Malaria can be prevented with mosquito protection and preventive medication. Liv Hospital supports international patients with expert guidance and care.
Send us all your questions or requests, and our expert team will assist you.
Prevention and Control of Malaria
Effective prevention and control of malaria remains a global health priority, especially for travelers and communities in endemic regions. Each year, malaria claims hundreds of thousands of lives, yet many cases are avoidable with coordinated measures. This page provides a detailed guide for international patients, travelers, and health professionals seeking evidence‑based strategies to reduce malaria risk. We will cover vector management, personal protection, community programs, surveillance, and travel preparation, all aligned with the standards upheld by Liv Hospital.
Understanding how the disease spreads, which interventions work best, and how to access timely care can dramatically lower infection rates. Whether you are planning a trip to a high‑risk area or supporting a public‑health initiative, the information below equips you with practical steps for comprehensive malaria prevention and control. Let’s explore the science‑backed approaches that protect individuals and populations alike.
Understanding Malaria Transmission and Risk Factors
Malaria is transmitted through the bite of infected Anopheles mosquitoes, which thrive in warm, humid environments. Recognizing where and when transmission occurs is the first pillar of effective prevention and control. Key risk factors include proximity to stagnant water, lack of indoor residual spraying, and limited access to health education.
Endemic zones are primarily located in sub‑Saharan Africa, parts of South‑East Asia, and Latin America. Seasonal rainfall often spikes mosquito breeding, increasing transmission rates during the rainy months.
Children under five, pregnant women, and immunocompromised individuals face the highest mortality risk. Socio‑economic challenges, such as inadequate housing and limited healthcare access, further exacerbate vulnerability.
Vector Control Strategies for Mosquito Management

Targeting the mosquito vector is central to malaria prevention and control. Integrated vector management combines environmental, chemical, and biological tactics to suppress mosquito populations sustainably.
Removing standing water eliminates breeding sites. Community clean‑up campaigns that drain puddles, cover water storage containers, and maintain proper waste disposal are cost‑effective measures.
Indoor residual spraying (IRS) with long‑acting insecticides and the distribution of long‑lasting insecticidal nets (LLINs) have proven efficacy in reducing indoor mosquito contact.
Intervention | Typical Coverage | Effectiveness
|
|---|---|---|
IRS (Indoor Residual Spraying) | 80‑90% of households | 40‑60% reduction in malaria incidence |
LLINs (Long‑Lasting Insecticidal Nets) | 70‑85% of at‑risk population | 50‑70% reduction in child mortality |
Larval Source Management | Variable, site‑specific | Up to 30% reduction when combined with IRS/LLINs |
Combining these methods creates a layered defense that significantly curtails mosquito density and human exposure.
Personal Protective Measures and Chemoprophylaxis
Individual actions complement community‑wide efforts in malaria prevention and control. Travelers and residents should adopt a suite of protective behaviors and, when appropriate, take antimalarial medication.
Sleeping under an LLIN, wearing long‑sleeved clothing, and using repellents containing DEET or picaridin reduce bite risk.
Common prophylaxis options include:
Selection depends on travel destination, drug resistance patterns, and personal medical history. Consultation with a travel medicine specialist at Liv Hospital ensures the regimen aligns with your health profile.

Community‑Based Prevention Programs and Education
Sustainable malaria prevention and control hinges on community ownership. Educational outreach, school programs, and local health worker training empower residents to adopt and maintain protective practices.
Interactive workshops that demonstrate net installation, proper use of repellents, and recognition of malaria symptoms increase early treatment seeking.
Engaging local leaders and religious figures helps disseminate messages effectively. Incentive‑based schemes, such as distributing free nets to households that attend training, boost participation rates.
These grassroots initiatives create a feedback loop where community members report breeding sites, facilitating rapid vector control responses.
Surveillance, Diagnosis, and Prompt Treatment
Robust surveillance systems are essential for tracking malaria trends and guiding prevention and control policies. Early diagnosis and immediate treatment break the transmission cycle.
Rapid diagnostic tests (RDTs) and microscopy remain the gold standards. In endemic areas, point‑of‑care RDTs enable quick decision‑making, while laboratory microscopy provides species‑specific data.
Artemisinin‑based combination therapies (ACTs) are the first‑line treatment for uncomplicated Plasmodium falciparum infection. Prompt administration within 24 hours of symptom onset reduces complications and onward transmission.
Stage | Key Action | Outcome
|
|---|---|---|
Case Detection | RDT or microscopy at health facility | Accurate identification of infection |
Treatment Initiation | ACT regimen within 24 h | Rapid parasite clearance |
Follow‑up | Day‑3 parasite check | Confirm cure, detect resistance |
Liv Hospital’s infectious‑disease specialists offer rapid diagnostic services and evidence‑based treatment plans for international patients, ensuring seamless care from detection to recovery.
Travel Preparation and International Guidelines
For travelers, aligning personal precautions with World Health Organization (WHO) and Centers for Disease Control and Prevention (CDC) recommendations forms the backbone of malaria prevention and control before departure.
A thorough medical review at Liv Hospital evaluates vaccine needs, existing conditions, and medication interactions. The specialist will provide a personalized prophylaxis plan and educate on emergency measures.
Maintain consistent use of LLINs, apply repellents at dawn and dusk, and stay in screened or air‑conditioned accommodations. Carry a travel health kit that includes a spare net, repellent, and a rapid test kit if feasible.
Following these steps minimizes exposure risk and ensures swift medical response should infection occur.
Why Choose Liv Hospital ?
Liv Hospital provides internationally accredited, JCI‑standard care with a dedicated focus on infectious diseases. Our multidisciplinary team combines cutting‑edge diagnostics, personalized prophylaxis, and comprehensive treatment pathways for malaria. International patients benefit from coordinated appointment scheduling, interpreter services, and assistance with travel logistics, ensuring a seamless experience from consultation to recovery.
Ready to safeguard your health against malaria? Contact Liv Hospital today to schedule a pre‑travel consultation or discuss personalized prevention strategies. Our experts are here to guide you every step of the way.

Send us all your questions or requests, and our expert team will assist you.
The disease spreads when an Anopheles mosquito bites a person after feeding on the blood of an infected individual. The parasite develops inside the mosquito and is passed to the next host during a subsequent bite. Transmission is highest in areas with stagnant water, limited indoor residual spraying, and poor housing conditions. Understanding these factors helps target vector control measures such as eliminating breeding sites and using insecticide‑treated nets.
Effective personal protection includes sleeping under an LLIN every night, wearing long‑sleeved shirts and trousers, and applying skin‑safe repellents containing at least 30% DEET or picaridin to exposed skin during peak mosquito activity at dawn and dusk. Selecting screened or air‑conditioned accommodation further reduces exposure. Combining these measures with chemoprophylaxis provides layered protection against infection.
IRS involves coating the interior surfaces of homes with insecticides that remain active for several months. Mosquitoes resting on treated walls pick up a lethal dose, dramatically lowering indoor biting rates. Studies show IRS can achieve a 40‑60% reduction in malaria incidence when coverage reaches 80‑90% of households. It works best when combined with other interventions such as LLINs and environmental management.
Atovaquone‑proguanil is taken daily and is well‑tolerated, making it suitable for short trips. Doxycycline is also daily and offers antibacterial benefits, but may cause photosensitivity. Mefloquine is taken weekly and is useful for long‑term travelers, though it can have neuropsychiatric side effects. The choice depends on the malaria species prevalent in the destination, local drug‑resistance data, and the traveler’s medical history. A pre‑travel consultation at Liv Hospital tailors the regimen.
Community‑based programs use workshops, school curricula, and local leader engagement to teach proper net installation, repellents use, and symptom recognition. When households understand how malaria spreads, they are more likely to participate in clean‑up campaigns, report stagnant water, and attend health‑worker visits. Incentive schemes, such as free nets for training attendance, increase adoption rates. These grassroots actions create a feedback loop that strengthens surveillance and vector‑control responses.

 Infectious Diseases
Infectious Diseases Infectious Diseases
Infectious Diseases Infectious Diseases
Infectious Diseases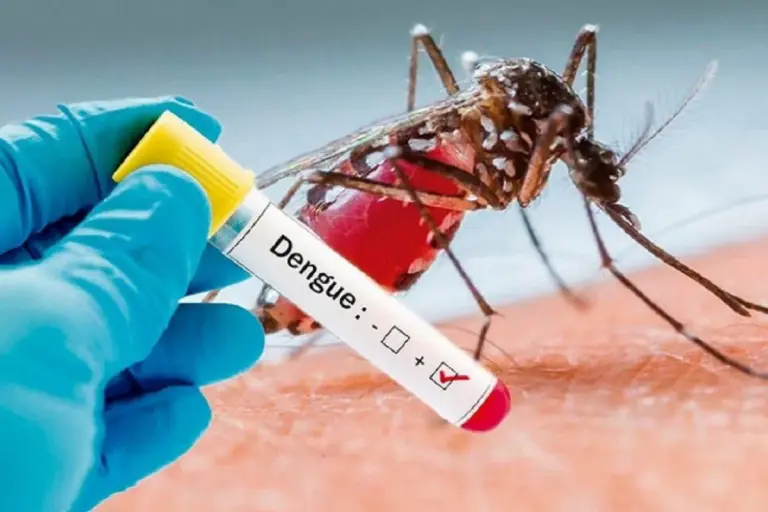 Infectious Diseases
Infectious Diseases Infectious Diseases
Infectious Diseases Infectious Diseases
Infectious DiseasesYour Comparison List (you must select at least 2 packages)