
Every year, over 600,000 cardiac pacemaker operations are done worldwide. This makes it a common way to manage heart rhythm problems. Yet, the thought of getting a pacemaker surgery can worry many people.
It is common to have concerns regarding the risks and side effects associated with pacemaker implantation. We know patients want all the facts to make smart choices about their health.
We focus on heart rhythm management at our place. We make sure patients get the top care. The implantable cardioverter-defibrillator and other devices are key. They save lives by stopping dangerous heart rhythms.
Key Takeaways
- Pacemaker implantation is a relatively common and safe procedure.
- Understanding the risks and benefits is key for making good choices.
- New technology has made pacemakers safer and more effective.
- Good care after the surgery helps avoid problems.
- Talking to your doctor about your worries is important.
Understanding Pacemakers and Their Purpose

Pacemakers have changed the game for heart health, helping millions globally. These small devices manage heart rhythm disorders, keeping the heart beating right.
” “They’ve enabled us to treat conditions that were previously difficult to manage.”
What is a Pacemaker and How Does it Work?
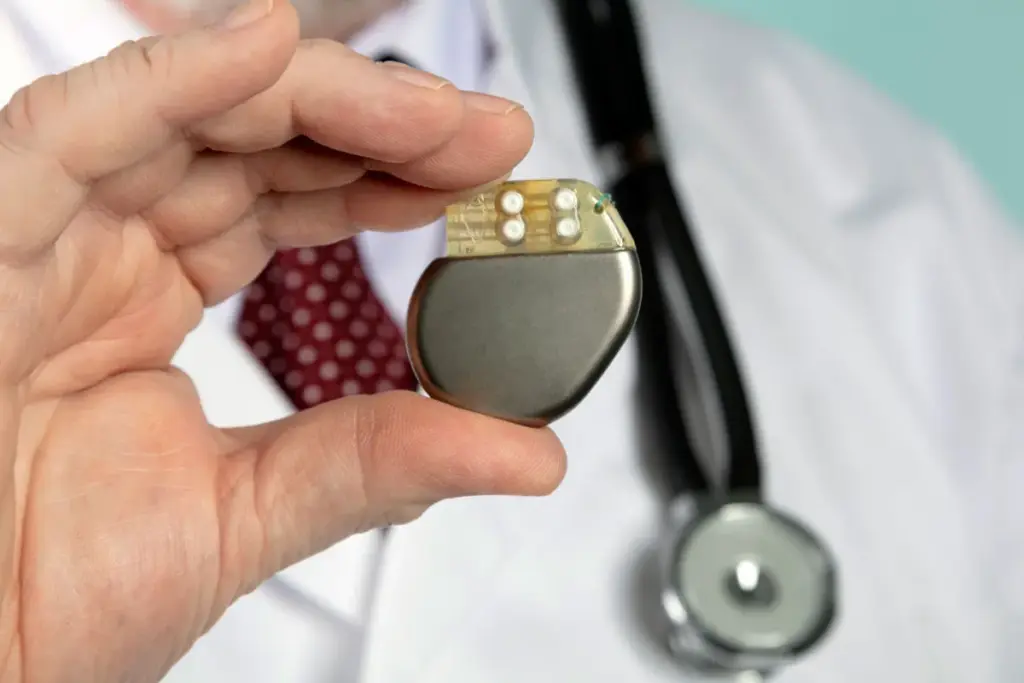
A pacemaker is a small device implanted under the skin, near the collarbone. It has two parts: the pulse generator and the leads. The pulse generator is a small computer that sends electrical impulses. The leads are thin wires that carry these impulses to the heart.
The pacemaker watches the heart’s rhythm and sends impulses when needed. This keeps the heart pumping blood well throughout the body.
Common Heart Conditions Requiring Pacemakers
Pacemakers treat various heart issues, like arrhythmias. These are when the heart beats too slow or too fast. Some common conditions needing a pacemaker include:
- Atrioventricular (AV) block
- Sick sinus syndrome
- Heart failure
- Cardiac arrest
These conditions can really affect a person’s life. Pacemakers help manage symptoms and improve health.
Evolution of Pacemaker Technology
Pacemaker tech has grown a lot, with better design and function. Today’s pacemakers are more advanced, with features like:
- Remote monitoring
- MRI compatibility
- Leadless designs
- Cardiac resynchronization therapy
These updates have made pacemakers safer and more effective. They’re now a trusted treatment for many worldwide.
Types of Cardiac Pacemakers and Devices
Cardiac pacemakers have come a long way, with many types to treat various heart issues. These advancements have greatly improved patient care and life quality. We’ll look at the different pacemakers and devices, their special features, and what conditions they help with.
Single Chamber vs. Dual Chamber Pacemakers
Pacemakers are divided by how many chambers they pace. Single chamber pacemakers have one lead in either the right atrium or ventricle. They help when the heart’s rhythm is off. Dual chamber pacemakers have two leads, in both chambers, for better pacing that matches the heart’s natural beat.
Biventricular Pacemakers
Biventricular pacemakers, or CRT devices, treat heart failure. They pace both ventricles and the right atrium with three leads. This ensures the heart’s chambers beat in sync, helping heart failure patients.
Implantable Cardioverter-Defibrillators (ICDs)
ICDs prevent sudden death from arrhythmias by shocking the heart when needed. They’re for those at high risk of dangerous arrhythmias. ICDs can also act as pacemakers, providing both shock and pacing therapies.
Leadless Pacemakers
Leadless pacemakers are a big step forward in pacemaker tech. They’re small devices placed directly in the heart’s ventricle without leads. They’re great for those at risk from traditional pacemaker leads.
Each pacemaker or device has its own use, benefits, and risks. Knowing these differences is key for patients and doctors to choose the best treatment.
The Role of Cardiac Electrophysiologists
Cardiac electrophysiologists are cardiologists with a special focus. They deal with arrhythmias and heart rhythm disorders. They also manage pacemakers.
What is a Cardiac Electrophysiologist?
A cardiac electrophysiologist is a doctor with extra training. They specialize in heart rhythm problems. They use tests and procedures to fix heart electrical issues.
Training and Expertise Required
To become a cardiac electrophysiologist, one needs a lot of education. They start with a residency in internal medicine. Then, they do a fellowship in cardiology and more training in electrophysiology.
Key aspects of their training include:
- Advanced understanding of heart anatomy and physiology
- Expertise in interpreting electrocardiograms (ECGs) and other diagnostic tests
- Proficiency in performing procedures like catheter ablation and pacemaker implantation
When to See an Electrophysiologist vs. General Cardiologist
General cardiologists handle many heart issues. But, for complex arrhythmias and pacemaker management, electrophysiologists are the best choice. If you have irregular heartbeats, fainting, or a pacemaker, see an electrophysiologist.
Electrophysiologists are key in these situations:
- Diagnosing and treating complex arrhythmias
- Managing patients with implanted cardiac devices
- Performing advanced procedures like lead extraction or catheter ablation
Pre-Surgical Evaluation and Preparation
Getting ready for pacemaker surgery is a big step. It involves several important steps to make sure everything goes smoothly. Let’s look at what you need to do before the surgery.
Required Medical Tests
We do many medical tests before surgery to check your health and heart. These tests are:
- Electrocardiogram (ECG): This records your heart’s electrical activity.
- Echocardiogram: An ultrasound to see how your heart works.
- Blood Tests: To find any infections or health issues.
- Chest X-ray: To look at your lungs and heart.
These tests help us find any risks and plan the surgery well.
Medication Adjustments
Some medicines might need to be changed or stopped before surgery. We’ll check your medicines and tell you what to do. This could mean:
- Blood Thinners: We might ask you to stop or change these to avoid bleeding.
- Other Medications: Some medicines could react with anesthesia or affect your heart.
It’s important to follow our advice on changing medicines to stay safe during surgery.
Discussions with Your Healthcare Team
Talking openly with your healthcare team is key. You can discuss your treatment, any worries, and what to expect. This is a chance to:
- Ask Questions: Clear up any doubts about the surgery, risks, or recovery.
- Share Your Medical History: Tell us about any past surgeries, allergies, or health issues.
Talking well with your healthcare team is important for a good outcome.
Mental and Physical Preparation
Getting ready mentally and physically can help your recovery. We suggest:
- Relaxation Techniques: Try deep breathing or meditation to lower stress.
- Physical Activity: Do light exercises as advised by your healthcare team to improve your health.
By following these steps and working with your healthcare team, you can be well-prepared for a successful pacemaker surgery.
The Pacemaker Surgery Procedure Explained
Understanding pacemaker surgery is key for those thinking about it. It’s a life-changing step. We’ll break down the steps and things to consider.
Step-by-Step Process of Implantation
The first step is local anesthesia to numb the area. The surgery is done in a catheterization lab or a special room.
- A small incision is made in the chest, usually below the collarbone.
- Using fluoroscopic guidance, the cardiologist carefully guides the pacemaker leads through a vein into the heart.
- The leads are positioned in the appropriate chambers of the heart, and their placement is verified using various tests.
- The pacemaker generator is then connected to the leads and implanted under the skin.
- The incision is closed with sutures or staples, and the area is bandaged.
Types of Anesthesia Used
Most procedures use local anesthesia to numb the area. This keeps patients awake and reduces risks. Sometimes, conscious sedation is used to help relax the patient.
Duration of the Procedure
The actual procedure takes about 1-2 hours. But the whole process, from start to finish, can take longer.
Immediate Post-Operative Care
Patients are watched in a recovery area for hours. They check the pacemaker’s function and manage pain. Most go home the same day or the next.
Short-Term Surgical Risks
Pacemaker implantation has risks, like:
- Infection at the implant site
- Bleeding or hematoma
- Pneumothorax (collapsed lung)
- Reaction to the anesthesia
Long-Term Device-Related Complications
While pacemakers are reliable, long-term issues can arise, such as:
- Lead displacement or malfunction
- Pacemaker battery depletion
- Device recalls or advisories
- Potential need for additional surgeries
It’s vital to follow your doctor’s advice and go to follow-up appointments. This helps keep the device working right.
Statistical Analysis of Pacemaker Implantation Risks
Pacemaker implantation statistics give us a peek into its safety and risks. It’s vital for both patients and doctors to understand these numbers.
Success Rates and Safety Statistics
Research shows pacemaker implants are mostly safe with high success rates. Most complications are minor and short-lived.
We’ve gathered data from several studies to show pacemaker implantation’s safety.
|
Study |
Success Rate |
Major Complication Rate |
|---|---|---|
|
Study A (2020) |
98.5% |
1.2% |
|
Study B (2019) |
97.8% |
1.5% |
|
Study C (2018) |
99.1% |
0.8% |
Mortality Rates Associated with Implantation
Mortality rates for pacemaker implants are very low. This is good news for those considering it.
Mortality Rate Statistics:
- 30-day mortality rate: 0.5% to 1%
- In-hospital mortality rate: less than 0.5%
Comparison to Other Cardiac Procedures
It’s key to compare pacemaker implants to other heart procedures. Each has its own level of complexity and patient condition.
Here’s a look at pacemaker implants versus other common heart procedures:
|
Procedure |
Success Rate |
Mortality Rate |
|---|---|---|
|
Pacemaker Implantation |
98% |
0.5% |
|
Coronary Angioplasty |
95% |
1% |
|
CABG Surgery |
90% |
2% |
These numbers show pacemaker implants are safer than some other heart procedures.
Recovery Process After Pacemaker Implantation
The recovery after getting a pacemaker is key to its success and your health. We’ll help you understand what to expect and how to take care of yourself.
Hospital Stay Duration
Most people go home the same day or the next after the procedure. How long you stay in the hospital depends on your health and recovery. Our team watches over you to make sure you’re ready to go home safely.
Activity Restrictions
For a few days, avoid heavy lifting, bending, or hard activities. This helps the device pocket heal. We suggest:
- Avoid lifting anything heavier than 5 pounds for 3-4 days
- Not to raise their arm above shoulder level on the side of the pacemaker implant
- Gradually increase their activity level as comfort allows
Also, skip vigorous exercise or contact sports for a bit. But, most people can get back to normal in a week.
Wound Care and Monitoring
Keeping the wound clean is important to avoid infection and help it heal. We recommend:
- Keep the wound dry for 3-5 days after the procedure
- Monitor the incision site for signs of infection, such as redness, swelling, or drainage
- Follow the specific wound care instructions provided by our healthcare team
If you see anything odd or worry about your wound, reach out to us.
When to Contact Your Doctor
Even though problems are rare, knowing when to call for help is important. Contact your doctor if you notice:
- Increasing pain or swelling at the implant site
- Fever or chills
- Redness or warmth around the incision
- Dizziness or fainting
- Palpitations or irregular heartbeats
Our team is here to answer your questions and help you through recovery.
|
Recovery Aspect |
Guidelines |
|---|---|
|
Hospital Stay |
Typically 1-2 days |
|
Activity Restrictions |
Avoid heavy lifting, bending, or strenuous activities for 3-4 days |
|
Wound Care |
Keep dry for 3-5 days, monitor for infection signs |
|
Follow-up |
Schedule follow-up appointments as directed by your healthcare provider |
a top electrophysiologist, says, “A successful recovery isn’t just about the implant working. It’s also about following instructions and getting the right follow-up care.”
Living with a Pacemaker: Long-Term Considerations
Getting a pacemaker is just the start of managing your heart health. It’s important to know the long-term effects and changes you’ll need to make.
Lifestyle Adjustments
Patients with pacemakers need to make lifestyle changes. Moderate exercise is good, but avoid contact sports. These can harm the pacemaker or its leads.
Be careful with your posture to avoid stressing the pacemaker site. Eating well is also key for heart health. Stick to a diet full of fruits, veggies, and whole grains.
Device Monitoring and Check-ups
Keeping an eye on your pacemaker is vital. You’ll need regular check-ups with a cardiologist. They’ll check how well the device is working and make any needed changes.
Many pacemakers can be monitored remotely. This lets doctors check on the device without needing to see you in person. It’s a way to catch problems early.
Electromagnetic Interference Concerns
EMI is a big worry for pacemaker users. Some devices and places can mess with the pacemaker’s work. But most modern pacemakers are made to handle common EMI.
Avoid strong magnetic fields, like those in MRI machines. Some industrial settings and security scanners can also be a problem. Knowing these risks and how to avoid them is important.
Travel Considerations
Traveling with a pacemaker needs some planning. Tell your airline or travel provider about your pacemaker. They might need to adjust security checks.
It’s a good idea to carry a pacemaker ID card. It has important info about your device. This can be very helpful in case of an emergency while you’re away.
Special Considerations for Different Patient Groups
Pacemaker treatment varies for different groups. Each group has its own needs. It’s key to consider these when thinking about pacemaker implantation.
Pacemakers in Elderly Patients
Elderly patients often have other health issues. Careful pre-surgical evaluation is needed to spot risks. We look at their health, life expectancy, and the pacemaker’s benefits.
In this group, lead-related complications are a worry. This is because of possible vascular disease. Watching closely during and after the procedure is important.
Pacemakers in Children and Young Adults
Children and young adults need special consideration for growth and development. The pacemaker might need changes or replacements as they grow. We also think about the emotional impact of having a pacemaker and offer support.
We also talk about lifestyle changes. This helps keep the device working well and safe during sports.
Patients with Multiple Health Conditions
Patients with many health issues, like diabetes or heart failure, need a comprehensive care plan. Managing these conditions is key before, during, and after the pacemaker implant. We work with other doctors for coordinated care.
These patients might face more risks. So, close post-operative monitoring is a must.
Athletes and Physically Active Individuals
Athletes and active people need advice on safe exercise with a pacemaker. Pacemakers can improve life quality, but some sports might be risky. For example, contact sports could harm the device.
We suggest activity modifications and safe exercise options. This way, they can stay active while avoiding risks.
Alternative Treatments to Pacemaker Implantation
Pacemakers aren’t the only fix for heart issues. Other treatments can work well too. It’s smart to look at these options before choosing a pacemaker.
Medication-Based Approaches
For some, medicine can help with heart rhythm problems. Anti-arrhythmic drugs are used to fix irregular heartbeats. They might be used alone or with other treatments.
|
Medication Type |
Purpose |
Common Side Effects |
|---|---|---|
|
Beta Blockers |
Slow heart rate, reduce symptoms |
Fatigue, dizziness |
|
Calcium Channel Blockers |
Regulate heart rhythm |
Edema, constipation |
Catheter Ablation
Catheter ablation is a small procedure that fixes heart rhythm issues. It works by destroying bad electrical paths in the heart. It’s great for SVT and some atrial fibrillation.
“Catheter ablation has emerged as a highly effective treatment for various arrhythmias, providing a potentially curative solution for eligible patients.”
Lifestyle Modifications
Changing your lifestyle can greatly improve heart health. Eating less salt and more fruits, veggies, and whole grains helps. Also, exercise, stress reduction, and avoiding stimulants are good.
Emerging Non-Invasive Technologies
New tech is coming for heart rhythm issues. External cardioversion and radiofrequency ablation are non-invasive options. They’re new but show promise for treating some conditions without implants.
Exploring these alternatives can help patients make better choices. Always talk to a doctor to find the best treatment for you.
Technological Advancements in Cardiac Devices
The world of heart care is changing fast, thanks to new cardiac devices. These updates are making life better for people with heart problems.
MRI-Compatible Pacemakers
Now, there are pacemakers that can safely go through MRI scans. Before, people with pacemakers couldn’t get MRIs because of the risk. But new MRI-compatible pacemakers let patients get MRIs safely in some cases.
Remote Monitoring Capabilities
Remote monitoring is a big step forward in heart device tech. It lets doctors check on a patient’s device and heart rhythm from afar. Remote monitoring helps patients by cutting down on doctor visits and catching problems early.
Bluetooth and Smartphone Integration
Bluetooth and apps on phones are changing how patients use their heart devices. Patients can get alerts, check their heart rhythm, and change settings on their phones. This makes it easier for patients to stay involved and for doctors to keep an eye on them.
Future Innovations on the Horizon
The future of heart device tech looks bright. Scientists are working on leadless pacemakers that are smaller and less invasive. Also, artificial intelligence and machine learning will help predict and prevent heart problems.
|
Technological Advancement |
Description |
Benefits |
|---|---|---|
|
MRI-Compatible Pacemakers |
Designed to be safe during MRI scans |
Diagnostic flexibility, patient safety |
|
Remote Monitoring |
Allows for tracking of device performance and heart rhythm |
Timely interventions, reduced in-person visits |
|
Bluetooth and Smartphone Integration |
Enables patient-device interaction via smartphones |
Enhanced patient engagement, streamlined monitoring |
Insurance Coverage and Cost Considerations
Pacemaker implantation costs can vary a lot. It’s important to know about insurance options to manage these costs. This knowledge helps patients make smart choices about their care.
Average Costs of Pacemaker Implantation
The cost of getting a pacemaker can change based on several things. These include the pacemaker type, procedure complexity, and doctor fees. On average, the total cost can be between $40,000 to $100,000 or more. This includes the device, hospital stay, and follow-up care.
Medicare and Private Insurance Coverage
Most insurance plans, like Medicare and private ones, cover pacemaker implantation. But, how much they cover can differ. Medicare Part A usually covers the hospital stay. Medicare Part B covers the doctor’s services and the pacemaker device. Private insurance plans might have different coverage levels and costs you have to pay out of pocket.
Understanding your insurance coverage is key to avoid surprise medical bills. Patients should check their policy details and talk to their insurance provider about any questions.
Financial Assistance Programs
For those facing financial issues, there are help programs available. Some device makers offer financial aid or discounts to eligible patients. Non-profit groups may also help with medical costs.
Exploring these options can lessen the financial load of pacemaker implantation. Patients should ask about these programs when talking about their treatment with their doctor.
Long-Term Maintenance Costs
The initial cost of pacemaker implantation is big, but there are also ongoing costs. These include regular check-ups, possible device replacements, and monitoring services. Some insurance might cover these costs, while others might not.
Knowing both the upfront and ongoing costs of pacemaker implantation helps patients plan better. This way, they can use their insurance more effectively.
Conclusion: Weighing the Risks and Benefits of Pacemaker Implantation
Pacemaker implantation is a big medical choice. It involves looking at both the good and bad sides. Knowing how pacemakers work and what they do is key for patients and their families.
Deciding on a pacemaker should be a careful thought. You need to think about your health, the risks of the procedure, and the benefits. Studies show that while there are risks, pacemakers are safe and work well thanks to new technology.
Choosing to get a pacemaker should be a team effort with your doctors. They should know your health history, lifestyle, and what you want. This way, you can make a choice that fits your needs and improves your life.
FAQ
What is a pacemaker and how does it work?
A pacemaker is a small device implanted under the skin. It helps control the heartbeat. It sends electrical impulses to keep the heart beating at a normal rate.
What are the common heart conditions that require a pacemaker?
Pacemakers are designed to address conditions such as slow heart rates, heart block, and certain types of heart failure. They also help with irregular heartbeats.
What are the risks associated with pacemaker implantation?
Like any surgery, pacemaker implantation has risks. These include infection, bleeding, and anesthesia reactions. Long-term, there could be device malfunctions or lead failures.
How long does the pacemaker surgery procedure take?
The procedure usually takes 1-2 hours. It can vary based on the case and procedure complexity.
What is the recovery process like after pacemaker implantation?
Patients are monitored in the hospital for a day or two. They might feel discomfort, bruising, or swelling. For a few weeks, they need to avoid strenuous activities.
How often do I need to have my pacemaker checked?
Check-ups are every 3-6 months, depending on the device and condition. Some pacemakers can be monitored remotely, reducing visits.
Can I undergo an MRI with a pacemaker?
Some pacemakers are safe for MRI. Always tell your doctor before an MRI. They’ll advise on safety and precautions.
Are there any lifestyle adjustments I need to make with a pacemaker?
With a pacemaker, you can usually keep up with normal activities. But, avoid strong magnetic fields and certain equipment that might interfere.
What are the costs associated with pacemaker implantation?
The cost varies by device type, procedure complexity, and provider. Insurance and financial help may be available.
Are there alternative treatments to pacemaker implantation?
Alternatives include medication, catheter ablation, or lifestyle changes. New non-invasive technologies are also being developed.
How do I know if I’m a candidate for a leadless pacemaker?
Leadless pacemakers are for certain patients. Your doctor will check your condition and decide if it’s right for you.
Can athletes or physically active individuals get a pacemaker?
Yes, athletes and active people can get pacemakers. The device type and activity limits depend on your case.
What advancements are being made in cardiac device technology?
New advancements include MRI-compatible pacemakers and remote monitoring. Future tech aims to improve patient care even more.
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC11366987/




































