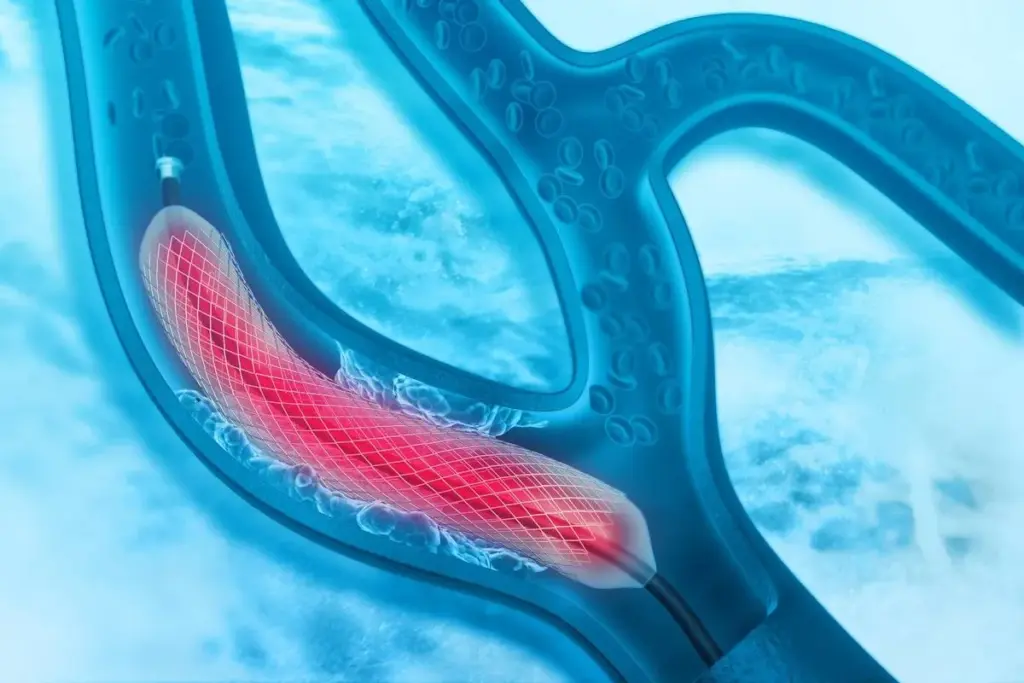
Nearly 1 million coronary stenting procedures happen every year in the United States. These procedures greatly improve the lives of those with coronary artery disease. But, a big question is: how long do these life-saving devices last? Learn how long heart stents last and factors affecting their durability. heart stent durability
We will look at the different types of coronary stents and how long they usually last. We will also talk about what affects their durability. Knowing about stent longevity is key for those who have had stents placed. It affects their long-term health and happiness.
Thanks to medical tech advancements, many stents have been developed. Each is made for a specific need and to improve patient results. By looking at the latest in heart stent technology, we can understand what patients can expect in terms of stent longevity.
Key Takeaways
- Coronary stents greatly improve the lives of patients with coronary artery disease.
- The durability of stents varies based on several factors, including type and patient health.
- Understanding stent longevity is key for patient care and long-term health.
- Advancements in stent technology continue to improve patient outcomes.
- Different types of stents are designed to meet specific patient needs.
What Are Heart Stents and Why Are They Used?

Heart stents are small, mesh-like tubes that help keep arteries open. This ensures blood flows properly. They are usually made of metal or a metal alloy and are put in place with a balloon angioplasty procedure.
These devices are used to support artery walls. They improve blood flow to the heart and lower the risk of heart attacks. The main job of a stent is to keep the artery open, ensuring normal blood flow.
Definition and Basic Function of Cardiac Stents
A cardiac stent is a permanent implant, though some newer ones dissolve over time. Its main role is to:
- Keep the artery open after angioplasty
- Improve blood flow to the heart muscle
- Reduce the risk of the artery narrowing again (restenosis)
To place a stent, a catheter is used to deliver it to the affected area. A balloon then inflates to expand the stent. It stays in the artery to keep it open.
The Historical Development of Stent Technology
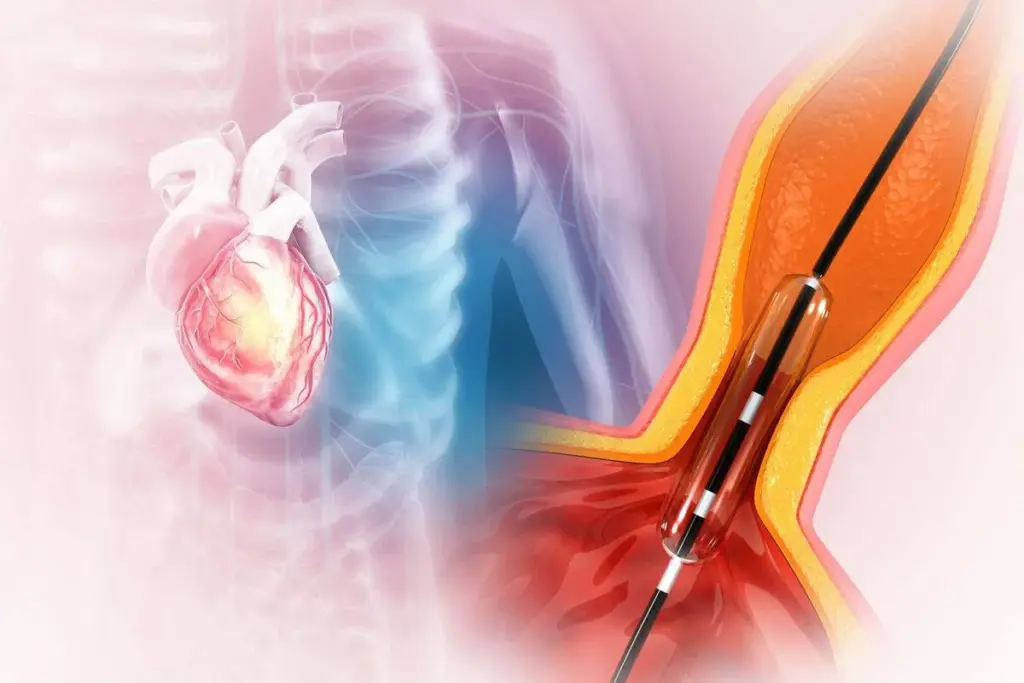
The first coronary stent was introduced in the late 1980s. This marked a new era in heart treatments. Over time, stent technology has greatly improved, thanks to advances in materials and design.
Early stents had high rates of restenosis and thrombosis. But newer stents have seen big improvements. These include:
|
Generation |
Characteristics |
Advantages |
|---|---|---|
|
Bare-Metal Stents (BMS) |
Simple metal mesh |
Easy to deploy |
|
Drug-Eluting Stents (DES) |
Coated with medication |
Reduced restenosis rates |
|
Bioresorbable Vascular Scaffolds (BVS) |
Made of absorbable material |
Temporary support, reduced long-term complications |
Types of Heart Stents Available in Modern Cardiology
Modern cardiology has seen a big change with the development of heart stents. Now, we have many types of stents to fit each patient’s needs. This has improved treatment outcomes and quality of life.
Heart stents are mainly divided into three types: Bare-Metal Stents (BMS), Drug-Eluting Stents (DES), and Bioresorbable Vascular Scaffolds (BVS). Each has its own benefits and possible drawbacks.
Bare-Metal Stents: Structure and Function
Bare-Metal Stents (BMS) are the first type of coronary stent. They are made from stainless steel and keep the artery open. BMS have been used for years but have a higher chance of restenosis than others.
BMS are simple and have fewer long-term risks. They need dual antiplatelet therapy for a shorter time than DES. But, they might need more careful patient selection and follow-up because of restenosis risk.
Drug-Eluting Stents: Medication Benefits
Drug-Eluting Stents (DES) release medicine that stops new tissue growth, lowering restenosis risk. This technology has greatly improved PCI outcomes for patients.
DES keep the artery open by preventing new tissue growth. They are a favorite for many patients. But, they need longer dual antiplatelet therapy to avoid stent thrombosis.
Bioresorbable Vascular Scaffolds: Temporary Support
Bioresorbable Vascular Scaffolds (BVS) are a newer stent type. They offer temporary support and then dissolve, aiming to reduce long-term issues.
BVS are made from materials that the body can break down over time. This might lower long-term stent-related problems. But, BVS are under study, and their long-term effects are being looked into in clinical trials.
In conclusion, choosing a heart stent depends on many factors like patient health and artery condition. Knowing about the different stents helps make better choices for heart care.
The Expected Lifespan of Different Heart Stent Types
Heart stents come in different types, each with its own lifespan. This affects how doctors treat heart disease. Knowing about these lifespans is key for both doctors and patients.
Average Durability Timeframes by Stent Category
Research shows that stent lifespans vary by type. Bare-metal stents (BMS) don’t last as long as drug-eluting stents (DES). BMS can last 5 to 10 years but are more likely to cause restenosis.
On the other hand, DES can last 10 years or more. This is because they release medicine that stops cells from growing too much.
Bioresorbable vascular scaffolds (BVS) are made to dissolve in 2 to 3 years. They support the artery wall temporarily but don’t last long-term.
Comparative Longevity Between Stent Varieties
Drug-eluting stents last longer than bare-metal stents. Studies show DES have fewer problems like restenosis and stent thrombosis. This makes them more durable.
Newer DES have even better results, with fewer heart problems. BVS dissolve in the body but can cause stent thrombosis in some cases. This shows the importance of choosing the right stent for each patient.
Choosing a stent depends on many factors. These include the patient’s health, the type of blockage, and the doctor’s opinion. Knowing how long each stent lasts helps doctors make better choices for their patients.
Heart Stent Durability: Key Factors Influencing Longevity
Many factors affect how long a heart stent lasts. These include the stent’s material and the patient’s health. Knowing these helps make stents last longer and improve patient care.
Material Composition and Engineering Design
The stent’s material and design are key to its durability. Today’s stents are made from strong, flexible materials like stainless steel and cobalt-chromium. These materials are also safe for the body.
Drug-eluting stents, for example, have a special coating. This coating helps prevent the stent from getting clogged again. The design of stents has also improved. Changes in thickness and texture help the stent fit better and reduce clotting risks.
Patient-Specific Factors Affecting Stent Performance
Each patient’s health can affect how well a stent works. Conditions like diabetes and kidney disease can slow healing and increase risks.
- Diabetes: People with diabetes face higher risks of stent problems due to insulin issues and inflammation.
- Kidney Disease: Kidney problems can make it hard for the body to remove drugs and toxins, affecting the stent.
- Hypertension: High blood pressure can stress the stent, leading to problems or complications.
Bare-Metal Stents: Durability Profile and Considerations
Bare-metal stents don’t have a drug coating like other stents. They work by keeping the artery open mechanically. We’ll look at how well they last and the challenges they face.
Typical Duration of Effectiveness
Bare-metal stents usually last several years after they’re put in. Research shows they work well at first but might not last as long as drug-eluting stents. This is because they have a higher chance of restenosis.
Common Issues Affecting Longevity
One big worry with bare-metal stents is restenosis. This is when the artery gets narrow again. It might mean more treatments, like more stenting or angioplasty.
Other things can affect how long a bare-metal stent lasts. These include the patient’s health, like diabetes, and the type of blockage. Also, how well the stent is placed matters a lot.
Bare-metal stents might have a higher risk of restenosis. But, they have some benefits. For example, they need less dual antiplatelet therapy after being put in. This is good for patients who are at risk of bleeding or need surgery.
Knowing about the durability and issues of bare-metal stents helps doctors make better choices. This is for treating coronary artery disease.
Drug-Eluting Stents: Long-Term Effectiveness Analysis
Drug-eluting stents have changed how we treat heart disease. They help keep arteries open by stopping cell growth. This reduces the chance of arteries narrowing again.
We’ll look at how these stents have evolved. We’ll compare old and new stents. We’ll also see how the timing of the medication release affects their lasting power.
First-Generation vs. Newer Generation DES Longevity
Older drug-eluting stents were a big step up from bare-metal stents. But, they had a higher risk of clotting later on. Newer stents have better designs and drugs to fix these problems.
Key advancements in newer generation DES include:
- Thinner struts for easier delivery and less clotting
- More effective and safer drugs to stop cell growth
- Biodegradable or no polymer designs
These changes have made newer stents safer and more effective than the old ones.
Medication Release Timeline and Its Impact on Durability
The timing of when the medication is released is key for drug-eluting stents. It affects how well the stent works and how safe it is.
Drug-eluting stents release medication slowly over months. They start with a strong dose and then release less. This keeps the artery open and lowers the risk of problems.
The benefits of the medication release timeline include:
- Less chance of arteries narrowing again
- Lower risk of clotting and safer use
- Stents last longer
Knowing how the medication release timeline affects durability helps doctors plan better. It helps them meet patient needs and choose the best treatment.
Bioresorbable Stents: Understanding Their Temporary Nature
Bioresorbable stents offer a new way to treat heart problems. They provide temporary support without the need for a metal stent. These stents dissolve over time, which could reduce long-term issues seen with metal stents.
This technology is exciting in cardiology. It could lead to better health outcomes for patients.
Absorption Timeline and Biological Process
The time it takes for bioresorbable stents to dissolve varies. It usually happens in 2 to 3 years. The stent breaks down into harmless parts that the body can easily process.
Key aspects of the absorption process include:
- Gradual degradation of the stent material
- Breakdown into harmless byproducts
- Metabolism by the body
Benefits and Limitations of Biodegradable Stent Technology
Bioresorbable stents have many advantages. They might lower the risk of serious problems like stent thrombosis. They also help the blood vessel work like normal again.
But, there are downsides. They might cause more problems early on. Also, doctors need to keep a close eye on patients after they get these stents.
The benefits of bioresorbable stents are:
- Reduced risk of long-term complications
- Restoration of normal vascular function
As we learn more about bioresorbable stents, we’ll better understand their role. This knowledge is key to giving patients the best care possible.
Warning Signs That a Heart Stent May Be Failing
Knowing the signs of heart stent failure is key for those with coronary stents. Heart stents help blood flow to the heart. But sometimes, they don’t work right. Spotting these signs early can help get quick medical help.
Recurring Cardiac Symptoms to Monitor
People with heart stents need to watch for signs of stent failure. Look out for:
- Chest Pain or Discomfort: This could mean the stent isn’t working or there’s a blockage.
- Shortness of Breath: Feeling out of breath even when resting might be a sign of stent trouble.
- Fatigue: Feeling very tired or weak, and it lasts, is something to tell your doctor.
- Palpitations or Irregular Heartbeat: Changes in heart rhythm could mean stent problems.
These symptoms can be different in everyone. But any new or getting worse symptoms need to be talked about with a doctor.
When to Seek Immediate Medical Attention
If you have any of these, get medical help right away:
- Severe Chest Pain: Intense chest pain that doesn’t stop with rest or medicine.
- Severe Shortness of Breath: Sudden and severe trouble breathing.
- Dizziness or Fainting: Feeling dizzy or fainting, with other symptoms.
Quick medical check-ups are vital for these signs. They could mean serious issues like heart attacks or stent problems. It’s important to take care of your health and get help when you need it.
Common Complications Affecting Stent Longevity
Heart stents are usually safe, but some complications can shorten their life. It’s important for patients and doctors to know about these issues to get the best results.
Restenosis: Mechanisms, Causes, and Prevention Strategies
Restenosis is when arteries narrow again after a stent is placed. It happens because the body grows new tissue in response to the stent. This can block the artery again.
Several things can increase the risk of restenosis. These include:
- Patient-specific factors such as diabetes and hypertension
- Stent-related factors like the type of stent used (bare-metal vs. drug-eluting)
- Procedural factors, including stent sizing and deployment techniques
To prevent restenosis, doctors use drug-eluting stents. These stents release medicine to stop cell growth. They also choose patients carefully and use specific techniques during procedures.
Stent Thrombosis: Risk Factors and Management Approaches
Stent thrombosis is when a blood clot forms in the stent. It’s rare but very dangerous. Factors that increase the risk include stopping antiplatelet therapy too soon, stent not being fully deployed, and patient factors like not responding to antiplatelet drugs.
When stent thrombosis happens, doctors need to act fast. They might do emergency procedures like removing the clot or placing more stents. Long-term, patients need to keep taking their antiplatelet drugs and get regular check-ups.
|
Risk Factor |
Description |
Management Strategy |
|---|---|---|
|
Premature discontinuation of antiplatelet therapy |
Stopping medication too early increases clot risk |
Adherence to prescribed therapy duration |
|
Stent underdeployment |
Incomplete stent expansion against artery wall |
Optimal stent deployment techniques |
|
Resistance to antiplatelet medications |
Some patients may not respond well to standard therapy |
Alternative antiplatelet therapies or testing for resistance |
Stent Fracture and Structural Deformation Issues
Stent fracture or structural deformation is another problem. It can happen because of stress on the stent, like in areas that move a lot. This is common near the start of a coronary artery.
Symptoms of stent fracture might include chest pain or even a heart attack. Doctors use imaging like angiography or ultrasound to find out.
To fix stent fracture, doctors might need to put in more stents or even surgery. To prevent it, they choose stents that are flexible and strong for each patient’s body.
Post-Stent Care Protocols to Maximize Durability
Keeping heart stents working well needs a full plan for aftercare. Taking good care of your stent after it’s placed is key. It helps your stent last longer and keeps your heart healthy.
Medication Adherence: Critical Importance for Stent Maintenance
Following your medication is very important for your stent’s health. You need to take the medicines your doctor gave you. These medicines help stop blood clots from forming.
- Take medications as directed by your healthcare provider
- Understand the purpose and possible side effects of each medicine
- Tell your doctor if you have any problems with your medicine
Dual antiplatelet therapy (DAPT) is often used after a stent is placed. This means taking two medicines to stop blood clots. How long you take DAPT depends on your stent type and health.
Lifestyle Modifications for Optimal Stent Performance
Changing your lifestyle is key for your stent to work its best. These changes include:
- Eating a diet full of fruits, veggies, and whole grains
- Doing regular exercise, as your doctor suggests
- Stopping smoking and staying away from smoke
- Using stress-reducing activities like meditation or yoga
Keeping a healthy weight and managing health issues like diabetes and high blood pressure are also important. They help your stent last longer.
Follow-up Schedule and Long-term Monitoring
Seeing your doctor regularly is vital for checking on your stent and heart health. These visits include:
- Regular check-ups to see how your stent and heart are doing
- Tests like stress tests or angiograms to check stent health
- Changing your medicine or lifestyle advice if needed
By following these care steps, you can make your stent last longer and lower your risk of problems. It’s important to work with your healthcare team to create a care plan that’s right for you.
The Role of Dual Antiplatelet Therapy in Extending Stent Lifespan
Dual antiplatelet therapy (DAPT) is key in keeping heart stents working longer, mainly for those with drug-eluting stents. It uses two medicines to stop platelets from clumping and lowers the chance of stent blockage.
We suggest that patients with drug-eluting stents follow a DAPT plan for a certain time to extend their stent’s life. The exact time depends on the stent type and the patient’s health.
Recommended Duration Based on Specific Stent Type
The time needed for DAPT changes based on the stent type.
- Patients with bare-metal stents (BMS) should take DAPT for at least a month.
- Those with first-generation drug-eluting stents (DES) need DAPT for 12 months.
- Newer DES might need DAPT for 6 to 12 months, depending on the patient’s risk.
Risks and Consequences of Premature Therapy Discontinuation
Stopping DAPT too soon can greatly raise the risk of stent blockage, a serious issue. We stress the importance of sticking to the DAPT plan to our patients.
Stent blockage can lead to heart attacks and even death. It’s vital for patients to know the dangers of stopping DAPT early and the benefits of following the recommended time.
By teaming up with their doctors, patients can lower risks and extend their stent’s life with the right use of DAPT.
Latest Technological Advancements Improving Heart Stent Longevity
The field of heart stent technology is rapidly evolving. New innovations are coming to make stents last longer. We’re seeing big improvements in design, materials, and function of heart stents.
New materials and protective coatings are key advancements. Researchers are finding materials that are more friendly to the body and last longer. For example, some stents now have nanocoatings that release medicine slowly, making them more effective.
Next-Generation Design Features Enhancing Durability
New design features are also making heart stents better. These include:
|
Design Feature |
Benefit |
|---|---|
|
Improved strut design |
Enhanced flexibility and reduced risk of fracture |
|
Enhanced drug delivery systems |
More effective prevention of restenosis |
|
Adaptive stent architecture |
Better conformability to the vessel wall, reducing complications |
As we keep improving heart stent technology, we’re seeing better results for patients. The future looks bright, with ongoing research aiming to make stents even more effective and durable.
Research Studies and Clinical Evidence on Long-Term Stent Outcomes
Many research studies have shown how heart stents perform over time. We’ve learned a lot about their durability and effectiveness. This knowledge comes from detailed clinical trials and studies.
Key Clinical Trials and Their Findings on Stent Durability
Important clinical trials have looked into stent performance over the years. For example, the SIRIUS trial found drug-eluting stents safe and effective for five years. The ABSORB trial explored bioresorbable vascular scaffolds, showing how they break down.
These studies found drug-eluting stents much better than bare-metal stents at preventing restenosis. This information helps doctors choose the best stent for each patient.
Statistical Data on Long-Term Stent Performance
Statistical analysis from trials and registries has given us a clear picture of stent performance. The table below shows key findings on stent durability.
|
Stent Type |
Average Durability |
Restenosis Rate |
|---|---|---|
|
Bare-Metal Stents |
5-7 years |
20-30% |
|
Drug-Eluting Stents |
10+ years |
5-15% |
|
Bioresorbable Stents |
2-5 years (until absorption) |
10-20% |
The table shows the different lifespans of stent types. Drug-eluting stents last longer and have fewer restenosis cases than bare-metal stents. Bioresorbable stents, though temporary, might reduce long-term issues by fully dissolving.
When Stent Replacement or Additional Interventions Become Necessary
Stent replacement or more treatments are needed when a stent fails or gets worse. We’ll look at why this happens and what treatment choices are available.
Clinical Indicators for Secondary Intervention
Several signs may mean a stent needs to be replaced or more treatments. These include:
- Recurrence of symptoms such as chest pain or shortness of breath
- Evidence of in-stent restenosis or stent thrombosis
- Stent fracture or structural deformation
- Failure to respond to medication or other treatments
In-stent restenosis is a common reason for needing more treatment. It happens when tissue grows inside the stent, causing another blockage. Quickly finding and treating these problems is key to keeping patients healthy.
Treatment Options for Failed or Aging Stents
When a stent fails or gets old, there are several ways to treat it. These include:
|
Treatment Option |
Description |
Benefits |
|---|---|---|
|
Balloon Angioplasty |
A procedure using a balloon to widen the stent |
Minimally invasive, quick recovery |
|
Stent-in-Stent Placement |
Placing a new stent within the existing one |
Effective for treating in-stent restenosis |
|
Medication Adjustment |
Changing or adjusting medications to manage symptoms |
Non-invasive, can be effective for symptom management |
Choosing the right treatment depends on many things. These include the patient’s health, the stent type, and the problem’s nature. We help patients choose the best treatment for them.
Knowing when to replace a stent or do more treatments is key for good patient care. By spotting the signs and looking at treatment options, we support patients with heart stents well.
Frequently Asked Patient Questions About Heart Stent Durability
Many patients worry about how long their heart stents will last. We help them understand their treatment options and answer their questions about stent longevity.
Addressing Common Concerns About Stent Longevity
Patients often wonder about the average lifespan of heart stents. They also ask what affects their durability. The lifespan of a stent depends on several things.
- Type of Stent: Different stents last longer or shorter. Drug-eluting stents, for example, can last longer than bare-metal stents because they prevent restenosis.
- Patient Health: Conditions like diabetes or kidney disease can affect how long a stent lasts. Keeping healthy through lifestyle changes is important.
- Post-Stent Care: Following medication and attending follow-up appointments is key to a stent’s long-term success.
Managing Expectations for Different Patient Populations
It’s important to manage what patients expect, as their situation can affect stent durability. We tailor our advice to each patient’s needs.
Some important things to consider include:
- Lifestyle Factors: Quitting smoking, eating right, and exercising can help a stent last longer.
- Medication Adherence: Taking all prescribed medicines is essential for a stent’s function.
- Regular Monitoring: Regular check-ups help us keep an eye on the stent and catch any problems early.
By understanding these factors and working with healthcare providers, patients can manage their expectations better. This can help improve their stent’s longevity.
Conclusion: The Future of Heart Stent Technology and Durability
Heart stent durability is shaped by many things. These include the stent type, patient health, and how the procedure is done. New heart stent technology has made treating coronary artery disease better and safer for patients.
New research and development will keep improving stent technology. We’ll see better materials, designs, and drug-eluting stents. These changes will help more patients worldwide.
As stent technology grows, treatments will get more personal. This means treatments will fit each patient’s needs better. With better stent designs and materials, patients with coronary artery disease will see better results.
FAQ
What is the average lifespan of a heart stent?
The lifespan of a heart stent depends on its type. Bare-metal stents last 10-15 years. Drug-eluting stents can last 15 years or more. Bioresorbable stents dissolve in 2-3 years.
What factors influence the longevity of a heart stent?
Several things affect a heart stent’s lifespan. These include the stent’s material and design, the patient’s age and health, and how well the stent is placed.
How can I maximize the durability of my heart stent?
To make your heart stent last longer, follow your medication plan. Quit smoking and exercise often. Also, keep up with follow-up appointments for monitoring.
What are the warning signs that a heart stent may be failing?
Signs a heart stent might be failing include chest pain, shortness of breath, or feeling very tired. If you notice these, get medical help right away.
Can a heart stent be replaced or revised?
Yes, a heart stent can be replaced or revised if needed. This might happen if the stent fails or if complications arise. Treatment options include more stenting, angioplasty, or other procedures.
How does dual antiplatelet therapy impact stent longevity?
Dual antiplatelet therapy is key to keeping stents working longer, mainly for drug-eluting stents. The therapy’s length depends on the stent type. Stopping it too soon can lead to stent thrombosis.
What are the latest advancements in heart stent technology?
New stent technologies include better materials, coatings, and designs. These advancements aim to make stents last longer and work better, reducing complications.
What is the role of bioresorbable stents in modern cardiology?
Bioresorbable stents provide temporary support and then dissolve. They might reduce long-term complications. Yet, their benefits and limitations are being studied and improved.
How do I manage my expectations after receiving a heart stent?
After getting a heart stent, understand its type, lifespan, and care needs. Follow your doctor’s advice and attend regular check-ups to monitor the stent’s performance.
References
New England Journal of Medicine. Evidence-Based Medical Insight. Retrieved from https://www.nejm.org/doi/full/10.1056/NEJMoa042753


































