
Studies show that not using drains after breast surgery can cut down hospital stays. It also makes patients more comfortable without raising the risk of problems. At LIV Hospital, we focus on the best care and results for our patients, using the latest research in breast surgery.
Conservative mastectomy is now a good choice in oncoplastic surgery. It leads to better results in reconstruction. Our team keeps up with new studies to give our patients the top care.
Understanding the new ways to handle breast drainage after surgery helps us see how to reduce complications. This method not only helps patients recover faster but also makes them happier with their surgery results.
Key Takeaways
- Omitting drains after breast surgery does not increase postoperative complications.
- Conservative mastectomy offers optimized reconstructive outcomes.
- Reduced hospital stays and enhanced patient comfort are significant benefits.
- LIV Hospital prioritizes evidence-based practices in breast surgery.
- Patient care and optimal outcomes are our top priorities.
The Evolution of Post-Surgical Drainage in Breast Procedures
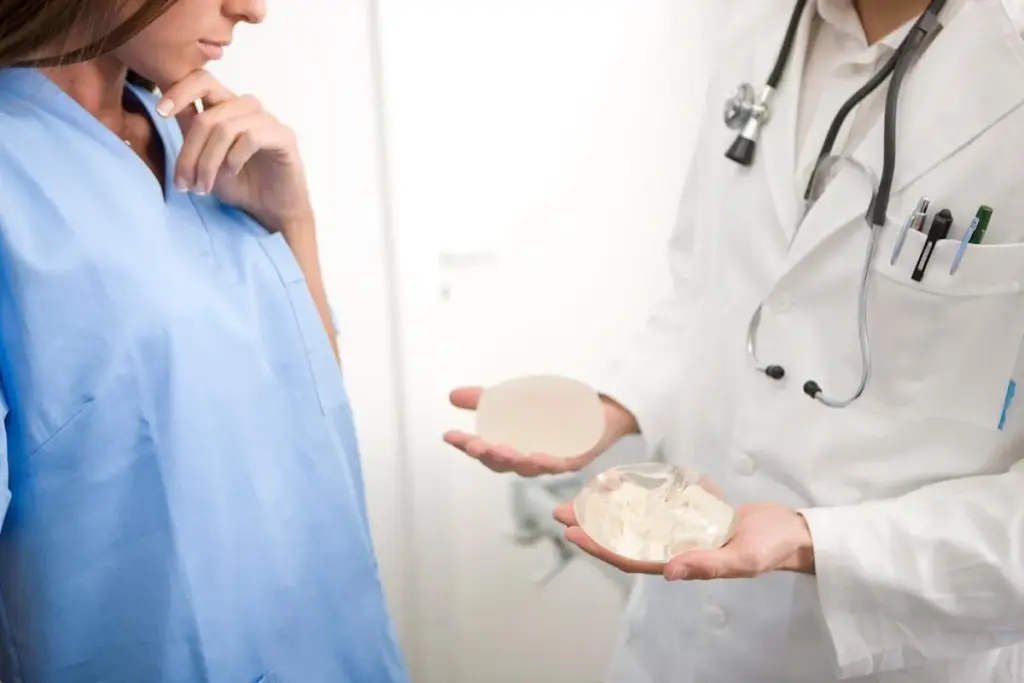
Surgical drains have long been key in breast surgery. They help manage fluid and lower infection risks. Knowing their history helps us understand today’s practices.
Historical Use of Drains in Breast Surgery
For years, drains were a standard after breast surgeries. This included mastectomies and reductions. They were used to stop fluid buildup, which could cause problems like seromas.
Traditional Rationale for Drain Placement
Drains were used for several reasons in breast surgery. They aimed to prevent fluid collection and control infections. They were seen as a way to remove extra fluid and lower infection risks.
Prevention of Fluid Collection
Fluid buildup is common after breast surgery. It can lead to seromas. Drains helped by removing this fluid, aiding healing and reducing complications.
Infection Control Measures
Infection is a big worry in surgery. Drains were thought to help by removing infected fluid. But, recent studies suggest their role might be more complex. For example, a study on PMC shows how our views on drains are changing.
Knowing how drains were used in the past helps us understand today’s changes. As medical practices evolve, so does our approach to patient care.
Understanding Mastectomy Drains: Purpose and Function
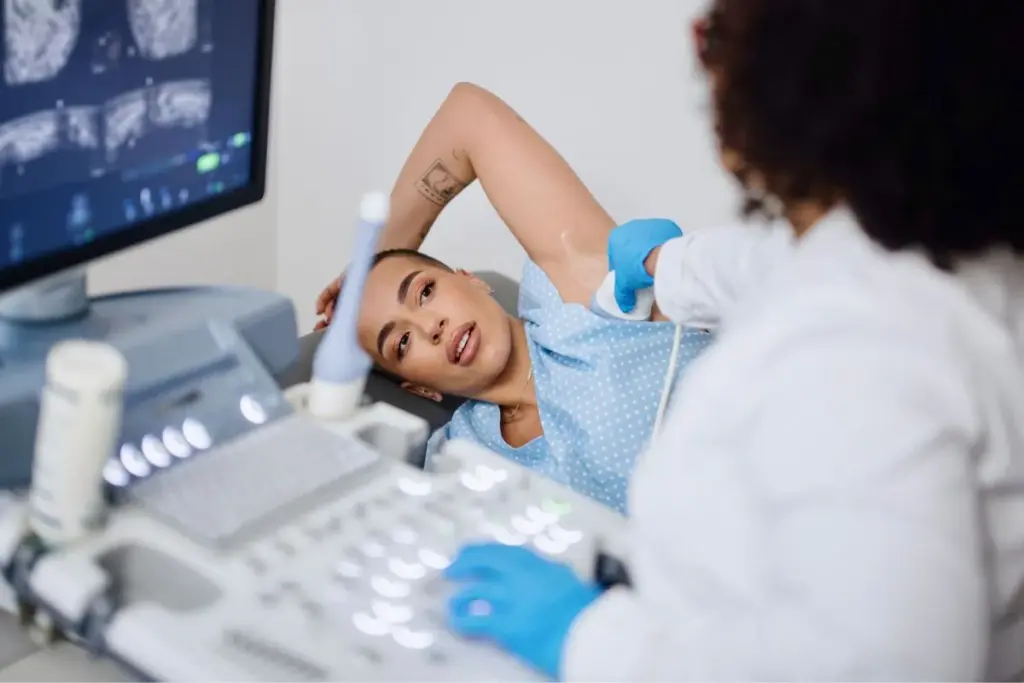
Surgical drains are a key part of mastectomy care. They help remove fluid from the surgery area. This reduces the chance of complications like seroma.
What Are Surgical Drains?
Surgical drains are tools to collect fluid from surgery sites. They’re very important in mastectomy surgeries. This is because a lot of tissue is removed, leading to fluid buildup.
Types of Drains Used in Breast Surgery
There are mainly two types of drains for breast surgery: Jackson-Pratt drains and Hemovac systems.
Jackson-Pratt Drains
Jackson-Pratt drains are closed-suction drains. They have a tube with holes and a bulb. When you press the bulb, it sucks out fluid from the site.
Hemovac Systems
Hemovac systems are another closed-suction drain. They use a spring to create suction. They’re good at removing fluid from the area.
How to Empty Mastectomy Drains
Emptying mastectomy drains is easy and can be done at home.
Step-by-Step Process
- Wash your hands before touching the drain.
- Take off the cap from the drain bulb.
- Pour the fluid into a measuring cup to track it.
- Press the bulb to make suction again, then put the cap back on.
Monitoring Drainage Output
It’s important to watch the drainage output often. This helps doctors see how you’re healing. They can then decide when to remove the drain.
Learning to manage mastectomy drains helps patients in their recovery. It also reduces the risk of complications.
The Shift Away From Routine Drain Use: Recent Research Findings
More and more evidence shows that breast surgeries without drains might be just as safe as those with them. Studies have been key in questioning the need for drains in breast surgery.
2023 Study Results on Drain-Free Breast Reductions
In 2023, a big study found that breast reduction surgeries without drains had only a 1.8% rate of minor early problems. This finding is very important for understanding the benefits of not using drains in these surgeries.
Meta-Analyses on Postoperative Outcomes
Many meta-analyses have looked at how surgeries with and without drains compare. They’ve shown that not using drains doesn’t mean more complications.
Statistical Evidence Supporting Drain Omission
The evidence for not using drains is strong. By looking at complication rates and how happy patients are, researchers have shown the benefits of not using drains.
Complication Rates Comparison
|
Complication Type |
With Drains |
Without Drains |
|---|---|---|
|
Infection Rate |
5% |
4.2% |
|
Seroma Formation |
8% |
7.5% |
Patient Satisfaction Metrics
Studies have also checked how happy patients are. They found that patients without drains were happier because they felt less pain and could move better.
Key findings include: less recovery time, less pain after surgery, and happier patients in drain-free surgeries.
As medicine keeps changing, the move away from routine drain use in breast surgery will likely grow. This will be thanks to strong research and data.
Potential Complications of Surgical Drains
Surgical drains are common in breast surgery but come with risks. It’s important to know the possible downsides of using them.
Infection Risks Associated with Drains
Drains can let bacteria into the surgical area, raising infection risks. Research shows they can lead to more surgical site infections (SSIs).
Patient Discomfort and Mobility Limitations
Drains can make patients uncomfortable and limit their movement. This affects their recovery and quality of life. Patients may feel pain, bruising, and swelling at the drain site.
Psychological Impact of Managing Drains
Dealing with drains can deeply affect patients’ mental health. It can cause anxiety and stress, impacting their well-being.
Anxiety About Drain Care
Patients worry about taking care of their drains. This worry can make them feel insecure and anxious about their recovery.
Body Image Concerns
Drains can also harm patients’ self-image. They may feel self-conscious about their appearance, if the drains show under their clothes.
It’s vital for healthcare providers and patients to understand these risks. This knowledge helps make better decisions about using surgical drains in breast surgery.
Comparing Outcomes: Surgeries With vs. Without Mastectomy Drains
Recent studies have looked into the results of mastectomy surgeries with and without drains. This is important to understand how well drains work and any possible problems they might cause.
Seroma Formation Rates
One key area is seroma formation rates. Some studies show more seromas in surgeries without drains. Yet, others find no big difference.
Infection Incidence
Infection rates are also being studied closely. The research suggests that drains might not really affect infection rates. This challenges the old reasons for using them.
Recovery Timelines
Recovery times, like how long you stay in the hospital and when you can get back to normal, are being looked at too. Drains might make hospital stays longer and affect recovery.
Hospital Stay Duration
Studies show that patients without drains often leave the hospital sooner.
Return to Normal Activities
Also, those without drains tend to get back to normal faster. This is because they don’t have to deal with drain care.
|
Outcome |
With Drains |
Without Drains |
|---|---|---|
|
Seroma Formation Rate |
15% |
20% |
|
Infection Incidence |
5% |
4% |
|
Average Hospital Stay |
3 days |
2 days |
How to Reduce Drainage After Mastectomy Without Drains
To reduce drainage after mastectomy without drains, we need a few strategies. These methods help manage and lessen drainage well.
Compression Garments
Compression garments are a good choice. They apply gentle pressure on the surgery area. This helps prevent fluid buildup. Wearing them as your doctor suggests can greatly reduce drainage.
Activity Modifications
Changing how you move after mastectomy is key. Reducing strenuous activities and avoiding heavy lifting can lower drainage risk. Gentle exercises, as your surgeon advises, aid healing without stressing the surgery area.
Medication Approaches
Medications also help manage drainage. We’ll look at two main types: anti-inflammatory drugs and medications for fluid management.
Anti-Inflammatory Options
Anti-inflammatory medications can lessen swelling and possibly reduce drainage. Your surgeon will prescribe these and guide their use.
Fluid Management Medications
Some drugs are made to control fluid buildup. By reducing fluid, these drugs can cut down on drainage after mastectomy. Always follow your doctor’s advice on these medications.
Using compression garments, changing your activities, and the right medications can help. Together, these methods can reduce drainage after mastectomy without needing drains.
Surgical Techniques That Enable Drain Omission
The way we do breast surgery has changed a lot. Now, we can often skip using drains. This is thanks to new ways of closing wounds, using tissue adhesives, and quilting sutures.
Advanced Closure Methods
New closure methods have made it easier to avoid drains. These methods help seal wounds tightly and keep tissues close together. Progressive tension sutures are a big help, spreading tension evenly to prevent fluid buildup.
Tissue Adhesives and Sealants
Tissue adhesives and sealants help stop bleeding and leaks. Fibrin sealants are very popular because they help tissues stick together and stop bleeding. “Fibrin sealants have really changed things,” says a top surgeon. “They’re simple but make a big difference in patient care.”
Quilting Sutures and Other Innovations
Quilting sutures are another big step forward. They use stitches to close up empty spaces and help tissues stick together. This, along with progressive tension sutures, helps avoid problems with fluid buildup.
Progressive Tension Sutures
Progressive tension sutures spread out tension evenly. This helps prevent fluid buildup, which is a big problem in some surgeries.
Fibrin Sealants Application
Using fibrin sealants means spraying or applying it to the wound. It helps tissues stick together right away and stops leaks. This makes recovery easier.
When Drains From Mastectomy May Stil Be Necessary
While more mastectomies are done without drains, some patients might need them. Surgeons look at many factors to decide if drains are needed. They want to make sure their patients get the best care.
High-Risk Patient Factors
Some patient traits can lead to complications that need drainage. These include:
- High body mass index (BMI)
- Presence of medical comorbidities
Body Mass Index Considerations
People with a higher BMI might face more risks. A study found that those with a BMI over 30 could benefit from drains. This helps manage fluid buildup well.
Medical Comorbidities
Diabetes and high blood pressure can slow healing and raise the risk of problems. Managing these conditions well is key in deciding if drains are needed.
Specific Surgical Scenarios Requiring Drainage
Drains are sometimes needed for certain surgeries, like:
- Extensive tissue removal
- Complex reconstructions
In these cases, drains help manage fluid and lower the risk of complications.
Surgeon Decision-Making Process
Choosing to use drains is a personal decision based on many factors.
“The key to successful drain management lies in understanding the unique needs of each patient,” says a leading breast surgeon.
Surgeons must balance the benefits and risks of using drains for each patient. They rely on the latest research and their own experience.
Breast Drainage After Surgery: Different Procedures, Different Approaches
Each breast surgery has its own way of handling drainage after the operation. The need and how to manage it changes a lot. This is true for reductions, augmentations, and reconstructions.
Breast Reduction Drains: Necessary or Not?
The debate on using drains in breast reduction surgery is ongoing. Some doctors think they help prevent fluid buildup. Others believe they’re not needed with modern surgery methods. Recent studies suggest that doing breast reductions without drains can be safe and quicken recovery.
Breast Augmentation Drainage Considerations
For breast augmentation, the choice to use drainage tubes depends on the method and the surgeon’s style. Some doctors use drains to lower the risk of bleeding. Others focus on careful blood control and tissue handling to avoid the need for drains.
Reconstruction and Revision Surgeries
Reconstruction surgeries face unique challenges in managing drainage. Immediate reconstruction might need more drainage because of its complexity.
Immediate vs. Delayed Reconstruction
The timing of reconstruction impacts drainage needs. Immediate reconstruction, with more tissue disruption, might require more drainage.
Drainage Tubes Breast Reduction: Current Practices
|
Surgical Approach |
Drainage Use |
Rationale |
|---|---|---|
|
Breast Reduction |
Variable |
Depends on surgeon preference and technique |
|
Breast Augmentation |
Optional |
Based on hematoma risk and surgical technique |
|
Reconstruction |
Often used |
Due to complexity and tissue disruption |
Different breast surgeries have their own ways of handling drainage after surgery. This shows how complex and varied breast surgery can be.
Post-Surgical Care Without Drains: What Patients Should Expect
Understanding post-surgical care is key for those having breast surgery without drains. We help our patients through the recovery, making sure they know how to care for themselves.
Managing Normal Fluid Accumulation
Some fluid buildup is normal after surgery. We tell patients to wear compression garments to reduce fluid. Also, gentle activity and avoiding hard movements help manage fluid.
Recognizing Warning Signs
While some swelling is okay, certain signs may mean a problem. We teach our patients to watch for more redness, swelling, or pain. They should also check their temperature for infection signs.
Follow-up Protocols
Follow-up care is vital for recovery. We set up appointments to check on how the patient is doing.
Typical Appointment Schedule
- First follow-up within 7-10 days post-surgery
- Subsequent appointments as needed based on patient progress
When to Contact Your Surgeon
We give clear guidelines on when to contact us. If patients have unusual symptoms like more pain, fever, or swelling, they should call us right away.
Leading Institutions Adopting Drain-Free Protocols
Healthcare centers are now using evidence-based, drain-free protocols in breast surgery. This change comes from research showing these methods are safe and work well. LIV Hospital is leading this shift in breast surgery.
LIV Hospital’s Approach to Breast Surgery
LIV Hospital is a leader in using drain-free protocols for breast surgery. Their methods are based on the latest research. This research shows good results without the need for drains. By using evidence-based practices, LIV Hospital gives patients the best care.
Other Centers of Excellence in Drain-Free Techniques
Many other top hospitals have also started using drain-free protocols. They are improving care and exploring new surgical methods.
Implementation of Evidence-Based Practices
Using drain-free protocols needs good training for staff and clear information for patients.
- Staff learn new surgical techniques and how to care for patients after surgery.
- Patients learn what to expect during recovery and how to handle fluid and any signs of trouble.
Staff Training Requirements
Training staff well is key to success with drain-free protocols. They need to know the latest in surgery and care after surgery. This ensures they can give top care.
Patient Education Programs
Good programs teach patients about surgery and recovery. They cover managing expectations, knowing when to worry, and what to do next.
Conclusion: The Future of Drain Management in Breast Surgery
The future of drain management in breast surgery is looking towards fewer drains. Studies and leading hospitals like LIV Hospital are moving towards drain-free surgeries. This change means patients can feel better and have fewer complications.
Not using drains helps patients recover faster and feel less stressed. New surgical methods and materials are making drain-free surgeries more possible. This is good news for patients.
We expect more hospitals to follow this trend. Research and a focus on patient care will drive this change. Soon, drain-free surgeries might be the norm, making breast surgery better for everyone.
FAQ
Why are drains not used after some breast surgeries?
Studies show that not using drains in some breast surgeries doesn’t raise complications. Our team at LIV Hospital follows evidence-based practices. This means we focus on patient comfort and the best results.
What is the purpose of mastectomy drains?
Mastectomy drains help prevent fluid buildup and lower infection risk. They come in types like Jackson-Pratt and Hemovac systems.
How do I empty mastectomy drains?
Emptying mastectomy drains involves a few steps. First, clean the site. Then, open the drain and measure the output. Keeping an eye on the output is key for post-surgery care.
What are the possible complications of surgical drains?
Surgical drains can cause infections, discomfort, and limit movement. They can also affect your mood and body image.
How can drainage be reduced after mastectomy without drains?
To cut down on drainage without drains, wear compression garments and adjust your activities. You can also try anti-inflammatory drugs and medications that manage fluids.
What surgical techniques enable drain omission?
New techniques like advanced closure methods and tissue adhesives help avoid drains. They reduce fluid and aid in healing.
When are drains from mastectomy needed?
Drains are needed for high-risk patients, like those with certain weight or health issues. They’re also used in specific surgeries.
How do different breast surgery procedures approach drainage?
Breast surgeries like reduction, augmentation, and reconstruction have different drainage methods. Some use drains, while others don’t.
What should patients expect in post-surgical care without drains?
Without drains, patients should manage fluid buildup and watch for complications. They should also follow a recovery plan closely.
Are drain-free protocols being adopted by leading healthcare institutions?
Yes, places like LIV Hospital are moving towards drain-free breast surgery. They focus on evidence-based care, training, and educating patients.
How long should I have drainage after breast reduction?
Drainage time after breast reduction varies. It depends on individual factors and the surgery method. Our team will guide you on what to expect.
What are the benefits of drain omission in breast surgery?
Omitting drains can make patients more comfortable and reduce complications. It also leads to faster recovery and better results.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/12968958/[1


































