
Posterior subcapsular cataracts (PSC) are a common issue for millions worldwide. Early recognition and management are key to avoid vision problems.
A PSC cataract has a cloudy patch at the back of the lens. This patch blocks light, causing blurry vision, even if it’s small.
Knowing the risk factors helps doctors prevent and treat PSC. At Liv Hospital, experts in ophthalmology work together with patients. They aim to provide the best care.
Key Takeaways
- PSC cataracts significantly impact vision and quality of life.
- Early detection is critical for effective management.
- Metabolic factors play a big role in PSC development.
- Preventive strategies and surgical options are available.
- Liv Hospital offers advanced ophthalmology care.
Understanding Posterior Subcapsular Cataract Characteristics
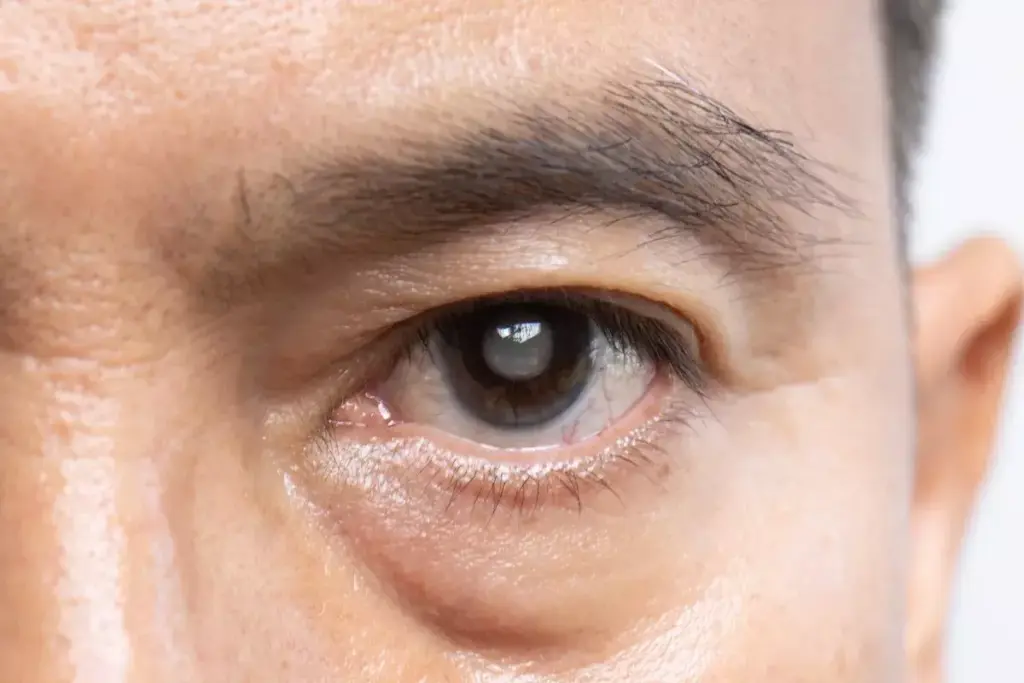
The posterior subcapsular cataract is a unique type of cataract. It affects the back of the lens in the eye. This is different from other cataracts like nuclear or cortical ones.
Definition and Unique Features
Posterior subcapsular cataracts are found at the back of the lens. They can cause big problems with vision. PSC affects the posterior subcapsular region, causing light scattering and glare. This is worse under bright lights or at night, like when driving.
Studies show that PSC is linked to metabolic issues. Things like high triglycerides, high blood sugar, and obesity can lead to PSC early on.
Common Symptoms and Visual Impact
People with PSC often see glare and feel light sensitivity. They also struggle with reading or doing close work. These issues can really affect daily life.
- Glare and light sensitivity
- Difficulty with reading or close work
- Vision disturbances at night or in bright light
Prevalence Statistics and Demographics
Knowing who is at risk for PSC is key. Some metabolic conditions and demographics raise the risk of getting PSC.
| Demographic Factor | Prevalence of PSC |
| Diabetes | Higher prevalence |
| Obesity | Increased risk |
| Hyperglycemia | Associated with PSC development |
Understanding PSC better helps us see why it needs special care. This way, we can manage it more effectively.
Identifying Risk Factors and Prevention Strategies
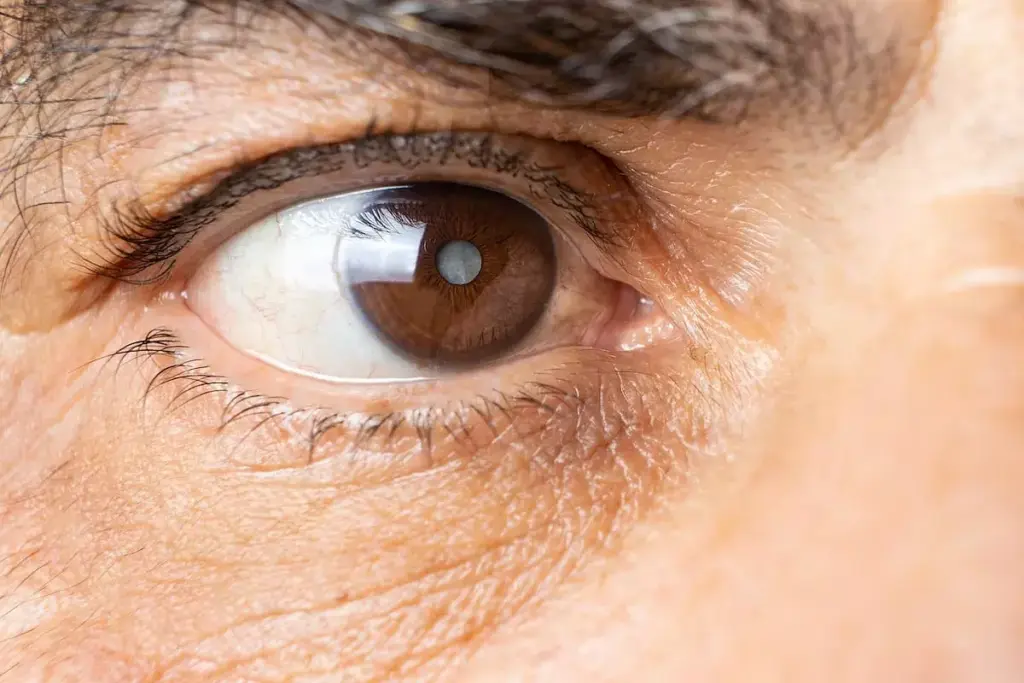
Posterior subcapsular cataracts can be caused by several factors, including metabolic conditions and certain medications. Knowing these factors helps in finding ways to prevent them.
Metabolic Contributors
Conditions like obesity and high blood sugar can lead to posterior subcapsular cataracts. Obesity is linked to many diseases and increases cataract risk. High blood sugar, common in diabetes, can also cause eye lens changes, speeding up cataract growth.
Diabetes Management and PSC Risk Reduction
Diabetes is a big risk factor for posterior subcapsular cataracts. People with diabetes are 6.6 times more likely to get PSC than those without. Keeping blood sugar in check is key to lowering PSC risk. This involves healthy living, regular checks, and managing diabetes well.
| Diabetes Management Strategy | Impact on PSC Risk |
| Blood Glucose Monitoring | Helps in maintaining optimal glucose levels, reducing PSC risk |
| Lifestyle Modifications | Diet and exercise can improve insulin sensitivity and reduce PSC risk |
| Medication Adherence | Ensures consistent control of diabetes, lowering PSC risk |
Steroid Use Considerations
Long-term use of steroids can cause posterior subcapsular cataracts. People on steroids for a long time should get regular eye checks. Looking for other treatments can help avoid this risk.
Blood Pressure Control
Keeping blood pressure in check is also important. High blood pressure can harm eye blood vessels, leading to cataracts. Lowering blood pressure through diet and exercise helps eye health.
For more on cataracts, their causes, and how to prevent them, check out our detailed article on the subject.
Treatment Options for Posterior Subcapsular Cataracts
Posterior subcapsular cataracts are common and can affect your life quality. It’s important to find the right treatment early on.
Early-Stage Management Approaches
In the early stages, treatments aim to ease symptoms and slow the cataract’s growth. You might need new glasses or anti-glare glasses to help with light sensitivity. It’s also key to manage conditions like diabetes, as high blood sugar can make cataracts worse.
Regular check-ups with an eye doctor are vital. They help track the cataract’s growth and adjust treatment plans as needed.
Surgical Intervention Timing
If your vision is severely affected, surgery is often the best option. The decision to have surgery depends on how much your daily life is impacted. Surgery removes the cloudy lens and replaces it with a clear one, improving your vision.
Patients usually see a big improvement in their vision after surgery, thanks to the new lens.
Modern Surgical Techniques
Today’s cataract surgery is more advanced, with quicker recovery times and better results. Phacoemulsification breaks up the cataract with sound waves and removes it through a small cut. This method heals fast and lowers the chance of problems.
Laser-assisted cataract surgery uses a laser to make precise cuts and break up the cataract. This can lead to more accurate surgery.
Post-Surgical Care Protocol
After surgery, following a detailed care plan is essential for healing. This includes using eye drops to prevent infection and attending follow-up visits. You’ll also start doing normal activities again slowly.
It’s important to avoid heavy lifting, bending, or rubbing your eyes during the healing time. By doing so, you can reduce the risk of complications and get the best vision possible.
Conclusion
It’s key to know about posterior subcapsular cataract to manage it well. Spotting symptoms and risk factors early helps keep your vision sharp.
Acting fast on PSC cataract can make a big difference. We stress the need for thorough eye care and support for those seeking medical help abroad.
Our team is dedicated to top-notch healthcare for international patients. We offer timely care and tailor our approach to each patient. This way, we help manage posterior subcapsular cataracts and keep eyes healthy.
With the right treatment, subcapsular posterior cataracts can be tackled. This lets people see clearly again and live better lives.
FAQ
What is a posterior subcapsular cataract?
A posterior subcapsular cataract (PSC) is a type of cataract. It affects the back of the lens in the eye. This causes vision problems.
How does PSC affect vision?
PSC can cause glare and halos. It also makes night vision hard. Sometimes, it leads to blurred or double vision.
Who is most at risk for developing PSC?
People with diabetes and those taking steroids are at higher risk. Also, those with a family history of cataracts are more likely to get PSC.
Can managing diabetes help prevent PSC?
Yes, managing diabetes can lower the risk of PSC. This includes lifestyle changes and medication.
How does steroid use impact PSC risk?
Long-term steroid use increases PSC risk. It’s important to talk to a healthcare provider about the risks and benefits.
What are the treatment options for PSC?
Treatment options include early management, surgery, and post-surgical care. These help manage PSC symptoms.
When is surgical intervention necessary for PSC?
Surgery is needed when PSC affects daily activities. This includes driving or reading. It’s also necessary when other treatments fail.
What are the benefits of modern surgical techniques for PSC?
Modern techniques, like phacoemulsification, offer faster recovery. They also reduce complications and improve outcomes.
How common are posterior subcapsular cataracts?
Posterior subcapsular cataracts are common, mainly in older adults. They are also common in people with certain medical conditions.
Can anterior subcapsular cataracts occur?
Yes, anterior subcapsular cataracts can happen. They are less common than posterior subcapsular cataracts.
What is the difference between posterior subcapsular and posterior capsular cataract?
The terms are often used the same way. But, posterior subcapsular cataract refers to clouding in the posterior subcapsular region of the lens.
How can I reduce my risk of developing PSC?
A healthy lifestyle and managing chronic conditions help. Regular eye exams also reduce PSC risk.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/9627663/




































