
People thinking about parathyroidectomy surgery worry about the incision size and the scar. These worries are key because they affect how well you recover and how you look afterward.
Fortunately, parathyroidectomy surgery has gotten better. Now, doctors can make smaller cuts. This means less scarring and a quicker recovery. It’s all thanks to new surgical tools and methods.
Key Takeaways
- Modern parathyroidectomy techniques have significantly reduced incision sizes.
- Smaller incisions result in less scarring and faster recovery times.
- Advanced surgical technology enables more precise procedures.
- Patients can expect improved cosmetic outcomes.
- Minimally invasive parathyroidectomy is supported by leading international standards.
What Happens During a Parathyroidectomy Procedure
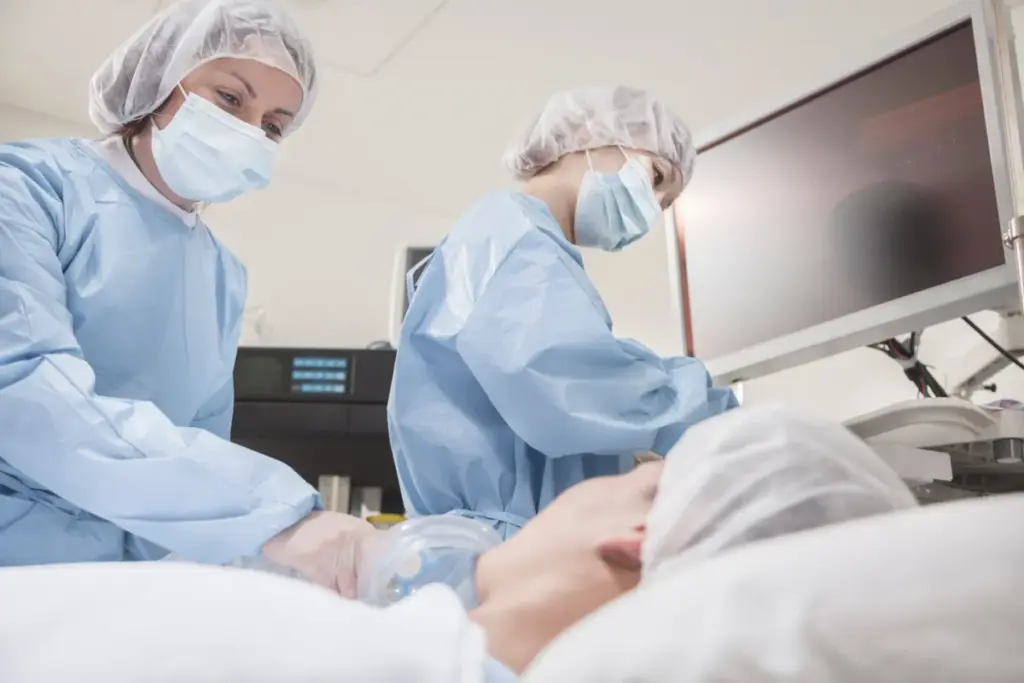
When parathyroid glands work too hard, surgery might be needed. This surgery, called a parathyroidectomy, removes overactive glands. It’s important for patients to know why and how this surgery works.
The Function of Parathyroid Glands
The parathyroid glands help keep calcium levels right in our blood. They make parathyroid hormone (PTH) to keep calcium balanced. But, if these glands make too much PTH, it can lead to hyperparathyroidism.
This condition can cause problems like weak bones, kidney stones, and heart issues.
Common Reasons for Parathyroid Surgery
Mostly, people get parathyroid surgery for hyperparathyroidism. This usually happens because of a benign tumor on one gland. Luckily, most patients only need a small surgery because of this.
This smaller surgery is thanks to better ways to find the problem before surgery. It means less pain and quicker healing for patients.
Knowing why parathyroidectomy is needed and how glands work helps patients get ready. This surgery is a proven way to treat hyperparathyroidism. With today’s methods, it’s done with less harm, leading to faster recovery.
The Evolution of Parathyroidectomy Incision Sizes
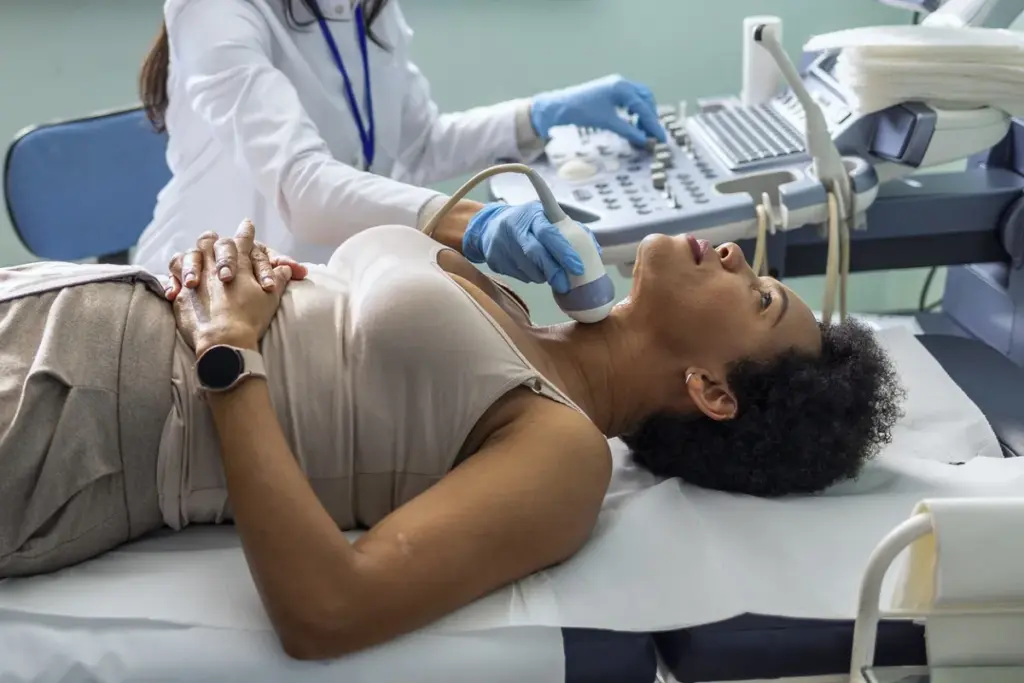
The way we do parathyroidectomy surgery has changed a lot over time. This change is mainly in the size of the incisions. As we learn more about treating hyperparathyroidism, our surgery methods have improved.
Oldly, parathyroidectomy needed big cuts to explore the neck well. But, this made recovery longer and left big scars.
Traditional Large Incisions: Historical Approach
Before, surgeons made big cuts to see and reach the parathyroid glands. This old way was needed because of the tech limits back then.
“The old open way meant longer hospital stays and longer recovery,” a study on parathyroid surgery history says.
The Shift Toward Minimally Invasive Techniques
New tech in finding and checking the glands during surgery has led to smaller cuts. Now, parathyroid surgery often uses cuts of 2.5–3.5 cm, much smaller than before.
This change has made the surgery look better and recover faster. It makes treating hyperparathyroidism more appealing to patients.
Thanks to these new tools, surgeons can do the surgery more accurately and with less harm to the patient. This shows the progress in modern surgery.
Modern Parathyroidectomy Incision Measurements
Parathyroid surgery has changed a lot, moving towards smaller incisions. This change helps with recovery and looks better. It’s thanks to new surgical methods and technology.
Standard Incision Size: 2.5-3.5 cm
Older parathyroidectomy incisions were 2.5 to 3.5 cm. This size lets surgeons easily find and remove the affected gland. But, these incisions can leave noticeable scars.
Minimally Invasive Incisions: As Small as 15-20 mm
Now, with minimally invasive parathyroidectomy, incisions can be just 15-20 mm. This is true when the gland’s location is known beforehand. It means smaller scars and less damage to tissue. This leads to quicker parathyroidectomy recovery and better looks.
What These Measurements Mean for Patients
Smaller incisions mean big benefits for patients. They cause less damage, lower the risk of problems, and hurt less after surgery. Plus, the scars are smaller and less visible. This makes minimally invasive parathyroidectomy a good choice for many.
In short, smaller incisions in parathyroid surgery are a big step forward. Knowing about these sizes helps patients make better choices. It means they can get the latest in surgical care.
Factors That Determine Your Parathyroidectomy Incision Size
Many things can affect how big your parathyroidectomy incision will be. Knowing these can help you get ready for your surgery. It also helps you understand what to expect after.
Patient Body Mass Index (BMI)
Your BMI is important for figuring out your incision size. People with a higher BMI might need a bigger incision. This is because it’s easier for the surgeon to see and work inside. Our doctors think about this when they plan your surgery.
Thyroid Size and Neck Anatomy
The size of your thyroid gland and your neck’s shape matter too. If your thyroid is big or your neck is shaped differently, you might need a bigger incision. This ensures the surgery is safe and done right.
Number of Glands Requiring Exploration
How many parathyroid glands need to be checked during surgery also matters. If you need to have more glands looked at, your incision might be bigger. This is different from someone who only needs one gland checked.
Surgeon Experience and Technique
The skill and method of your surgeon are key in deciding your incision size. More experienced surgeons can often make smaller incisions. They do this while keeping the surgery safe and effective. Our surgeons use special techniques to make scars smaller and help you heal faster.
We look at all these factors to make sure your surgery is just right for you. This way, we can lower the chances of problems. And we aim to get the best results for you.
Single Gland vs. Multiple Gland Disease
Knowing if you have single gland or multiple gland disease is key. It decides how big the incision will be and how complex the surgery will be.
Why 80-85% of Patients Qualify for Smaller Incisions
Most patients (80–85%) have just one bad gland. This means they can have smaller, more precise cuts. Pre-operative tests help find the bad gland. This makes the surgery less invasive, cheaper, and faster.
When Full Neck Exploration Is Necessary
But, if more glands are sick, a bigger surgery is needed. This surgery looks at the whole neck to find and remove the bad glands. It’s more invasive but makes sure the surgery is safe and works well.
Pre-operative Testing and Its Impact
Tests before surgery are very important. They show how much disease there is and plan the surgery. New imaging helps figure out if it’s one gland or more. This helps the surgeon choose the right cut and plan.
By knowing how many glands are sick, we can make the surgery fit the patient’s needs. This way, we get the best results for them.
Types of Parathyroidectomy Surgical Approaches
Modern surgery has led to many parathyroidectomy methods. Each has its own benefits. The right approach depends on the patient’s health, the surgeon’s skill, and the parathyroid glands’ details.
Traditional Bilateral Neck Exploration
This method uses a big incision to see both sides of the neck. It was common but now less used because of newer, better ways.
Focused (Minimally Invasive) Parathyroidectomy
This method is popular for its small incision and less harm to tissue. It’s best for those with just one bad parathyroid gland.
Endoscopic and Video-Assisted Techniques
These use small cuts and special tools to see the glands. They cause less scarring and help patients heal faster.
Radio-guided Parathyroidectomy
This method uses a radioactive tracer to find the glands during surgery. It’s great when the glands are hard to find.
|
Surgical Approach |
Incision Size |
Benefits |
|---|---|---|
|
Traditional Bilateral Neck Exploration |
Larger incision |
Comprehensive visualization of both sides of the neck |
|
Focused (Minimally Invasive) Parathyroidectomy |
Smaller incision (2.5-3.5 cm) |
Less tissue trauma, quicker recovery |
|
Endoscopic and Video-Assisted Techniques |
Very small incisions |
Minimal scarring, rapid recovery |
|
Radio-guided Parathyroidectomy |
Varies |
Improved localization of parathyroid glands |
Each method has its own time and place. The right choice depends on the patient’s health and their parathyroid disease specifics.
Pre-Operative Localization Studies
Starting a successful parathyroidectomy needs to find the right spot for the surgery. We use top-notch imaging to spot the PTH gland or glands. This makes sure the surgery hits its mark.
Sestamibi Scans and Ultrasound
Sestamibi scans are key in finding the parathyroid glands. They work well with ultrasound to pinpoint the bad gland. This combo helps plan a minimally invasive parathyroidectomy with great accuracy.
4D CT Scans and MRI
At times, we need 4D CT scans or MRI for more details. These scans give us a clear picture of the glands’ location. They help plan the parathyroid gland removal surgery.
How Accurate Localization Enables Smaller Incisions
Finding the right spot before surgery lets us use smaller cuts. Knowing exactly where the gland is, surgeons can focus their work. This means smaller cuts and quicker healing. It’s all about top-notch care for our patients.
What to Expect Before Your Parathyroidectomy
Before your parathyroidectomy, knowing what to expect can make you feel more in control. We’ll help you get ready for your surgery with the key steps to take.
Pre-surgical Consultations
You’ll meet with your surgeon and healthcare team before surgery. These talks are key to discuss your medical history and the surgery details. It’s your chance to ask about parathyroid surgery recovery and healing.
Discussing Incision Size With Your Surgeon
Talk about the incision size for your calcium gland removal with your surgeon. They’ll explain how they decide and what scarring you might see. Knowing this can ease worries about how you’ll look after.
Preparation in the Days Before Surgery
You’ll get instructions on how to prepare for your surgery. This might include changing your diet, stopping certain meds, and more. It’s important to follow these steps closely for a smooth surgery and recovery.
|
Pre-Surgical Task |
Description |
Timeline |
|---|---|---|
|
Consultations |
Meet with your surgeon and healthcare team to discuss your surgery and recovery. |
1-2 weeks before surgery |
|
Dietary Changes |
Adjust your diet as instructed by your healthcare team. |
2-3 days before surgery |
|
Medication Adjustment |
Stop or adjust medications as directed by your surgeon. |
As instructed |
The Day of Your Parathyroidectomy Surgery
Getting ready for your parathyroid surgery can make you feel less anxious. Knowing what happens on the day can make things easier. A lot of steps are planned to make sure everything goes smoothly.
Anesthesia Options
You’ll get anesthesia to keep you comfortable during the surgery. General anesthesia is usually used, so you’ll be asleep. This keeps the area clean and pain-free.
Positioning and Preparation
Once you’re asleep, you’ll be placed on the table for the best access. Your neck will be cleaned to prevent infection. We do everything we can to keep you safe and make the PTH surgery successful.
The Incision Process
The incision size and location are planned carefully. We aim for a small incision to remove the gland(s) safely. For many, the incision is about 2-3 cm long.
Intraoperative Monitoring
We monitor the surgery closely to make sure it’s going right. We check your PTH levels to confirm the gland(s) are removed. This helps us get the best results and avoid problems.
|
Step |
Description |
Purpose |
|---|---|---|
|
Anesthesia Administration |
General anesthesia is given to the patient. |
To ensure patient comfort and maintain a sterile environment. |
|
Positioning |
Patient is positioned for optimal access. |
To facilitate the surgical procedure. |
|
Incision |
A carefully planned incision is made. |
To access the parathyroid glands with minimal scarring. |
|
Intraoperative Monitoring |
PTH levels are monitored during surgery. |
To confirm the removal of the correct gland(s) and adjust as necessary. |
Knowing what happens during your parathyroid surgery can make you feel more ready. If you have any questions or worries, we’re here to help. We’ll support you from the start to the parathyroid surgery recovery time.
Comparing Parathyroidectomy Incisions to Other Neck Surgeries
Understanding the size of incisions in parathyroidectomy can be easier when compared to other neck surgeries. This comparison helps patients grasp the relative size and impact of these incisions.
Thyroidectomy vs. Parathyroidectomy Incisions
Comparing parathyroidectomy to thyroidectomy incisions is common. Both surgeries are in the neck but target different glands. Thyroidectomy removes the thyroid gland, which is larger. So, thyroidectomy incisions are usually 3 to 5 cm.
On the other hand, parathyroidectomy incisions are smaller. They range from 2.5 to 3.5 cm. With minimally invasive techniques, they can be as small as 1.5 to 2 cm.
Lymph Node Dissection Incisions
Lymph node dissection removes neck lymph nodes, often for cancer treatment. The incision size varies with the extent of the dissection. Generally, lymph node dissection requires larger incisions than parathyroidectomy, sometimes several centimeters long.
Tracheostomy and Other Neck Procedure Comparisons
Tracheostomy creates an airway by making an incision in the trachea. The incision size is usually small, around 1 to 2 cm. Other neck procedures, like those for cysts or tumors, have varying incision sizes based on the lesion’s size and location.
When comparing these to parathyroidectomy, it’s clear that minimally invasive parathyroidectomy often results in smaller incisions than many other neck surgeries.
In conclusion, comparing parathyroidectomy incisions to other neck surgeries shows their relatively small size. This comparison can help ease concerns for patients considering surgery.
Recovery and Healing of Parathyroidectomy Incisions
Knowing what to expect after a parathyroidectomy can reduce anxiety. The healing of the incision site is key. Understanding this can help manage expectations and improve outcomes.
Immediate Post-Operative Appearance
Right after surgery, the incision will be swollen, bruised, and tender. This is normal. The incision is closed with sutures or staples, which are removed later. Keeping the area clean and dry is important to avoid infection.
Week-by-Week Healing Timeline
Healing times vary, but here’s a general outline:
- First Week: The incision is most sensitive. Swelling and bruising peak and then decrease.
- 2-4 Weeks: The incision starts to close, and swelling reduces. Patients can usually start normal activities.
- 6-12 Weeks: The scar fades and flattens. Following scar management techniques is important.
For more detailed information, patients can refer tothis guideon parathyroid surgery recovery.
Long-term Scar Appearance
The scar’s long-term look depends on skin type, incision size, and post-operative care. Scars from parathyroidectomy are usually minimal and fade. Scar management techniques can improve the scar’s look.
Scar Management Techniques
Effective scar management can improve the scar’s appearance. Techniques include:
- Massaging the scar gently
- Using silicone products
- Avoiding direct sun exposure
Patients should talk to their surgeon about these options.
Understanding the recovery and healing process helps patients prepare. While the initial stages may seem daunting, most patients recover well. Life expectancy after parathyroid surgery is generally not affected. Successful surgery can greatly improve the quality of life for those with parathyroid disease.
Potential Complications Related to Incision Size
While rare, complications from incision size in parathyroidectomy can happen. It’s important for patients to know about these risks. The size of the incision can affect the chance of problems after surgery.
Infection Risks and Prevention
Infection is a risk with any surgery, including parathyroidectomy. Proper wound care and post-operative follow-up are key to reduce this risk. We make sure the incision site is clean and teach patients how to keep it clean.
Nerve Injury Considerations
The parathyroid glands are close to important nerves in the neck. Nerve injury is a possible complication. We use careful techniques and monitoring during surgery to lower this risk. Patients should talk to their surgeon about their specific risks.
Hypertrophic Scarring and Keloids
Some people might get hypertrophic scarring or keloids. Advanced wound closure techniques and scar care after surgery can help. We help patients plan for scar management that fits their needs.
Reoperation Challenges
If a second surgery is needed, the first incision size and location matter. We plan and document the first surgery well for future operations. A detailed table outlining the considerations for reoperation is provided below:
|
Consideration |
Impact on Reoperation |
|---|---|
|
Initial Incision Size |
Affects the complexity of subsequent surgery |
|
Surgical Technique |
Influences the ease of reoperation |
|
Documentation |
Detailed records facilitate future surgeries |
Knowing about these possible complications and their link to incision size helps patients make better choices for their parathyroidectomy surgery.
Patient Experiences with Parathyroidectomy Incisions
People thinking about hyperparathyroidism treatment often find it helpful to hear from others who’ve had parathyroidectomy. These stories give insights into what to expect, like the size of the incision and how it affects recovery.
Common Patient Concerns
Patients usually worry about the incision size, how visible the scar will be, and the recovery time. They might think a bigger incision means more pain or a longer healing time. But, thanks to parathyroid surgery improvements, incisions are now smaller, easing these worries.
Satisfaction Rates with Cosmetic Outcomes
Research shows most patients are happy with how their parathyroidectomy scars look. The use of minimally invasive techniques has made scars less noticeable. Many say their scars are almost invisible once they’ve healed.
Tips from Former Patients
People who’ve had the surgery suggest talking openly with their surgeon about concerns. They recommend asking about the incision size, the surgery method, and what recovery will be like. Also, following post-op care instructions closely can help reduce scarring and make recovery smoother.
Learning from others can make prospective patients feel more ready for their parathyroid surgery. They’ll know what to expect and how to get the best results.
Technological Advances Reducing Parathyroidectomy Incision Size
Recent years have seen a big change in parathyroid surgery. New technologies have made surgery better and recovery faster. We’ll look at how these changes are making parathyroidectomy better.
High-Definition Imaging Systems
High-definition imaging has made parathyroid surgery more precise. These systems give surgeons a clear view of the area. This is key for minimally invasive parathyroidectomy, allowing for smaller cuts.
Specialized Surgical Instruments
New surgical tools have also helped reduce incision sizes. These tools are made for precise and less invasive surgery. They’re essential for minimally invasive parathyroidectomy techniques.
Intraoperative PTH Monitoring
Intraoperative parathyroid hormone (PTH) monitoring is a big advance. It lets surgeons check the surgery’s success in real-time. This helps confirm the surgery’s success, making smaller cuts possible.
Future Innovations on the Horizon
We’re expecting even more changes in parathyroid surgery. New technologies like better imaging and robotic surgery will help. These will likely lead to even smaller cuts and quicker recovery.
In conclusion, new technologies have greatly improved parathyroid surgery. They’ve made the surgery more effective and the recovery faster. As technology keeps improving, we’ll see even better minimally invasive parathyroidectomy techniques.
Choosing a Surgeon for Optimal Incision Results
When it comes to parathyroid surgery, your surgeon’s skill matters a lot. Picking the right surgeon is key for the best results, like smaller incisions and faster recovery.
Volume of Procedures Performed Annually
Look at how many parathyroid surgeries your surgeon does each year. Surgeons who do more often have better techniques. This can mean smaller cuts and fewer problems. Studies show high-volume surgeons get better results for their patients.
|
Annual Volume of Parathyroidectomies |
Average Incision Size |
Complication Rate |
|---|---|---|
|
Low (<10) |
3-4 cm |
5-7% |
|
Medium (10-50) |
2-3 cm |
2-4% |
|
High (>50) |
1-2 cm |
1-2% |
Questions to Ask About Surgical Approach
Ask your surgeon about their method for parathyroid surgery. Find out if they use small incisions, what anesthesia they use, and how they reduce scars and risks. Knowing this can make you feel more sure about your surgeon.
Finding Specialists in Minimally Invasive Techniques
Minimally invasive surgery can lead to smaller cuts and faster healing. Look for surgeons who are experts in these methods and have good results.
The Importance of a Dedicated Parathyroid Surgeon
A surgeon focused on parathyroid surgery has the right knowledge and experience. They are more likely to use the latest techniques. This means you get the best care possible.
Conclusion: Balancing Surgical Success with Cosmetic Outcomes
Parathyroidectomy has changed a lot. Now, doctors use new methods to make smaller cuts. This way, they can fix the problem without leaving big scars.
Patients can learn about these changes. They can understand how to pick the right surgeon. This helps them get the best results.
We talked about many things related to parathyroidectomy. This includes how doctors find the right spot to operate and how patients recover. The main aim is to cure the disease and keep the surgery looking good.
Choosing a skilled surgeon is key. They use the newest tools and methods. This means smaller cuts and better looks for patients.
Our conversation shows how important it is to think about looks and health together. This leads to happier patients and a better life for them.
FAQ
What is the typical incision size for a parathyroidectomy?
The size of the incision for a parathyroidectomy has gotten smaller. It now averages 2.5–3.5 cm. With new techniques, it can be as small as 15–20 mm.
What is parathyroidectomy surgery?
Parathyroidectomy surgery removes overactive parathyroid glands. This is often needed for hyperparathyroidism.
How long is the recovery time for parathyroid surgery?
Recovery times vary. But, minimally invasive methods usually lead to faster healing.
What are the risks and complications of parathyroidectomy?
Risks include infection, nerve injury, and scarring. Reoperation challenges are rare but possible.
How do pre-operative localization studies impact parathyroidectomy?
Studies like sestamibi scans help locate the problem gland. This allows for smaller incisions.
What is the difference between single gland and multiple gland disease in parathyroidectomy?
Most patients (80–85%) have one bad gland. This means smaller incisions are possible. But, if there are multiple glands, a bigger surgery might be needed.
What are the different surgical approaches to parathyroidectomy?
There are several ways to do the surgery. These include traditional neck exploration and minimally invasive methods. There are also endoscopic and video-assisted techniques, and radio-guided surgery.
How do technological advances impact parathyroidectomy incision size?
New imaging and tools help make the incision smaller. This includes high-definition systems and special instruments.
What should I expect before undergoing parathyroidectomy surgery?
Before surgery, you’ll have consultations and talks about the incision. You’ll also prepare for the big day.
How do I choose a surgeon for optimal parathyroidectomy results?
Look for a surgeon who does many of these surgeries. Ask about their methods and if they use the latest techniques.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/14557134/



































