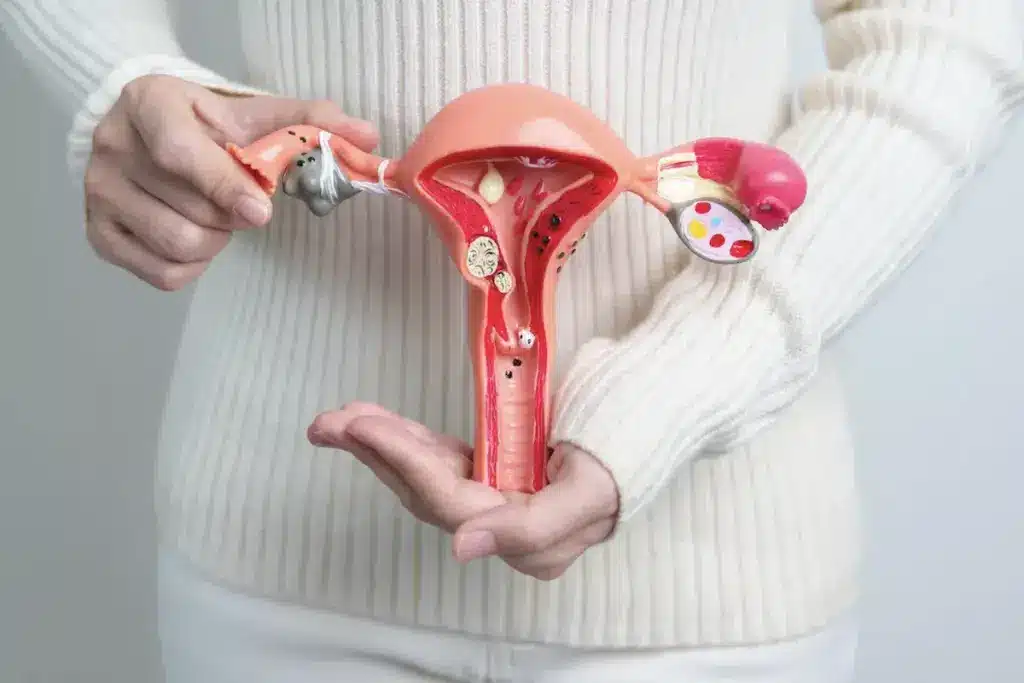
Choosing to have a hysterectomy surgery is a big decision. It’s important to know the best surgical method for a good result. Stories like Alla Feldbeyn’s and Colleen’s show how important quick and right medical care is. It’s key to have all the facts to make a smart choice.
For uterus removal, there are many surgical ways, like laparoscopic hysterectomy and others. The right surgery depends on the patient’s health and why they need it. We’ll walk you through the types of hysterectomy, explaining the good and bad of each.
Key Takeaways
- Understanding the different surgical approaches for uterus removal is key.
- Laparoscopic hysterectomy is a less invasive option with many benefits.
- The choice of hysterectomy surgery depends on individual health factors.
- Having all the information helps in making a well-informed decision.
- Quick medical care is essential for a good outcome.
Understanding Hysterectomy: What It Means for Your Body
When you think about a hysterectomy, it’s key to know the basics and its effects. This surgery removes the uterus. It’s important for those thinking about it to understand what it means.
Definition and Basic Concepts
A hysterectomy is a surgical procedure that involves removing a woman’s uterus, typically when alternative treatments have been ineffective for certain gynecological conditions. After this surgery, a woman can’t get pregnant and will stop menstruating.
There are different kinds of hysterectomies. Some remove the uterus and cervix, while others just take out the uterus. The choice depends on the health issue being treated.
When a Hysterectomy Becomes Necessary
A hysterectomy is often needed for endometrial cancer, uterine fibroids, and other gynecological issues. It’s a common solution when other treatments don’t work.
Some reasons for a hysterectomy include severe uterine prolapse and chronic pelvic pain. The choice to have a hysterectomy should be made after talking to healthcare professionals. They consider the patient’s health, the severity of the condition, and reproductive plans.
Common Medical Conditions Leading to Hysterectomy

Hysterectomy is a treatment for many gynecological issues. These problems can cause a lot of pain and discomfort. They affect not just the body but also a woman’s emotional health.
Uterine Fibroids and Their Impact
Uterine fibroids are non-cancerous growths in or around the uterus. They are common, affecting many women, mainly in their 30s and 40s. Some women may not feel any symptoms, but others may have heavy bleeding, long periods, and pain.
If symptoms are severe and other treatments don’t work, a hysterectomy might be suggested.
Endometriosis and Adenomyosis
Endometriosis is when tissue like the uterus lining grows outside the uterus. Adenomyosis is when this tissue grows into the uterus wall. Both can cause a lot of pain and heavy bleeding.
When these conditions are very bad and other treatments don’t help, a hysterectomy might be the last option.
Uterine Prolapse
Uterine prolapse happens when the uterus slips into the vagina. It’s often due to weak muscles and ligaments. Symptoms include feeling heavy in the pelvis, bleeding, and pain during sex.
In severe cases, surgery like a hysterectomy might be needed to fix the prolapse and ease symptoms.
Gynecological Cancers
Gynecological cancers, like cervical, uterine, and ovarian cancer, might need a hysterectomy as part of treatment. The choice to do a hysterectomy depends on the cancer type, stage, and the patient’s health.
In some cases, a radical hysterectomy is done. This means removing the uterus, cervix, and part of the vagina, along with tissues and lymph nodes.
Types of Hysterectomy Procedures: An Overview
It’s important to know about the different types of hysterectomy. This surgery is big, and knowing the options helps you talk to your doctor.
Total vs. Partial Hysterectomy
A total hysterectomy removes the whole uterus and cervix. It’s often done for health reasons. A partial hysterectomy, or subtotal, takes out the top part of the uterus but keeps the cervix.
Choosing between these depends on your health and what your doctor suggests.
Radical Hysterectomy for Cancer Treatment
A radical hysterectomy is more serious. It takes out the uterus, cervix, and part of the vagina. Sometimes, it also removes ovaries and fallopian tubes. It’s for cancer in the cervix, uterus, or ovaries.
This surgery is complex and needs careful thought and planning.
Supracervical Hysterectomy
Supracervical hysterectomy is like a partial one. It removes the top part of the uterus but keeps the cervix. It’s not as common but might be an option for some.
|
Procedure |
Description |
Common Indications |
|---|---|---|
|
Total Hysterectomy |
Removal of the entire uterus and cervix |
Fibroids, endometriosis, uterine prolapse |
|
Partial Hysterectomy |
Removal of the upper uterus, leaving the cervix |
Certain cases of fibroids or abnormal bleeding |
|
Radical Hysterectomy |
Removal of the uterus, cervix, part of the vagina, and sometimes ovaries and fallopian tubes |
Cervical, uterine, or ovarian cancer |
|
Supracervical Hysterectomy |
Removal of the upper uterus, leaving the cervix |
Similar to partial hysterectomy, with specific patient criteria |
Each hysterectomy type has its own reasons and benefits. Knowing these helps you make a better choice for your care.
Traditional Abdominal Hysterectomy
The traditional abdominal hysterectomy is a common surgery for many gynecological issues. It involves opening the abdomen to remove the uterus.
The Procedure Explained
In a traditional abdominal hysterectomy, a surgeon makes a cut in the belly. The cut’s shape depends on the patient’s body, the surgery’s reason, and the surgeon’s style. After the cut, the surgeon carefully finds and removes the uterus and its support.
Recovery Timeline and Expectations
Recovering from this surgery takes longer than some others. Patients usually stay in the hospital for 1 to 3 days. At home, it can take 6 to 8 weeks to fully recover. During this time, they should avoid heavy lifting, bending, and hard work.
Managing pain well is key during recovery. Doctors often give pain meds to help. Having someone at home to help during the first few weeks is also a good idea.
Advantages and Disadvantages
There are good and bad sides to traditional abdominal hysterectomy. Knowing these can help patients decide if it’s right for them.
|
Advantages |
Disadvantages |
|---|---|
|
Allows for direct visualization and access to the uterus and surrounding structures |
Longer recovery time compared to minimally invasive procedures |
|
Can be used in complex cases or when other methods are not feasible |
Larger incision may result in more postoperative pain |
|
Surgeons are highly familiar with this traditional technique |
Higher risk of complications such as infection or adhesions |
By considering these points, patients and doctors can decide if this surgery is best for them.
Vaginal Hysterectomy: A Less Invasive Approach
Vaginal hysterectomy is a less invasive way to remove the uterus. It often leads to quicker recovery times. This method removes the uterus through the vagina, without the need for big cuts on the belly.
Procedure Details and Candidacy
This surgery is done under general or regional anesthesia. The surgeon makes a small cut in the vagina to take out the uterus. It’s best for women with uterine issues like prolapse or those who’ve had vaginal births.
Who can get a vaginal hysterectomy depends on several things:
- The size and how mobile the uterus is
- Any adhesions or scar tissue
- The patient’s health and medical history
- The surgeon’s skill in doing vaginal hysterectomies
Recovery Process
Recovering from a vaginal hysterectomy is usually faster than other surgeries. Women can usually get back to normal in 4 to 6 weeks. But, it’s important to follow the doctor’s advice to avoid problems.
Recovery includes:
- Managing pain with the right medicine
- Not lifting heavy or doing hard activities
- Going to check-ups to see how healing is going
Benefits and Limitations
Vaginal hysterectomy has many benefits. It causes less pain, shorter hospital stays, and often no visible scars. But, it’s not right for everyone, like those with certain health issues or past pelvic surgery.
Some downsides are:
- It’s not for everyone because of uterus size or mobility
- It might be harder to see and work on during surgery
- You need a skilled surgeon who knows how to do vaginal hysterectomies
In summary, vaginal hysterectomy is a good choice for some women needing a hysterectomy. It’s less invasive. Knowing the details, who it’s for, how to recover, and its limits helps patients make the best choice for themselves.
Laparoscopic Hysterectomy: The Modern Standard
Laparoscopic hysterectomy is now the top choice for removing the uterus. It’s a less invasive option compared to old surgical methods. This method uses small cuts in the belly to insert tools, making the surgery more precise and less painful.
How Laparoscopic Procedures Work
This surgery uses a thin tube with a camera and light, called a laparoscope. It lets surgeons see the pelvic area on a screen. They use this view to carefully remove the uterus, either through the vagina or small cuts in the belly.
The small cuts are usually just 0.5 to 1 cm. This means less damage and pain compared to open surgery. The laparoscope also lets surgeons see more clearly, helping them find and fix problems they might miss in open surgery.
Types of Laparoscopic Hysterectomies
There are a few types of laparoscopic hysterectomies:
- Total Laparoscopic Hysterectomy (TLH): The whole uterus is removed through small cuts.
- Laparoscopic-Assisted Vaginal Hysterectomy (LAVH): The laparoscope helps remove the uterus through the vagina.
- Laparoscopic Supracervical Hysterectomy (LSH): Only the top part of the uterus is removed, leaving the cervix.
Each type is chosen based on the patient’s needs and the surgeon’s advice.
Ideal Candidates for This Approach
Women with uterine fibroids, endometriosis, or heavy bleeding might be good candidates. They should talk to a healthcare provider to see if this surgery is right for them. The decision depends on their health, symptoms, and past surgeries.
Laparoscopic hysterectomy has many benefits. Patients often have shorter hospital stays, less pain, and faster recovery. But, it’s important to talk to a doctor about the risks and benefits to make the best choice.
Robotic-Assisted Hysterectomy: Technology in Surgery
Medical technology keeps getting better, and robotic-assisted hysterectomy is now a top choice for uterus removal surgery. This new method uses robots to make the surgery safer and more effective.
The da Vinci Surgical System
The da Vinci Surgical System is a cutting-edge robot that changes how we do surgery. It lets surgeons do complex tasks with more precision and control. The system has a surgeon’s console, robotic arms, and a 3D vision system.
Key Features of the da Vinci Surgical System:
- High-definition 3D visualization
- Robotic arms with precise instrumentation
- Enhanced dexterity and range of motion
- Improved ergonomics for surgeons
Comparing Robotic vs. Standard Laparoscopic Techniques
Robotic-assisted hysterectomy has many benefits over traditional laparoscopic methods. It can lead to less blood loss and fewer complications. Plus, patients might recover faster. But, it’s important to think about the longer surgery times and higher costs.
|
Feature |
Robotic-Assisted |
Laparoscopic |
|---|---|---|
|
Blood Loss |
Less |
Moderate |
|
Recovery Time |
Faster |
Moderate |
|
Cost |
Higher |
Lower |
Cost Considerations and Insurance Coverage
The cost of robotic-assisted hysterectomy is often higher than other methods. Insurance coverage can vary, and some plans might not cover the extra costs. It’s key for patients to talk to their healthcare provider about insurance to know what they’ll have to pay.
When talking to your surgeon about robotic-assisted hysterectomy, ask about:
- The surgeon’s experience with the da Vinci Surgical System
- The benefits and risks for your specific situation
- The estimated costs and insurance coverage
Comparing Recovery Times Across Different Procedures
Recovery times for different hysterectomy procedures vary a lot. Knowing these differences helps patients set realistic expectations and choose the best option for their health.
Hospital Stay Duration
The length of hospital stay is a key indicator of recovery. More invasive procedures usually mean longer hospital stays. For example, a traditional abdominal hysterectomy often requires 2 to 4 days in the hospital.
In contrast, laparoscopic and robotic-assisted hysterectomies tend to have shorter stays. Some patients might even go home the same day or the next day.
|
Procedure Type |
Average Hospital Stay |
|---|---|
|
Traditional Abdominal Hysterectomy |
2-4 days |
|
Laparoscopic Hysterectomy |
1-2 days |
|
Robotic-Assisted Hysterectomy |
1 day or less |
|
Vaginal Hysterectomy |
1-2 days |
Return to Normal Activities
Recovery times for returning to normal activities also vary. Minimally invasive surgeries like laparoscopic or robotic-assisted hysterectomies usually take 2 to 4 weeks. Traditional abdominal hysterectomies can take 6 to 8 weeks or more.
Return to Normal Activities Timeline:
- Laparoscopic/Robotic-Assisted: 2-4 weeks
- Vaginal Hysterectomy: 3-6 weeks
- Traditional Abdominal: 6-8 weeks
Pain Management Differences
Pain management is a big part of recovery. The pain level can differ based on the hysterectomy type. Minimally invasive procedures usually cause less pain than more invasive ones. Good pain management is key for a smooth recovery.
“Pain is what we experience, and suffering is what we make of it.” – M. Scott Peck
Understanding recovery times and pain management for different hysterectomy procedures helps patients make better choices. It’s important to talk to a healthcare provider to find the best option for your needs.
Potential Risks and Complications of Different Hysterectomy Types
When thinking about a hysterectomy, knowing the risks is key. This surgery is often needed and changes lives. But, knowing what might happen helps you make a smart choice for your health.
Short-Term Surgical Risks
Hysterectomy, like any big surgery, has immediate risks. These can be infection, bleeding, or damage to nearby organs like the bladder or bowel. The chance of these problems depends on the type of hysterectomy.
Types of Hysterectomy and Associated Risks:
|
Type of Hysterectomy |
Common Risks |
|---|---|
|
Abdominal Hysterectomy |
Infection, bleeding, adhesions |
|
Vaginal Hysterectomy |
Infection, bleeding, vault prolapse |
|
Laparoscopic Hysterectomy |
Infection, bleeding, injury to surrounding organs |
Long-Term Health Implications
Hysterectomy can also affect your health long-term. This might include early menopause if your ovaries are removed. You could also see changes in pelvic floor support and how you pee or have sex.
Emotional and Psychological Considerations
Choosing to have a hysterectomy is not just about your body. It also affects your mind and feelings. You might feel relieved or sad, depending on why you’re having the surgery.
It’s important to understand these emotional and psychological effects. Getting support from doctors, family, and friends can help you deal with these changes.
Life After Hysterectomy: What to Expect
A hysterectomy ends a woman’s ability to have children, but it’s just the start of a new chapter. Understanding what comes next can make the transition smoother.
Hormonal Changes and Management
If you haven’t reached menopause, a hysterectomy will start it. You might feel hot flashes, mood swings, and vaginal dryness. Talking to your doctor about hormone replacement therapy (HRT) can help manage these symptoms.
HRT can ease some menopause symptoms, but it’s important to consider the risks. We’ll help you decide what’s best for you.
Sexual Function and Intimacy
Many worry about how a hysterectomy will affect sex. The surgery removes the uterus but doesn’t change sexual desire or orgasm. Yet, some women might notice changes in sexual sensation or vaginal dryness. These can be treated.
Keeping intimacy alive is key. Talk openly with your partner about any changes or worries. Counseling or therapy can also help you adjust.
Physical and Emotional Adjustment
Recovering from a hysterectomy is about more than just healing physically. It’s also about emotional adjustment. You might feel a mix of emotions, from relief to grief. We’re here to support you, guiding you through both physical and emotional recovery.
Doing gentle exercises, like pelvic floor exercises, can help you regain strength. Also, joining support groups can offer valuable insights and emotional support from others who’ve gone through similar experiences.
Alternatives to Hysterectomy Worth Considering
Hysterectomy is sometimes needed, but there are other treatments too. These alternatives can help with symptoms, keep fertility, and cut down on recovery time.
Medication Options
For some conditions, medicine can be a good choice. Hormonal therapies can manage symptoms of endometriosis or uterine fibroids. Nonsteroidal anti-inflammatory drugs (NSAIDs) and tranexamic acid help with heavy bleeding from fibroids.
Uterine Artery Embolization
Uterine artery embolization (UAE) is a small procedure. It blocks blood to the uterus, shrinking fibroids. It’s great for women with fibroids who don’t want surgery or want to keep their fertility.
Endometrial Ablation
Endometrial ablation destroys the uterine lining to stop heavy bleeding. It’s for women close to menopause or who have no more kids. It doesn’t fix fibroids or endometriosis but cuts down bleeding a lot.
Myomectomy for Fibroid Removal
Myomectomy removes fibroids but keeps the uterus. It’s for women who want to keep their fertility or avoid hysterectomy. The choice depends on fibroid size, number, and location, and the woman’s health.
|
Procedure |
Description |
Best For |
|---|---|---|
|
Medication Options |
Hormonal therapies and NSAIDs to manage symptoms |
Endometriosis, fibroids, heavy menstrual bleeding |
|
Uterine Artery Embolization |
Minimally invasive procedure to block blood supply to fibroids |
Symptomatic fibroids, fertility preservation |
|
Endometrial Ablation |
Destroys the uterine lining to reduce bleeding |
Heavy menstrual bleeding, women nearing menopause |
|
Myomectomy |
Surgical removal of fibroids |
Fibroids, fertility preservation |
Each alternative has its own benefits and risks. It’s important for women to talk to their doctor. This way, they can choose the best treatment for their health and goals.
How to Choose the Right Hysterectomy Procedure for You
There are many hysterectomy procedures to choose from. Patients need to think carefully about what’s best for them. The right choice depends on your health, the reason for the surgery, and what you prefer.
Important Questions to Ask Your Doctor
Talking to your doctor is key before making a decision. Here are some important questions to ask:
- Why do you think a hysterectomy is needed?
- What risks and complications could there be?
- What are the differences between the procedures, and which fits my situation best?
- What can I expect in terms of recovery and results?
- Are there other treatments I should look into?
Considering Your Medical History and Condition
Your medical history and current health are important in choosing a procedure. For example, if you’ve had pelvic surgery before, you might need a certain type of surgery.
Getting a detailed review of your medical history is important. Your doctor will look at your past surgeries, current medications, and any health issues you have.
Weighing Recovery Time vs. Surgical Benefits
When picking a hysterectomy procedure, think about the benefits and how long it takes to recover. Each procedure has its own recovery time and benefits.
|
Procedure |
Recovery Time |
Surgical Benefits |
|---|---|---|
|
Abdominal Hysterectomy |
6-8 weeks |
Effective for large fibroids or complex conditions |
|
Laparoscopic Hysterectomy |
3-6 weeks |
Minimally invasive, less pain, quicker recovery |
|
Vaginal Hysterectomy |
3-6 weeks |
No abdominal scars, faster recovery |
|
Robotic-Assisted Hysterectomy |
3-6 weeks |
Enhanced precision, less blood loss |
Conclusion: Making an Informed Decision About Uterus Removal
When thinking about removing the uterus, it’s important to make a well-informed choice. We’ve looked at different types of hysterectomies, how long it takes to recover, and possible risks. Knowing these details helps patients choose what’s best for their health.
For some, there are other options like medicines, uterine artery embolization, or myomectomy. We suggest talking to a doctor about these alternatives. This way, patients can find the right treatment for them.
The choice to remove the uterus should be carefully thought out. Patients need to understand the procedure and its effects. By considering their own health needs, they can make a choice that fits their health goals.
FAQ
What is a hysterectomy, and why is it performed?
A hysterectomy is a surgery to remove the uterus. It’s done for many reasons like fibroids, endometriosis, and cancer.
What are the different types of hysterectomy procedures?
There are a few types. Total hysterectomy removes the uterus and cervix. Partial hysterectomy keeps the cervix. Radical hysterectomy removes more tissue. Supracervical hysterectomy removes the upper uterus.
What is laparoscopic hysterectomy, and how does it differ from traditional hysterectomy?
Laparoscopic hysterectomy is a less invasive surgery. It uses small incisions and a camera. It’s less invasive than traditional surgery, leading to quicker recovery and less scarring.
What are the benefits of robotic-assisted hysterectomy?
Robotic-assisted hysterectomy offers better precision and control. It can lead to less blood loss and quicker recovery. This makes it a good option for some patients.
How long does recovery take after a hysterectomy, and what are the differences between procedures?
Recovery times vary. Traditional surgery takes 6-8 weeks. Laparoscopic and robotic surgeries take 2-4 weeks. Vaginal surgery is the quickest, taking 4-6 weeks.
What are the possible risks and complications of hysterectomy?
Risks include infection and blood clots. There’s also a chance of injury to other organs. Long-term effects like early menopause or pelvic floor problems can occur. Emotional and psychological adjustments are common too.
Are there alternatives to hysterectomy that I should consider?
Yes, there are alternatives. Medication can help manage symptoms. Uterine artery embolization shrinks fibroids. Endometrial ablation treats heavy bleeding. Myomectomy removes fibroids while keeping the uterus.
How do I choose the right hysterectomy procedure for my condition?
Choosing the right procedure involves talking to your doctor. Consider recovery time, benefits, and risks. This helps make an informed decision.
What can I expect after a hysterectomy in terms of hormonal changes and sexual function?
Women not in menopause may continue to have hormonal cycles. Sexual function can be maintained. But, some women may experience changes in libido or vaginal dryness.
Will I need to stay in the hospital after a hysterectomy, and for how long?
Hospital stay varies. Traditional surgery needs 2-4 days. Laparoscopic and vaginal surgeries may allow for same-day discharge or a shorter stay.
Can I have sex after a hysterectomy?
Yes, most women can resume sex after 6-8 weeks. Always consult with a healthcare provider for specific instructions.
What is the difference between laparoscopic hysterectomy and robotic-assisted hysterectomy?
Laparoscopic hysterectomy uses traditional instruments. Robotic-assisted hysterectomy uses a robotic system. This offers more precision and less trauma to the patient.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC5558366/
























