Explaining that the medical abbreviation for rheumatoid arthritis is RA, and providing common context for its use.
Knowing about rheumatoid arthritis is key when looking at health info. RA is a long-term disease that millions face, mostly women. At places like Liv Hospital, we focus on catching it early and caring for each patient.
RA means rheumatoid arthritis. It causes inflammation in joints and nearby tissues. It’s a condition that can last a lifetime and even affect other parts of the body. Learning about RA helps patients and their families make better choices for their health.
Key Takeaways
RA is a chronic autoimmune disease that affects joints and surrounding tissues.
Early diagnosis is key to managing RA well.
Putting the patient first is vital for better RA care.
RA can harm more than just joints.
Knowing about RA helps patients and families make smart health choices.
Understanding the Medical Abbreviation for Rheumatoid Arthritis

Knowing medical abbreviations is key for good patient care, like with Rheumatoid Arthritis (RA). Rheumatology uses many abbreviations to make diagnoses and treatments easier. RA is a well-known term in medical talk.
Common Medical Abbreviations in Rheumatology
Rheumatology studies diseases of the musculoskeletal system and connective tissues. It uses many abbreviations. Here are some common ones:
- RA: Rheumatoid Arthritis
- OA: Osteoarthritis
- SLE: Systemic Lupus Erythematosus
- AS: Ankylosing Spondylitis
These abbreviations help doctors write and talk faster. They make sure patients get the right care on time.
Why RA is the Standard Abbreviation
The term RA is the top choice for Rheumatoid Arthritis. It’s used a lot because of several reasons:
RA is a long-term condition that doctors often talk about in patient records.
The full name of the condition, Rheumatoid Arthritis, is hard to write fast in busy clinics.
The RA abbreviation is clear and easy to understand, which helps avoid mistakes.
Using RA helps doctors talk and write about patient care quickly. This makes care better for everyone.
The Science Behind Rheumatoid Arthritis

Rheumatoid arthritis, or RA, is a chronic disease that mainly affects the joints. It’s an autoimmune disorder, meaning the body’s immune system attacks its own healthy tissues. This leads to inflammation and damage.
Understanding RA’s autoimmune nature is key to knowing how it progresses. The immune system’s attack on the joints’ lining (synovium) causes inflammation. This results in pain, swelling, and can lead to joint deformity and loss of function.
Autoimmune Nature of RA
The autoimmune aspect of RA involves a complex interplay between the immune system’s components. Cytokines, signaling molecules, play a significant role in the inflammation. They help immune cells communicate, promoting the inflammation seen in RA.
Activation of T-cells and B-cells, types of immune cells, contributes to the disease process.
The production of autoantibodies, such as rheumatoid factor, is a hallmark of RA and aids in its diagnosis.
The immune system’s attack on the synovium leads to its thickening and the formation of pannus, a tissue that invades and destroys the joint.
Inflammatory Processes in Joints
The inflammatory processes in RA involve immune cells infiltrating the synovium. This leads to the release of various inflammatory mediators. This results in:
Synovial inflammation and hyperplasia.
Joint effusion due to the accumulation of inflammatory fluid.
Destruction of cartilage and bone, leading to joint damage and deformity.
Understanding these processes is essential for developing effective treatment strategies. By targeting the autoimmune nature and inflammatory processes, we can work towards better management and potentially remission of the disease.
Epidemiology of RA: Global and U.S. Statistics
To grasp the extent of rheumatoid arthritis, we must look at global and regional data. RA is a chronic autoimmune disorder affecting millions worldwide. It causes significant pain and impacts daily life.
RA’s global prevalence is around 0.5% to 1% of adults. This means a large number of people are affected, showing the need for awareness and effective treatments.
Worldwide Prevalence Rates
Research indicates that RA’s prevalence is similar across different populations, from 0.5% to 1% of adults. This consistency highlights the importance of global health efforts to tackle RA.
Genetic predisposition, environmental triggers, and lifestyle play roles in RA development. Understanding these factors is key to creating effective interventions.
U.S. Population Impact
In the U.S., RA affects about 1.3 million people, or 0.6% to 1% of the population. This large number stresses the need for effective healthcare strategies for RA management.
The economic and social impact of RA in the U.S. is significant. It includes healthcare costs, lost productivity, and reduced quality of life.
Increasing Incidence Trends Over 32 Years
Studies reveal that RA’s incidence has been rising over the last few decades. This trend is seen globally and in the U.S., pointing to the need for ongoing research into RA causes and treatments.
Understanding RA’s epidemiology is vital for healthcare providers, policymakers, and patients. By examining global and regional data, we can tackle the challenges RA poses more effectively.
Gender Disparities in RA Diagnosis
Gender is key in diagnosing rheumatoid arthritis (RA), with women more at risk than men. This difference is seen in many studies. We will look into why this happens and what it means.
Female-to-Male Ratio Analysis
The female-to-male ratio in RA is about 3:1. This means women are three times more likely to get RA than men. This ratio is seen in different groups and studies.
Understanding this ratio is key for doctors and patients. It helps spot risk factors and guide treatments.
Lifetime Risk Differences
Women and men have different lifetime risks of getting RA. Women face a 3.6% risk, while men face a 1.7% risk. This shows a big gender gap in RA risk.
These numbers are vital for making healthcare providers and the public aware of the higher risk women have.
Hormonal Factors in RA Development
Hormones are thought to affect RA development, mainly in women. Changes in hormone levels, like during pregnancy and menopause, can change RA symptoms and when it starts.
Research on how hormones affect RA is ongoing. Learning more about this could help in managing and treating RA better.
Clinical Presentation and Symptoms of RA
RA symptoms can differ from person to person. They often include joint pain and swelling, morning stiffness, and feeling very tired. Knowing these symptoms is key to catching RA early and managing it well.
Joint Pain and Swelling Patterns
RA is known for causing pain and swelling in joints. These symptoms usually show up in a symmetrical way. For example, if one hand hurts, the other hand might too.
The joints most often hit by RA are in the hands, feet, wrists, and knees. This pain and swelling can really limit a person’s ability to move if not treated early.
Morning Stiffness and Fatigue
Waking up stiff for more than an hour is a big sign of RA. This stiffness makes it hard to do everyday things. Many people with RA also feel very tired, which can really lower their quality of life.
It’s very important to tackle morning stiffness and tiredness in RA patients. This can be done through medicine, changing how you live, and other treatments.
Symmetrical Joint Involvement
RA is special because it affects joints in a symmetrical way. This is different from other types of arthritis, like osteoarthritis, which can hit joints in a more random or one-sided way.
Symptom | Description | Impact on Patient |
|---|---|---|
Joint Pain and Swelling | Typically symmetrical, affecting small joints | Significant disability if not managed |
Morning Stiffness | Lasting more than an hour | Impacts daily activities |
Fatigue | Debilitating and persistent | Affects overall quality of life |
Understanding RA’s symptoms helps doctors diagnose and treat it better. This leads to better outcomes for patients.
Commonly Affected Joints in Rheumatoid Arthritis
Knowing which joints RA affects is key for diagnosis and treatment. Rheumatoid arthritis is a disease that attacks the joints, causing pain and damage. It leads to inflammation and can harm the joints severely.
RA often targets specific areas of the body. The way it affects joints can help doctors diagnose RA. This helps them tell it apart from other types of arthritis.
Small Joints of Hands and Feet
The small joints in hands and feet are usually the first to get hit by RA. This includes the MCPs and PIPs in hands and the MTPs in feet.
These joints get inflamed, causing pain, swelling, and stiffness. This is worse after rest or inactivity. Over time, it can lead to deformities and make it hard to use hands and feet.
Wrist and Ankle Involvement
RA also hits the wrists and ankles. Wrist problems can cause pain and make it hard to move. Ankle issues can make walking painful.
The inflammation in these areas can make them tender and swollen. This makes daily tasks tough.
Larger Joint Manifestations
RA can also affect bigger joints like knees, hips, shoulders, and elbows. These problems can cause a lot of pain and limit how you can move.
Some people get these problems early, while others get them later. Knees are often affected, leading to pain, stiffness, and less mobility.
Joint Area | Common Symptoms | Potential Complications |
|---|---|---|
Small Joints of Hands and Feet | Pain, Swelling, Stiffness | Deformities, Functional Impairment |
Wrist and Ankle | Pain, Reduced Mobility, Swelling | Tenderness, Difficulty with Daily Activities |
Larger Joints (Knees, Hips, Shoulders, Elbows) | Pain, Stiffness, Reduced Mobility | Significant Functional Limitations |
RA can hit many joints, from small ones in hands and feet to bigger ones like knees and hips. Knowing which joints are affected is key for diagnosing and treating RA.
“Early diagnosis and treatment of RA are critical to preventing long-term joint damage and improving patient outcomes.”
– Expert in Rheumatology
Diagnostic Criteria for RA
Diagnosing rheumatoid arthritis (RA) is a detailed process. It involves clinical checks, lab tests, and imaging studies. This thorough approach is key to accurately identify RA and differentiate it from other arthritis types.
ACR/EULAR Classification Criteria
In 2010, the American College of Rheumatology (ACR) and the European League Against Rheumatism (EULAR) set new RA classification criteria. These criteria help spot RA early and accurately. They look at joint involvement, blood tests, inflammation markers, and symptom duration. A score of 6 or more out of 10 means a person has RA.
The ACR/EULAR criteria have greatly improved RA detection. Early diagnosis is critical for starting treatments that slow the disease and improve outcomes.
Laboratory Tests for Diagnosis
Laboratory tests are essential in diagnosing RA. The main tests include:
Rheumatoid factor (RF): Found in 70-80% of RA patients, but also in other conditions.
Anti-citrullinated protein antibody (anti-CCP): More specific for RA, found in 60-70% of patients.
Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP): Indicate inflammation, often high in RA.
These tests help confirm RA and measure inflammation levels. It’s important to note that no single test is definitive for RA. Diagnosis relies on clinical findings, patient history, and lab results together.
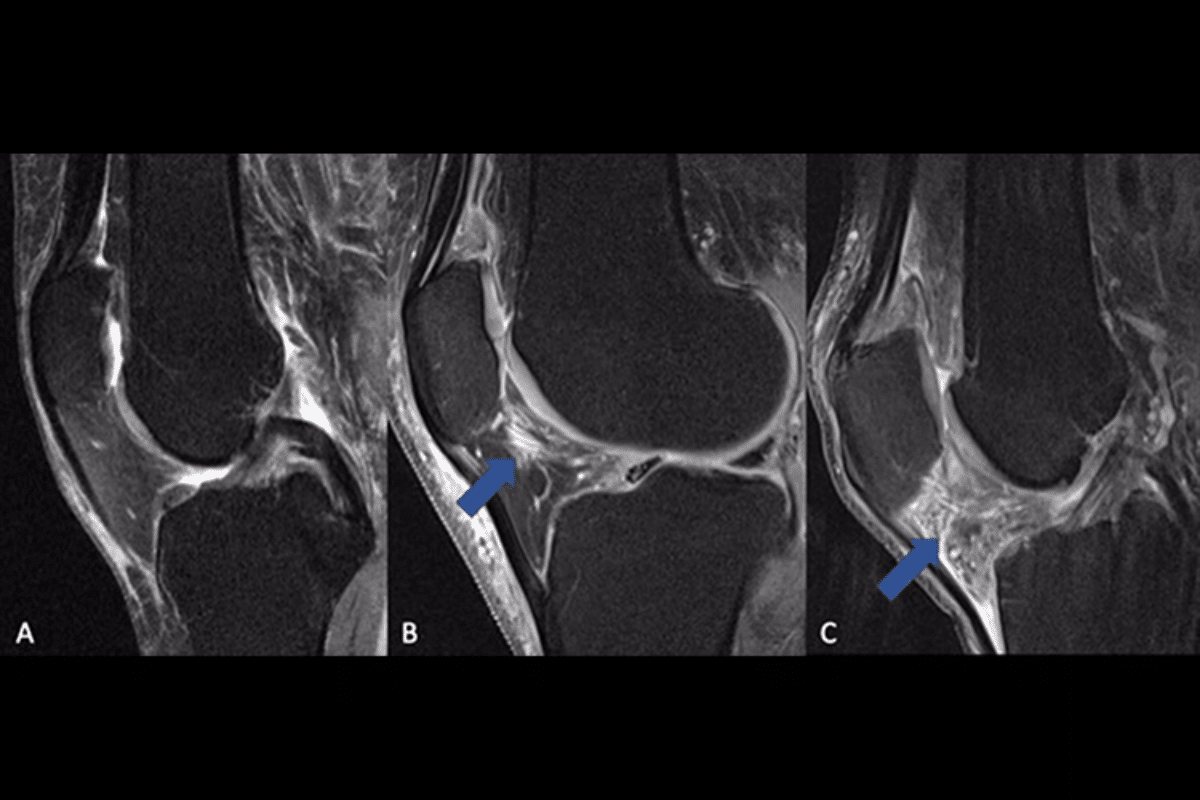
Imaging Studies in RA Assessment
Imaging studies are vital for checking joint damage and tracking RA progression. The main imaging tools are:
X-rays: Show joint erosions and joint space narrowing.
Ultrasound: Better than X-rays for spotting early erosions and inflammation.
Magnetic Resonance Imaging (MRI): Offers detailed views of soft tissues and early RA changes.
Imaging helps in diagnosing and monitoring treatment success. It also catches complications early. Regular imaging helps guide treatment and improves patient care.
Progression and Complications of Untreated RA
If RA is not treated, it can cause serious problems. RA is a chronic disease that mainly affects the joints. It leads to inflammation, pain, and damage to the joints.
As RA gets worse, it can lead to many complications. These can greatly affect a person’s life. We will look at joint damage, disability, and other systemic issues.
Joint Deformities and Erosions
Untreated RA can cause joint deformities and erosions. The inflammation can destroy cartilage and bone. This results in:
Joint misalignment
Bone erosions
Deformities, such as swan neck or boutonniere deformity in the fingers
These changes can cause chronic pain and limit joint function. This makes everyday tasks hard.
Disability and Functional Limitations
As RA gets worse, patients may lose more ability to function. The inflammation and damage can lead to:
Reduced range of motion
Decreased grip strength
Difficulty with daily activities, such as dressing or grooming
This disability can greatly affect a person’s independence and well-being.
Systemic Complications
RA is not just a joint disease; it can affect the whole body. Untreated RA can increase the risk of:
Cardiovascular disease
Osteoporosis
Infections
Other autoimmune disorders
These complications show why early treatment is so important. It helps prevent long-term damage.
In conclusion, untreated RA can lead to severe joint damage, disability, and systemic complications. Early treatment is key to prevent these problems. It helps improve the quality of life for those with RA.
Modern Treatment Approaches for RA
Modern treatments for RA have changed how we manage this chronic condition. We now have many tools to fight RA. These tools help reduce inflammation, slow the disease, and improve life quality.
Disease-Modifying Antirheumatic Drugs (DMARDs)
DMARDs are key in treating RA. They change how the disease works, slowing it down or stopping it. There are two main types:
- Synthetic DMARDs: These are traditional DMARDs, with methotrexate being the most used. Others include sulfasalazine, hydroxychloroquine, and leflunomide.
- Targeted DMARDs: Also known as biologic DMARDs, these target specific molecules in inflammation.
DMARDs are often started early to prevent joint damage and improve long-term results.
Biological Therapies
Biological therapies, or biologic DMARDs, have changed RA treatment. They target specific parts of the immune system causing inflammation and damage. Common ones include:
Tumor Necrosis Factor (TNF) inhibitors, such as etanercept and adalimumab
Interleukin-6 (IL-6) inhibitors, like tocilizumab
B cell-targeting therapies, including rituximab
Biological therapies are often used with synthetic DMARDs, like methotrexate, to work better.
Emerging Treatment Options
Research into RA treatment keeps evolving, with new options showing promise:
- Janus Kinase (JAK) inhibitors: Oral drugs that block certain inflammatory pathways.
- Stem cell therapies: New treatments trying to repair or replace damaged tissues.
- Personalized medicine approaches: Tailoring treatment to each patient based on genetic and biomarker profiles.
These new treatments offer hope for better RA management and outcomes.
Managing RA needs a mix of medication, lifestyle changes, and ongoing care. By keeping up with the latest treatments, patients and doctors can create the best plan together.
Living with RA: Management Strategies
Living with RA can be tough, but the right strategies can make a big difference. It’s not just about medical treatment. A full approach is needed.
Physical Therapy and Exercise
Physical therapy is key in managing RA. It keeps joints moving, strengthens muscles, and boosts function. Yoga and swimming are great because they’re easy on the body and fit all fitness levels.
Staying active helps control RA symptoms and boosts overall health. It’s important to create an exercise plan with a healthcare expert. This plan should match your health and abilities.
Lifestyle Modifications and Diet
Making lifestyle changes is vital in managing RA. Keeping a healthy weight eases joint stress. Eating foods that fight inflammation is also helpful. Omega-3 rich foods like salmon and flaxseeds are good choices.
Quitting smoking and drinking less alcohol can also help. These habits can make RA symptoms worse. Stress-reducing activities like meditation and deep breathing are also beneficial.
Assistive Devices and Accommodations
Using assistive devices and making home changes can greatly help. Simple tools like jar openers and ergonomic utensils can make daily tasks easier.
Changing your home to ease joint strain is also smart. Installing grab bars, using raised toilet seats, and keeping things within reach are good ideas.
By using these strategies, people with RA can manage their symptoms better. This helps them live a better life.
Conclusion: Understanding the Impact of RA
Rheumatoid Arthritis (RA) is a chronic disease that affects many people. It causes inflammation and is an autoimmune disease. We’ve looked at its symptoms, diagnosis, treatment, and how to manage it.
Knowing about RA is key to managing it well. The term for Rheumatoid Arthritis is used a lot in healthcare. Being aware of it can help patients get better care.
RA doesn’t just affect one person; it impacts families and communities too. We need more research and awareness to tackle this disease. This will help find better treatments.
By understanding RA and its effects, we can improve care and treatment. This will make a big difference in the lives of those with RA.
FAQ
What does RA stand for in medical terms?
RA stands for Rheumatoid Arthritis. It’s a chronic disease that causes inflammation and affects joints and other parts of the body.
What is the medical abbreviation for Rheumatoid Arthritis?
The medical term for Rheumatoid Arthritis is RA.
Why is RA the standard abbreviation used for Rheumatoid Arthritis?
RA is widely recognized by healthcare professionals. It makes communication easier and more efficient.
What are the common symptoms of Rheumatoid Arthritis?
Symptoms include joint pain, swelling, and morning stiffness. Fatigue and symmetrical joint involvement are also common.
Which joints are commonly affected by Rheumatoid Arthritis?
RA often affects small joints in the hands and feet. It also impacts wrists, ankles, and larger joints like knees and elbows.
How is Rheumatoid Arthritis diagnosed?
Diagnosis uses the ACR/EULAR criteria and lab tests like rheumatoid factor. Imaging studies like X-rays and ultrasound are also used.
What are the possible complications of untreated Rheumatoid Arthritis?
Untreated RA can cause joint deformities and erosions. It can lead to disability and systemic issues like heart disease and osteoporosis.
What are the modern treatment approaches for Rheumatoid Arthritis?
Modern treatments include DMARDs and biological therapies. New options like JAK inhibitors are also being explored.
How can Rheumatoid Arthritis be managed?
Management involves physical therapy, exercise, and lifestyle changes. Diet adjustments and using assistive devices can also improve quality of life.
What is the prevalence of Rheumatoid Arthritis worldwide?
RA affects about 0.5 to 1% of adults globally. Prevalence varies by region.
Are there any gender disparities in RA diagnosis?
Yes, RA is more common in women. The female-to-male ratio is about 3:1, with women having a higher lifetime risk.
References
https://www.ncbi.nlm.nih.gov/books/NBK441999




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News




























