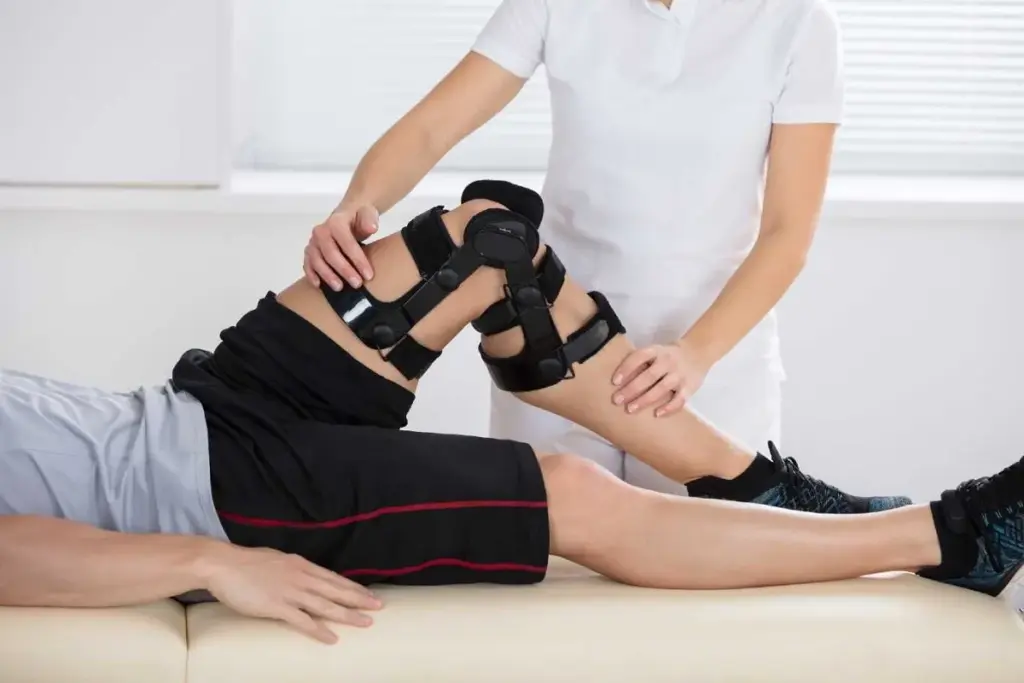
Physical therapy helps people get better from injuries and manage long-term health issues. Orthopedic physical therapy is a special part that deals with bone, joint, and muscle problems.
Regular physical therapy covers many treatments. But orthopedic therapy focuses on bones, joints, and muscles. We use proven methods to help patients get stronger and move better.
Knowing the difference between these therapies is key to getting the right treatment for you.
Key Takeaways
- Orthopedic physical therapy is a specialized branch of physical therapy.
- It focuses on treating musculoskeletal disorders and injuries.
- Regular physical therapy encompasses a broader range of treatments.
- Orthopedic physical therapy targets issues related to bones, joints, and muscles.
- Evidence-based techniques are used to promote recovery and improve mobility.
Understanding Physical Therapy Basics

Physical therapy is key in helping people get better. It has a long history and keeps growing. Let’s look at what physical therapy is, why it matters, and how it has changed over time.
Definition and Purpose of Physical Therapy
Physical therapy helps people stay active, get better, or move better. It’s a big part of helping people live better lives. This is true for those with injuries or chronic conditions.
The primary goal of physical therapy is to address the root cause of pain or limited movement. Physical therapists create plans just for each patient. They help people recover from surgery, manage long-term health issues, or boost their physical abilities.
At its heart, physical therapy uses methods that don’t involve surgery or drugs. Therapists use hands-on techniques, exercises, and teach about posture and movement. This helps patients heal and function better.
Physical therapy does more than just treat patients. It teaches them how to handle their health on their own. This helps the healthcare system by reducing the need for surgery and medication.
The Evolution of Physical Therapy as a Medical Discipline
Physical therapy has changed a lot over the years. It started after World War I to help people recover. Now, it helps a wide range of people with different health issues.
Physical therapy has grown thanks to better education, research, and practice. Today, it’s based on the latest scientific studies. Therapists keep learning to stay up-to-date with new research.
What is Regular Physical Therapy?
Regular physical therapy is a key part of healthcare. It offers treatment plans tailored to each patient’s needs. Knowing what regular physical therapy is helps us see its value in patient care.
Core Components of General Physical Therapy
General physical therapy has several key parts. These are essential for effective treatment. They include:
- Assessment and Evaluation: Initial and ongoing checks to see how patients are doing and adjust plans as needed.
- Therapeutic Exercises: Personalized exercise plans to boost strength, flexibility, and movement.
- Manual Therapy: Techniques like massage and joint mobilization to help recovery.
- Modalities: Heat, cold, and electrical stimulation to manage pain and aid healing.
Conditions Typically Treated with Regular PT
Regular physical therapy helps with many conditions. These include:
- Musculoskeletal Injuries: Sprains, strains, and fractures.
- Neurological Conditions: Stroke, Parkinson’s disease, and multiple sclerosis.
- Cardiovascular Conditions: Heart disease and recovery after surgery.
- Respiratory Conditions: COPD and other breathing problems.
Settings Where General PT is Practiced
General physical therapy is done in many places. This makes it easy and flexible for patients. These places are:
- Hospitals: Both inpatient and outpatient services.
- Private Practices: Clinics focused on specific areas of physical therapy.
- Rehabilitation Centers: Programs for full rehabilitation.
- Sports Facilities: For preventing and treating sports injuries.
- Home Healthcare: Therapy given in the patient’s home.
Understanding the core parts, conditions treated, and where it’s practiced shows its wide role in healthcare and rehab.
What is Ortho PT? Exploring Orthopedic Physical Therapy
Orthopedic physical therapy, or ortho PT, is a special part of physical therapy. It deals with musculoskeletal disorders and injuries. This therapy focuses on bones, joints, muscles, and soft tissues.
Specialized Focus of Orthopedic Physical Therapy
Ortho PT focuses on the musculoskeletal system. Physical therapists in this field get extra training. They learn about musculoskeletal injuries and conditions.
They can give treatments to help patients feel better. This includes reducing pain and improving life quality.
The musculoskeletal emphasis in ortho PT is key. Therapists know how to treat many conditions. This includes acute injuries and chronic conditions like osteoarthritis.
The Musculoskeletal Emphasis
The musculoskeletal focus in ortho PT is very important. It helps find and fix the causes of pain and dysfunction. By understanding bones, joints, muscles, and soft tissues, therapists can create detailed treatment plans.
These plans might include manual therapy, exercises, and teaching about movement. This helps prevent future injuries.
- Manual therapy techniques, such as joint mobilization and soft tissue mobilization
- Personalized exercise programs to improve strength, flexibility, and range of motion
- Education on posture correction and body mechanics
- Modalities such as heat, cold, and electrical stimulation to manage pain and inflammation
Common Orthopedic Conditions Treated
Ortho PT is good for many orthopedic conditions. Some common ones include:
- Fractures and post-surgical rehabilitation
- Tendinitis and bursitis
- Osteoarthritis and rheumatoid arthritis
- Sprains and strains
- Chronic pain conditions
Ortho PT practitioners tailor treatments for each patient. They help with recovery from surgery or managing chronic pain. Ortho PT is key for rehabilitation and health.
Educational Requirements: Regular vs. Orthopedic PT
Becoming a physical therapist requires a lot of education and training. Both regular and orthopedic physical therapists start with the same basic education. But, orthopedic specialists often get extra certifications.
Base Education for All Physical Therapists
To become a physical therapist, you need a Doctor of Physical Therapy (DPT) degree. This degree takes three years after a bachelor’s degree. You’ll learn about anatomy, biomechanics, and physiology.
Getting hands-on experience is also key. Students do internships or clinical rotations. This makes sure they can handle many conditions.
Additional Certifications for Orthopedic Specialists
While a DPT degree is enough for general practice, orthopedic physical therapists get extra certifications. The Orthopedic Certified Specialist (OCS) certification is highly respected. To get it, they must pass a tough exam.
Orthopedic specialists with OCS certification are experts in musculoskeletal conditions. They are very valuable in rehabilitation.
Continuing Education Requirements
Continuing education is key for all physical therapists. It keeps them up-to-date with new techniques and research. Both regular and orthopedic physical therapists need to keep learning to keep their licenses.
Orthopedic specialists might learn more about manual therapy or sports rehabilitation. This keeps them at the top of their game.
“Continuing education is not just a requirement; it’s an opportunity for physical therapists to enhance their skills and provide the best possible care for their patients,” said a leading physical therapy educator.
By getting foundational education, specialized certifications, and ongoing learning, physical therapists can give top-notch care. They tailor their care to meet their patients’ needs.
Key Differences in Assessment Techniques
Assessment techniques in physical therapy vary, depending on whether it’s for general or orthopedic care. The first evaluation is key to finding the best treatment plan.
General PT Evaluation Methods
General physical therapy starts with a full check-up. This includes looking at the patient’s medical history, current symptoms, and how well they can function. Standardized assessment tools are used to measure pain, range of motion, strength, and balance.
This helps physical therapists find the root cause of the problem. They then create a treatment plan to meet the patient’s needs and improve their life quality.
Specialized Orthopedic Assessment Protocols
Orthopedic physical therapy uses special tests for musculoskeletal issues. These tests check the stability of joints, muscle strength, and how well joints move.
Advanced tools and technologies are also used to see how severe the injury is. This helps in making a treatment plan that fits the patient’s needs.
Diagnostic Tools and Technologies
Diagnostic tools and technologies are key in both general and orthopedic physical therapy. But, orthopedic therapy often uses more advanced tools like ultrasound imaging and electromyography (EMG) to check muscle and tendon injuries.
|
Diagnostic Tool |
Description |
Application in Orthopedic PT |
|---|---|---|
|
Ultrasound Imaging |
Uses high-frequency sound waves to create images of internal structures. |
Assesses muscle and tendon injuries, guides injections. |
|
Electromyography (EMG) |
Measures the electrical activity of muscles. |
Evaluates muscle function, detects nerve damage. |
|
X-ray |
Uses X-rays to create images of bone structures. |
Assesses bone fractures, degenerative changes. |
Knowing the differences in assessment techniques helps patients understand the specialized care they get. Our physical therapists use the right methods to create effective treatment plans.
Treatment Approaches: How They Differ
It’s important to know the differences between regular and orthopedic physical therapy. Both aim to improve patient outcomes, but they use different methods. Understanding these differences helps patients find the right care for their needs.
Regular PT Treatment Modalities
Regular physical therapy uses many treatment methods. These include therapeutic exercises, manual therapy techniques, and other modalities like heat or electrical stimulation. The goal is to boost mobility, strength, and function, improving the patient’s life quality.
For example, someone recovering from a stroke might get PT to regain motor skills. They might do exercises to improve balance and use assistive devices.
Specialized Orthopedic Treatment Techniques
Orthopedic physical therapy focuses on musculoskeletal conditions. Orthopedic PTs use advanced techniques like joint mobilization and manipulation. These methods aim to relieve pain and enhance function.
A patient with a rotator cuff injury might get PT to strengthen the shoulder. They might also get manual therapy to improve joint mobility and reduce pain.
Evidence-Based Practice Differences
Both regular and orthopedic PT rely on evidence-based practice. But, the evidence base varies due to the conditions treated. Orthopedic PT uses the latest research in musculoskeletal therapy.
The use of outcome measures is key in both types of PT. These measures help track patient progress and adjust treatment plans. This ensures care is effective and efficient.
Orthopedic Physical Therapy Specialization in Musculoskeletal Therapy
Orthopedic physical therapy has changed how we treat musculoskeletal disorders. We, as orthopedic physical therapists, can handle many musculoskeletal issues. This includes both sudden injuries and long-term pain.
Joint Mobilization and Manipulation
We use joint mobilization and manipulation in our therapy. This method applies specific forces to joints. It helps improve mobility, reduces pain, and boosts function.
Joint mobilization is great for those with limited movement due to injury or long-term conditions.
We adjust the type of mobilization based on the patient’s needs. For example, we use softer techniques for those with a lot of pain or swelling. More intense methods are used for those needing more joint movement.
Advanced Soft Tissue Techniques
We also use advanced soft tissue techniques to work on muscle and tissue problems. These include myofascial release, trigger point therapy, and soft tissue mobilization. They help reduce pain, improve tissue flexibility, and aid in healing.
These methods are very helpful for patients with issues like tendinopathies, scar tissue, and myofascial pain syndrome. By focusing on soft tissues, we can greatly improve a patient’s recovery and ability to function.
Therapeutic Exercise Prescription
Therapeutic exercise is a key part of orthopedic physical therapy. We create custom exercise plans to boost strength, flexibility, balance, and coordination. These exercises are made just for the patient, taking into account their condition, fitness level, and goals.
Through exercise, we help patients recover from musculoskeletal injuries and teach them how to prevent future problems. This proactive approach to musculoskeletal health is a key part of orthopedic physical therapy.
Orthopedic Rehabilitation Services: What to Expect
Patients in orthopedic rehabilitation get a plan made just for them. This helps them reach their recovery goals. The services focus on each patient’s needs, aiming to improve strength, mobility, and function after injuries or surgery.
Comprehensive Orthopedic Rehab Programs
Our orthopedic rehab programs offer a range of treatments. They include manual therapy and exercises made just for the patient’s condition and goals.
Therapeutic exercises are key, helping to boost strength, flexibility, and movement. We also teach education on proper body mechanics and posture. This helps prevent future injuries and keeps patients healthy long-term.
Duration and Frequency of Treatment
The length and how often you need treatment depends on your condition and health. Rehab programs usually last from weeks to months.
- Initial intensive phase: 2-3 times per week
- Progressive phase: 1-2 times per week
- Maintenance phase: as needed, based on patient progress
Measuring Progress and Outcomes
We check how well patients are doing regularly. We look at their function, pain, and recovery. This helps us see if they’re getting better and make changes if needed.
Our aim is to help patients manage their condition well. We want them to keep the progress they make during rehab.
Sports Injury Rehab: The Orthopedic Physical Therapy Approach
Sports injuries need a special rehab plan. Orthopedic physical therapy is perfect for this. These therapists know how to help athletes get back to their sports.
“A good rehab plan is key,” saysa sports medicine expert. “Orthopedic physical therapists can create these plans.”
Athletic Recovery Protocols
Recovery plans are made just for each athlete. They consider the injury, the athlete’s health, and their goals. These plans include manual therapy, exercises, and treatments like heat or cold.
For example, someone with a knee injury might do exercises to strengthen muscles. They also do moves to keep the knee flexible and reduce pain.
Return-to-Play Assessment
Checking if an athlete is ready to play again is important. Orthopedic physical therapists look at strength, flexibility, and how well the athlete moves. They make sure the athlete can play safely.
This process is more than just moving right. It’s about moving right and safely. Athletes do tests and drills that mimic their sport.
Injury Prevention Strategies
Preventing injuries is also a big part of what orthopedic physical therapists do. They teach athletes how to train right. They give exercises to strengthen weak spots and advice on gear to avoid injuries.
By teaching injury prevention, these therapists help athletes recover and stay safe from future injuries.
In conclusion, orthopedic physical therapy is all about helping athletes fully recover. They focus on recovery plans, assessments, and prevention. This way, athletes can get back to their sports and stay healthy.
Physical Therapist vs. Orthopedist: Understanding the Distinctions
It’s important to know the difference between a physical therapist and an orthopedist. Both help with musculoskeletal health, but they do it in different ways. Their expertise and how they care for patients are quite different.
Scope of Practice Differences
Physical therapists help people with injuries or conditions that make it hard to move. They use exercises and manual therapy to improve strength and function. On the other hand, orthopedists are doctors who deal with musculoskeletal problems. They might use surgery to treat these issues.
Physical therapists help patients recover from injuries or surgery. They also manage chronic conditions and improve physical function. Orthopedists use various treatments, including medication and surgery, to treat musculoskeletal problems.
When to See Each Professional
Choosing between a physical therapist or an orthopedist depends on your condition. If you have musculoskeletal pain or limited mobility, start with a physical therapist. They can help improve your function and reduce pain.
But if you need surgery or a detailed medical check-up, see an orthopedist. They can diagnose complex conditions, recommend treatments, and perform surgery if needed.
Collaborative Care Models
Physical therapists and orthopedists often work together. An orthopedist might refer a patient to a physical therapist for rehabilitation. A physical therapist might also send a patient to an orthopedist for further evaluation.
This teamwork ensures patients get the best care for their needs. By working together, physical therapists and orthopedists can improve patient outcomes and overall musculoskeletal health.
Physiatrist vs. Orthopedist: Complementary Roles in Rehabilitation
It’s important to know the difference between physiatrists and orthopedists for good rehabilitation. Both are key in patient care but have different ways and areas of focus.
Specialization and Training Differences
Physiatrists, or PM&R doctors, help patients with chronic pain and musculoskeletal injuries. They use non-surgical methods to treat a wide range of conditions.
Orthopedists, who are surgeons, focus on the musculoskeletal system. They can do surgery but also offer non-surgical care.
|
Specialist |
Primary Focus |
Training |
|---|---|---|
|
Physiatrist |
Non-surgical rehabilitation |
PM&R residency |
|
Orthopedist |
Surgical and non-surgical musculoskeletal care |
Orthopedic surgery residency |
Treatment Philosophy Comparisons
Physiatrists focus on non-invasive treatments like physical therapy and medication. Orthopedists, who can also do non-surgical care, might suggest surgery if needed.
Orthopedists often mix conservative management with surgery in their plans. This depends on the patient’s condition.
Patient Referral Patterns
Who refers patients to physiatrists or orthopedists depends on the patient’s needs and the doctor’s network. Primary care doctors usually send patients to physiatrists for chronic pain or rehab.
Orthopedists get more referrals for patients needing surgery for musculoskeletal issues. This includes joint replacements or fracture repairs.
Knowing the roles of physiatrists and orthopedists helps patients get the right care. It makes their rehabilitation journey smoother and more effective.
PA vs. Physical Therapist: Clarifying Professional Boundaries
Healthcare is getting more complex. It’s key to understand the roles of physician assistants (PAs) and physical therapists. They both help patients, but they do different things and have different training.
Education and Training Differences
Physician assistants and physical therapists have different paths to their careers. PAs get a master’s degree in physician assistant studies. This includes classes and hands-on training to work with doctors.
Physical therapists earn a Doctor of Physical Therapy (DPT) degree. Their studies focus on helping people with physical issues. This includes helping with movement and daily activities.
|
Profession |
Typical Degree |
Education Focus |
|---|---|---|
|
Physician Assistant |
Master’s |
Medical care under physician supervision |
|
Physical Therapist |
Doctorate (DPT) |
Diagnosis and treatment of physical disabilities |
Practice Authority and Limitations
The work PAs can do varies by state. They often need a doctor’s supervision. PAs can diagnose, create treatment plans, and prescribe medicine in many places.
Physical therapists work more on their own in some states. They can treat patients without a doctor’s referral. But, they only work on physical therapy, helping with movement and pain.
Collaborative Care Approaches
PAs and physical therapists often team up to help patients. PAs might send patients to physical therapists. Physical therapists might talk to PAs or doctors to plan care.
This teamwork makes sure patients get all the care they need. It covers their medical and physical therapy needs.
Difference Between Sports Medicine and Physical Therapy
Sports medicine and physical therapy are often confused with each other. But they have different roles in treating injuries. Sports medicine covers many areas like orthopedic surgery and physical medicine. It focuses on preventing, diagnosing, and treating sports injuries.
Physical therapy, on the other hand, is a specific field. It helps patients move better and do daily activities. Physical therapists treat injuries that limit movement.
Scope of Practice Comparisons
Sports medicine deals with a wide range of treatments, including surgery. Physical therapy, while treating injuries, uses non-surgical methods like exercise and manual therapy.
Key differences in scope of practice include:
- Sports medicine involves a team of professionals, including doctors and physical therapists.
- Physical therapy focuses on rehabilitation and is a standalone profession.
|
Aspect |
Sports Medicine |
Physical Therapy |
|---|---|---|
|
Scope of Practice |
Diagnosis, treatment, prevention of sports injuries; may include surgery |
Rehabilitation, functional restoration through non-surgical means |
|
Professional Involvement |
Team-based, including physicians, surgeons, PTs |
Standalone profession, PTs work independently or in teams |
|
Treatment Focus |
Broad, including surgical and non-surgical interventions |
Non-surgical interventions: exercise, manual therapy, education |
Integrated Treatment Models
Sports medicine and physical therapy often work together. For example, an athlete might see a sports medicine doctor first. Then, a physical therapist helps with rehabilitation.
Integrated care models benefit patients by:
- Ensuring complete care from start to finish.
- Improving communication among healthcare providers.
- Enhancing recovery outcomes through coordinated care.
Choosing the Right Specialist for Athletic Injuries
Choosing between sports medicine and physical therapy depends on the injury and treatment stage. Sports medicine is often the first choice for acute injuries. Physical therapy is key for rehabilitation.
Considerations for choosing the right specialist include:
- The severity and nature of the injury.
- The need for surgical versus non-surgical interventions.
- The stage of recovery and rehabilitation needs.
Choosing Between Orthopedic and Regular Physical Therapy
Choosing between orthopedic and regular physical therapy depends on your condition and insurance. It’s important to know the differences and how they meet your needs.
Assessment of Your Specific Condition
First, figure out if you need orthopedic or regular physical therapy. Orthopedic therapy is for musculoskeletal issues like fractures or sprains. Regular therapy is for a wider range of problems, including neurological issues or fitness.
Consider these factors:
- The severity and type of your musculoskeletal issue
- Your overall health and any comorbid conditions
- The recommendations of your primary care physician or specialist
Insurance and Cost Considerations
Insurance and cost are key when choosing therapy. Most plans cover physical therapy, but coverage varies. Check with your provider to know what’s covered and what you’ll pay out-of-pocket.
|
Factor |
Orthopedic Physical Therapy |
Regular Physical Therapy |
|---|---|---|
|
Average Cost per Session |
$100-$150 |
$80-$120 |
|
Insurance Coverage |
Typically covered for musculoskeletal conditions |
Coverage varies by condition and insurer |
|
Specialized Care |
Yes, for musculoskeletal and orthopedic conditions |
No, general physical therapy |
Questions to Ask Your Healthcare Provider
Ask your healthcare provider the right questions. Consider asking:
- What type of physical therapy is most appropriate for my condition?
- Are there any specific physical therapists you recommend?
- How often will I need to attend physical therapy sessions, and for how long?
- What are the expected outcomes of physical therapy for my condition?
By understanding your condition, insurance, and asking questions, you can choose the right therapy for you.
Conclusion
Orthopedic physical therapy and regular physical therapy have different goals and methods. Both aim to improve patient outcomes, but they focus on different areas. Orthopedic physical therapy deals with complex musculoskeletal issues, using specialized techniques.
Orthopedic physical therapy is vital for patients with musculoskeletal disorders. It offers targeted treatments that improve quality of life. Regular physical therapy, on the other hand, helps with a wide range of conditions, boosting overall health.
Knowing the difference between these therapies is important when choosing physical therapy. Whether you need orthopedic expertise or general rehabilitation, understanding your options helps you choose the right care.
FAQ
What is the main difference between orthopedic physical therapy and regular physical therapy?
Orthopedic physical therapy focuses on musculoskeletal issues. This includes injuries and conditions affecting bones, joints, and muscles. Regular physical therapy treats a wider range of conditions, like neurological and cardiovascular issues.
Do orthopedic physical therapists require additional education or certifications?
Yes, orthopedic physical therapists often get extra certifications. For example, they might become Orthopedic Certified Specialists (OCS). This shows they have more knowledge and skills in treating musculoskeletal problems.
What conditions are typically treated with orthopedic physical therapy?
Orthopedic physical therapy treats many conditions. These include osteoarthritis, tendonitis, ligament sprains, fractures, and post-operative care for orthopedic surgeries. The goal is to improve function, reduce pain, and enhance quality of life.
How do assessment techniques differ between regular and orthopedic physical therapy?
Orthopedic physical therapy uses detailed musculoskeletal evaluations and diagnostic tests. This is to accurately diagnose and treat musculoskeletal conditions. Regular physical therapy might use more general assessment methods.
Can a physiatrist and an orthopedist work together in rehabilitation?
Yes, physiatrists and orthopedists often work together. Physiatrists help patients with chronic diseases or injuries regain function. Orthopedists focus on surgical interventions for musculoskeletal issues.
What is the difference between a physical therapist and a physician assistant in orthopedic care?
Physical therapists specialize in movement and rehabilitation. They help patients recover from injuries or surgery. Physician assistants work under a physician’s supervision. They diagnose and treat patients, including prescribing medications.
How does sports medicine differ from physical therapy in treating athletic injuries?
Sports medicine is a broad field focused on preventing, diagnosing, and treating sports-related injuries. Physical therapy is a key part of sports medicine. It provides rehabilitation services to help athletes recover and return to their sport.
What should I consider when choosing between orthopedic and regular physical therapy?
Consider the nature of your condition when deciding. If you have a musculoskeletal issue, like a sports injury or osteoarthritis, orthopedic physical therapy might be better. Also, think about insurance coverage and the therapists’ expertise in your area.
Are there specific questions I should ask my healthcare provider about orthopedic physical therapy?
Yes, ask about the therapist’s experience with your condition. Also, find out about the treatment duration, frequency, and how progress will be measured. Knowing the treatment plan and what to expect helps you make informed decisions.
Reference
BMJ (British Medical Journal). Evidence-Based Medical Insight. Retrieved from https://bmj.com/content/11/5/e045123




































