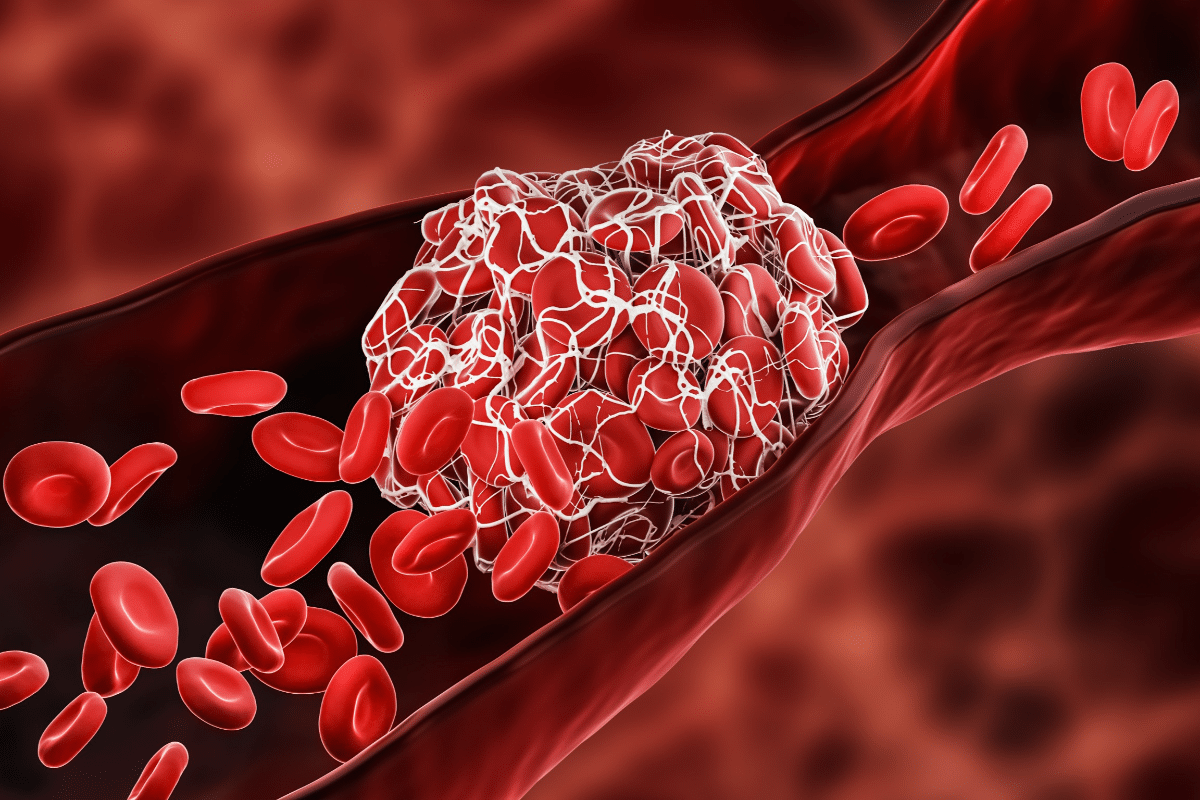
We are here to help you understand allergic vasculitis. It’s a condition where small blood vessels get inflamed. This usually happens because of an allergic reaction to medicines, infections, or other things.
This condition is also known as hypersensitivity vasculitis or cutaneous leukocytoclastic vasculitis. It shows up as red or purple spots on the skin. These spots can appear just days after being exposed to something that triggers it.
It’s very important to spot the early signs of this condition. This is because getting a diagnosis and treatment early can stop things from getting worse. It helps both patients and doctors to take action and avoid serious problems.
Key Takeaways
- Allergic vasculitis is a type of vasculitis that occurs due to an allergic reaction.
- It is characterized by inflammation of small blood vessels.
- Symptoms include red or purple raised spots on the skin.
- Timely diagnosis and treatment are key to prevent complications.
- Understanding the condition empowers patients and healthcare providers.
What Is Allergic Vasculitis?
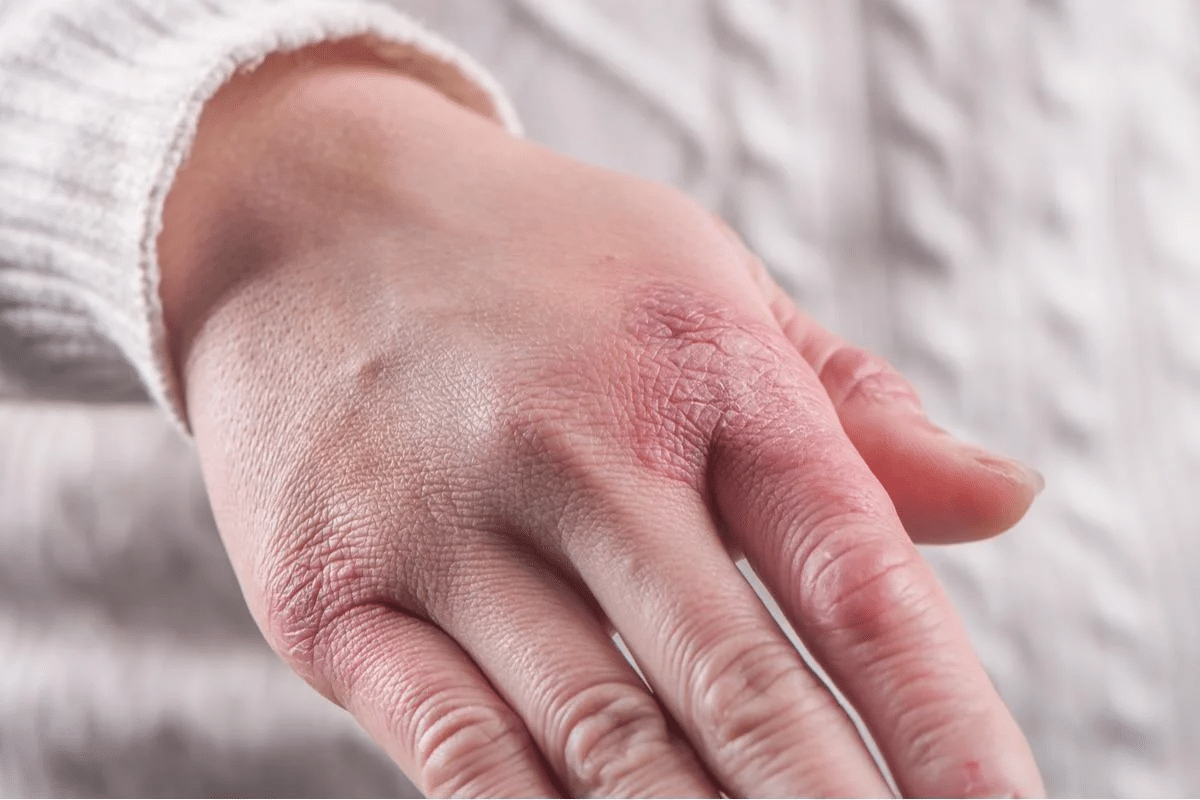
Allergic vasculitis is a specific type of vasculitis linked to hypersensitivity reactions. It’s also known as hypersensitivity vasculitis. This condition causes inflammation in small blood vessels. It’s a complex disorder that damages blood vessel walls due to an immune response.
Definition and Classification
Allergic vasculitis is classified as a small-vessel vasculitis. It affects small blood vessels like capillaries, venules, and arterioles. Vasculitis classification depends on vessel size, autoantibodies, and histological features.
The Chapel Hill Consensus Conference (CHCC) system places allergic vasculitis in single-organ vasculitis or vasculitis with a specific cause. This shows how complex and varied vasculitis can be.
|
Vasculitis Classification |
Vessel Size |
Characteristics |
|---|---|---|
|
Large-Vessel Vasculitis |
Aorta and its major branches |
Involves large arteries, often with granulomatous inflammation |
|
Medium-Vessel Vasculitis |
Main visceral arteries and their branches |
Affects medium-sized arteries, often with necrotizing inflammation |
|
Small-Vessel Vasculitis |
Capillaries, venules, arterioles |
Involves small vessels, often with immune complex deposition |
Relationship to Hypersensitivity Reactions
Allergic vasculitis is often caused by hypersensitivity reactions to medications, infections, or other antigens. These reactions lead to immune complex formation. These complexes deposit in small blood vessel walls, causing inflammation and damage.
“Hypersensitivity vasculitis is a term used to describe a type of vasculitis that is triggered by an immune response, often to a drug or infection.”
Small-Vessel Vasculitis Characteristics
Allergic vasculitis is marked by its impact on small blood vessels. It shows leukocytoclastic vasculitis on histopathology, indicating neutrophil debris. Symptoms include palpable purpura, skin lesions, and sometimes systemic symptoms.
Understanding allergic vasculitis is key for diagnosis and management. We’ll explore its causes, symptoms, and treatment options further.
Common Causes and Triggers
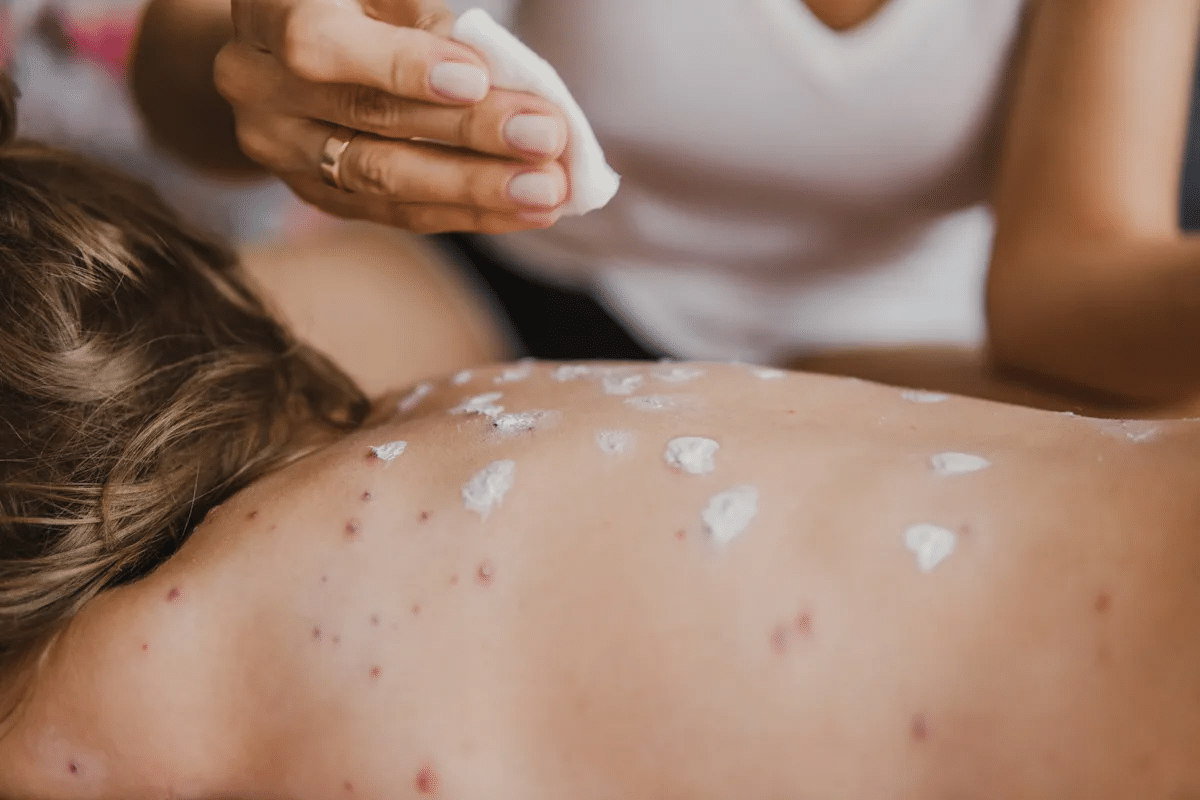
It’s important to know what causes allergic vasculitis to treat it well. This condition makes blood vessels swell. It can happen for many reasons.
Medication-Induced Reactions
Some medicines can cause allergic vasculitis. This includes antibiotics and pain relievers. If a medicine causes this, stop using it to stop more swelling.
Infection-Related Triggers
Infections can also lead to allergic vasculitis. This includes infections from bacteria, viruses, and more. It’s key to treat the infection to manage symptoms.
Idiopathic Cases: When No Cause Is Found
Sometimes, no cause is found, even after checking hard. These cases are hard to manage because there’s no clear cause. Treatment then aims to ease symptoms and prevent problems.
Knowing what causes allergic vasculitis helps doctors create better treatment plans. This is based on what each patient needs.
Recognizing Skin Manifestations of Allergic Vasculitis
It’s key to spot the skin signs of allergic vasculitis early. This condition causes blood vessel inflammation due to an allergic reaction. It mainly shows up through the skin.
Palpable Purpura: The Hallmark Sign
The main sign of allergic vasculitis is palpable purpura. It looks like raised red or purple spots on the skin. These spots can be felt when touched, which is why they’re called palpable.
Palpable purpura happens when small blood vessels get inflamed. It’s a key sign doctors look for to diagnose the condition.
Characteristics of Vasculitic Lesions
Vasculitic lesions in allergic vasculitis can look different. But they often include purpura, which can be red or purple. Sometimes, you might see erythema (redness), urticaria (hives), or even necrosis in severe cases.
These spots are usually tender. They might have a red ring around them.
Common Distribution Patterns
The spots’ location can help doctors figure out what’s going on. In allergic vasculitis, they often show up on the lower legs, around the ankles and feet. They can also appear on the buttocks and other spots.
The spots usually show up on both sides of the body and look the same. Knowing about these patterns helps doctors diagnose and treat the condition better.
Timeline and Progression of Symptoms
Knowing when allergic vasculitis symptoms show up is important for both patients and doctors. This hypersensitivity skin disorder has symptoms that follow a pattern. It’s key to understand this pattern.
Latency Period After Exposure (7-10 Days)
Symptoms of allergic vasculitis usually start 7 to 10 days after being exposed to something that triggers it. This wait is because the immune system takes time to react. It’s like the body is getting ready to fight off the antigen.
Evolution of Skin Lesions
The skin signs of allergic vasculitis often show up on the legs as red spots. At first, they might look like small, red or purple spots that hurt when touched. As time goes on, these spots can grow or merge into bigger areas.
Duration and Resolution Patterns
How long allergic vasculitis symptoms last can vary a lot. For many, the symptoms go away within weeks after the cause is removed. But for some, the symptoms can stick around or come back, needing more medical help. Knowing how symptoms resolve helps doctors and patients plan the best course of action.
Allergic Vasculitis Beyond the Skin
Allergic vasculitis can affect more than just the skin. It can also impact other organs, which is why it’s important to watch for signs. This condition mainly shows up on the skin but can spread to other parts of the body in severe cases.
Systemic Symptoms to Watch For
People with allergic vasculitis might feel fever, tiredness, and lose weight. These signs can mean the disease is spreading. It’s vital to keep an eye on these symptoms because they can show the disease is getting worse.
Organ Involvement in Severe Cases
In serious cases, allergic vasculitis can harm organs like the kidneys, joints, and stomach. This can cause problems like kidney disease, joint pain, and stomach issues. The severity of organ damage often affects how well a person will do.
|
Organ/System |
Possible Complications |
|---|---|
|
Kidneys |
Nephritis, Renal Failure |
|
Joints |
Arthritis, Joint Pain |
|
Gastrointestinal Tract |
Abdominal Pain, Gastrointestinal Bleeding |
Distinguishing Cutaneous-Only vs. Systemic Disease
Telling cutaneous-only allergic vasculitis from the systemic kind is key. Systemic cases need stronger treatments and closer checks.
For a proper diagnosis, doctors use tests and scans. This helps them create a treatment plan that fits each patient’s needs. It leads to better results for those with systemic allergic vasculitis.
Differentiating from Similar Conditions
To accurately diagnose allergic vasculitis, it’s key to tell it apart from similar conditions. Allergic vasculitis, also known as hypersensitivity vasculitis, shows symptoms that can be mixed up with other vasculitis types and skin issues.
Other Types of Vasculitis
Vasculitis is a group of diseases that cause inflammation in blood vessels. Other types of vasculitis, like Henoch-Schönlein purpura, microscopic polyangiitis, and granulomatosis with polyangiitis, can look similar to allergic vasculitis. A detailed vasculitis differential diagnosis is needed to tell them apart.
Non-Vasculitic Purpuric Rashes
Purpura can show up in many conditions not related to vasculitis, like thrombocytopenia, clotting disorders, and trauma. Non-vasculitic purpura doesn’t have the inflammation seen in allergic vasculitis. Tests and lab work help figure out the difference.
Allergic Reactions Without Vasculitis
Some allergic reactions can look like allergic vasculitis but don’t have the vasculitis. For example, urticarial rashes or drug reactions can cause purpura or petechiae without true vasculitis. Knowing the patient’s history and doing a skin biopsy can help tell these apart.
In conclusion, to tell allergic vasculitis from other conditions, a detailed approach is needed. This includes clinical checks, lab tests, and sometimes biopsies. By knowing the differences and similarities, doctors can make better diagnoses and treatment plans.
Diagnostic Process and Confirmation
Diagnosing allergic vasculitis takes a detailed approach. It includes physical exams, lab tests, and sometimes a skin biopsy. This method is key to correctly identifying the condition and differentiating it from others.
Physical Examination Findings
A thorough physical exam is the first step. Doctors look for signs like palpable purpura, which are typical of this condition. The look and where these skin lesions appear can give important clues.
Laboratory Tests and Imaging
Labs are vital in confirming the diagnosis. Tests like complete blood counts and ESR are common. Imaging might be used to see how far the condition has spread.
The Importance of Skin Biopsy
A skin biopsy is often the best way to diagnose allergic vasculitis. It lets doctors directly look at the skin, showing the inflammation in blood vessels. As one expert says,
“A skin biopsy can provide definitive evidence of vasculitis, helping to confirm the diagnosis and guide treatment decisions.”
Identifying the Underlying Trigger
After confirming the diagnosis, finding the cause is next. This might involve looking at medications, checking for infections, or doing more tests.
By using these methods, doctors can accurately diagnose allergic vasculitis. They can then create a treatment plan that meets the patient’s needs.
Treatment Approaches and Management
Treating allergic vasculitis needs a full plan. This includes getting rid of the cause and managing symptoms. Finding and removing the cause is the first step.
Removing the Triggering Agent
The first step is to stop using the thing that causes the problem. This could be a medicine, infection, or something else. Stopping it can help symptoms go away.
Medication Options for Symptom Relief
There are medicines to help with symptoms. These include:
- Antihistamines to reduce itching and discomfort
- Corticosteroids to decrease inflammation
- Nonsteroidal anti-inflammatory drugs (NSAIDs) for pain relief
Managing Severe or Persistent Cases
For serious or ongoing problems, stronger treatments might be needed. This could include:
|
Treatment |
Description |
|---|---|
|
Immunosuppressive therapy |
To reduce the immune system’s abnormal response |
|
Biologic agents |
Targeted therapy to address specific aspects of the immune response |
Follow-up and Monitoring
Regular check-ups are key to track the condition and adjust treatment. This keeps the treatment working well and catches any new problems early.
With a detailed treatment plan, we can manage allergic vasculitis well. This helps patients get better.
Conclusion: When to Seek Medical Attention
Understanding allergic vasculitis is key for quick diagnosis and treatment. We’ve covered what it is, why it happens, its symptoms, and how to treat it. It can show up as palpable purpura on the legs and make your skin very sensitive.
If your symptoms don’t go away or get worse, you should see a doctor. Vasculitis in the legs might mean there’s something serious going on. Getting help early can make your symptoms better and stop things from getting worse.
To manage allergic vasculitis, the first thing to do is avoid what triggers it. Your doctor might also suggest medicine to help with your symptoms. If your case is severe, you might need more treatment to handle your body’s overall symptoms.
Knowing when to get medical help is important for managing allergic vasculitis well. If you see signs of vasculitis or your skin is very sensitive, talk to a doctor. They can check you out and give you the right care.
FAQ
What is allergic vasculitis?
Allergic vasculitis, also known as hypersensitivity vasculitis, is a condition. It causes inflammation in small blood vessels. This usually happens because of an allergic reaction to medicines, infections, or other substances.
What are the common causes of allergic vasculitis?
Common causes include reactions to medicines and infections. Sometimes, there’s no clear cause found.
What is the hallmark sign of allergic vasculitis?
The main sign is palpable purpura. This is a rash that feels like a bump on the skin. It often shows up on the legs.
How long does it take for symptoms to appear after exposure to the triggering agent?
Symptoms usually show up 7-10 days after being exposed to the cause.
Can allergic vasculitis affect organs other than the skin?
Yes, in severe cases, it can affect organs beyond the skin. This can lead to serious symptoms and complications.
How is allergic vasculitis diagnosed?
Doctors use physical exams, lab tests, imaging, and sometimes a skin biopsy. This helps confirm vasculitis and find the cause.
What is the treatment for allergic vasculitis?
Treatment includes stopping the cause and using medicines to help symptoms. In severe cases, more intense treatment might be needed.
How can allergic vasculitis be differentiated from other similar conditions?
Doctors use clinical evaluation and tests to tell it apart from other conditions. This includes checking for vasculitis and looking for the cause.
What is the prognosis for allergic vasculitis?
The outcome depends on how severe it is and if it affects other organs. Usually, stopping the cause helps symptoms go away.
When should I seek medical attention for allergic vasculitis?
See a doctor if you have symptoms, if they get worse, or if you think you’ve been exposed to something that caused it.
What are the characteristics of vasculitic lesions in allergic vasculitis?
Vasculitic lesions are palpable purpura. These are red or purple spots on the skin that can be felt. They often appear on the legs.
Can hypersensitivity vasculitis be managed at home?
Mild cases might be treated with rest and avoiding the cause. But severe cases or those affecting other parts of the body need medical help.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK482159/


































