Choosing how many embryos to transfer in IVF is key in fertility care.how many embryos are transferred in ivfWhere do embryonic stem cells come from? The American Society for Reproductive Medicine (ASRM) has guidelines. These aim to help have single babies and lower risks of having twins or more.
ASRM guidelines have changed how we do things. They show that choosing to transfer just one embryo can work well. It also helps avoid more serious problems.
We know it’s important to find a balance. We want success in having a baby, but also safety for the mother. Following ASRM’s advice helps doctors give the best care to their patients.
Key Takeaways
- ASRM guidelines promote singleton gestation and reduce multiple pregnancy risks.
- Selective single embryo transfer can achieve excellent outcomes while minimizing complications.
- Balancing success rates with patient safety is key in fertility care.
- ASRM recommendations help healthcare providers deliver the best possible care.
- Evidence-based guidelines are essential in determining the number of embryos to transfer.
The Fundamentals of IVF Embryo Transfer
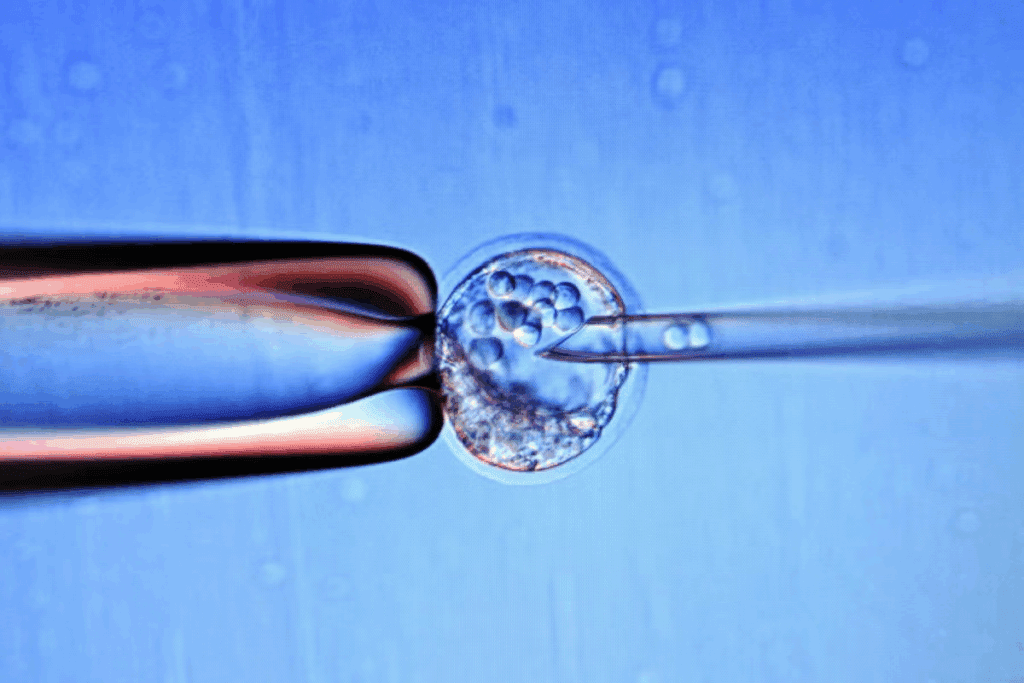
Understanding IVF embryo transfer is key for those going through fertility treatments. This process is complex and involves many steps to increase its success rate.
The Clinical Procedure Explained
The IVF embryo transfer is a crucial step in the IVF journey. It involves putting one or more embryos into the woman’s uterus. This happens 3-5 days after egg retrieval.
We use ultrasound to guide the placement of embryos. This helps ensure they are placed correctly, boosting the chances of a successful implantation.
The process starts with a detailed review of the patient’s medical history and embryo quality. On the transfer day, the patient lies on an examination table. The cervix is then cleaned.
A catheter with the embryos is inserted through the cervix into the uterus. The embryos are released into the uterine cavity. The catheter is then removed carefully to confirm all embryos have been transferred.
Why Transfer Numbers Matter
The number of embryos to transfer is a critical decision. It greatly affects IVF success and the risk of multiple pregnancies. Too many embryos can lead to complications for the mother and babies. Too few may lower the chances of a successful pregnancy.
The American Society for Reproductive Medicine (ASRM) offers guidelines. These help fertility specialists and patients decide on the number of embryos to transfer. The goal is to reduce the risks of multiple pregnancies.
We work with our patients to find the best number of embryos to transfer. We consider their individual situation, medical history, and embryo quality. This approach helps balance the desire for a successful pregnancy with the need to minimize risks.
How Many Embryos Are Transferred in IVF: Standard Practices
To understand IVF, we need to look at current practices and what influences them. The debate over how many embryos to transfer is ongoing. It’s about finding the right balance between successful pregnancies and the risks of having twins or more.
Statistical Trends in the United States
The Society for Assisted Reproductive Technology (SART) and the American Society for Reproductive Medicine (ASRM) have shared important data. They show a trend towards transferring just one embryo at a time, mainly for younger patients and those with a good chance of success.
Key statistics include:
- More women under 35 are choosing single embryo transfers (SET).
- The average number of embryos per cycle is going down.
- There’s a lot of variation in practices across different clinics and areas.
International Comparison of Transfer Practices
IVF practices vary worldwide. Some places follow stricter guidelines for embryo transfers, influenced by laws and rules.
Notable international trends include:
- Countries like Sweden and Japan are leading in single embryo transfers, thanks to guidelines and patient choices.
- Other places have higher rates of transferring more than one embryo, due to insurance and clinic policies.
- National guidelines and laws play a big role in how embryo transfers are handled.
Looking at these trends helps us understand the complexities of IVF. It shows us the factors that decide how many embryos are transferred and why.
ASRM Guidelines for Embryo Transfer
It’s key for IVF patients to know about ASRM’s embryo transfer advice. The American Society for Reproductive Medicine (ASRM) sets rules. These rules help doctors tell patients how many embryos to transfer. This balance aims to increase pregnancy chances while avoiding too many babies.
Current Recommendations by Patient Category
ASRM sorts patients by age, health, and other factors. For those with good chances of success, single embryo transfer is often advised. This reduces the risk of having twins or more. The guidelines are specific to each age group and situation, making care more personal.
Evolution of Guidelines Over Time
ASRM has updated its rules over the years. These changes reflect new IVF tech and patient trends. Now, they suggest transferring fewer embryos to lower the risk of multiple births. This shows the need to keep up with new research and practices.
Scientific Basis for Recommendations
The ASRM guidelines are based on a deep look at research and data. They use studies on IVF success, embryo quality, and patient health. This ensures the advice is backed by science. Following these guidelines helps doctors tailor care for each patient, aiming for the best IVF outcome.
By sticking to ASRM’s embryo transfer rules, patients and doctors make smart choices. They aim for a successful pregnancy while keeping risks low. As IVF tech gets better, these guidelines will keep being a key tool for doctors.
Elective Single Embryo Transfer (eSET)
Elective single embryo transfer (eSET) is a key part of IVF treatments. It aims to lower the risk of multiple births while keeping success rates high. This method involves choosing and transferring just one embryo, unlike the old way of transferring many to up the pregnancy chances.
Definition and Criteria for eSET
eSET means transferring a single embryo with a strong chance of implantation and pregnancy. The choice for eSET depends on the patient’s age, embryo quality, and past IVF results. Women under 35 with top-notch embryos and no failed IVF cycles are often picked for eSET.
Doctors follow guidelines from groups like the American Society for Reproductive Medicine (ASRM) when deciding on eSET. These rules help find the right patients for eSET, cutting down the risk of having twins or more.
Success Rates and Outcomes
Research shows eSET lowers the risk of multiple births without hurting the chances of a live birth for those with a good chance of success. In fact, eSET’s live birth rate can match that of transferring two embryos, but with much less risk of twins or more.
Also, eSET cuts down on pregnancy problems like preterm labor and low birth weight, common in multiple births. This makes eSET a safer choice for both mom and baby.
Who Benefits Most from eSET
Those most likely to benefit from eSET are women under 35 with high-quality embryos and no failed IVF cycles. Also, those at risk for multiple births, like those with a history of twins or certain health issues, can also see benefits from eSET.
Choosing eSET should be a personal decision, considering each patient’s unique situation, goals, and preferences. This way, patients can make choices that best fit their needs and increase their chances of a healthy pregnancy.
Double Embryo Transfer Considerations
IVF patients often face a big decision: whether to choose a double embryo transfer. This choice weighs the benefits of higher pregnancy success rates against the risks of multiple pregnancies.
Medical Indications for Multiple Embryo Transfer
Double embryo transfer might be suggested for those with a tough time getting pregnant. This includes people who have failed IVF cycles before, are older, or have poor embryo quality. In these cases, transferring two embryos could up the chances of getting pregnant.
But, it’s vital to look at the individual’s medical history and current health before deciding. Things like the patient’s age, embryo quality, and past IVF results are key in choosing the right path.
Risk Assessment for Twin Pregnancies
One big risk of double embryo transfer is the chance of having twins. Twin pregnancies pose higher risks for both mom and babies, including pregnancy and childbirth complications.
Women expecting twins face a higher risk of gestational diabetes, hypertension, and preterm labor. Also, twin pregnancies need more prenatal care and monitoring, which can be expensive and time-consuming.
Balancing Success Rates with Health Risks
Choosing double embryo transfer means balancing the wish for a successful pregnancy with the risks. While two embryos might up the pregnancy chances, it’s important to think about the risks of multiple gestations.
We work closely with our patients to find the best option for them. This includes talking about the benefits and risks of double embryo transfer and creating a plan that fits their reproductive goals and health.
By carefully looking at medical indications and risks, we help patients make informed choices about their IVF treatment.
Age-Related Factors in Embryo Transfer Decisions
Age is key when deciding how many embryos to transfer during IVF. As women get older, their eggs quality and number drop. This affects IVF success rates. The American Society for Reproductive Medicine (ASRM) has guidelines to help. They consider age to increase pregnancy chances and lower multiple birth risks.
Recommendations for Women Under 35
Women under 35 should usually transfer just one embryo, says ASRM. This is called elective single embryo transfer (eSET). It reduces twin pregnancy risks while keeping success rates high. Women under 35 with good embryos often succeed with eSET.
Considerations for Women 35-37
Women 35-37 see egg quality decline more. ASRM suggests transferring one or two embryos, based on embryo quality and past IVF results. The choice depends on a detailed patient assessment and history.
Approaches for Women 38-40
Women 38-40 might need to transfer two embryos. Success with one might be lower due to egg quality and quantity decline. But, transferring two embryos increases twin pregnancy risks.
Strategies for Women Over 40
Women over 40 face lower IVF success rates due to egg quality and quantity drop. ASRM suggests transferring two or more embryos to increase pregnancy chances. But, this must weigh against the higher risks of multiple pregnancies in older women.
In summary, age is a major factor in choosing how many embryos to transfer in IVF. Following ASRM guidelines helps healthcare providers make informed decisions. This balances the desire for a successful pregnancy with the need to avoid risks.
Embryo Quality and Grading Systems
Grading embryos is a complex process that greatly affects IVF success. The quality of an embryo is key to getting pregnant through IVF. We use a grading system to check the embryo’s shape and health.
Understanding Embryo Grading
Grading embryos looks at their shape, cell count, and how evenly cells divide. High-quality embryos have more cells, even sizes, and little to no damage. Our team uses a detailed system to pick the best embryo for transfer.
How Quality Affects Transfer Decisions
The embryo’s quality decides how many to transfer in IVF. High-quality embryos are more likely to implant and lead to a pregnancy. So, we often choose to transfer just one high-quality embryo to avoid multiple pregnancies and keep success rates high.
Blastocyst vs. Cleavage Stage Transfers
Embryo transfer can happen at two stages: cleavage (day 3) or blastocyst (day 5 or 6). Blastocyst transfer is more natural and lets us pick better embryos. It usually has a higher success rate than cleavage-stage transfer.
Knowing the differences between these stages and embryo quality is key for making good IVF choices. Our aim is to offer personalized care that boosts success rates and reduces risks.
The Impact of PGT-A Testing on Transfer Numbers
Preimplantation genetic testing for aneuploidy (PGT-A) has changed IVF. It helps pick the best embryos for transfer. This leads to better implantation rates and fewer risks of multiple pregnancies.
Single Euploid Embryo Transfer Success Rates
Single euploid embryo transfers with PGT-A show high success rates. Only healthy embryos are transferred, boosting implantation chances and lowering miscarriage risks. This is great for those who’ve struggled with getting pregnant or having miscarriages.
Research backs up PGT-A’s role in improving IVF results. A single healthy embryo transfer can match or beat the success of multiple embryo transfers without testing.
Multiple Euploid Embryo Transfer Considerations
Though single embryo transfer is common, sometimes transferring more is considered. This depends on the patient’s age, embryo quality, and past IVF results. But, it’s important to think about the risks of twin pregnancies.
Doctors must weigh the pros and cons of embryo transfer numbers. Personalized treatment plans help make decisions that fit each patient’s needs and wishes.
Cost-Benefit Analysis of Testing Before Transfer
PGT-A testing’s cost is a big factor in IVF. Though it’s expensive upfront, its long-term benefits are worth it. It cuts down on failed transfers and the risks of multiple pregnancies, saving money in the long run.
The emotional and mental benefits of a successful single pregnancy are huge. PGT-A testing helps make IVF more positive by increasing the chances of a healthy single birth.
Previous IVF Cycle Outcomes and Their Influence
Previous IVF cycle results are key in planning future transfers. They help doctors tailor treatments to boost success rates.
Adjusting Strategy After Failed Transfers
Failed IVF cycles mean it’s time to rethink the approach. We look at embryo quality, how ready the uterus is, and when to transfer. We might tweak medication doses, how we stimulate ovaries, or the embryo transfer method.
Table: Considerations for Adjusting IVF Strategy
| Factor | Potential Adjustments |
|---|---|
| Embryo Quality | Consider PGT-A testing, adjust culture media |
| Uterine Receptivity | Evaluate uterine lining, consider hysteroscopy |
| Transfer Technique | Adjust catheter placement, consider ultrasound guidance |
Recurrent Implantation Failure Approaches
Dealing with recurrent implantation failure (RIF) is tough. It’s when many IVF cycles don’t lead to pregnancy. We look into reasons like immune issues, blood clotting problems, or uterine shape. We might suggest more tests or specific treatments based on what we find.
Success Patterns and Predictive Factors
Studying past IVF results helps spot trends and what might work. We consider age, how well ovaries are doing, and embryo quality. This helps us guess the chances of success and decide on embryo numbers.
By looking at past results and adjusting plans, we can increase the chances of a successful pregnancy.
The Shared Decision-Making Process
Choosing the right number of embryos for IVF is a team effort. This way, both the doctor’s advice and the patient’s wishes are considered.
Physician Guidance and Recommendations
Doctors are key in helping patients make this choice. They use medical facts, the patient’s history, and the IVF cycle details to guide them.
Our doctors look at many things like the patient’s age, embryo quality, and past IVF results. They give advice that fits the patient’s needs.
Patient Preferences and Values
What the patient wants and values is very important. Everyone’s situation and goals are different.
Things like wanting twins, worries about pregnancy risks, and personal beliefs about embryo transfer play a big role in the decision.
Informed Consent Requirements
Getting informed consent is a big part of the decision-making process. Patients need to know the risks and benefits of each option.
We make sure patients understand the possible outcomes of transferring one or more embryos. This helps them make a well-informed choice.
Exceptions to Standard Guidelines
Even with guidelines, there are times when they don’t apply. This might be because of past IVF failures or certain health issues.
Our team works with patients to find out if they need a special plan. They help create a treatment plan that fits their unique situation.
| Factors Influencing Embryo Transfer Decisions | Considerations | Impact on Decision |
|---|---|---|
| Patient Age | Embryo quality and quantity | Significant impact on success rates |
| Previous IVF Outcomes | Success or failure of previous cycles | Influences the number of embryos to transfer |
| Embryo Quality | Grading and genetic testing results | Affects the likelihood of successful implantation |
Financial and Insurance Considerations
Knowing the financial side of IVF is key for those starting this journey. IVF can cost a lot, and planning your finances is important. This helps manage the costs of embryo transfer strategies.
Cost Implications of Transfer Strategies
Choosing how many embryos to transfer affects the cost. Single embryo transfers (SET) might lower the risk of having twins or more. This could save money by avoiding extra medical care for multiple births.
Cost Comparison of Different Transfer Strategies:
| Transfer Strategy | Average Cost per Cycle | Risk of Multiple Pregnancy |
|---|---|---|
| Single Embryo Transfer (SET) | $15,000 – $20,000 | Low |
| Double Embryo Transfer (DET) | $15,000 – $20,000 | Higher |
Insurance Coverage Variations
IVF insurance coverage varies a lot. Some plans help pay for IVF, while others don’t cover it at all.
“Insurance coverage for IVF can significantly impact a patient’s financial burden. Understanding the specifics of your coverage is critical.” – IVF Specialist
State Mandates and Their Impact
In the U.S., some states require insurance to cover IVF. These laws can make IVF more affordable and accessible for patients.
Long-term Cost Considerations
Think about the long-term costs of raising a child, whether it’s one or more. The financial impact goes beyond the initial IVF costs.
- Initial treatment costs
- Costs of pregnancy and delivery
- Long-term costs of raising a child
Understanding these financial aspects helps patients make better choices about their IVF treatment. This includes deciding how many embryos to transfer.
Conclusion
Choosing the right number of embryos for IVF is a tough decision. It depends on many things like age, how good the embryos are, and past IVF results. We’ve looked at the ASRM guidelines and how they help make this choice. We also talked about how treating each patient as an individual is key to success in IVF.
The American Society for Reproductive Medicine (ASRM) guidelines are very important. They help doctors and patients make the best choices for IVF. These guidelines take into account things like how old the patient is and the quality of the embryos. This way, they try to avoid too many babies while making sure the IVF cycle works.
To wrap it up, the number of embryos in IVF should be based on solid advice and fit each patient’s needs. By treating each person uniquely, we can make IVF better. This approach helps more people succeed and lowers the risks of having too many babies, making IVF more successful overall.
FAQ
What are the ASRM guidelines for multiple embryo transfer?
The American Society for Reproductive Medicine (ASRM) has rules for how many embryos to transfer during IVF. These rules consider things like how old the patient is, the quality of the embryos, and past IVF results.
How many embryos should be transferred during IVF?
The right number of embryos to transfer depends on many things. This includes the patient’s age, the quality of the embryos, and past IVF results. ASRM guidelines help figure this out.
What is elective single embryo transfer (eSET), and who is it suitable for?
Elective single embryo transfer (eSET) means transferring just one embryo. It’s often suggested for people with high-quality embryos, like those under 35. This helps avoid the risks of multiple pregnancies.
What are the benefits and risks of double embryo transfer?
Double embryo transfer might increase the chance of a successful IVF cycle. But, it also raises the risk of twin pregnancies. These pregnancies can be risky for both the mother and the babies.
How does age influence the decision on the number of embryos to transfer?
Age is very important when deciding how many embryos to transfer. ASRM guidelines suggest being more careful with younger patients. For older patients, the guidelines are more open.
What is the role of embryo grading in IVF?
Embryo grading helps evaluate embryo quality. It helps decide how many embryos to transfer and predicts the success of the IVF cycle.
How does preimplantation genetic testing for aneuploidy (PGT-A) affect the number of embryos transferred?
PGT-A testing finds embryos with the right number of chromosomes. This allows for transferring just one healthy embryo. It can improve success rates and lower the risk of multiple pregnancies.
How do previous IVF cycle outcomes influence subsequent embryo transfer decisions?
Past IVF results are important when deciding on future embryo transfers. They help tailor the approach to the individual’s needs.
What is the importance of shared decision-making in determining the number of embryos to transfer?
It’s key for doctors and patients to make decisions together. This ensures that medical advice and patient wishes are balanced. It helps in making informed choices.
How do financial and insurance considerations impact embryo transfer decisions?
Money and insurance can affect decisions on embryo transfers. Some people might choose to transfer more embryos to increase their chances of success, given the cost and coverage limits.
What are the ASRM guidelines for embryo transfer in different age groups?
ASRM has age-specific guidelines for embryo transfers. These guidelines reflect the balance between success rates and the risks of multiple pregnancies at different ages.
References
Government Health Resource. IVF Embryo Transfer Number: ASRM Guidelines and Singleton Outcomes. Retrieved from https://www.asrm.org/practice-guidance/practice-committee-documents/guidance-on-the-limits-to-the-number-of-embryos-to-transfer-a—committee-opinion-2021/


































