Hematology focuses on diseases of the blood, bone marrow, and lymphatic system. Learn about the diagnosis and treatment of anemia, leukemia, and lymphoma.
Send us all your questions or requests, and our expert team will assist you.
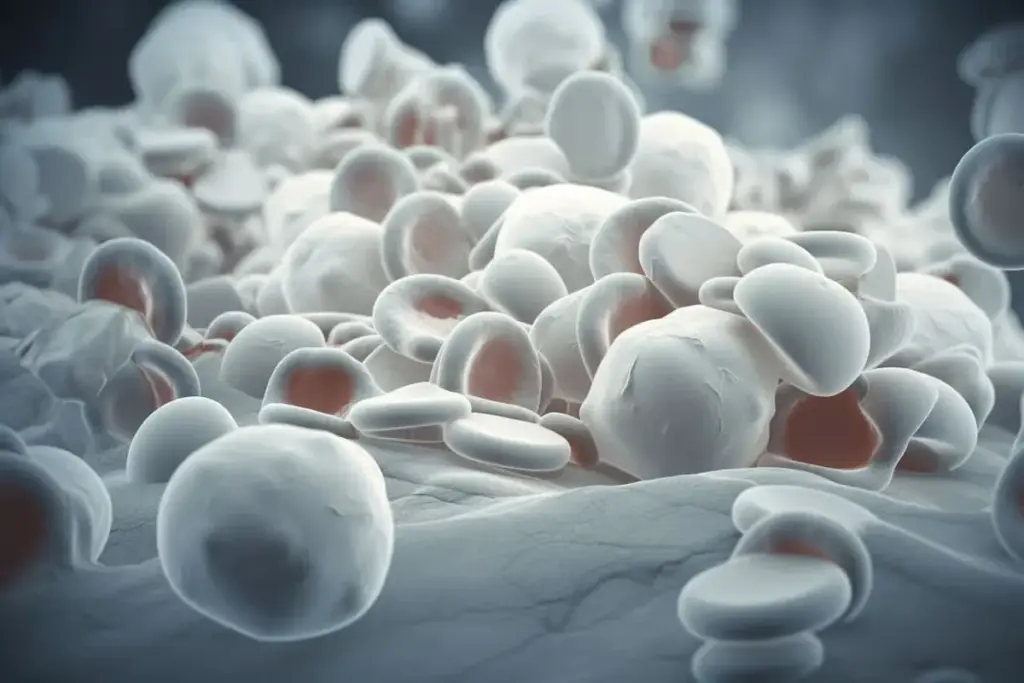
Diagnosing Myelodysplastic Syndrome is a meticulous process of exclusion and confirmation. Because the primary symptom—low blood counts—can be caused by simple vitamin deficiencies, infections, or medication side effects, doctors must rule out these reversible causes first. At Liv Hospital, the diagnostic pathway moves from peripheral blood analysis to the gold standard bone marrow examination, followed by advanced molecular profiling to determine the precise subtype and prognosis of the disease.
The first step is a detailed examination of the blood circulating in the veins.
This automated test measures the number of red cells, white cells, and platelets. In MDS, at least one of these lines will be low. The test also measures the Mean Corpuscular Volume (MCV), which indicates the size of the red blood cells. In MDS, red blood cells are often macrocytic, meaning they are larger than normal.
This measures young red blood cells. In a healthy person with anemia, the reticulocyte count should be high as the marrow tries to compensate. In MDS, the reticulocyte count is typically inappropriately low, indicating marrow failure.
A drop of blood is smeared on a slide and examined under a microscope. Pathologists look for dysplastic changes in the circulating cells, such as neutrophils with hyposegmented nuclei (Pseudo Pelger Huet anomaly) or giant platelets. They also check for the presence of blasts in the blood.
Before diagnosing a malignancy like MDS, other conditions must be excluded.
Low levels of Vitamin B12, folate, or copper can cause blood cells to look dysplastic and mimic MDS. Iron deficiency or chronic kidney disease can also cause anemia.
Chronic viral infections (like HIV or Hepatitis C) or autoimmune disorders can suppress the bone marrow.
Recent use of antibiotics, chemotherapy, or immunosuppressants can cause temporary cytopenias. Doctors carefully review the patient’s drug history.
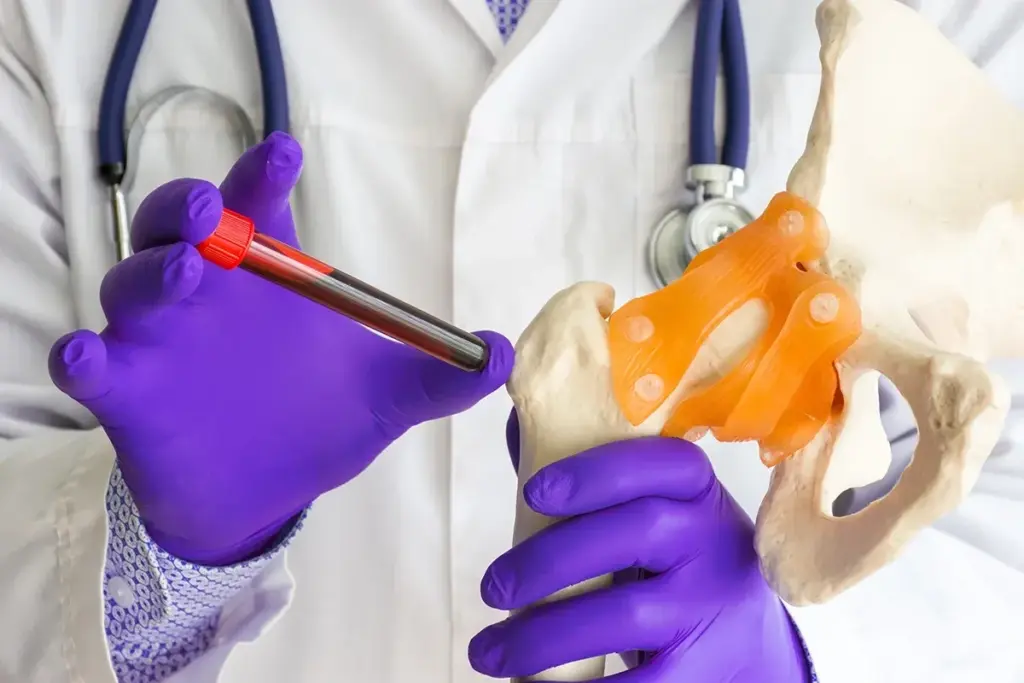
To confirm MDS, doctors must look directly at the factory where cells are made.
A needle is inserted into the posterior iliac crest (the back of the hip bone) to suction out the liquid portion of the marrow. This fluid is smeared on slides to assess the morphology (shape) of the developing cells.
A small core of solid bone and marrow tissue is removed. This allows the pathologist to assess the cellularity—how crowded the marrow is. In MDS, the marrow is usually hypercellular (too many cells) despite the low blood counts, reflecting the ineffective production.
The marrow sample is stained with Prussian blue dye to look for iron storage. In a specific subtype of MDS, iron accumulates in a ring around the nucleus of the red blood cell precursors. These are called “ring sideroblasts” and are a key diagnostic feature.
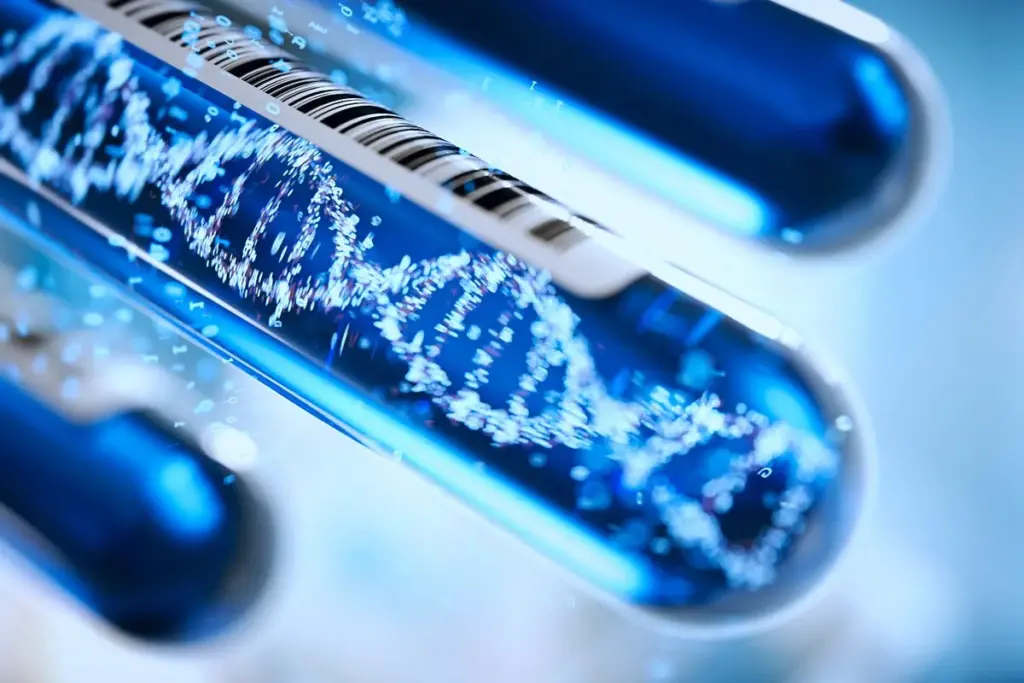
A portion of the marrow aspirate is sent for karyotyping.
This test photographs the chromosomes of the dividing cells. It identifies large structural changes, such as missing chromosomes (monosomy 7) or deleted parts (del 5q). These findings are critical for diagnosis and are the most powerful predictors of the disease course.
If dividing cells are hard to find, FISH can be used to tag specific DNA sequences with fluorescent probes to detect common abnormalities even in resting cells.
Modern diagnosis increasingly relies on identifying specific gene mutations.
Labs use NGS to screen for a panel of genes frequently mutated in MDS, such as SF3B1, TET2, SRSF2, ASXL1, and TP53.
Finding a mutation can help confirm MDS in difficult cases where the microscopic changes are subtle. For example, finding an SF3B1 mutation strongly supports a diagnosis of MDS with ring sideroblasts.
Some mutations, like TP53, are associated with a more aggressive disease and resistance to standard treatments, while others, like SF3B1, are associated with a better outcome.
Once the diagnosis is confirmed, patients are stratified by risk to guide treatment.
This is the standard tool used worldwide. It calculates a score based on five factors:
Based on the score, patients are classified into five risk groups: Very Low, Low, Intermediate, High, and Very High.
MDS can look very similar to other bone marrow disorders.
In aplastic anemia, the marrow is empty (hypocellular) and the cells are not dysplastic; they are just absent. In MDS, the marrow is usually full.
The distinction is based on the blast count. If blasts are <20%, it is MDS. If >20%, it is AML.
In these disorders, the marrow produces too many effective cells (high counts), whereas in MDS, it produces too many ineffective cells (low counts). There is also an overlap category called MDS/MPN (e.g., CMML) where patients have features of both.

Send us all your questions or requests, and our expert team will assist you.
It is performed under local anesthesia to numb the skin and bone surface. Most patients feel pressure and a brief sharp sensation during aspiration, but it is generally well tolerated and quick.
Genetic testing tells doctors how aggressive the MDS is. This helps decide if you need a stem cell transplant or if you can be managed with milder treatments.
It is an immature red blood cell with a ring of iron deposits around its nucleus. Seeing these in the marrow helps doctors diagnose a specific, usually milder, type of MDS.
It means the bone marrow is packed full of cells. In MDS, this is a sign that the marrow is trying hard to make blood, but the cells are dying before they get out.
No. While blood tests can strongly suggest MDS, a bone marrow biopsy is required to see the dysplastic cells and check genetics for a final confirmation.

 Hematology
Hematology Hematology
Hematology Hematology
Hematology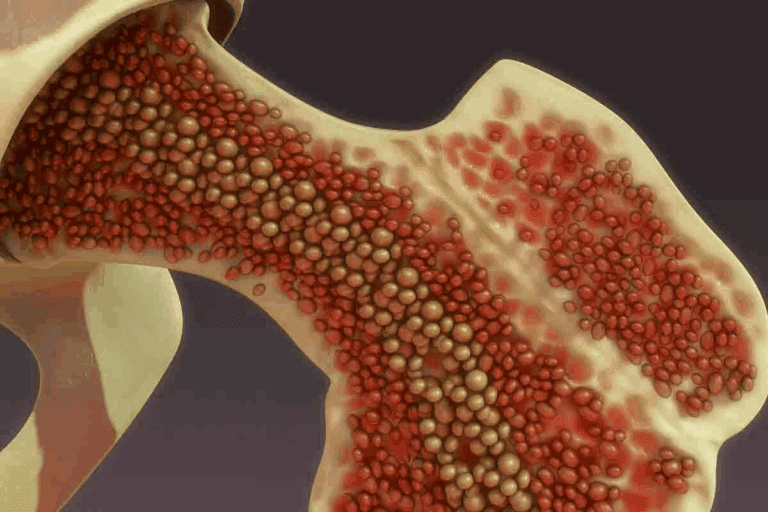 Hematology
Hematology Hematology
Hematology Hematology
Hematology
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)