
Coronary artery bypass grafting (CABG) is a surgery to improve blood flow to the heart. It can save lives but also comes with risks, like heart failure. We look into how common heart failure is after CABG and what factors increase the risk.
Studies on over 65,000 CABG patients found that those with ejection fractions under 35% before surgery had higher heart failure rates after CABG. Knowing these risks helps improve surgery results and care after the operation.
Key Takeaways
- Heart failure is a significant complication after CABG.
- Pre-operative ejection fraction is a key predictor of post-CABG heart failure.
- Patients with lower ejection fractions are at higher risk.
- Understanding risk factors can improve surgical outcomes.
- Post-operative care can be tailored based on pre-operative risk factors.
Understanding Heart Failure and Bypass Surgery
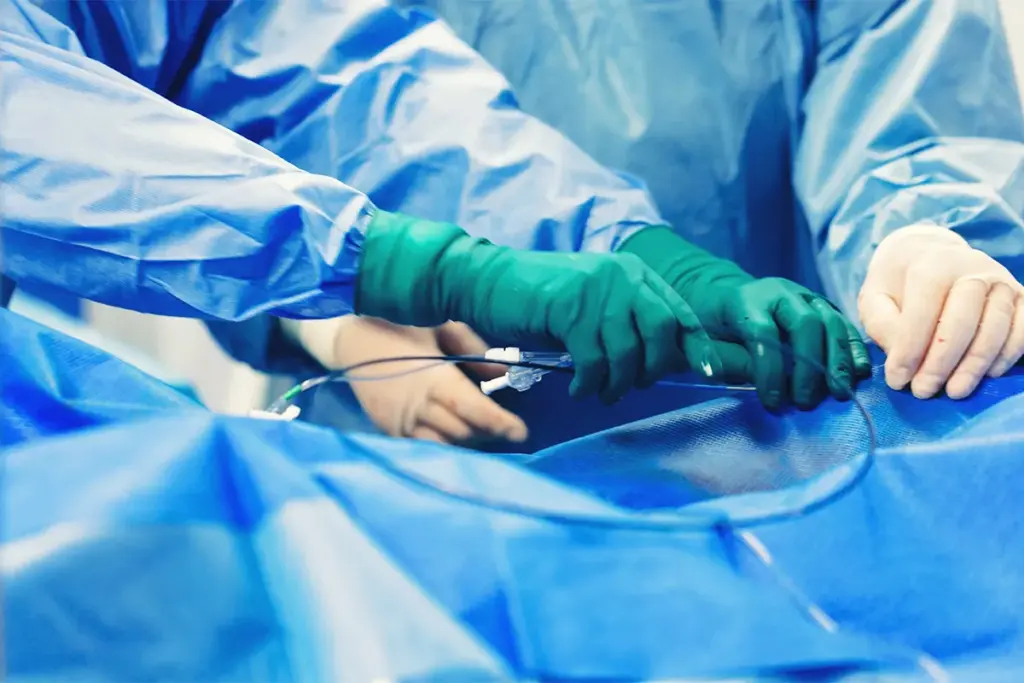
Heart failure and CABG have a complex relationship. Heart failure means the heart can’t pump enough blood. CABG is a surgery to improve blood flow by bypassing blocked arteries.
What is Heart Failure?
Heart failure happens when the heart can’t pump enough blood. This can be due to many reasons like coronary artery disease. Understanding heart failure is key to managing it and improving life quality.
Symptoms of heart failure include shortness of breath and fatigue. Early diagnosis and treatment are important to slow the disease’s progress.
The Purpose of Coronary Artery Bypass Grafting (CABG)
CABG aims to relieve symptoms of coronary artery disease. It does this by bypassing blocked arteries. This improves blood flow to the heart.
The main goal of CABG is to restore blood flow to the heart. This reduces symptoms like chest pain and improves heart function. It can also help prevent heart failure by making the heart pump better.
Relationship Between Cardiac Function and Bypass Procedures
The link between cardiac function and CABG is complex. CABG can improve blood flow to the heart muscle. But, the surgery can also affect heart function in different ways.
|
Aspect |
Pre-CABG |
Post-CABG |
|---|---|---|
|
Cardiac Function |
Compromised due to blocked arteries |
Potentially improved due to restored blood flow |
|
Symptoms |
Chest pain, shortness of breath |
Reduced symptoms, improved quality of life |
|
Risk of Heart Failure |
Higher due to compromised cardiac function |
Potentially lower due to improved cardiac function |
Understanding this relationship is vital for managing patient expectations and outcomes. By evaluating cardiac function before and after CABG, healthcare providers can tailor treatment plans. This helps minimize risks and maximize benefits.
Incidence Rates of Post-CABG Heart Failure
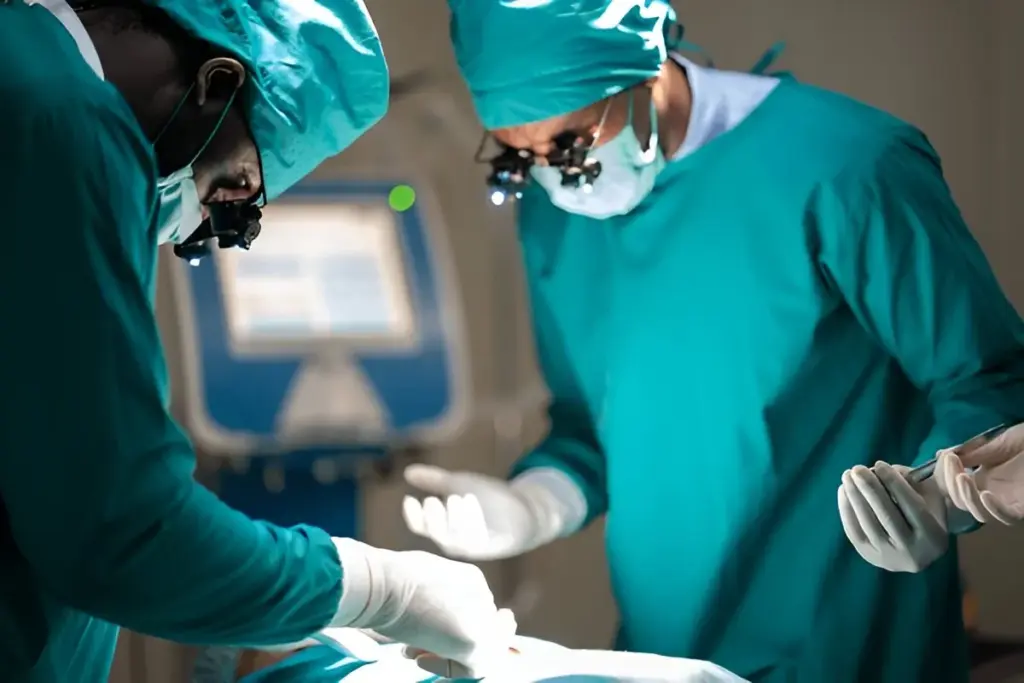
Post-CABG heart failure rates vary a lot. This is because of things like the patient’s heart health before surgery. Knowing these rates helps doctors set realistic goals for patient care.
Statistical Overview of Heart Failure After Bypass
Research shows that heart failure rates after CABG vary widely. A study in the Journal of the American College of Cardiology found rates up to 20% in the first year. This shows the importance of choosing the right patients and caring for them well after surgery.
“Heart failure after CABG is a complex issue,” say cardiothoracic surgery experts. It’s influenced by the patient’s heart health before surgery and other health problems.
Short-term vs. Long-term Incidence Rates
It’s important to know the difference between short-term and long-term heart failure rates after CABG. Short-term rates are about the surgery’s immediate effects. Long-term rates are about ongoing health issues and new heart problems.
A study in the Annals of Thoracic Surgery showed short-term rates are low. But long-term rates can be much higher, for patients with diabetes and high blood pressure.
Comparison to Other Cardiac Procedures
When comparing heart failure rates after CABG to other heart surgeries, like PCI, we must look at the patients and their health. CABG is for more severe heart disease, which raises the risk of heart failure.
A study in the Circulation Journal found CABG patients face a higher risk of heart failure. This is because their disease is more severe.
Understanding heart failure rates after CABG helps doctors improve patient care. It also helps them find ways to lower these risks.
Key Risk Factors for Developing Heart Failure After CABG
It’s important to know the risk factors for heart failure after coronary artery bypass grafting (CABG). Several factors can increase the chance of heart failure after surgery.
Pre-existing Cardiac Conditions
Pre-existing heart conditions are a big factor in heart failure risk after CABG. Patients with past heart attacks, left ventricular dysfunction, or heart failure are at higher risk. Assessing cardiac function before surgery is key to spotting these issues and managing them.
Age-Related Risk Factors
Being older is a big risk factor for heart failure after CABG. Older patients often have less physical strength and more health problems. Considering age-related factors is important when deciding if a patient should have CABG.
Comorbidities That Increase Risk
Some health conditions make heart failure more likely after CABG. These include high blood pressure, diabetes, and kidney disease. It’s vital to manage these conditions well before and after surgery. A thorough check-up before surgery helps identify and manage these issues.
By understanding and tackling these risk factors, doctors can lower the chance of heart failure after CABG. This helps improve patient results.
The Role of Ejection Fraction in Post-Bypass Heart Failure
Ejection fraction is key in checking heart failure risk after coronary artery bypass grafting (CABG). It shows how much blood the heart’s left ventricle pumps out with each beat. Knowing this helps predict heart failure chances in CABG patients.
Understanding Ejection Fraction Measurements
Ejection fraction (EF) is a percentage showing how much blood the left ventricle pumps out with each heartbeat. A normal EF is between 55% and 70%. Numbers below this might mean the heart isn’t working as well.
EF Measurement Techniques:
- Echocardiography
- Cardiac MRI
- Ventriculography
Critical Thresholds for Increased Risk
Patients with an EF below 35% before surgery face a higher risk of heart failure after CABG. This is a key number because it shows a big increase in heart failure risk after surgery.
“A reduced ejection fraction is a strong predictor of adverse outcomes after cardiac surgery.” –
Cardiologist
Monitoring Ejection Fraction Before and After Surgery
Keeping an eye on EF before and after CABG is key to managing heart failure risk. Checking EF before surgery helps spot high-risk patients. This allows for better care plans before and after surgery.
|
EF Range |
Risk Level |
Recommended Monitoring |
|---|---|---|
|
55%-70% |
Normal |
Standard post-operative care |
|
35%-54% |
Moderate Risk |
Close monitoring, possible medication adjustment |
|
Below 35% |
High Risk |
Intensive monitoring, possible additional interventions |
By watching ejection fraction, doctors can manage heart failure risk better after CABG. This helps improve patient results.
Mortality Rates and Survival Statistics
Looking at mortality rates and survival stats after CABG is key. It helps us see how well the surgery works and its risks. These numbers give us clues about the surgery’s success and dangers.
One-Year and Two-Year Mortality Rates
One-year and two-year death rates tell us a lot about survival after CABG. Research shows that those with higher rates in the first two years often face bigger challenges later on.
A study in a top medical journal found a 5% death rate at one year and 8% at two years after CABG. These numbers show why it’s vital to watch patients closely in the first couple of years after surgery.
Factors Influencing Survival Outcomes
Many things can affect how well someone does after CABG. These include heart problems before surgery, age, and other health issues. People with heart failure or other heart problems are more likely to face risks after CABG.
Older patients and those with conditions like diabetes or kidney problems also face higher risks. Knowing these risks helps doctors plan better care for patients after surgery.
Long-term Survival Trends (10-Year Data)
Looking at survival over 10 years gives us a full picture of CABG’s success. Studies show that while there’s a risk of death early on, many patients see big benefits later.
A 10-year study on CABG patients found a big drop in heart-related deaths. This shows CABG can really help extend life for people with heart disease.
By studying these numbers, doctors can make better choices for patient care. This info is key to improving outcomes and quality of life for CABG patients.
Recognizing Symptoms of Heart Failure After Bypass Surgery
It’s important to know the signs of heart failure after bypass surgery. This helps get medical help quickly. We’ll talk about the main symptoms to look out for. This way, patients can get help when they need it.
Early Warning Signs
The first signs of heart failure after CABG are often small but very important. Look out for:
- Shortness of breath, which gets worse when lying down or moving
- Fatigue and weakness, making simple tasks hard
- Swelling in the legs, ankles, and feet from fluid buildup
- Rapid or irregular heartbeat
- Coughing up pink, frothy mucus
These signs mean the heart might not be working right after surgery. It’s key to watch these signs closely and tell your doctor about any changes.
Progressive Symptoms Development
As heart failure gets worse, symptoms can get more severe and new ones can appear. These include:
- Increased shortness of breath, even when resting
- Significant weight gain from fluid retention
- Difficulty concentrating or feeling less alert
- Chest pain or discomfort that gets worse with activity
Spotting these symptoms early helps in making treatment plans better for managing heart failure.
When to Seek Medical Attention
If you notice any of these, get medical help right away:
- Severe shortness of breath that makes daily tasks hard
- Chest pain or pressure that doesn’t get better with rest
- Severe swelling or pain in the legs
- Confusion or feeling disoriented
Getting help quickly can greatly improve outcomes for heart failure after CABG. We stress the need to be alert to these symptoms and talk openly with your healthcare team.
Diagnostic Approaches for Post-CABG Heart Failure
Diagnosing heart failure after a coronary artery bypass grafting (CABG) is key. It needs a mix of clinical checks and advanced tools. This is vital for quick treatment and care.
Clinical Evaluation Methods
At the heart of diagnosing heart failure post-CABG is clinical evaluation. We look at patients’ medical history for signs like dyspnea, fatigue, and edema. A detailed physical check is done to spot signs like jugular venous distension and peripheral edema.
“Early spotting of heart failure symptoms is key for good management,” say recent guidelines. We also check how well patients can function using the New York Heart Association (NYHA) scale.
Imaging Techniques
Imaging is vital in diagnosing heart failure after CABG. Echocardiography helps check the left ventricle’s function and valve health. It’s important for knowing the ejection fraction, a heart failure indicator.
Cardiac MRI and CT angiography are used too. They help see the heart’s structure and function. They also check if grafts and native arteries are open.
Laboratory Tests and Biomarkers
Laboratory tests are key for diagnosing and managing heart failure post-CABG. B-type natriuretic peptide (BNP) and N-terminal pro-b-type natriuretic peptide (NT-proBNP) are important biomarkers. High levels mean heart failure is severe.
We also do complete blood count, electrolyte levels, and renal function tests. These help find other issues and check the patient’s health.
A leading cardiology journal says, “Using clinical checks, imaging, and lab tests makes diagnosing heart failure post-CABG more accurate.” This detailed method helps doctors create a care plan that fits the patient’s needs.
Heart Failure Surgery: Interventions Beyond CABG
There are many surgical options for heart failure beyond CABG. These include mechanical circulatory support and heart transplantation. These treatments are for those with severe heart failure who don’t get better with usual treatments.
Mechanical Circulatory Support Options
Mechanical circulatory support (MCS) devices help the heart pump in advanced heart failure. They can save lives. They are used as a bridge to heart transplant or for those not eligible for transplant.
Common MCS devices include:
- Left ventricular assist devices (LVADs)
- Right ventricular assist devices (RVADs)
- Biventricular assist devices (BiVADs)
- Total artificial hearts (TAHs)
The right MCS device depends on the patient’s heart condition and other health issues.
Valve Repair or Replacement Procedures
Valve disease is common in heart failure patients. Surgery to fix or replace valves can help. It improves heart function, reduces symptoms, and boosts quality of life.
Important factors for valve surgery include:
- The severity of valve disease
- Symptoms like shortness of breath or chest pain
- The patient’s overall heart health and other health issues
New surgical techniques and valves have made valve surgery safer and more effective.
Heart Transplantation Considerations
Heart transplant is the best option for some with advanced heart failure. Choosing to transplant involves looking at the patient’s health, heart failure severity, and other health issues.
“Heart transplantation is a life-changing procedure that offers a second chance to patients with end-stage heart failure.”
After transplant, patients need lifelong medication and regular check-ups to watch for rejection or other problems.
Preventive Strategies to Reduce Post-CABG Heart Failure
To lower the risk of heart failure after CABG, we need to take steps before and during surgery. Focusing on the right medications before surgery and improving surgical methods can help. This way, we can make post-CABG heart failureless likely.
Pre-operative Medication Management
Managing medications before surgery is key to avoiding heart failure after CABG. Studies show that beta-blockers can cut down on heart failure admissions after CABG. Beta-blockers help control heart rate and lessen the heart’s workload, which lowers heart failure risk.
Other drugs to consider include:
- ACE inhibitors or ARBs to control blood pressure and ease heart strain.
- Statins to keep plaques stable and reduce inflammation.
- Aspirin for its antiplatelet effects.
Surgical Technique Considerations
Surgical methods are also vital in preventing heart failure after CABG. Careful handling of the heart and coronary vessels during surgery can reduce damage and aid in healing.
|
Surgical Technique |
Benefits |
|---|---|
|
Off-pump CABG |
Reduces the risk of cardiopulmonary bypass-related complications. |
|
Minimally invasive CABG |
Less tissue trauma and potentially quicker recovery. |
|
Complete revascularization |
Ensures that all areas of the heart receive adequate blood flow. |
By using these preventive strategies, we can greatly lower heart failure rates after CABG. It’s important to customize these approaches based on each patient’s unique risk factors and medical history.
Recovery Process and Heart Failure Management
Recovering from CABG needs a full plan. This includes care right after surgery, rehab, and long-term plans to avoid heart failure. We know recovery is complex, with many steps to manage risks.
Immediate Post-Surgical Care
The first days after CABG are very important. Patients stay in an ICU or step-down unit. Right after surgery, care focuses on keeping the patient stable, managing pain, and watching for complications like bleeding or heart failure.
Immediate care includes:
- Watching vital signs and heart function closely
- Using medicine and other ways to control pain
- Moving patients early to prevent blood clots
- Helping with breathing to get off the ventilator
Cardiac Rehabilitation Programs
Cardiac rehab is key to getting better. It helps patients get stronger, improve heart health, and lower heart risks. These programs mix exercise, heart-healthy education, and stress counseling.
|
Component |
Description |
Benefits |
|---|---|---|
|
Exercise Training |
Supervised exercise sessions tailored to the patient’s condition |
Improves cardiovascular health, increases strength |
|
Education |
Information on diet, exercise, and lifestyle changes |
Empowers patients to manage their condition |
|
Counseling |
Support to manage stress and emotional challenges |
Enhances mental well-being, reduces anxiety and depression |
Long-term Management Strategies
Managing heart failure long-term after CABG is complex. It includes taking medicine, making lifestyle changes, and seeing doctors often. Good long-term care can greatly improve life and survival.
Key strategies are:
- Following the doctor’s advice on medicine
- Making healthy lifestyle choices like eating right and exercising
- Going to regular check-ups with doctors
Comparing CABG to Other Interventions for Heart Disease
Choosing between CABG and percutaneous coronary intervention for heart disease depends on many things. These include the patient’s health and their specific heart conditions. Both methods help ease symptoms and improve life for those with coronary artery disease.
CABG vs. Percutaneous Coronary Intervention
CABG is a surgery that bypasses blocked arteries with grafts from the patient’s own body. On the other hand, percutaneous coronary intervention uses a catheter to place a stent in the artery. The choice between these options depends on the disease’s complexity, the patient’s health, and their personal preferences.
Impact on Heart Failure Development
The risk of heart failure after CABG or percutaneous coronary intervention changes based on several factors. These include the patient’s heart function, other health conditions, and age. Both methods can lower heart failure risk by improving blood flow to the heart. Yet, long-term results can vary based on the patient’s specific situation.
Selecting the Right Procedure Based on Risk Factors
Doctors look at many risk factors when deciding between CABG and percutaneous coronary intervention. These include the disease’s severity, diabetes, and kidney function. For complex multi-vessel disease, CABG might be better because it can fully revascularize the heart. But, percutaneous coronary intervention might be better for simpler cases or those at higher surgical risk.
The choice between CABG and percutaneous coronary intervention should be made carefully for each patient. By considering each patient’s unique needs and risks, doctors can improve outcomes and lower heart failure risk.
Living With Heart Failure After Bypass Surgery
Living with heart failure after CABG means big changes in your lifestyle and medical care. It’s key to understand the many steps needed to manage heart failure well.
Lifestyle Modifications
Healthy habits are essential for heart failure management. This includes:
- Dietary Changes: Eating less sodium and more fruits, veggies, and whole grains.
- Physical Activity: Doing regular, moderate exercise as your doctor suggests.
- Smoking Cessation: Stopping smoking to lower heart risk.
- Weight Management: Keeping a healthy weight through diet and exercise.
Medication Adherence
Following your medication plan is critical for heart failure control. Your medications might include:
- ACE inhibitors or ARBs to lower blood pressure and ease heart work.
- Beta-blockers to slow the heart rate and reduce its work.
- Diuretics to remove extra fluid from your body.
|
Medication Type |
Purpose |
Common Side Effects |
|---|---|---|
|
ACE Inhibitors |
Reduce blood pressure, decrease heart workload |
Cough, dizziness |
|
Beta-blockers |
Slow heart rate, reduce heart workload |
Fatigue, dizziness |
|
Diuretics |
Remove excess fluid |
Increased urination, dehydration |
Quality of Life Considerations
Keeping a good quality of life is important with heart failure. This means:
- Monitoring Symptoms: Watching for symptom changes and telling your doctor.
- Emotional Support: Getting help from loved ones or support groups for emotional health.
- Staying Informed: Learning about heart failure care and new treatments.
By focusing on these areas, people with heart failure after CABG can live better and enjoy life more.
Multidisciplinary Approach to Post-CABG Heart Failure Care
For patients with heart failure after CABG surgery, a team effort is key. This team approach looks at all parts of a patient’s health. It leads to better care for their condition.
The Cardiac Care Team
The cardiac care team is essential for managing heart failure after CABG. This team includes cardiologists, surgeons, primary care doctors, nurses, and more. Working together, they provide complete care.
A study on the National Center for Biotechnology Information (NCBI) website shows the value of a team. for heart failure management it says. This underlines the need for teamwork in patient care.
Coordinating Specialists and Primary Care
It’s important for specialists and primary care doctors to work together. They need to communicate well, share patient records, and have a clear plan. This ensures patients get consistent care.
- Regular check-ups with cardiologists and primary care doctors.
- A dedicated team for patient questions and concerns.
- Specialists for managing other health issues.
Good teamwork helps catch problems early and act fast. This improves patient results.
Patient Education and Self-Management
Teaching patients about their heart failure is key. Knowing about their condition, treatment, and lifestyle changes helps them manage their health. This includes sticking to medication, eating right, and exercising.
|
Aspect of Care |
Educational Focus |
|---|---|
|
Medication Management |
Understanding medication purpose and side effects. |
|
Lifestyle Modifications |
Changes in diet, exercise, and stress management. |
|
Symptom Monitoring |
Spotting early signs of worsening heart failure and when to seek help. |
A leading cardiologist says,
“Patient education is not just about giving info; it’s about empowering them to manage their health.”
This shows how important patient education is in treating heart failure after CABG.
Conclusion
Heart failure after coronary artery bypass grafting (CABG) is a big problem. It affects how well patients do and their quality of life. We’ve looked into how common it is, what causes it, and how to manage it.
Our study shows we need more research to find better ways to prevent heart failure after CABG. Knowing the risks, like old age and heart problems, helps us focus on high-risk patients. This way, we can give them the best care.
Managing heart failure after CABG needs a team effort. We must use new surgery methods, medicines, and cardiac rehab. By getting better at treating patients, we can make their lives better. This will help lessen the impact of heart failure after CABG.
FAQ
What is the risk of heart failure after coronary artery bypass grafting (CABG)?
The risk of heart failure after CABG depends on several factors. These include the patient’s health before surgery and their heart’s condition. Studies show that those with lower heart function before surgery are at higher risk.
What is heart failure, and how is it related to CABG?
Heart failure means the heart can’t pump enough blood for the body’s needs. CABG helps by bypassing blocked arteries. This improves the heart’s function.
What are the primary risk factors for developing heart failure after CABG?
Several factors increase the risk of heart failure after CABG. These include heart conditions, age, and other health issues.
How is ejection fraction used to assess cardiac function and predict the risk of heart failure after CABG?
Ejection fraction measures heart function. A lower fraction means a higher risk of heart failure after CABG.
What are the early warning signs and progressive symptoms of heart failure after CABG?
Early signs include shortness of breath, fatigue, and leg swelling. If these worsen, it’s important to seek medical help quickly.
What diagnostic approaches are used to identify heart failure after CABG?
Doctors use several methods to diagnose heart failure after CABG. These include clinical checks, imaging, and lab tests.
What surgical interventions are available beyond CABG for managing heart failure?
Beyond CABG, options include mechanical support, valve repair, and heart transplant.
How can the incidence of heart failure after CABG be reduced?
To lower heart failure risk after CABG, preventive steps are key. These include managing medications before surgery and choosing the right surgical techniques.
What is the recovery process like after CABG, and how is heart failure managed?
Recovery involves immediate care, cardiac rehab, and long-term management. These steps help manage heart failure after CABG.
How does CABG compare to other interventions like percutaneous coronary intervention (PCI) in terms of heart failure development?
CABG and PCI affect heart failure differently. The best choice depends on the patient’s health and risk factors.
What lifestyle modifications are necessary for living with heart failure after CABG?
Living with heart failure after CABG requires a healthy diet, regular exercise, and stress management.
Why is a multidisciplinary approach important for caring for patients with heart failure after CABG?
A team approach is vital for managing heart failure after CABG. It involves a cardiac team, specialists, and educating patients for better outcomes.
What are the chances of having a heart attack after CABG?
Heart attack risk after CABG varies. It depends on the patient’s heart condition and overall health.
What are the long-term side effects of open heart surgery?
Long-term effects can include heart failure, arrhythmias, and other heart issues. Continuous monitoring and management are necessary.
How does congestive heart failure surgery impact overall cardiac health?
Surgery for congestive heart failure, like CABG, aims to improve heart function and overall health.
References:
New England Journal of Medicine. Evidence-Based Medical Insight. Retrieved from https://www.nejm.org/doi/full/10.1056/NEJMoa1100358




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News






























