
For those with hyperparathyroidism, parathyroid surgery is often a top choice. Many worry if removed parathyroid glands can grow back. It’s important to know the details of this surgery, as it affects those considering or going through it.
Parathyroid glands don’t grow back after parathyroidectomy. But, the hormone they produce can start making too much again. Our goal is to give top-notch health info. We help patients worldwide with detailed care plans.
Key Takeaways
- Parathyroid glands do not regrow after removal.
- Parathyroid hormone overproduction may recur after surgery.
- Understanding hyperparathyroidism treatment options is key.
- Parathyroid surgery is a big medical step.
- How often it happens can vary for each person.
The Anatomy and Function of Parathyroid Glands
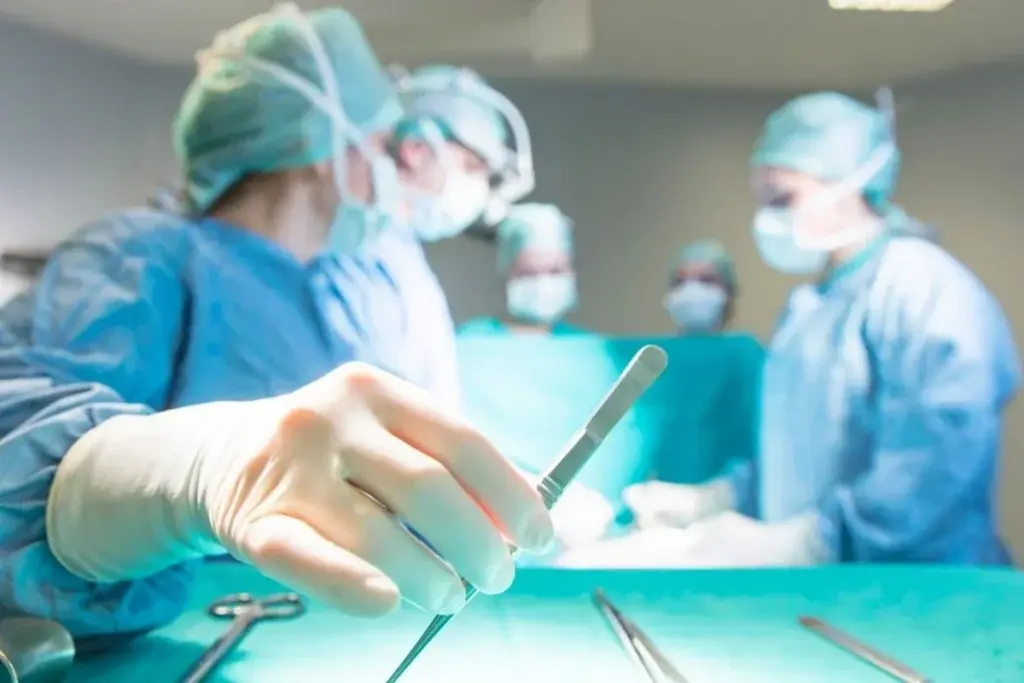
The parathyroid glands are near the thyroid gland and help keep our calcium levels balanced. They are small, like rice, and found in the neck. Knowing how they work is key to understanding parathyroid surgery.
Location and Number of Parathyroid Glands
Most people have four parathyroid glands. They are near the thyroid gland, with two on each side. Their exact spot can differ from person to person, which matters in surgery.
Role in Calcium Regulation
The parathyroid glands control our body’s calcium levels. Calcium is important for muscles, nerves, and bones. They make parathyroid hormone (PTH) to keep calcium levels right.
Parathyroid Hormone (PTH) Production
PTH is a hormone made by the parathyroid glands. It helps keep calcium levels balanced. When calcium levels drop, PTH is released. It helps increase calcium by releasing it from bones and improving absorption from food.
In short, the parathyroid glands are key for calcium balance through PTH. Knowing how they work helps us understand parathyroid disorders and surgery.
Common Parathyroid Disorders Requiring Surgery
It’s important to know about parathyroid disorders that need surgery. These conditions can really affect a person’s life. Surgery is often the best way to treat them.
Secondary Hyperparathyroidism
Secondary hyperparathyroidism happens when the parathyroid glands get too much stimulation. This usually comes from chronic kidney disease or not enough vitamin D. It makes the glands produce too much parathyroid hormone (PTH), upsetting calcium levels.
If not treated, this condition can lead to serious problems. These include bone disease and heart issues. Surgery, like removing part of the gland, might be needed to fix it.
Parathyroid Adenomas and Hyperplasia
Parathyroid adenomas and hyperplasia are common causes of primary hyperparathyroidism. An adenoma is a benign tumor on a gland. Hyperplasia means the glands get too big.
Both cause the glands to make too much PTH. This leads to too much calcium in the blood. Symptoms include weak bones, kidney stones, and brain problems. Taking out the affected gland(s) is usually the best treatment.
Symptoms and Diagnosis
Symptoms of parathyroid disorders vary. They can include feeling tired, bone pain, kidney stones, and brain fog. Doctors use blood tests and imaging to find the problem.
Getting the right diagnosis is key to treating these disorders. Here’s a table that shows what doctors look for:
|
Condition |
Serum Calcium |
PTH Level |
Common Symptoms |
|---|---|---|---|
|
Primary Hyperparathyroidism |
Elevated |
Elevated or normal |
Bone pain, kidney stones, fatigue |
|
Secondary Hyperparathyroidism |
Normal or low |
Elevated |
Bone disease, cardiovascular issues |
|
Parathyroid Adenoma/Hyperplasia |
Elevated |
Elevated |
Osteoporosis, neuropsychiatric symptoms |
A leading expert says, “Getting the right diagnosis and surgery is key to treating parathyroid disorders. It improves patient outcomes.”
“Understanding the cause and choosing the right surgery is the secret to success.”
A Parathyroid Surgeon
Understanding Parathyroid Surgery Procedures
It’s important for patients to know about the different parathyroid surgery procedures. These surgeries have evolved, with new techniques for each patient’s needs. This makes treatment more precise and effective.
Minimally Invasive Parathyroidectomy
Minimally invasive parathyroidectomy uses smaller cuts and less damage than old surgeries. It’s chosen when the bad gland can be found before surgery. This method leads to less pain, quicker recovery, and better looks.
Traditional Four-Gland Exploration
When it’s hard to find the bad gland before surgery, a bigger surgery is needed. This lets the surgeon check all glands for problems. It’s more invasive but ensures a thorough check.
Subtotal Parathyroidectomy
Subtotal parathyroidectomy removes most of the gland but keeps a bit to help function. It’s for those with many glands affected. It aims to remove bad tissue while keeping enough to avoid too little parathyroid hormone.
Total Parathyroidectomy With Autotransplantation
This surgery removes all glands and then moves some to the forearm. It’s for high-risk cases of hyperparathyroidism. It makes it easier to watch for any return of the disease.
Each surgery has its own reasons, benefits, and risks. The right choice depends on the disease, how far it’s spread, and the patient’s health. Knowing these options helps patients make better choices for their treatment.
Do Removed Parathyroid Glands Grow Back?
Many patients worry if their parathyroid glands can grow back after surgery. The answer is simple: removed parathyroid glands do not regrow. But, there are some details to explore further.
The Biology of Parathyroid Tissue
Parathyroid glands are special organs that help control calcium levels in our bodies. They make parathyroid hormone (PTH). Knowing how these glands work is key to understanding if they can grow back.
These glands are near the thyroid gland in the neck. Usually, there are four of them. They produce PTH to keep calcium levels balanced. If they become too active or sick, surgery might be needed to remove them.
Scientific Evidence on Regeneration
Research has given us insights into parathyroid tissue’s regrowth abilities. Studies show that while parathyroid tissue can be transplanted and work, it doesn’t grow back in its original spot.
A study in a well-known medical journal found that transplanted parathyroid tissue can work well. But, this doesn’t mean the original glands grow back. The success of transplanting parathyroid tissue shows it can adapt and function in different places.
|
Study |
Findings |
Implications |
|---|---|---|
|
Parathyroid Autograft Study |
Functioning parathyroid tissue can be successfully transplanted |
Potential for treating hypoparathyroidism |
|
Regeneration Study |
No evidence of parathyroid gland regrowth in original location |
Removed glands do not regrow |
Misconceptions About Regrowth
Even though science agrees, there are myths about parathyroid gland regrowth. Some think symptoms returning means the glands have grown back. But, other reasons like extra glands or not removing all diseased tissue can cause symptoms to come back.
It’s important for patients to know that while the removed glands don’t grow back, other issues can cause symptoms to return. Understanding this helps manage expectations and plan for follow-up care.
By clearing up these myths and knowing the science behind parathyroid tissue, patients can better understand their condition and treatment options.
Remnant Tissue: A Source of Recurrent Disease
Understanding remnant tissue’s role in recurrent disease is key to managing and treating it. Parathyroid surgery aims to remove the bad tissue causing hyperparathyroidism. But, sometimes, leftover tissue can cause the disease to come back.
Incomplete Removal During Surgery
One main reason for hyperparathyroidism coming back is not removing all tissue during surgery. This can happen if the surgeon can’t find all bad glands or if glands are in hard-to-spot places.
Incomplete removal means the disease might not go away, needing more tests and maybe more surgery. New imaging and hormone tests help, but there’s always a chance not all tissue is removed.
Supernumerary (Extra) Parathyroid Glands
Some people have supernumerary parathyroid glands, extra glands beyond the usual four. These extra glands can cause the disease to come back if they’re not found and removed first.
Research shows these extra glands are more common than thought, found in up to 13% of people. This shows how important it is to do detailed tests and surgery to find and remove all hormone-making tissue.
Ectopic Parathyroid Tissue
Ectopic parathyroid tissue is glands or tissue in the wrong place, like in the thyroid or thymus. Finding and removing this tissue can be hard and might lead to the disease coming back if not done right.
The challenge of ectopic parathyroid tissue shows the need for a skilled surgeon. They must use the latest imaging and surgery methods to find and remove all bad tissue.
Parathyroid Autotransplantation and Long-Term Outcomes
Parathyroid autotransplantation is a surgery that puts back parathyroid tissue. It’s key for those who have had a lot of parathyroid tissue removed. This helps restore normal parathyroid function.
The Process of Tissue Reimplantation
In this surgery, the removed parathyroid tissue is put back in the body. It’s usually in the forearm or neck muscles. This helps the body control calcium levels again.
We check if autotransplantation is right for each patient. We look at how bad the parathyroid disease is and the patient’s health.
Functionality Rates at 10 Years
Research shows that autotransplantation works well over time. About 49% of patients keep their autografts working 10 years after surgery. This means their parathyroid function is mostly back to normal.
Recurrence Rates After Autografting
Even with autotransplantation, some patients might see their condition come back. In some cases, up to 83% of patients experience recurrence. So, it’s important to keep an eye on patients over the long term.
|
Outcome |
Rate |
Follow-up Period |
|---|---|---|
|
Functionality Rate |
49% |
10 years |
|
Recurrence Rate |
Up to 83% |
Varies |
Knowing how autotransplantation works over time helps us manage patient hopes and care. We keep a close eye on patients to make sure their treatment is working and to fix any problems quickly.
Recurrence Rates Following Different Surgical Approaches
It’s important to know how often hyperparathyroidism comes back after surgery. The type of surgery can affect how likely it is to come back. So, it’s key to look at how different surgeries do.
After Subtotal Parathyroidectomy
Subtotal parathyroidectomy removes most but not all parathyroid tissue. It’s used to treat hyperparathyroidism while keeping some function. Studies show that it can come back in 10% to 20% of people over 10 years.
Key factors influencing recurrence include how much tissue is removed and if any hyperfunctioning tissue is left. “The goal of subtotal parathyroidectomy is to balance the need for disease control with the preservation of parathyroid function,” experts say.
After Total Parathyroidectomy
Total parathyroidectomy removes all parathyroid glands, sometimes with autotransplantation to avoid permanent hypoparathyroidism. The rate of coming back is about 14%. But, it can change based on autotransplantation and the surgery method.
Recurrence can happen even after total parathyroidectomy if there’s leftover or ectopic parathyroid tissue. So, it’s important to keep an eye on it over time.
Risk Factors for Recurrent Disease
Several things can make hyperparathyroidism come back after surgery. These include:
- Incomplete removal of hyperfunctioning parathyroid tissue
- Presence of supernumerary or ectopic parathyroid glands
- Genetic predispositions, such as in familial hyperparathyroidism syndromes
Knowing these risk factors helps manage patient hopes and plan follow-up care. As we get better at surgery and monitoring, we can lower recurrence rates. This improves how well patients do.
Persistent vs. Recurrent Hyperparathyroidism
It’s important to know the difference between persistent and recurrent hyperparathyroidism. This helps doctors plan the best treatment and talk to patients clearly.
Defining Persistence (Failed Initial Surgery)
Persistent hyperparathyroidism means the disease stays after surgery. It happens when the first surgery didn’t fix the problem. This could be because not all bad tissue was removed or because there are ectopic glands.
Doctors look for high PTH and calcium levels right after surgery to diagnose persistent hyperparathyroidism.
Defining Recurrence (Return After Successful Surgery)
Recurrent hyperparathyroidism is when the disease comes back after it seemed to be fixed. This means PTH and calcium levels were normal for a while before they went back up. It can happen because of tissue growth or new disease.
Diagnostic Criteria and Differentiation
To tell persistent from recurrent hyperparathyroidism, doctors use several tools. They look at:
- PTH levels: High or normal levels show the disease is present.
- Calcium levels: High calcium is common, but it can also be normal.
- When it happens: If it’s right after surgery, it’s persistent. If it comes back later, it’s recurrent.
Knowing the difference is key for treatment. It helps doctors decide if more surgery, medicine, or watching is needed. By understanding these differences, doctors can help patients better.
Post-Operative Monitoring of Parathyroid Function
After surgery, it’s key to watch how the parathyroid glands work. Patients need to see their doctors often to check their hormone and calcium levels. This makes sure they’re okay.
PTH and Calcium Level Testing Protocols
Testing PTH and calcium levels is very important. PTH level testing shows if the glands are working right. Calcium level testing is also key because it tells us if there are problems with the glands.
These tests are done at set times during check-ups. How often depends on the patient’s health and the doctor’s advice.
Frequency of Follow-up Evaluations
How often you see a doctor after surgery can change. At first, you might see them a lot, then less often if you’re doing well.
At these visits, doctors check your health and do tests. They look at your PTH and calcium levels to see if everything is okay.
Interpreting Post-Surgical Lab Results
Understanding lab results after surgery is tricky. Doctors look at PTH and calcium levels to see if they’re normal. They watch for any signs of trouble.
If PTH levels stay high, it might mean there’s more gland tissue or another problem. Low levels could mean the glands aren’t making enough hormone.
By watching these levels closely, doctors can make sure patients do well after surgery.
Elevated PTH After Parathyroidectomy
After parathyroidectomy, some patients have high PTH levels but normal calcium. This is a tricky situation. We will look into how common it is, what it means, and how to manage it.
Prevalence of Persistently High PTH
About 24% of patients have high PTH levels after parathyroidectomy. Research on the National Institutes of Health shows this is not rare. It’s important to keep a close eye on these patients.
Normal Calcium with Elevated PTH: What It Means
Having normal calcium but high PTH means the body’s metabolism is complex. This could be because of vitamin D deficiency or the body not responding well to PTH. We must dig deeper to find out why.
Treatment Approaches for Persistent Elevation
Managing high PTH after parathyroidectomy requires a detailed plan. We monitor calcium and PTH levels, check for vitamin D deficiency, and might use medications like calcimimetics. A good treatment plan is key to helping patients.
|
Cause |
Management Strategy |
|---|---|
|
Vitamin D Deficiency |
Vitamin D Supplementation |
|
Renal Resistance to PTH |
Monitoring and Adjusting Treatment as Necessary |
|
Residual Parathyroid Tissue |
Further Surgical Evaluation |
Complications and Risks of Parathyroid Surgery
It’s important to know the risks and complications of parathyroid surgery. This knowledge helps patients make informed decisions. While surgery is usually safe and effective, there are possible complications.
Short-Term Complications
Short-term issues after parathyroid surgery include:
- Hemorrhage or Hematoma: Bleeding can happen, which might block the airway. This is a serious and potentially life-threatening problem.
- Nerve Injury: The surgery might damage nerves. This can affect your voice or cause vocal cord paralysis.
- Hypocalcemia: Low calcium levels can occur. This might be due to hungry bone syndrome or damage to the parathyroid glands.
These issues are rare but can greatly affect recovery and quality of life.
Long-Term Complications
Long-term issues can have lasting effects on health and well-being. Some of these include:
- Persistent or Recurrent Hyperparathyroidism: Sometimes, the condition can stay or come back. This might need more treatment or surgery.
- Hypoparathyroidism: If the parathyroid glands are damaged or removed, it can lead to chronic low calcium levels. This requires lifelong management.
- Osteoporosis: Changes in bone density can happen. This might lead to osteoporosis, which is a concern if PTH levels are significantly altered.
Hypocalcemia and Hypoparathyroidism
Hypocalcemia and hypoparathyroidism are big concerns after parathyroid surgery. Hypocalcemia means low calcium levels in the blood. It can cause symptoms like tingling, muscle cramps, and in severe cases, seizures. Hypoparathyroidism is when the parathyroid glands don’t work well. This leads to not enough PTH, a hormone that helps regulate calcium.
Managing these conditions involves watching calcium and PTH levels closely. Treatment includes calcium and vitamin D supplements, and sometimes synthetic PTH.
Reoperation for Recurrent Hyperparathyroidism
When hyperparathyroidism comes back after surgery, a second surgery might be needed. This second surgery is a big deal. It’s important to think about why it’s happening and what risks and benefits it might have.
Indications for Second Surgery
Doctors might suggest a second surgery if the disease comes back. This usually means the parathyroid hormone levels are high again. They use imaging to find the problem tissue.
Some reasons for a second surgery include:
- Recurrent or persistent hyperparathyroidism with significant symptoms or complications
- Failure of medical management to control the condition
- Presence of a parathyroid adenoma or hyperplasia that was not adequately addressed during the initial surgery
Surgical Approaches for Recurrent Disease
The second surgery can be harder because of scarring and changed anatomy. Surgeons might use a minimally invasive method if the disease is in one spot.
Surgical Techniques:
|
Surgical Approach |
Description |
Advantages |
|---|---|---|
|
Minimally Invasive Parathyroidectomy |
A focused approach using intraoperative PTH monitoring to confirm removal of the affected gland |
Less invasive, potentially fewer complications, quicker recovery |
|
Traditional Four-Gland Exploration |
A thorough check of all parathyroid glands |
Good for complex cases, might be more successful |
Success Rates and Increased Risks
The success of a second surgery can vary. Some studies show a cure rate of 80% to over 90%. But, there are more risks, like vocal cord problems and low parathyroid hormone levels.
It’s key to talk to your surgeon about the risks and benefits. This helps you decide if a second surgery is right for you.
Non-Surgical Management Options
Not everyone with hyperparathyroidism needs surgery. There are good non-surgical ways to manage it. These options are for those who can’t or don’t want to have surgery.
Calcimimetic Medications
Calcimimetics are drugs that act like calcium on the parathyroid gland. They help lower parathyroid hormone (PTH) levels. Cinacalcet is a well-known calcimimetic that helps manage hyperparathyroidism.
- Cinacalcet is great for secondary hyperparathyroidism in patients with chronic kidney disease.
- It works by activating calcium-sensing receptors on the parathyroid gland, reducing PTH secretion.
Bisphosphonates and Other Drug Therapies
Bisphosphonates are used to manage hyperparathyroidism, focusing on bone issues. They:
- Reduce bone resorption
- Increase bone density
- Lower the risk of fractures
Other treatments include vitamin D analogs. They help manage secondary hyperparathyroidism by lowering PTH levels and improving calcium absorption.
Monitoring Without Intervention
For some with mild or asymptomatic hyperparathyroidism, just monitoring is enough. This means:
- Regular checks of calcium and PTH levels
- Assessments of bone density
- Looking at symptoms and possible complications
Healthcare providers can decide when to start treatment, whether it’s surgery or not, by watching the condition closely.
Every patient is different. The choice of treatment depends on how severe the condition is, the patient’s health, and what they prefer.
Advances in Parathyroid Surgery Techniques
Parathyroid surgery has seen big changes thanks to new imaging, monitoring, and minimally invasive methods. These updates have made surgeries better and made patients happier.
Intraoperative PTH Monitoring
One big step forward is using intraoperative parathyroid hormone (PTH) monitoring. This method lets surgeons check if the surgery is working right away. Intraoperative PTH monitoring has been shown to improve the accuracy of parathyroidectomy, cutting down on the need for more surgeries.
Improved Imaging for Localization
New imaging methods have made it easier to find parathyroid glands. Tools like high-resolution ultrasound, 4D CT scans, and sestamibi scans give clear pictures of where the abnormal glands are. This helps surgeons plan more precise and less invasive surgeries.
- High-resolution ultrasound offers detailed images of the neck and parathyroid glands.
- 4D CT scans provide both anatomical and functional information about the parathyroid glands.
- Sestamibi scans help identify parathyroid adenomas and hyperplastic glands.
Minimally Invasive Approaches
Minimally invasive parathyroidectomy is getting more popular. It offers less recovery time and less pain after surgery. This method uses smaller cuts and is helped by new imaging and PTH monitoring. It makes surgery more focused, which can lower the risk of problems.
These new ways of doing parathyroid surgery have changed the field a lot. They give patients better, less invasive treatments. As technology keeps getting better, we’ll see even more progress in how we care for patients.
Choosing a Specialized Parathyroid Surgery Center
Choosing the right parathyroid surgery center is key to a good surgery. Patients need to trust their surgical team and know they’ll get top-notch care.
Surgeon Experience and Volume
The surgeon’s experience and how often they do parathyroid surgeries matter a lot. A surgeon who does many parathyroid surgeries is likely to be very skilled. It’s smart to ask how much experience your surgeon has with these surgeries.
“The more surgeries a surgeon has done, the better they are at handling tough cases,” says a top parathyroid surgery expert.
Questions to Ask Your Surgeon
It’s important to ask the right questions to make sure you’re in good hands. You might want to ask about:
- The surgeon’s experience with parathyroid surgery
- The surgical method they suggest for your case
- If they use intraoperative PTH monitoring
- How they handle follow-up care and monitoring after surgery
Benefits of Multidisciplinary Care
A team of doctors, including endocrinologists and radiologists, work together in parathyroid surgery. This team effort means your whole situation is looked at, leading to better care and treatment.
Choosing a center with a team like this offers many benefits. You get:
- A detailed check-up before surgery
- A treatment plan made just for you
- Better care and check-ups after surgery
In short, picking a specialized parathyroid surgery center with a skilled team is essential for the best results. By researching and asking the right questions, you can make a smart choice and start your journey to a successful surgery.
Conclusion: Living Well After Parathyroid Surgery
Patients can live well after parathyroid surgery with the right care. We’ve looked at the challenges of parathyroid disorders and the different surgery options. We also talked about the need for post-operative checks.
Recovering from parathyroid surgery means keeping an eye on your health. This includes regular check-ups and blood tests to check your calcium and PTH levels. Knowing the pros and cons of surgery helps patients make the best choices for themselves.
We aim to help international patients with detailed information and care. With the right support, patients can get through the recovery and feel better. Focusing on long-term health helps patients enjoy a better life after surgery.
FAQ
What is parathyroid surgery?
Parathyroid surgery, also known as parathyroidectomy, is a procedure to remove parathyroid glands or tumors. These are the causes of hyperparathyroidism.
Can a removed parathyroid gland grow back?
No, removed parathyroid glands do not grow back. But, leftover tissue can cause hyperparathyroidism again.
What are the common disorders that require parathyroid surgery?
Common disorders include primary and secondary hyperparathyroidism. Also, parathyroid adenomas and hyperplasia need surgery.
What is the difference between minimally invasive parathyroidectomy and traditional four-gland exploration?
Minimally invasive parathyroidectomy is a less invasive procedure. It targets a single gland or a known disease area. Traditional four-gland exploration examines all four parathyroid glands.
What is parathyroid autotransplantation?
Parathyroid autotransplantation is a procedure. It involves reimplanting parathyroid tissue into another body part. This is often done during total parathyroidectomy.
How is parathyroid function monitored after surgery?
Parathyroid function is checked through PTH and calcium level tests. The frequency of these tests depends on the surgeon.
What does it mean to have elevated PTH after parathyroidectomy?
Elevated PTH after surgery can mean hyperparathyroidism is not fully treated. Further evaluation is needed to find the cause.
What are the possible complications of parathyroid surgery?
Possible complications include hypocalcemia and hypoparathyroidism. There are also short-term and long-term complications.
When is reoperation necessary for recurrent hyperparathyroidism?
Reoperation is considered when hyperparathyroidism comes back. This is when other treatments have failed.
What are the non-surgical management options for hyperparathyroidism?
Non-surgical options include calcimimetic medications and bisphosphonates. Monitoring without treatment is also an option.
How do I choose a specialized parathyroid surgery center?
Choose a center based on the surgeon’s experience and volume. Ask about their approach and look for a multidisciplinary team.
What are the benefits of intraoperative PTH monitoring during parathyroid surgery?
Intraoperative PTH monitoring ensures the removal of hyperfunctioning parathyroid tissue. It reduces the risk of hyperparathyroidism coming back.
What is the role of imaging in parathyroid surgery?
Imaging is key in finding parathyroid adenomas or hyperplastic glands. It guides the surgical approach.
References
https://www.ncbi.nlm.nih.gov/books/NBK563274


































