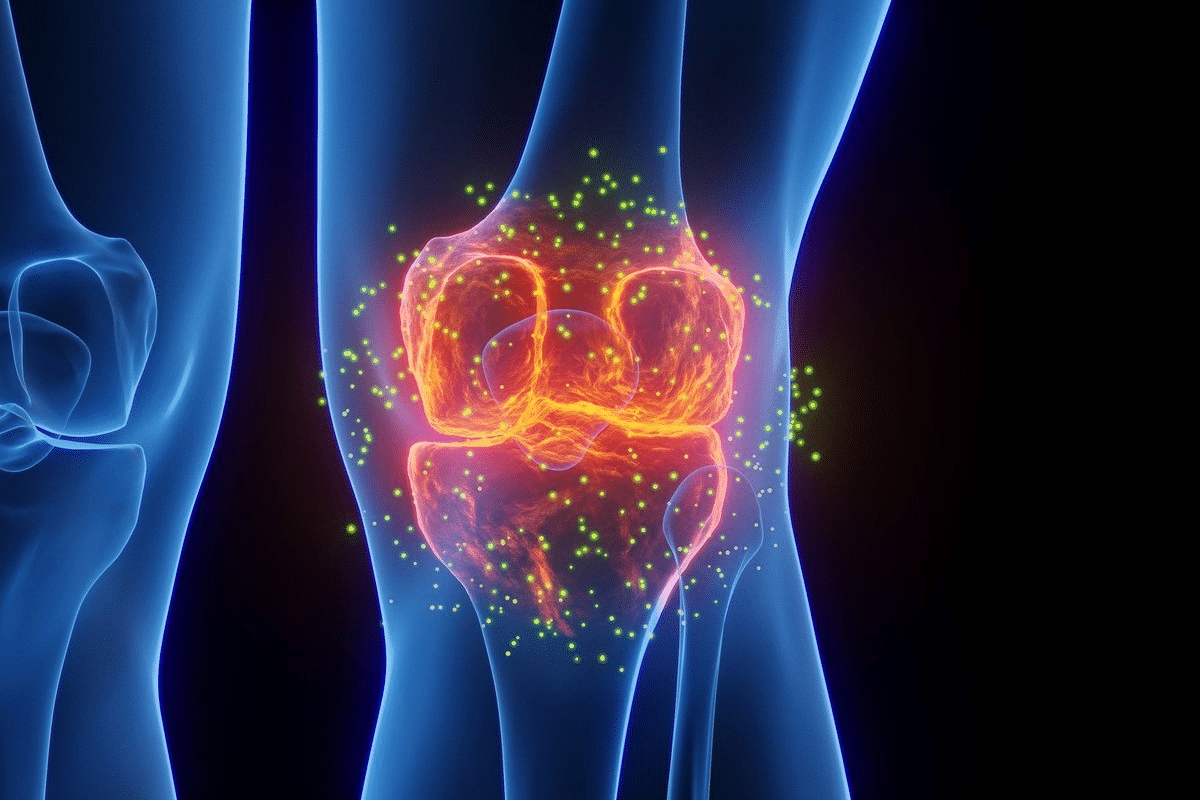
Rheumatoid arthritis is a chronic disease that affects about 1% of people worldwide. It is a systemic, multi-factorial, inflammatory, and progressive autoimmune disease. Detailed explanation of therheumatoid arthritis disease progression pathophysiology, focusing on immune attack on the synovium.
Diagnosing rheumatoid arthritis can be tough. Symptoms often come and go, as noted by Vivien Williams. Knowing how rheumatoid arthritis works is key to finding good treatments.
We understand how complex this condition is and its effects on patients. Our goal is to offer complete care and support.
Key Takeaways
- Rheumatoid arthritis is a complex autoimmune condition.
- It affects approximately 1% of the global population.
- Understanding its pathophysiology is vital for effective treatment.
- Diagnosing rheumatoid arthritis can be challenging.
- Comprehensive care and support are essential for managing the condition.
Understanding Rheumatoid Arthritis: A Systemic Autoimmune Disease
Rheumatoid arthritis (RA) is a long-lasting disease where the immune system attacks the body. It mainly affects the joints, causing pain and damage. Medical Expert, leading to inflammation in the joints.
Definition and Classification
RA is known for its ongoing inflammation in the joints. Doctors use specific criteria to diagnose it. This includes checking for certain antibodies like rheumatoid factor (RF) and anti-citrullinated protein antibodies (ACPAs).
Distinguishing Features from Other Arthritides
RA is different from other arthritis types because of its symmetrical joint damage. It also has systemic effects and specific antibodies. Extra-articular symptoms, like nodules and vasculitis, can occur too.
“The immune system’s deregulation in RA leads to a cascade of inflammatory events that result in joint damage and potentially other systemic complications.”Medical Expert
Here are the main features of RA:
|
Characteristics |
Description |
|---|---|
|
Symmetric Joint Involvement |
Affects joints on both sides of the body equally |
|
Autoantibodies |
Presence of RF and ACPAs |
|
Systemic Manifestations |
Involvement of other body systems beyond joints |
Epidemiology of Rheumatoid Arthritis

It’s important to know about rheumatoid arthritis (RA) to help those at risk. RA is a chronic disease that affects millions worldwide. It greatly impacts their quality of life.
Global Prevalence and Incidence
About 1% of the world’s population has RA. This means around 40 people out of 100,000 get it every year. The numbers vary by region and population.
Key statistics on RA prevalence include:
- Higher prevalence in developed countries
- Increased incidence with age, peaking between the ages of 30 and 60
- Greater affectation of women compared to men, with a female-to-male ratio ranging from 2:1 to 3:1
Demographic Distribution and Risk Factors
RA’s spread is influenced by genetics, environment, and hormones. Some groups are more at risk due to their genes. Smoking and other environmental factors also play a big role.
Key risk factors for RA include:
- Genetic predisposition, like HLA-DRB1 alleles
- Smoking and other environmental exposures
- Hormonal influences, with a higher prevalence in women
- Family history of RA or other autoimmune diseases
Understanding these factors helps us find at-risk groups. This way, we can improve early detection and treatment of RA.
Genetic Predisposition in Rheumatoid Arthritis
Genetic factors play a big role in rheumatoid arthritis. People with a family history of RA are more likely to get it. This shows how important genetics are.
Rheumatoid arthritis is a complex disease. It’s influenced by genes and the environment. Certain genes can make a person more likely to get RA.
HLA-DRB1 Shared Epitope
The HLA-DRB1 gene is a big risk factor for RA. The “shared epitope” (SE) alleles in this gene increase the risk. They also make the disease worse.
The HLA-DRB1 SE is a key genetic risk factor. It affects how the immune system works. It helps decide if the body sees something as self or not.
Non-HLA Genetic Risk Factors
Other genes, not just HLA-DRB1, can increase RA risk. Genes like PTPN22 and STAT4 are involved. They help T-cells work right.
These genes can change how immune cells work. This can lead to RA. Knowing about these genes helps us understand RA better.
Gene-Environment Interactions
Genetics aren’t the only thing that matters in RA. The environment also plays a big part. Things like smoking can increase the risk of RA.
How genes and environment work together is important. For example, smoking can make the risk of RA higher in people with certain genes. This shows how both genetics and environment matter.
Looking at how genes and environment interact helps us understand RA better. It might also help us find new ways to treat it.
Environmental Triggers and Initiating Factors
Environmental factors are key in starting Rheumatoid Arthritis in people who are at risk. Even though genes play a part, things around us can start the disease.
Tobacco Exposure and Smoking
Research shows that smoking is a big risk for getting RA. Smoking not only raises the risk of RA but also makes the disease worse and harder to treat. It starts inflammation and can change how the immune system works.
Smoking can make proteins change in a way linked to RA. This is because of the presence of anti-citrullinated protein antibodies (ACPAs), a key sign of RA. Smoking and genes, like HLA-DRB1, together increase the risk of RA a lot.
- Smoking is linked to a higher risk of RA, more so in people with a genetic risk.
- The more you smoke, the higher the risk.
- Quitting smoking is important for RA patients who smoke.
Infectious Agents and Microbiome Influence
Infectious agents might start RA. Bacteria and viruses are being studied for their role. The microbiome’s effect on inflammation and the immune system is being researched, showing it might play a part in RA.
“The gut-joint axis is an emerging area of research, suggesting that changes in the gut microbiome may influence joint inflammation and disease activity in RA.”
Specific infections, like periodontal disease from Porphyromonas gingivalis, are being looked at. They might start RA by causing inflammation and immune reactions.
Physical Trauma and Mechanical Stress
Physical trauma and stress might start RA in some. While not as clear as smoking, there are hints that trauma could lead to RA in some cases.
The process might involve inflammation and starting an autoimmune response in people already at risk.
- Physical trauma can cause local inflammation.
- Mechanical stress might start or make joint damage worse.
- The link between trauma and RA might be stronger with other risk factors.
Knowing about these triggers is key to preventing and managing RA. By understanding and reducing these risks, we can lower the chance and severity of the disease, even in those with a genetic risk.
Immunopathogenesis of Rheumatoid Arthritis
The immune system goes wrong in Rheumatoid Arthritis. This leads to long-lasting inflammation and damage to joints.
Innate Immune System Dysfunction
The innate immune system is the first defense against germs. In RA, it doesn’t work right, causing too much inflammation. Pattern recognition receptors (PRRs) on these cells keep the inflammation going by reacting to body’s own signals.
When innate immune cells like macrophages and dendritic cells get activated, they make pro-inflammatory cytokines. TNF-α and IL-1β are among these. They fuel the inflammation, causing harm to joints.
Adaptive Immune Response Abnormalities
The adaptive immune response, with T cells and B cells, is also off in RA. Autoreactive T cells attack the body’s own cells, causing an immune response against itself. This leads to the making of autoantibodies, like rheumatoid factor (RF) and anti-citrullinated protein antibodies (ACPAs).
B cells are key in RA’s disease process. They make autoantibodies, present antigens to T cells, and release cytokines that control the immune response.
Cytokine Networks and Inflammatory Cascades
Cytokines are important molecules in the immune system. In RA, there’s too much of the bad kind. TNF-α is a major player in this, causing inflammation and joint damage.
The mix of cytokines and immune cells creates a cycle of inflammation. This cycle keeps the disease going. Knowing how these cytokines work is key to finding new treatments.
T-Cell and B-Cell Dysfunction in Rheumatoid Arthritis
Rheumatoid arthritis is marked by T-cell and B-cell dysfunction. This leads to ongoing inflammation and damage to joints. The interaction between these immune cells plays a big role in the disease’s development.
T-Cell Activation and Differentiation
T-cells are key in the adaptive immune response, and their malfunction is a key feature of RA. T-cell activation happens when they meet specific antigens. This leads to their transformation into different types, like Th1, Th17, and Treg cells.
The balance between these T-cell types is vital for the immune response’s outcome. In RA, there’s often an imbalance. This imbalance, with too much Th1 and Th17 activity, fuels inflammation and joint damage.
B-Cell Abnormalities and Antibody Production
B-cells are essential for the adaptive immune system, making antibodies. In RA, B-cells are overactive, producing autoantibodies like rheumatoid factor (RF) and anti-citrullinated protein antibodies (ACPAs).
These autoantibodies help form immune complexes that settle in joints. This triggers inflammation and tissue damage. B-cell depletion therapy has been effective in lowering disease activity in RA patients. This shows how important B-cells are in the disease.
Lymphocyte Interactions in the Synovium
The synovium is the main area of inflammation in RA. It’s where T-cells and B-cells meet other immune cells and synovial fibroblasts. These interactions cause the release of pro-inflammatory cytokines and mediators, keeping the inflammation going.
The complex interactions between lymphocytes and other cells in the synovium cause the joint inflammation and damage seen in RA. Knowing about these interactions is key to creating targeted treatments.
The Role of Autoantibodies in Rheumatoid Arthritis
Autoantibodies are key in diagnosing Rheumatoid Arthritis. They are antibodies that attack the body’s own tissues. This helps doctors understand and treat the disease.
Rheumatoid Factor (RF)
Rheumatoid Factor targets the Fc region of IgG. It’s found in 70-80% of RA patients. But, it’s not unique to RA and can appear in other diseases and healthy people too.
Anti-Citrullinated Protein Antibodies (ACPAs)
Anti-Citrullinated Protein Antibodies are very specific to RA. They are found in about 67% of RA patients. These antibodies target proteins that have been modified. Their presence often means the disease will be more severe.
Other Autoantibodies and Their Clinical Significance
RA also involves other autoantibodies like anti-carbamylated and anti-acetylated protein antibodies. These may offer more clues for diagnosis and predicting the disease’s course.
|
Autoantibody |
Prevalence in RA |
Clinical Significance |
|---|---|---|
|
Rheumatoid Factor (RF) |
70-80% |
Diagnostic criterion, associated with disease severity |
|
Anti-Citrullinated Protein Antibodies (ACPAs) |
67% |
High specificity for RA, prognostic marker for disease severity |
|
Anti-Carbamylated Protein Antibodies |
Variable |
Additional diagnostic and prognostic information |
Knowing about autoantibodies in RA is vital for diagnosis and treatment. The types and levels of these antibodies help doctors make treatment plans and predict how the disease will progress.
Rheumatoid Arthritis Disease Progression: Mechanisms and Stages
Rheumatoid arthritis (RA) goes through several stages, from the start to when joints are badly damaged. Knowing these stages is key for catching the disease early and treating it well.
Pre-clinical Phase and Disease Initiation
The pre-clinical phase of RA is when autoantibodies and possible triggers are present. This stage is heavily influenced by genetics, which plays a big role in starting the disease.
Research shows that people with a family history of RA are more likely to get it. This points to the role of genetics in the disease.
Early Inflammatory Phase
The early inflammatory phase is when joint inflammation starts. This leads to pain and swelling in the joints. It’s a critical time for early treatment to avoid lasting damage.
Key Features of Early Inflammatory Phase:
- Synovial inflammation
- Joint pain and swelling
- Presence of inflammatory markers
Established Disease and Chronicity
As RA moves to the established disease stage, chronic inflammation causes joint damage and deformity. At this point, a detailed treatment plan is needed.
Chronic inflammation is a key feature of established RA. It leads to the destruction of cartilage and bone.
|
Stage |
Characteristics |
Clinical Features |
|---|---|---|
|
Pre-clinical |
Autoantibody presence, genetic predisposition |
Asymptomatic |
|
Early Inflammatory |
Synovial inflammation, inflammatory markers |
Joint pain, swelling |
|
Established Disease |
Chronic inflammation, joint damage |
Joint deformity, loss of function |
|
End-Stage |
Severe joint destruction, loss of joint function |
Significant disability |
End-Stage Joint Destruction
The end-stage of RA is marked by severe joint destruction and significant disability. At this point, surgery might be needed to improve joint function.
Understanding how RA progresses is vital for creating effective treatments and better outcomes for patients.
Joint Involvement and Synovial Pathology
RA often starts with small joints in a symmetrical pattern. This pattern is key in diagnosing the disease.
Symmetric Pattern of Joint Involvement
RA’s unique feature is the symmetrical joint involvement. Hands, wrists, and feet are usually the first to show signs. The disease often hits the MCP and PIP joints first.
Table 1 shows how joint involvement can tell us about RA’s progression and severity.
|
Joint Region |
Commonly Affected Joints |
Characteristics of Involvement |
|---|---|---|
|
Hands |
MCP, PIP |
Swelling, tenderness, reduced range of motion |
|
Feet |
MTP |
Pain on walking, swelling |
|
Wrists |
Radiocarpal, ulnocarpal |
Swelling, reduced grip strength |
Synovial Membrane Inflammation and Hyperplasia
The synovial membrane is vital in RA. Its inflammation and growth lead to a thickened synovium. This is a major cause of joint damage.
A leading rheumatologist notes, “The inflamed synovium in RA has immune cells like T cells, B cells, and macrophages. They start the inflammatory process.”
This inflammation leads to the production of pro-inflammatory cytokines. These include TNF-alpha and IL-6, key in the disease.
Pannus Formation and Invasive Properties
Pannus formation is a key part of RA. The inflamed synovium invades and damages cartilage and bone. It acts like a tumor, causing permanent damage.
Cartilage and Bone Erosion Mechanisms
Cartilage and bone erosion in RA is complex. It involves inflammatory cytokines, proteases, and cell interactions. Synovial fibroblasts and immune cells produce MMPs and other enzymes. These break down the extracellular matrix.
Knowing these mechanisms is key for developing effective treatments. It helps slow down the disease’s progression.
Post-Translational Modifications and Cellular Processes
Rheumatoid Arthritis (RA) is influenced by many cellular processes and post-translational modifications. These changes are key in the disease’s development. They affect how proteins work and how the immune system reacts.
Citrullination Process and Pathogenic Significance
Citrullination changes arginine to citrulline, impacting protein function and immune recognition. In RA, this process is vital. It leads to the creation of anti-citrullinated protein antibodies (ACPAs), specific to the disease.
ACPAs are not just markers for RA but also play a role in its development. Citrullination can make proteins more likely to trigger an immune response. This happens through enzymes called peptidylarginine deiminases (PADs), which are active during cell death and inflammation.
“The citrullination of proteins in Rheumatoid Arthritis synovium contributes to the generation of ACPAs, which play a significant role in the disease’s immunopathogenesis.” — Source on Rheumatoid Arthritis Research
Glycosylation Abnormalities
Glycosylation changes are also important in RA. These changes can affect protein stability, function, and how the immune system recognizes them. For example, altered glycosylation of immunoglobulins can change their ability to fight infections and contribute to autoimmunity.
|
Glycosylation Change |
Effect on Protein Function |
Implication in RA |
|---|---|---|
|
Altered IgG glycosylation |
Enhanced pro-inflammatory activity |
Increased joint inflammation |
|
Changes in galactosylation |
Affects antibody-dependent cellular cytotoxicity |
Contributes to autoimmune responses |
Autophagy Dysregulation in Rheumatoid Arthritis
Autophagy is a process where cells break down and recycle their parts. In RA, autophagy is not working right. This leads to aggressive behavior in synovial fibroblasts, causing joint damage.
Research shows that controlling autophagy can reduce inflammation and damage in RA models. Understanding how autophagy goes wrong could lead to new treatments.
Carbamylation and Other Protein Modifications
Carbamylation is a post-translational modification linked to RA. It changes lysine to homocitrulline, creating anti-carbamylated protein antibodies. These antibodies are found in RA patients and affect the disease’s activity.
Other modifications, like phosphorylation and ubiquitination, also play roles in RA’s immune and inflammatory responses. Studying these modifications can give a full picture of RA’s disease mechanisms.
In conclusion, post-translational modifications and cellular processes are key to understanding RA. Further research into these areas could lead to new treatments for the disease.
Epigenetic Factors and Biomarkers in Disease Monitoring
Epigenetic factors are key in rheumatoid arthritis (RA). They affect how the disease acts and grows. Biomarkers are also vital for tracking RA. We’ll look at how these elements help in monitoring RA.
DNA Methylation Patterns
DNA methylation changes gene expression. In RA, these changes are off-balance. Hypomethylation makes some genes work too much, causing inflammation. On the other hand, hypermethylation silences important immune genes.
Histone Modifications and Chromatin Remodeling
Histone changes are key in epigenetics. They can open or close chromatin, affecting gene use. In RA, these changes mess with inflammatory pathways. Histone deacetylase inhibitors might help fix this.
MicroRNA Regulation
MicroRNAs (miRNAs) control gene use after transcription. In RA, some miRNAs don’t work right. This affects inflammation and joint damage. miR-146a and miR-155 are involved in inflammation.
Biomarkers for Disease Activity and Progression
Biomarkers are essential for tracking RA. They help see how the disease is doing and how it might change. New biomarkers, like miRNAs and epigenetic signs, could make tracking better. Personalized medicine using these could lead to better treatments.
Conclusion: Integrating Pathophysiology into Clinical Understanding
Understanding rheumatoid arthritis (RA) is key to better treatments. By using pathophysiology in our work, we can help patients more. This makes managing RA better for everyone.
RA is complex, with genetics, environment, and immune issues playing parts. Knowing this helps doctors tailor treatments for each patient. This approach improves how we manage RA.
As we learn more about RA, we can find new ways to help patients. By mixing clinical knowledge with pathophysiology, we can offer better care. This is good news for those with RA.
FAQ
What is rheumatoid arthritis?
Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes inflammation in the synovium, leading to pain and joint damage. It affects multiple joints, often in a symmetrical pattern.
What are the risk factors for developing rheumatoid arthritis?
Risk factors for RA include genetics and environmental factors. Smoking and certain infections can also increase the risk. Being female and older also raises the risk.
How does the immune system contribute to the development of rheumatoid arthritis?
The immune system is key in RA. It has problems with both innate and adaptive responses. This leads to chronic inflammation and joint damage. T-cells, B-cells, and autoantibodies like rheumatoid factor are involved.
What is the role of autoantibodies in rheumatoid arthritis?
Autoantibodies, like rheumatoid factor, are important in diagnosing RA. They also play a role in the disease’s progression. They contribute to inflammation and joint damage.
How does rheumatoid arthritis progress?
RA goes through stages, from early to end-stage damage. The speed of progression varies. Factors like autoantibodies and treatment effectiveness play a role.
What is the significance of the HLA-DRB1 shared epitope in rheumatoid arthritis?
The HLA-DRB1 shared epitope is a genetic risk factor for RA. It increases the risk of developing the disease. It’s also linked to a more severe disease course and certain autoantibodies.
How does citrullination contribute to the pathogenesis of rheumatoid arthritis?
Citrullination is a process that can lead to RA. It’s linked to the production of anti-citrullinated protein antibodies. These antibodies are a hallmark of the disease.
What is the role of epigenetic factors in rheumatoid arthritis?
Epigenetic factors, like DNA methylation, are important in RA. They regulate gene expression and contribute to disease development. They can also be biomarkers for disease activity.
Is rheumatoid arthritis a systemic disease?
Yes, RA is a systemic disease. It affects not just joints but also organs like the skin, lungs, and heart. It increases the risk of other diseases, like heart disease and osteoporosis.
What is the prognosis for patients with rheumatoid arthritis?
The prognosis for RA patients varies. It depends on disease severity, autoantibodies, and treatment effectiveness. Modern treatments can improve symptoms and quality of life for many patients.
How does rheumatoid arthritis affect the joints?
RA causes inflammation in the synovium, leading to pain and swelling. It damages and destroys joints. Small joints, like those in hands and feet, are often affected symmetrically.
Reference
National Center for Biotechnology Information. Rheumatoid Arthritis: Understanding Disease Progression. Retrieved from https://pubmed.ncbi.nlm.nih.gov/26545940/


































