Nearly 30,000 people in the United States are treated for brain aneurysms every year. Many need either endovascular or neurosurgical treatments. It’s important to know the difference between these medical specialties. Find out how long does it take to become an interventional neurologist. A crucial look at the powerful training path for this specialty.
Endovascular neurosurgery uses minimally invasive procedures. Surgeons insert catheters and other tools through blood vessels. This helps treat vascular conditions in the brain and spine.
On the other hand, traditional neurosurgery is open surgery. It allows direct access to the brain or spine.
It’s key to understand these differences. This helps us see the unique training and skills needed for each field. This is true for those looking to become interventional neurologists or neurointerventional radiologists.
Key Takeaways
- Endovascular neurosurgery is a minimally invasive procedure.
- Traditional neurosurgery involves open surgery.
- Both approaches require unique training and skills.
- Interventional neurology and neurointerventional radiology are specialized fields.
- Understanding the differences is key for medical professionals and patients.
The Fundamentals of Neurosurgery

Neurosurgery has a rich history and follows certain principles today. It’s a specialized field that treats brain, spine, and nervous system problems. This field is all about surgery for these issues.
The history of neurosurgery is filled with innovation and discovery. It started with ancient skull surgeries and now includes modern microsurgery. The 20th century brought big changes with better technology and imaging.
Historical Development of Neurosurgical Techniques
Neurosurgery began with ancient skull surgeries. But it became a real medical field in the late 19th and early 20th centuries. New tools like X-rays and MRI changed everything.
In the mid-20th century, microsurgery became possible. This allowed for more precise and less invasive surgeries. Now, neurosurgery includes many techniques, from open surgeries to tiny endovascular procedures.
Core Principles and Surgical Approaches
Neurosurgery aims to protect the nervous system while treating problems. Neurosurgeons learn many surgical methods. They treat brain tumors, aneurysms, and spinal issues with open surgeries.
The right surgery depends on the condition, the patient’s health, and the risks. Neurosurgeons must keep up with new technologies and methods. This helps them give the best care to their patients.
Endovascular Procedures: A Minimally Invasive Alternative
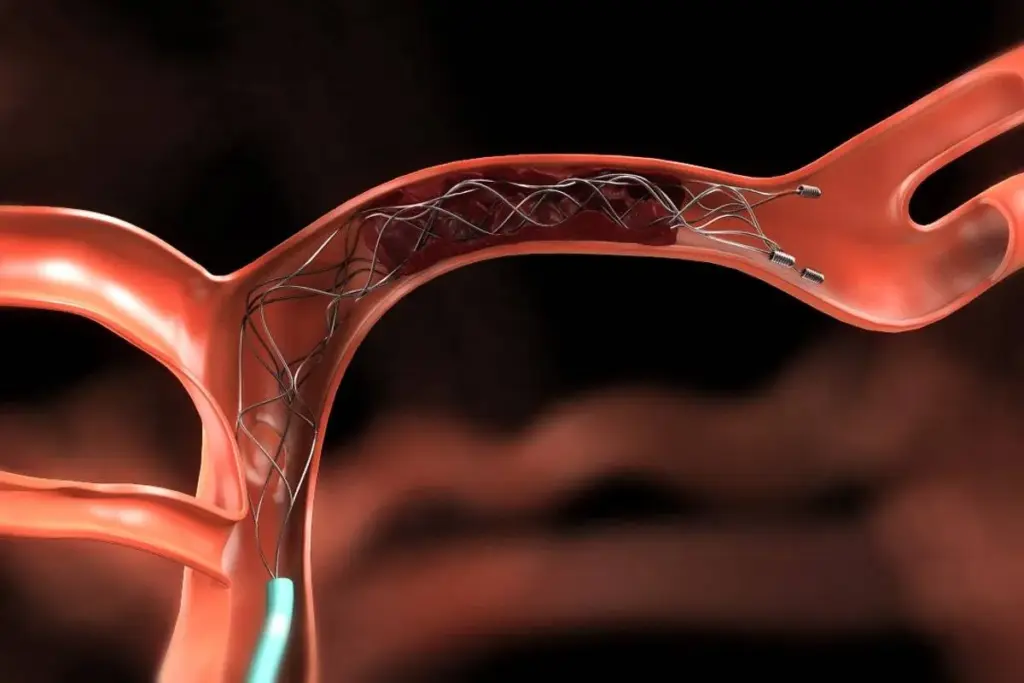
Endovascular neurosurgery is a new way to treat brain and spine vascular diseases. It’s a less invasive method compared to traditional surgery.
Defining Endovascular Interventions
Endovascular interventions use catheters and devices inserted through arteries. They aim to treat conditions like aneurysms, AVMs, and acute ischemic stroke. The endovascular meaning in neurosurgery means using these methods to treat neurovascular diseases.
These interventions have many benefits. They lead to faster recovery, fewer complications, and can treat hard-to-reach areas. As endovascular neurosurgery grows, it’s becoming key in treating neurovascular disorders.
Evolution of Catheter-Based Techniques
Advances in technology have driven the growth of catheter-based techniques. New imaging and catheter designs have improved treatments. Modern endovascular surgical neuroradiology uses the latest imaging and interventions for precise treatments.
|
Technique |
Description |
Advantages |
|---|---|---|
|
Coiling |
A procedure used to treat aneurysms by filling them with coils to prevent further bleeding. |
Minimally invasive, reduces risk of rupture |
|
Stenting |
Involves placing a stent to keep arteries open and improve blood flow. |
Reduces risk of stroke, improves vascular patency |
|
Thrombectomy |
A procedure to remove blood clots from arteries to restore blood flow. |
Effective in treating acute ischemic stroke, improves outcomes |
New technologies and techniques keep improving endovascular neurosurgery. They offer new ways to treat complex neurovascular conditions.
Comparing Endovascular and Traditional Neurosurgery: Key Differences
Endovascular and traditional neurosurgery are two different ways to treat brain and spinal problems. They use different methods, tools, and have different results.
Surgical Approach and Invasiveness
Endovascular surgery is less invasive than traditional neurosurgery. Traditional neurosurgery often means opening the skull or spine. This can lead to longer recovery times and more risks.
Endovascular procedures, on the other hand, use small instruments inserted through blood vessels. This approach is less invasive.
Key benefits of endovascular surgery include:
- Reduced risk of infection
- Less tissue damage
- Shorter hospital stays
- Faster recovery times
Equipment and Technology Requirements
The tools and technology used in endovascular and traditional neurosurgery are different. Endovascular surgery uses advanced imaging like angiography and fluoroscopy. These help guide instruments through blood vessels.
Some of the key technologies used in endovascular surgery include:
- Microcatheters and guidewires
- Stents and coils
- Advanced imaging systems
Patient Recovery and Complication Profiles
Recovery and complications differ between endovascular and traditional neurosurgery. Endovascular surgery usually means shorter recovery times and fewer complications. But, both methods have risks.
The choice between them depends on the condition and the patient’s health.
|
Aspect |
Endovascular Neurosurgery |
Traditional Neurosurgery |
|---|---|---|
|
Invasiveness |
Minimally invasive |
Invasive |
|
Recovery Time |
Generally shorter |
Often longer |
|
Complication Risk |
Lower |
Higher |
Neurology vs. Neurosurgery: Understanding the Distinct Specialties
It’s important to know the difference between neurology and neurosurgery. Both are key in treating brain and nervous system problems. But they have different ways of working and areas of focus.
The Neurologist’s Role in Diagnosis and Medical Management
Neurologists are doctors who deal with brain, spinal cord, and nervous system issues. They use medicine, lifestyle changes, and other non-surgical methods to treat these problems.
Key responsibilities of neurologists include:
- Conducting thorough neurological examinations
- Interpreting diagnostic tests such as EEGs and EMGs
- Prescribing medications for neurological conditions
- Managing chronic neurological disorders
When Neurological Conditions Require Surgical Intervention
Neurosurgeons are trained for surgical treatments of brain and nervous system issues. They work with neurologists to decide when surgery is needed.
The decision to opt for surgery is typically made when:
- A condition is life-threatening or significantly impacts quality of life
- Medical management has been ineffective
- Surgical intervention offers a significant improvement
Neurologists and neurosurgeons work together for conditions like stroke, brain tumors, and vascular malformations.
|
Aspect |
Neurology |
Neurosurgery |
|---|---|---|
|
Primary Approach |
Medical Management |
Surgical Intervention |
|
Common Conditions |
Epilepsy, Multiple Sclerosis, Parkinson’s Disease |
Brain Tumors, Aneurysms, Vascular Malformations |
|
Treatment Modalities |
Medications, Lifestyle Changes |
Surgery, Endovascular Procedures |
In conclusion, neurology and neurosurgery are two different fields. But they work together to give the best care to patients with brain and nervous system problems. Knowing their roles and how they help each other is key for the best patient results.
Interventional Neurology: Bridging Medical and Surgical Neurological Care
Interventional neurology is a new field that connects medical and surgical care for the brain. It helps patients with brain and blood vessel problems. This field uses small, safe procedures to improve treatment results.
The Emergence of Interventional Neurology as a Subspecialty
Interventional neurology started from the mix of neurology, radiology, and vascular surgery. It has grown fast thanks to new tech and skills. Interventional neurologists can now do many procedures that used to be done by others.
This new field is needed because of the need for safe, small treatments for brain and blood vessel diseases. Now, problems like stroke, brain spasms, and aneurysms can be treated better and with less risk.
Scope of Practice and Common Procedures
Interventional neurologists do many procedures. They treat stroke, brain spasms, and blood vessel problems. They need to know a lot about brain and blood vessel anatomy.
A study says, “Interventional neurology has changed how we treat brain and blood vessel diseases. It offers new ways to help patients and better results.”
“The future of brain and blood vessel care is bright. It will keep getting better with interventional neurology’s small, safe methods and focus on the patient.”
The work of interventional neurologists is growing. They use new imaging and tools for their work. This helps them do their job better and safer.
Neurointerventional Radiology: Imaging-Guided Treatments
Neurointerventional radiology combines advanced imaging with interventional procedures. It treats many neurological conditions. This field is key in diagnosing and treating neurovascular diseases. It offers less invasive options than traditional surgery.
The Role of Advanced Imaging in Neurointerventional Procedures
Technologies like angiography and fluoroscopy are vital in neurointerventional radiology. They let neurointerventional radiologists see blood vessels in real-time. This helps guide the precise delivery of treatments.
Key Imaging Modalities:
- Digital Subtraction Angiography (DSA)
- Fluoroscopy
- Roadmapping
- 3D Rotational Angiography
Diagnostic and Therapeutic Applications
Neurointerventional radiology covers a wide range of procedures. It helps diagnose vascular issues and treat acute ischemic strokes. The field is growing, with more applications being found.
|
Procedure |
Description |
Clinical Application |
|---|---|---|
|
Cerebral Angiography |
Diagnostic imaging of cerebral vessels |
Detection of aneurysms, arteriovenous malformations |
|
Mechanical Thrombectomy |
Removal of blood clots from cerebral vessels |
Treatment of acute ischemic stroke |
|
Coiling of Aneurysms |
Endovascular occlusion of aneurysms |
Prevention of aneurysmal rupture |
A leading neurointerventional radiologist notes, “Advanced imaging and interventional techniques have changed neurovascular disease treatment. They offer safer, more effective options for patients.”
“The future of neurointerventional radiology lies in its ability to continue innovating and improving patient outcomes through minimally invasive procedures.”
Neurointerventional Radiologist
The field of neurointerventional radiology is rapidly evolving. Advances in imaging and endovascular techniques are ongoing. As it grows, neurointerventional radiology will play a bigger role in managing neurovascular conditions.
How Long Does It Take to Become an Interventional Neurologist?
Becoming an interventional neurologist takes many years of hard work. You need to go through a lot of academic and clinical training. This training helps you learn everything you need to know and do well in this field.
Undergraduate and Medical School Requirements
First, you need to get an undergraduate degree in a science field. Then, you spend four years in medical school to get your MD or DO. In medical school, you learn a lot about medicine and start to see if neurology is for you.
Neurology Residency Training
After medical school, you start a neurology residency. This lasts from three to four years. You learn a lot about brain disorders and how to treat them. You work with experienced neurologists to get better at taking care of patients.
Interventional Neurology Fellowship
Then, you do a fellowship in interventional neurology. This lasts one to two years. You learn about the special techniques and tools used in this field, like treating strokes.
Board Certification and Continuing Education
After that, you get certified in neurology and maybe in interventional neurology too. To keep your certification, you need to keep learning new things. This is important because the field of interventional neurology is always changing.
It takes over a decade of hard work to become an interventional neurologist. But for those who really care about helping people with brain problems, it’s all worth it.
The Path to Becoming an Endovascular Neurosurgeon
To become an endovascular neurosurgeon, one must go through a tough journey. This includes education, residency, and fellowship training. It’s a field that needs a deep understanding of neurosurgery and endovascular techniques.
Neurosurgery Residency Timeline and Requirements
The first step is a neurosurgery residency program. These programs last 6-7 years. They offer training in neurosurgical techniques, patient care, and related sciences.
Residents get hands-on experience in various neurosurgical procedures. This includes vascular neurosurgery. Residency programs are very competitive. Selection is based on academic performance, research experience, and letters of recommendation.
The curriculum includes both clinical and research parts. This ensures residents are well-rounded and ready for neurosurgical practice.
Endovascular Fellowship Training for Neurosurgeons
After finishing a neurosurgery residency, aspiring endovascular neurosurgeons go for endovascular fellowship programs. These programs focus on endovascular neurosurgery techniques like aneurysm coiling and thrombectomy.
Endovascular fellowship programs last 1-2 years. They offer deep training in catheter-based interventions and imaging techniques. Fellows work with experienced endovascular neurosurgeons to learn how to manage complex neurovascular conditions.
By combining a neurosurgery residency with endovascular fellowship training, surgeons get the advanced skills needed. This training is key for delivering top-notch care to patients with neurovascular disorders.
Training as a Neurointerventional Radiologist
Specializing in neurointerventional radiology requires a tough training program. It mixes diagnostic radiology with advanced interventional techniques. You need to know a lot about radiology and neurological disorders.
Diagnostic Radiology Residency
The journey starts with a diagnostic radiology residency. It teaches the basics of radiological imaging and diagnostic techniques. You’ll learn to interpret images and understand radiation safety.
This residency lasts four years. You’ll work in different radiology departments. This training is key for becoming good at neurointerventional radiology.
Neuroradiology and Neurointerventional Fellowships
After the residency, you need to do fellowship training. Neuroradiology fellowships focus on imaging and diagnosing neurological conditions. Neurointerventional fellowships teach you about treatments for neurovascular diseases.
These fellowships last one to two years. You’ll get to practice complex procedures under expert supervision.
Alternative Pathways for Radiologists
If you can’t do a dedicated fellowship, there are other ways. Some places offer shorter programs or courses. These help you learn specific skills.
Professional societies like the Society of NeuroInterventional Surgery (SNIS) also help. They offer educational resources and conferences. This keeps you up-to-date with the latest in neurointerventional radiology.
Common Endovascular Neurosurgical Procedures
Endovascular neurosurgery uses minimally invasive methods to treat brain and spine vascular issues. These methods have changed how we manage complex neurovascular diseases. They offer safer options than traditional surgery.
Aneurysm Treatment: Coiling, Stenting, and Flow Diversion
Aneurysms are abnormal blood vessel dilations that can rupture. This can lead to serious bleeding. Endovascular methods are now the top choice for treating many aneurysms.
Coiling fills the aneurysm with platinum coils to stop blood flow. Stenting and flow diversion are for more complex cases. They use a stent or flow diverter to block the aneurysm from the blood flow.
Acute Stroke Intervention: Thrombectomy and Thrombolysis
Acute ischemic stroke happens when a blood clot blocks a brain artery. Thrombectomy removes the clot with special devices. Thrombolysis uses drugs to dissolve the clot.
These treatments must be done quickly to save brain tissue. They are critical for restoring blood flow.
|
Procedure |
Description |
Indications |
|---|---|---|
|
Coiling |
Filling aneurysm with platinum coils |
Aneurysm treatment |
|
Thrombectomy |
Mechanical removal of blood clot |
Acute ischemic stroke |
|
Flow Diversion |
Placing flow diverter across aneurysm neck |
Complex aneurysm treatment |
Vascular Malformation Management
Vascular malformations, like AVMs, can cause symptoms or bleeding. Endovascular methods are used to shrink these malformations. This reduces the risk of bleeding.
Endovascular neurosurgery keeps improving, thanks to new technology and techniques. These procedures are key to modern neurovascular care.
Traditional Open Neurosurgical Procedures
Traditional open neurosurgery involves surgeries that need direct access to the brain or spine. These methods have been improved over years to treat complex brain and spine issues well.
Cranial Procedures are key in neurosurgery. They treat brain tumors, vascular lesions, and other brain conditions. Neurosurgeons use advanced tools and imaging to find and treat these problems accurately.
Cranial Procedures: Brain Tumors and Vascular Lesions
Brain tumors need surgery to relieve pressure, remove the tumor, or prepare for other treatments. Vascular lesions, like aneurysms and AVMs, also require surgery. Techniques like clipping for aneurysms or removing AVMs are vital for managing these serious conditions.
Spine Surgery and Peripheral Nerve Interventions
Spine surgery treats many spinal disorders, like herniated discs and spinal stenosis. It can help with pain, stabilize the spine, and improve function. Peripheral nerve interventions, like decompressing or repairing nerves, treat issues like carpal tunnel syndrome.
The need for skill and precision in these surgeries highlights the importance of neurosurgery. New techniques, tools, and technology are making these surgeries more effective for patients.
The Multidisciplinary Approach: When Specialties Collaborate
Treating complex neurovascular conditions needs a team effort. Specialists from different fields work together. This is key in stroke care, where quick and coordinated action can make a big difference.
“A team-based approach is essential for treating neurovascular diseases,” says a medical expert. This is shown in how stroke centers work. They have neurologists, neurosurgeons, and more, all working together.
Comprehensive Stroke Centers and Team-Based Care
Comprehensive stroke centers focus on top-notch, coordinated care for stroke patients. They have a team of experts, including neurologists and neurosurgeons. This team ensures patients get the right care fast, leading to better results.
The benefits of these centers are clear:
- Quick assessment and treatment of stroke patients
- Access to many specialists
- Coordinated care across different fields
- Improved patient outcomes thanks to timely care
Hybrid Operating Rooms and Combined Procedures
Hybrid operating rooms are a big step forward in treating complex neurovascular conditions. They mix traditional operating room features with advanced imaging. This lets surgeons and endovascular specialists work together in one place.
Hybrid ORs make complex cases easier to handle. For example, they can handle both surgical clipping and endovascular coiling of aneurysms at the same time. This can cut down on the number of procedures needed and improve patient results.
Hybrid ORs offer several benefits:
- Improved teamwork between surgical and endovascular teams
- More efficient handling of complex cases
- Less need for multiple procedures or transfers
- Better patient outcomes thanks to better care coordination
A top neurosurgeon says, “Hybrid ORs have changed how we tackle complex neurovascular cases. They let us give our patients more complete and effective care.”
Career Comparison: Lifestyle, Compensation, and Job Market
Choosing a career in neurology or neurosurgery is a big decision. Each field has its own challenges and rewards that affect your lifestyle and money. It’s important to know these things if you’re thinking about a career in these areas.
Work Hours and Call Responsibilities
Neurologists and neurosurgeons work long hours. But their jobs are different. Neurosurgeons might have schedules that change a lot because of surgery.
On-call responsibilities also differ. Neurosurgeons often have to be on call more because their work is urgent.
Salary Expectations Across Specialties
How much neurologists and neurosurgeons make can vary a lot. This depends on where they work, their practice type, and how long they’ve been doing it.
|
Specialty |
Median Salary |
Range |
|---|---|---|
|
Neurologist |
$280,000 |
$220,000 – $350,000 |
|
Neurosurgeon |
$620,000 |
$450,000 – $750,000 |
Geographic Distribution and Practice Settings
The job market for neurologists and neurosurgeons changes depending on where you are. Cities usually have more job options than rural areas. Also, whether you work in an academic setting, private practice, or a mix can affect how happy you are with your job.
Practice settings are key to job satisfaction. Some like working in academia, while others prefer private practice.
Knowing these details can help you decide which career path is right for you.
Technological Innovations Shaping Both Fields
Advanced technologies are changing how we treat neurological issues. They make neurosurgery more precise and effective.
Technologies keep improving in neurology and neurosurgery. Advances in imaging and navigation systems make surgeries safer and more precise. These tools help surgeons see and work on complex areas better.
Advances in Imaging and Navigation Systems
Modern imaging like high-resolution MRI and CT scans gives surgeons detailed views for planning. Navigation systems, including augmented reality, offer real-time feedback. This helps surgeons aim for the right spots and avoid damage.
- Improved visualization through advanced imaging modalities
- Enhanced precision with navigation systems
- Better patient outcomes due to reduced risk of complications
A recent study showed how vital these technologies are in neurosurgery. They make complex surgeries safer and more effective.
“The future of neurosurgery lies in the continued integration of technology and surgical expertise, pushing the boundaries of what is currently possible.”
Next-Generation Devices and Materials
are opening up new possibilities in neurosurgery. New stents, coils, and agents are helping treat tough neurovascular problems.
These new tools are making treatments more effective and reducing recovery times. For example, biodegradable stents and drug-eluting devices are giving hope to those with hard-to-treat vascular issues.
- Bioactive stents for improved vascular health
- Advanced aneurysm coils for better occlusion
- Novel embolic agents for effective treatment
As new technologies come along, they will keep changing neurological care. They promise better treatments and outcomes for patients.
Patient Selection: When to Choose Endovascular vs. Open Neurosurgery
Choosing between endovascular and open neurosurgery depends on many factors. These include the type of condition and the patient’s health. Each case is unique, requiring a tailored approach.
Condition-Specific Considerations
The location and type of lesion are key in deciding the best surgery. Some vascular issues are better treated with endovascular methods. Others need open neurosurgery.
Key condition-specific factors include:
- Location and accessibility of the lesion
- Type and size of the vascular lesion
- Presence of comorbidities or complicating factors
Patient Factors Influencing Treatment Decisions
Patient health and history also shape treatment choices. These factors include the patient’s overall health and personal wishes.
Patient factors to consider:
|
Factor |
Endovascular Considerations |
Open Neurosurgery Considerations |
|---|---|---|
|
Age and Health Status |
May be preferred for older patients or those with significant comorbidities |
May be more suitable for younger patients with fewer comorbidities |
|
Lesion Characteristics |
Ideal for certain vascular lesions or aneurysms |
Preferred for lesions that are not accessible or suitable for endovascular treatment |
|
Patient Preference |
Some patients may prefer minimally invasive procedures |
Others may prefer a more definitive treatment approach |
Healthcare providers must weigh both condition-specific and patient-related factors. This ensures the best treatment for each patient.
Conclusion: The Future of Neurovascular Care and Specialization
The field of neurovascular care is changing fast. This is thanks to new tech and our growing knowledge of neurovascular diseases. As we move forward, specialization in neurology and neurosurgery will be key to top-notch patient care.
New treatments and methods are on the horizon. They will need teamwork and creativity from neurologists, neurosurgeons, and radiologists. The future of neurovascular care will also be influenced by the latest in imaging and device technology.
As more people need specialized care, it’s vital for these experts to work together. This way, we can better care for patients and push the boundaries of neurovascular care.
FAQ
What is the difference between endovascular neurosurgery and traditional neurosurgery?
Endovascular neurosurgery uses small tools inserted through blood vessels. Traditional neurosurgery involves open surgery to directly access the brain or spine.
What is interventional neurology?
Interventional neurology combines medical and surgical care. It uses minimally invasive procedures to treat vascular conditions in the brain and spine.
What is neurointerventional radiology?
Neurointerventional radiology uses advanced imaging to guide procedures. It helps diagnose and treat neurovascular conditions.
How long does it take to become an interventional neurologist?
It takes a lot of time to become an interventional neurologist. You need to finish college, medical school, and a residency. Then, you do a fellowship and get certified.
What is the role of a neurointerventional radiologist?
Neurointerventional radiologists work with other specialists. They use their imaging and intervention skills to treat neurovascular conditions.
Can neurologists perform surgery?
No, neurologists usually don’t do surgery. But, interventional neurologists can do minimally invasive procedures.
What is the difference between neurology and neurosurgery?
Neurology focuses on diagnosing and treating medicine. Neurosurgery involves surgery when needed.
What is endovascular meaning?
Endovascular means using minimally invasive procedures through blood vessels.
What is the training pathway to become an endovascular neurosurgeon?
To become an endovascular neurosurgeon, you need a neurosurgery residency. Then, you get specialized training through fellowship programs.
What are common endovascular neurosurgical procedures?
Common procedures include treating aneurysms and managing vascular malformations. They also include acute stroke intervention.
What is the role of advanced imaging in neurointerventional procedures?
Advanced imaging, like angiography, guides neurointerventional procedures. It helps with precise treatment.
References
National Institutes of Health. Evidence-Based Medical Insight. Retrieved from https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Brain-Aneurysms-Fact-Sheet




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News






























