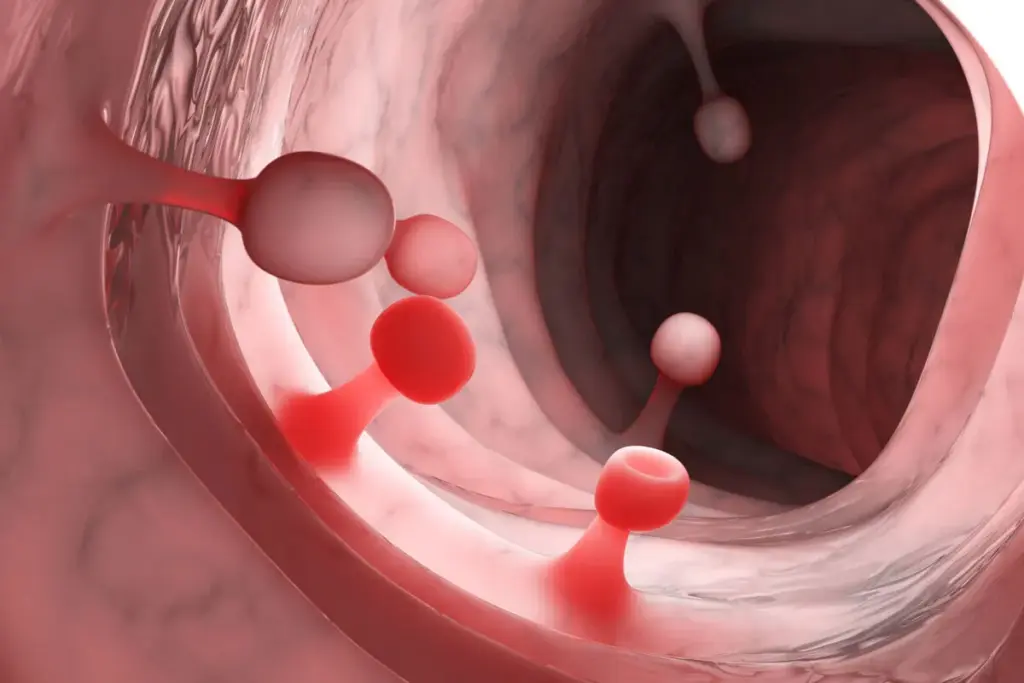
During a colonoscopy, finding colon polyps is key to knowing your colorectal cancer risk. Studies show that more than 10 polyps raise this risk a lot. This changes how doctors watch for and treat patients worldwide. How many polypsa are scary? Learn amazing facts about counts and find powerful ways to manage your vital and essential colorectal health.
Having 5-10 polyps in colon under 10 mm means you need to see your doctor more often. But, the link between colorectal polyps and cancer risk is more complicated.
It’s important to understand this link. It helps decide how often you should see your doctor. This can lower your chance of getting colorectal cancer in the future.
Key Takeaways
- The number of polyps found during colonoscopy is a key risk factor for future colorectal cancer.
- Having more than 10 polyps dramatically increases the risk of colorectal cancer.
- Current guidelines recommend more frequent surveillance for individuals with 5-10 polyps under 10 mm.
- The risk of colorectal cancer is directly related to the number of colon polyps detected.
- Understanding the connection between polyps and cancer risk is vital for effective care.
What Are Colorectal Polyps and Why Do They Form?
Colorectal polyps are growths on the colon or rectum lining. They are important to find early. Knowing about them helps us understand their role in health.
Definition and Common Characteristics of Polyps
Colorectal polyps are abnormal growths on the colon or rectum lining. They can be benign, meaning they won’t turn into cancer, or precancerous, which means they might. Most polyps are benign, but some types, like adenomatous polyps, are more likely to become cancerous.
Polyps can be pedunculated (with a stalk) or sessile (flat). Their size and shape also matter in determining their cancer risk.
How Polyps Develop in the Colon
Polyps form from abnormal cell growth in the colon lining. This growth can turn into a polyp over time. Adenomatous polyps, for example, start in the colon’s glandular epithelium and can turn into cancer.
Risk Factors for Polyp Formation
Many things can increase the chance of getting colorectal polyps. These include getting older, having a family history of polyps or cancer, and having inflammatory bowel disease. Eating a lot of red meat, not exercising, being overweight, and smoking also raise the risk.
Knowing these risk factors helps us figure out who might get polyps. It also helps us take steps to prevent them.
The Critical Connection Between Polyps and Colorectal Cancer
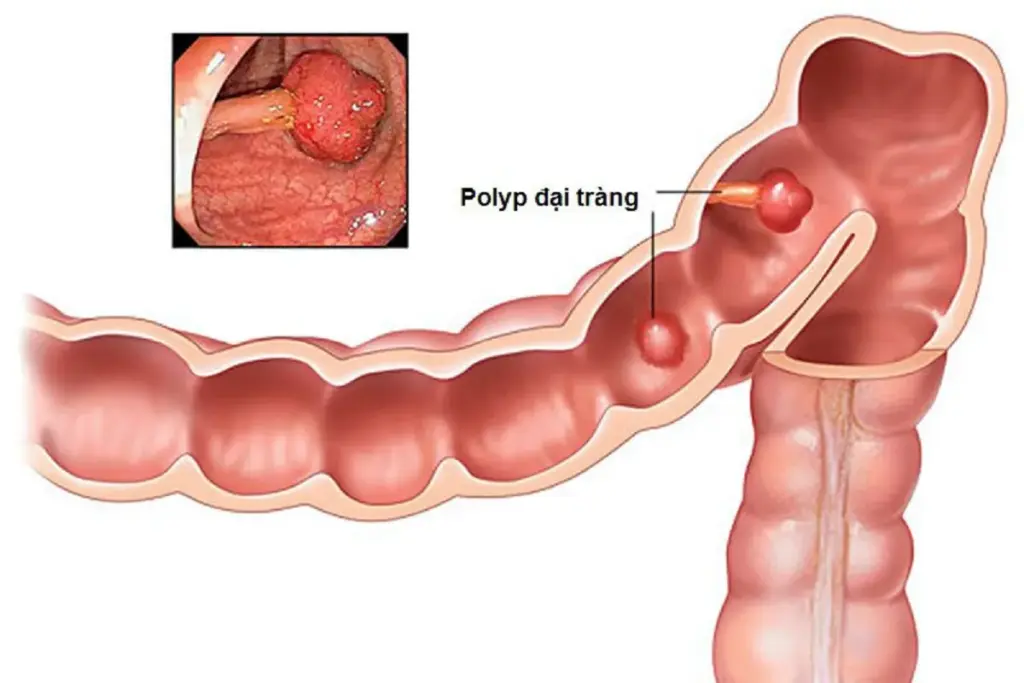
Colorectal polyps can lead to colorectal cancer. It’s important to understand this link. The relationship between polyps and cancer is complex, with many factors at play.
The Adenoma-Carcinoma Sequence
The adenoma-carcinoma sequence shows how benign polyps can turn into cancer. This happens through genetic changes that disrupt normal cell function. These changes lead to cancer.
Key stages in the adenoma-carcinoma sequence include:
- The formation of adenomatous polyps, which are considered precancerous lesions.
- The accumulation of genetic mutations within these polyps, leading to dysplasia.
- The progression from low-grade to high-grade dysplasia, indicating an increasing risk of cancer.
- The eventual invasion of cancer cells through the muscularis mucosa, marking the transition to invasive carcinoma.
Transformation Timeline: How Long It Takes for Polyps to Become Cancerous
The time it takes for a polyp to turn cancerous varies. Studies show it can take 10 to 15 years or more. This time can change based on the polyp type and patient factors.
Not All Polyps Are Created Equal: Benign vs. Precancerous
It’s key to tell benign from precancerous polyps. Benign polyps, like hyperplastic ones, usually don’t turn cancerous. But adenomatous polyps are precancerous and need to be removed.
The size, shape, and type of polyp affect its cancer risk. For example, sessile serrated polyps are more likely to have cancer or turn into it.
Why Polyp Count Matters in Your Colonoscopy Report
The number of colon polyps found during a colonoscopy is key to knowing your risk of colorectal cancer. This info is important for both patients and doctors. It helps decide how often you should have another colonoscopy.
Single vs. Multiple Polyps: Risk Stratification
Having more than one polyp raises your risk of colorectal cancer. Risk stratification based on polyp count helps doctors sort patients into risk groups. This guides how they should be managed.
- Patients with 1-2 small polyps are generally considered low-risk.
- Those with 3-4 polyps or larger polyps may be classified as intermediate-risk.
- Individuals with 5 or more polyps are often considered high-risk.
The Significance of Polyp Burden on Future Cancer Risk
The total burden of polyps, including their number, size, and characteristics, directly impacts the risk of developing colorectal cancer. Studies have shown that a higher polyp count is associated with an increased risk of cancer. For instance, having more than 10 polyps significantly elevates this risk.
How Doctors Use Polyp Count in Clinical Decision-Making
Doctors use the polyp count, along with other factors like polyp size and histology, to determine the appropriate surveillance interval for the next colonoscopy. For example:
- Patients with 1-2 small (less than 10mm or 0.4 inches) tubular adenomas typically require a follow-up colonoscopy in 5-10 years.
- Those with 3-4 adenomas or larger polyps may need a follow-up in 3 years.
- Individuals with 5 or more adenomas, or very large adenomas (> 20mm or 0.8 inches), usually require a follow-up in 1 year.
By understanding the significance of polyp count, patients can better appreciate the importance of adhering to the recommended follow-up schedule. This helps reduce their risk of colorectal cancer.
Clinical Guidelines on Polyp Quantity: The Numbers That Matter
Knowing about polyp quantity guidelines is key for patients after a colonoscopy. These rules help doctors figure out cancer risk and suggest next steps.
Low-Risk Category: 1-4 Small Polyps
Patients with 1-4 small polyps are usually at low risk. Small polyps are under 10 mm. The chance of these polyps being cancerous is low. Yet, it’s vital to stick to follow-up plans to watch for any changes.
Intermediate Risk: 5-10 Polyps Under 10mm
Having 5-10 polyps under 10 mm puts a person in the intermediate risk group. This means there’s a moderate chance of colorectal cancer. Regular monitoring is key to stop cancer from developing.
High-Risk Category: More Than 10 Polyps
More than 10 polyps raise the risk of colorectal cancer a lot. People in this group need more frequent checks and might need stronger treatments. Many polyps could mean a genetic condition like polyposis colon diseases.
The size and type of polyps also matter. For example, polyps over 4 cm (about 1.6 inches) are big and risky, no matter the number.
Understanding these guidelines helps patients grasp their risk better. They can then work with their doctors to manage their health well.
Size and Morphology: Beyond Just Counting Polyps
Polyp size and shape matter more than just how many there are. They help figure out cancer risk. We look at their size, shape, and type to understand the risk.
Small Polyps (Less Than 10mm): Are They Significant?
Small polyps, under 10mm, are seen as less risky. But, we shouldn’t ignore them. Even small ones can have high-grade dysplasia. They need to be watched closely.
Medium Polyps (10-20mm or 0.4-0.8 inches)
Medium polyps, 10mm to 20mm, have a moderate risk. They are bigger than small ones and need to be removed. This helps prevent cancer.
Large Polyps (Greater Than 20mm or 0.8 inches)
Large polyps, over 20mm, are risky and might have cancer. They are hard to remove and can cause problems. Endoscopic removal is used for these big polyps.
Sessile Polyps vs. Pedunculated Polyps: Shape Matters
Polyp shape affects their cancer risk. Sessile polyps are flat and hard to spot and remove. Pedunculated polyps have a stalk and are easier to manage.
|
Polyp Characteristic |
Cancer Risk |
Clinical Management |
|---|---|---|
|
Small ( |
Low |
Monitoring |
|
Medium (10-20mm) |
Moderate |
Removal recommended |
|
Large (>20mm) |
High |
Endoscopic removal |
|
Sessile |
Higher due to difficulty in detection |
Advanced endoscopic techniques |
|
Pedunculated |
Variable |
Standard endoscopic removal |
Types of Polyps and Their Varying Cancer Risk
Polyps come in different types, each with its own risk of becoming cancerous. Knowing these differences helps us understand their risks and how to handle them.
Adenomatous Polyps: The Precancerous Kind
Adenomatous polyps, or adenomas, are precancerous. They are common in the colon and can turn into colorectal cancer if not removed. The chance of an adenomatous polyp becoming cancerous depends on its size, type, and how abnormal it is.
Key characteristics of adenomatous polyps include:
- Potential to become malignant
- Variability in size and histology
- Presence of dysplasia, which can range from low-grade to high-grade
Serrated Polyps: The Often-Missed Danger
Serrated polyps are also precancerous but harder to spot during a colonoscopy because they are flat. They can be split into hyperplastic polyps, sessile serrated lesions, and traditional serrated adenomas. Some, like sessile serrated lesions, have a higher risk of turning into colorectal cancer.
The importance of serrated polyps is their risk of being missed and their varying cancer risk.
Hyperplastic and Other Benign Polyps: When Not to Worry
Hyperplastic polyps are usually harmless and found in the lower colon and rectum. They are small and rarely turn into cancer. Other benign polyps include inflammatory and hamartomatous polyps. While they are not precancerous, they might signal other health issues that need attention.
It’s vital to know the differences between polyp types to understand their importance and how to manage them.
The Importance of Polyp Location in the Colon
The location of polyps in the colon is key to finding them and understanding their cancer risk. Knowing about polyp location helps us manage colorectal health better.
Polyps in the Cecum and Right Colon: Higher Miss Rates
Polyps in the cecum and right colon are tricky to spot. Their location, with larger diameter and more fluid, makes them harder to see during a colonoscopy. Studies show that polyps in these areas are missed more often than others.
They can be hidden behind folds or in hard spots, making them tough to find. A gastroenterologist, says, “We must be extra careful in the cecum and right colon. Missing polyps here can have serious consequences for patients.”
Left-Sided Colorectal Polyps: Different Biology, Different Risks
Polyps on the left side of the colon are different. They are often easier to find during a colonoscopy because of the narrower left colon. But, left-sided polyps can be more aggressive and carry a higher cancer risk.
It’s important to understand these differences for better care. As we learn more about colorectal polyps, knowing where they are will keep being a big part of patient care.
Surveillance Intervals Based on Your Polyp Count
The number and type of polyps found during a colonoscopy affect how often you should get checked again. Knowing these guidelines helps you plan your next colonoscopy.
Normal Follow-up: When You Have 0-4 Small Polyps
If you have 0-4 small polyps, usually under 10mm, you should get checked again in 5-10 years. This is because these polyps are less likely to be cancerous.
3-Year Follow-up: The 5-10 Polyp Protocol
Those with 5-10 polyps, all under 10mm, should get checked again in 3 years. This is because more polyps mean a higher risk of cancer.
1-Year Follow-up: When You Have More Than 10 Polyps
If you have more than 10 polyps, you need to get checked again within 1 year. This is because a lot of polyps mean a higher risk.
Sticking to these follow-up times is key to catching cancer early. Regular check-ups help spot new polyps or changes in old ones, so you can act fast.
Knowing your polyp count and the risks it brings helps you plan your care. This way, you can stay on top of your colon health.
Multiple Polyps and Hereditary Syndromes: When Genetics Play a Role
Genetics are key in the growth of many colorectal polyps. This often points to hereditary syndromes. Some conditions raise the risk of colorectal cancer and polyp growth. Knowing these conditions helps find and manage those at high risk.
Familial Adenomatous Polyposis (FAP)
Familial Adenomatous Polyposis (FAP) is a rare genetic disorder. It causes hundreds to thousands of polyps in the colon and rectum. Without treatment, people with FAP face a nearly 100% chance of colorectal cancer by age 40. It’s caused by APC gene mutations.
Key Features of FAP:
- Multiple polyps (often hundreds or thousands)
- Early onset (often in teenage years)
- High risk of colorectal cancer if untreated
- Genetic testing available for APC gene mutations
Lynch Syndrome
Lynch syndrome, also known as Hereditary Nonpolyposis Colorectal Cancer (HNPCC), raises the risk of colorectal cancer. It’s different from FAP because it doesn’t cause many polyps. Instead, it increases the risk of colorectal, endometrial, ovarian, and other cancers.
Key Features of Lynch Syndrome:
- Fewer polyps compared to FAP
- Increased risk of colorectal, endometrial, ovarian, and other cancers
- Caused by mutations in DNA mismatch repair genes (MLH1, MSH2, MSH6, PMS2)
- Genetic testing available
Other Hereditary Polyposis Colon Diseases
There are other rare syndromes linked to colorectal polyps and cancer, aside from FAP. These include:
|
Syndrome |
Characteristics |
Genetic Cause |
|---|---|---|
|
Attenuated Familial Adenomatous Polyposis (AFAP) |
Fewer polyps than FAP, later onset |
APC gene mutations |
|
MUTYH-Associated Polyposis (MAP) |
Multiple colorectal polyps, increased cancer risk |
MUTYH gene mutations |
|
Serrated Polyposis Syndrome |
Multiple serrated polyps, increased colorectal cancer risk |
Multiple genetic and environmental factors |
Knowing about these syndromes is key for early cancer detection and management. Genetic testing and counseling help identify those at risk. This guides how to manage their care.
Treatment Approaches for Patients with Multiple Polyps
Dealing with multiple polyps during a colonoscopy needs a custom plan. This ensures they are removed well and lowers future risks. It’s key to stop colorectal cancer and get the best results for patients.
Endoscopic Removal Techniques for Numerous Polyps
Endoscopic removal is usually the first choice for many polyps. Techniques like endoscopic mucosal resection (EMR) and endoscopic submucosal dissection (ESD) are used. They help remove big or many polyps safely, often during a colonoscopy.
The right endoscopic method depends on the polyp’s size, location, and shape. For example, EMR works well for big, flat polyps. ESD is better for complex or deep polyps. The skill of the gastroenterologist is very important in picking the best method.
When Surgery Becomes Necessary for Polyp Burden
If there are too many polyps or they’re too hard to remove endoscopically, surgery might be needed. Options include laparoscopic-assisted polypectomy or colectomy. The choice to have surgery depends on the patient’s health, the polyps’ characteristics, and the surgery’s risks and benefits.
Surgery is often advised for those with lots of polyps, big polyps hard to remove, or high cancer risk. The aim is to take out the colon part with polyps to lower cancer risk.
Knowing the treatment options helps patients with multiple polyps make better choices. They can work with their healthcare team to find the best treatment plan.
Prevention Strategies to Reduce Future Polyp Formation
There are ways to lower the chance of getting new polyps. Preventing polyps is key to stopping colorectal cancer. Eating right, staying active, and taking some medicines can help.
Dietary Modifications That May Help
What you eat matters a lot in preventing polyps. Eating foods high in fiber, like fruits, veggies, and whole grains, can help. Also, add foods full of antioxidants and omega-3s to your diet. But, cut down on red and processed meats and foods with lots of saturated fats.
- Fiber-rich foods: Include a variety of fruits, vegetables, and whole grains in your diet.
- Antioxidant-rich foods: Consume foods high in antioxidants, such as berries, leafy greens, and other fruits and vegetables.
- Omega-3 fatty acids: Found in fatty fish, flaxseeds, and walnuts, these can help reduce inflammation.
Lifestyle Changes to Consider
Changing your lifestyle can also help prevent polyps. Being active regularly can lower your risk. Keeping a healthy weight and not smoking are also important. Drinking less alcohol can help too.
- Regular Exercise: Engage in at least 150 minutes of moderate-intensity or 75 minutes of vigorous-intensity exercise per week.
- Healthy Weight: Maintain a BMI between 18.5 and 25 through a combination of diet and exercise.
- Avoid Smoking: Smoking cessation can significantly reduce the risk of many health issues, including colorectal polyps.
- Limit Alcohol: Reduce alcohol intake to minimize its harmful effects.
Medications That May Reduce Polyp Recurrence
Some medicines can help prevent polyps from coming back. Aspirin and NSAIDs have shown to lower the risk. But, talk to your doctor before starting these medicines. They can help but also have risks.
- Aspirin: Regular aspirin use has been associated with a reduced risk of colorectal polyps and cancer.
- NSAIDs: Other NSAIDs may also reduce the risk, but their use should be carefully considered due to possible side effects.
By using these prevention strategies, you can lower your risk of new polyps and colorectal cancer. It’s important to work with your doctor to find the best prevention plan for you.
Finding Expert Care for Complex Polyp Cases
When you have many or complex polyps, seeing a specialist can really help. People with complex or multiple polyps need special care. This care offers advanced treatments and focuses on each person’s needs.
When to Seek a Specialist for Multiple Polyps
If you have many polyps or ones that are hard to remove, you should see a specialist. A gastroenterologist with skills in polypectomy and advanced endoscopy can help. Look for a specialist if you have:
- More than 10 polyps found during a colonoscopy
- Polyps bigger than 2 cm in diameter
- Polyps that are hard to remove or need special techniques
- A family history of colorectal cancer or genetic syndromes
Specialists are trained to handle tough cases. They ensure you get the best care. Advanced endoscopic techniques can remove many polyps at once. This means fewer surgeries for you.
Questions to Ask Your Doctor About Your Polyp Count
It’s important to know about your polyp count and risks. Here are some questions to ask your doctor:
|
Question |
Why It Matters |
|---|---|
|
What is my polyp count, and what does it mean for my future risk? |
Knowing your risk helps plan for future care. |
|
Are the polyps precancerous, and if so, what are the next steps? |
Knowing the polyp type helps decide treatment. |
|
What are the recommended surveillance intervals based on my polyp count? |
Regular check-ups are key for catching new polyps early. |
|
Are there any lifestyle changes or treatments that can reduce my risk of developing new polyps? |
Changing your lifestyle or taking certain meds can lower your risk. |
By asking these questions, you can understand your situation better. You can work with your doctor to create a plan. This plan will help manage your polyp count and lower your risk of colorectal cancer.
Conclusion
Knowing how polyp count affects colorectal cancer risk is key for patients. The number of polyps found during a colonoscopy helps figure out future cancer risk. This knowledge helps patients plan their follow-up care and lower their risk of colorectal cancer. We’ve looked at how polyp count, size, and shape affect cancer risk. Patients with many polyps, like more than 10, are at higher risk. They need more frequent checks. This shows why care should be based on each person’s polyp details. To handle personal risk well, patients should team up with their doctors. They’ll create a follow-up plan that fits the patient’s needs. This plan considers the polyp number, size, and type, plus other risk factors. This way, patients can lower their cancer risk and get help when needed.
FAQ
What is considered a high number of polyps during a colonoscopy?
More than 10 polyps are seen as high-risk. This might mean you need to have more frequent check-ups.
Are all polyps precancerous?
No, not all polyps are precancerous. For example, hyperplastic polyps are usually not harmful. But, adenomatous and serrated polyps have a chance of becoming cancerous.
How does the size of a polyp affect its cancer risk?
Polyps bigger than 20mm (0.8 inches) are more likely to be cancerous. Smaller ones have a lower risk.
What is the difference between sessile and pedunculated polyps?
Sessile polyps are flat and harder to spot during a colonoscopy. They have a higher risk of being missed. Pedunculated polyps, on the other hand, are stalked and easier to find.
How often should I have a follow-up colonoscopy if I have 5-10 polyps?
You should have a follow-up colonoscopy in 3 years if you have 5-10 polyps that are under 10mm.
Can genetics play a role in the development of multiple polyps?
Yes, genetics can play a role. Conditions like Familial Adenomatous Polyposis (FAP) and Lynch syndrome increase the risk of getting many polyps and colorectal cancer.
What are the treatment options for patients with multiple polyps?
Treatment options include removing polyps through endoscopy. Sometimes, surgery is needed to remove a large number of polyps.
Can lifestyle changes help reduce the risk of future polyp formation?
Yes, making dietary changes and lifestyle adjustments can help lower the risk of getting more polyps.
When should I seek a specialist for my polyp count?
If you have a lot of polyps or a family history of colorectal cancer, see a specialist. They can give you personalized advice and management.
What questions should I ask my doctor about my polyp count?
Ask about your personal risk, how often you should have check-ups, and what treatments or prevention strategies you might need.


































