Nearly 1 in 3 adults in the United States has high cholesterol. This is a key part of hyperlipidemia. It’s important to know what is hyperlipidemia. It’s when your blood has too much lipid, raising your heart disease risk. It’s key to manage high cholesterol symptoms to avoid heart problems.
But, the good news is that reversing hyperlipidemia is doable. You can do it through changing your lifestyle and using medical treatments. This gives hope to those dealing with it.
Key Takeaways
- Hyperlipidemia is a condition of elevated lipid levels in the blood.
- It increases the risk of cardiovascular disease.
- Lifestyle changes can help manage hyperlipidemia.
- Medical interventions are available for reversing hyperlipidemia.
- Understanding high cholesterol symptoms is key for management.
What Is Hyperlipidemia?
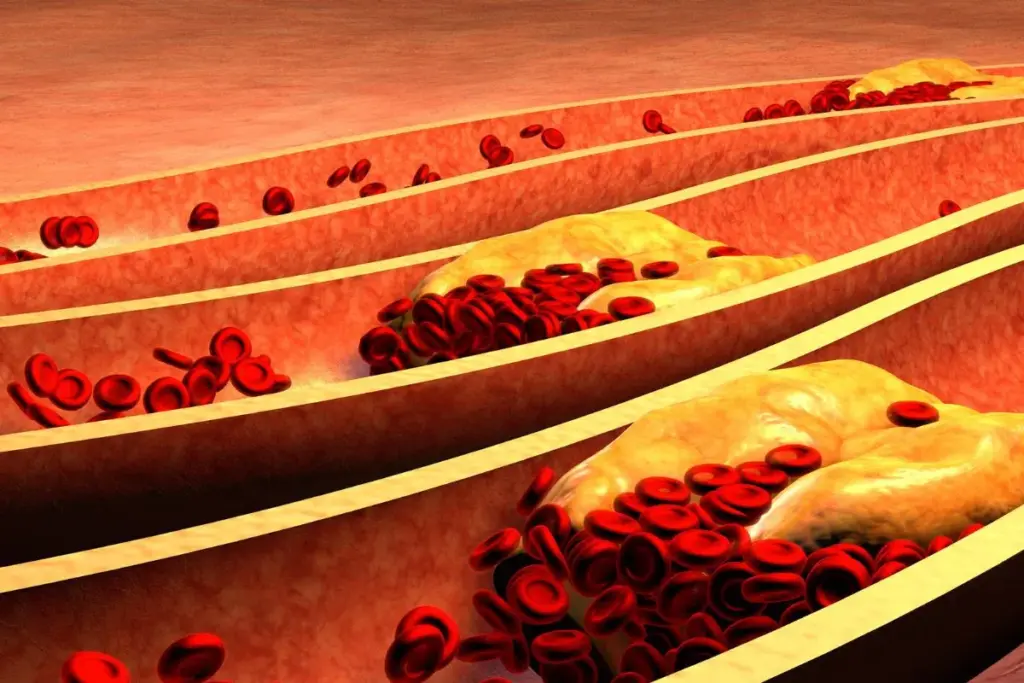
Hyperlipidemia is a condition where the blood has too much cholesterol and triglycerides. It’s a big risk for heart diseases. Heart diseases are a top cause of death in the U.S.
Definition and Medical Terminology
Doctors call hyperlipidemia when there’s too much low-density lipoprotein cholesterol (LDL-C), triglycerides, or both. At the same time, there’s less high-density lipoprotein cholesterol (HDL-C). Some people use “dyslipidemia” instead, but it’s often the same thing.
It’s key to manage hyperlipidemia. This helps lower the risk of heart problems.
Types of Hyperlipidemia
There are two main types of hyperlipidemia. Primary hyperlipidemia is inherited and can be familial hypercholesterolemia or combined hyperlipidemia. Secondary hyperlipidemia is caused by lifestyle, other health issues, or some medicines.
“The identification and treatment of hyperlipidemia are critical for preventing cardiovascular disease and reducing the risk of heart attacks and strokes.”
Prevalence Statistics in the United States
In the U.S., millions of adults have hyperlipidemia. Over 100 million adults have high cholesterol. Many don’t even know they have it.
About 1 in 3 adults in the U.S. has high LDL cholesterol. It gets more common with age. It also affects some ethnic groups more.
The Science of Blood Lipids
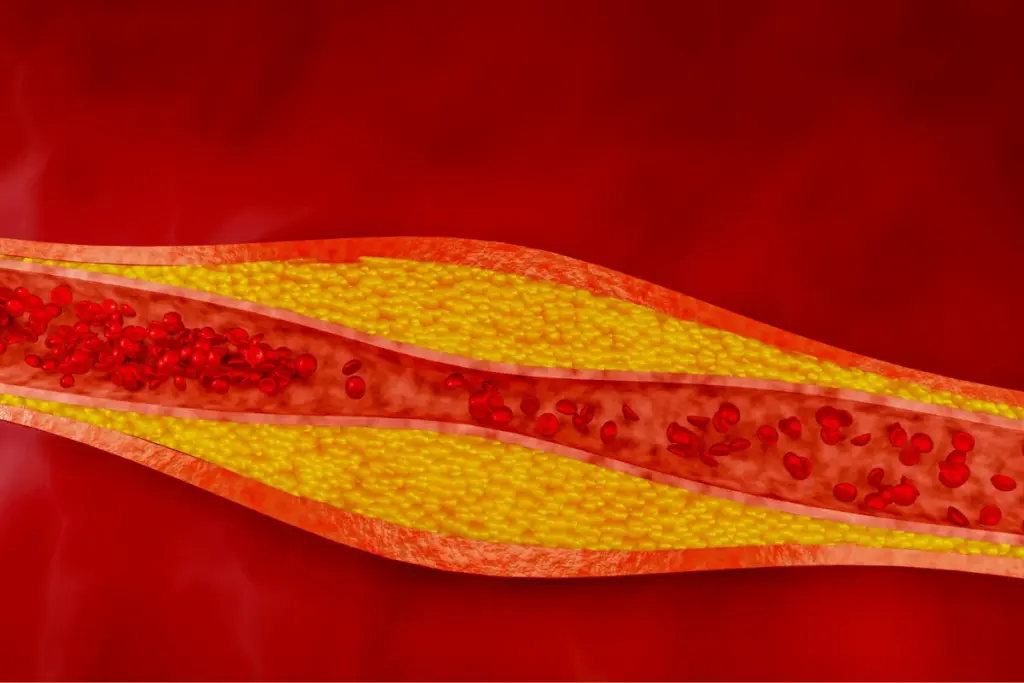
Exploring blood lipids shows how vital it is to keep cholesterol and triglycerides in balance.
Understanding Cholesterol: HDL vs. LDL
Cholesterol is a lipid in our blood, key for our body’s functions. It’s carried by lipoproteins, which mix lipids and proteins. There are two main cholesterol types: HDL (High-Density Lipoprotein) and LDL (Low-Density Lipoprotein).
HDL is good cholesterol. It helps clear out extra cholesterol, lowering heart disease risk. LDL, or bad cholesterol, can cause artery blockages, raising heart disease risk.
Triglycerides and Their Function
Triglycerides are lipids in our blood, acting as energy sources. When we eat more than we need, our body turns the extra into triglycerides. These are stored in fat cells. High triglycerides can up heart disease risk and link to metabolic syndrome.
Normal vs. Abnormal Lipid Levels
Knowing the normal lipid levels is key for spotting and managing high lipids. Here’s a table showing lipid level categories:
|
Lipid Type |
Normal/Desirable Level |
Borderline High |
High |
|---|---|---|---|
|
LDL Cholesterol |
<100 mg/dL |
130-159 mg/dL |
≥160 mg/dL |
|
HDL Cholesterol |
≥60 mg/dL |
<40 mg/dL | |
|
Triglycerides |
<150 mg/dL |
150-199 mg/dL |
≥200 mg/dL |
Keeping lipid levels in the normal range is key to lowering heart disease risk.
Common Causes of Hyperlipidemia
It’s important to know what causes hyperlipidemia to manage it well. This condition means your blood has too much lipid. It comes from a mix of genetics, health issues, and lifestyle choices.
Primary (Genetic) Hyperlipidemia
Primary hyperlipidemia is due to genes that affect lipid levels. Conditions like familial hypercholesterolemia (FH) are passed down. They cause very high LDL cholesterol levels. Some people are more likely to have high lipid levels because of their genes, even if they eat well.
Secondary Causes and Medical Conditions
Secondary hyperlipidemia comes from other health problems or factors. Diabetes, hypothyroidism, and kidney disease can lead to it. Also, some medicines, like steroids and certain blood pressure drugs, can raise lipid levels.
Lifestyle Factors Contributing to High Lipids
Our lifestyle choices greatly affect our lipid levels. Eating too much saturated fats, trans fats, and cholesterol raises LDL cholesterol. Not moving enough, smoking, and drinking too much alcohol also play a part. Eating right, staying active, and keeping a healthy weight can help control lipid levels.
In summary, hyperlipidemia is caused by genetics, health issues, and lifestyle. Knowing these causes helps in finding the right treatment and management.
Recognizing High Cholesterol Symptoms
Hyperlipidemia, or high cholesterol, often doesn’t show symptoms until it’s too late. This makes it hard for people to know they have it until they face a big health problem.
The Challenges of Detection
The way hyperlipidemia grows quietly is a big worry. As a cardiologist notes, “High cholesterol is a silent killer because it doesn’t usually cause symptoms until the disease is advanced.” This shows why knowing your risk and getting checked regularly is key.
“The lack of symptoms in hyperlipidemia makes regular check-ups vital for early detection and management.”
Potential Physical Indicators
Even though hyperlipidemia often doesn’t show symptoms, some rare signs might hint at high cholesterol. These include:
- Xanthomas: fatty deposits under the skin
- Xanthelasma: yellowish patches around the eyes
- Corneal arcus: a white or gray ring around the cornea
These signs aren’t just for hyperlipidemia but can point to lipid disorders too.
When to Seek Medical Attention
If you notice any of these, you should see a doctor right away:
- Chest pain or discomfort
- Shortness of breath
- Pain or weakness in the legs or arms
These signs might mean you have heart disease, a serious risk with untreated high cholesterol. Catching it early and treating it can make a big difference.
Getting regular health checks and screenings is essential for managing hyperlipidemia. If you’re at risk or have high cholesterol, working with your doctor to create a plan can help avoid serious problems.
Diagnosing Hyperlipidemia
To find out if you have hyperlipidemia, doctors use a detailed lipid panel test. This test helps them see your lipid levels and plan the right treatment.
Comprehensive Lipid Panel Testing
A lipid panel test checks your blood for different lipids. It looks at total cholesterol, HDL (good) cholesterol, LDL (bad) cholesterol, and triglycerides. You need to fast for 9-12 hours before the test for the most accurate results.
Lipid Profile Components:
- Total Cholesterol
- HDL (Good) Cholesterol
- LDL (Bad) Cholesterol
- Triglycerides
Understanding Your Lipid Profile Results
It’s important to know what your lipid test results mean. The results show how your lipids compare to healthy levels. This makes it easier to see if you need to make changes.
|
Lipid Component |
Desirable Level |
Borderline |
High Risk |
|---|---|---|---|
|
Total Cholesterol |
< 200 mg/dL |
200-239 mg/dL |
≥ 240 mg/dL |
|
LDL Cholesterol |
< 100 mg/dL |
100-129 mg/dL |
≥ 130 mg/dL |
|
HDL Cholesterol |
≥ 60 mg/dL |
40-59 mg/dL |
< 40 mg/dL |
|
Triglycerides |
< 150 mg/dL |
150-199 mg/dL |
≥ 200 mg/dL |
Frequency of Testing Recommendations
How often you need a lipid test depends on your health risks. Adults with normal levels should get tested every 5 years. Those at higher risk might need more tests.
Talking to your doctor is key to figuring out the right testing schedule for you.
Health Risks of Untreated Hyperlipidemia
Hyperlipidemia can be silent but dangerous if not treated. It’s when your blood has too much lipid. This condition increases the risk of heart diseases.
Cardiovascular Disease and Atherosclerosis
Not treating hyperlipidemia can cause atherosclerosis. This is when plaque builds up in arteries. It can lead to heart attacks and other heart problems.
People with untreated hyperlipidemia face a higher risk of heart disease. High LDL cholesterol can make arteries narrow and stiff.
Stroke and Cerebrovascular Complications
Hyperlipidemia also raises the risk of stroke. A stroke happens when brain blood supply is cut off. High LDL cholesterol can block brain blood vessels, causing ischemic strokes.
Hyperlipidemia can also cause other brain problems. This includes transient ischemic attacks (TIAs) and vascular dementia.
Other Organ System Effects
Hyperlipidemia can harm more than just the heart and brain. It can cause pancreatitis, an inflammation of the pancreas. This is due to high triglycerides.
It also increases the risk of peripheral artery disease. This is when narrowed arteries reduce blood flow to the limbs.
|
Organ System |
Potential Complications |
|---|---|
|
Cardiovascular |
Atherosclerosis, Heart Attack |
|
Cerebrovascular |
Stroke, Transient Ischemic Attack (TIA) |
|
Other |
Pancreatitis, Peripheral Artery Disease |
Knowing these risks shows why managing hyperlipidemia is key. It’s important to make lifestyle changes, take medication, or both. This helps prevent serious health problems.
Is Hyperlipidemia Reversible?
Yes, hyperlipidemia can be reversed with lifestyle changes and medical help. “Reversal” means getting lipid levels back to normal or improving them a lot. This lowers the risk of heart disease.
Defining “Reversal” in Medical Terms
“Reversal” in hyperlipidemia means getting lipid levels back to normal. This can happen through diet, exercise, and sometimes medicine.
Factors Affecting Reversibility
Many things can affect how well you can reverse hyperlipidemia. These include the cause of the condition, other health issues, and how well you respond to treatment. Lifestyle changes can work better than medicine for some people.
Success Rates and Timeframes
How well you can reverse hyperlipidemia varies. You might see big changes in a few months. Here’s a table showing when you might see improvements.
|
Treatment Approach |
Timeframe for Improvement |
|---|---|
|
Dietary Changes |
2-6 months |
|
Increased Physical Activity |
3-6 months |
|
Medication |
1-3 months |
Genetic vs. Lifestyle-Induced Hyperlipidemia
It’s important to know if your hyperlipidemia is genetic or caused by lifestyle. Changing your diet and exercise can help with lifestyle-related cases. But, genetic cases might need more medical help.
Key Considerations:
- Lifestyle changes are key for managing hyperlipidemia.
- Medical treatment might be needed for genetic or severe cases.
- Regular check-ups are important to see if your treatment is working.
Understanding what affects hyperlipidemia reversibility is important. With the right approach, you can improve your lipid levels and lower heart disease risk.
Dietary Approaches to Lower Cholesterol
Eating right can lower cholesterol and boost heart health. Changing your diet is key to managing high cholesterol. Certain foods can greatly affect your cholesterol levels.
Foods That Raise Cholesterol Levels
Knowing which foods raise cholesterol is important. Foods high in saturated fats, trans fats, and cholesterol can increase bad cholesterol. Examples include:
- Red meat and processed meats
- Full-fat dairy products
- Baked goods and fried foods
- Processed snacks
Avoiding or limiting these foods can help keep cholesterol levels healthy.
Cholesterol-Lowering Food Choices
Adding foods that lower cholesterol is beneficial. These include:
- Oatmeal and other soluble fiber-rich foods
- Fatty fish like salmon and mackerel
- Nuts and seeds, such as almonds and flaxseeds
- Fruits and vegetables, high in antioxidants
Plant-based diets are rich in these cholesterol-lowering foods.
The Mediterranean Diet for Lipid Management
The Mediterranean diet is great for managing cholesterol. It focuses on:
- High amounts of fruits, vegetables, and whole grains
- Olive oil as the main fat source
- Moderate amounts of fish, poultry, and dairy
- Low amounts of red meat and processed foods
This diet not only lowers LDL cholesterol but also improves heart health.
Plant Sterols and Stanols
Plant sterols and stanols are found in plants. They help lower LDL cholesterol by reducing cholesterol absorption. Foods fortified with them, like certain margarines and orange juices, are good for cholesterol.
|
Food |
Effect on Cholesterol |
|---|---|
|
Oatmeal |
Lowers LDL |
|
Fatty Fish |
Improves overall lipid profile |
|
Plant Sterols/Stanols |
Reduces cholesterol absorption |
By using these dietary approaches, you can manage cholesterol levels and lower heart disease risk.
How to Reduce Cholesterol in 7 Days
Lowering cholesterol in just 7 days is a big goal. But, some diet and exercise changes can help. These quick steps can start you on the path to better cholesterol levels.
Immediate Dietary Interventions
To quickly lower cholesterol, changing what you eat is key. Eat foods that help lower cholesterol. These include:
- Oatmeal and other soluble fiber-rich foods
- Fatty fish like salmon, rich in omega-3 fatty acids
- Nuts and seeds, such as almonds and flaxseeds
- Fresh fruits and vegetables, high in fiber and antioxidants
- Plant sterols and stanols found in fortified foods
Stay away from foods that can raise cholesterol. Avoid saturated and trans fats in red meat, full-fat dairy, and processed snacks.
Short-Term Exercise Strategies
Exercise is also vital for lowering cholesterol. Regular activity boosts “good” cholesterol. Here are some quick exercise tips:
- Aerobic exercises like brisk walking, cycling, or swimming for at least 150 minutes per week
- High-intensity interval training (HIIT) for improved cardiovascular health
- Resistance training to build muscle and boost metabolism
Even a 7-day program can be beneficial with consistent, moderate exercise.
Realistic Expectations for Quick Results
While diet and exercise can help, be realistic. Big cholesterol drops usually take longer than 7 days. But, starting a healthy diet and exercise plan can show improvements quickly.
Key Takeaways:
- Immediate dietary changes focusing on cholesterol-lowering foods
- Incorporating short-term exercise strategies
- Understanding that significant cholesterol reduction takes time
Exercise Regimens for Improving Lipid Profiles
Exercise plans tailored to your needs can boost cholesterol levels and heart health. Regular activity not only improves lipid profiles but also boosts overall health.
Aerobic Exercise Benefits for Cholesterol
Aerobic exercises like walking, jogging, cycling, and swimming are great for cholesterol. They increase HDL (good) cholesterol and lower LDL (bad) cholesterol.
Aerobic Exercise Benefits:
- Increased HDL cholesterol
- Reduced LDL cholesterol
- Improved cardiovascular health
Resistance Training and Lipid Levels
Resistance training, like weightlifting and bodyweight exercises, also helps improve lipid profiles. It builds muscle, which helps burn calories and improve metabolic health.
Resistance Training Benefits:
- Increased muscle mass
- Enhanced metabolic rate
- Better overall lipid profile management
Creating an Effective Exercise Routine
To make a good exercise plan, think about your health goals, fitness level, and any health issues. A good routine should mix aerobic exercises and resistance training.
|
Exercise Type |
Frequency |
Duration |
|---|---|---|
|
Aerobic Exercise |
3-5 times/week |
30 minutes/session |
|
Resistance Training |
2-3 times/week |
20-30 minutes/session |
Mixing aerobic exercise with resistance training can greatly improve lipid profiles and heart health.
Weight Management and Hyperlipidemia
Managing your weight is key to treating hyperlipidemia. Hyperlipidemia means your blood has too much lipid. It’s a big risk for heart disease. Keeping a healthy weight helps control lipid levels.
The Obesity-Cholesterol Connection
Being obese raises your risk of hyperlipidemia. Obesity and bad lipid levels are linked. Visceral fat, in particular, harms your health by causing insulin resistance and bad lipid levels.
Studies show obese people often have less good cholesterol and more bad cholesterol and triglycerides.
Sustainable Weight Loss Approaches
Keeping weight off is key to better lipid levels. Good weight loss comes from diet, exercise, and lifestyle changes. Eating less saturated fat and more fiber can lower cholesterol.
Regular exercise boosts HDL cholesterol and aids in weight loss.
Here are some tips for lasting weight loss:
- Set achievable goals and track your progress.
- Eat a variety of healthy foods.
- Do regular physical activity, like walking or swimming.
- Stay away from quick fixes and focus on lasting lifestyle changes.
Impact of Weight Loss on Lipid Markers
Weight loss improves lipid markers. Losing 5-10% of your body weight can boost HDL and lower LDL and triglycerides. The table below shows how weight loss can change lipid levels.
|
Lipid Marker |
Change with Weight Loss |
|---|---|
|
LDL Cholesterol |
Decrease |
|
HDL Cholesterol |
Increase |
|
Triglycerides |
Decrease |
In conclusion, managing your weight is vital for hyperlipidemia. Understanding obesity’s link to cholesterol, using lasting weight loss methods, and seeing how weight loss affects lipid levels can help. This way, you can manage your condition and lower heart disease risk.
Medication Options for Treating Hyperlipidemia
There are many medicines to treat high lipid levels. Each one works differently and has its own benefits. These drugs help control high lipids and lower heart disease risk.
Statins: Mechanisms and Effectiveness
Statins are a top choice for treating high lipids. They block a liver enzyme that makes cholesterol. This lowers bad cholesterol and slightly raises good cholesterol.
Studies show statins greatly reduce heart problems and death. Common statins include atorvastatin, simvastatin, and rosuvastatin.
PCSK9 Inhibitors and Newer Medications
PCSK9 inhibitors are a newer type of lipid-lowerer. They target PCSK9, helping the liver remove more bad cholesterol. This lowers bad cholesterol levels.
Alirocumab and evolocumab are examples of PCSK9 inhibitors. They are very effective, mainly for those with high cholesterol or heart risk.
Other Lipid-Lowering Medications
Other drugs help manage high lipids too. These include:
- Bile acid sequestrants, which lower bad cholesterol by binding to bile acids.
- Fibrates, which mainly cut down triglycerides and boost good cholesterol.
- Niacin (nicotinic acid), which improves all lipid levels but is less used due to side effects.
- Ezetimibe, which stops cholesterol absorption in the small intestine.
Medication Side Effects and Management
Lipid-lowerers are mostly safe but can have side effects. Statins often cause muscle pain and liver issues. PCSK9 inhibitors might lead to injection site reactions.
Dealing with side effects might mean changing the dosage or switching meds. Supplements can also help. Regular check-ups with your doctor are key to managing risks and benefits.
Natural Supplements for Cholesterol Management
Natural supplements are gaining attention for managing cholesterol. They should not be a replacement for medical treatment. But, some supplements might help when a healthcare professional guides their use.
Evidence-Based Natural Remedies
Some natural supplements have shown promise in managing cholesterol. These include:
- Plant Sterols and Stanols: Known to help lower LDL cholesterol.
- Berberine: Some studies suggest it may help reduce cholesterol levels.
- Garlic: May have a modest effect on lowering cholesterol.
Fish Oil and Omega-3 Fatty Acids
Fish oil, rich in omega-3 fatty acids, is often considered for its cardiovascular benefits. It mainly affects triglycerides, not LDL cholesterol. Yet, it plays a role in heart health.
Supplement Safety and Doctor Consultation
Before starting any supplements, it’s key to talk to a healthcare provider. Supplements can interact with medications or cause side effects, mainly in large doses.
Key considerations include:
- Potential interactions with other medications.
- The quality and purity of the supplement.
- Monitoring for any adverse effects.
Managing Mixed Hyperlipidemia
Mixed hyperlipidemia is a condition where many lipids are too high. It includes high triglycerides, low HDL cholesterol, and high LDL cholesterol. This makes it hard to manage.
Characteristics of Combined Lipid Disorders
Managing mixed hyperlipidemia is a big challenge. It raises the risk of heart disease because of the many lipid problems. Knowing these issues is key to a good treatment plan.
Because of the many lipid problems, treatment needs to be more detailed. Doctors must focus on each lipid issue separately.
Specialized Treatment Approaches
Dealing with mixed hyperlipidemia requires lifestyle changes and medicines. Lifestyle changes like better diet, more exercise, and losing weight are important. They help improve lipids and lower heart disease risk.
Medicines like statins, fibrates, or combinations are used. The right medicine depends on the lipid levels and the patient’s health.
Monitoring Multiple Lipid Abnormalities
It’s important to check lipid levels often. Blood tests are used to see how different lipids are doing. This helps adjust treatments as needed.
Checking lipid levels regularly shows if treatments are working. It helps make changes to keep lipid levels in check and lower heart disease risk.
Long-Term Management and Monitoring
Managing hyperlipidemia well needs a mix of regular checks and tweaks to treatment plans. This approach is key to keeping lipid levels healthy and avoiding heart problems.
Follow-up Testing Schedules
It’s important to keep an eye on how treatments are working. How often you need tests depends on your health and how serious your hyperlipidemia is.
Recommended Testing Schedule:
|
Patient Category |
Initial Testing Frequency |
Follow-up Testing Frequency |
|---|---|---|
|
Low-risk patients |
Every 5 years |
Every 5 years if normal |
|
High-risk patients |
At diagnosis |
Every 6-12 months |
|
Patients on lipid-lowering therapy |
Before starting therapy |
Every 6-12 weeks until target is reached, then every 6-12 months |
Adjusting Treatment Over Time
As your health changes, so might your treatment. This could mean switching medications, changing doses, or focusing more on lifestyle changes. Regular checks help doctors make the best choices for you.
Things that might lead to changes in treatment include changes in your lipid levels, side effects, or changes in your health or lifestyle.
Lifestyle Maintenance Strategies
Keeping up with healthy habits is vital for managing hyperlipidemia long-term. This means eating right, staying active, keeping a healthy weight, and not smoking.
Lifestyle Tips:
- Eat a diet rich in fruits, vegetables, whole grains, and lean proteins.
- Engage in at least 150 minutes of moderate-intensity aerobic exercise or 75 minutes of vigorous-intensity aerobic exercise per week.
- Maintain a healthy weight through a combination of diet and exercise.
- Avoid smoking and limit exposure to secondhand smoke.
Conclusion
Managing hyperlipidemia is key to avoiding heart problems and boosting health. Knowing the causes, signs, and treatments helps people control their cholesterol. This is a big step towards better health.
Handling hyperlipidemia well means making lifestyle changes, getting medical help, and keeping an eye on your health. Eating right, exercising often, staying at a healthy weight, and following your doctor’s advice are important. These steps help control cholesterol levels.
By following these steps, people can keep their cholesterol in check. This lowers the risk of heart disease and improves life quality. It’s also important to keep checking your health and changing your treatment plan if needed. This ensures the best management of hyperlipidemia and cholesterol control.
FAQ
What is hyperlipidemia?
Hyperlipidemia is when your blood has too much cholesterol and triglycerides. It’s a big risk for heart disease.
What are the symptoms of high cholesterol?
High cholesterol often doesn’t show symptoms. But, it can cause fatty deposits under the skin, called xanthomas.
How is hyperlipidemia diagnosed?
Doctors use a lipid panel test to find out if you have hyperlipidemia. This test checks your HDL, LDL, and triglycerides.
Can hyperlipidemia be reversed?
Yes, you can manage or reverse hyperlipidemia. Making healthy lifestyle choices and taking medicine can help.
What dietary changes can help lower cholesterol?
Eating less saturated and trans fats helps. Also, eat more soluble fiber and foods with omega-3s, like fish.
How can I reduce my cholesterol levels in 7 days?
You can’t drastically lower cholesterol in 7 days. But, eating more soluble fiber and exercising can help a bit.
What is the role of exercise in managing hyperlipidemia?
Exercise, like cardio and strength training, improves your lipid levels. It raises HDL and lowers LDL and triglycerides.
How does weight loss impact lipid markers?
Losing weight improves your lipid levels. It lowers LDL and triglycerides and raises HDL, thanks to diet and exercise.
What medications are used to treat hyperlipidemia?
Statins and PCSK9 inhibitors are used to treat hyperlipidemia. They help by reducing liver cholesterol production or removing LDL from the blood.
Are there any natural supplements that can help manage cholesterol?
Yes, supplements like fish oil and omega-3s, plant sterols, and soluble fiber can help. But, always talk to a doctor before taking them.
How often should I have my lipid levels checked?
Adults should get their lipid levels checked every 5 years. If you have a history of heart disease, you might need to go more often.
What is mixed hyperlipidemia?
Mixed hyperlipidemia has high LDL, low HDL, and high triglycerides. It needs special treatment to manage all these lipid issues.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6322297/


































