Liv Hospital provides fast and accurate diagnosis with expert care.
Send us all your questions or requests, and our expert team will assist you.
Food Poisoning Diagnosis and Evaluation
Diagnosis and Evaluation is the cornerstone of effective care for patients who present with suspected food poisoning, especially for international travelers seeking treatment at Liv Hospital. Understanding how to quickly identify the cause, assess severity, and initiate appropriate therapy can prevent complications and reduce hospital stay. In Turkey, food‑borne illnesses affect an estimated 1 in 10 travelers, underscoring the need for a systematic approach that blends clinical expertise with state‑of‑the‑art diagnostics.
This page is designed for patients, caregivers, and healthcare professionals who need a clear roadmap of the diagnostic pathway. We will explore symptom recognition, clinical assessment, laboratory and imaging studies, differential diagnosis, and how the results shape a personalized treatment plan. Whether you are arriving from abroad or coordinating care with a local physician, the information below reflects the protocols followed by Liv Hospital’s JCI‑accredited infectious disease team.
By the end of this guide, you will understand the step‑by‑step process that transforms initial complaints into a definitive diagnosis, enabling timely and targeted therapy.
Recognizing Symptoms and Patient History

Accurate food poisoning diagnosis begins with a thorough review of symptoms and exposure history. Patients typically present within hours to days after ingesting contaminated food, and the pattern of symptoms can hint at the responsible pathogen.
Collecting a detailed history is essential. Key questions include:
Onset Time | Typical Pathogen | Key Clinical Feature |
|---|---|---|
1–6 hours | Staphylococcus aureus, Bacillus cereus (emetic type) | Rapid vomiting, mild diarrhea |
6–24 hours | Clostridium perfringens, Vibrio cholerae | Profuse watery diarrhea |
24–72 hours | Salmonella, Campylobacter, E. coli (STEC) | Bloody diarrhea, fever |
By aligning symptom timing with likely organisms, clinicians can prioritize specific tests during the diagnosis and evaluation process.
Initial Clinical Assessment and Physical Examination
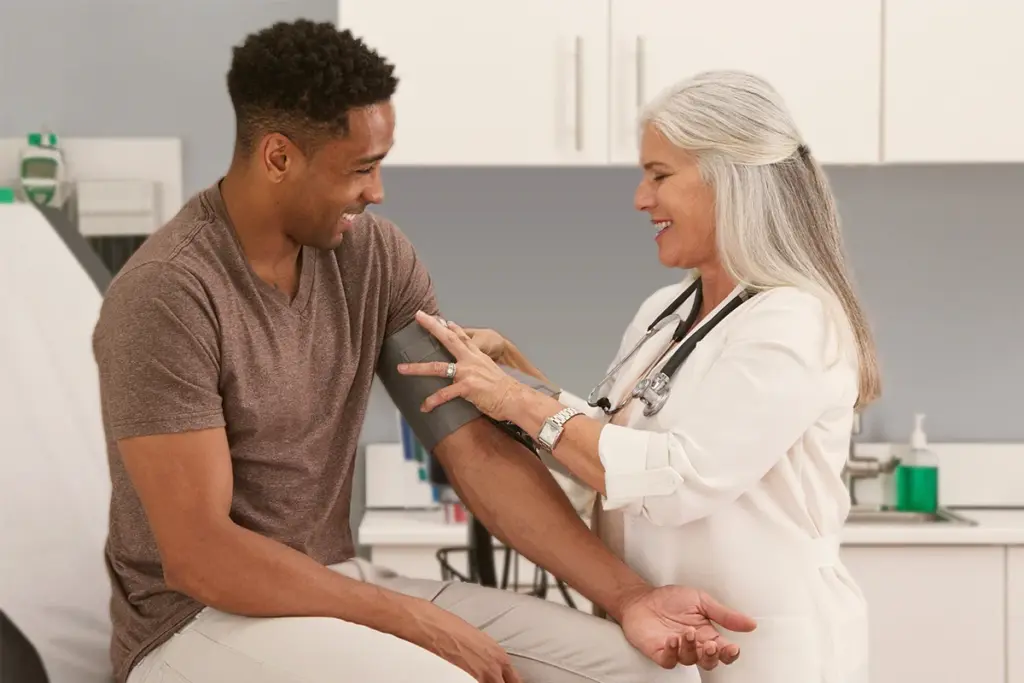
After the history, a focused physical exam determines the patient’s hemodynamic status and identifies red‑flag signs that require urgent intervention.
Clinicians use a standardized scoring system, such as the Acute Physiology and Chronic Health Evaluation (APACHE) II, to quantify severity. The following table illustrates how findings translate into clinical decisions:
Finding | Interpretation | Recommended Action
|
|---|---|---|
BP < 90/60 mmHg | Hypotension → possible shock | Immediate IV fluid resuscitation |
Temp > 38.5 °C | Fever → systemic infection | Obtain blood cultures, consider antibiotics |
Severe abdominal guarding | Possible perforation or peritonitis | Urgent imaging, surgical consult |
The assessment guides the urgency of laboratory and imaging studies, ensuring that critical patients receive rapid diagnosis and evaluation while stable individuals can follow a more measured work‑up.
Laboratory Tests and Diagnostic Procedures
Laboratory analysis provides objective data to confirm the causative agent and evaluate the patient’s systemic response.
Liv Hospital employs rapid molecular panels that deliver results within hours, shortening the time to targeted therapy. The table below compares conventional culture with modern PCR methods:
Test | Turnaround Time | Sensitivity | Typical Use
|
|---|---|---|---|
Stool culture | 48–72 hours | 70–85 % | Broad bacterial detection |
Multiplex PCR panel | 2–4 hours | 90–99 % | Rapid identification of multiple pathogens |
These results, combined with clinical findings, complete the diagnosis and evaluation cycle and allow physicians to prescribe pathogen‑specific therapy or supportive care.

Imaging and Specialized Examinations
While most cases of food poisoning are diagnosed clinically and with laboratory data, imaging becomes crucial when complications are suspected.
In Liv Hospital’s diagnostic algorithm, imaging is ordered after initial assessment if any of the following are present:
Imaging findings are integrated with lab results to refine the differential diagnosis and guide surgical or medical intervention.
Differential Diagnosis: Excluding Other Gastrointestinal Disorders
Food poisoning shares symptoms with several other gastrointestinal conditions. A systematic differential diagnosis prevents mismanagement.
Condition | Key Distinguishing Feature | Relevant Test
|
|---|---|---|
Viral gastroenteritis (e.g., norovirus) | Often linked to outbreaks in closed settings | Stool PCR for viral RNA |
Inflammatory bowel disease | Chronic course, weight loss, extra‑intestinal signs | Colonoscopy with biopsies |
Clostridioides difficile infection | Recent antibiotic use, pseudomembranous colitis | Toxin assay or PCR |
Acute pancreatitis | Epigastric pain radiating to back, elevated lipase | Serum amylase/lipase, CT abdomen |
By systematically ruling out these alternatives, clinicians ensure that the diagnosis and evaluation process remains focused on the true etiology, leading to appropriate therapy.
Developing a Personalized Treatment Plan Based on Evaluation
Once the causative agent and disease severity are identified, a tailored management strategy is formulated. The plan balances antimicrobial therapy, supportive care, and monitoring.
Liv Hospital’s multidisciplinary team—including infectious disease specialists, gastroenterologists, and nutritionists—collaborates to ensure that each international patient receives culturally sensitive instructions and follow‑up arrangements.
Follow‑Up, Monitoring, and Prevention Strategies
Effective follow‑up confirms resolution and prevents recurrence. The schedule varies with disease severity and the identified pathogen.
Preventive counseling focuses on food safety practices, especially for travelers:
Through diligent monitoring and education, Liv Hospital helps patients maintain health long after the acute episode resolves.
Why Choose Liv Hospital ?
Liv Hospital combines JCI accreditation, cutting‑edge diagnostics, and a dedicated international patient service team. Our experts speak multiple languages, arrange airport transfers, and coordinate accommodation, ensuring a seamless experience from arrival to discharge. With a focus on personalized care and evidence‑based protocols, we deliver safe, effective treatment for food‑borne illnesses and many other complex conditions.
Ready to begin your personalized evaluation? Contact Liv Hospital today to schedule a consultation with our infectious disease specialists. Our 360‑degree support team will guide you through every step, from travel arrangements to post‑treatment follow‑up.

Send us all your questions or requests, and our expert team will assist you.
Food poisoning usually presents within hours to a few days after ingesting contaminated food. Early signs are nausea and vomiting, often appearing within 1–6 hours. Diarrhea can be watery or bloody and may last from a few hours to several days. Abdominal cramping can be severe and colicky. Fever is generally low‑grade but may exceed 38.5 °C with bacterial infections. In severe cases, patients may show systemic signs such as dehydration, dizziness, or altered mental status, indicating the need for urgent medical attention.
At Liv Hospital, clinicians first obtain a thorough exposure history, noting foods eaten in the 24–72 hours before symptom onset, travel details, and any recent antibiotic use. A focused physical examination assesses vital signs, hydration status, abdominal findings, and neurological status. Based on these findings, specific laboratory tests such as CBC, electrolytes, stool culture, multiplex PCR, and blood cultures are ordered. Imaging studies like abdominal X‑ray, ultrasound, or CT are reserved for patients with persistent pain, peritoneal signs, or worsening labs. The integration of clinical, laboratory, and imaging data leads to a definitive diagnosis.
The laboratory work‑up starts with a complete blood count to detect leukocytosis, suggesting bacterial infection. Serum electrolytes and renal function tests evaluate dehydration and metabolic disturbances. Stool culture remains the traditional method for detecting bacterial pathogens, though it takes 48–72 hours. Multiplex PCR panels provide rapid (2–4 hours) identification of a wide range of bacterial, viral, and parasitic agents with high sensitivity (90–99 %). Blood cultures are indicated when fever or sepsis is suspected. Specific serology or toxin assays, such as Clostridium difficile toxin testing, are used when particular pathogens are suspected.
While most food poisoning cases are diagnosed clinically and with labs, imaging becomes essential when red‑flag signs suggest complications. An abdominal X‑ray screens for ileus or perforation. Ultrasound evaluates gallbladder disease that can mimic food‑borne symptoms. Contrast‑enhanced CT of the abdomen detects severe colitis, abscesses, or ischemic bowel. Endoscopy is reserved for persistent severe diarrhea or suspicion of inflammatory bowel disease. Liv Hospital follows a protocol where imaging is pursued after the initial assessment if any of the following occur: pain lasting more than 12 hours, signs of peritoneal irritation, unexplained high‑grade fever, or rapidly deteriorating laboratory parameters.
Management is tailored to the identified pathogen and disease severity. Mild cases receive oral rehydration salts, while moderate to severe dehydration requires IV crystalloids. Antimicrobial therapy is reserved for invasive bacterial pathogens such as severe Salmonella or Campylobacter, guided by susceptibility patterns. Specific antitoxin or antidiarrheal agents, like oral vancomycin for C. difficile, are used selectively. Nutritional support involves gradual re‑introduction of a bland diet after symptom control. Comprehensive patient education covers safe food handling, travel precautions, and warning signs that necessitate urgent care. Liv Hospital’s multidisciplinary team ensures culturally sensitive instructions and coordinated follow‑up.
Liv Hospital schedules a structured follow‑up plan. A telephone check‑in on days 1–2 assesses hydration status and symptom progression. An in‑person visit between days 3–7 allows repeat laboratory testing if initial results were abnormal. A 2–4 week evaluation screens for post‑infectious complications such as reactive arthritis or hemolytic uremic syndrome. For severe bacterial infections, a stool culture may be repeated at 6 months to confirm eradication. Throughout, the international patient service team assists with language support, travel logistics, and coordination with local physicians to ensure continuity of care.
Travelers can markedly reduce their risk by following food safety practices. Avoid raw or undercooked meats, eggs, and seafood. Choose pasteurized dairy products and avoid unpasteurized cheeses. Drink bottled or filtered water in regions with questionable sanitation, and use it for brushing teeth. Wash fruits and vegetables thoroughly, preferably with safe water. Before travel, check for any local outbreak alerts and heed public health advisories. Liv Hospital provides pre‑travel counseling to international patients, emphasizing these measures and offering resources for safe dining options abroad.

 Food Poisoning
Food Poisoning Food Poisoning
Food Poisoning Food Poisoning
Food Poisoning Food Poisoning
Food Poisoning Food Poisoning
Food Poisoning Food Poisoning
Food Poisoning
Leave your phone number and our medical team will call you back to discuss your healthcare needs and answer all your questions.
Your Comparison List (you must select at least 2 packages)