BNP levels show how well the heart is doing.
BNP levels should be under 100 pg/mL. If they’re higher, it might mean heart failure and more tests are needed.
N-terminal pro-B-type Natriuretic Peptide (NT-proBNP)
NT-proBNP is linked to BNP and helps diagnose heart failure. It shows how severe heart failure is. The normal range for NT-proBNP changes with age.
Troponin Levels
Troponin is a protein in heart muscle cells. It’s in the blood when the heart muscle is damaged. Troponin is mostly for heart attacks but can also show heart failure.
Troponin levels show heart damage. Even small increases are important. They mean the heart is stressed. A cardiology expert says troponin helps plan treatment.
In summary, BNP, NT-proBNP, and troponin are vital for diagnosing and managing heart failure. Knowing about these biomarkers helps doctors care for patients better.
Other Blood Markers That May Indicate Heart Failure
Many blood tests can give insights into heart health, beyond the usual biomarkers. These tests help doctors understand a patient’s condition better. They guide further steps in diagnosis.
Complete Blood Count (CBC)
A Complete Blood Count (CBC) checks different parts of the blood. It looks at red and white blood cells and platelets. It’s not a direct test for heart failure but can show related issues like anemia or infections.
Anemia, for example, can make the heart work harder. This can worsen heart failure symptoms. Doctors can then create a better treatment plan based on these findings.
Metabolic Panel
A Metabolic Panel tests how the body’s metabolism works. It checks electrolyte levels, kidney function, and blood sugar. These are key to heart health, as imbalances can harm the heart.
Electrolyte imbalances, like potassium and sodium, can affect heart rhythm. Kidney disease, which this test also checks, raises heart failure risk. These tests help doctors understand heart health better.
Inflammatory Markers
Inflammatory markers, like C-reactive protein (CRP), show body inflammation. Chronic inflammation is linked to heart diseases, including heart failure.
High levels of these markers may mean a higher risk or presence of heart failure. Fighting inflammation is key in managing heart failure. This can involve lifestyle changes and medical treatments.
Looking at these extra blood markers helps doctors understand heart health better. They can then create a treatment plan that fits each patient’s needs.
Accuracy and Reliability of Blood Tests for Heart Failure
The accuracy of blood tests for heart failure depends on several factors. These include the biomarkers tested and the patient’s condition. Knowing these factors helps in understanding test results.
Sensitivity and Specificity
Sensitivity and specificity are key to blood test accuracy. Sensitivity shows a test’s ability to spot those with heart failure. Specificity shows its ability to spot those without it. Biomarkers like BNP and NT-proBNP are good at this.
A study showed BNP levels are high in heart failure patients. It had 85% sensitivity and 80% specificity. NT-proBNP is also useful, with a high negative predictive value.
Factors Affecting Test Results
Several factors can impact blood test accuracy for heart failure. These include:
- Age and gender: BNP and NT-proBNP levels change with age and gender.
- Kidney function: Poor kidney function can raise BNP and NT-proBNP levels.
- Obesity: Obesity might lower BNP levels, leading to false negatives.
- Comorbid conditions: Other health issues can affect biomarker levels.
When Blood Tests Might Miss Heart Failure
Blood tests are useful for diagnosing heart failure but can miss it in some cases. For example:
- Early stages of heart failure: Biomarker levels might not be high enough in the beginning.
- Presence of other conditions: Certain conditions, like kidney disease, can make biomarker levels hard to interpret.
- Technical issues: Lab errors or sample handling problems can affect test accuracy.
It’s important for healthcare providers to know these limitations. This helps them accurately interpret blood test results and make the right treatment decisions.
The Complete Heart Failure Diagnosis Process
To accurately diagnose heart failure, healthcare providers must conduct a thorough physical examination. They also assess the patient’s medical history and evaluate their symptoms. This approach helps in making a more accurate diagnosis and creating an appropriate treatment plan.
Physical Examination
A physical examination is key in diagnosing heart failure. Healthcare providers look for signs such as swelling in the legs, ankles, and feet. They also check for jugular venous distension, which can indicate fluid buildup.
Medical History Assessment
Understanding a patient’s medical history is vital. We review their past medical conditions, such as hypertension, diabetes, and coronary artery disease. These conditions are common contributors to heart failure.
Symptom Evaluation
Evaluating symptoms is a critical part of the diagnosis process. Patients with heart failure often experience shortness of breath, fatigue, and swelling. We assess the severity and duration of these symptoms to determine the stage of heart failure.
Imaging Tests for Heart Failure Diagnosis
Healthcare professionals use imaging tests to diagnose heart failure. These tests help understand the heart’s structure and function. This information is key for accurate diagnoses and treatment plans.
Echocardiogram
An echocardiogram is a non-invasive test that uses sound waves to create images of the heart. It shows the heart’s size, shape, and function. It also checks how well the heart chambers and valves work.
This test is great for spotting heart failure signs. It can show if the heart is not pumping well or if the heart walls are moving abnormally.
Chest X-ray
A chest X-ray is used to check heart failure. It shows images of the heart and lungs. Doctors look for heart enlargement or lung fluid buildup, signs of heart failure.
Even though it doesn’t measure heart function, a chest X-ray is helpful. It shows the heart’s size and lung congestion.
MRI and CT Scans
MRI (Magnetic Resonance Imaging) and CT (Computed Tomography) scans give detailed heart pictures. MRIchecks the heart’s structure and function, including muscle and valve condition. CT scans look at the heart’s structure and find coronary artery blockages.
Both MRI and CT scans are key for diagnosing heart failure. They help doctors see the heart’s condition clearly. This guides treatment choices.
|
Imaging Test |
Primary Use in Heart Failure Diagnosis |
|---|---|
|
Echocardiogram |
Assesses heart function, size, and valve operation |
|
Chest X-ray |
Evaluates heart size and detects lung congestion |
|
MRI |
Provides detailed images of heart structure and function |
|
CT Scans |
Assesses heart structure and detects coronary artery blockages |
Other Diagnostic Procedures for Heart Failure
Other tests are key in diagnosing heart failure, aside from blood tests and imaging. These tests help doctors understand how well the heart works. They also find out what might be causing heart failure and plan the best treatment.
Electrocardiogram (ECG/EKG)
An Electrocardiogram (ECG/EKG) is a simple test that checks the heart’s electrical activity. It can spot irregular heartbeats and signs of past heart attacks. Even though it can’t directly say if you have heart failure, it gives important info about the heart’s electrical activity.
The ECG is great for finding problems that might lead to heart failure. For example, it can find atrial fibrillation, a common problem in heart failure patients.
Stress Tests
Stress tests check how the heart works when it’s under stress, usually through exercise or medicine. They help find coronary artery disease, a big cause of heart failure. They also see how well the heart handles stress.
There are a few types of stress tests:
- Exercise stress test
- Nuclear stress test
- Stress echocardiogram
These tests are very important. They help doctors figure out and manage heart failure.
Cardiac Catheterization
Cardiac catheterization is a more detailed test. It involves putting a catheter into a blood vessel and guiding it to the heart. This test can find coronary artery disease, check the heart’s function, and spot problems in the heart’s chambers and valves.
During this test, doctors can also do things like angioplasty or stenting. These help open blocked arteries.
|
Diagnostic Procedure |
Purpose |
Key Findings |
|---|---|---|
|
Electrocardiogram (ECG/EKG) |
Measures electrical activity of the heart |
Irregular heart rhythms, signs of ischemia |
|
Stress Tests |
Evaluates heart function under stress |
Coronary artery disease, heart’s response to stress |
|
Cardiac Catheterization |
Assesses heart function and coronary arteries |
Blockages, abnormalities in heart chambers and valves |
These tests, along with others, give a full picture of heart failure. They help doctors find the best treatment.
When to Seek Medical Attention for Possible Heart Failure
Knowing when to get medical help for heart failure can save lives. Heart failure happens when the heart can’t pump blood well. Spotting its warning signs is key to getting help fast.
Warning Signs and Symptoms
Heart failure symptoms differ from person to person. But, common signs include:
- Shortness of breath during simple tasks or when lying down
- Fatigue and feeling weak
- Swelling in the legs, ankles, and feet
- Rapid or irregular heartbeat
- Coughing up pink, frothy mucus
- Swelling or pain in the abdomen
If you notice any of these signs, see your doctor right away. Early treatment can greatly improve heart failure outcomes.
Emergency Situations
Heart failure symptoms can sometimes become emergencies. If you or someone with you is facing:
- Severe trouble breathing
- Chest pain or pressure
- Fainting or severe dizziness
- Confusion or feeling disoriented
you must get help immediately. Call emergency services or rush to the nearest ER.
Preparing for Your Doctor’s Appointment
When you’re seeing your doctor for heart failure concerns, being ready is smart. Here’s how:
- Write down your symptoms and when they happen
- Remember any medicines you’re taking
- Bring a friend or family member for support
- Make a list of your questions and worries
Being ready can make your doctor’s visit more effective. It ensures your doctor has all the info needed for a correct diagnosis and treatment plan.
Treatment Options Following Heart Failure Diagnosis
After a heart failure diagnosis, doctors look at many treatment options. They aim to ease symptoms and slow the disease’s progress. The goal is to make the patient’s life better and increase their chances of survival.
Medication Approaches
Medicines are key in managing heart failure. They help lessen symptoms, slow the disease, and improve survival chances. Some common medicines include:
- ACE inhibitors: These relax blood vessels, easing the heart’s workload.
- Beta-blockers: They slow the heart rate and reduce its workload.
- Diuretics: Known as “water pills,” they reduce fluid buildup in the body.
- ARNI: A mix of medicines that replaces ACE inhibitors in some cases, providing extra benefits.
Doctors often mix these medicines to fit each patient’s needs.
Surgical Interventions
In some cases, surgery is needed to treat heart failure. It can fix problems that cause heart failure or improve heart function. Surgical options include:
- Coronary artery bypass grafting (CABG): It improves blood flow to the heart.
- Heart valve repair or replacement: It fixes valve problems that may cause heart failure.
- Implantable cardioverter-defibrillators (ICDs): Devices that prevent sudden death from dangerous heart rhythms.
- Cardiac resynchronization therapy (CRT): It helps the heart’s chambers beat in sync.
Lifestyle Modifications
Changing your lifestyle is also important in managing heart failure. This can include:
- Dietary changes: Eating less salt, managing fluid intake, and following a heart-healthy diet.
- Exercise: Doing regular, moderate exercise as advised by doctors.
- Smoking cessation: Quitting smoking to protect the heart further.
- Limiting alcohol: Reducing or avoiding alcohol.
By using these treatments together, heart failure patients can see better symptoms and quality of life.
Cardiac Rehabilitation Programs for Heart Failure Patients
Heart failure patients can greatly benefit from cardiac rehabilitation programs. These programs help improve heart health and overall well-being. They are a key part of the recovery process, helping patients regain strength and improve their heart health.
What is Cardiac Rehabilitation?
Cardiac rehabilitation is a program that includes exercise, education, and stress counseling. It’s made to help patients recover from heart failure and other heart issues. The goal is to improve health and lower the risk of future heart problems.
Phases of Cardiac Rehab
Cardiac rehab goes through several phases. The first phase starts in the hospital, with basic exercises and education. The second phase, after discharge, involves more intense workouts and education. The third phase is for long-term maintenance, done at home or in a community setting.
Cardiac Rehab Exercises
The exercise part of cardiac rehab is safe and effective. It includes aerobic, strength, and flexibility exercises. These are monitored by healthcare professionals to ensure they are done correctly and safely.
- Aerobic exercises, such as walking or cycling, to improve cardiovascular health
- Strength training to build muscle and enhance overall physical function
- Flexibility exercises to improve range of motion and reduce stiffness
Finding Cardiac Rehab Near You
Looking for a cardiac rehabilitation program? It’s important to find one that’s close and meets your needs. Ask your healthcare provider for suggestions or search online. Many hospitals and cardiac centers offer these services, so it’s worth asking about their programs.
Living with Heart Failure: Long-term Management
Managing heart failure long-term means watching your health closely. It’s about monitoring, testing, and changing your lifestyle. Knowing how to handle these parts is key to living well with heart failure.
Monitoring Your Condition
It’s important to watch for signs of heart failure getting worse. Look out for shortness of breath, swelling in your legs, or sudden weight gain. Keeping a symptom journal helps track changes and find patterns. This way, you can get help when you need it.
“The key to managing heart failure is early detection of changes in your condition,” says a leading cardiologist. “By being proactive and monitoring your symptoms closely, you can work with your healthcare team to adjust your treatment plan and prevent complications.”
Regular Follow-up Testing
Regular tests are key to seeing if your treatment is working. You might have echocardiograms, blood tests, and other tests. These help check how well your heart is working and your overall health.
- Schedule regular appointments with your healthcare provider to review your condition and adjust your treatment plan as needed.
- Keep track of your test results and ask questions if you’re unsure about your progress or any changes in your care.
Quality of Life Considerations
Heart failure care isn’t just about medicine. It’s also about living well. This means eating right, staying active, and managing stress.
“Living with heart failure requires a holistic approach that addresses not just the physical aspects of the condition but also the emotional and social well-being of the patient,” notes a healthcare professional. “By focusing on overall wellness, patients can lead fulfilling lives despite their diagnosis.”
By understanding the importance of monitoring, testing, and quality of life, you can manage your heart failure better. This helps improve your overall well-being.
Conclusion
Diagnosing and managing heart failure needs a full plan. This includes finding the problem, treating it, and keeping an eye on it. Blood tests are key in finding heart failure, using markers like BNP and NT-proBNP.
Other tests like imaging help find the problem too. Treatment can be medicines, surgery, or changes in lifestyle. Programs like cardiac rehab help patients live better with heart failure.
Living with heart failure means regular checks and tests. Knowing about heart failure helps patients make good choices for their health. We stress the need for a complete plan to help heart failure patients get the care they need.
FAQ
Does heart failure show up in blood work?
Yes, blood tests can show signs of heart failure. Biomarkers like BNP and NT-proBNP are used. But, blood tests are just one part of diagnosing heart failure.
What is cardiac rehabilitation, and how can it help heart failure patients?
Cardiac rehab is a program that helps patients recover from heart issues. It includes exercise, education, and support. It improves heart health and quality of life.
What are the phases of cardiac rehab?
Cardiac rehab has three phases: Phase 1 (inpatient), Phase 2 (outpatient), and Phase 3 (maintenance). Each phase focuses on different recovery aspects.
What exercises are typically included in cardiac rehab programs?
Rehab exercises include walking, cycling, swimming, and strength training. They are tailored to each person’s needs and health.
How do I find cardiac rehab programs near me?
Search online for rehab programs in your area. Ask your doctor for suggestions. Contact local hospitals or cardiac centers for more information.
Can exercise repair heart damage caused by heart failure?
Exercise can’t fix damaged heart tissue. But, regular activity in rehab can improve heart function and reduce symptoms.
How long does cardiac rehab typically last?
Rehab duration varies by individual and program. Phase 2 lasts several months. Phase 3 is ongoing.
What are the benefits of cardiac rehabilitation for heart failure patients?
Rehab improves heart health and reduces hospital risks. It also enhances quality of life and survival rates for heart failure patients.
Are there any disadvantages to cardiac rehabilitation?
Some may feel tired or uncomfortable at first. But, these feelings are usually short-term and monitored by healthcare professionals.
How soon can I start exercising after a heart attack or heart surgery?
Exercise timing varies by health and doctor’s advice. Patients start with gentle exercises in hospital and progress through rehab.
What is the importance of walking after open heart surgery?
Walking is key after surgery. It prevents complications, improves circulation, and aids healing.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC11194781/



































