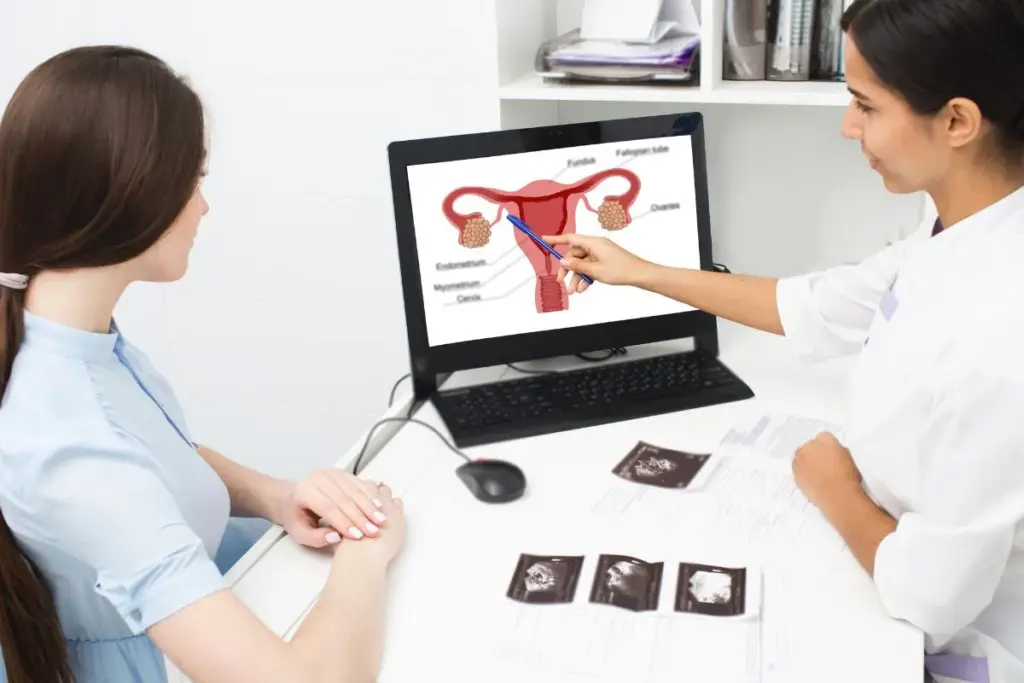
Finding this common hormonal disorder is vital for your long-term wellness and peace of mind. Many women around the world face these complex health challenges without clear answers. Our medical team provides a gentle, supportive place for helping you navigate your clinical assessment.
Finding the root cause of your symptoms involves a pcos diagnosis test and a review of your history. We also use specialized tests for polycystic ovarian syndrome such as blood panels to ensure accuracy. This thorough process helps us create a care plan that fits your specific health goals and concerns.
Understanding how this condition is detected empowers you in taking charge of your health today. Early recognition is a key step in preventing future issues with metabolism or fertility. We provide guidance through every medical step with expertise and sincere care.
Key Takeaways
- This condition affects roughly 10-13% of women in their reproductive years worldwide.
- Diagnosis requires a combination of medical history, physical exams, and lab work.
- There is no single test to confirm the syndrome immediately.
- Up to 70% of women with these symptoms remain undiagnosed globally.
- Testing focuses on identifying irregular periods, high androgen levels, and ovarian cysts.
- Early detection is key for managing long-term metabolic and heart health.
Recognizing When to Seek PCOS Testing

Knowing when to get tested for PCOS is a big step in managing the condition. PCOS, or Polycystic Ovary Syndrome, is a hormonal disorder that affects women of childbearing age. Its symptoms can vary a lot among those who have it.
Menstrual Cycle Irregularities as Warning Signs
Irregular menstrual cycles are a key sign that might lead a woman to get tested for PCOS. This can show up as oligomenorrhea, which means having infrequent or light periods, or amenorrhea, which is when you don’t get your period at all. These signs often point to hormonal imbalances typical of PCOS.
If you’re having trouble with your menstrual cycle, it’s a good idea to talk to a doctor. They might ask you to keep track of your cycles, discuss your health history, and possibly run tests to find out what’s going on.
Physical Symptoms of Hormonal Imbalance
Other signs can also hint at hormonal imbalances linked to PCOS. These include hirsutism, or too much hair on your face and body, acne, and male-pattern hair loss. You might also notice weight gain or find it hard to lose weight if you have PCOS.
| Symptom | Description | Potential Implication |
| Irregular Menstrual Cycles | Infrequent or absent menstruation | Hormonal imbalance |
| Hirsutism | Excessive hair growth on face and body | Androgen excess |
| Acne | Skin condition causing pimples and inflammation | Hormonal imbalance |
| Male-pattern Hair Loss | Hair thinning or loss, particular on the scalp | Androgen excess |
| Weight Gain | Difficulty losing weight or unexplained weight gain | Metabolic issues associated with PCOS |
Knowing about these symptoms and what they might mean can help women know when to see a doctor for PCOS. Catching it early and getting the right treatment is key to managing it well and keeping your health in check.
Which Doctors Diagnose PCOS
Doctors from different fields can diagnose PCOS, based on the patient’s symptoms and needs. We’ll look at who can diagnose PCOS, helping you know who to see for a correct diagnosis.
The Role of Gynecologists in PCOS Diagnosis
Gynecologists are often the first doctors women see for PCOS symptoms like irregular periods or trouble getting pregnant. They have the knowledge to diagnose PCOS because of their focus on women’s reproductive health. A gynecologist can do the needed exams, take a detailed medical history, and order tests to see if PCOS is the cause.
Gynecologists are key in spotting and managing PCOS early. They can help with symptoms, getting periods regular, and fertility issues. For many, a gynecologist is the best doctor to diagnose and treat PCOS.
When to Consult an Endocrinologist
Seeing an endocrinologist might be a good idea if there are big metabolic or hormonal issues. Endocrinologists focus on hormone-related conditions and can give deep insights into PCOS’s hormonal imbalances. They can also help with symptoms like excess hair growth or insulin resistance, common in PCOS.
An endocrinologist’s expertise is very helpful for PCOS patients with complex hormonal or metabolic problems. They work with patients to create a treatment plan that meets their specific needs.
Choosing between a gynecologist and an endocrinologist depends on your symptoms and health goals. Both can diagnose PCOS and provide care, often working together for the best treatment.
How to Diagnose PCOS Using the Rotterdam Criteria
Diagnosing Polycystic Ovary Syndrome (PCOS) uses the Rotterdam Criteria. This method is widely accepted for diagnosing PCOS. It helps doctors identify the condition accurately.
Understanding the Two-Out-of-Three Diagnostic Rule
The Rotterdam Criteria say at least two of three key features must be present for a PCOS diagnosis. These features are:
- Irregular or absent menstruation
- Clinical or biochemical evidence of androgen excess
- Polycystic ovarian morphology on ultrasound
Meeting any two of these criteria is enough for a diagnosis. This makes the Rotterdam Criteria a flexible yet effective tool for diagnosing PCOS.
Criterion One: Irregular or Absent Menstruation
Irregular or absent menstruation is a key sign of PCOS. It can show up as infrequent or no menstruation at all. This often points to ovulation problems, a common feature of PCOS.
Criterion Two: Clinical or Biochemical Androgen Excess
Androgen excess is another important criterion. You might see hirsutism (excessive hair growth in a male pattern), acne, or male-pattern baldness. High levels of androgens in the blood also indicate this. These signs show hormonal imbalance, a key part of PCOS.
Criterion Three: Polycystic Ovarian Morphology
The third criterion is the presence of polycystic ovarian morphology on ultrasound. This means having multiple cysts on the ovaries, usually 12 or more in one ovary, or an ovarian volume over 10 mL. This is a big sign of PCOS, but it’s not the only sign.
Using the Rotterdam Criteria, doctors can accurately diagnose PCOS. This helps them create the right treatment plans. The criteria’s flexibility means more women can get the care they need, even if they don’t show all the classic symptoms.
Specific Medical Tests Used to Detect PCOS
PCOS diagnosis relies on several medical tests. These tests check hormone levels and look at the ovaries. They are key to confirming the diagnosis and understanding how severe it is.
Comprehensive Blood Tests for Hormone Levels
We use blood tests to check hormone levels, like androgens. These tests help spot hormonal imbalances typical of PCOS.
Blood tests measure:
- Androgens: High androgens can cause acne and extra hair growth.
- Luteinizing hormone (LH) and follicle-stimulating hormone (FSH): The LH to FSH ratio can change in PCOS.
- Thyroid hormones: To check for thyroid issues that might cause similar symptoms.
- Fasting glucose and insulin levels: To see if there’s insulin resistance.
| Hormone | Normal Range | PCOS Indication |
| Testosterone | 0.1-0.5 ng/mL | Elevated levels |
| LH/FSH Ratio | <1 | Ratio >2 |
| Fasting Insulin | <20 μU/mL | Elevated levels indicating insulin resistance |
Transvaginal Ultrasound Examination Procedure
A transvaginal ultrasound is a key tool for diagnosing PCOS. It lets doctors check the ovaries’ shape.
During the ultrasound, a special probe takes pictures of the ovaries. This helps spot multiple cysts, a common sign of PCOS.
- Polycystic ovarian morphology: Seeing 20 or more follicles in each ovary.
- Ovarian volume: Large ovaries are often linked to PCOS.
These tests together give a full picture of PCOS. This helps doctors create a good treatment plan.
Conclusion
Diagnosing PCOS is a detailed process. It includes looking at your medical history and doing specific tests. These tests are blood tests and ultrasound.
Healthcare providers use these steps to find out if you have PCOS. They look at your hormone levels and your ovaries. Knowing how to diagnose PCOS is key to treating it well.
Doctors use their knowledge and these tests to diagnose PCOS. This helps them create a treatment plan just for you. Tests for PCOS are important for finding the right care.
FAQ
Can you test for PCOS with a single blood draw?
No, there’s no single blood test for PCOS. We use several blood tests to check hormone levels, along with your health history and ultrasound, for a diagnosis.
How do they test for polycystic ovary syndrome in a clinical setting?
We follow a multi-step process. First, we review your menstrual history and symptoms. Then, we do blood work for hormone levels. Lastly, we might do a pelvic ultrasound to check your ovaries.
Who diagnose PCOS most frequently?
Gynecologists or reproductive endocrinologists usually diagnose PCOS. While a general practitioner might suspect it, these specialists have the tools and knowledge to confirm it.
How do I find out if I have PCOS if my periods are regular?
Even with regular periods, you can be tested. The Rotterdam Criteria say you can be diagnosed with PCOS if you have high androgens and polycystic ovaries, even without irregular periods.
Does PCOS show up on ultrasound for every patient?
Not always. While many have the “polycystic” look on ultrasound, others meet criteria through other signs. The ultrasound is helpful but not required for everyone.
How do they test for PCOS in terms of specific hormones?
We mainly look at “male-pattern” hormones like testosterone and DHEA-S. We also check the LH to FSH ratio, as imbalances are common.
Can you be tested for polycystic ovarian syndrome if you are on birth control?
Testing on birth control can be tricky because it affects hormone levels. For a formal diagnosis, we might suggest stopping the medication briefly, under medical supervision, to get accurate results.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/19969033/
































