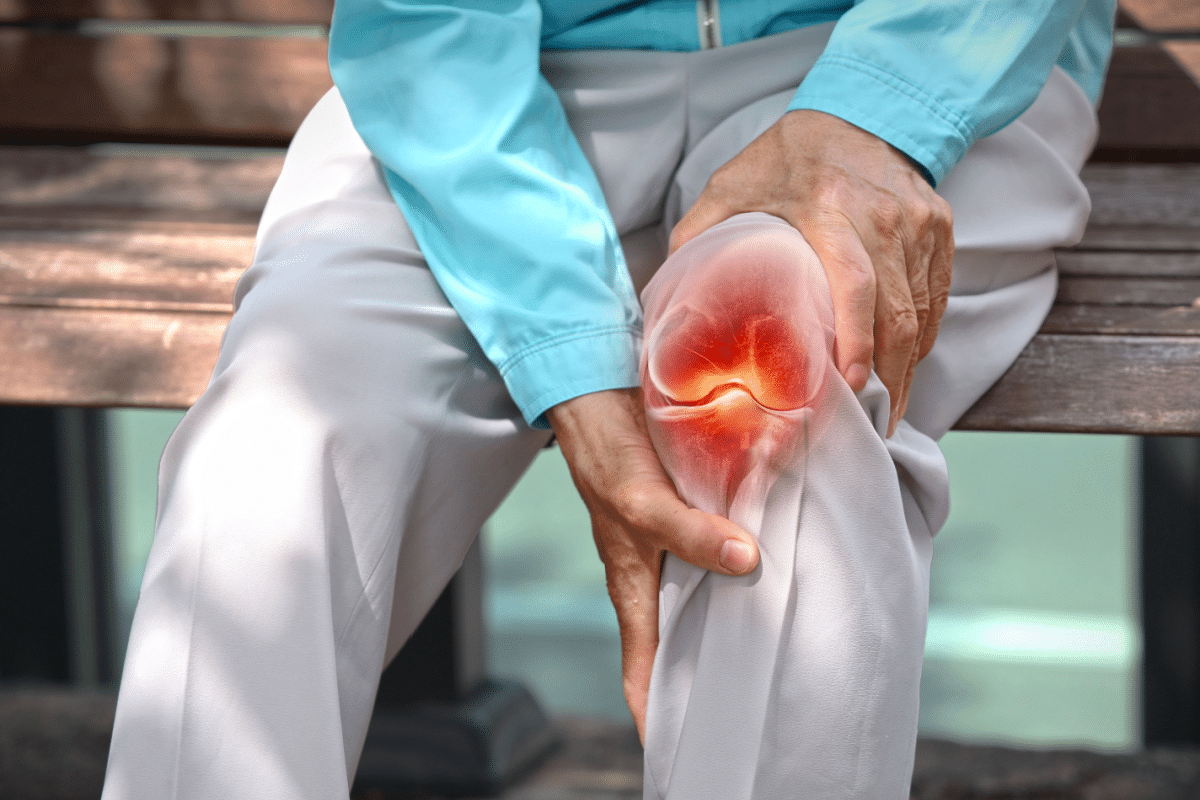
Explaining how traumatic arthritis develops after a joint injury and detailing steps for prevention and early management.
Post-traumatic arthritis is a condition that can develop after a joint injury. It affects millions of people around the world. When a joint is injured, it can start to change. This leads to inflammation, swelling, and pain.
At Liv Hospital, we understand how trauma can lead to arthritis. We offer detailed evaluations and care plans focused on our patients. Our goal is to help manage and prevent post-traumatic arthritis from getting worse.
Early recognition and intervention are key to reducing the long-term effects of post-traumatic arthritis.
Key Takeaways
- Post-traumatic arthritis can develop after a joint injury.
- Inflammation and pain are common symptoms.
- Understanding the condition is key to effective management.
- Liv Hospital offers complete care for post-traumatic arthritis.
- Early intervention can mitigate long-term effects.
The Link Between Injury and Arthritis Development
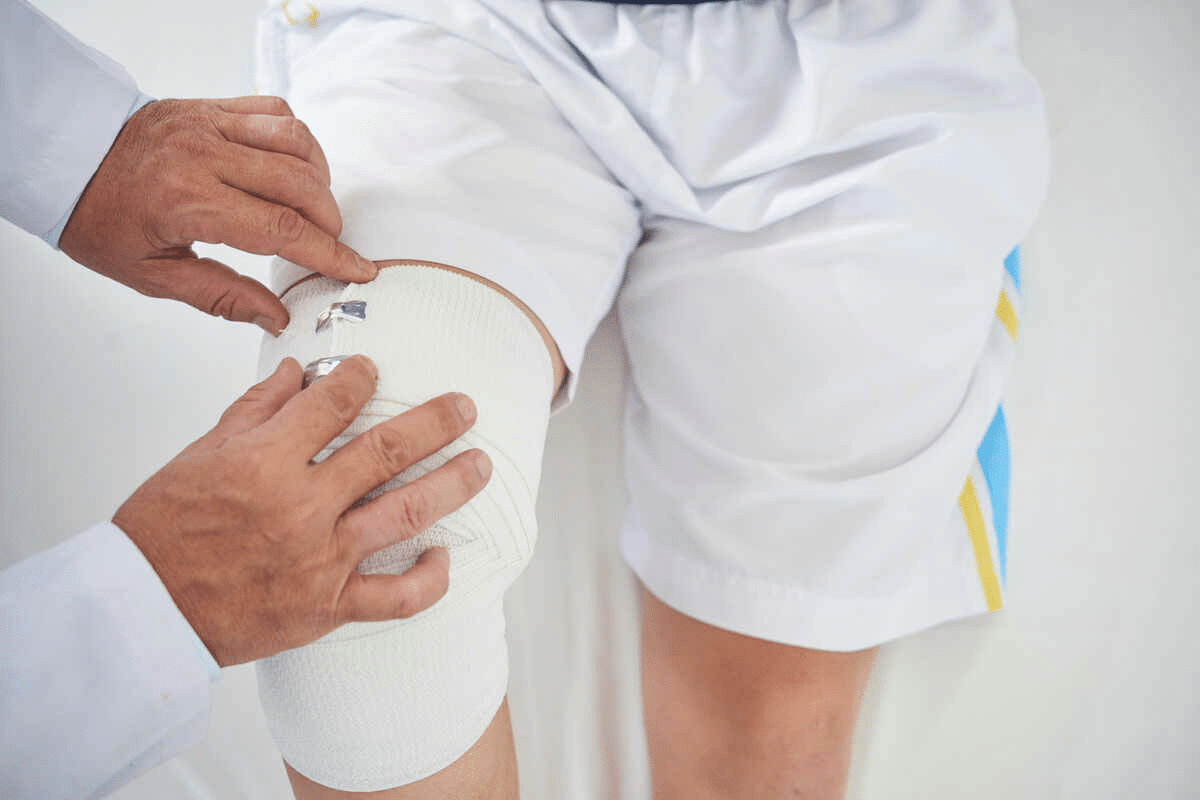
Injuries to joints can start a chain of events that may lead to arthritis. Studies show that posttraumatic arthritis affects over 5 million adults in the U.S. It’s responsible for about 12 percent of all osteoarthritis cases. An early injury, like an ACL tear or fracture, can cause OA to start much sooner.
How Joint Injuries Lead to Arthritis
When a joint is hurt, the damage to cartilage, bone, and soft tissues starts a series of changes. These changes include inflammation and changes in how the joint works. Over time, this can cause the joint to degenerate, leading to arthritis.
The severity and type of injury greatly affect the chance of getting post-traumatic arthritis. For example, injuries that badly damage cartilage or make the joint unstable are more likely to cause arthritis.
The Biological Mechanism of Post-Injury Joint Degeneration
The process of joint degeneration after an injury involves many cellular and molecular steps. After an injury, there’s an inflammatory response that can harm the joint. This response releases molecules that can make inflammation worse and damage the joint tissues.
Also, the injury can change how the joint works, putting extra stress on some areas. This stress can make the joint wear out faster, leading to arthritis over time.
What Is Traumatic Arthritis?
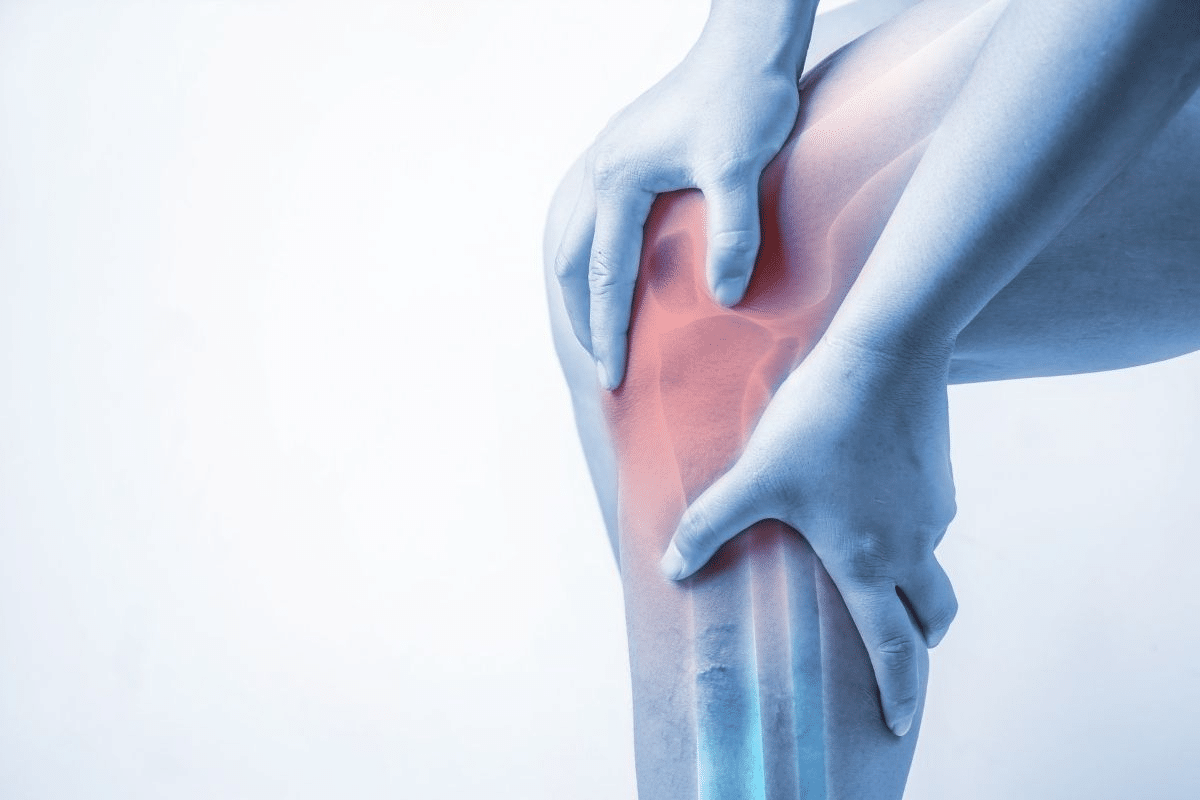
Post-traumatic arthritis happens after a direct injury to a joint. About 50 percent of people with such injuries get osteoarthritis. It’s a big worry for those who’ve had severe joint injuries from accidents or car crashes.
Definition and Classification
Traumatic arthritis, or post-traumatic arthritis, is a type of osteoarthritis. It starts after a joint injury. It causes cartilage and bone to wear down, leading to pain, stiffness, and less mobility. The severity of the injury and the damage to the joint decide how it’s classified.
Difference Between Post-Traumatic Arthritis and Other Forms of Arthritis
Post-traumatic arthritis is different from other arthritis types like rheumatoid arthritis. The main difference is the injury that leads to it. Knowing this helps doctors diagnose and plan treatment.
Common Terminology: Post-Traumatic Osteoarthritis (PTOA)
Post-traumatic osteoarthritis (PTOA) is another name for post-traumatic arthritis. It’s osteoarthritis that comes after a joint injury. It often happens after serious injuries like fractures or severe sprains.
Important things about PTOA include:
- A healthy joint becomes arthritic after trauma.
- There might be a long time between the injury and when symptoms start.
- Early diagnosis and treatment are key to managing symptoms and slowing the disease.
We know that post-traumatic arthritis is a complex issue that needs thorough care. Understanding its definition, classification, and how it differs from other arthritis types helps us tackle diagnosis and treatment better.
Prevalence and Statistics
It’s important to know how common post-traumatic arthritis is. This condition, often called post-traumatic osteoarthritis (PTOA), is a big worry after serious injuries.
Incidence Rates in the United States
Studies show that 20 to over 50 percent of people get post-traumatic arthritis after big injuries. For example, over 50% of those with early ACL tears end up with PTOA 20 years later. This shows how serious joint injuries can be over time.
Demographic Patterns
Post-traumatic arthritis can hit people of all ages and backgrounds. But, some groups are more likely to get it. This includes young athletes in high-impact sports, for instance.
Economic Impact of Post-Traumatic Arthritis
The cost of post-traumatic arthritis is huge. It includes the cost of treatments and lost work time. Here’s a detailed look at these costs:
|
Cost Category |
Average Annual Cost per Patient |
Total Annual Cost in the United States |
|---|---|---|
|
Direct Medical Costs |
$5,000 |
$2 billion |
|
Indirect Costs (Lost Productivity) |
$3,000 |
$1.2 billion |
|
Total Economic Burden |
$8,000 |
$3.2 billion |
The big cost of post-traumatic arthritis shows we need better ways to prevent and treat it. This will help both individuals and society.
Common Causes of Post-Traumatic Arthritis
Post-traumatic arthritis often comes from big injuries. Many incidents can cause it, hitting different parts of the body, like joints.
Sports-Related Injuries
Sports injuries are a big reason for post-traumatic arthritis. High-impact sports, contact, or sudden stops can hurt joints. For example, knee injuries from football, basketball, or soccer are common.
Post-traumatic arthritis of the knee is a big worry for those who’ve had such injuries.
Vehicular Accidents
Car accidents also lead to post-traumatic arthritis. The crash can damage joints, causing pain and inflammation. The force from a crash can break bones or dislocate joints, raising the risk of arthritis.
Falls and Workplace Injuries
Falls and work injuries also cause post-traumatic arthritis. Falls can lead to fractures or severe sprains, which may cause arthritis later. Workplace injuries, like heavy lifting or bending, can also damage joints.
Military Service-Related Trauma
Military trauma is a big risk for post-traumatic arthritis. Military people face high-impact injuries, like blasts or falls, that can harm joints. The demands of military life and the risk of injury make them more likely to get post-traumatic arthritis.
Most Affected Joints and Their Vulnerabilities
Joints like the knee and ankle are more likely to get post-traumatic arthritis. This is because they can easily get hurt. The knee, being big and complex, carries a lot of weight and stress. This makes it more likely to get injured and develop arthritis.
Posttraumatic Arthritis of the Knee
The knee is very prone to post-traumatic arthritis after injuries. Trauma to the knee can change how the joint works. This can cause uneven wear on the cartilage, a sign of osteoarthritis. Studies show that knee injuries, like those from sports, raise the risk of arthritis in the knee.
A study on athletes found that ACL injuries increased the risk of knee osteoarthritis later in life. This shows how important it is to manage and rehab knee injuries to avoid arthritis.
Ankle Joint Vulnerability
The ankle is also often affected by post-traumatic arthritis. Ankle fractures or severe sprains can make the joint unstable. This can raise the risk of arthritis. The ankle’s complex structure makes it more likely to get hurt and have lasting effects.
- Ankle fractures that involve the joint surface can lead to post-traumatic arthritis.
- Severe ankle sprains, like those with ligament tears, can also contribute to arthritis.
Other Commonly Affected Joints
While the knee and ankle are most affected, other joints like the hip, shoulder, and elbow can also get post-traumatic arthritis. The severity and type of initial trauma play a big role in whether arthritis will develop in a joint.
In conclusion, knowing which joints are most at risk is key to managing and preventing post-traumatic arthritis. By understanding the risks of certain injuries, healthcare providers can take steps to prevent long-term damage to joints.
Risk Factors for Developing Arthritis After Injury
It’s important to know what increases the chance of getting arthritis after an injury. When we get hurt, many things can affect if we’ll get arthritis later. This includes how bad the injury was and our overall health.
Severity and Type of Initial Trauma
The severity and type of injury matter a lot. For example, injuries that cause fractures or damage to ligaments raise the risk. The more damage to the joint, the higher the chance of arthritis later.
BMI Correlation
Our Body Mass Index (BMI) also plays a big role. Studies show that a higher BMI increases the risk of arthritis by 35% for every five units. Keeping a healthy weight is key to lowering this risk.
Age and Gender Considerations
Age is a big factor, with most arthritis cases happening in people over 65. Women are also more likely to get arthritis, starting at 50. Knowing these facts helps us understand who might be at higher risk.
Genetic Predisposition
Our genes also affect our risk. If your family has a history of arthritis, you might be more likely to get it after an injury. Knowing this can help us take steps to prevent it.
|
Risk Factor |
Description |
Impact on Risk |
|---|---|---|
|
Severity of Initial Trauma |
More severe injuries increase the risk. |
High |
|
BMI |
A higher BMI correlates with increased risk. |
Moderate to High |
|
Age |
Risk increases significantly after age 65. |
High |
|
Gender |
Women are at higher risk, specially after 50. |
Moderate |
|
Genetic Predisposition |
Family history of osteoarthritis increases risk. |
Moderate to High |
Knowing these risk factors helps us prevent and manage arthritis after injuries. This can lead to better outcomes for those who have been hurt.
Recognizing Post-Traumatic Arthritis Symptoms
Post-traumatic arthritis symptoms can start off small but are important to catch early. When we get a joint injury, we often focus on the immediate pain and swelling. But, it’s also key to watch out for long-term effects like post-traumatic arthritis.
Early Warning Signs
The first signs of post-traumatic arthritis include persistent joint pain, swollen joints, and fluid buildup in the joints. These signs can be hard to tell apart from the injury itself. But, if these signs keep going or get worse, it might mean you have post-traumatic arthritis.
Medical Expert. Heckman, an orthopedic surgeon, says, “Early spotting and treatment of post-traumatic arthritis are key. Anyone with ongoing joint pain or stiffness after an injury should see a doctor.”
Progressive Symptom Development
As post-traumatic arthritis gets worse, symptoms get more obvious. Joint pain might grow, and moving around can become harder. Some people find they can’t do as much physical activity because of pain or discomfort. It’s important to keep an eye on these changes and adjust treatment plans as needed.
- Gradual increase in joint pain
- Swelling and inflammation
- Reduced range of motion
- Increased stiffness, mostly after resting
Differentiating from Acute Injury Pain
Telling apart post-traumatic arthritis symptoms from acute injury pain can be tricky. Acute injury pain usually goes away as the injury heals. But, post-traumatic arthritis pain sticks around or comes back over time. If you’re feeling pain that doesn’t go away or gets worse, you should talk to a doctor.
“Post-traumatic arthritis needs a full treatment plan, tackling symptoms and the root causes.” –
Medical Expert, Rheumatologist
When to Seek Medical Attention
If you notice any of these signs, it’s time to see a doctor:
- Persistent or getting worse joint pain
- Swelling or inflammation that doesn’t get better with rest and treatment
- Less mobility or stiffness
- More pain or discomfort when doing physical activities
Getting a diagnosis and treatment early can really help manage post-traumatic arthritis. By spotting symptoms early and getting medical help when needed, we can improve outcomes and keep our joints healthy.
Diagnosis and Assessment Methods
To diagnose post-traumatic arthritis, doctors use a detailed approach. This includes clinical checks, advanced imaging, and lab tests. These steps help doctors understand the joint damage and plan the best treatment.
Clinical Evaluation Process
The first step in diagnosing post-traumatic arthritis is a thorough check-up. Doctors review your medical history and perform a physical exam. They look at how well your joint works, your pain, and how much you can move it.
Doctors search for signs of joint instability, muscle weakness, and limited movement. Knowing your injury history and past treatments helps them understand your current symptoms better.
Imaging Techniques
Imaging is key in diagnosing post-traumatic arthritis. Doctors use X-rays, CT scans, and MRIs to see the joint and tissues. These tests show bone spurs, cartilage damage, and other issues not seen in physical exams.
X-rays check bone health and joint alignment. CT scans show bone details, and MRIs help with soft tissue and cartilage damage. Together, these images give a full picture of the joint’s state.
“Imaging studies are essential for diagnosing post-traumatic arthritis, as they provide a clear visual representation of the joint damage and help guide treatment decisions.”
Laboratory Tests and Their Role
Laboratory tests help confirm post-traumatic arthritis and rule out other causes. Doctors might test your blood for inflammation or other conditions causing joint pain.
Lab tests aren’t the only way to diagnose post-traumatic arthritis. But, they help doctors rule out other conditions. By combining lab results with clinical and imaging findings, doctors can make a precise diagnosis and plan treatment.
Treatment Approaches for Post-Traumatic Arthritis
Managing post-traumatic arthritis needs a detailed plan. This plan might include non-surgical steps, surgery, and new treatments. Every case is different, so we tailor our treatment to fit each person’s needs.
Conservative Management Strategies
First, we try non-surgical methods to treat post-traumatic arthritis. These methods aim to lessen pain and improve joint use. Here are some key steps:
- Physical Therapy: We create special exercise plans to boost joint movement and muscle strength.
- Pain Management: We use medicines like NSAIDs, pain relievers, and steroid shots to control pain and swelling.
- Lifestyle Modifications: We help patients change their daily habits to ease joint stress. This includes keeping a healthy weight and using aids when needed.
Surgical Interventions
If non-surgical methods don’t work, surgery might be needed. We choose surgery based on how severe the arthritis is and the patient’s health. Some common surgeries include:
- Joint Debridement: We remove damaged tissue and bone spurs to help the joint work better.
- Osteotomy: We adjust the bones to spread out the weight-bearing stress.
- Joint Fusion or Arthrodesis: We join the bones together to stop joint movement and lessen pain.
- Joint Replacement: We replace the damaged joint with an artificial one to improve function and reduce pain.
Emerging Treatments and Clinical Trials
New research is finding promising treatments for post-traumatic arthritis. Some of these include:
- Biologic Therapies: These treatments target inflammation and might slow the disease’s progress.
- Stem Cell Therapy: This is an experimental treatment that could help heal and grow new tissue.
- Advanced Surgical Techniques: New surgical methods, like less invasive surgeries and 3D-printed implants, are being explored.
We are dedicated to keeping up with these new treatments. This way, we can offer our patients the latest and most effective options.
Prevention Strategies Following Joint Injury
After a joint injury, taking steps to prevent arthritis is key. It’s important to act fast to lessen the injury’s long-term effects.
Immediate Post-Injury Care
The first steps after a joint injury are vital. They help stop arthritis from developing. Here’s what to do:
- Get a quick medical check to see how bad the injury is.
- Use proper immobilization to avoid more harm.
- Start anti-inflammatory treatments early.
Rehabilitation Importance
Rehabilitation is essential to prevent arthritis. It helps your joint work better, makes muscles stronger, and boosts flexibility. A physical therapist can help create a plan just for you.
Weight Management
Keeping a healthy weight is important for your joints. It helps prevent arthritis. Eating right and exercising regularly can make a big difference.
Activity Modification and Joint Protection
Changing how you do things is important. It helps protect your joint. Here’s how:
- Stay away from activities that put too much stress on your joint.
- Use protective gear or tools when needed.
- Slowly go back to normal activities with a doctor’s advice.
By following these prevention strategies, you can lower your risk of arthritis after a joint injury. Being proactive and working with doctors is key to a good prevention plan.
Conclusion
Understanding post-traumatic arthritis is key for prevention and treatment. This condition often comes from serious injuries. It can cause long-term pain and disability if not handled right.
Early detection and the right treatment can greatly improve life for those with this condition. Knowing the risks, like the injury’s severity and who is at risk, helps us prevent it better.
Preventing and treating traumatic arthritis needs a wide approach. This includes quick care after injury, rehab, managing weight, and changing how active you are. These steps can lower the chance of getting post-traumatic arthritis and help those who do.
FAQ
What is post-traumatic arthritis?
Post-traumatic arthritis happens after a joint injury. This can be a fracture, dislocation, or severe sprain. It causes joint pain, stiffness, and limited movement due to degenerative changes after the injury.
Can any injury cause arthritis?
Not every injury leads to arthritis. But, injuries to the joints can raise the risk. The risk depends on the injury’s severity and type, along with individual factors.
How common is post-traumatic arthritis?
Post-traumatic arthritis is a big concern for many. It affects a lot of people who have had joint injuries. The exact number varies by the joint and injury type.
What are the most common causes of post-traumatic arthritis?
Common causes include sports injuries, car accidents, falls, and workplace injuries. Military service trauma also plays a role. These can lead to fractures, dislocations, and other severe injuries that may cause arthritis.
Which joints are most vulnerable to post-traumatic arthritis?
The knee and ankle are most at risk. This is because they bear a lot of weight and are prone to injury. Other joints, like the hip, shoulder, and elbow, can also be affected, depending on the injury.
What are the symptoms of post-traumatic arthritis?
Symptoms include joint pain, stiffness, swelling, and reduced mobility. These symptoms can get worse over time as the condition progresses.
How is post-traumatic arthritis diagnosed?
Doctors use a combination of clinical evaluation, imaging, and lab tests. These help assess joint damage and rule out other causes of symptoms.
What treatment options are available for post-traumatic arthritis?
Treatment options range from physical therapy and pain management to surgery. New treatments and clinical trials are also being explored.
Can post-traumatic arthritis be prevented?
While not all cases can be prevented, some steps can help. Immediate care, rehabilitation, managing weight, and modifying activities can reduce the risk after a joint injury.
What is post-traumatic osteoarthritis (PTOA)?
Post-traumatic osteoarthritis (PTOA) is a type of arthritis that occurs after a joint injury. It’s characterized by degenerative changes in the joint. It’s a common term for this condition.
How does the severity of the initial trauma affect the risk of developing post-traumatic arthritis?
The severity of the initial trauma greatly affects the risk of post-traumatic arthritis. More severe injuries increase the risk.
Are there any risk factors that increase the likelihood of developing post-traumatic arthritis?
Yes, several factors increase the risk. These include the severity and type of initial trauma, BMI, age, gender, and genetic predisposition.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://pubmed.ncbi.nlm.nih.gov/17062981/

































