
Neuroblastoma is a type of cancer that develops in certain nerve cells. It often affects young children. This makes it a big worry in pediatric oncology. Childhood cancer statistics show it’s a top cause of illness in kids most common solid tumor children.
Receiving a diagnosis of a pediatric solid tumor can be an overwhelming experience, highlighting the importance of understanding this condition. As a top healthcare provider, we’re here to help. We offer full support and the latest treatments for patients from around the world.
Key Takeaways
- Neuroblastoma is a significant concern in pediatric oncology.
- Childhood cancer statistics highlight the importance of early detection.
- Advanced treatment options are available for pediatric solid tumors.
- Comprehensive support is key for international patients seeking care.
- Our healthcare provider is dedicated to delivering world-class treatment.
Overview of Pediatric Cancer
Cancer in children is a big concern that needs to be understood well. It’s rare but serious, affecting kids all over the United States.
Childhood cancer isn’t just one disease. It’s many different kinds, each with its own challenges. Knowing about these cancers helps doctors find better treatments and support families.
Prevalence of Childhood Cancer in the United States
Childhood cancer is a top cause of death in kids in the U.S. About 11,000 kids get cancer every year. Though it’s a small part of all cancers, it has a big impact on families.
| Age Group | Most Common Cancer Types | Estimated Annual Diagnoses |
| 0-4 years | Neuroblastoma, Leukemia | 2,500 |
| 5-9 years | Leukemia, Brain Tumors | 2,200 |
| 10-14 years | Leukemia, Lymphoma | 2,000 |
| 15-19 years | Lymphoma, Brain Tumors | 2,300 |
Distinction Between Solid and Hematologic Malignancies
Pediatric cancers fall into two main groups: solid tumors and hematologic malignancies. Solid tumors are tumors that form a mass. Hematologic malignancies affect the blood and bone marrow.
Solid tumors in kids include neuroblastoma and rhabdomyosarcoma. These tumors can grow in different parts of the body. Hematologic malignancies, like leukemia, affect the blood and lymph system.
It’s important to know the difference between these cancers. This helps doctors choose the right treatment and predict how well a child will do. Each type needs a special approach because of its unique characteristics.
The Most Common Solid Tumor in Children
Neuroblastoma is the most common solid tumor outside the brain in kids. It’s important to know about it. This cancer starts from nerve cells that are not fully grown. It can happen in places like the adrenal glands, neck, chest, or pelvis.
Looking into neuroblastoma helps us understand its impact on kids. The numbers tell us how big of a deal it is in childhood cancers.
Neuroblastoma: Leading the Statistics
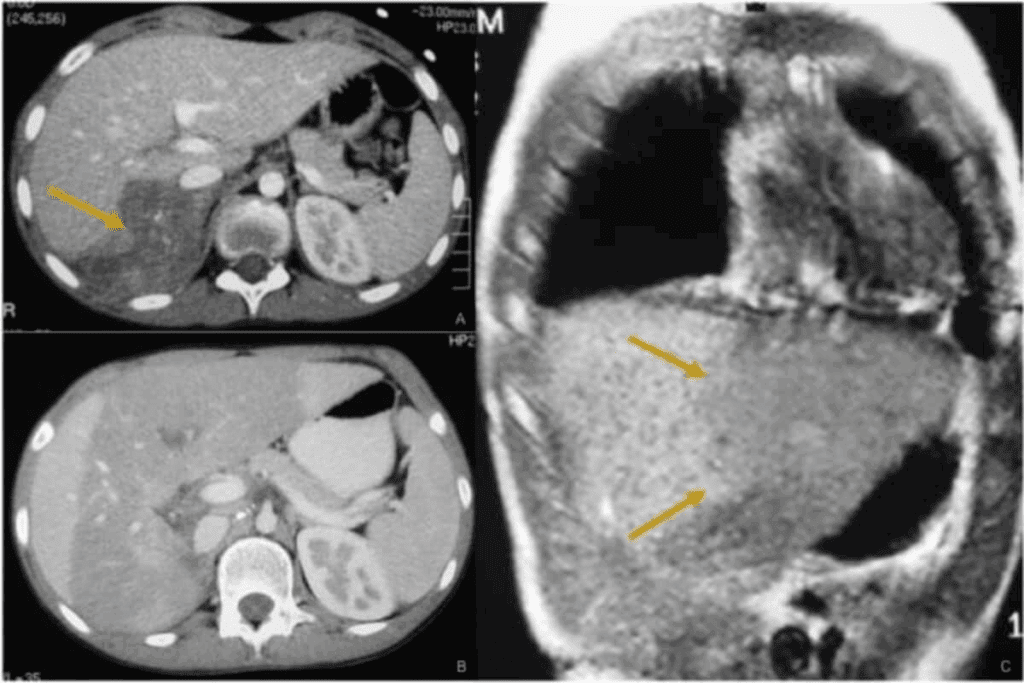
Neuroblastoma is a big deal in childhood cancers, hitting kids under five hard. It’s the top cancer in babies under one. Some cases are found before birth, while others are found later.
| Age at Diagnosis | Incidence Rate |
| Less than 1 year | 30% |
| 1-4 years | 50% |
| 5-9 years | 15% |
| 10 years and older | 5% |
Age Distribution and Demographics
Most kids with neuroblastoma are under five, with a median age of 18 months. It’s more common in boys than girls. The numbers also change based on ethnicity and where you live.
Knowing these details helps us find ways to prevent and treat neuroblastoma. More research is needed to help kids with this cancer.
Understanding Neuroblastoma
To fight neuroblastoma, we must first understand its biology. It’s a cancer that starts in neural crest cells. These cells are key to the nervous system’s growth.
Origin in Neural Crest Cells
Neural crest cells form early in an embryo. They move to different parts of the body. There, they become various cell types, like neurons and glial cells.
When these cells don’t mature right, they turn cancerous. This leads to neuroblastoma. The tumor can pop up anywhere in the sympathetic nervous system. This includes the adrenal glands, neck, chest, abdomen, and pelvis.
Common Sites of Tumor Development
Neuroblastoma can show up in many places. But it often starts in the adrenal glands, on top of the kidneys. It also likes the neck, chest, abdomen, and pelvis.
The tumor’s spot can change how the disease feels and looks. For example, an abdomen tumor might cause swelling or pain. A chest tumor could make breathing hard.
The variety in where tumors grow shows how complex neuroblastoma is. It comes from cells that move around in the embryo. Knowing where tumors often appear helps find and treat neuroblastoma early.
Risk Factors for Developing Neuroblastoma
Knowing the risk factors for neuroblastoma is key for early detection and prevention. This disease is complex, influenced by genetics and environment.
Genetic Predisposition
Genetics play a big role in neuroblastoma. Certain genetic mutations raise the risk. For example, ALK and PHOX2B gene mutations are linked to higher risk.
Families with neuroblastoma history are at higher risk too. But most cases are not linked to family history.
| Genetic Mutation | Associated Risk |
| ALK gene mutation | Increased risk of neuroblastoma |
| PHOX2B gene mutation | Increased risk of neuroblastoma |
Environmental Factors
Research is ongoing to find environmental links to neuroblastoma. Exposure to chemicals and radiation might be risk factors. Prenatal drug exposure and maternal health could also play a role.
Current Research: Studies are looking into environmental exposures and neuroblastoma. This could lead to preventive strategies.
Understanding genetic and environmental risks helps in early detection and prevention of neuroblastoma.
Clinical Presentation and Symptoms
Neuroblastoma is the most common solid tumor outside the brain in kids. It shows different symptoms based on where the tumor is and how big it is. Spotting these signs early is key for a quick diagnosis and treatment.
Common Signs of Neuroblastoma
Kids with neuroblastoma might show a few signs. These include:
- Abdominal mass or swelling
- Bone pain or limping
- Proptosis (bulging eyes)
- Periorbital bruising
- Spinal cord compression symptoms, such as weakness or paralysis
These signs can be hard to spot because they’re not specific. A detailed check-up is needed to confirm the diagnosis.
Symptoms Based on Tumor Location
The place where the tumor starts affects the symptoms. For example:
- Tumors in the adrenal gland or abdominal sympathetic chain can cause stomach pain.
- Thoracic tumors might lead to breathing problems like coughing or shortness of breath.
- Pelvic tumors can cause issues with the bladder or bowel.
- Cervical or thoracic tumors can lead to Horner syndrome, with symptoms like droopy eyelids, small pupils, and no sweat.
Knowing how symptoms relate to tumor location helps doctors suspect neuroblastoma. This leads to the right tests for diagnosis.
Paraneoplastic Syndromes
Some patients with neuroblastoma have paraneoplastic syndromes. These are rare conditions caused by substances from the tumor affecting other parts of the body. Common ones include:
- Opsoclonus-myoclonus syndrome (OMS), with fast, odd eye movements and muscle twitches.
- Secretory diarrhea caused by vasoactive intestinal peptide (VIP).
Spotting these syndromes is important. They can be the first sign of neuroblastoma, helping in early diagnosis.
In summary, neuroblastoma shows different symptoms based on the tumor’s location and paraneoplastic syndromes. Recognizing these symptoms early is vital for a quick diagnosis and treatment.
Other Common Pediatric Solid Tumors
Other common tumors in kids include Wilms tumor, brain tumors, rhabdomyosarcoma, and retinoblastoma. These tumors are serious and need quick diagnosis and treatment.
Wilms Tumor (Nephroblastoma)
Wilms tumor, or nephroblastoma, is a kidney cancer in kids. It’s a common kidney tumor in children.
- Typically presents in children aged 3 to 4 years
- Often associated with genetic mutations, such as those affecting the WT1 gene
- May be part of a syndrome, such as WAGR (Wilms tumor, Aniridia, Genitourinary anomalies, and mental Retardation) syndrome
Brain and Central Nervous System Tumors
Brain and CNS tumors are cancers in the brain and spinal cord. They are the second most common cancer in kids.
These tumors can be benign or malignant. They vary in aggressiveness and treatment needs.
| Type | Characteristics |
| Medulloblastoma | A highly malignant tumor originating in the cerebellum |
| Glioma | A broad category of tumors arising from glial cells, ranging from low-grade to high-grade |
| Ependymoma | Tumors arising from the ependymal cells lining the ventricles and central canal of the spinal cord |
Rhabdomyosarcoma
Rhabdomyosarcoma is a soft tissue sarcoma from skeletal muscle precursors. It’s the most common soft tissue sarcomain kids.
- Can occur in any part of the body, but most commonly affects the head and neck, urinary tract, or limbs
- Has several subtypes, including embryonal and alveolar rhabdomyosarcoma
- Treatment often involves a combination of surgery, chemotherapy, and radiation therapy
Retinoblastoma
Retinoblastoma is a rare eye cancer in young children. It starts in the retina, the light-sensitive tissue at the back of the eye.
Early detection is key for effective treatment and saving vision.
- Often presents with leukocoria (white pupillary reflex) or strabismus
- Can be hereditary or sporadic, with the hereditary form often associated with germline mutations in the RB1 gene
- Treatment options include chemotherapy, laser therapy, cryotherapy, and enucleation in advanced cases
Comparative Analysis of Most Common Solid Tumor Children
We looked into the most common solid tumors in kids. This study gives us key insights into their spread. We focused on the types of tumors, how they change with age, and where they are more common in the U.S.
Statistical Breakdown by Tumor Type
Kids can get different types of solid tumors. Neuroblastoma is the top one outside the brain. It makes up about 7% of all childhood cancers. Other common ones are Wilms tumor, rhabdomyosarcoma, and retinoblastoma.
Our research used data from the Surveillance, Epidemiology, and End Results (SEER) program. It shows:
- Neuroblastoma: 10.2 cases per million children per year
- Wilms Tumor: 7.1 cases per million children per year
- Rhabdomyosarcoma: 4.5 cases per million children per year
- Retinoblastoma: 3.4 cases per million children per year
Age-Related Patterns
The age when kids get these tumors varies a lot. Neuroblastoma and retinoblastoma often hit kids under 5. But Wilms tumor and rhabdomyosarcoma can happen in kids of any age.
Early detection is key:
- Neuroblastoma: Most common in 0-4 years
- Wilms Tumor: Most common in 3-4 years
- Rhabdomyosarcoma: Peaks in 2-5 and 15-19 years
- Retinoblastoma: Usually diagnosed by age 5
Geographical Variations in the United States
Some areas in the U.S. see more of these tumors than others. The SEER data shows this. Some states have higher rates for certain tumors.
“Regional differences in cancer incidence may be attributed to various factors, including genetic predisposition, environmental exposures, and access to healthcare services.”
Our study found that:
| State | Neuroblastoma Incidence | Wilms Tumor Incidence |
| California | 11.5 cases/million/year | 7.5 cases/million/year |
| New York | 10.8 cases/million/year | 7.2 cases/million/year |
Knowing these differences helps plan better healthcare and focus on prevention.
Diagnostic Approaches and Workup
Diagnosing pediatric solid tumors like neuroblastoma is key for good treatment. It uses many diagnostic methods. We’ll look at how these methods help identify and understand these tumors.
Initial Evaluation and Physical Examination
The first step is a detailed check-up and physical exam. We look at the child’s health for signs of a tumor. This includes checking for masses, swelling, or neurological issues.
Imaging Techniques
Imaging is vital for finding neuroblastoma. We use different imaging tools to see the tumor and how big it is.
- Ultrasound: Often used first, mainly for belly masses.
- Computed Tomography (CT) Scan: Gives detailed images to see the tumor’s size and where it is.
- Magnetic Resonance Imaging (MRI): Shows detailed images, great for soft tissue and brain effects.
- Metaiodobenzylguanidine (MIBG) Scan: A special scan that’s very good at finding neuroblastoma.
Laboratory Tests
Lab tests are key for diagnosing and understanding neuroblastoma. We do tests to learn about the tumor’s biology.
- Complete Blood Count (CBC): Checks overall health and blood cell counts.
- Urine Tests: Looks for high levels of catecholamines or their breakdown products, linked to neuroblastoma.
- Blood Chemistry Tests: Checks liver and kidney function and other metabolic factors.
- Tumor Markers: Measures substances made by neuroblastoma cells, like lactate dehydrogenase (LDH).
Biopsy and Histopathology
A biopsy is the main way to diagnose neuroblastoma. We take tissue samples and study them to confirm the diagnosis and understand the tumor.
- Histological Examination: Shows the tumor’s cell structure and how aggressive it is.
- Molecular Studies: Includes genetic tests to find specific mutations or chromosomal changes in neuroblastoma.
By using these methods together, we can accurately diagnose neuroblastoma. Then, we can plan a treatment that fits the child’s needs.
Staging and Risk Classification
Staging and risk stratification are key in managing neuroblastoma. They help decide treatment plans and predict outcomes. These systems help us understand how far the disease has spread and what the future might hold.
International Neuroblastoma Staging System
The International Neuroblastoma Staging System (INSS) is a common way to classify neuroblastoma. It looks at how far the tumor has spread and if it can be removed. This helps doctors know how to treat the disease and what to expect.
| Stage | Description |
| 1 | Localized tumor with complete gross excision |
| 2A | Localized tumor with incomplete gross excision |
| 2B | Localized tumor with or without complete gross excision, with ipsilateral lymph node involvement |
| 3 | Unresectable unilateral tumor infiltrating across the midline, or localized unilateral tumor with contralateral lymph node involvement |
| 4 | Any primary tumor with dissemination to distant lymph nodes, bone, bone marrow, liver, skin, or other organs |
| 4S | Localized primary tumor with dissemination limited to skin, liver, or bone marrow in children younger than 1 year |
The INSS has made it easier to compare treatment results worldwide. It helps doctors understand how well treatments work.
Risk Stratification Approaches
Risk stratification in neuroblastoma looks at several factors. These include age, stage, tumor type, and genetics. It helps doctors decide how intense the treatment should be.
- Low-Risk: Patients with a good chance of being cured with less treatment.
- Intermediate-Risk: Patients needing more treatment, with a moderate chance of the disease coming back.
- High-Risk: Patients with a high chance of the disease coming back, needing very aggressive treatment.
Prognostic Factors
Several factors help predict how well a patient will do with neuroblastoma. These include age, stage, MYCNamplification, and tumor type. Knowing these helps doctors tailor treatments to each patient.
“The presence of MYCN amplification is associated with a more aggressive disease course and poorer prognosis in neuroblastoma patients.”
Source: Journal of Clinical Oncology
By using staging, risk stratification, and prognostic factors, we can create a treatment plan that meets each patient’s needs. This approach helps improve outcomes for neuroblastoma patients.
Treatment Modalities for Neuroblastoma
Neuroblastoma treatment involves many steps. We use different methods to fight this complex cancer. Each patient gets a treatment plan that fits their needs.
Surgical Approaches
Surgery is key for treating neuroblastoma, mainly for tumors that are close to the surface. The goal is to remove the tumor completely without harming nearby important areas. We use new surgical methods to make recovery easier and better.
Key considerations for surgical approaches include:
- Tumor location and size
- Involvement of surrounding vital structures
- Patient’s overall health and age
Chemotherapy Protocols
Chemotherapy is a main part of treating neuroblastoma, mainly for those with high-risk or spread-out disease. We use different chemotherapy plans to kill cancer cells. The plan depends on how high-risk the disease is and how well the patient responds to treatment.
Chemotherapy protocols may include:
- Induction chemotherapy to reduce tumor size
- Consolidation chemotherapy to eliminate residual disease
- Maintenance chemotherapy to prevent relapse
Radiation Therapy
Radiation therapy is also a big part of treating neuroblastoma. It helps control local disease and ease symptoms. We use new radiation methods to target the tumor well and protect healthy tissues.
Radiation therapy is useful for:
- Tumors that are hard to remove or have leftover disease after surgery
- Palliative care to ease pain and other symptoms
Immunotherapy
Immunotherapy is a new area in neuroblastoma treatment. It uses the body’s immune system to fight cancer. We are looking into different immunotherapies, like monoclonal antibodies and CAR-T cell therapy, to help patients with high-risk neuroblastoma.
Immunotherapy offers several benefits:
- Targeted killing of neuroblastoma cells
- Less harm compared to traditional chemotherapy
- Potential for long-term disease control
In conclusion, treating neuroblastoma needs a detailed and personalized approach. By knowing the good and bad of each treatment, we can make plans that help patients live better and longer.
Treatment Approaches for Other Pediatric Solid Tumors
Managing different types of pediatric solid tumors needs a mix of treatments. This mix helps get the best results for kids.
Wilms Tumor Management
Wilms tumor, or nephroblastoma, is a common kidney cancer in kids. Treatment usually includes surgery, chemotherapy, and sometimes radiation. The exact plan depends on the tumor’s stage and type.
Surgical removal is often the first step. It aims to take out the tumor and check its type. Chemotherapy is then used before and after surgery to kill any cancer cells left.
Brain Tumor Therapies
Brain tumors in kids need careful treatment because of their location and possible long-term effects. Treatments include surgery, radiation, and chemotherapy. The choice depends on the tumor’s type, location, and how aggressive it is.
Surgery tries to remove as much of the tumor as possible without harming the brain. Radiation therapy and chemotherapy target any cancer cells left behind to lower the chance of it coming back.
Sarcoma Treatment Strategies
Sarcomas are tumors from mesenchymal cells. Treatment for kids includes surgery, chemotherapy, and radiation. The plan varies based on the sarcoma’s type and stage.
Chemotherapy before surgery helps shrink the tumor. Radiation therapy might be used with surgery to control the disease locally.
Multimodal Approach to Pediatric Solid Tumors
For pediatric solid tumors, a mix of treatments is key. This mix includes surgery, chemotherapy, radiation, and sometimes immunotherapy. It aims for the best results.
This approach boosts survival rates and lowers the risk of cancer coming back. It lets doctors tailor treatment to each child’s needs.
In summary, treating pediatric solid tumors needs a detailed and mixed approach. By using different treatments together, we can better help kids with these serious diseases.
Prognosis and Survival Outcomes
Children with solid tumors have seen big improvements in treatment. This is good news for families and doctors dealing with pediatric cancer. Knowing about these improvements helps everyone involved.
Factors Affecting Prognosis
Receiving a diagnosis of a pediatric solid tumor can be an overwhelming experience, highlighting the importance of understanding this condition.
Tumor biology is very important too. Some tumors are easier to treat than others. For example, some genetic traits can make a tumor more or less likely to respond to treatment.
How well a child does at first treatment is also a clue. A good start often means a better chance of recovery. Some genetic changes, like MYCN in neuroblastoma, can make the disease worse.
Survival Rates by Tumor Type and Stage
Survival rates for kids with solid tumors depend on the type and how far it has spread. We’ve made big strides in making these rates better. Here’s a look at 5-year survival rates for some common tumors.
| Tumor Type | Localized | Regional | Distant |
| Neuroblastoma | 95% | 80-90% | 50-60% |
| Wilms Tumor | 90-95% | 80-90% | 60-70% |
| Rhabdomyosarcoma | 80-90% | 60-80% | 30-50% |
Recurrence and Relapse Patterns
Recurrence is a big worry for kids with solid tumors. The timing and pattern of recurrence differ by tumor type and treatment. Some tumors come back sooner, while others may take longer.
We’re always learning more about when and how tumors come back. Our goal is to find better ways to treat relapse. This includes new treatments and clinical trials.
Late Effects and Long-term Complications
Children treated for solid tumors may face late effects that affect their quality of life. As survival rates improve, it’s key to tackle these long-term issues for full care.
Physical Late Effects
Treatment for pediatric solid tumors can lead to physical late effects. These include:
- Growth and development issues
- Organ dysfunction (e.g., cardiac, renal)
- Secondary cancers
- Neurological impairments
Table: Common Physical Late Effects by Treatment Modality
| Treatment Modality | Potential Late Effects |
| Chemotherapy | Cardiac dysfunction, ototoxicity |
| Radiation Therapy | Growth abnormalities, secondary cancers |
| Surgery | Organ dysfunction, adhesions |
Psychological Impact
Receiving a diagnosis of a pediatric solid tumor can be an overwhelming experience, highlighting the importance of understanding this condition.
Quality of Life Considerations
Improving the quality of life for pediatric solid tumor survivors is complex. It involves physical, emotional, and social needs. We must look at education, work, and social life too.
Long-term care is vital for managing late effects and boosting quality of life. Knowing the long-term treatment effects helps us offer specific support. This way, we can improve the well-being of these individuals.
Screening and Prevention Strategies
Screening and prevention are key in finding and treating pediatric solid tumors early. Early detection can greatly improve treatment success and survival rates for kids with these cancers.
Current Screening Recommendations
Receiving a diagnosis of a pediatric solid tumor can be an overwhelming experience, highlighting the importance of understanding this condition.
For neuroblastoma, a common childhood cancer, urine tests are used to find catecholamines. These tests help find tumors early, when they are easier to treat.
| Tumor Type | Screening Method | Target Population |
| Neuroblastoma | Urine catecholamines, Ultrasound | Infants, high-risk children |
| Wilms Tumor | Ultrasound | Children with genetic predisposition |
| Retinoblastoma | Ophthalmologic examination | Children with family history |
Genetic Counseling for High-Risk Families
Receiving a diagnosis of a pediatric solid tumor can be an overwhelming experience, highlighting the importance of understanding this condition.
For instance, families with a history of retinoblastoma can get genetic tests to see if their kids are at risk. Genetic counseling also offers emotional support and advice on family planning and managing risk.
Research on Prevention Approaches
Research is ongoing to find ways to prevent pediatric solid tumors. It looks into environmental factors and genetic risks. Clinical trials are working on new ways to detect and treat these cancers early.
Prevention might include using medicines to stop tumors from growing in high-risk people. Understanding the genetics of these tumors is also key for finding prevention strategies.
Current Research and Emerging Therapies
The field of pediatric oncology is changing fast. New research brings hope to kids with solid tumors. We now understand these cancers better, leading to better treatments.
Advances in Molecular Understanding
Receiving a diagnosis of a pediatric solid tumor can be an overwhelming experience, highlighting the importance of understanding this condition.
This knowledge helps us use precision medicine. Treatments are now made just for each patient’s tumor.
Targeted Therapies in Development
Targeted therapies are a big hope. They aim to hit cancer’s weak spots, reducing side effects. These therapies target specific genetic flaws that tumors rely on.
| Therapy | Target | Tumor Type |
| Crizotinib | ALK | Neuroblastoma |
| Lenvatinib | VEGFR | Various Solid Tumors |
| Selumetinib | MEK | Low-grade Gliomas |
Immunotherapy Innovations
Immunotherapy is a strong tool against cancer, including in kids. Scientists are looking into CAR T-cell therapy, checkpoint inhibitors, and vaccines.
Early trials show great promise. Some patients have seen big tumor drops or even complete remission.
Promising Clinical Trials
Many trials are testing new treatments for solid tumors in kids. They’re checking if new combos of therapies work well.
For example, a Phase III trial is using a mix of chemo and immunotherapy for neuroblastoma. Early signs are very encouraging.
Support Resources for Families
When a child is diagnosed with a solid tumor, it’s a big shock. Families need strong support resources to cope.
Dealing with pediatric cancer treatment is tough. Families need help from many places. This includes national groups, financial aid, emotional support, and learning tools.
National Organizations and Foundations
Many national groups help families with pediatric cancer. Some key ones are:
- The Children’s Cancer and Blood Foundation
- The National Children’s Cancer Society
- The Pediatric Cancer Research Foundation
Financial Assistance Programs
Financial help is key for many families. Groups provide aid with:
| Program | Description | Benefit |
| Cancer Financial Assistance | Helps with treatment costs | Reduces financial burden |
| Travel Assistance | Aids with travel expenses for treatment | Facilitates access to care |
| Medication Assistance | Assists with medication costs | Ensures continuity of treatment |
Psychosocial Support Services
Psychosocial support is very important for families with pediatric cancer. Services include:
- Counseling and therapy
- Support groups for families
- Mental health services for children and siblings
These services help families deal with the emotional side of cancer treatment.
Educational Resources
Educational resources give families the knowledge they need. They include:
- Informational materials on pediatric cancer
- Workshops and seminars on cancer care
- Online resources and webinars
With all this support, families can face pediatric cancer challenges better.
Conclusion
It’s key to understand pediatric solid tumors to give kids the best care. Neuroblastoma is the top solid tumor in kids. Many things can affect how it grows and spreads.
We talked about the need for a complete care plan for kids with solid tumors. This includes surgery, chemo, radiation, and immunotherapy. Also, support for their mental health and learning needs is important.
Helping kids with solid tumors needs teamwork from doctors, researchers, and families. By learning more and finding better treatments, we can make life better for these kids.
FAQ
What is the most common solid tumor in children?
Neuroblastoma is the most common solid tumor outside the brain in kids. It starts from neural crest cells.
What are the common signs and symptoms of neuroblastoma?
Symptoms depend on where the tumor is. They can be an abdominal mass, bone pain, bulging eyes, or nerve problems. Some kids might also have other health issues.
How is neuroblastoma diagnosed?
Doctors use imaging like ultrasound, CT, or MRI to find the tumor. They also check urine for certain substances and do a biopsy to confirm.
What are the treatment modalities for neuroblastoma?
Treatment includes surgery, chemotherapy, radiation, and immunotherapy. These are often used together, based on how serious the tumor is.
What is the prognosis for children with neuroblastoma?
The outlook depends on the child’s age, how advanced the tumor is, and other factors. Survival rates range from under 50% for high-risk cases to over 90% for low-risk ones.
Are there other common pediatric solid tumors beside neuroblastoma?
Yes, other common ones include Wilms tumor, brain tumors, rhabdomyosarcoma, and retinoblastoma.
How are pediatric solid tumors staged?
Staging varies by tumor type. For example, neuroblastoma uses a specific staging system. Wilms tumor is staged based on how big the tumor is and its appearance under a microscope.
What are the late effects of treating pediatric solid tumors?
Late effects can be physical, like organ damage, or emotional, like anxiety or depression. They affect the child’s quality of life and need ongoing care.
Are there screening recommendations for pediatric solid tumors?
Yes, there are screenings for some tumors, like neuroblastoma in babies. Genetic counseling is also recommended for families at high risk.
What support resources are available for families of children with solid tumors?
Families can find help from national groups, financial aid, counseling, and educational resources. These are all tailored to meet their specific needs.
What are the current research directions for pediatric solid tumors?
Research focuses on understanding tumors better, finding new treatments, and improving outcomes. This includes new therapies and clinical trials.
Receiving a diagnosis of a pediatric solid tumor can be an overwhelming experience, highlighting the importance of understanding this condition.
The type and stage of the tumor greatly influence treatment plans. Doctors use a mix of surgery, chemotherapy, radiation, and other therapies based on the tumor and the child’s health.
References:
- Howlader, N., et al. (2022). SEER Cancer Statistics Review, 1975-2019. National Cancer Institute.https://seer.cancer.gov/csr/1975_2019/




































