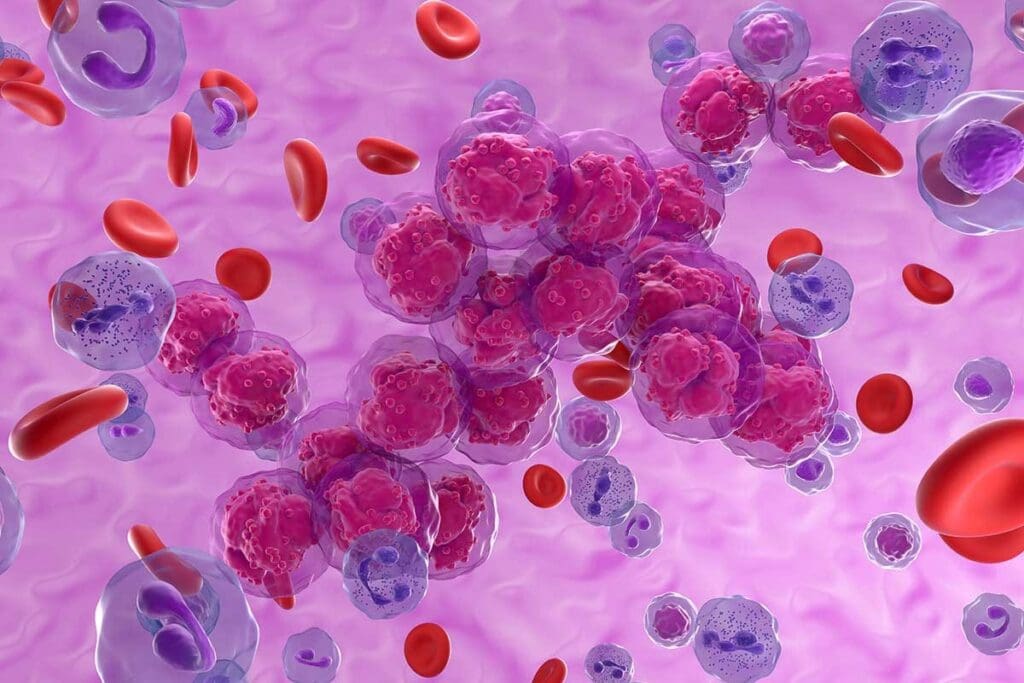
At Liv Hospital, we know how complex precursor B-cell acute lymphoblastic leukemia is. It’s a cancer where immature B lymphoblasts grow too much in the bone marrow and blood. This is the most common type of ALL, hitting kids the hardest.
We’re here to help those with this condition. Our team creates custom treatment plans. We use the newest medical research and tech.
Knowing the facts and symptoms of Pre-B ALL is key to catching it early. We aim to guide patients and their families towards healing.
Key Takeaways
- Pre-BALL is an aggressive cancer characterized by the uncontrolled proliferation of immature B lymphoblasts.
- It is the most common subtype of ALL, especially in children.
- Early diagnosis is critical for effective treatment.
- Liv Hospital offers personalized treatment plans for patients with PPre-BALL.
- Our team is committed to delivering complete care and support.
What is Pre-B ALL? Understanding the Basics
Pre-B ALL is a cancer that starts in precursor B cells. These cells are key to our immune system. They grow into mature B cells, helping us fight off infections.
But in Pre B ALL, genetic changes cause these cells to grow out of control. This leads to too many immature cells in the body.
Definition and Classification of Precursor B-Cell Leukemia
Pre-BLL is a fast-growing cancer of the blood and bone marrow. It’s called “acute” because it spreads quickly if not treated. It’s a type of leukemia where immature B cells, or lymphoblasts, are found in the blood and bone marrow.
Doctors say that finding these lymphoblasts is key to diagnosing Pre-B ALL. They look for specific markers to confirm the diagnosis.
A leading hematologist explains, “The type of Pre B ALL is based on when the leukemia starts in B-cell development.” This helps doctors choose the best treatment.
How Abnormal B Lymphoblasts Develop and Multiply
Abnormal B lymphoblasts in Pre B ALL come from genetic changes. These changes let the cells grow without stopping. This leads to too many bad cells in the bone marrow.
This makes it hard for the body to make normal blood cells. It can cause anemia and make infections more likely.
A study on cancer says, “This growth of bad cells can cause the bone marrow to fail. It can lead to anemia and make infections more likely.” Knowing how this happens helps doctors find better treatments.
The Prevalence and Epidemiology of Pre-B ALL
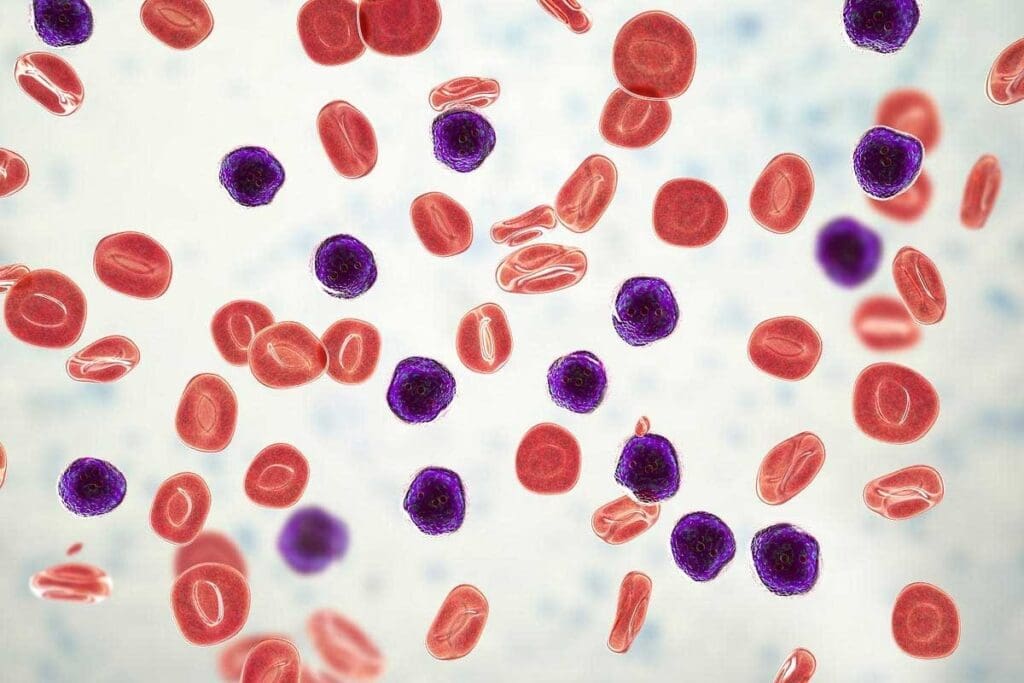
Pre B ALL affects both children and adults, with peaks in different age groups. It’s the most common cancer in kids, making up about 25% of all cancers in those under 15.
Incidence Rates in Children vs. AdultsPre-BB ALL’s incidence changes a lot between kids and adults. Kids see a peak between 1 to 4 years old. Adults see a peak around 50 years old. This shows different risk factors and patterns in each age group.
Incidence Comparison: Kids get Pre B ALL more often than adults, with different age peaks.
| Age Group | Incidence Rate |
| 1-4 years | High |
| 50 years and above | Moderate |
Risk Factors and Demographic Patterns
Genetic predispositions and environmental exposures are key risk factors for Pre-B ALL. It affects some groups more than others, based on ethnicity and where they live.
Epidemiological studies show that Down syndrome increases Pre-B ALL. Ionizing radiation also raises the risk of leukemia.
Knowing who gets Pre B ALL helps in planning health strategies and awareness. This knowledge helps in better managing and treating the disease.
Key Facts About Pre-B ALL That Patients Should Know
When you’re diagnosed with Pre-B ALL, knowing the basics is key. Pre B ALL, or Precursor B-Cell Acute Lymphoblastic Leukemia, is a blood and bone marrow cancer. It’s caused by too many immature B cells, called lymphoblasts.
Most Common Subtype of Acute Lymphoblastic Leukemia
Pre-B ALL is the top ALL subtype, mainly in kids. It makes up about 80-85% of ALL cases in children. This shows why early detection is so important.
Age-Related Differences in Presentation
Pre B ALL shows up differently in kids and adults. Kids often have anemia, infections, and bleeding. Adults might feel tired, lose weight, or have bone pain.
Importance of Early Detection and Treatment
Getting Pre B ALL treated early is key to better outcomes. Quick diagnosis means starting treatment sooner. This can greatly improve survival chances. Treatments include chemotherapy, targeted therapy, and sometimes stem cell transplants.
In short, knowing about Pre-B ALL is essential. It helps patients and families understand the condition better. By knowing the common subtype, age differences, and the need for early treatment, they can make better health choices.
Common Symptoms and Warning Signs of Pre-B ALL
It’s important to know the symptoms of Pre-B ALL early. This type of leukemia can be tricky to spot because its symptoms are not always clear. Knowing these signs can help with early treatment.
Early Symptoms That May Go Unnoticed
In the beginning, Pre-B ALL can seem like other illnesses. You might feel tired, have pale skin, or just not feel right.
Knowing these early signs is key. For example, if you’re always tired, even after resting, it could be a warning. Also, if your skin looks pale, it might mean you have anemia from leukemia.
Advanced Symptoms Requiring Immediate Attention
As Pre B ALL gets worse, symptoms get more serious. You might notice easy bruising, bone pain, or swollen lymph nodes. These are signs you need to see a doctor right away.
Severe cases can lead to infections because your immune system is weak. If you have a high fever, chills, or trouble breathing, get help fast. These are serious signs.
| Symptom | Early Stage | Advanced Stage |
| Fatigue | Mild, persistent tiredness | Severe, interferes with daily activities |
| Pale Skin | Slight pallor | Noticeable anemia |
| Fever | Low-grade fever | High fever, potentially life-threatening |
| Bruising/Bleeding | Minimal | Easy bruising, prolonged bleeding |
Knowing these symptoms and how they change can help you get help quickly. This can make a big difference in your treatment.
“Early diagnosis and treatment of acute lymphoblastic leukemia (ALL) are key to the best results. Spotting the signs early is the first step to getting the right care.”
– Medical Expert
Anemia and Fatigue in Pre-BALL Patients
It’s important to know why Pre B ALL causes anemia and fatigue. We’ll look at how it affects red blood cell production. We’ll also give tips on boosting energy during treatment.
How Leukemia Affects Red Blood Cell Production
Pre B ALL harms the bone marrow’s ability to make red blood cells, causing anemia. Anemia means fewer red blood cells or less hemoglobin. This makes it hard for oxygen to reach tissues, leading to fatigue, weakness, and shortness of breath.
In a healthy person, the bone marrow makes new red blood cells to replace old ones. But in Pre-B ALL patients, leukemia cells fill the bone marrow. This stops normal blood cell production, leading to anemia.
Managing Energy Levels During Treatment
It’s key for Pre-B ALL patients to manage their energy during treatment. Here are ways to fight fatigue:
- Prioritize Rest: Make sure to sleep and rest enough. Listen to your body and take breaks when needed.
- Stay Hydrated: Drink lots of fluids to keep your energy up and support your health.
- Balanced Diet: Eat foods rich in iron, vitamins, and minerals. This helps make red blood cells and keeps you healthy.
- Gentle Exercise: Do gentle exercises like walking or yoga. They can boost your energy without being too hard.
Understanding how Pre B ALL affects red blood cells and using strategies to fight fatigue can improve life during treatment.
Infection Susceptibility: A Critical Concern in Pre-B ALL
People with Pre-B ALL are very likely to get infections. This is because their immune system is weak. They don’t make enough normal white blood cells, which fight off infections.
Why White Blood Cell Function Is Compromised
In Pre B ALL, the bone marrow makes bad B lymphoblasts. These bad cells take over, leaving less room for good immune cells. So, the body can’t make enough good white blood cells to fight off infections.
Impact on White Blood Cells: The disease and treatments can lower the number and strength of white blood cells. Neutrophils and lymphocytes are key in fighting off infections.
Infection Prevention Strategies
To lower the chance of getting infections, several steps can be taken. These include:
- Maintaining good hygiene practices, such as frequent handwashing.
- Avoiding close contact with individuals who are sick.
- Staying up-to-date with recommended vaccinations.
- Using prophylactic antibiotics as prescribed by healthcare providers.
| Infection Prevention Measures | Description | Benefit |
| Good Hygiene Practices | Frequent handwashing, avoiding touching the face | Reduces the risk of contracting infections |
| Avoiding Sick Contacts | Limiting contact with people who are ill | Decreases exposure to possible infections |
| Prophylactic Antibiotics | Using antibiotics as a preventive measure | Helps prevent infections in high-risk patients |
By knowing why infections are a big risk and using good prevention methods, we can help manage Pre-B ALL better. This can lead to better health outcomes for patients.
Bleeding Complications and Bruising in Pre-B ALL
It’s important to know why bleeding happens in Pre-B ALL. This is because of a low platelet count. This is a big worry for those with Pre-B ALL.
Thrombocytopenia, or low platelets, is common in Pre-B ALL. Leukemia cells take over the bone marrow. This means fewer platelets are made, making it hard to stop bleeding.
Platelet Deficiency in Pre-BB ALL
A low platelet count, or thrombocytopenia, is a big problem in Pre-B ALL. It makes it hard for blood to clot. This can cause bleeding without injury or bleeding that won’t stop.
Platelets should be between 150,000 and 450,000 per microliter of blood. But in Pre B ALL, this number drops. This makes bleeding more likely. How bad the bleeding is depends on how severe the leukemia is.
| Platelet Count (per microliter) | Bleeding Risk Level |
| 150,000 – 450,000 | Normal |
| 50,000 – 149,000 | Mild |
| 20,000 – 49,000 | Moderate |
| < 20,000 | Severe |
Recognizing Dangerous Bleeding Symptoms
It’s key for Pre-B ALL patients and their caregivers to know the signs of bad bleeding. Look out for:
- Frequent or severe nosebleeds
- Bleeding gums or mouth sores
- Easy bruising or petechiae (small red or purple spots on the skin)
- Prolonged bleeding from cuts or injuries
- Blood in the urine or stool
- Headaches or confusion, which could indicate intracranial bleeding
It’s vital to catch and treat bleeding problems early. If you see any of these signs, get help right away.
Diagnostic Process and B-Cell Markers for Pre-B ALL
The journey to diagnose Pre-B ALL starts with blood tests and a physical check-up. Then, more detailed tests follow. Accurate diagnosis is key to a good treatment plan.
Initial Blood Tests and Physical Examination
First, blood tests check for any odd cell counts. A complete blood count (CBC) looks for signs of anemia or infection. A physical exam checks for swollen lymph nodes or an enlarged spleen.
Bone Marrow Biopsy Procedures
A bone marrow biopsy is a key test for Pre-B ALL. It takes a sample from the hipbone to look for cancer cells. The test is done under local anesthesia, and the sample is checked for leukemia.
CD19 and cCD22 Markers in Diagnosis
CD19 and cCD22 markers are important for diagnosing Pre B ALL. These proteins are found on B cells and are detected by flow cytometry. Their presence confirms Pre-B ALL and differentiates it from other leukemias.
The table below shows the main tests and markers for Pre-B ALL diagnosis:
| Diagnostic Test | Purpose | Key Findings |
| Initial Blood Tests | Analyze blood cell counts | Anemia, infection, or bleeding disorders |
| Physical Examination | Check for symptoms | Swollen lymph nodes, enlarged spleen |
| Bone Marrow Biopsy | Examine bone marrow for cancerous cells | Presence of leukemia cells, genetic abnormalities |
| CD19 and cCD22 Markers | Confirm diagnosis of Pre-B ALL | Presence of specific B-cell markers |
By using these tests and markers, doctors can accurately diagnose Pre-B ALL. This helps them create a focused treatment plan.
Genetic Testing and Risk Stratification in Pre-B ALL
Understanding the genetic makeup of Pre-B ALL patients is key to effective treatment. Genetic testing is now a mainstay in managing PrPre-BLL. It gives vital information that guides treatment choices.
Genetic testing spots specific chromosomal translocations and genetic abnormalities in Pre-B ALL. These genetic profiles help in risk stratification. This determines how intense the treatment should be.
Chromosomal Translocations and Their Significance
Chromosomal translocations swap genetic material between chromosomes. This creates fusion genes that can lead to leukemia. In Pre-B ALL, some translocations are linked to a higher risk of relapse or treatment failure.
Some common chromosomal translocations in Pre B ALL include:
- The t(9;22) translocation, also known as the Philadelphia chromosome, is associated with a poorer prognosis.
- The t(12;21) translocation, which involves the TEL-AML1 fusion gene and is generally associated with a favorable prognosis.
- The t(4;11) translocation, involving the MLL-AF4 fusion gene, is often seen in infant ALL and is associated with a high-risk disease.
Genetic testing helps identify these translocations. This allows clinicians to group patients by risk. It helps tailor the treatment to each patient’s risk profile.
How Genetic Profiles Determine Treatment Approaches
The genetic profile of a Pre-B ALL patient is vital in choosing the right treatment. Patients with high-risk genetic features may need more intense chemotherapy or targeted therapies.
For example, patients with the Philadelphia chromosome-positive Pre B ALL may benefit from tyrosine kinase inhibitors (TKIs). Patients with other genetic abnormalities may be candidates for immunotherapy or other new treatments.
Genetic testing is integrated into the diagnostic workflow. This helps create personalized treatment plans based on each patient’s genetic characteristics. This approach aims to improve outcomes by ensuring patients get the most effective therapy for their disease.
Key benefits of genetic testing in Pre-B ALL include:
- Accurate risk stratification
- Personalized treatment planning
- Identification of targets for therapy
- Improved patient outcomes through tailored treatment approaches
Treatment Approaches for Pre-B ALL Patients
Pre-B ALL treatment uses many strategies to help patients. We’ll talk about the main ways to treat it. These include chemotherapy, targeted therapies, immunotherapies, and stem cell transplants.
Standard Chemotherapy Protocols
Chemotherapy is key in treating Pre-B ALL. Doctors use a mix of drugs like vincristine and anthracyclines. The goal is to get rid of the cancer and keep it away.
We adjust the treatment based on how high the risk is. This way, we make sure the treatment is right for each patient. It helps avoid too much harm while being effective.
Targeted Therapies and Immunotherapies
Targeted and immunotherapies are new and important in Pre-B ALL treatment. They target specific parts of cancer cells. This can be less harsh than traditional chemotherapy.
Monoclonal antibodies, like blinatumomab, are used to attack cancer cells. They’ve shown great results in clinical trials. This is good news for patients with hard-to-treat cases.
Stem Cell Transplantation Considerations
Stem cell transplantation is for high-risk cases or when cancer comes back. It uses strong chemotherapy and healthy stem cells to fight cancer.
Choosing to do a stem cell transplant is a big decision. We look at the patient’s health, how bad the cancer is, and the risks. We decide what’s best for each patient.
| Treatment Modality | Key Features | Indications |
| Standard Chemotherapy | Multi-agent regimen, risk-adapted approach | Initial treatment, consolidation, maintenance |
| Targeted Therapies | Monoclonal antibodies (e.g., CD19 targeting) | Refractory or relapsed disease |
| Immunotherapies | Agents like blinatumomab | Refractory or relapsed disease |
| Stem Cell Transplantation | High-dose chemotherapy followed by healthy stem cell infusion | High-risk disease, relapse |
Prognosis and Survival Rates: Children vs. Adults
The outlook for Pre-B ALL differs a lot between kids and adults. Age is a key factor in how well treatment works. Kids have seen big improvements, but adults face bigger hurdles.
85% Cure Rate in Pediatric Patients
Kids with Pre-B ALL have a high cure rate, around 85%. This success is thanks to better chemotherapy and care.
“The cure rate for children with ALL has improved dramatically over the past few decades, with modern treatment protocols achieving cure rates of around 85% or higher in many cases.”
40% Five-Year Survival in Adult Patients
Adults with Pre-B ALL have a tougher time, with a five-year survival rate of about 40%. This gap is because of differences in the disease and how it responds to treatment.
Factors That Influence Treatment Outcomes
Many things affect how well Pre-B ALL patients do. These include:
- Age: Younger patients usually do better.
- Genetic abnormalities: Some genetic changes can impact treatment success.
- Response to initial treatment: Those who do well at first tend to have a better outlook.
Knowing these factors helps doctors create better treatment plans for each patient.
Conclusion: Advances in Pre-B ALL Research and Future Directions
Recent research has greatly improved our understanding of pre-B-cell b, a complex and aggressive cancer. We’ve found over 200 gene fusions or mutations. This knowledge helps us offer more personalized treatments to patients with Acute Lymphoblastic Leukemia (ALL).
The field of pre-b is growing fast. New genetic tests and ways to group patients by risk are changing how we treat them. Targeted and immunotherapies are also showing great promise, giving hope to those with hard-to-treat cases.
We’re dedicated to top-notch healthcare, including support for patients from around the world. By keeping up with the latest in pre-b all research, we aim to improve the lives of those with this disease.
FAQ
What is Pre-B ALL?
Pre-B ALL is a cancer that affects the blood and bone marrow. It’s caused by the growth of immature B lymphoblasts without control.
What are the symptoms of Pre-B ALL?
Early signs of Pre-B ALL include anemia, fatigue, and infections. As it gets worse, symptoms like bleeding, bruising, and severe infections may appear. These need quick medical help.
How is Pre-B ALL diagnosed?
Doctors use blood tests, physical exams, and bone marrow biopsies to diagnose Pre-B ALL. They look for B-cell markers like CD19 and cCD22 to confirm it.
What is the role of genetic testing in Pre-B ALL?
Genetic testing is key in managing Pre-B ALL. It helps find chromosomal changes and other genetic issues. This info is vital for planning treatment.
What are the treatment options for Pre-B ALL?
Treating Pre-B ALL involves several steps. This includes standard chemotherapy, targeted therapies, and immunotherapies. In some cases, stem cell transplantation is considered.
What is the prognosis for Pre-B ALL patients?
The outlook for Pre-B ALL patients differs by age. Children have a better chance of being cured, with an 85% survival rate. Adults face a tougher battle, with a 40% five-year survival rate.
How does Pre-B ALL affect the immune system?
Pre-B ALL weakens the immune system. It makes patients more prone to infections and affects red blood cell production. This leads to anemia and fatigue.
What are the risk factors for Pre-B ALL?
The risk of Pre-B ALL changes with age. Children and adults have different risk factors and patterns. These include age, genetic predisposition, and environmental factors.
Can Pre-B ALL be cured?
Pre-B ALL is a challenging cancer, but research has made treatments better. This has led to cures for some, mainly children.
References
- National Center for Biotechnology Information. (2023, August 25). Acute lymphocytic leukemia – StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK459149/




































