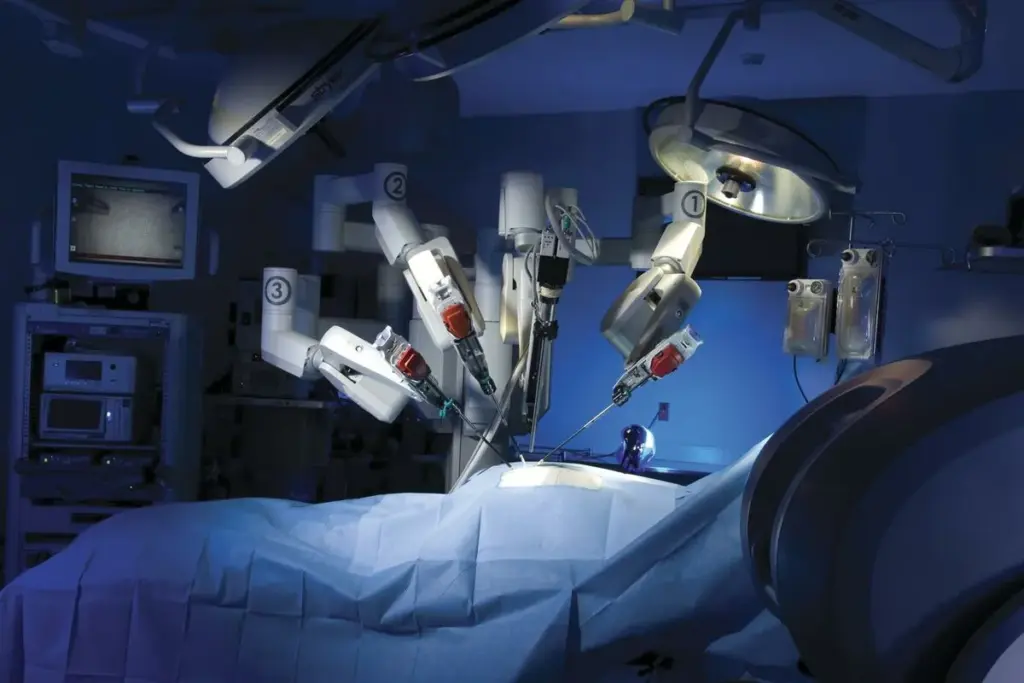
Robotic hysterectomy is a surgery that removes the uterus with great precision. We understand that undergoing such a surgery can be daunting. It’s important to know what to expect during hysterectomy recovery.
During a robotic hysterectomy, surgeons use advanced robotic technology. This method offers several benefits. These include smaller incisions, less blood loss, and shorter hospital stays. Knowing how the uterus is removed can help ease concerns and prepare patients for the procedure.
Key Takeaways
- Robotic hysterectomy is a minimally invasive procedure.
- The surgery involves the use of advanced robotic technology.
- It allows for precise removal of the uterus.
- Benefits include smaller incisions and less blood loss.
- Understanding the procedure can help alleviate patient concerns.
Understanding Hysterectomy: Definition and Medical Necessity

A hysterectomy is a big surgery that removes the uterus. Patients should be well-informed about hysterectomy before making a decision. We’ll look at what hysterectomy is, its types, and why it’s needed.
What is a hysterectomy and why is it performed?
A hysterectomy removes a woman’s uterus. It’s done for many reasons, like uterine cancer or severe bleeding. Doctors usually try other treatments first before suggesting a hysterectomy.
Different types of hysterectomies (total, partial, radical)
There are many types of hysterectomies, each with its own level of surgery:
- Total Hysterectomy: This removes the whole uterus, including the cervix.
- Partial (or Subtotal) Hysterectomy: Only the top part of the uterus is taken out, leaving the cervix.
- Radical Hysterectomy: This is a bigger surgery that takes out the uterus, cervix, and part of the vagina. It’s often for cancer.
Medical conditions requiring surgical removal of the uterus
Many health issues might need a hysterectomy. These include:
- Uterine Fibroids: Big or painful fibroids that cause heavy bleeding.
- Endometriosis: Tissue like the uterus lining grows outside, causing pain.
- Uterine Prolapse: The uterus falls into the vagina.
- Gynecologic Cancer: Cancers of the uterus, cervix, or ovaries might need a hysterectomy.
- Abnormal Uterine Bleeding: Heavy or irregular bleeding that can’t be fixed with other treatments.
Knowing what a hysterectomy is and why it’s done helps patients make better choices. It’s key to understanding treatment options and health decisions.
Evolution of Hysterectomy Techniques
Hysterectomy techniques have changed a lot, moving from old open surgeries to new robotic-assisted ones. This change has greatly improved how patients recover, including hysterectomy recovery time and overall recovery from hysterectomy.
Traditional Open Abdominal Hysterectomy
Long ago, open abdominal hysterectomy was the main way to do this surgery. It needed a big cut in the belly to reach the uterus. This method was good but took longer to heal and hurt more after surgery than newer ways.
Vaginal Hysterectomy Approach
Vaginal hysterectomy is a less invasive option. It removes the uterus through the vagina. This can lead to a shorter hysterectomy recovery time and less visible scars. But, it’s not right for everyone, depending on the uterus’s size and how it moves.
Laparoscopic Techniques
Laparoscopic surgery is a big step forward. It uses small cuts and a camera to guide the surgery. Laparoscopic hysterectomy has less pain after surgery and faster healing.
Introduction of Robotic-Assisted Surgery
The newest way is robotic-assisted surgery, like robotic hysterectomy. It uses a robotic system, like the da Vinci Surgical System, to help the surgeon. Robotic hysterectomy gives better precision, flexibility, and view, leading to better results and recovery from hysterectomy.
The changes in hysterectomy techniques are shown in the table below:
|
Surgical Technique |
Invasiveness |
Recovery Time |
Precision |
|---|---|---|---|
|
Open Abdominal Hysterectomy |
High |
Long |
High |
|
Vaginal Hysterectomy |
Low |
Short |
Moderate |
|
Laparoscopic Hysterectomy |
Moderate |
Moderate |
High |
|
Robotic Hysterectomy |
Low |
Short |
Very High |
The evolution of hysterectomy techniques has greatly improved patient care. Moving to less invasive methods, like robotic hysterectomy, shows the ongoing effort to better surgical results and shorten hysterectomy recovery time.
Robotic Hysterectomy: Advanced Surgical Technology
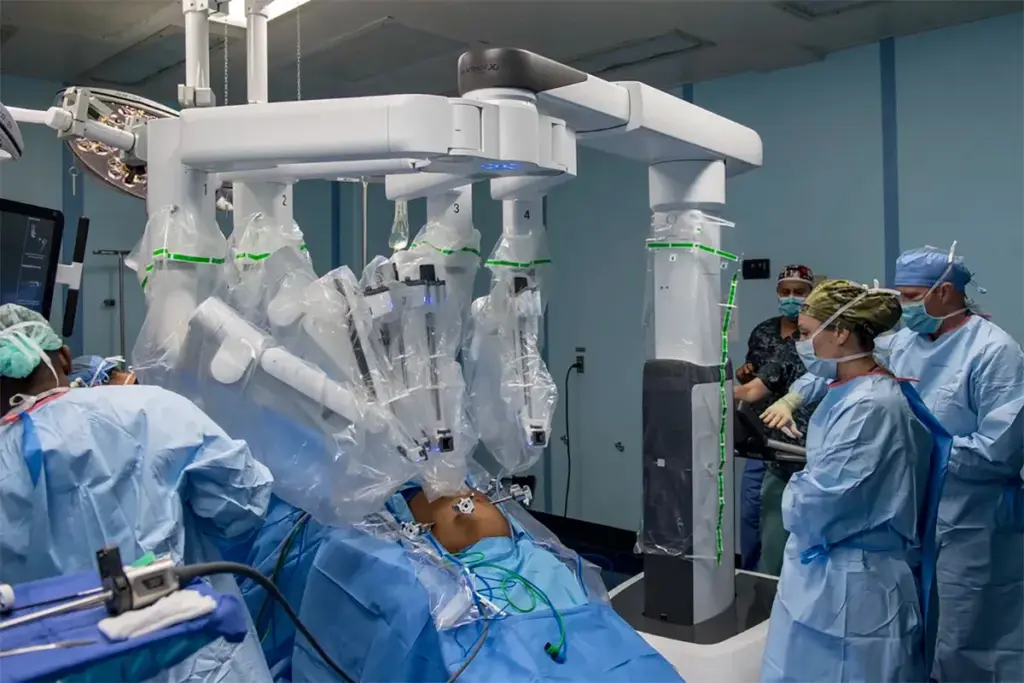
The da Vinci Surgical System has changed gynecological surgery. It lets surgeons do complex surgeries like hysterectomy with better precision. This tech has made recovery times shorter and scars smaller.
The da Vinci Surgical System Explained
The da Vinci Surgical System is a high-tech robot for complex surgeries. It has a surgeon’s console, a cart with robotic arms, and a 3D vision system. The surgeon can see everything clearly and control the instruments precisely.
Advantages Over Traditional Laparoscopic Methods
Robotic hysterectomy beats traditional laparoscopy in many ways. It offers better vision, more control, and less shaking. The 3D view and special instruments make surgeries easier and more accurate. It also means less blood loss, less pain, and faster recovery.
Surgeon Control and Precision During the Procedure
The da Vinci System gives surgeons great control and precision. It’s designed to be comfortable for surgeons, reducing fatigue. The robotic arms move exactly as the surgeon’s hands do, making delicate tasks easier.
Patient Selection Criteria for Robotic Approach
Not every patient is right for robotic hysterectomy. Doctors look at the patient’s health, the surgery’s complexity, and if there are any reasons it can’t be done robotically. Some patients, like those with a lot of previous surgery or certain health issues, need extra checks.
|
Criteria |
Description |
Considerations |
|---|---|---|
|
Overall Health |
Patient’s general medical condition |
Presence of comorbidities, previous surgeries |
|
Surgical Complexity |
Nature of the hysterectomy required |
Total, partial, or radical hysterectomy |
|
Contraindications |
Conditions that may preclude robotic surgery |
Severe adhesions, certain cardiac conditions |
Preparing for Your Robotic Hysterectomy
Getting ready for a robotic hysterectomy is key. It’s important for both your body and mind. Knowing what to expect can make a big difference.
Pre-surgical Consultations and Testing
You’ll have to go to meetings before surgery. Your team will do tests like blood work and imaging. This makes sure you’re ready for the surgery.
Key tests and evaluations may include:
- Complete blood count (CBC) to check for anemia or infection
- Imaging tests like ultrasound or MRI to assess the uterus and surrounding structures
- Cardiac evaluation if you have a history of heart conditions
Medication Adjustments and Dietary Guidelines
Your doctor will tell you about your meds and diet. It’s important to follow these to stay safe during and after surgery.
Medication adjustments may involve:
- Stopping blood thinners a few days before surgery
- Adjusting diabetes medications if applicable
- Avoiding certain herbal supplements that could interfere with anesthesia or bleeding
Dietary guidelines often recommend:
- Avoiding heavy meals the day before surgery
- Staying hydrated by drinking plenty of water
- Possibly following a specific diet a few days before surgery to prepare your bowel
What to Expect on the Day of Surgery
On surgery day, you’ll go to the hospital. You’ll get ready for the surgery, including anesthesia and positioning.
Here’s what you can expect:
- Arrival and registration
- Pre-operative preparations, including changing into a surgical gown
- Administration of anesthesia to ensure comfort during the procedure
- Positioning on the operating table to allow the surgical team to perform the robotic hysterectomy
Mental and Emotional Preparation
Getting ready for surgery is not just physical. Your mind and emotions are just as important. It’s normal to feel nervous or unsure.
“The psychological preparation for surgery is just as important as the physical. Patients who are mentally prepared tend to have a smoother recovery.”
To prepare emotionally:
- Discuss your concerns with your healthcare provider or a counselor
- Practice relaxation techniques such as deep breathing or meditation
- Have a support system in place, including family and friends
By preparing well for your robotic hysterectomy, you can feel less anxious. Always follow your doctor’s advice and ask questions if you need to.
The Robotic Hysterectomy Procedure: Step by Step
The da Vinci Surgical System makes robotic hysterectomies more precise. This technology has changed gynecological surgery. It offers a less invasive option with fewer complications and quicker recovery.
Anesthesia Administration and Positioning
The first step is giving anesthesia. We use general anesthesia for comfort. Then, we position the patient for the best access.
Port Placement and Docking the Robot
We make small incisions for ports. These ports let us use the robotic instruments and camera. After, we dock the da Vinci robot for a stable connection.
Surgeon’s Console Operation
The surgeon controls the instruments from a console. They use a 3D system for clear vision. This setup helps with precise movements and suturing.
Key Surgical Steps in Detaching the Uterus
We start by finding and cutting the uterine arteries. Then, we remove the ligaments. Next, we carefully separate the uterus from other parts. The table below shows these steps:
|
Surgical Step |
Description |
|---|---|
|
Identification of Uterine Arteries |
Careful dissection to locate and ligate the uterine arteries |
|
Ligament Dissection |
Detachment of ligaments supporting the uterus |
|
Uterus Detachment |
Separation of the uterus from surrounding structures |
Knowing these steps helps patients understand the surgery’s complexity. It can ease their concerns and prepare them for the journey ahead.
Uterus Extraction Methods During Robotic Hysterectomy
There are several ways to remove the uterus during robotic hysterectomy. The choice depends on the uterus size, the patient’s health, and the surgeon’s experience. Each method is tailored to meet the patient’s needs.
Vaginal Extraction Technique
Vaginal extraction removes the uterus through the vagina. It’s often chosen because it leaves no scars on the belly. The surgeon must plan carefully to avoid harming nearby tissues.
Morcellation for Larger Uteri
Morcellation is used for bigger uteri. It cuts the uterus into smaller pieces for easier removal. But, it carries a risk of spreading cancer cells, so strict protocols are followed.
Contained Extraction Using Specimen Bags
Specimen bags are used to reduce morcellation risks. The uterus is put in a bag before being cut. This keeps the tissue inside, making the process safer.
Mini-Laparotomy Approach When Necessary
In some cases, a mini-laparotomy is done. This makes a small cut in the belly to remove the uterus. It leaves a small scar but is effective when other methods can’t be used.
|
Extraction Method |
Benefits |
Potential Complications |
|---|---|---|
|
Vaginal Extraction |
No visible abdominal scars, less invasive |
Potential for vaginal trauma, limited by uterus size |
|
Morcellation |
Effective for larger uteri, can be done through robotic ports |
Risk of spreading cancer cells, requires careful protocol |
|
Contained Extraction |
Enhances safety by containing tissue within a bag |
Requires specialized equipment, may add to procedure time |
|
Mini-Laparotomy |
Effective for various uterus sizes, allows direct visualization |
Leaves a small scar, possible infection or complications |
Knowing about uterus extraction methods during robotic hysterectomy is important. Each method has its own benefits and risks. The right choice depends on the patient and the surgeon’s skills.
Hysterectomy Recovery: Timeline and Milestones
Recovering from a robotic hysterectomy is a journey with many stages. It needs careful planning and following postoperative care instructions. Knowing the typical recovery timeline helps patients set realistic goals and spot any issues early.
Hospital Stay Duration After Robotic Procedure
How long you stay in the hospital after a robotic hysterectomy varies. But most patients go home in 1 to 2 days. This short stay is a big plus of robotic surgery, as it causes less damage and quicker healing than traditional surgery.
Factors influencing hospital stay duration include:
- Overall health and presence of any comorbidities
- Specific surgical details and any complications encountered
- Patient’s ability to manage postoperative pain and discomfort
First 48 Hours Post-Surgery
The first 48 hours after surgery are key for recovery. Patients should rest and avoid hard activities. It’s normal to feel some pain, discomfort, and vaginal bleeding during this time. Following a postoperative care plan is important. This includes managing pain, taking care of the wound, and knowing when to start doing normal activities again.
First Two Weeks at Home
In the first two weeks at home, patients usually start feeling better. It’s vital to stick to the postoperative instructions given by your healthcare team. This includes avoiding lifting, bending, or driving too soon.
Key activities during this period include:
- Slowly increasing mobility and doing light exercise as you can
- Watching for signs of infection or complications
- Going to follow-up appointments as scheduled
Weeks 2-6 Recovery Progression
Between two to six weeks after surgery, most patients keep getting better and return to their usual activities. The speed of recovery depends on the surgery’s extent and the patient’s health.
By six weeks, many patients have fully recovered from their robotic hysterectomy. But it’s important to follow your healthcare provider’s advice on activity levels and follow-up care.
Physical Changes Inside the Body After Hysterectomy
After a hysterectomy, the body goes through many changes. These changes can affect a woman’s health in different ways. We will look at these changes in detail.
Anatomical Rearrangement
The uterus’s removal causes anatomical rearrangement in the pelvic area. Organs like the intestines might move into the space left by the uterus. This can sometimes cause discomfort as the body adjusts.
Pelvic Floor Adaptations
The pelvic floor muscles are key in supporting organs after a hysterectomy. Pelvic floor adaptations help keep everything in place and prevent prolapse. Women might need to do exercises to strengthen these muscles.
Bladder and Bowel Function Adjustments
Women might notice changes in bladder and bowel function after a hysterectomy. Issues like constipation or changes in how often they need to urinate can happen. These changes usually go away on their own but can be helped with diet and sometimes medicine.
Hormonal Impacts Based on Ovary Preservation
Keeping or removing the ovaries during hysterectomy affects hormones. If the ovaries stay, hormone levels stay steady, avoiding sudden menopause. But if they’re removed, women might experience sudden menopause. Hormone therapy might then be needed.
It’s important to understand these changes to manage expectations and recovery after a hysterectomy. Talking to a healthcare provider can help ensure the best recovery.
Managing Side Effects of Hysterectomy
Managing side effects after a hysterectomy is key for a smooth recovery. A hysterectomy is often needed for gynecological issues. But, it can cause short-term and long-term side effects.
Common Short-term Side Effects
Short-term side effects happen right after surgery, usually in the first few weeks. These include:
- Pain and discomfort
- Bloating and gas
- Vaginal discharge or bleeding
- Urinary tract infections
- Constipation
These can be managed with medicine, diet changes, and rest. It’s important to follow your doctor’s advice for care after surgery.
Long-term Physical Considerations
Some women may face long-term physical issues after a hysterectomy. These can include:
|
Consideration |
Description |
|---|---|
|
Early Menopause |
If the ovaries are removed, women may enter early menopause. Hormone therapy might be suggested. |
|
Pelvic Floor Changes |
Changes in pelvic floor support can cause issues like incontinence or prolapse. |
|
Osteoporosis Risk |
Removing the ovaries can raise the risk of osteoporosis due to lower estrogen levels. |
Regular check-ups with healthcare providers can help manage these long-term issues.
Potential Complications and Warning Signs
Complications after a hysterectomy are rare but can happen. It’s important to know the warning signs of complications, such as:
- Heavy bleeding or hemorrhage
- Infection signs (fever, redness, swelling)
- Severe pain not relieved by medication
- Leg pain or swelling (possible blood clot)
- Shortness of breath
As one study noted, “Early recognition and management of complications are key to preventing long-term morbidity.” If you experience any of these symptoms, seek medical help right away.
“The key to a successful recovery lies not just in the surgery itself, but in the complete care provided before, during, and after the procedure.”
— Expert in Gynecological Surgery
Understanding the side effects and complications of hysterectomy helps prepare for recovery. It’s vital to follow your healthcare provider’s advice and report any concerns quickly.
Post-Hysterectomy Care: Essential Recovery Tips
After a hysterectomy, it’s key to follow certain care tips for a smooth recovery. This period can be tough, but with the right info and support, you can avoid complications and stay well.
Incision and Wound Care
Keeping the incision clean and dry is vital for healing. Gently wash the area with mild soap and water, and dry it with a clean towel. Don’t soak the wound in water until your doctor says it’s okay. Watch for signs of infection like redness, swelling, or discharge, and tell your doctor right away.
Activity Restrictions and Gradual Resumption
Rest is important, but so is starting to move again slowly. Avoid heavy lifting, bending, or hard work for four to six weeks. Start with short walks and light stretching as your doctor suggests, and slowly do more based on how you feel and their advice.
Sleep Positions and Comfort Measures
Getting comfortable sleep is key for healing. Try sleep positions that feel good and help your body heal. Placing a pillow between your knees can ease pelvic strain. Also, use a supportive mattress and keep your room cool for better sleep.
When to Contact Your Healthcare Provider
Knowing when to call your doctor is important. If you have severe pain, heavy bleeding, fever, or signs of infection, reach out. Being aware of these issues and getting help when needed is a big part of your recovery.
By following these recovery tips, you can manage your post-hysterectomy care well. This helps avoid complications and makes your healing process smoother and more comfortable.
Nutrition and Exercise for Optimal Hysterectomy Recovery
Recovering from a hysterectomy needs careful attention to nutrition and exercise. A good diet and the right physical activity can greatly help. They can reduce the risk of complications and improve your overall health.
Dietary Recommendations to Promote Healing
Eating a balanced diet is key for recovery after a hysterectomy. We recommend:
- Protein-rich foods like lean meats, fish, and legumes to support tissue repair
- Fruits and vegetables high in vitamins and minerals for overall health
- Whole grains for fiber and sustained energy
- Adequate hydration through plenty of water intake
Adding foods high in antioxidants, like berries and leafy greens, can also help. They reduce inflammation and promote healing.
Preventing Constipation After Surgery
Constipation is common after surgery, due to pain medication. To prevent it, we suggest:
- Increasing fiber intake through diet or supplements
- Drinking plenty of water
- Engaging in light physical activity as soon as it’s safe to do so
Your healthcare provider might also recommend a stool softener to manage constipation.
Safe Exercise Progression Timeline
Exercise is important for recovery, but progress slowly. We advise:
- Starting with gentle movements and stretching within the first few days post-surgery
- Gradually increasing activity levels over the following weeks
- Avoiding heavy lifting, bending, or strenuous activities for at least 6 weeks
Always follow your healthcare team’s specific guidance on exercise and physical activity.
Pelvic Floor Strengthening Exercises
Pelvic floor exercises, like Kegels, can strengthen the muscles that support the pelvic organs. To do Kegels:
- Tighten the muscles you would use to stop the flow of urine
- Hold for a few seconds, then release
- Repeat this process several times throughout the day
Doing these exercises consistently is important. They can be continued long after the initial recovery period.
Here’s a summary of the key nutrition and exercise recommendations in a tabular format:
|
Aspect |
Recommendations |
Benefits |
|---|---|---|
|
Diet |
Protein-rich foods, fruits, vegetables, whole grains, adequate hydration |
Supports tissue repair, overall health, and healing |
|
Constipation Prevention |
High fiber intake, plenty of water, light physical activity |
Reduces the risk of constipation |
|
Exercise |
Gentle movements, gradual increase in activity, avoid heavy lifting |
Promotes safe recovery, strengthens pelvic floor muscles |
|
Pelvic Floor Strengthening |
Kegel exercises |
Supports pelvic organ function and overall pelvic health |
Emotional and Psychological Aspects of Recovery
Recovering from a hysterectomy is more than just healing physically. It also means adjusting emotionally and psychologically. Patients often face a mix of feelings that can be hard to handle.
Influence of Hormonal Changes on Mood
Hormonal shifts after a hysterectomy can really affect a patient’s mood. Even if the ovaries stay, the surgery can mess with hormone levels. This can lead to mood swings, anxiety, or depression. It’s key for patients to talk about these changes with their doctors.
Common emotional responses include:
- Feelings of loss or grief
- Anxiety about the future
- Mood swings
- Depression
Processing Feelings About Fertility Changes
Deciding to have a hysterectomy often means accepting the end of fertility. This can be tough, for those who wanted more kids. Counseling or support groups offer a place to share these feelings.
Body Image and Identity Adjustments
A hysterectomy can change how a woman sees her body and her identity. Some might feel their femininity or sexuality has changed. It’s important to talk about these feelings with healthcare providers or therapists to stay emotionally well.
Support Resources and Counseling Options
There are many ways to get support during the emotional and psychological parts of recovery. These include:
- Counseling or therapy sessions
- Support groups, either in-person or online
- Educational materials and resources
- Online forums and communities
Using these resources can help patients deal with emotional challenges. They can come out of recovery stronger and more resilient.
Conclusion: Advances in Robotic Hysterectomy and Recovery
Robotic hysterectomy has changed gynecological surgery a lot. It gives patients a new, less invasive way to get surgery. This method is more precise and helps patients recover faster.
Knowing how to recover from a hysterectomy is key. It helps patients get through their post-surgery time well. Getting good care during this time is very important for feeling better and getting back to normal.
We talked about the good things about robotic hysterectomy. It means patients can stay in the hospital less and feel less pain after surgery. This makes the recovery easier. As technology gets better, robotic hysterectomy will keep getting even better for patients.
Healthcare providers play a big role in helping patients recover from hysterectomy. They give them the info and support they need. This makes the recovery process better for everyone. We keep working to make medical care better and more focused on the patient.
FAQ
What is a robotic hysterectomy?
A robotic hysterectomy is a surgery to remove the uterus. It uses the da Vinci Surgical System. This technology helps surgeons work more precisely.
How long does a robotic hysterectomy take?
The time needed for a robotic hysterectomy varies. It usually takes 1 to 3 hours. This depends on the case’s complexity and the surgeon’s skill.
What are the benefits of robotic hysterectomy compared to traditional methods?
Robotic hysterectomy has many advantages. It uses smaller cuts, leading to less blood loss and fewer complications. Recovery is also faster than with traditional surgery.
How is the uterus removed during a robotic hysterectomy?
The uterus can be removed in different ways. This includes vaginal extraction, morcellation, or mini-laparotomy. The choice depends on the uterus’s size and the surgeon’s preference.
What is the recovery time for a robotic hysterectomy?
Recovery from a robotic hysterectomy is quicker than open surgery. Most patients can get back to normal in 2-6 weeks.
What are the common side effects of hysterectomy?
Side effects of hysterectomy include pain, bleeding, infection, and emotional changes. Proper care can help reduce these risks.
How can I manage pain after a robotic hysterectomy?
Managing pain involves medication and rest. Always follow your healthcare provider’s advice on pain management.
When can I resume normal activities after a robotic hysterectomy?
You can start with light activities a few days to a week after surgery. Gradually increase to more strenuous activities over 2-6 weeks.
What dietary recommendations are suggested after a hysterectomy?
Eat a balanced diet with fruits, vegetables, and fiber. This helps with healing and prevents constipation. Drinking plenty of water is also important.
Are there any exercises I should do after a hysterectomy?
Yes, gentle exercises like Kegels can support recovery. Always follow a safe exercise plan given by your healthcare provider.
How can I cope with emotional changes after a hysterectomy?
Seek support from healthcare providers, counselors, or support groups. Processing feelings about fertility and body image changes can also help.
What are the signs of potentially complications after a hysterectomy?
Watch for severe pain, heavy bleeding, fever, or trouble urinating. Contact your healthcare provider right away if you notice these symptoms.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC3015554/[2























