
Choosing the right vascular access for dialysis patients is key for their health and happiness. Vascular access is very important for those on dialysis. Why is a hemodialysis dialysis fistula the best? Discover amazing long-term benefits and vital, powerful reasons to choose this access.
Studies show that arteriovenous fistulas are the best choice. They are safe, last long, and work well. This makes them the top pick for dialysis patients and doctors everywhere.
We focus on caring for our patients. Our aim is to give them all the info they need. This helps them make smart choices about vascular access.
Key Takeaways
- The autogenous arteriovenous fistula (AVF) is considered the gold standard for dialysis access.
- AVF offers lower rates of infection and thrombosis compared to other vascular access options.
- Superior long-term patency is a significant advantage of AVF.
- Choosing the right vascular access is key for patient outcomes and quality of life.
- Healthcare providers prioritize patient-centered care in managing vascular access.
Understanding Dialysis and the Need for Vascular Access
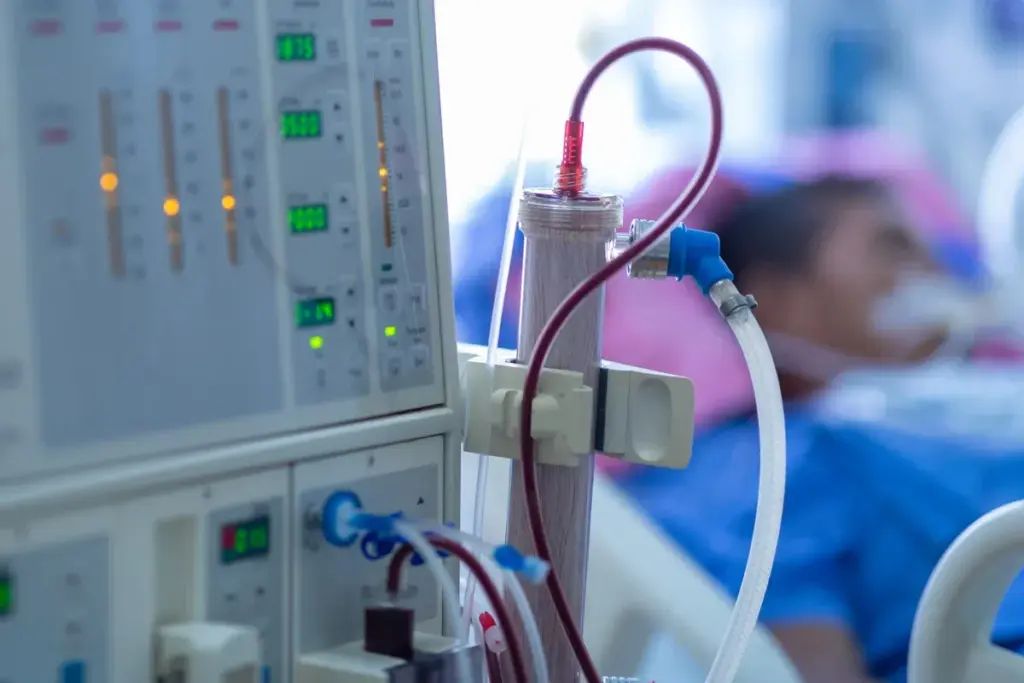
Dialysis is key for treating end-stage kidney disease. It filters waste from the blood when kidneys fail. This treatment is a lifeline for many patients.
Dialysis is more than a treatment; it’s a lifesaver. It needs careful management, focusing on vascular access. The National Kidney Foundation’s 2019 guidelines stress choosing vascular access based on patient needs. This approach improves satisfaction and outcomes.
The Role of Dialysis in End-Stage Kidney Disease
Dialysis cleans the blood using a machine when kidneys fail. There are types of dialysis, like hemodialysis and peritoneal dialysis. Each needs a specific vascular access.
Hemodialysis cleans blood outside the body. It returns the cleaned blood to the body. A hemodialysis catheter or other access is needed for this process.
Why Vascular Access is Critical for Effective Treatment
Vascular access is vital for hemodialysis patients. It allows blood to flow between the patient and the dialysis machine. A good vascular access ensures effective dialysis by removing waste.
The choice of vascular access affects patient outcomes. Options include arteriovenous fistulas (AVFs), arteriovenous grafts (AVGs), and catheter hemodialyse. Each has its benefits and challenges, depending on the patient’s health and preferences.
|
Type of Vascular Access |
Description |
Advantages |
Disadvantages |
|---|---|---|---|
|
Arteriovenous Fistula (AVF) |
Surgically created connection between an artery and a vein |
High blood flow rate, lower risk of infection, long-term durability |
Requires surgical creation, may take time to mature |
|
Arteriovenous Graft (AVG) |
Synthetic graft connecting an artery and a vein |
Can be used sooner than AVF, relatively durable |
Higher risk of thrombosis and infection compared to AVF |
|
Central Venous Catheter |
Catheter placed into a large vein for dialysis |
Can be used immediately, less surgical complexity |
Higher risk of infection and thrombosis, less ideal for long-term use |
Understanding dialysis and vascular access helps healthcare providers. They can improve patient care and outcomes. This leads to a better quality of life for patients.
Types of Vascular Access for Hemodialysis
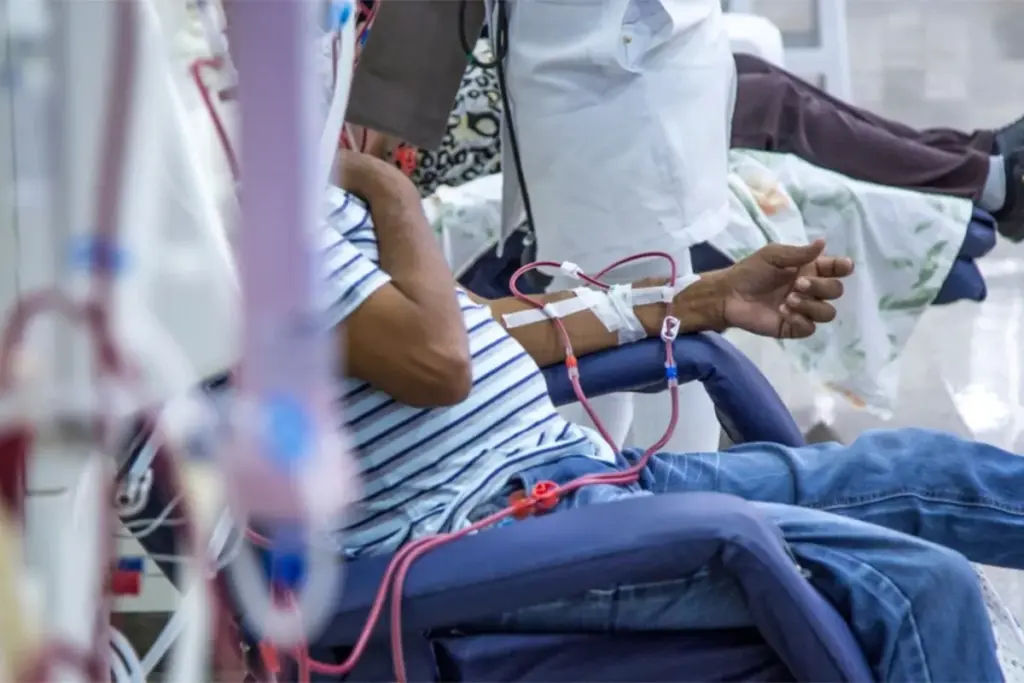
Vascular access is key for hemodialysis. Knowing the different types is vital for both patients and healthcare teams. We must weigh various factors to pick the right access for effective treatment.
Overview of Access Options
There are several vascular access options for hemodialysis. These include arteriovenous fistula (AVF), arteriovenous graft (AVG), and central venous catheters (CVCs). Each has its own pros and cons.
Temporary vs. Permanent Access Solutions
It’s important to know the difference between temporary and permanent vascular access. Central Venous Catheters (CVCs) are temporary, used in emergencies or when waiting for a permanent solution. AVFs and AVGs are more permanent choices.
|
Access Type |
Advantages |
Disadvantages |
|---|---|---|
|
Arteriovenous Fistula (AVF) |
Lower risk of infection and thrombosis, higher patency rates |
Requires surgical creation, may take time to mature |
|
Arteriovenous Graft (AVG) |
Can be used sooner than AVF, relatively durable |
Higher risk of thrombosis and infection compared to AVF |
|
Central Venous Catheter (CVC) |
Can be used immediately, useful for temporary access |
High risk of infection and thrombosis, not ideal for long-term use |
Understanding each vascular access type helps patients and healthcare teams make better choices. This improves treatment results.
Arteriovenous Fistula: The Gold Standard in Hemodialysis Dialysis Fistula
The arteriovenous fistula is the top choice for hemodialysis access. It has many benefits over other options. An AVF is a surgical link between an artery and a vein, usually in the forearm. This setup ensures high blood flow for effective dialysis.
Definition and Creation Process
An arteriovenous fistula is made by a surgeon connecting an artery to a vein. This surgery is done under local anesthesia and takes 1-2 hours. The aim is to make a strong, high-flow access for dialysis.
We suggest creating an AVF before starting dialysis. This allows the vein to mature and get ready for cannulation.
Advantages of AVF Over Other Access Types
AVFs are better than arteriovenous grafts (AVGs) and central venous catheters (CVCs) because they have fewer complications. AVFs have lower rates of infection and thrombosis. They also last longer than other access types.
The benefits of AVF include:
- Lower risk of infection
- Improved patency rates
- Reduced risk of thrombosis
- Better overall survival for patients
Maturation Timeline and Considerations
The maturation time for an AVF varies, but it usually takes 4-6 weeks. The patient’s vascular health, vessel size and quality, and surgical method affect maturation.
To help the AVF mature well, patients should follow post-surgery care. This includes exercises to improve blood flow and regular check-ups with healthcare professionals.
Understanding AVFs helps healthcare providers improve hemodialysis outcomes. We stress the need for timely AVF creation and proper care. This enhances patient quality of life and treatment success.
Arteriovenous Grafts: An Alternative Permanent Access
For patients needing hemodialysis, arteriovenous grafts (AVGs) are a key option when AVFs aren’t possible. AVGs are synthetic tubes that connect an artery and a vein. They offer a reliable way to access the body for dialysis treatment.
When and Why AVGs Are Used
AVGs are chosen for patients with veins that can’t support AVF creation. This might be due to small vein size or past vascular damage. We opt for AVGs when a patient’s veins aren’t good for a lasting AVF or if previous AVFs have failed.
Choosing an AVG requires looking at the patient’s overall health and dialysis needs. AVGs are great for patients needing dialysis right away and can’t wait for an AVF to be ready.
Comparison to Arteriovenous Fistulas
AVFs are the top choice for vascular access because they have fewer complications. But AVGs have their own benefits. They can be used sooner, usually in 2-4 weeks, unlike AVFs which take months to mature.
|
Characteristics |
Arteriovenous Fistula (AVF) |
Arteriovenous Graft (AVG) |
|---|---|---|
|
Maturation Time |
Several months |
2-4 weeks |
|
Complication Risk |
Lower |
Higher |
|
Primary Patency Rate |
Higher |
Lower |
Expected Longevity and Complications
AVGs face a higher risk of problems like stenosis, thrombosis, and infection. They also have a lower primary patency rate, meaning they might need more upkeep to stay working.
Even with these issues, AVGs are a vital option for those with few other choices. We must keep a close eye on AVGs and fix any problems quickly to make them last longer.
“The choice between AVF and AVG depends on individual patient factors, including vascular anatomy, comorbid conditions, and dialysis requirements.”
Understanding AVGs’ role in managing vascular access helps us give better care to hemodialysis patients. We can tailor our care to meet their unique needs.
Central Venous Catheters and Dialysis Ports
Managing vascular access is key for dialysis patients. They use central venous catheters and dialysis ports. These tools are vital for hemodialysis, allowing blood to flow in and out during treatment.
Types of Dialysis Catheters
Dialysis catheters come in two main types: non-tunneled and tunneled. Non-tunneled catheters are for short-term use, often in emergencies. Tunneled dialysis catheters (TDCs) are for long-term use, providing stable access.
Tunneled Dialysis Catheters (TDC) Explained
Tunneled dialysis catheters are inserted under the skin and into a vein. This method lowers infection risk and boosts catheter stability. TDCs are popular for their reliable, long-term access.
- TDCs are made from biocompatible materials to reduce adverse reactions.
- They’re designed for long-term use, lasting months or years.
- Keeping TDCs clean and well-maintained is key to avoid infections or blockages.
Chest Port Options for Dialysis Patients
Chest ports, or implantable ports, are another choice for long-term access. They’re implanted under the skin for safe, easy access to the bloodstream for dialysis.
Central venous catheters and dialysis ports are essential for dialysis patients. Knowing about different catheters and chest ports helps healthcare providers better care for patients on hemodialysis.
Understanding Dialysis Shunts and Their Role
It’s important to know how dialysis access methods have changed over time. Dialysis shunts were once a key part of treatment but are now less common. They played a big role in helping patients with vascular access for hemodialysis.
Defining Dialysis Shunts in Modern Practice
Today, dialysis shunts are not the first choice for vascular access. They have been replaced by safer and more effective options. Knowing about dialysis shunts helps us understand the progress in vascular access technology.
A dialysis shunt is a surgical connection between an artery and a vein for hemodialysis. The term “shunt” can mean different things, but in dialysis, it means a bypass for blood access.
Historical Context of Shunt Development
Dialysis shunts started in the early days of hemodialysis. They were used to access the blood for dialysis. The first shunts were external, with tubes connecting patients to machines. Later, internal shunts were made, but they had many problems like infections and blood clots.
Shunts vs. Fistulas: Key Differences
Shunts and fistulas differ in how they are made, how they work, and their risks. Arteriovenous fistulas (AVFs) are the best choice for dialysis access. They have fewer infections and blood clots than shunts. AVFs connect an artery directly to a vein, improving blood flow and reducing risks.
|
Characteristics |
Dialysis Shunts |
Arteriovenous Fistulas |
|---|---|---|
|
Construction |
External or internal bypass |
Direct artery-vein connection |
|
Infection Risk |
Higher |
Lower |
|
Thrombosis Risk |
Higher |
Lower |
Understanding the history and progress from shunts to fistulas helps us see the ongoing work to improve dialysis access. This progress is key for better care of dialysis patients.
Clinical Evidence Supporting AVF as Preferred Access
AVF is the top choice for hemodialysis access due to strong evidence. We’ll look at the key points that show AVF’s benefits over other options.
Infection and Thrombosis Rates Across Access Types
Infection rates are much lower in AVF patients. This means fewer serious problems and hospital stays. For example, a study showed AVF’s infection rate was 0.24 per 1,000 patient-days. AVGs and CVCs had higher rates.
Long-term Patency Statistics
AVF also leads in long-term use. Studies show it keeps working well over time, making dialysis reliable. A study found AVF’s primary patency rate was 60% at one year, much better than others.
The long-term patency of AVF means fewer interventions and more efficient dialysis. This is key for patient care and happiness.
Impact on Patient Survival and Quality of Life
AVF greatly improves patient survival and quality of life. It lowers complications and keeps access reliable. This leads to fewer hospital stays and better health, improving life quality.
Patient survival also benefits from AVF. The lower risk of infections and blood clots, along with AVF’s reliability, helps patients live longer while on hemodialysis.
National Kidney Foundation Guidelines on Vascular Access
Vascular access management has grown more advanced, thanks to the National Kidney Foundation (NKF). The NKF has played a key role in shaping vascular access for dialysis patients. It does this through evidence-based recommendations.
Evolution of Access Recommendations
The NKF’s vascular access guidelines have changed a lot over the years. They reflect the latest clinical evidence and best practices. At first, the focus was on finding the most effective vascular access for hemodialysis.
Now, the guidelines also consider patient-centered care and managing vascular access complications. As new evidence comes in, the NKF updates its recommendations. It now favors arteriovenous fistulas (AVFs) over other access types because of their better patency rates and lower complication risk.
“The NKF’s guidelines emphasize the importance of a patient-centered approach to vascular access management, recognizing that individual patient needs and preferences should guide clinical decision-making.”
NKF Guidelines
The 2019 Patient-Centered Approach
In 2019, the NKF introduced a patient-centered approach to its guidelines. This approach focuses on aligning vascular access decisions with each patient’s needs and preferences. It recognizes that vascular access is not one-size-fits-all and that patient outcomes improve when care is tailored to their unique circumstances.
|
Key Elements |
Description |
Benefits |
|---|---|---|
|
Patient Education |
Educating patients about their vascular access options |
Informed decision-making, improved patient satisfaction |
|
Personalized Care Plans |
Developing care plans that reflect individual patient needs |
Improved outcomes, enhanced quality of life |
|
Multidisciplinary Teams |
Collaboration among healthcare professionals to manage vascular access |
Comprehensive care, reduced complications |
Implementation Challenges in Clinical Practice
Implementing a patient-centered approach to vascular access management can be tough. Barriers include variability in patient education, limited resources, and the need for coordinated care among healthcare providers.
To overcome these challenges, healthcare providers must work together. They need to develop and implement effective strategies for vascular access management. These strategies should prioritize patient needs and preferences.
Patient Preferences and Economic Considerations
When we talk about vascular access management, we must think about patient preferences, cost, and how well treatment works. Choosing the right vascular access is key for hemodialysis. It affects how happy patients are and how well they do with treatment.
Factors Influencing Patient Access Choices
Many things affect what patients choose for vascular access. These include how easy it is to use, the chance of problems, and how it affects their life. Patient education and being part of the decision-making is key. It makes sure the access chosen fits the patient’s needs and wants.
“The patient’s view is very important in picking vascular access,” a study says. “Understanding what patients want helps doctors give better care.”
Patient Willingness to Pay for Extended Access Patency
Studies show patients are ready to pay more for longer-lasting access. A study found patients value longer-lasting access. They are willing to spend money on their health.
The Nordic-Baltic Study: Insights on Patient Choice
The Nordic-Baltic study has given us new insights into what patients want for dialysis treatment. It shows how important education and teamwork in healthcare are. These factors greatly influence a patient’s choice in dialysis access.
65% Preference for Home Dialysis
The study found that 65% of patients want home dialysis. This shows a big demand for treatments that fit the patient’s life better. Home dialysis lets patients manage their treatment at home, giving them more control and comfort.
A leading researcher said, “The high preference for home dialysis shows a move towards care that focuses more on the patient.” This change comes from patients wanting to control their treatment and keep up with their daily lives.
Barriers to Optimal Access Placement
Even though many patients want home dialysis, there are barriers to getting the best access placement. These include late referrals to vascular surgeons, not enough education before starting dialysis, and a lack of teamwork in care. Overcoming these challenges is key to making sure patients get the best dialysis access.
- Late referrals to vascular surgeons
- Inadequate pre-dialysis education
- Lack of coordinated care
Lessons for Global Dialysis Programs
The Nordic-Baltic study teaches us important lessons for dialysis programs worldwide. By knowing what patients want and the obstacles to good care, healthcare providers can make better plans to help patients. The study stresses the need for multidisciplinary care teams and patient education to help patients make informed choices.
“The Nordic-Baltic study highlights the importance of a patient-centered approach to dialysis care, stressing the need for education and teamwork.”
As we look ahead, it’s vital to use these insights to improve dialysis care everywhere. This way, we can make patients happier, reduce problems, and make dialysis better for everyone.
The Patient Journey: Long-term Access Planning
Understanding the patient journey is key for healthcare providers. It helps them plan for long-term access needs. As patients start dialysis, their vascular access needs change. This requires a detailed care plan.
Pre-dialysis Education and Preparation
Pre-dialysis education is vital for long-term planning. It teaches patients about their treatment options and vascular access. This knowledge empowers them to make better care choices.
Studies show that educated patients tend to use arteriovenous fistulas (AVFs) more. They also use fewer catheters.
Key elements of pre-dialysis education include:
- Discussion of treatment options, including hemodialysis and peritoneal dialysis
- Information about vascular access types, including AVFs and arteriovenous grafts (AVGs)
- Emphasis on the importance of timely access placement
Transitioning Between Access Types
Patients may need to switch vascular access types as they progress. This could be due to access failure or the need for a better type. A smooth transition is key to keep treatment going without interruption.
Effective transition strategies include:
- Regular monitoring of access function and patency
- Timely identification of access complications
- Collaboration between healthcare providers to coordinate access placement and maintenance
Optimizing the Lifelong Dialysis Experience
Long-term access planning is an ongoing process. It requires constant monitoring and adjustments. By understanding the patient journey, we can improve their dialysis experience.
Our aim is to provide complete care for dialysis patients. This approach enhances their quality of life and treatment outcomes.
Multidisciplinary Approach to Access Management
A team effort is key to better dialysis access outcomes. It takes teamwork among many healthcare experts to manage vascular access well.
Role of Nephrologists, Vascular Surgeons, and Interventional Radiologists
Nephrologists, vascular surgeons, and interventional radiologists are all important. Nephrologists take care of dialysis patients and handle vascular access issues. Vascular surgeons make and fix access sites with their surgical skills. Interventional radiologists do small procedures to keep access open.
Working together, these experts give patients full care. This care goes from first check-up to long-term access management.
“The team effort improves vascular access care. It makes sure patients get the right help on time.”
Vascular Mapping and Access Planning
Vascular mapping is key for planning access. It lets doctors see the patient’s blood vessels and pick the best spot for access. They use ultrasound to check the blood vessels’ quality.
Planning access also looks at the patient’s health, lifestyle, and wishes. This way, doctors create access that works well and improves the patient’s life.
|
Specialist |
Role in Access Management |
|---|---|
|
Nephrologist |
Overall patient care, complication management |
|
Vascular Surgeon |
Creation and revision of vascular access sites |
|
Interventional Radiologist |
Minimally invasive procedures for access maintenance |
Coordinated Care for Access Maintenance
Coordinated care is vital for keeping vascular access working. Regular checks and quick action can stop access problems. This avoids the need for big surgeries.
The team effort ensures patients get smooth care from start to finish. This teamwork not only helps patients but also makes their experience better.
Home Dialysis Considerations and Access Requirements
Home dialysis is becoming more popular. It offers comfort and flexibility. But, it needs special access and training for success.
Peritoneal Dialysis Catheter Options
Peritoneal dialysis (PD) uses the abdomen’s lining to filter blood. Choosing the right catheter is key for good treatment.
There are different PD catheters, each with benefits:
- Straight Tenckhoff Catheter: Simple and effective.
- Coiled Tenckhoff Catheter: Helps prevent catheter movement.
- Swan Neck Catheter: Reduces complications at the exit site.
|
Catheter Type |
Key Features |
Complication Rate |
|---|---|---|
|
Straight Tenckhoff |
Simple design, easy to place |
Moderate |
|
Coiled Tenckhoff |
Reduced tip migration |
Low to Moderate |
|
Swan Neck |
Pre-shaped bend, reduced exit-site issues |
Low |
Home Hemodialysis Access Needs
Home hemodialysis (HHD) needs reliable access for long sessions. AVFs and AVGs are common choices.
Key Considerations for HHD Access:
- Patency Rates: Long-lasting access is essential.
- Infection Risk: Keeping infections away is critical.
- Patient Training: Patients must learn to care for their access.
Self-Care Training for Access Management
Good self-care training is vital for home dialysis patients. It helps them manage their access and dialysis safely.
Components of Self-Care Training:
- Access care and maintenance techniques
- Dialysis procedure training
- Monitoring for complications and troubleshooting
- Emergency preparedness and response
Comprehensive training empowers patients to manage their treatment. This improves their dialysis experience and outcomes.
Future Innovations in Dialysis Access Technology
New technologies are changing dialysis access for the better. These advancements aim to make dialysis safer and more effective. They are designed to tackle the problems that come with dialysis access.
Advancements in Materials and Creation Techniques
New materials are being made for dialysis access. These materials are stronger and better for the body. For example, bioengineered grafts might help avoid blood clots and infections.
- Improved graft materials that reduce thrombosis and infection rates
- Advanced surgical techniques for creating more durable access sites
- Innovative vascular imaging technologies to enhance access planning
Bioengineered Vessels and Access Solutions
Bioengineered vessels are a big step forward in dialysis access. They are made to work like real blood vessels. This could make dialysis safer and less likely to cause problems
Making bioengineered vessels is a complex task. It involves using tissue engineering and regenerative medicine. These methods aim to create blood vessels for dialysis that could improve patient lives.
Wearable and Implantable Dialysis Systems
Wearable and implantable dialysis systems are gaining attention. They aim to make dialysis easier and less invasive. Wearable devices can dialyze continuously, which could lead to better health outcomes.
Implantable systems might offer a permanent fix. They could reduce the need for external access points. This could lower the risk of infections and other issues.
Looking ahead, new technologies will be key in improving dialysis access. By embracing these innovations, we can make dialysis safer and better for patients. This will help advance dialysis care.
Conclusion
Effective vascular access is key for dialysis patients. The autogenous arteriovenous fistula (AVF) is the top choice. It’s supported by clinical evidence and patient care.
We’ve talked about how AVF benefits dialysis patients. It has better patency rates and fewer complications than other options. Patient care is essential in managing vascular access.
By focusing on patient care and new technologies, we can improve dialysis outcomes. This includes bioengineered vessels and wearable dialysis systems. Proper vascular access planning is vital.
Looking ahead, we must keep a patient-centered approach. We should use the latest in hemodialysis fistula and vascular access. This will ensure top care for dialysis patients.
FAQ
What is the preferred vascular access for dialysis patients?
For dialysis patients, an autogenous arteriovenous fistula (AVF) is best. It has fewer complications and better outcomes.
What are the benefits of an arteriovenous fistula (AVF) for hemodialysis?
AVF has many advantages. It has lower infection and clotting rates. It also lasts longer and improves survival and quality of life.
What is the difference between an arteriovenous fistula (AVF) and an arteriovenous graft (AVG)?
An AVF connects an artery directly to a vein. An AVG uses a synthetic graft. AVFs are safer and preferred.
What are the types of dialysis catheters used for hemodialysis?
Dialysis catheters include tunneled and non-tunneled types. Tunneled catheters are safer for long-term use.
What is the role of a chest port in dialysis treatment?
A chest port is used for hemodialysis. It’s for patients needing long-term dialysis and have few other options.
How do National Kidney Foundation guidelines influence vascular access management?
The National Kidney Foundation guidelines recommend AVFs. They focus on patient care and AVFs as the best choice.
What are the challenges of implementing National Kidney Foundation guidelines in clinical practice?
Following the guidelines is hard. It’s due to patient health, blood vessel issues, and limited resources.
How does patient education impact vascular access management?
Educating patients is key. It helps them make informed choices and manage their access better.
What is the importance of a multidisciplinary approach to access management?
A team of doctors, surgeons, and radiologists is vital. They ensure the best care and outcomes for patients.
What are the emerging trends and technologies in dialysis access?
New developments include bioengineered vessels and wearable dialysis systems. There are also new materials and techniques for access devices.
How does home dialysis impact vascular access requirements?
Home dialysis needs specific access solutions. This includes peritoneal dialysis catheters and home hemodialysis access. These must be carefully planned and managed.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC4925201/[4



































