
Do you often feel unexplained fatigue, have persistent joint pain, or see recurring inflammation? These signs might point to an autoimmune disease. This is when your immune system mistakenly attacks healthy cells instead of protecting you. Explaining what doesautoimmune disease mean and detailing the key signs and symptoms that indicate a disorder.
Autoimmune diseases happen when your immune system gets too active. It starts to attack and damage your body’s own tissues. This can cause a variety of health problems, from mild to severe.
Liv Hospital is dedicated to providing care based on solid evidence and educating patients. They help people spot these often-overlooked conditions. Knowing the signs and symptoms of autoimmune diseases is key to catching them early and treating them well.
Key Takeaways
- Autoimmune diseases occur when the immune system mistakenly attacks healthy cells.
- Common symptoms include unexplained fatigue, joint pain, and recurring inflammation.
- Early detection and treatment are critical for managing autoimmune diseases.
- Liv Hospital offers evidence-based care and patient education for autoimmune conditions.
- Understanding the signs and symptoms is essential for identifying autoimmune diseases.
What Does Autoimmune Disease Mean?
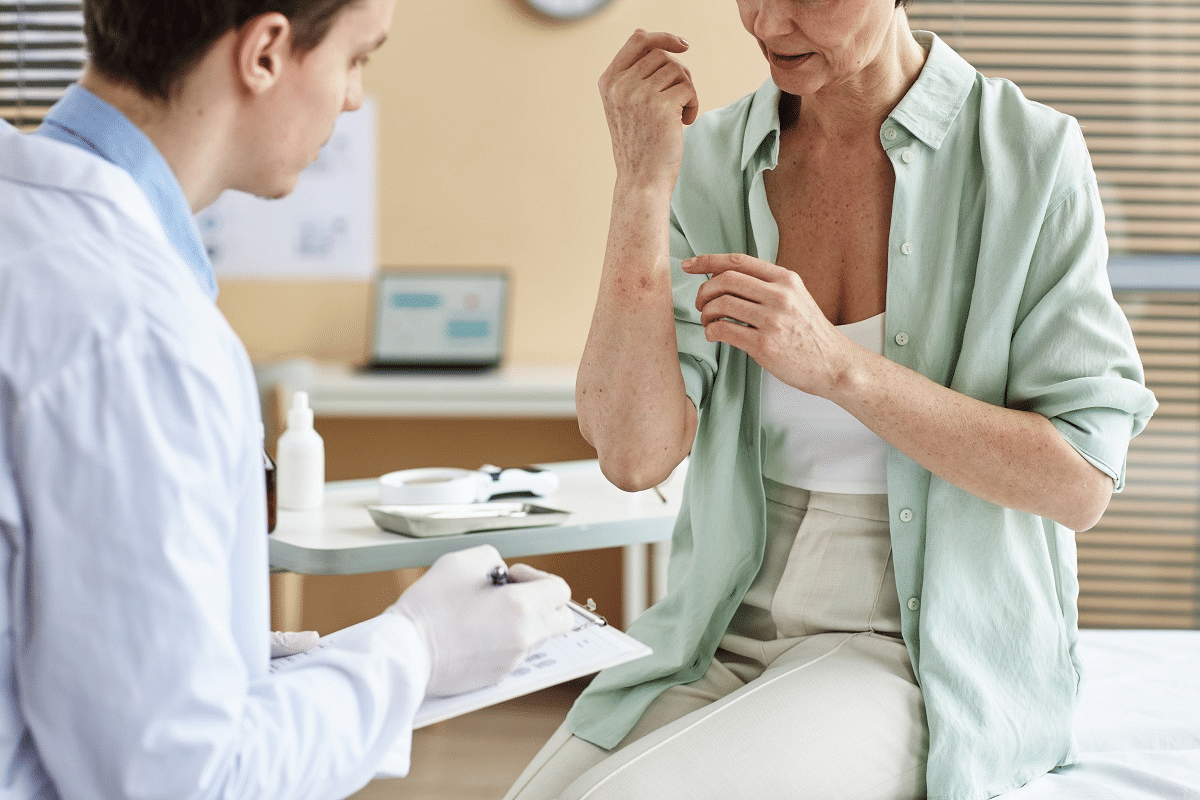
Autoimmune diseases are a group of disorders where the immune system attacks the body’s own cells and tissues. This happens because the immune system can’t tell the difference between self and non-self. As a result, it attacks the body’s own cells, causing damage and symptoms.
The Immune System’s Misguided Attack
In a normal body, the immune system fights off invaders. But in autoimmune diseases, it attacks the body’s own cells. This leads to inflammation, tissue damage, and symptoms.
This attack can cause many health problems, depending on what part of the body is targeted. For example, attacking the joints can cause rheumatoid arthritis. Targeting the pancreas can lead to type 1 diabetes.
The Core Definition of Autoimmunity
Autoimmunity happens when the immune system loses tolerance to its own antigens. This loss of tolerance causes the immune system to attack the body’s own tissues. The exact reasons for this loss are complex, involving genetics, environment, and hormones.
Understanding autoimmunity is key to treating these diseases. It requires a detailed approach that looks at all the factors involved.
The Scope: Over 100 Different Conditions
There are over 100 autoimmune diseases, affecting more than 24 million people in the U.S. These diseases range from common ones like type 1 diabetes to rarer conditions like lupus and multiple sclerosis.
Autoimmune diseases have different symptoms, but some common ones include fatigue, fever, and joint pain. This makes diagnosing them challenging.
The Rising Prevalence of Autoimmune Conditions
Recent studies show a worrying trend: autoimmune diseases are becoming more common. These conditions affect about 10% of the world’s population, posing a big challenge for public health.
In the United States, the situation is even more alarming. Recent statistics show that autoimmune diseases affect around 50 million Americans. This has a big impact on both those affected and the healthcare system.
Current Statistics in the United States
Studies have given us valuable insights into autoimmune diseases. The data shows a steady increase in cases over the years. This rise is due to genetic, environmental, and lifestyle factors.
Gender Disparities: 13% of Women vs. 7% of Men
Autoimmune diseases show a clear gender gap. About 13% of women are affected, compared to 7% of men. Hormonal and genetic factors might explain this difference.
The reasons for this gap are complex. Research suggests that sex hormones could affect the immune system. This might explain why more women are affected.
Alarming Trends in Autoimmune Markers
Autoimmune markers are also on the rise. These markers signal a higher risk of autoimmune diseases. The trend is alarming, showing an increase in those at risk.
Understanding these trends is key to finding solutions. By identifying the causes of rising autoimmune markers, healthcare can work to reduce risks. This is essential for preventing and treating autoimmune diseases.
How a Healthy Immune System Functions
Understanding the immune system is vital for health. It keeps us safe from infections and protects us from our own body’s harm.
Your immune system makes proteins called antibodies to fight off harmful substances. This is key to defending against pathogens.
The Body’s Defense Mechanisms
The immune system has many layers of protection. The first line of defense includes the skin and mucous membranes. They stop pathogens from getting in.
- The skin keeps many pathogens out.
- Mucous membranes in the body trap pathogens and foreign particles.
Self vs. Non-Self Recognition
The immune system knows the difference between self and non-self. This is key to not attacking the body’s own cells.
It uses complex cell types and signaling molecules for this. Autoimmune diseases happen when it gets confused, attacking the body’s own tissues.
The Normal Inflammatory Response
Inflammation is a normal immune response to injury or infection. It brings immune cells to the area to fight off the cause.
- Increased blood flow makes the area red and warm.
- Chemical signals attract immune cells.
- Immune cells clear pathogens and debris.
A healthy immune system fights infections without causing too much inflammation. This prevents damage to the body’s own tissues.
The Autoimmune Process: When Protection Becomes Destruction
The immune system fails to tell self from non-self, leading to attacks on the body’s own tissues. This complex issue involves many factors and pathways. It results in tissue damage and disease.
Breaking Down Self-Tolerance
Self-tolerance is when the immune system knows not to attack the body’s own cells. In autoimmune diseases, this fails, causing the immune system to attack the body’s cells and tissues. This failure is due to genetics, environment, and immune system problems.
Key factors contributing to the loss of self-tolerance include:
- Genetic mutations affecting immune regulatory genes
- Environmental triggers such as infections or exposure to certain chemicals
- Dysregulation of immune cells, including T cells and B cells
The Inflammatory Cascade in Autoimmunity
The inflammatory cascade is key in autoimmune diseases. When self-tolerance fails, the immune system starts an inflammatory response. This response causes tissue damage and is a major symptom of autoimmune disorders.
The inflammatory cascade involves:
- Activation of autoreactive T cells and B cells
- Production of autoantibodies and immune complexes
- Release of pro-inflammatory cytokines and chemokines
- Infiltration of immune cells into target tissues
Tissue and Organ Damage Mechanisms
Tissue and organ damage in autoimmune diseases come from the immune response. Autoantibodies and immune complexes can directly harm cells and tissues. Cytokines and other inflammatory mediators also play a role in tissue destruction.
The mechanisms of tissue damage include:
- Direct cytotoxic effects of autoantibodies and immune cells
- Inflammation-mediated tissue destruction
- Disruption of normal cellular function due to chronic inflammation
Understanding these mechanisms is key to treating autoimmune diseases. We need to restore self-tolerance, control inflammation, and protect tissues.
Common Types of Autoimmune Diseases
It’s important to know the different types of autoimmune diseases for proper diagnosis and treatment. These diseases can be split into two main groups: systemic autoimmune conditions and organ-specific autoimmune diseases.
Systemic Autoimmune Conditions
Systemic autoimmune conditions affect many parts of the body. They cause widespread inflammation and can disrupt various bodily functions.
- Rheumatoid Arthritis (RA): A condition that mainly affects the joints, causing pain, swelling, and potentially leading to deformity.
- Systemic Lupus Erythematosus (Lupus): A disease that can affect the skin, joints, kidneys, brain, and other organs, leading to a wide range of symptoms.
- Multiple Sclerosis (MS): A condition that affects the central nervous system, leading to symptoms such as vision loss, pain, fatigue, and impaired coordination.
These systemic conditions need a detailed treatment plan. This plan often includes a mix of medications and lifestyle changes.
Organ-Specific Autoimmune Diseases
Organ-specific autoimmune diseases target specific organs or tissues. This leads to conditions such as:
- Type 1 Diabetes: Results from the immune system attacking the insulin-producing beta cells in the pancreas, requiring insulin therapy for management.
- Hashimoto’s Thyroiditis: A condition where the immune system attacks the thyroid gland, leading to hypothyroidism.
- Psoriasis: An autoimmune condition that speeds up the life cycle of skin cells, causing cells to build up rapidly on the surface of the skin.
It’s key to recognize the signs of autoimmune diseases and understand the symptoms of autoimmune conditions for early diagnosis and treatment. Symptoms can vary widely based on the condition and affected organs. Common symptoms include fatigue, fever, and joint pain.
By understanding the different types of autoimmune diseases and their effects on the body, individuals can better navigate the diagnostic process. This helps them work towards managing their condition effectively.
Signs and Symptoms of Autoimmune Disorders
It’s important to know the signs and symptoms of autoimmune disorders early. This is because these diseases can show up in many ways. This makes it hard to diagnose them.
The 5 Common Symptoms Across Autoimmune Conditions
Autoimmune diseases have different symptoms, but some are common. These include:
- Fatigue: Feeling very tired that doesn’t go away with rest.
- Joint Pain: Pain and stiffness in the joints, like arthritis.
- Inflammation: Swelling and redness in different parts of the body.
- Skin Rashes: Different kinds of rashes, depending on the disease.
- Fever: Having fevers that keep coming back.
How Symptoms Differ Between Conditions
Even though some symptoms are the same, how they show up can be different. For example:
|
Condition |
Common Symptoms |
|---|---|
|
Rheumatoid Arthritis |
Joint pain, swelling, and stiffness, mainly in hands and feet. |
|
Lupus |
Butterfly-shaped rash on the face, joint pain, fever, and kidney issues. |
|
Type 1 Diabetes |
High blood sugar, more thirst and urination, and feeling tired. |
Symptoms Specific to Women
Women are more likely to get autoimmune diseases. Some symptoms are more common in women. These include:
- Hormonal Imbalance: Some diseases can mess with hormone levels, causing irregular periods or other hormonal issues.
- Pregnancy Complications: Women with these diseases might face problems during pregnancy, like early labor or preeclampsia.
Spotting these signs early is key to treating autoimmune disorders in women well.
Early Warning Signs: How to Tell if You Have an Autoimmune Disease
Knowing the early signs of autoimmune diseases can help you get medical help sooner. This can lead to an earlier diagnosis and treatment. Autoimmune diseases happen when your body’s immune system attacks its own cells, tissues, and organs. The symptoms can be vague and varied, making it hard to diagnose.
Recognizing the Initial Symptoms
The first signs of autoimmune diseases can be subtle and might look like other conditions. Common early signs include:
- Fatigue: Feeling very tired that doesn’t get better with rest.
- Joint Pain: Pain, stiffness, or swelling in the joints, which can move or affect certain joints.
- Skin Rashes: Different types of rashes, like the butterfly-shaped rash on the face seen in lupus.
- Muscle Weakness: Feeling weak or painful in the muscles, which can make daily activities hard.
When to Consult a Healthcare Provider
If you notice any of these signs, it’s important to see a healthcare provider:
- Persistence of Symptoms: If your symptoms keep getting worse or don’t go away.
- Combination of Symptoms: If you have symptoms that affect different parts of your body.
- Family History: If your family has a history of autoimmune diseases.
Distinguishing Autoimmune Symptoms from Other Conditions
Telling autoimmune symptoms from other conditions can be tricky. But, some signs might point to an autoimmune disease:
- Symptom Duration: Autoimmune symptoms often last or come back over time.
- Symptom Variability: Autoimmune diseases can cause many symptoms that change in severity.
- Response to Treatment: Symptoms that don’t get better with usual treatments might be autoimmune.
Recognizing autoimmune disease symptoms early and talking to a healthcare provider is key. If you’re worried about your symptoms, don’t wait to get medical help.
The Diagnostic Journey: Challenges and Approaches
Finding out you have an autoimmune disease can take a long time. It often takes many visits to different doctors. Some patients see four doctors over 4.5 years before they get a diagnosis.
Why Autoimmune Diseases Are Difficult to Diagnose
Autoimmune diseases are hard to diagnose because their symptoms are not specific. These symptoms can look like symptoms of other diseases. It’s hard to figure out what’s causing the symptoms because the immune system reacts in complex ways.
Common challenges in diagnosing autoimmune diseases include:
- Symptom overlap with other conditions
- Lack of definitive diagnostic tests
- Variability in patient symptoms
The 4.5-Year Average Path to Diagnosis
It usually takes 4.5 years to figure out if you have an autoimmune disease. During this time, you might see many doctors. This long wait is because autoimmune diseases are complex and need a detailed check-up.
A typical diagnostic path may involve:
- Initial consultation with a primary care physician
- Referral to specialists such as rheumatologists or immunologists
- Conducting diagnostic tests to rule out other conditions
Common Diagnostic Tests and Procedures
To diagnose autoimmune diseases, doctors use a few key methods. These include looking at your medical history, doing tests, and checking your symptoms. Some common tests are:
|
Test |
Purpose |
|---|---|
|
Antinuclear Antibody (ANA) Test |
Detects antibodies against the cell nucleus, indicative of autoimmune diseases like lupus |
|
Rheumatoid Factor (RF) Test |
Measures the level of rheumatoid factor in the blood, associated with rheumatoid arthritis |
|
Erythrocyte Sedimentation Rate (ESR) Test |
Assesses inflammation levels in the body |
Building Your Healthcare Team
Autoimmune diseases are complex, so you need a team of doctors. This team should include your primary care doctor, specialists, and other experts. They help manage your condition and improve your health.
Key members of your healthcare team may include:
- Primary care physician for overall health management
- Specialists for condition-specific care
- Nutritionists or dietitians for dietary guidance
- Physical therapists for rehabilitation and mobility
Risk Factors and Causes of Autoimmune Disease
The exact causes of autoimmune diseases are not fully understood. But, several risk factors have been found. Knowing these factors helps in finding better ways to prevent and treat these diseases.
Genetic Predisposition
Genetics are a big part of autoimmune diseases. People with a family history of these conditions are more likely to get them. Specific genetic markers are linked to higher risks for some diseases.
Environmental Triggers
Environmental factors like chemicals, infections, and diet can start autoimmune responses. The hygiene hypothesis says not getting enough microorganisms in childhood might lead to autoimmune diseases.
Hormonal Influences
Autoimmune diseases are more common in women, possibly due to hormonal differences. Estrogen levels can affect the immune system, possibly changing how autoimmune conditions start and get worse.
The Connection Between Stress and Autoimmunity
Long-term stress can hurt the immune system, making autoimmune responses worse. Stress management techniques like meditation and yoga are suggested as part of treatment.
Scientists are studying how genetics, environment, hormones, and stress affect autoimmune diseases. Most treatments try to calm the immune system. Understanding risk factors is key to this effort.
Conclusion: Living with Autoimmune Disease
It’s key to understand autoimmune diseases to manage them well. Even though there’s no cure yet, treatments can control your immune system. This helps manage symptoms.
Dealing with autoimmune disease needs a full plan. This includes knowing the signs, the diagnostic steps, and risk factors. Being informed helps face the challenges better.
Managing autoimmune diseases requires medical care, lifestyle changes, and regular checks. Knowing the symptoms can greatly improve life for those with these diseases.
FAQ
What are autoimmune diseases?
Autoimmune diseases happen when the immune system attacks the body’s own tissues. This leads to different conditions. There are over 100 types of autoimmune diseases, affecting various parts of the body.
What are the common symptoms of autoimmune disorders?
Symptoms include fatigue, joint pain, skin rashes, and stomach problems. Each condition and person can have different symptoms.
How do autoimmune diseases differ between men and women?
Women are more likely to get autoimmune diseases than men. About 13% of women are affected, compared to 7% of men. Women often get conditions like lupus and rheumatoid arthritis more than men.
What are the risk factors for developing an autoimmune disease?
Risk factors include genetics, environmental triggers, hormones, and stress. Having a family history of autoimmune diseases increases your risk.
How are autoimmune diseases diagnosed?
Diagnosing autoimmune diseases is hard. It involves medical history, physical exams, lab tests, and imaging. Blood tests and biopsies are common to check for damage.
What is the average time to diagnosis for autoimmune diseases?
It usually takes about 4.5 years to diagnose autoimmune diseases. This time can vary a lot based on the disease and individual.
Can stress trigger or exacerbate autoimmune diseases?
Yes, stress can make autoimmune diseases worse for some people. Changing your lifestyle and managing stress can help.
How can I distinguish autoimmune symptoms from those of other conditions?
It’s hard to tell autoimmune symptoms from others. Seeing a healthcare provider is key to find the cause and get a correct diagnosis.
What are the treatment options for autoimmune diseases?
Treatments depend on the disease. They might include medicines to control the immune system, manage symptoms, and prevent damage. Changing your lifestyle and managing stress are also important.
How can I manage my autoimmune disease effectively?
Effective management means working with a healthcare team to create a treatment plan. Making lifestyle changes and staying informed about your condition and treatments is also important.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://pubmed.ncbi.nlm.nih.gov/11502124/


































