
When people face chronic pain or serious injuries, they often look for a rehabilitation doctor, also known as a physiatrist. These doctors are key in helping patients get back their strength and mobility.
Finding your way through the healthcare system can be tough. But knowing what a physiatrist does can really help. They are trained to handle many conditions, from sports injuries to neurological problems, without surgery.
Physiatrists focus on physical medicine and rehabilitation (PM&R). They aim to help patients function at their best and live better lives. As we dive into physiatry, it’s clear these doctors are vital in healthcare.
Key Takeaways
- Physiatrists are medical doctors who specialize in physical medicine and rehabilitation.
- They diagnose and treat conditions without surgery, focusing on patient recovery and mobility.
- Physiatrists play a vital role in helping patients regain strength and improve their quality of life.
- Physical medicine and rehabilitation (PM&R) is a key part of healthcare.
- Physiatrists treat a wide range of conditions, from sports injuries to neurological disorders.
The Field of Rehabilitation Medicine
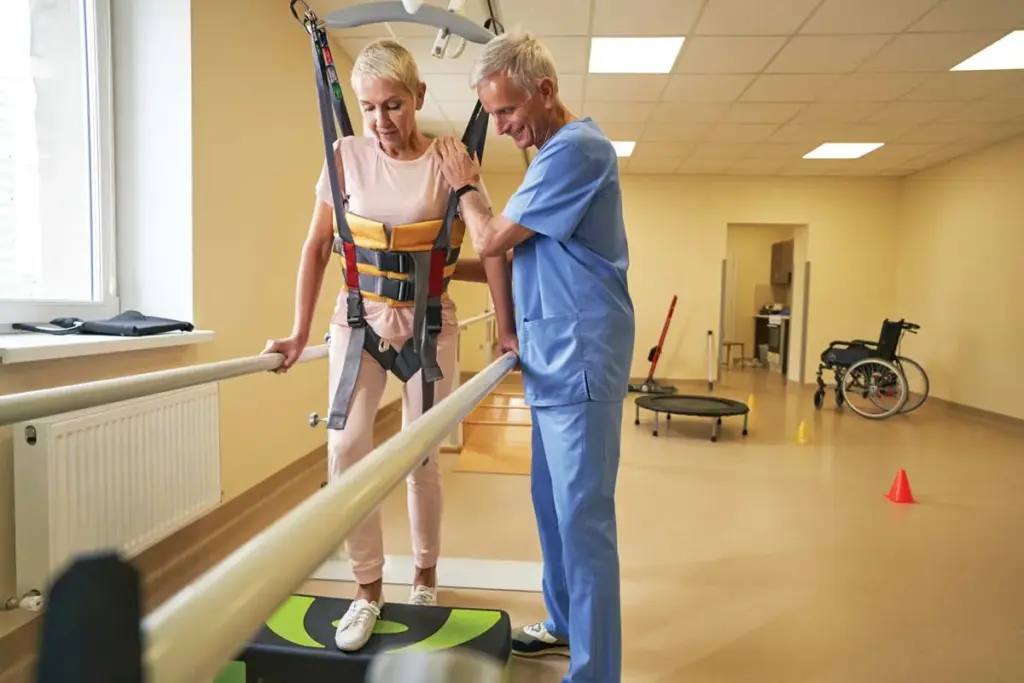
Healthcare is getting better, and so is the role of rehabilitation medicine. This field, also known as physical medicine and rehabilitation (PM&R), helps patients get better from injuries and manage long-term conditions. It also improves their quality of life.
Historical Development of Rehabilitation Medicine
Rehabilitation medicine has roots in ancient times. Back then, doctors used different methods to help patients regain strength and move better. But, it wasn’t until the early 20th century that it became a special field.
The two World Wars were key in its growth. The need to help wounded soldiers recover was huge. Thanks to medical tech and understanding of the body, the field has grown a lot.
Now, rehabilitation medicine offers many treatments for physical disabilities. Physiatrists, the doctors in this field, work with teams to make plans for each patient. They aim to help patients reach their goals.
The Growing Importance in Modern Healthcare
Rehabilitation medicine is very important today. With more older people and chronic conditions like stroke and spinal cord injuries, we need more help. It helps patients become independent again, feel less pain, and do daily tasks better.
Studies show that early rehabilitation helps a lot. Patients who get help early recover faster and don’t stay in the hospital as long. As healthcare keeps changing, rehabilitation medicine will grow. It will use new tech and ways to help patients.
What is a Physiatrist?
The term ‘physiatrist’ might be new to many, but they play a key role in rehabilitation medicine. A physiatrist, also known as a Physical Medicine and Rehabilitation (PM&R) doctor, helps patients regain function and improve their quality of life.
Definition and Core Focus
A physiatrist focuses on non-surgical treatments and rehabilitation. They manage medical conditions affecting the brain, spinal cord, nerves, bones, and more. Their goal is to help patients achieve maximum function and independence.
Physiatrists treat many conditions, including chronic pain and musculoskeletal injuries. They create personalized treatment plans that may include physical therapy and other non-surgical interventions.
The Etymology of “Physiatrist”
The term “physiatrist” comes from Physical Medicine and Rehabilitation (PM&R). It combines “physikos,” meaning natural, and “iatros,” meaning healer or physician. So, a physiatrist is a natural healer who focuses on non-surgical treatments.
“Physiatrists are the unsung heroes of the medical world, helping patients navigate the complexities of rehabilitation and regain their independence.”
Common Misconceptions About Physiatrists
Many think physiatrists are just sports medicine doctors or physical therapists. But their scope is much broader. They treat sports injuries and complex medical conditions with a holistic approach.
|
Misconception |
Reality |
|---|---|
|
Physiatrists only treat sports injuries. |
They treat a wide range of conditions, including chronic pain, musculoskeletal injuries, and neurological disorders. |
|
Physiatrists are the same as physical therapists. |
Physiatrists are medical doctors who design treatment plans, while physical therapists implement these plans under the physiatrist’s supervision. |
|
Physiatrists only work in rehabilitation centers. |
They work in various settings, including hospitals, outpatient clinics, and sports medicine centers. |
Understanding physiatrists’ role and expertise helps us see the care they provide. Their focus on non-surgical treatments and rehabilitation makes them vital in healthcare.
Physical Medicine and Rehabilitation (PM&R) Explained
Physical Medicine and Rehabilitation (PM&R) is a wide field. It aims to help patients with physical disabilities. It focuses on improving their quality of life and restoring function.
Understanding the PM&R Medical Abbreviation
PM&R stands for Physical Medicine and Rehabilitation. It’s a medical field that treats disorders affecting muscles, nerves, and more. “Physical Medicine” uses treatments like heat and exercise. “Rehabilitation” helps patients regain their independence.
Scope of Physical Medicine
Physical Medicine in PM&R treats pain and improves mobility. It includes:
- Exercise and physical therapy
- Assistive devices and adaptive equipment
- Modalities like ultrasound and electrical stimulation
- Manual therapy, including massage
The Rehabilitation Component Defined
The rehabilitation part of PM&R aims to help patients reach their full ability. It involves:
|
Rehabilitation Aspect |
Description |
|---|---|
|
Functional Goal Setting |
Setting specific goals based on the patient’s needs and abilities. |
|
Interdisciplinary Team Leadership |
Working with a team of healthcare professionals for complete care. |
|
Assistive Technology and Devices |
Using technology and devices to help patients live independently. |
Understanding PM&R helps patients see the full care they receive. This field is key in recovery, managing chronic conditions, and improving physical function.
The Educational Path to Becoming a Physiatrist
Becoming a physiatrist takes a lot of education and training. We’ll cover the main steps, from medical school to getting certified.
Medical School Requirements
The journey to becoming a physiatrist begins with medical school. You need a Doctor of Medicine (M.D.) or Doctor of Osteopathic Medicine (D.O.) degree. This takes four years and includes classes and clinical work.
It’s good to take PM&R electives or internships in medical school. This helps you understand the field better. You’ll learn about treating chronic pain and musculoskeletal disorders.
Residency and Fellowship Training
After medical school, you need a PM&R residency, which lasts four years. You’ll work with experienced physiatrists. This training covers inpatient and outpatient settings.
Some physiatrists do fellowships for one to two years. These focus on areas like sports medicine and pediatric rehabilitation. It’s a chance to specialize further.
Board Certification Process
To get certified, you must pass the ABPMR exam. It tests your knowledge and skills in PM&R. Getting certified shows you’re committed to the field.
To keep your certification, you need to keep learning. You must do CME courses and follow ABPMR rules. This keeps you up-to-date with PM&R advancements.
Becoming a physiatrist is a long and hard journey. But for those who want to help patients, it’s a fulfilling career.
How Physiatrists Differ from Other Medical Specialists
Physiatrists are known for their focus on non-surgical treatments and helping patients regain function. It’s important for patients to know these differences to get the right care.
Comparison with Orthopedic Surgeons
Physiatrists and orthopedic surgeons both treat musculoskeletal issues. But they use different methods. Orthopedic surgeons often perform surgery. On the other hand, physiatrists use non-surgical treatments like medicine and physical therapy to help patients.
Comparison with Neurologists
Neurologists and physiatrists both deal with nervous system issues. But they focus on different things. Neurologists mainly use medicine to diagnose and treat. Physiatrists, on the other hand, focus on helping patients regain lost abilities through rehabilitation.
Comparison with Pain Management Specialists
Pain management specialists and physiatrists both treat chronic pain. But physiatrists look at the bigger picture. They use physical medicine and rehabilitation techniques to manage pain and improve function.
The Unique Value of Physiatry
Physiatry offers a unique approach to patient care. Physiatrists look at the whole person, not just the injury. This way, they can provide personalized care that improves rehabilitation and outcomes.
The Physiatrist’s Approach to Patient Care
Physiatry puts the patient first, focusing on their overall well-being. This is key for physiatrists, who aim to meet all their patients’ needs. They provide care that covers everything from physical health to emotional support.
Whole-Person Treatment Philosophy
Physiatrists look at patients as more than just their physical health. They consider their emotional and social well-being too. This way, they create care plans that improve patients’ lives in many ways.
By treating the whole person, physiatrists tackle the real causes of health issues. They don’t just treat symptoms. This approach helps patients live better lives.
Functional Goal Setting
Setting functional goals is a big part of what physiatrists do. They work with patients to set achievable goals. This helps patients improve their function and independence.
This teamwork makes sure treatment plans meet patients’ needs. It also gives patients a sense of control over their care.
Interdisciplinary Team Leadership
Physiatrists often lead teams of healthcare experts. They work together to give patients the best care. This team includes physical therapists, occupational therapists, and more.
Physiatrists lead these teams to make care smooth and effective. They use their knowledge to create care plans that focus on the patient. This teamwork improves patient outcomes.
Common Conditions Treated by Physiatry Specialists
Physiatry specialists deal with many medical conditions. They help with neurological disorders, musculoskeletal injuries, and post-surgical needs. They know how to diagnose and treat conditions affecting the brain, spinal cord, nerves, and more.
Neurological Conditions
Physiatrists handle various neurological issues. These include:
- Stroke and cerebral palsy
- Spinal cord injuries and disorders
- Multiple sclerosis and other demyelinating diseases
- Parkinson’s disease and other movement disorders
They create treatment plans that might include medicine, physical therapy, and changes in lifestyle.
Musculoskeletal Disorders
Musculoskeletal disorders are a big part of what physiatrists do. They treat conditions like:
- Back pain and sciatica
- Arthritis and other degenerative joint diseases
- Tendinitis and bursitis
- Fibromyalgia and other chronic pain syndromes
They use physical therapy, medicine, and sometimes interventional procedures to treat these conditions.
Sports Injuries
Sports injuries are a big part of physiatry. They include:
- Muscle strains and ligament sprains
- Tendon ruptures and other acute injuries
- Overuse injuries, such as tendinitis
- Concussions and other traumatic brain injuries
Physiatrists help athletes get back to sports safely with rehabilitation plans.
Post-Surgical Rehabilitation
After surgery, patients need to get strong and mobile again. Physiatrists lead the team in:
- Creating personalized rehabilitation plans
- Coordinating physical and occupational therapy
- Managing pain and other post-surgical symptoms
- Optimizing recovery and outcomes
By focusing on functional goals, physiatrists help patients get the best results after surgery.
Diagnostic Methods Used by PM&R Doctors
Physiatrists use many specialized methods to diagnose and treat patients. These methods help us understand a patient’s condition fully.
Physical Examination Techniques
A thorough physical exam is key in PM&R. We check muscle strength, reflexes, and range of motion. Manual muscle testing and reflex assessments are used to evaluate these areas.
We also look at posture, gait, and movement patterns. This helps us spot issues and plan treatment.
Electrodiagnostic Studies
Electrodiagnostic studies are vital in PM&R. Electromyography (EMG) and nerve conduction studies (NCS) are used. EMG checks muscle electrical activity, while NCS looks at nerve signals.
These studies help diagnose nerve damage and muscle diseases. They guide us in creating effective treatment plans.
Imaging and Other Diagnostic Tools
We also use imaging like X-rays, MRI, and CT scans. These tools show us internal structures. This helps us understand bone, muscle, and nerve anatomy.
Diagnostic injections and lab tests are used too. For example, injections can pinpoint pain sources.
|
Diagnostic Tool |
Description |
Common Uses |
|---|---|---|
|
EMG |
Measures electrical activity of muscles |
Diagnosing muscle damage, radiculopathy |
|
NCS |
Assesses nerve conduction speed and strength |
Diagnosing nerve damage, neuropathy |
|
MRI |
Provides detailed images of soft tissues |
Diagnosing musculoskeletal and neurological conditions |
The American Academy of Physical Medicine and Rehabilitation highlights the importance of electrodiagnostic medicine. It’s a key part of a physiatrist’s diagnostic tools.
Non-Surgical Treatment Options in Physical Medicine
In physical medicine, non-surgical treatments are key for recovery and managing chronic conditions. Physical medicine and rehabilitation (PM&R) focus on improving function and quality of life without surgery.
Exercise Prescription
Exercise prescription is a main tool for physiatrists. It tailors exercise to each patient’s needs. This helps improve strength, flexibility, and endurance.
Benefits of Exercise Prescription:
- Improved muscle strength and flexibility
- Enhanced cardiovascular health
- Better management of chronic conditions
- Reduced risk of future injuries
Physical and Occupational Therapy
Physical and occupational therapy are key in non-surgical treatments. Physical therapy helps regain mobility and strength. Occupational therapy helps with daily activities and returning to routines.
“Therapy is not just about recovery; it’s about empowering patients to take control of their health and well-being.” – A Physiatrist’s Perspective
Key Aspects of Physical and Occupational Therapy:
|
Therapy Type |
Focus |
Goals |
|---|---|---|
|
Physical Therapy |
Regaining mobility and strength |
Improved physical function |
|
Occupational Therapy |
Performing daily activities |
Independence in daily living |
Assistive Devices and Adaptive Equipment
Assistive devices and adaptive equipment help patients with disabilities or impairments. They make daily life easier. From wheelchairs to specialized utensils, these tools enhance independence and participation in activities.
Lifestyle Modifications
Lifestyle modifications are critical in non-surgical treatment. Making changes to diet, exercise, and lifestyle can improve health and reduce chronic disease risk.
Examples of Lifestyle Modifications:
- Adopting a balanced diet rich in nutrients
- Engaging in regular physical activity
- Managing stress through mindfulness or meditation
- Getting adequate sleep
By using these non-surgical treatments, we offer patients care that meets their needs. This promotes optimal recovery and function.
Interventional Procedures Performed by Physiatrists
Physiatrists are experts in physical medicine and rehabilitation. They use interventional procedures to help patients. These methods are key for managing musculoskeletal disorders and neurological injuries.
Joint Injections
Physiatrists often use joint injections to ease pain and swelling. These injections contain corticosteroids or hyaluronic acid. They help reduce swelling and improve joint lubrication.
For example, someone with severe osteoarthritis can get hyaluronic acid injections. This can help them move their joints better and feel less pain.
Spinal Interventions
Spinal interventions, like epidural steroid injections, are used to manage spinal pain. They are helpful for those with herniated discs, spinal stenosis, or facet joint syndrome. By targeting the pain area, physiatrists can lessen pain and aid in recovery.
Regenerative Medicine Techniques
Physiatrists are using regenerative medicine, like platelet-rich plasma (PRP) therapy and stem cell therapy. PRP therapy uses the patient’s own blood to stimulate healing. It’s promising for treating tendon injuries, osteoarthritis, and ligament sprains.
Ultrasound-Guided Procedures
Ultrasound guidance has changed interventional procedures. It lets physiatrists see the target area live. This makes injections more accurate and safer.
Ultrasound-guided procedures are great for reaching small or hard-to-access areas. This includes tendons and nerves.
Interventional procedures are a big part of physiatric practice. They offer effective treatments for many conditions. By combining these with other rehabilitation methods, physiatrists help patients achieve better outcomes and quality of life.
Pain Management Approaches in Physiatry
Pain management in physiatry is complex. We use many treatments together to tackle pain’s many sides. Our goal is to help patients feel better and live better lives.
Acute vs. Chronic Pain Treatment
Knowing the difference between acute and chronic pain is key. Acute pain comes from injuries or surgery and goes away when the injury heals. Chronic pain lasts longer and needs a detailed plan to manage.
We adjust our treatment based on the patient’s pain type. For acute pain, we focus on healing and easing discomfort. For chronic pain, we use a mix of treatments to manage pain and improve function.
Multimodal Pain Management
Multimodal pain management uses different treatments together for best results. This might include medications, physical therapy, interventional procedures, and lifestyle changes. By attacking pain from many sides, we often get better results than with one treatment alone.
|
Treatment Modality |
Description |
Benefits |
|---|---|---|
|
Medications |
Pharmacological interventions to manage pain |
Rapid pain relief, can be tailored to specific pain types |
|
Physical Therapy |
Exercise and physical modalities to improve function and reduce pain |
Improves strength, flexibility, and functional ability |
|
Interventional Procedures |
Minimally invasive procedures to target pain sources |
Provides targeted pain relief with minimal recovery time |
|
Lifestyle Modifications |
Changes in daily habits to reduce pain and improve health |
Promotes long-term health and pain management |
Alternatives to Opioid Medications
We’re now using non-opioid alternatives for pain management more. This includes NSAIDs, anticonvulsants, and antidepressants. These options help manage pain without the risk of opioid addiction.
Psychological Aspects of Pain Treatment
The mind plays a big role in pain treatment. Chronic pain can hurt mental health, leading to depression and anxiety. We use cognitive-behavioral therapy (CBT) and other psychological interventions to help patients cope and feel better.
By adding psychological support to our care, we offer a more complete approach. We address both the physical and emotional sides of pain.
Rehabilitation Settings Where Physiatrists Practice
Physiatrists work in many places, from inpatient facilities to sports medicine centers. They use their skills to help patients in different ways.
Inpatient Rehabilitation Facilities
In these facilities, patients get a lot of therapy and medical care. They might have had big injuries or illnesses, like strokes or spinal cord injuries. Physiatrists lead teams here to help patients get better and be independent again.
Outpatient Clinics
Outpatient clinics are for patients who need to keep getting better but don’t need to stay in the hospital. Physiatrists here treat many conditions, like muscle or nerve problems. They use therapy, medicine, and lifestyle changes to help.
Acute Care Hospitals
In acute care hospitals, physiatrists are key in the beginning of patient care. They work with patients who have had big injuries or complex surgeries. They manage pain, prevent problems, and help patients move early to get better faster.
Sports Medicine Centers
Sports medicine centers focus on athletes and active people with sports injuries. Physiatrists here use treatments like injections and physical therapy. They aim to get patients back to their activities safely and quickly.
|
Rehabilitation Setting |
Patient Needs |
Physiatrist’s Role |
|---|---|---|
|
Inpatient Rehabilitation Facilities |
Intensive therapy and medical care for significant injuries or illnesses |
Lead interdisciplinary teams to achieve functional independence |
|
Outpatient Clinics |
Ongoing rehabilitation for less severe conditions |
Diagnose and treat conditions using a combination of therapies |
|
Acute Care Hospitals |
Early stage care for traumatic injuries or post-surgery recovery |
Manage pain, prevent complications, and facilitate early mobilization |
|
Sports Medicine Centers |
Treatment for sports-related injuries |
Use various treatments to help patients return to activities quickly and safely |
Physiatrists work in many places to meet different patient needs. They help with everything from intense rehab to managing chronic conditions and treating sports injuries.
Subspecialties Within Physical Medicine and Rehabilitation
PM&R is not a one-size-fits-all field; it includes several subspecialties. These allow physiatrists to provide targeted care to patients with diverse needs. Healthcare providers can focus on specific areas, improving patient outcomes with specialized treatment.
Sports Medicine
Sports medicine focuses on treating sports-related injuries. Physiatrists in this field help athletes recover from injuries. They use non-surgical treatments like physical therapy and medication for injuries such as tendonitis and muscle strains.
Spinal Cord Injury Medicine
Spinal cord injury medicine addresses the complex needs of individuals with spinal cord injuries. Physiatrists manage acute and chronic conditions, promoting functional independence. They use rehabilitation therapies, pain management, and assistive devices to improve quality of life.
Brain Injury Rehabilitation
Brain injury rehabilitation focuses on patients with traumatic brain injuries or other brain damage. Physiatrists develop rehabilitation plans that include cognitive therapy and medication management. These plans help patients regain lost functions and adapt to their condition.
Pediatric Rehabilitation
Pediatric rehabilitation helps children with disabilities or injuries achieve their full potentials. Physiatrists work with children who have conditions like cerebral palsy. They create individualized treatment plans that include physical, occupational, and speech therapy to support development and functional abilities.
The subspecialties within PM&R show the field’s versatility. By focusing on specific areas, physiatrists can deliver specialized care. This improves patient outcomes.
Patient Success Stories: The Impact of Physiatric Care
At the heart of physiatric care are the inspiring stories of patients who have overcome significant health challenges. These stories not only highlight the expertise of physiatrists but also underscore the compassionate care provided.
Recovery from Traumatic Injuries
Many patients who suffer traumatic injuries benefit greatly from physiatric care. For example, a young athlete with a severe spinal cord injury regained mobility and independence. The road to recovery was long and challenging, but with the right care, the patient was able to return to competitive sports.
Managing Chronic Conditions
Physiatrists also play a key role in managing chronic conditions. For instance, a patient with chronic back pain saw a significant reduction in pain. This holistic approach to care improved the patient’s quality of life.
- Personalized treatment plans
- Multidisciplinary care teams
- Advanced interventional procedures
Returning to Sports and Activities
For many patients, the goal of physiatric care is not just recovery but also returning to their favorite sports and activities. Through sports medicine programs, physiatrists help athletes regain their strength and performance. A notable example is a professional football player who, after undergoing treatment for a career-threatening injury, was able to return to the field.
These success stories illustrate the profound impact of physiatric care on patients’ lives. They enable patients to recover, adapt, and thrive despite significant health challenges.
When to See a PM&R Doctor
Knowing when to see a Physical Medicine and Rehabilitation (PM&R) doctor is key to your recovery. PM&R doctors, or physiatrists, help patients with chronic pain and musculoskeletal disorders. They guide you on when it’s time to see one.
Common Referral Reasons
People often see PM&R doctors for chronic pain, musculoskeletal injuries, and more. For example, if you have back pain that won’t go away, they can help.
Self-Referral vs. Physician Referral
You can see a PM&R doctor on your own in many cases. But, some insurance plans need a referral. Always check your insurance first.
Knowing your insurance coverage is important. Here’s a quick guide:
What to Expect at Your First Appointment
At your first visit, the doctor will check you thoroughly. They’ll look at your medical history and develop a treatment plan. This plan might include physical therapy or medication.
Insurance Coverage and Accessibility
Insurance for PM&R services can differ a lot. Make sure you know what your insurance covers before you go. Many clinics also offer flexible hours and help for those without insurance.
Conclusion: The Vital Role of Physiatrists in Healthcare
Physiatrists are key players in healthcare, focusing on helping patients get better. They use their knowledge of physical medicine and rehabilitation. This helps people regain their abilities and live better lives.
Physiatrists use non-surgical treatments and procedures to care for patients. They work in many places, from hospitals to clinics. This shows their flexibility and dedication to helping others.
As healthcare changes, physiatrists’ role stays the same. We see how important they are in giving top-notch care. They meet the complex needs of people with physical disabilities or chronic conditions.
FAQ
What is a physiatrist, and what do they do?
A physiatrist is a doctor who specializes in physical medicine and rehabilitation (PM&R). They help patients recover from injuries or illnesses. They also work to improve patients’ ability to function.
What is the difference between a physiatrist and an orthopedic surgeon?
A physiatrist focuses on non-surgical treatments like physical therapy and medications. Orthopedic surgeons often perform surgery. Both treat musculoskeletal conditions but in different ways.
What is physical medicine and rehabilitation (PM&R)?
PM&R is a medical field that helps patients with physical disabilities. It includes treatments like physical therapy and pain management. The goal is to improve patients’ quality of life.
What conditions do physiatrists typically treat?
Physiatrists treat many conditions, like neurological disorders and musculoskeletal injuries. They also help with chronic pain and injuries to the brain and spinal cord.
Do I need a referral to see a physiatrist?
Usually, you don’t need a referral to see a physiatrist. But, it’s good to check with your insurance first.
What can I expect during my first appointment with a physiatrist?
At your first visit, the physiatrist will take your medical history and do a physical exam. They might also order tests. Then, they’ll create a treatment plan just for you.
What is the role of a physiatrist in pain management?
Physiatrists are key in pain management. They use treatments like medications and alternative therapies. This helps patients with both acute and chronic pain.
Can physiatrists perform surgery?
Some physiatrists can do certain procedures, like joint injections. But, they usually don’t do surgery. Their main focus is on non-surgical treatments and rehabilitation.
How do I find a qualified physiatrist?
To find a good physiatrist, ask your doctor for a referral. You can also check with your insurance or search online for board-certified physiatrists in your area.
What is the difference between a physiatrist and a pain management specialist?
Physiatrists and pain management specialists both treat pain. But, physiatrists look at the whole person. They find the cause of pain and create treatment plans that use many therapies.
Can physiatrists help with rehabilitation after surgery?
Yes, physiatrists are important in post-surgical care. They help patients recover, manage pain, and regain their abilities.
Are physiatrists qualified to treat sports injuries?
Yes, many physiatrists are trained in sports medicine. They can treat sports injuries, including muscle and bone problems and concussions.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC3309231/



































