
Keratoconus is a disease that makes the cornea thin and bulge. It has been hard for both patients and doctors to treat. But, Intacs corneal implants offer a new hope. They are a small, non-invasive way to fix vision problems.
Doctors put small, crescent-shaped devices in the cornea. This reshapes the eye’s front surface. It might even stop the need for corneal transplant surgery. This method is backed by many eye care experts who look for proven treatments.
Key Takeaways
- Intacs corneal implants are a minimally invasive treatment for keratoconus.
- These implants help reshape the cornea to improve vision.
- The procedure is recognized for potentially delaying the need for a corneal transplant.
- Intacs are made of polymethylmethacrylate (PMMA) and are surgically inserted.
- The FDA granted Intacs a Humanitarian Device Exemption in 2004 for keratoconus treatment.
Understanding Intacs Corneal Implants for Keratoconus
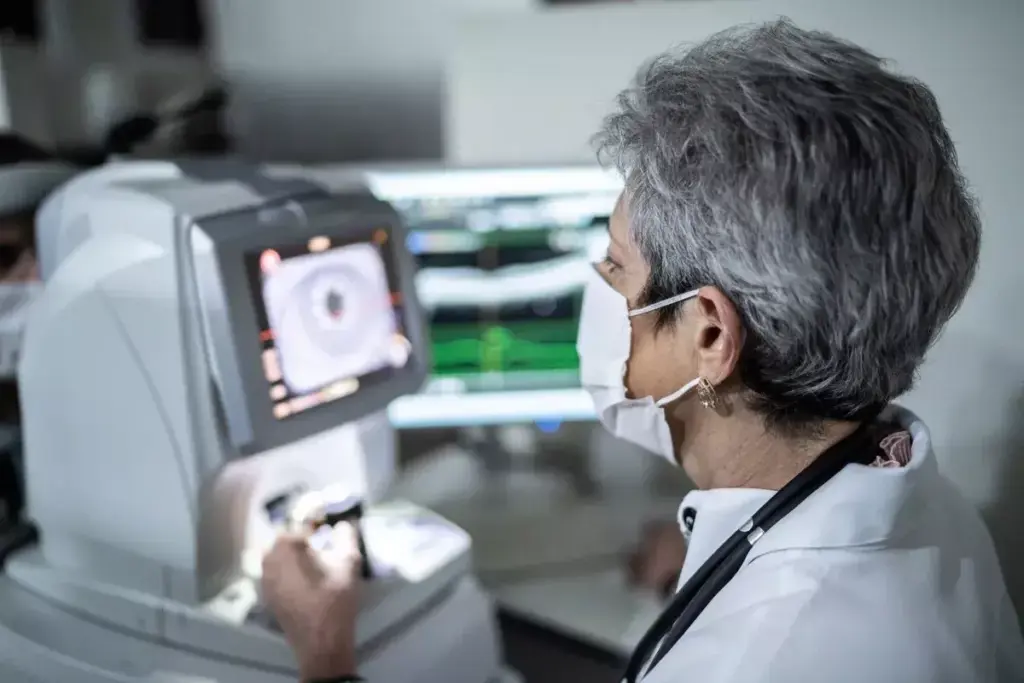
Intacs corneal implants are a new hope for keratoconus patients worldwide. They are a key treatment for this eye condition. Let’s explore how Intacs work to help those with keratoconus.
What Are Intacs Corneal Implants?
Intacs are thin, clear half-rings made of a safe material called PMMA. They are placed in the cornea to support it and make its shape more even. This helps reduce the distortions from keratoconus and improves vision.
Key Features of Intacs Corneal Implants:
- Made from biocompatible PMMA material
- Available in various sizes to fit different corneas
- Designed to reshape the cornea and enhance vision
How Intacs Work to Treat Keratoconus
Intacs flatten the steep part of the cornea, reducing vision distortions. They are inserted into the cornea through surgery. This reshapes the cornea, making it more regular. It’s a minimally invasive surgery for those with keratoconus looking to improve their vision.
Studies show Intacs can greatly improve vision and reduce corneal steepness in keratoconus patients.
| Benefits of Intacs | Description |
| Minimally Invasive | The Intacs procedure is considered minimally invasive, reducing recovery time. |
| Reversible | Intacs can be removed if necessary, making the treatment reversible. |
| Improved Vision | Intacs can significantly improve visual acuity by reshaping the cornea. |
The Intacs Corneal Implants Procedure
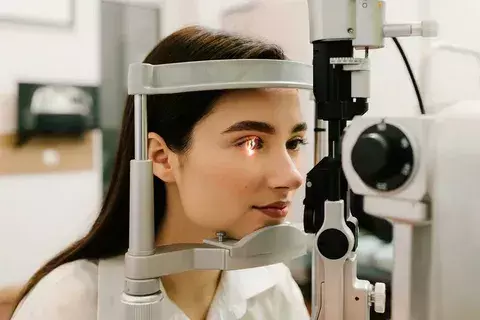
Intacs corneal implants are a big step forward in treating keratoconus, a disease that can make vision worse. The surgery puts Intacs in the cornea to change its shape and help eyes see better.
Pre-Surgery Evaluation and Candidacy
Before the Intacs surgery, patients get checked to see if they can have it. Doctors look at how bad the keratoconus is, how thick the cornea is, and the eye’s health. Our experienced corneal surgeons use special tools to check each patient and plan the best treatment.
They look at a few important things:
- Corneal topography to map the cornea’s surface
- Pachymetry to measure corneal thickness
- Refraction and visual acuity tests to assess the impact of keratoconus on vision
Step-by-Step Surgical Process
On surgery day, the procedure is done under local anesthesia to keep patients comfortable. The surgery has a few key steps:
- Creating a small tunnel within the corneal stroma using a femtosecond laser
- Inserting the Intacs implants into the tunnel
- Adjusting the position of the Intacs to achieve optimal corneal reshaping
Anesthesia and Duration
The surgery is quick, taking about 15-20 minutes per eye. Local anesthesia makes sure patients don’t feel pain. Our skilled surgeons work hard to make the process easy, and patients can go home the same day.
After the surgery, patients must follow a care plan to get the best results. They’ll see our team for follow-ups to check on healing and answer any questions.
Benefits and Effectiveness of Intacs for Keratoconus
Intacs corneal implants have changed how we treat keratoconus. They offer a good alternative to corneal transplants. Studies show that Intacs can make vision better and lessen keratoconus symptoms.
Clinical Research and Success Rates
Many studies prove Intacs work well for keratoconus. For example, a study with 58 patients showed big improvements in vision. Their uncorrected vision went from worse than 20/200 to better than 20/60 after getting Intacs.
Key findings from clinical research include:
- Improved uncorrected visual acuity
- Reduced need for corneal transplants
- Minimally invasive procedure with quick recovery
| Treatment Option | Reversibility | Complication Rate | Visual Acuity Improvement |
| Intacs | Yes | Low | Significant |
| ICL | No | Moderate | Significant |
| Corneal Transplant | No | High | Variable |
Advantages Over Other Treatment Options
Intacs have many benefits over other treatments for keratoconus. They are reversible, unlike ICL, which makes them more flexible. Also, Intacs have fewer complications than more invasive surgeries like corneal transplants.
When looking at treatments for keratoconus, it’s key to consider the pros and cons. Intacs stand out because they are effective, can be reversed, and have a low risk of problems.
Recovery and Aftercare Following Intacs Surgery
The journey to full vision recovery after Intacs corneal implants involves careful post-operative care. Ensuring a smooth and effective recovery is key for the best results.
Immediate Post-Operative Care
After Intacs surgery, patients need to use antibiotic and anti-inflammatory eye drops. These drops help prevent infection and reduce inflammation. They are vital for the cornea to heal properly.
Key aspects of immediate post-operative care include:
- Using prescribed eye drops as directed
- Avoiding rubbing the eyes
- Attending follow-up appointments
We also recommend avoiding strenuous activities and exposure to dust or chemicals. These can irritate the eyes during the initial healing period.
Long-Term Follow-Up
Long-term follow-up care is essential to monitor the healing process. Regular check-ups with an eye care professional help detect issues early. This includes complications like segment migration or corneal neovascularization.
| Follow-Up Care | Description | Frequency |
| Initial Follow-Up | Check for immediate post-surgery complications | 1-2 days post-surgery |
| Short-Term Follow-Up | Monitor healing progress | 1 week, 1 month post-surgery |
| Long-Term Follow-Up | Assess long-term outcomes and manage complications | 3 months, 6 months, 1 year post-surgery |
Potential Complications and Management
While Intacs corneal implants are generally safe, complications can occur. These include segment migration, corneal neovascularization, and other rare but significant issues.
Management strategies for these complications:
- Regular monitoring through follow-up appointments
- Adjusting or removing Intacs segments if necessary
- Treating associated conditions such as dry eye or infection
By understanding the recovery process and following post-operative care instructions, patients can minimize complications. This helps achieve the best possible outcomes from their Intacs surgery.
Conclusion
Intacs corneal implants have changed how we treat keratoconus. They offer a safe and effective way to help those with this eye disease. By reshaping the cornea, Intacs improve vision and reduce the need for more serious surgeries.
Intacs are a less invasive option compared to traditional surgeries. Studies show they work well, improving vision and quality of life for patients.
If you’re thinking about Intacs, talk to an experienced eye doctor. They can help decide if Intacs are right for you. Our team is dedicated to top-notch care and support for our patients with keratoconus.
FAQ
What are Intacs corneal implants?
Intacs are small, crescent-shaped devices made of a safe material called PMMA. They are placed in the cornea to reshape it. This helps improve vision in people with keratoconus.
How do Intacs work to treat keratoconus?
Intacs flatten the cone-shaped cornea. This reduces distortions and improves vision. They are a minimally invasive and reversible treatment for keratoconus.
What is the Intacs corneal implant procedure like?
The procedure starts with a detailed pre-surgical check-up. Then, Intacs are inserted into the cornea using a laser. The whole process takes about 15-20 minutes per eye, done under local anesthesia.
Are Intacs corneal implants reversible?
Yes, Intacs can be removed if needed. This makes them a reversible procedure.
What are the benefits of Intacs for keratoconus treatment?
Intacs improve vision and reduce keratoconus symptoms. They are also a low-risk treatment option. Plus, they are minimally invasive.
What is the recovery process like after Intacs surgery?
After surgery, patients need to follow a careful recovery plan. This includes using eye drops and attending follow-up appointments. They should also avoid activities that could harm the cornea.
What are the possible complications of Intacs surgery?
Possible complications include segment migration and corneal neovascularization. But these are rare. Proper care and follow-up can manage these risks.
How effective are Intacs in treating keratoconus?
Intacs are effective in improving vision and reducing keratoconus symptoms. Studies show significant improvements in vision for patients who get Intacs.
Can Intacs be used in conjunction with other treatments for keratoconus?
Yes, Intacs can be used with other treatments like corneal cross-linking. But, the best approach depends on individual needs. It’s best to discuss with an experienced ophthalmologist.
Are Intacs FDA-approved for keratoconus treatment?
Yes, the FDA approved Intacs in 2004 for treating keratoconus. This marked a big step forward in managing the condition.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/15488778/




































