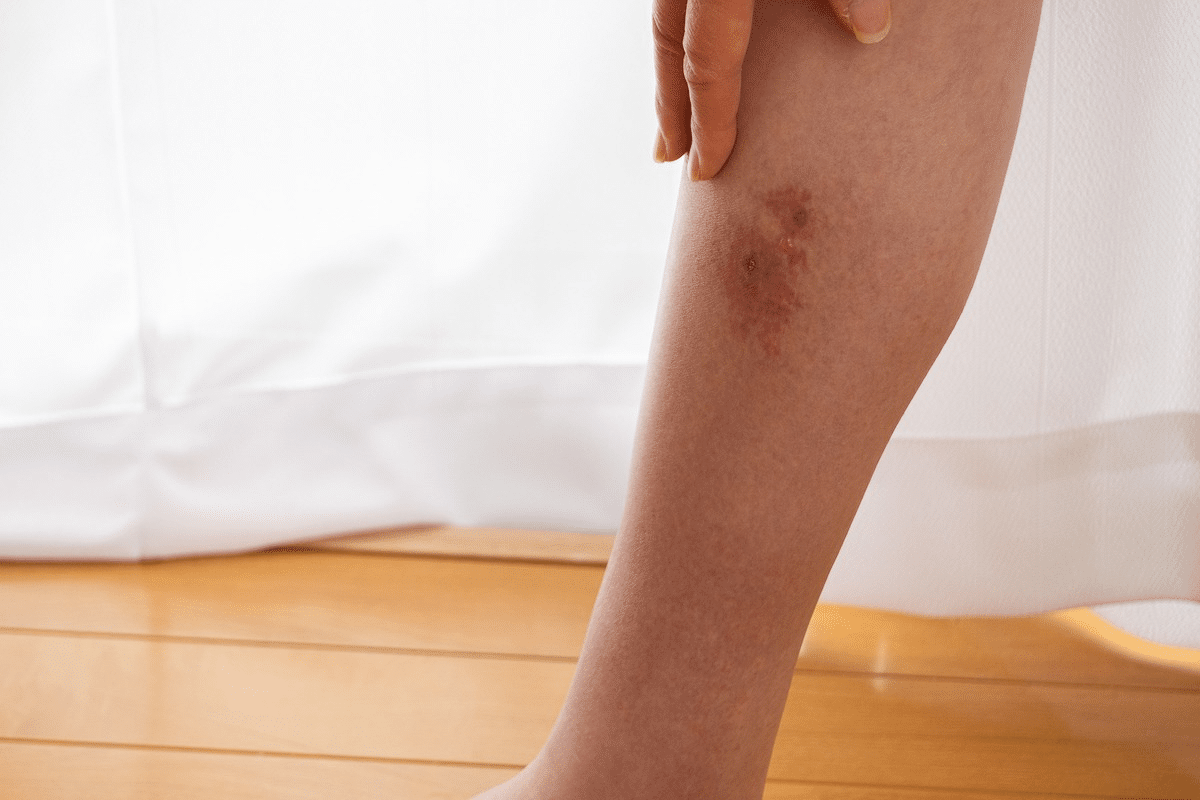
Leukocytoclastic vasculitis (LCV) is a condition that affects the skin and sometimes other parts of the body. It’s important to know what LCV is and how it shows up.
LCV is marked by neutrophilic inflammation of small postcapillary venules in the dermis. This leads to a specific skin rash. It’s also known as hypersensitivity vasculitis and affects both men and women equally.
The main sign of LCV is a painful, purple rash on the legs. Though it’s not very common, about 10-30 people per million get it each year. Spotting it early and getting the right diagnosis is key for the best results.
Key Takeaways
- Leukocytoclastic vasculitis is a small-vessel vasculitis affecting the skin and sometimes other organs.
- The condition is characterized by neutrophilic inflammation of small postcapillary venules.
- LCV manifests as a painful, purple rash mainly on the legs.
- The incidence of LCV is about 10-30 persons per million annually.
- Early recognition and proper diagnosis are vital for the best outcomes.
Understanding Leukocytoclastic Vasculitis (LCV)
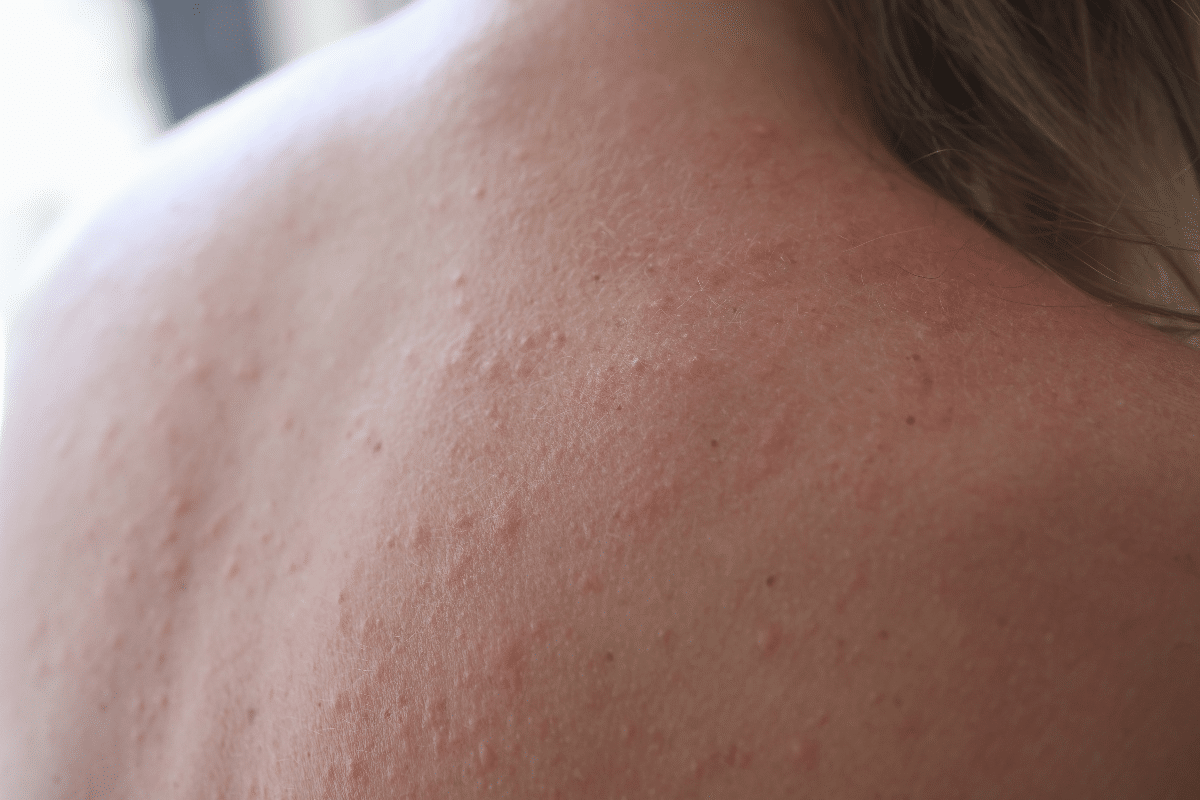
Leukocytoclastic vasculitis (LCV) is a condition that affects small blood vessels. It leads to inflammation and various symptoms. Knowing about LCV’s definition, prevalence, and impact on patients is key.
Definition and Overview
LCV is marked by neutrophilic inflammation of small postcapillary venules. It falls under vasculitides that target small vessels. The term “leukocytoclastic” points to the destruction of white blood cells, a key feature.
Doctors diagnose LCV by looking at symptoms and tissue damage. They search for signs like palpable purpura and skin ulcers. These are signs of inflammation and damage to small blood vessels.
Epidemiology and Prevalence
LCV can strike anyone, but its frequency varies. It’s considered rare, and exact numbers are hard to find. Triggers include infections, medications, and autoimmune disorders.
Research shows LCV is linked to systemic diseases. This makes managing underlying conditions critical. Its prevalence might be higher than reported due to its varied symptoms and sometimes unknown causes.
Impact on Quality of Life
LCV can greatly affect a person’s life. Symptoms like painful skin lesions and fatigue hinder daily activities. The visible nature of the condition can also cause emotional distress.
Effective management of LCV requires a team effort. This includes dermatology care, managing underlying conditions, and improving quality of life. Understanding LCV helps healthcare providers offer better care.
LCV Medical Abbreviation: What Does It Stand For?
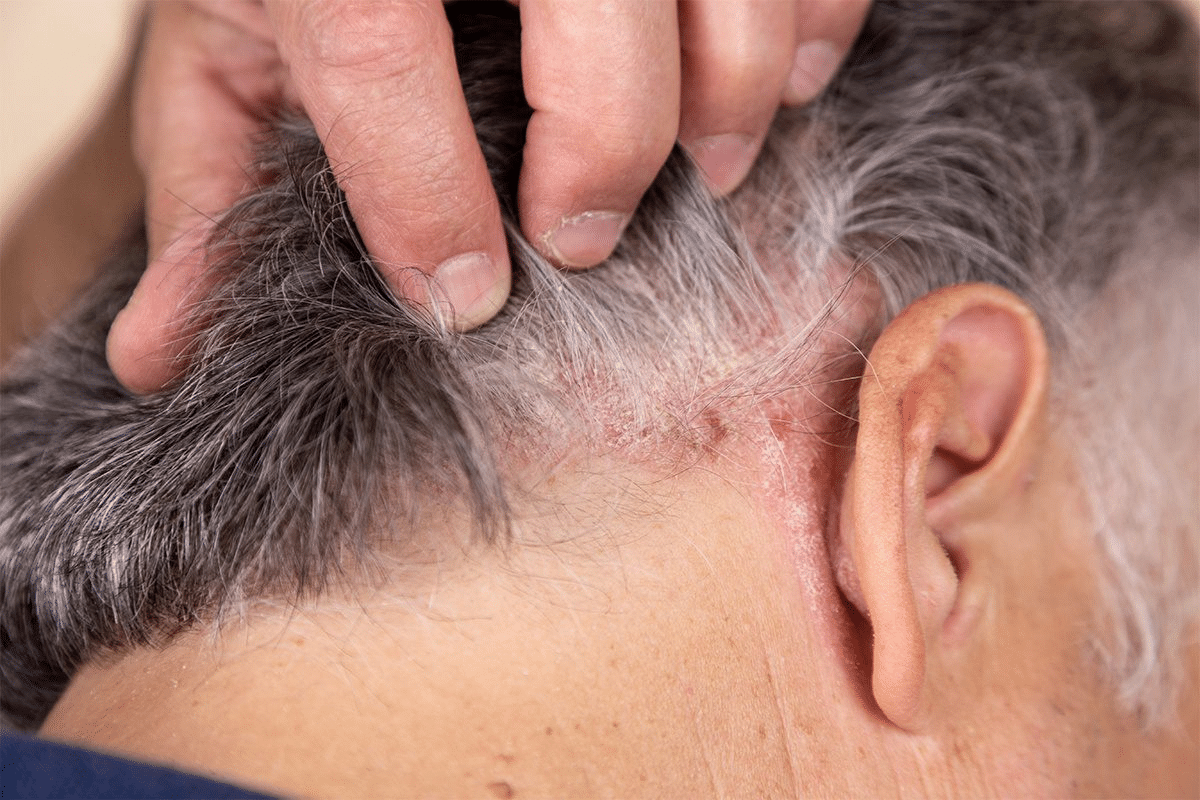
The term LCV is often seen in medical settings, but what does it mean? LCV stands for Leukocytoclastic Vasculitis, a condition that causes blood vessel inflammation.
Knowing what LCV means is key for doctors and patients. It’s a type of vasculitis that affects small blood vessels. This can lead to various symptoms and problems.
Origin of the Term “Leukocytoclastic”
The word “leukocytoclastic” means the breakdown of white blood cells. It comes from “leukocyte,” meaning white blood cell, and “clastic,” meaning broken or destroyed.
This term is important because it describes how Leukocytoclastic Vasculitis works. White blood cells are broken down, causing inflammation and damage to blood vessel walls.
Related Medical Terminology
Several terms are linked to LCV, including:
- Vasculitis: Inflammation of the blood vessels.
- Leukocytoclasis: The destruction of white blood cells.
- Purpura: Purple spots on the skin, often seen with LCV.
Knowing these terms helps in diagnosing and treating LCV well.
Common Misconceptions
Many think LCV is rare. While it’s not as common as other vasculitis types, it’s significant and needs medical care.
Some also believe LCV only affects the skin. But, it can also affect other organs and systems. This makes getting a full diagnosis and treatment important.
By understanding LCV and its meaning, we can better handle its diagnosis and treatment. Knowing related terms and common misconceptions is key for managing the condition well.
Causes and Triggers of Leukocytoclastic Vasculitis
Knowing what causes LCV is key to treating it well. LCV can start from many things, so finding the cause is important.
Drug-Induced LCV
Some medicines can lead to LCV. This includes antibiotics and NSAIDs. Stopping the bad drug is often the first step in treating it.
|
Drug Category |
Examples |
|---|---|
|
Antibiotics |
Penicillins, Macrolides |
|
NSAIDs |
Ibuprofen, Naproxen |
|
Other Agents |
Allopurinol, Hydralazine |
Infection-Related LCV
Infections can also cause LCV. This includes bacterial, viral, and other infections. Knowing how infections link to LCV helps in managing it.
- Bacterial infections: streptococcal infections
- Viral infections: hepatitis B and C
- Other infections: parasitic and fungal infections
Autoimmune-Associated LCV
Autoimmune diseases can also lead to LCV. This includes conditions like rheumatoid arthritis. Managing the autoimmune disease is key.
Idiopathic LCV
Sometimes, the cause of LCV is not found, called idiopathic LCV. More research is needed to understand these cases.
Finding the cause of LCV is vital for good treatment. By knowing the triggers, doctors can create better treatment plans.
Pathophysiology of Leukocytoclastic Vasculitis
Leukocytoclastic vasculitis is caused by an immune response that inflames small blood vessels. This process involves the formation of immune complexes, neutrophil activation, and damage to blood vessels.
Immune Complex Formation
Immune complex formation is key in LCV. These complexes form when antibodies bind to antigens, like drugs or infections. They deposit in blood vessel walls, starting an inflammatory response.
Neutrophil Activation and Leukocytoclasis
When immune complexes are deposited, neutrophils are activated. These white blood cells release enzymes that damage the vessel wall. This damage is known as leukocytoclasis and causes inflammation and damage in LCV.
Vascular Damage Mechanisms
The damage in LCV comes from the inflammatory response. Neutrophils release chemicals that cause the vessel wall to die. This makes the vessel leak, leading to purpura and other skin issues.
Histopathological Features
The signs of LCV include fibrinoid necrosis and leukocytoclasis. Neutrophils also infiltrate the area. These are seen in skin biopsies and help diagnose LCV.
In summary, LCV’s pathophysiology involves immune complexes, neutrophil activation, and vascular damage. These lead to the condition’s distinctive clinical and histopathological features.
Clinical Presentation and Symptoms of LCV
Knowing how LCV presents is key for early diagnosis and treatment. LCV symptoms can vary, affecting the skin and sometimes other parts of the body.
Palpable Purpura: The Hallmark Sign
Palpable purpura is the main sign of LCV. It’s a raised purple rash that stands out. This rash is a big clue for doctors and helps tell LCV apart from other vasculitis types.
Palpable purpura happens when small blood vessels get inflamed. This leads to blood leaking into the skin.
Distribution Patterns on the Body
LCV lesions can show up anywhere on the body, but often on the lower legs. Each person’s pattern can be different. Some might see lesions on their legs, buttocks, or trunk.
Where the lesions appear can hint at what might be causing them.
Other Skin Manifestations
LCV can also cause macules, papules, and ulcers on the skin. These can change as the disease goes on. This makes it sometimes hard to diagnose.
Doctors need to look at all the symptoms carefully.
Systemic Symptoms
Some people with LCV also have systemic symptoms. These can be fever, feeling tired, joint pain, and stomach problems. These symptoms suggest the disease might be more serious.
They need a detailed check-up and possibly stronger treatment.
LCV symptoms can really affect a person’s life. So, doctors need to be kind and thorough in their care. Knowing all about LCV symptoms helps doctors help their patients better.
LCV Rash: Visual Identification and Characteristics
The LCV rash is hard to spot because it looks different in various ways. Knowing how to identify it is key to making a correct diagnosis.
Appearance of Early vs. Late Lesions
Early signs of LCV are palpable purpura. These are red or purple spots that feel like bumps on the skin. They usually show up on the legs.
Later, the rash can turn into ulcerative or necrotic lesions. Knowing how the rash changes is important for quick treatment.
Differentiating LCV from Other Vasculitic Rashes
It’s important to tell LCV apart from other vasculitis types. The main clue is finding leukocytoclasis in skin samples.
|
Characteristics |
LCV Rash |
Other Vasculitic Rashes |
|---|---|---|
|
Typical Location |
Lower Extremities |
Variable |
|
Lesion Type |
Palpable Purpura |
Purpuric, Ulcerative, or Vesicular |
|
Histopathology |
Leukocytoclasis |
Varies |
Photographic Examples of LCV Presentations
Photos can help a lot in spotting LCV rash. They show how the rash can look different.
When to Seek Medical Attention
If your rash gets worse, you have a fever, or your joints hurt, see a doctor. Quick action can make a big difference.
Diagnosis of Leukocytoclastic Vasculitis
To diagnose LCV, doctors use a detailed clinical evaluation. They also rely on tools like skin biopsies and lab tests.
Clinical Evaluation
The first step is a thorough clinical evaluation. This involves looking at your medical history and doing a physical exam. They check for signs of LCV on your skin.
They look for palpable purpura, a key sign of LCV. They also check how the lesions are spread out.
Skin Biopsy and Histopathology
A skin biopsy is key to confirming LCV. It shows inflammation in the blood vessel walls and leukocytoclasis.
The biopsy helps tell LCV apart from other conditions. It also shows how much damage there is to the blood vessels.
Laboratory Tests
Laboratory tests are important for supporting the diagnosis. They help find the cause or related conditions.
- Complete Blood Count (CBC) to check for infection or inflammation
- Erythrocyte Sedimentation Rate (ESR) or C-Reactive Protein (CRP) to see inflammation levels
- Urinalysis to check for kidney problems
- Serological tests to find autoimmune disorders or infections
|
Laboratory Test |
Purpose in LCV Diagnosis |
|---|---|
|
CBC |
Check for infection or inflammation |
|
ESR/CRP |
See inflammation levels |
|
Urinalysis |
Check for kidney problems |
|
Serological Tests |
Find autoimmune disorders or infections |
Imaging Studies
In some cases, imaging studies are needed. They help see how far the disease has spread or if there are complications.
These studies include X-rays, ultrasound, or other imaging. They depend on the symptoms and suspected organ problems.
Treatment Approaches for LCV
Managing Leukocytoclastic Vasculitis (LCV) needs a mix of strategies. We’ll look at how to tackle symptoms and find the root causes. This includes removing triggers, using medicine, and providing supportive care. We’ll also talk about new treatments.
Identifying and Removing Triggers
The first step is to find and get rid of triggers. This might mean stopping certain medicines or treating infections. A detailed medical check-up helps find the cause of LCV.
Common triggers include:
- Certain medications, such as antibiotics and NSAIDs
- Infections, including bacterial and viral infections
- Autoimmune disorders, such as rheumatoid arthritis and lupus
Pharmacological Management
Medicine is key in treating LCV symptoms and stopping more damage. Corticosteroids are often the first choice to fight inflammation.
|
Treatment |
Description |
Benefits |
|---|---|---|
|
Corticosteroids |
Anti-inflammatory medications |
Rapid reduction of inflammation |
|
Immunosuppressants |
Drugs that suppress the immune system |
Effective in severe cases or when corticosteroids are insufficient |
|
Colchicine |
Anti-inflammatory medication |
Useful in reducing the frequency of LCV episodes |
Supportive Care Measures
Supportive care is important for LCV management. It focuses on easing symptoms and improving life quality. We suggest wound care, pain management, and teaching patients about skin protection and avoiding triggers.
Emerging Therapies
New research on LCV is promising. It includes looking at biologic agents and other new treatments. These could help those with hard-to-treat or severe LCV.
By using a full treatment plan, we can manage LCV well. This includes finding and removing triggers, using medicine, supportive care, and new therapies. This approach helps improve patient outcomes.
Living with LCV: Management and Coping Strategies
Managing Leukocytoclastic Vasculitis (LCV) needs a mix of medical care, lifestyle changes, and support. A good care plan helps control symptoms and boosts quality of life.
Skin Care Recommendations
Good skin care is key for LCV management. It prevents infections and aids healing. Clean your skin gently with mild soap and lukewarm water. Stay away from harsh products that can irritate your skin and cause flare-ups.
Key Skin Care Tips:
- Use fragrance-free moisturizers to keep the skin hydrated.
- Avoid extreme temperatures that can cause skin irritation.
- Wear protective clothing to prevent skin injuries.
Lifestyle Modifications
Changing your lifestyle can help manage LCV symptoms. Eat healthy, drink plenty of water, and manage stress. Regular, gentle exercise can also help your well-being.
|
Lifestyle Change |
Benefit |
|---|---|
|
Healthy Diet |
Supports overall health and potentially reduces inflammation |
|
Stress Management |
Can help reduce frequency of flare-ups |
|
Regular Exercise |
Improves overall well-being and potentially reduces symptom severity |
Managing Flare-Ups
Knowing how to handle flare-ups is important for LCV patients. Spot early signs and act fast, like changing meds or using topical treatments.
Support Resources
Living with LCV can be tough, both physically and emotionally. Having access to support groups, counseling, and educational materials can be very helpful.
By using medical treatment and these strategies, people with LCV can live active and meaningful lives.
Conclusion
Leukocytoclastic Vasculitis (LCV) is a complex condition that affects blood vessels. It leads to symptoms like palpable purpura. Knowing the LCV medical abbreviation is key for both doctors and patients to handle diagnosis and treatment well.
Managing LCV involves finding and avoiding triggers, using medicine, and providing support. Teaching patients about their condition is also important. This shows the need for ongoing research and support.
In short, LCV needs a detailed management plan. This includes correct diagnosis, treatment, and lifestyle changes. By spreading awareness and understanding, we can help those with LCV live better lives. As medical research and care improve, so does our ability to manage LCV effectively.
FAQ
What is Leukocytoclastic Vasculitis (LCV)?
Leukocytoclastic Vasculitis (LCV) is a condition that affects the skin and sometimes other parts of the body. It causes inflammation in the blood vessels.
What does the medical abbreviation LCV stand for?
LCV stands for Leukocytoclastic Vasculitis.
What is the origin of the term “leukocytoclastic”?
The term “leukocytoclastic” comes from the destruction of white blood cells, mainly neutrophils. This is a key feature of LCV.
What are the common causes and triggers of LCV?
LCV can be caused by drugs, infections, autoimmune disorders, and sometimes without a known reason.
What is the hallmark sign of LCV?
The main sign of LCV is a skin rash called palpable purpura. It looks raised and purple.
How is LCV diagnosed?
Doctors use a skin biopsy, lab tests, and sometimes imaging to diagnose LCV.
What are the treatment options for LCV?
Treatment for LCV includes removing triggers, using medicine, and supportive care. New treatments are also being explored.
How can LCV be managed and what are the coping strategies?
Managing LCV means taking care of your skin, making lifestyle changes, and learning to handle flare-ups. Using support resources is also helpful.
What is the impact of LCV on quality of life?
LCV can greatly affect a person’s life, making daily tasks hard and causing discomfort. This is due to the skin symptoms and other symptoms.
Are there any photographic examples of LCV presentations available?
Yes, there are many photos showing how LCV rash can look different in different people.
When should one seek medical attention for suspected LCV?
If symptoms don’t get better or get worse, or if you have fever, joint pain, or kidney problems, see a doctor.
Can LCV be differentiated from other vasculitic rashes?
Yes, LCV can be told apart from other rashes through doctor’s evaluation, skin tests, and lab results.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3776861/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News




























