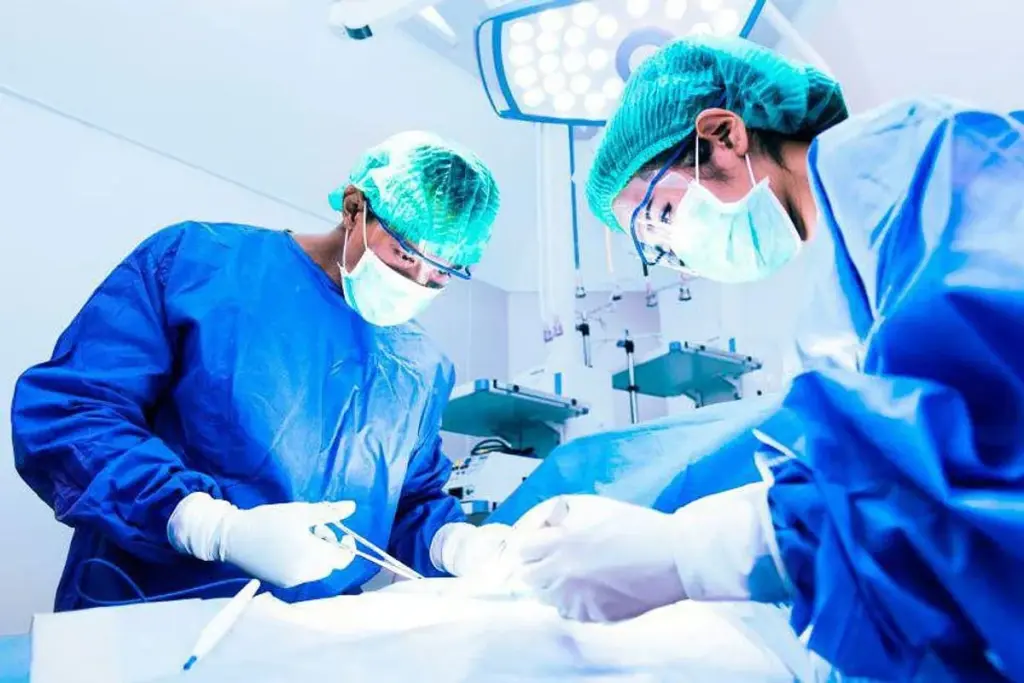
Replacing a cardiac pacemaker is a big deal for many people. Every year, over 50,000 pacemaker implantation procedures happen in the U.S. alone. It’s a surgery that can make you nervous, but knowing the risks and benefits is key.
Choosing to have implantable defibrillator surgery or replace a pacemaker is a significant decision that requires careful consideration of various factors. The surgery is done by making a small cut to get to the pacemaker pocket. Then, the old device is taken out, and a new one is put in. While it’s usually safe, there are risks like infection and bleeding.
Key Takeaways
- Replacing a pacemaker is a common procedure performed on thousands of patients annually.
- The surgery involves removing the old device and implanting a new one through a small incision.
- Risks include infection, bleeding, and possible damage to nearby tissue.
- Understanding the benefits and risks is vital for those thinking about the procedure.
- Thousands of pacemaker surgery procedures are done safely every year.
What Is a Pacemaker and Why Would It Need Replacement?
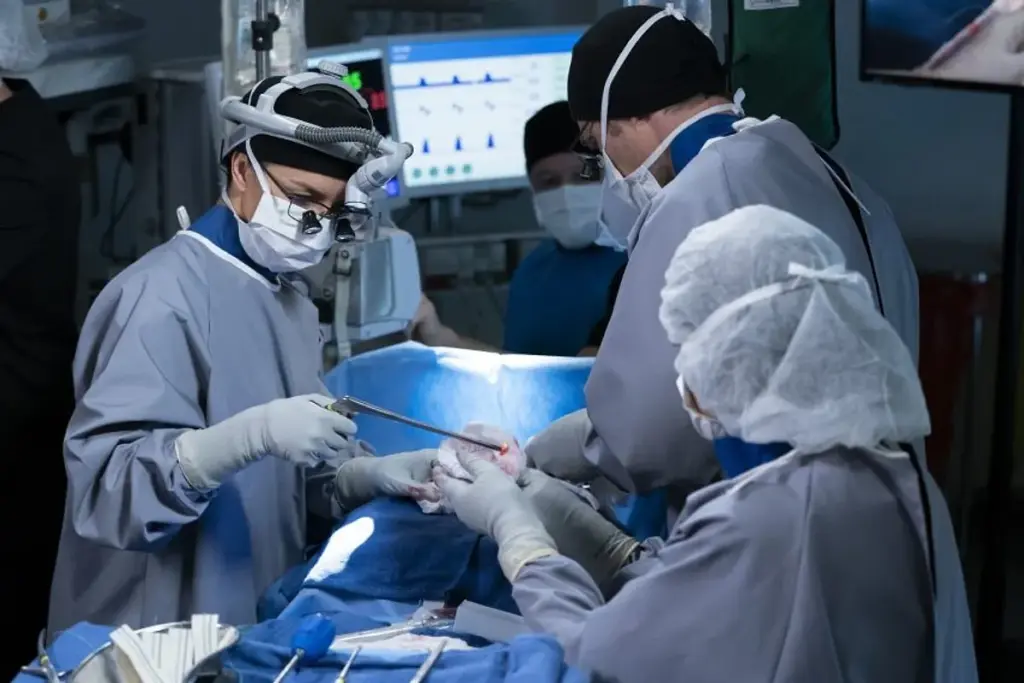
Cardiac pacemakers are advanced medical tools that help control heart rhythm. They are vital for managing heart rhythm disorders. This ensures the heart beats at the right rate and rhythm.
How Pacemakers Regulate Heart Rhythm
Pacemakers send electrical signals to make the heart muscle contract. These signals go through leads, thin wires in the heart. The device itself is hidden under the skin, often near the collarbone.
This device is key for people with arrhythmias or heart conditions. It helps the heart beat naturally.
Types of Modern Cardiac Pacemakers
There are many types of pacemakers, each for different heart issues:
- Single-chamber pacemakers: These have one lead in the right atrium or ventricle.
- Dual-chamber pacemakers: These have two leads, one in each chamber, for better pacing.
- Biventricular pacemakers: Used for cardiac resynchronization therapy, with three leads for better ventricle coordination.
Common Reasons for Device Replacement
The main reason for replacing a pacemaker is when the battery runs out. Modern pacemakers’ batteries last 5 to 15 years, depending on the model and settings.
|
Reason for Replacement |
Description |
|---|---|
|
Battery Depletion |
The battery life ends, typically after 5-15 years. |
|
Device Upgrade |
New technology or features become available. |
|
Lead Issues |
Problems with the leads, such as malfunction or fracture. |
The Role of Cardiologists in Pacemaker Management
Managing pacemaker patients is a big job. Cardiologists, who know a lot about heart rhythms, lead the way. They check if a pacemaker needs to be replaced and look at the patient’s heart health. They also pick the best device for each patient.
Electrophysiologists vs. General Cardiologists
General cardiologists help many heart patients. But, electrophysiologists are experts in heart rhythm problems. They get extra training to deal with arrhythmias, making them key in pacemaker care.
How Cardiovascular Specialists Evaluate Replacement Needs
Cardiovascular specialists use tests to see if a pacemaker needs to be replaced. They check the battery life and the heart rhythm. They also see if the current device fits the patient’s needs. They make sure the decision to replace a pacemaker is best for the patient.
The Heart Team Approach to Device Management
The Heart Team works together to care for pacemaker patients. This team includes cardiologists, surgeons, and others. They work together to make sure patients get the best care. A leading cardiologist says, ‘A team-based approach is key for complex heart conditions.’
“A team-based approach is essential in managing complex cardiac conditions, ensuring that patients receive comprehensive care“.
Leading Cardiologist
|
Specialist |
Training |
Role in Pacemaker Management |
|---|---|---|
|
General Cardiologist |
Standard cardiology training |
General heart care, initial pacemaker implantation |
|
Electrophysiologist |
Additional specialized training in electrophysiology |
Complex heart rhythm management, pacemaker follow-up, and replacement |
Pacemaker Surgery: Replacement vs. Initial Implantation
It’s important to know the differences between pacemaker replacement and initial implantation. Both are key for managing heart rhythm issues. Yet, they vary in surgical method, complexity, and results.
Key Differences in Surgical Approach
Replacing a pacemaker is different from the first time it’s implanted. When replacing, the old pocket is used, and the leads are already in place. This makes the surgery simpler. But, the surgeon must be careful to avoid problems like infection or damage to the leads.
For the first time, a new pocket is made, and the leads are placed. This is more complex and takes longer. The surgeon must plan carefully to place the device and leads right. This ensures they work well and reduces future problems.
Comparative Complexity of Procedures
Replacing a pacemaker is generally simpler than the first implant. This is because the initial steps of making a pocket and placing leads have been done. Yet, the new device must be connected and work right, which requires precision.
A study comparing these procedures is shown in the table below:
|
Procedure Aspect |
Initial Implantation |
Pacemaker Replacement |
|---|---|---|
|
Device Pocket Creation |
Required |
Existing |
|
Lead Placement |
Required |
Usually retained |
|
Average Procedure Time |
Longer |
Shorter |
|
Complexity Level |
Higher |
Lower |
Statistical Differences in Outcomes
The results of pacemaker replacement and initial implantation can differ. This depends on the patient’s health, the surgeon’s skill, and the technology used. Research shows both procedures are successful, but initial implantation might have a bit higher risk of issues because it’s more complex.
Studies found that replacement surgery usually has fewer complications. This is because it’s less invasive and the surgeon is more familiar with the anatomy.
Pre-Operative Assessment and Preparation
Before pacemaker replacement surgery, a detailed pre-operative assessment is key. It makes sure patients are ready for the surgery. This reduces risks and improves results.
Required Medical Evaluations
Patients get checked before surgery to see their heart and health status. These checks include:
- Electrocardiogram (ECG): To check the heart’s rhythm and find any issues.
- Echocardiogram: An ultrasound to look at the heart’s shape and how it works.
- Blood Tests: To find infections, check kidney health, and look at other health signs.
- Chest X-ray: To see the heart’s size and lung health.
Medication Adjustments Before Surgery
Managing medications is a big part of getting ready for surgery. We look at the patient’s meds to see if any need to be changed or stopped before surgery. This includes:
- Anticoagulants: These blood thinners might be stopped to lower bleeding risk during surgery.
- Antiplatelet Agents: These meds might also be adjusted based on the patient’s risk.
Patient Education and Expectation Setting
Telling patients about the surgery, recovery, and what to expect is very important. We focus on:
- Pre-Surgical Instructions: Clear steps on getting ready for surgery, like fasting and meds.
- Post-Surgical Care: How to care for the wound, what activities to avoid, and follow-up visits.
- Recovery Timeline: Giving a realistic view of how long recovery will take.
By preparing patients well with medical checks, medication changes, and education, we make pacemaker replacement surgery safer and more successful.
Step-by-Step Pacemaker Replacement Procedure
Replacing a pacemaker is a detailed process that needs precision and care. We’ll walk you through it, highlighting the important steps for a successful outcome.
Anesthesia Options and Selection Criteria
Choosing the right anesthesia is key for pacemaker replacement. We often use local anesthesia with sedation to reduce pain and anxiety. The choice depends on the patient’s health, medical history, and the procedure’s complexity.
Key considerations for anesthesia selection include:
- Patient’s medical history and current health status
- Potential allergies or sensitivities to certain anesthetics
- The need for sedation to manage anxiety or discomfort
Surgical Access to the Device Pocket
Accessing the pacemaker pocket is a delicate step. Our surgeons carefully find the pocket and make a precise incision. This step is critical to avoid damage to the surrounding tissue or the leads.
The surgical team must be meticulous in their approach to minimize the risk of complications.
Lead Management Decisions
Deciding how to manage the existing leads is a critical part of the procedure. We check the leads’ condition and function to decide if they can be reused or need replacement. This decision is based on several factors, including the lead’s age and performance.
Factors influencing lead management decisions include:
- The age and condition of the existing leads
- The presence of any lead-related complications
- The compatibility of the existing leads with the new pacemaker device
By carefully evaluating these factors, we can make informed decisions that optimize the outcome of the pacemaker replacement procedure.
Primary Risks of Pacemaker Replacement Surgery
Pacemaker replacement surgery is mostly safe, but there are risks to consider. Knowing these risks helps keep patients safe and informed.
Infection Risks and Prevention Strategies
Infection is a big risk with pacemaker surgery. We use antibiotics and keep the area clean to lower this risk. Even so, infections can happen. It’s important for patients to watch for signs like redness or fever after surgery.
Prevention strategies include good wound care and follow-up visits. Patients should keep the wound dry and avoid hard activities to help it heal.
Bleeding and Hematoma Formation
Bleeding and hematoma are possible complications. We use careful techniques to reduce bleeding. Some people might be more at risk due to their health or medicines.
We check and adjust medicines before surgery to lower bleeding risks. Watching patients closely after surgery helps catch any bleeding problems early.
Lead Dislodgement Concerns
Lead dislodgement is when the pacemaker leads move out of place. This can cause problems with pacing. We use special imaging to make sure the leads are in the right spot.
We teach patients to watch for signs like dizziness. If they notice these symptoms, they should see a doctor right away.
Cardiac Perforation Possibilities
Cardiac perforation is a rare but serious risk. It happens when the pacemaker lead goes through the heart wall. We use careful techniques and watch closely to avoid this.
If cardiac perforation does happen, we act fast. This might mean more surgery to fix the problem.
Patient-Specific Risk Factors to Consider
It’s key to know the specific risks for each patient before pacemaker replacement surgery. Things like age, health, and medicines can change how risky the surgery is.
Age-Related Considerations
Age plays a big role in pacemaker surgery risks. Older people might face more risks because of less physical strength and health problems. We must carefully assess the overall health of older patients to find the best surgery plan.
Even though age isn’t a direct no-go for surgery, we look at the patient’s health level more than just their age. This means checking their function, health problems, and overall well-being.
Impact of Pre-existing Medical Conditions
Medical conditions before surgery can also affect risks. Issues like diabetes, heart failure, and COPD can make surgery and recovery harder. We need to manage these conditions well before, during, and after surgery to lower risks.
- Diabetes: Needs careful blood sugar control to avoid wound problems.
- Heart Failure: May need better heart medicine and close watch during surgery.
- COPD: Needs lung function tests and better breathing status before surgery.
Medication Interactions and Concerns
Medicine interactions are also very important in pacemaker surgery. Some medicines, like blood thinners, can raise bleeding risks. We must check the patient’s medicines and change them if needed to balance bleeding and clot risks.
For example, people on blood thinners might need to stop or change their medicine before surgery. This choice should be made with a cardiologist or hematologist to manage risks well.
Post-Operative Complications and Management
The time after a pacemaker replacement is very important. Several complications can happen and need careful handling. We will talk about these issues and how they are managed.
Immediate Post-Surgical Complications
Right after surgery, problems like infection, bleeding, and reactions to anesthesia can occur. These are watched closely in the hospital. Patients stay for a few hours to catch any early signs of these issues.
Wound Healing Problems
Wound healing issues can cause infection or need more surgery. It’s key to take good care of the wound. Patients are told how to care for their wounds to lower the risk of problems.
Device Pocket Issues
Problems with the device pocket can happen, like hematoma or the device poking through the skin. These are fixed with the right surgical methods and care after surgery.
Cardiac Rhythm Disturbances
Heart rhythm problems can happen due to lead dislodgement or pacemaker issues. These are watched closely, and changes are made as needed to keep the heart beating right.
Handling post-operative complications well needs good planning before surgery, careful surgery, and care after. Knowing about these complications and how to handle them helps patients through their recovery.
|
Complication |
Management Strategy |
|---|---|
|
Infection |
Antibiotics, possible removal of the device |
|
Bleeding |
Monitoring, possible surgical intervention |
|
Wound Healing Issues |
Proper wound care, possible surgical revision |
“The key to managing post-operative complications lies in early detection and intervention.”Cardiologist
Recovery Timeline After Pacemaker Replacement
After getting a new pacemaker, patients follow a set recovery plan. This helps avoid problems and makes sure the device works well. This time is key for the surgery’s success and the patient’s health.
Hospital Stay Duration Expectations
The time in the hospital after pacemaker surgery varies. It depends on the patient’s needs and if there are any issues. Usually, patients stay for 24 to 48 hours to check the pacemaker’s work and watch for problems.
Our team keeps a close eye on the heart and looks for signs of infection or bleeding. They also manage pain and teach patients about their pacemaker care. This includes knowing when to seek help.
Activity Restrictions and Guidelines
Patients must avoid heavy lifting, bending, or hard work for 4 to 6 weeks after surgery. This helps with healing and lowers the risk of complications.
Light activities like walking are okay a few days after. But, it’s important to follow the specific advice from our team. It’s based on the patient’s situation and surgery details.
Follow-up Care Schedule
Regular check-ups are vital after pacemaker surgery. We see patients at 1 week, 1 month, and 3 months to check on healing and pacemaker function.
At these visits, we might do device checks and look at the patient’s health. We also answer any questions and use remote monitoring to keep an eye on the pacemaker between visits.
Long-term Outcomes and Quality of Life
Pacemaker replacement greatly improves a patient’s quality of life and health. It’s key to look at many factors that affect recovery and how well the device works.
Statistical Data on Replacement Success
Research shows pacemaker replacement surgeries are very successful. The success rate is over 95%. Many patients see their heart function and overall health improve right away.
Most patients feel better after the surgery. They have less fatigue, dizziness, and shortness of breath. This is because new pacemakers work better and meet the body’s needs more accurately.
Life Expectancy Considerations
Life expectancy after the surgery is a big concern for patients and their families. Studies show that successful replacement can lead to a longer life, mainly for those with severe heart issues. How long a patient lives after the surgery depends on their heart condition, overall health, and other medical issues.
Regular follow-up care and sticking to treatment plans lead to better outcomes. New pacemaker technology, like longer battery life and better monitoring, also helps patients live longer.
Activity Level and Lifestyle Improvements
Pacemaker replacement can greatly improve a patient’s activity level and lifestyle. Many patients can do things they couldn’t before because of their heart condition. This can range from light exercise and hobbies to more intense activities, based on their health and doctor’s advice.
We suggest patients talk to their healthcare provider about their lifestyle goals. This way, we can help set up the pacemaker and guide physical activity to improve their quality of life after the surgery.
Technological Advancements Reducing Surgical Risks
Pacemaker technology has made big strides, cutting down risks from surgery. New designs and functions have led to better results and fewer risks for patients.
Leadless Pacemakers
Leadless pacemakers are a big leap in heart pacing tech. They go straight into the heart, skipping the need for leads. A study in the.
|
Feature |
Traditional Pacemakers |
Leadless Pacemakers |
|---|---|---|
|
Lead-Related Complications |
Common |
Rare |
|
Implantation Method |
Surgical Pocket Creation |
Direct Heart Chamber Implantation |
|
Risk of Infection |
Higher |
Lower |
MRI-Compatible Devices
MRI-safe pacemakers are key for patients needing MRI scans. They work well during MRI, keeping patients safe.says, “MRI-safe pacemakers have changed how we manage patients with heart devices, making MRI scans safer.”
“The development of MRI-compatible pacemakers has been a game-changer for patients with cardiac devices, enabling them to undergo MRI scans without compromising their safety.”
Cardiologist
Remote Monitoring Capabilities
Remote monitoring lets doctors check on devices and patients anytime. It helps spot problems early and fix them fast. This tech cuts down on the need for in-person visits and boosts patient care.
Extended Battery Life Technologies
New battery tech means pacemakers last longer, needing fewer replacements. This reduces risks from surgery. Modern pacemaker batteries last much longer than before.
|
Pacemaker Model |
Battery Life |
|---|---|
|
Model A |
7-10 years |
|
Model B |
10-15 years |
|
Model C |
15+ years |
These advances make pacemaker replacement safer and more reliable. They improve patient outcomes and quality of life.
Selecting the Right Cardiac Specialist for Your Procedure
Choosing the right cardiac specialist is key for those thinking about pacemaker replacement. This specialist is vital for the success of the procedure and the patient’s health.
Looking for a cardiac specialist involves several important factors. We must consider their qualifications and experience with pacemaker surgeries.
Qualifications to Look For
A cardiac specialist should have the right qualifications and training. Board certification in cardiology or a related field is a must. It’s also important to find specialists with experience in pacemaker implantation and replacement.
- Board certification in cardiology or electrophysiology
- Fellowship training in cardiology or electrophysiology
- Experience with pacemaker procedures
Experience Level Considerations
The experience of the cardiac specialist is very important. We should ask about their experience with pacemaker replacement surgeries. This includes the number of procedures they’ve done and their complication rates.
|
Experience Level |
Number of Procedures |
Complication Rate |
|---|---|---|
|
Low |
<50 |
High |
|
Moderate |
50-100 |
Moderate |
|
High |
>100 |
Low |
Questions to Ask Your Potencial Surgeon
Before making a decision, it’s important to ask the right questions. We should ask about their experience, success rates, and how they handle complications.
- What is your experience with pacemaker replacement surgeries?
- What are your complication rates for this procedure?
- How do you handle emergencies during surgery?
By carefully evaluating these factors and asking the right questions, patients can make an informed decision. This helps when choosing a cardiac specialist for their pacemaker replacement procedure.
Insurance Coverage and Financial Considerations
Understanding the costs of pacemaker replacement surgery is key. Knowing what your insurance covers and what you might pay out-of-pocket is important. This helps you make smart choices about your health care.
Medicare Coverage for Device Replacement
If you have Medicare, you’re likely covered for pacemaker replacement. Medicare Part B usually pays for the device and the surgery. But, remember, Medicare might not cover all costs, like tests before surgery or care after.
Key aspects of Medicare coverage to consider:
- Coverage of the pacemaker device and implantation procedure
- Potential out-of-pocket costs for deductibles and coinsurance
- Limitations on coverage for related services
Private Insurance Policies
Private insurance plans can vary a lot in what they cover for pacemaker replacement. Some plans cover everything, while others might not. It’s important to check your plan to know what’s included and what’s not.
|
Insurance Aspect |
Medicare |
Private Insurance |
|---|---|---|
|
Device Coverage |
Generally covered under Part B |
Varies by policy |
|
Procedure Coverage |
Covered under Part B |
Varies by policy |
|
Out-of-Pocket Costs |
Deductibles and coinsurance apply |
Depends on policy specifics |
Out-of-Pocket Expenses to Anticipate
Even with insurance, you might have to pay some money for pacemaker replacement surgery. This could be for deductibles, coinsurance, or services not covered. Knowing these costs helps with planning your finances.
Tips for managing out-of-pocket expenses:
- Review your insurance policy to understand what is covered
- Ask your healthcare provider about possible costs
- Look into financial help programs if they’re available
Understanding your insurance and possible costs helps you deal with the financial side of pacemaker replacement surgery. Always talk to your insurance and healthcare team to get a clear idea of what you’ll pay.
Real Patient Experiences with Pacemaker Replacement
Learning from others who have had pacemaker replacement surgery can be very helpful. These stories share what to expect, the challenges faced, and the good results achieved.
Case Studies and Outcomes
Many case studies show the benefits of pacemaker replacement. For example, a study in a top cardiology journal found big improvements in patients’ lives. They felt better, had less heart failure symptoms, and could do more daily tasks.
A 75-year-old man was thrilled after his pacemaker was replaced. He could garden again without feeling tired or out of breath. Stories like his show the good things about pacemaker replacement.
Key findings from recent case studies include:
- Patients with new pacemakers lived longer than those without.
- The new devices worked better, lasting longer and having cool features like remote monitoring.
- Experienced cardiologists made the replacement safer and less complicated.
Common Patient Concerns and Resolutions
People thinking about pacemaker replacement worry about risks, recovery, and how it will change their life. Doctors and healthcare teams work hard to make sure the risks are low and recovery is smooth.
“The thought of another surgery scared me, but my cardiologist explained everything. From the anesthesia to follow-up care, it helped me feel better about it,” said a patient who had the surgery.
Common worries include:
- Concerns about surgery complications
- Worries about the device not working right
- Concerns about how long it takes to get better and what activities to avoid
Doctors and teams help by educating patients, planning carefully, and supporting them after the surgery.
Psychological Aspects of Device Dependence
Having a pacemaker means adjusting to relying on it. Support from doctors, family, and groups is key to helping patients deal with this.
While some feel anxious or depressed about their device, many feel safer and more confident. The impact on each person is different, showing the need for care tailored to each one.
Strategies to address the psychological aspects include:
- Regular counseling sessions
- Support groups for pacemaker patients
- Learning to manage device-related anxiety
When to Consider Alternative Options
Deciding on pacemaker replacement isn’t always easy. It involves looking at several factors. These include the patient’s health, the pacemaker’s condition, and the risks and benefits of replacing it.
Scenarios Where Replacement Might Be Delayed
In some cases, delaying pacemaker replacement might be a good choice. This could happen if:
- The pacemaker is working okay.
- The patient has other serious health issues that make surgery risky.
- The patient is close to the end of life, and a new pacemaker might not improve their quality of life.
Newer Device Options to Discuss
New pacemaker technology offers better features. These include:
|
Feature |
Benefit |
|---|---|
|
Leadless Pacemakers |
Less risk of problems with the leads. |
|
MRI-Compatible Devices |
Safe for MRI scans without needing to remove the device. |
|
Extended Battery Life |
Means fewer replacements over a patient’s lifetime. |
Watchful Waiting Approach in Certain Patients
For some, a watchful waiting approach might be best. This means keeping a close eye on the pacemaker and the patient’s health. It might avoid or delay the need for a new pacemaker unless it’s really needed.
By looking at these options, doctors can make choices that fit each patient’s needs. This helps ensure the best results for everyone.
Conclusion: Balancing Risks and Benefits of Pacemaker Replacement
Pacemaker replacement surgery is a big deal that needs careful thought about its risks and benefits. Knowing about the surgery, the role of specialists, and possible results helps patients make smart choices. We’ve looked at many parts of pacemaker replacement, like different types of pacemakers and the role of cardiologists.
It’s key to think about your own situation, like any health issues you have and the pacemaker type. New tech, like leadless pacemakers and remote monitoring, has made the surgery safer and more effective. Choosing a skilled cardiac specialist and following advice before and after surgery can help reduce risks and improve results.
In short, pacemaker replacement is a critical step for heart health. It has risks, but the benefits of better heart function and a better life often make it worth it. By understanding the details of pacemaker replacement and working with healthcare experts, patients can go through this process with confidence and get the best results.
FAQ
What is a pacemaker and why does it need replacement?
A pacemaker is a small device that helps control the heartbeat. It sends electrical impulses. It needs to be replaced when its battery runs out, usually after 5-15 years.
What are the different types of pacemakers available?
There are several types of pacemakers. Single-chamber, dual-chamber, and biventricular pacemakers are designed for different heart rhythm issues.
How do cardiologists manage pacemaker patients?
Cardiologists, like electrophysiologists, check if a pacemaker needs to be replaced. They look at the heart’s health and choose the best device for the patient.
What is the difference between initial pacemaker implantation and replacement surgery?
Replacement surgery is simpler. The initial pocket for the device is already made. The leads are already in place.
What are the primary risks associated with pacemaker replacement surgery?
Risks include infection, bleeding, damage to the heart or tissues, and lead dislodgement.
How can infection risks be mitigated during pacemaker replacement?
To lower infection risks, antibiotics are given before surgery. Sterile techniques are used. The patient is closely watched after surgery.
What patient-specific factors can impact the risks of pacemaker replacement?
Factors include age, health, pre-existing conditions, and medications. These can affect the surgery or device.
What is the typical recovery timeline after pacemaker replacement surgery?
Patients usually stay in the hospital briefly. Then, they rest and do limited activities. Follow-up care ensures the pacemaker works right.
How do advances in pacemaker technology improve patient outcomes?
New technologies like leadless pacemakers and MRI-compatible devices make devices safer and more reliable. Remote monitoring is also more convenient.
What should patients consider when selecting a cardiac specialist for pacemaker replacement?
Look for a specialist’s qualifications and experience. Ask questions about their care.
How can patients understand their insurance coverage for pacemaker replacement?
Review your insurance policies, including Medicare or private insurance. Know what’s covered and what you’ll pay out-of-pocket.
Are there alternative approaches to pacemaker replacement that patients should consider?
In some cases, delaying replacement or trying newer technologies may be options. This depends on the patient’s needs.
What are the long-term outcomes for patients after pacemaker replacement?
Studies show high success rates for pacemaker replacement. Many patients see improved health, longer life, and better quality of life.
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/20937934/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























