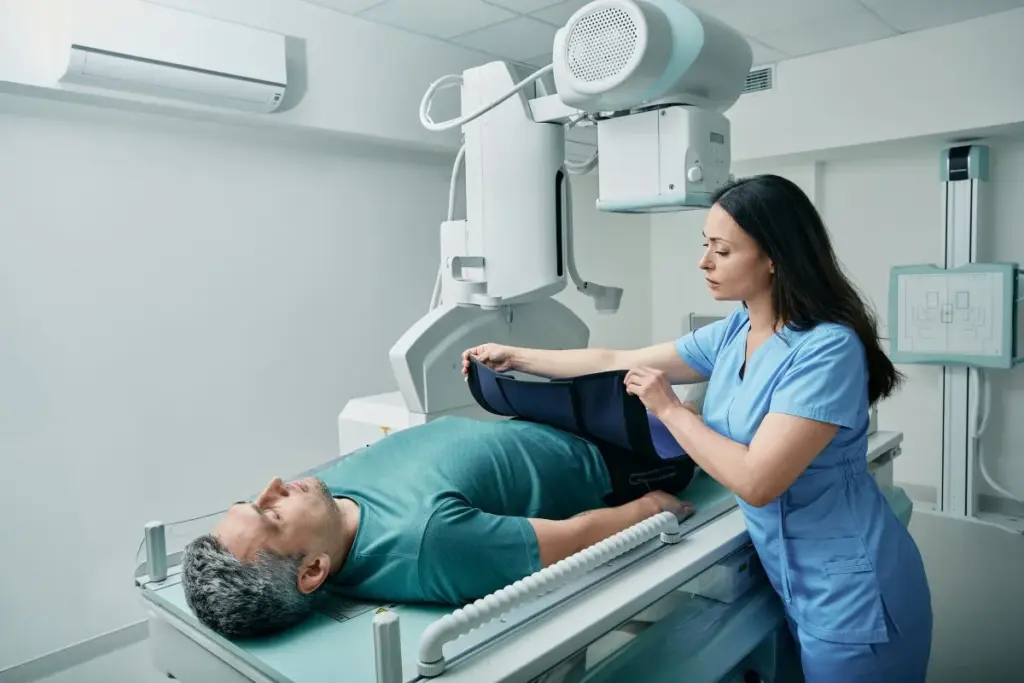
Interventional radiology nurses are key players in high-tech procedures. They work close to patients and fluoroscopic equipment. This raises concerns about their radiation exposure.
Occupational exposure is a big worry in medical settings, like interventional radiology. The International Commission on Radiological Protection says medical radiation exposure is when people get exposed during their own treatment.
Research shows that interventional radiology nurses do get exposed to radiation. But, thanks to proper protection, their exposure stays well under safety limits.
Key Takeaways
- Interventional radiology nurses are exposed to radiation during procedures.
- Proper protection measures are key to keep exposure low.
- Exposure levels for nurses are usually below safety limits.
- It’s vital to know the risks and safety steps for nurse safety.
- Top hospitals use many ways to protect their staff.
The Role of Nurses in Interventional Radiology
Nurses in interventional radiology do a lot, from caring for patients to handling equipment. They are key to the success of these precise procedures. These tasks need teamwork and careful planning.
Defining Interventional Radiology Procedures
Interventional radiology uses small, non-invasive methods guided by imaging like fluoroscopy. These can include fixing blood vessels or taking tissue samples. Each step needs great care and precision.
Fluoroscopy is a big part of this field, showing images in real-time. This helps doctors navigate the body’s structures. Nurses must know how to use this tech and keep radiation levels low.
Nurse Responsibilities During Fluoroscopic Procedures

Nurses are vital during these procedures. They help get patients ready, watch their health, and manage the equipment. Their tasks include:
- Keeping patients comfortable and safe
- Helping doctors with the equipment
- Watching patient health and readying for emergencies
Good communication among nurses, doctors, and the team is key for success.
Proximity to Radiation Sources During Patient Care
Nurses often stand close to radiation, like fluoroscopy. This can expose them to radiation. It’s important for them to know how to stay safe.
|
Radiation Safety Measure |
Description |
|---|---|
|
Personal Protective Equipment (PPE) |
Lead aprons, thyroid shields, and protective eyewear |
|
Distance Management |
Maintaining a safe distance from radiation sources |
|
Time Management |
Minimizing exposure time |
By using these safety steps, nurses can reduce their exposure. They can keep giving top-notch care to patients.
Understanding Radiation Exposure in Medical Settings
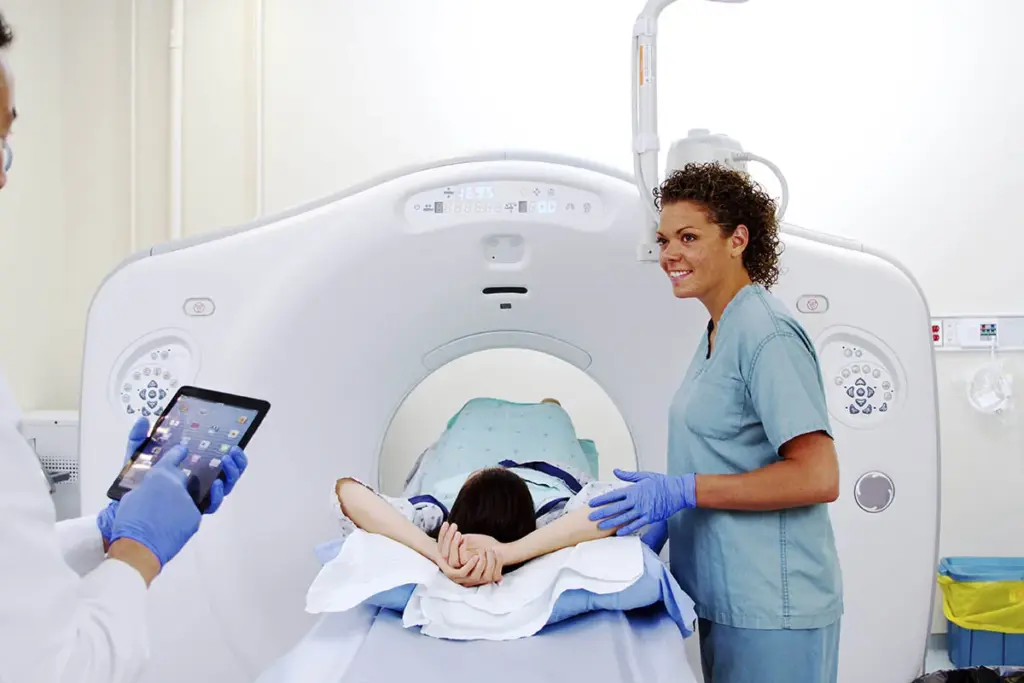
Interventional radiology uses different types of radiation. This affects both patients and medical staff. It’s key to know about radiation exposure to reduce risks.
Types of Radiation in Interventional Procedures
In interventional radiology, ionizing radiation is used. It has enough energy to remove electrons from atoms, creating ions. We use it in procedures like angiography and embolization for real-time imaging.
The main types of radiation are:
- X-rays: Used for imaging during procedures.
- Gamma rays: Used in some specific procedures.
Primary vs. Scattered Radiation
It’s important to know the difference between primary and scattered radiation. Primary radiation comes directly from the X-ray tube. Scattered radiation happens when the primary beam hits the patient’s body or objects.
Scattered radiation is a big risk for medical staff. It spreads out and can expose people nearby.
Factors Affecting Exposure Intensity
The intensity of radiation exposure depends on several things:
|
Factor |
Description |
Impact on Exposure |
|---|---|---|
|
Procedure Type |
Different procedures need different imaging. |
Affects how long and how intense the radiation is used. |
|
Equipment Used |
Modern equipment helps reduce radiation exposure. |
Can greatly lower exposure levels. |
|
Distance from Radiation Source |
How close staff are to the patient and X-ray tube. |
Exposure goes down with more distance. |
Knowing these factors helps us find ways to lower radiation exposure. This way, we can keep the high quality of care in interventional radiology.
Measuring Occupational Radiation Exposure
Measuring radiation exposure at work is very important in medical settings. It helps us know the risks and take safety steps.
Units of Measurement: mSv and Dose Equivalents
Radiation exposure is measured in millisieverts (mSv) or dose equivalents. The sievert (Sv) is the SI unit for dose equivalent. It shows the biological effect of radiation. One millisievert is one-thousandth of a sievert.
Dose equivalents consider the different effects of radiation types. This gives a better idea of the harm caused by radiation.
Understanding dose equivalents is key. It helps healthcare workers see the risk of different radiation types. For example, alpha particles are more harmful than gamma rays at the same dose.
Personal Dosimetry Methods
Personal dosimetry tracks an individual’s radiation exposure. The most common method uses a dosimeter, a device worn by workers. Dosimeters can be film badges, thermoluminescent dosimeters (TLDs), or electronic personal dosimeters (EPDs).
- Film badges darken with radiation exposure.
- TLDs measure exposure by heating a material and detecting light.
- EPDs show radiation dose in real-time and alert workers.
Interpreting Exposure Readings
It’s important to understand dosimeter readings to keep exposure safe. Regular checks help spot trends or spikes in exposure. This allows for quick action.
Readings are tracked over time to meet safety limits.
|
Dosimeter Type |
Measurement Method |
Advantages |
|---|---|---|
|
Film Badge |
Photographic film darkening |
Low cost, simple to use |
|
TLD |
Thermoluminescence |
High accuracy, reusable |
|
EPD |
Real-time electronic measurement |
Immediate feedback, alert system |
By accurately measuring radiation exposure, healthcare places can protect their staff better. Strong dosimetry programs are essential for a safe work environment for interventional radiology nurses.
Current Research on Nurse Radiation Exposure Levels
Recent studies have shed light on the levels of radiation exposure among nurses working in interventional radiology. We will examine the findings of these studies to understand the current state of knowledge on this topic.
The 2013 Study: 1.34 mSv/y Mean Effective Dose
A significant study conducted in 2013 investigated the radiation exposure levels among nurses in interventional radiology settings. The research found a mean effective dose of 1.34 mSv per year among the nurses studied. This information provides a baseline understanding of the average radiation exposure for nurses in this field.
Key findings from the 2013 study include:
- A mean effective dose of 1.34 mSv/y, indicating the average annual exposure.
- Variability in exposure levels based on factors such as procedure type and nurse role.
- The importance of proper protective measures in minimizing exposure.
Per-Procedure Exposure Rates (0.03-1.16 mSv)
The same research also examined per-procedure exposure rates, finding a range from 0.03 to 1.16 mSv. These rates highlight the variability in radiation exposure depending on the specific procedure being performed.
The factors influencing per-procedure exposure include:
- The type of interventional radiology procedure.
- The nurse’s proximity to the radiation source.
- The use and quality of protective shielding.
Cumulative Exposure in High-Volume Settings
Cumulative exposure is a critical concern in high-volume settings where nurses perform or assist in numerous procedures. The research indicates that while individual per-procedure exposure may be low, the cumulative effect over time can be significant.
For illustration, the following table provides an overview of the exposure levels.
|
Procedure Volume |
Average Annual Exposure (mSv) |
Cumulative Exposure Over 5 Years (mSv) |
|---|---|---|
|
Low |
0.5 |
2.5 |
|
Medium |
1.0 |
5.0 |
|
High |
2.0 |
10.0 |
Studies have shown that with proper protection, radiation exposure levels among nurses remain below safety limits. Ongoing research and adherence to safety protocols are key to maintaining a safe working environment.
International Safety Standards and Exposure Limits
International safety standards are key to protecting healthcare workers from radiation. They aim to reduce risks without harming medical care.
The Occupational Exposure Limit
The limit for radiation exposure is a vital part of these standards. It’s set at 50 mSv/y by regulatory bodies. This ensures workers aren’t exposed to dangerous levels of radiation yearly.
Regulatory Bodies and Their Guidelines
Many groups help set these safety standards. The International Commission on Radiological Protection (ICRP) is one. They offer guidelines for healthcare facilities around the world.
These guidelines cover important areas like protective gear, shielding, and safe practices.
Implementing Safety Standards in Hospitals
Hospitals like follow these standards closely. They have strict safety rules. This includes training staff, using dosimeters, and keeping equipment in top shape.
By following these standards, hospitals make their workplaces safer. They can also keep providing top-notch care to patients.
Health Risks Associated with Radiation Exposure
Understanding the health risks associated with radiation is crucial for interventional radiology nurses. Exposure can cause many health problems, from immediate effects to long-term issues.
Short-Term vs. Long-Term Effects
Radiation can cause both quick and delayed health problems. Quick effects might include skin burns or acute radiation syndrome. Long-term effects can show up years later and may increase cancer and disease risks.
We need to think about these risks to keep nurses safe. The long-term effects are scary because they can affect a nurse’s life and career.
Tissue-Specific Risks: Eyes, Thyroid, and Bone Marrow
Some tissues are more likely to be damaged by radiation. For example, the eyes can get cataracts, which can hurt your vision. The thyroid gland is also at risk for thyroid cancer. Bone marrow, which makes blood cells, can get damaged too, leading to leukemia.
Cancer and Non-Cancer Risks
Getting cancer is a big worry for people exposed to radiation. The type of cancer depends on how much and for how long they were exposed. Other risks include heart disease, brain problems, and more, which can affect a nurse’s life and how long they live.
To understand these risks better, let’s look at them in a clear way:
|
Health Risk |
Description |
Exposure Impact |
|---|---|---|
|
Cataracts |
Vision impairment due to lens damage |
High risk for eye exposure |
|
Thyroid Cancer |
Increased risk of thyroid malignancy |
Moderate risk with thyroid exposure |
|
Leukemia |
Bone marrow cancer affecting blood cells |
High risk with significant bone marrow exposure |
Knowing these health risks helps us protect interventional radiology nurses from radiation harm. We must follow safety rules and keep educating nurses to reduce these risks.
Radiation Protection Strategies for Interventional Nurses
To reduce radiation risks, interventional nurses need strong protection plans. Good radiation protection is key for keeping nurses and patients safe during procedures.
Essential Protective Equipment
Personal protective equipment (PPE) is vital in lowering radiation exposure. Lead aprons, thyroid shields, and lead glasses are must-haves for nurses. It’s important to check this gear often for any damage.
Structural Shielding Options
Structural shielding is also key in protecting against radiation. Lead-lined walls, ceilings, and floors in procedure rooms keep radiation in. Mobile shielding, like lead screens, adds extra protection during procedures.
Distance and Time Management Techniques
Managing distance and time is critical in radiation protection. Being farther from the radiation source lowers exposure. We should also spend less time near the source. Planning and efficient workflow help achieve this.
Implementing these strategies is essential to reducing radiation risks for interventional nurses. It’s our duty to stay safe and equipped with the right knowledge and tools.
The ALARA Principle in Nursing Practice
The ALARA principle is key in our fight against radiation in interventional radiology nursing. ALARA stands for “As Low As Reasonably Achievable.” It’s more than a rule; it’s a promise to cut down radiation for patients and nurses.
Exploring the ALARA principle, we see its core parts and how they shape our work. The principle aims to keep radiation exposure low, considering costs and society.
Defining “As Low As Reasonably Achievable”
The phrase “As Low As Reasonably Achievable” might seem simple, but it’s complex. It’s about finding a balance between good images and low radiation. A top radiation safety expert says,
“The ALARA principle is not just about reducing radiation doses, but about achieving a balance between image quality and radiation safety.”
This balance is key in our daily tasks. We must choose wisely to protect patients and ourselves.
Balancing Patient Care and Self-Protection
Applying the ALARA principle is tough. We need to care for patients well while keeping ourselves safe from radiation. We must watch our distance from radiation, how long we’re exposed, and use protective gear.
By using shields, staying far from radiation, and shortening procedures, we cut our exposure a lot. For example, using a lead apron and thyroid shield can cut exposure by up to 90%.
Practical Implementation in Daily Work
Putting the ALARA principle into action takes education, training, and following rules. We must keep up with new safety guidelines and tech.
Here are some steps we can take:
- Regularly review and update our knowledge of radiation safety rules
- Use personal dosimeters to track our radiation levels
- Work smarter to reduce exposure time and distance from radiation
By teaming up and sticking to the ALARA principle, we make a safer place for patients and ourselves.
Monitoring and Documentation Requirements
Keeping track of radiation exposure is key in interventional radiology. It’s not just about safety; it’s also about following the rules.
Types of Dosimeters and Their Proper Placement
Dosimeters help measure how much radiation we get. There are different kinds, like:
- Thermoluminescent dosimeters (TLDs)
- Optically stimulated luminescence (OSL) dosimeters
- Electronic personal dosimeters (EPDs)
Where we wear dosimeters matters for getting right readings. They go outside the lead apron, at the collar, to track thyroid and head exposure.
Record-Keeping and Exposure Tracking
Keeping good records of radiation exposure is important. It helps us see trends and find ways to get better. We track each nurse’s exposure to:
- See how much they’ve been exposed over time
- Find out which procedures or practices are riskier
- Make changes to lower exposure
By looking at these records, we can make our safety plans better. This ensures we meet safety standards.
Responding to Elevated Exposure Readings
If exposure readings go up, we investigate why. This might mean:
- Looking at how we do procedures
- Checking if we’re using enough protective gear
- Seeing if we need more training or to change how we do things
We aim to cut down on exposure without sacrificing patient care.
By carefully watching, recording, and acting on radiation data, we make a safer place for interventional radiology nurses to work.
Special Considerations for High-Risk Procedures
We know that some interventional radiology procedures are riskier for radiation. We plan and execute them carefully to keep patients and staff safe.
Some procedures are more complex and risky. These include work in cardiac catheterization labs, neurointerventional procedures, and emergency cases.
Cardiac Catheterization Laboratories
Cardiac catheterization labs are very risky for radiation. Procedures like coronary angiography and PCI use a lot of radiation and take a long time.
- Key Considerations:
- Use low-dose fluoroscopy when you can.
- Position patients to reduce radiation scatter.
- Use protective gear like lead aprons and thyroid shields.
Neurointerventional Procedures
Neurointerventional procedures, like stroke and aneurysm treatments, also have high radiation risks. They often need a lot of fluoroscopy time.
Mitigation Strategies: Use real-time dose monitoring and pulsed fluoroscopy. Try to reduce the number of exposures.
Emergency Interventional Radiology
Emergency procedures are urgent and risky for radiation. They often don’t allow for full safety protocols.
Training staff well and having emergency plans can help lower risks.
Understanding the challenges of high-risk procedures helps us take steps to reduce radiation risks. This keeps both staff and patients safe.
Institutional Responsibilities for Staff Safety
Healthcare institutions must protect their staff from radiation. This is not just a moral duty but also a legal one.
Ongoing Education and Training Programs
One key responsibility is providing ongoing education and training. These programs should teach the latest in radiation safety and how to use protective gear.
We think continuous learning is key for a safe work place. Our programs aim to give staff the knowledge to reduce radiation exposure.
|
Training Program |
Description |
Frequency |
|---|---|---|
|
Radiation Safety Basics |
Introduction to radiation safety principles and practices |
Annual |
|
Advanced Radiation Protection |
In-depth training on radiation protection techniques and equipment |
Bi-Annual |
|
Emergency Response Training |
Training on responding to radiation emergencies and incidents |
Quarterly |
Equipment Maintenance and Quality Control
Keeping radiation equipment in good shape is vital for staff safety. This means regular checks on imaging tools, protective gear, and dosimeters.
We make equipment maintenance a top priority to avoid malfunctions and ensure safety features work right.
Creating a Culture of Radiation Safety
Building a culture of radiation safety goes beyond just following rules. It needs a real commitment to safety from everyone in the organization.
We build a safety culture by encouraging open talk, letting staff report safety issues, and rewarding safe behavior.
- Promoting awareness about radiation safety
- Encouraging adherence to safety protocols
- Providing resources for safe working practices
Together, we can make a safe and healthy work space for our interventional radiology staff.
Future Trends in Minimizing Radiation Exposure
The future of interventional radiology is bright, thanks to new ways to cut down on radiation. This is good news for patients and medical staff. New trends are on the horizon, aiming to lower radiation exposure even more.
Technological Advancements in Imaging Equipment
New imaging equipment is being made with less radiation in mind. It has cool features like:
- Advanced pulse fluoroscopy
- Improved detector technology
- Enhanced image processing algorithms
- Real-time dose modulation
These updates help doctors get clear images while using less radiation. For example, advanced detector technology makes images better at lower doses. And real-time dose modulation adjusts radiation as needed.
Innovative Protective Gear Development
New protective gear for medical staff is also being developed. It’s designed to be better without making staff uncomfortable. Some examples include:
|
Protective Gear |
Features |
Benefits |
|---|---|---|
|
Lightweight Lead Aprons |
Reduced weight, enhanced flexibility |
Less fatigue for staff, improved mobility |
|
Thyroid Shields with Enhanced Protection |
Higher lead equivalence, better fit |
Increased protection for sensitive areas |
|
Radiation-Protective Gloves |
Improved dexterity, tactile sensitivity |
Better performance during procedures |
Procedural Modifications and Automation
There’s also a push to change procedures to use less radiation. This includes:
- Optimizing procedural protocols to minimize fluoroscopy time
- Using alternative imaging modalities when possible
- Implementing automated systems for dose tracking and management
By combining these efforts, we can greatly reduce radiation exposure. As these trends grow, we’ll see even better ways to protect everyone from radiation.
Conclusion
Interventional radiology nurses play a critical role in medical procedures but are exposed to various radiation risks. Studies show that with the right protection, their exposure stays safe. This is good news for their health.
This discussion has covered how nurses manage radiation exposure in their professional roles. We’ve also covered how to keep their exposure low. The International Commission on Radiological Protection sets safe dose limits. Personal dosimeters help track how much radiation nurses get.
For more on keeping nurses safe from radiation, check out the . By following the ALARA principle and using protective gear, we can reduce radiation risks. It’s our duty to make sure nurses have what they need to work safely.
FAQ
What is the primary source of radiation exposure for interventional radiology nurses?
The main source of radiation for nurses is scattered radiation from patients during fluoroscopic procedures.
How is occupational radiation exposure measured?
Occupational radiation exposure is tracked with personal dosimeters. These devices measure the dose equivalent in millisieverts (mSv).
What are the recommended exposure limits for occupational radiation exposure?
The limit for occupational exposure is 50 mSv per year. This is set by bodies like the International Commission on Radiological Protection (ICRP).
What are the health risks associated with radiation exposure for interventional radiology nurses?
Nurses face health risks like radiation-induced cataracts and cancer. These risks include thyroid cancer and leukemia.
What radiation protection strategies can interventional radiology nurses use?
Nurses can use lead aprons and thyroid shields for protection. They also use structural shielding and manage distance and time to reduce exposure.
What is the ALARA principle, and how is it applied in nursing practice?
The ALARA principle aims to minimize radiation exposure. Nurses apply it by balancing patient care with self-protection. They use strategies like shortening fluoroscopy time and staying far from radiation sources.
How can hospitals ensure a culture of radiation safety for their staff?
Hospitals can foster a culture of safety through education and training. They should also maintain equipment and promote safety among staff.
What are some future trends in minimizing radiation exposure for interventional radiology nurses?
Future trends include new imaging technology and protective gear. There will also be procedural changes and automation to lower exposure.
Why is monitoring and documentation important in radiation safety?
Monitoring and documentation are key for tracking exposure levels. They help identify areas for improvement and guide actions to reduce risks.
What are some special considerations for high-risk procedures?
High-risk procedures need extra protection measures. Nurses must plan carefully to minimize exposure risks during these procedures.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC3298647/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























