
When dealing with coronary artery disease, two main treatments are considered: coronary artery bypass graft and stent placement. We’ll look into how these heart surgery options differ and what they mean for patient care.Comparing the benefits and risks of each procedure using a bypass vs stent comparison to determine the best treatment.
It’s important to understand the cost of these treatments. Recent studies have found that bypass surgery and stent placement have different costs. This affects healthcare choices.
Key Takeaways
- Coronary artery bypass graft and stent placement are two main treatments for coronary artery disease.
- The choice between these procedures depends on various factors, including patient health and disease severity.
- Economic evaluations play a significant role in determining the cost-effectiveness of these treatments.
- Understanding the differences between bypass and stent procedures is essential for informed healthcare decisions.
- Patient outcomes and quality of life are critical considerations in choosing between these heart surgery options.
Understanding Coronary Artery Disease
Coronary artery disease happens when plaque builds up in the arteries. This buildup can lead to heart problems. The coronary arteries are the main blood vessels that feed the heart.
Plaque Buildup in Arteries
Plaque buildup starts with damage to the artery’s inner layer. High blood pressure, smoking, and high cholesterol can cause this damage. Over time, the plaque narrows the artery and cuts off blood flow to the heart.
As plaque grows, it can become unstable and rupture. This can cause a blood clot to form, blocking the artery. This blockage can lead to a heart attack. Knowing how this works is key to understanding the need for coronary artery disease treatment and heart disease interventions.
Symptoms and Diagnosis
Coronary artery disease often shows no symptoms until a blockage is severe. Some people may feel chest pain, shortness of breath, or fatigue. Doctors use medical history, physical exams, and tests like ECGs and coronary angiography to diagnose it.
“Early diagnosis and treatment of coronary artery disease can significantly improve outcomes and reduce the risk of complications,” says a leading cardiologist.
When Intervention Becomes Necessary
Intervention is needed when the disease severely limits blood flow to the heart. This can cause symptoms or increase the risk of a heart attack. Treatments include lifestyle changes, medications, and coronary blockage solutions like angioplasty or CABG.
|
Treatment Option |
Description |
Benefits |
|---|---|---|
|
Lifestyle Modifications |
Dietary changes, exercise, smoking cessation |
Reduces risk factors, improves overall health |
|
Medications |
Cholesterol-lowering drugs, beta-blockers, antiplatelet agents |
Manages symptoms, slows disease progression |
|
Angioplasty with Stenting |
Minimally invasive procedure to open blocked arteries |
Restores blood flow, reduces symptoms |
|
CABG |
Surgical bypass of blocked coronary arteries |
Improves blood flow, reduces risk of heart attack |
Knowing when to intervene is key to managing coronary artery disease. Recognizing symptoms and understanding heart disease interventions helps individuals make informed care choices.
What is Coronary Artery Bypass Graft (CABG) Surgery?
CABG surgery is a complex operation to fix blocked heart arteries. It’s for those with severe heart disease or who haven’t improved with other treatments. The goal is to keep the heart safe from heart attacks.
Definition and Basic Procedure
In CABG, a healthy blood vessel is taken from the body to bypass blocked arteries. This improves blood flow to the heart. The surgery is done under general anesthesia, and the heart is stopped.
The surgeon makes a chest incision to reach the heart. A graft is then attached to bypass the blockage. This ensures blood keeps flowing to the heart muscle.
Types of Bypass Grafts
There are different grafts used in CABG:
- The saphenous vein from the leg
- The internal mammary artery inside the chest
- The radial artery from the forearm
The choice of graft depends on the patient’s health and disease extent. The surgeon also plays a role in this decision.
Evolution of Bypass Surgery Techniques
CABG surgery has seen many improvements over time. These advancements aim to reduce recovery time and scarring. They also aim to improve patient outcomes.
|
Technique |
Description |
Benefits |
|---|---|---|
|
Off-pump CABG |
Surgery performed without stopping the heart or using a heart-lung machine |
Reduced risk of complications related to the heart-lung machine |
|
Minimally invasive CABG |
Surgery performed through smaller incisions |
Less scarring, quicker recovery |
|
Robotic CABG |
Surgery assisted by robotic systems for precision |
Enhanced precision, potentially fewer complications |
These advancements have made CABG surgery safer and more effective. They offer hope to those with complex heart conditions.
What are Coronary Stents?
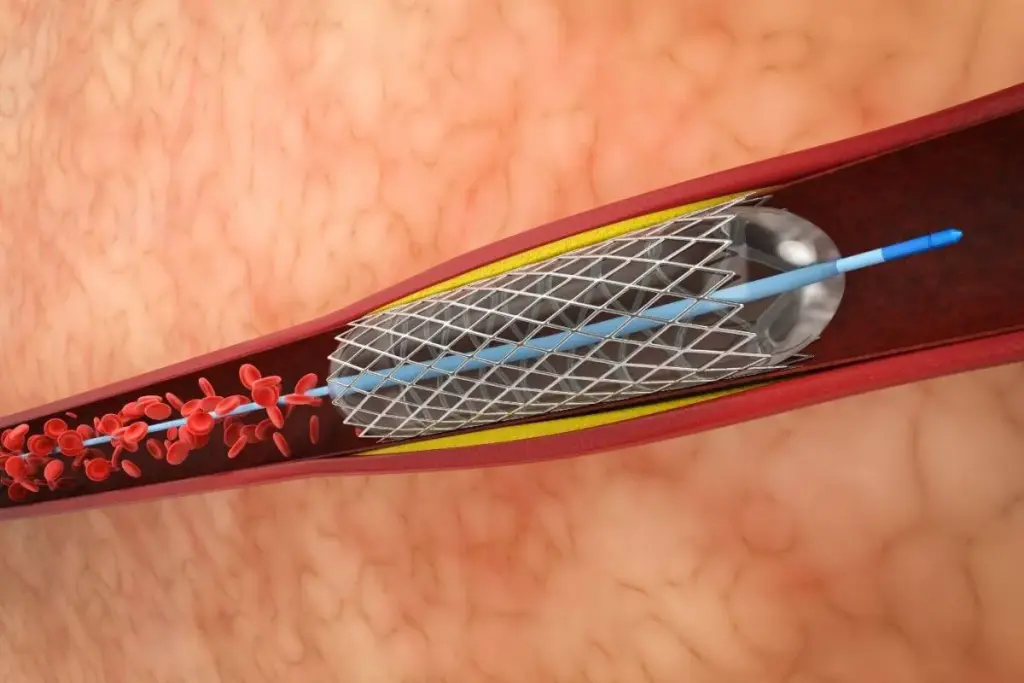
Coronary stents are small, mesh-like tubes used to widen narrowed arteries. They help improve blood flow to the heart. These devices are a key part of treating coronary artery disease, providing a less invasive option than surgery.
Definition and Basic Procedure
A coronary stent is placed during cardiac catheterization. A small incision is made in the groin or arm to reach the blocked artery. A catheter with a balloon and stent is then guided to the blockage.
Once in place, the balloon is inflated to expand the stent. After that, the balloon is deflated and removed, leaving the stent to keep the artery open.
The stent procedure has many benefits. It leads to quicker recovery times than open-heart surgery. It also treats blockages in a less invasive way, improving patient outcomes and lowering the risk of complications.
Types of Stents
There are different types of coronary stents, each for specific needs. The main types include:
- Bare-metal stents: These are the first type of stent, made from metal mesh. They are less used today because of a higher risk of restenosis.
- Drug-eluting stents: These stents release medication to prevent the artery from narrowing again. They are the most popular choice because they reduce restenosis rates.
- Bioresorbable stents: A newer type of stent that dissolves over time. They aim to reduce long-term complications.
Evolution of Stent Technology
Stent technology has made big strides over the years. Early stents had higher rates of restenosis and complications. But, new materials and designs have led to safer and more effective stents.
Today’s stents are more flexible, durable, and body-friendly. This reduces the risk of bad reactions. Stent technology keeps getting better, with ongoing research into new materials and designs.
The Bypass vs Stent Comparison: Key Differences
When looking at treatments for coronary artery disease, knowing the differences between bypass surgery and stent placement is key. Both methods aim to improve blood flow to the heart. Yet, they differ in how they’re done and what happens afterward.
Invasiveness and Surgical Approach
Bypass surgery, or CABG, is a more invasive method. It involves grafting a healthy blood vessel onto a blocked artery. This requires opening the chest for open-heart surgery.
On the other hand, stent placement is less invasive. It involves placing a small mesh tube (stent) in the narrowed artery. This is done through a small puncture in the leg or arm, guided by imaging.
“The invasiveness of bypass surgery is a significant factor that influences the decision-making process,” as noted by cardiovascular specialists. The choice between bypass and stent often depends on the severity and location of the blockage, as well as the patient’s overall health.
Duration of Procedures
The time needed for both procedures differs. Bypass surgery takes longer because it’s more invasive. It can last from 3 to 6 hours, depending on the case’s complexity.
Stent placement, on the other hand, is quicker. It usually takes 30 minutes to an hour. But, preparation and recovery times add to the overall visit duration.
- CABG: 3-6 hours
- Stent Placement: 30 minutes to 1 hour
Immediate Recovery Requirements
The recovery times for both procedures are different. Bypass surgery requires a longer hospital stay, usually 5 to 7 days. This is because patients need close monitoring post-surgery. They also need a more extensive rehabilitation program.
Stent placement, by contrast, allows for same-day discharge or a short overnight stay. Patients can return to normal activities quicker.
The recovery process is a critical aspect of the treatment journey. Knowing these differences helps patients prepare for what’s ahead. The choice between bypass surgery and stent placement is a personal one, based on individual needs and medical considerations.
Bypass Surgery: The Procedure in Detail
Coronary artery bypass grafting (CABG) is a detailed surgery that needs careful planning and execution. It’s a key treatment for heart disease, helping patients feel better and live better lives.
Preparation for Surgery
Before CABG, patients go through tests to check their health and find the best treatment. These tests include cardiac catheterization, stress tests, and imaging studies. Our team talks to patients about the surgery, its risks, and benefits, and answers their questions.
Patients are told to stop certain medicines before surgery. They also can’t eat or drink after midnight the night before. On surgery day, they go to the operating room and get general anesthesia to stay comfortable.
During the Operation
In CABG, the chest is opened to reach the heart. The patient is connected to a heart-lung machine to keep the heart and lungs working. Surgeons then take a healthy blood vessel, usually from the leg or arm, to use as a graft.
The graft is attached to the coronary artery, bypassing the blockage. This is done as needed to improve blood flow to the heart. Often, many grafts are used, depending on the heart disease.
Immediate Post-Operative Care
After surgery, patients go to the ICU for close care. The ICU team watches their vital signs, manages pain, and gives oxygen when needed. Patients usually stay in the ICU for one to two days.
As they recover, patients start to breathe on their own and move a bit. Our team helps with wound care, medicine, and follow-up visits.
Knowing about CABG helps patients prepare for surgery and recovery. This knowledge leads to a better outcome and a better life.
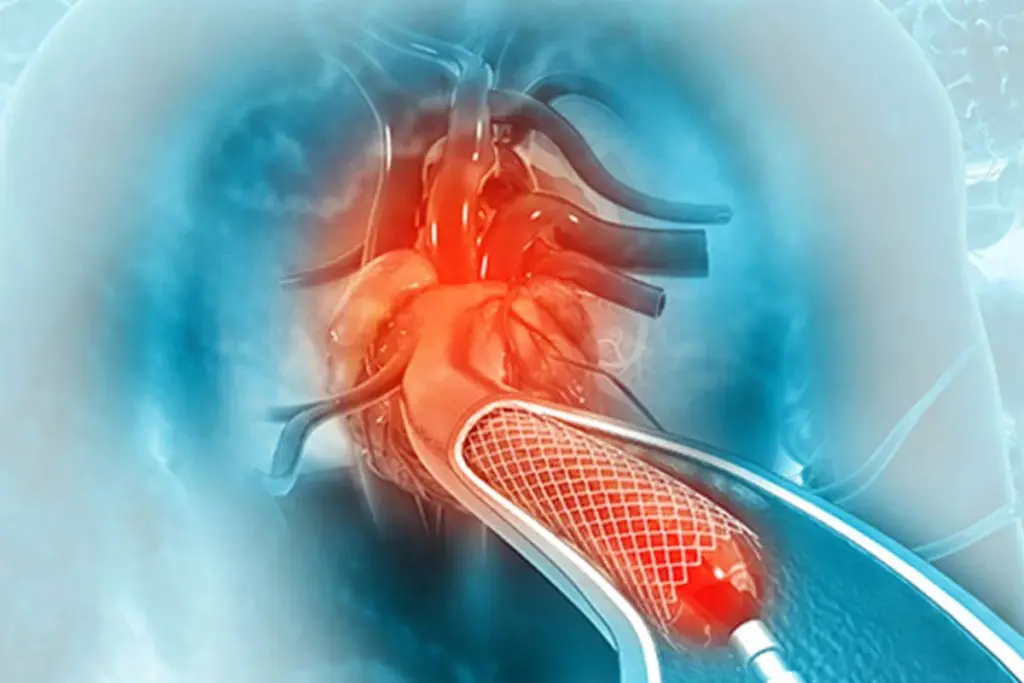
Stent Placement: The Procedure in Detail
Inserting a stent is a key part of treating heart disease. It uses a technique called cardiac catheterization. This method is less invasive and helps restore blood flow to the heart without surgery.
Preparation for Stent Placement
Before the procedure, patients get tested to check their health and artery condition. These tests include blood work, electrocardiograms, and angiograms.
On the day of the procedure, patients get local anesthesia in the groin or arm. They also take medication to relax.
During the Procedure
A catheter with a balloon is inserted through the artery to the blockage. The balloon is then inflated to expand the stent. This keeps the artery open even after the balloon is removed.
Drug-eluting stents release medication to prevent the artery from narrowing again. This has improved the procedure’s success rate.
Immediate Post-Procedure Care
Patients are watched for a few hours after the procedure. Most can go home the same day or the next morning.
To prevent clots, patients take antiplatelet therapy as directed by their doctor.
Benefits of Stent Placement
Stent placement has many advantages. It has a shorter recovery time than CABG and avoids the risks of open-heart surgery.
|
Procedure Aspect |
Stent Placement |
CABG |
|---|---|---|
|
Invasiveness |
Minimally invasive |
Highly invasive |
|
Recovery Time |
Short (days to weeks) |
Long (weeks to months) |
|
Risk of Complications |
Lower |
Higher |
Recovery and Rehabilitation
It’s key to know about recovery if you’re thinking about bypass surgery or stent placement for heart blockages. Each method has its own path to full recovery. This affects how long you stay in the hospital, your short-term recovery, and long-term care.
Hospital Stay Comparison
The time you spend in the hospital is different for bypass surgery and stent placement. Usually, stent placement means a shorter stay than bypass surgery.
|
Procedure |
Typical Hospital Stay |
|---|---|
|
Bypass Surgery |
5-7 days |
|
Stent Placement |
1-2 days |
Short-term Recovery Expectations
Recovery from stent placement is usually faster. You can start normal activities in a few days to a week. But, bypass surgery takes longer, often needing several weeks to get back to full strength.
Long-term Rehabilitation Requirements
Both procedures need lifestyle changes for long-term care. This includes diet, exercise, and taking your meds as directed. But, how intense and long this care is can vary.
Return to Normal Activities
How fast you get back to normal varies by procedure. Stent placement usually lets you get back to normal in a week or two. Bypass surgery might take 6 to 12 weeks.
Every patient’s recovery is different. Things like your health, age, and other health issues can affect how you recover. Our healthcare team offers personalized help and support every step of the way.
Effectiveness for Different Types of Blockages
When treating coronary artery disease, the choice between bypass surgery and stent placement depends on the blockage type and severity. Different heart disease interventions are best for different conditions.
Single Vessel Disease
For single vessel disease, where one artery is blocked, both methods can work. But, stent placement is often preferred because it’s less invasive and has a quicker recovery. Studies show stents have high success rates with lower risks than bypass surgery for single vessel disease.
“The choice between stent placement and bypass surgery for single vessel disease should be based on the patient’s overall health, the specific characteristics of the blockage, and patient preference,” according to recent clinical guidelines.
Multi-Vessel Disease
In multi-vessel disease, where more than one artery is blocked, bypass surgery is often more effective. It can treat multiple blockages at once, providing a more complete solution. Stent placement can also be used, but treating multiple arteries increases the risk of complications.
- Bypass surgery can treat multiple blockages simultaneously.
- Stent placement may require multiple procedures.
- The choice between the two should consider the patient’s overall health and the extent of the disease.
Left Main Coronary Artery Disease
Left main coronary artery disease is a serious condition where the main artery supplying blood to the heart is blocked. Bypass surgery has traditionally been the preferred treatment for left main coronary artery disease. It offers a more durable long-term solution. Recent studies suggest stent placement can be an effective alternative for certain patients, like those at high risk for surgery or with specific anatomical characteristics.
The decision between bypass surgery and stent placement for left main coronary artery disease should be made on a case-by-case basis. It depends on the patient’s health status, the complexity of the blockage, and other relevant factors.
Longevity and Durability of Results
When it comes to treating coronary artery disease, the long-term success of treatments is key. Both coronary artery bypass grafting (CABG) and percutaneous coronary intervention (PCI) with stenting are options. Knowing how well these treatments work over time helps patients and doctors make better choices.
Restenosis Rates
Restenosis, or the arteries getting narrow again, is a big concern. It affects how well treatments like CABG and stenting work. CABG often has lower restenosis rates, which is good for patients with complex disease.
A study in the Journal of the American College of Cardiology found CABG patients had less restenosis at 5 years. This compared to those who got PCI with drug-eluting stents.
Need for Repeat Procedures
How often patients need more procedures is another important factor. PCI patients often need more procedures because of restenosis or new disease. This is a drawback of PCI.
A meta-analysis showed CABG patients needed fewer repeat procedures over time. This is a big advantage of CABG.
Long-term Survival Statistics
Survival over the long term is a critical measure for both CABG and PCI. Studies have compared how these treatments affect survival.
|
Procedure |
1-Year Survival Rate |
5-Year Survival Rate |
|---|---|---|
|
CABG |
95% |
80% |
|
PCI with Stenting |
96% |
75% |
The table shows both treatments have high survival rates in the short term. But CABG seems to offer better long-term survival for some patients, like those with complex disease.
Every patient is different, and the choice between CABG and PCI depends on many factors. These include the disease’s extent, overall health, and personal preferences.
Risks and Complications
When looking at treatments for coronary artery disease, it’s key to know the risks of bypass surgery and stent placement. Both methods are effective but have their own complications. These can affect how well a patient does after treatment.
Bypass Surgery Risks
Coronary artery bypass grafting (CABG) is a big surgery. It’s used to improve blood flow to the heart by adding bypasses to the arteries. While safe, CABG has risks like:
- Infection at the surgical site
- Bleeding during or after surgery
- Adverse reactions to anesthesia
- Stroke or heart attack during surgery
- Graft failure
To lower these risks, choosing the right patient and using precise surgical methods are key. New techniques like off-pump CABG and minimally invasive CABG have also cut down on risks.
Stent Procedure Risks
Stent placement, or PCI, is less invasive than CABG. Yet, it has its own risks. Complications can include:
- Bleeding at the catheter site
- Allergic reactions to the contrast dye used during the procedure
- Damage to the coronary arteries
- Restenosis (re-narrowing of the stented artery)
- Stent thrombosis (clot formation within the stent)
These risks can be lessened by choosing the right patient, using the right stent size, and following up with the right medication. This includes antiplatelet therapy.
|
Complication |
Bypass Surgery (CABG) |
Stent Placement (PCI) |
|---|---|---|
|
Infection |
Common |
Rare |
|
Bleeding |
Possible during and after surgery |
Possible at catheter site |
|
Restenosis |
Less common due to grafting |
Possible, specially with bare-metal stents |
|
Stroke/Heart Attack |
Possible during surgery |
Rare during procedure |
It’s important for both doctors and patients to understand these risks and complications. This helps in making the right choice between bypass surgery and stent placement. By considering the benefits and risks, patients can make informed decisions about their treatment.
Medication Requirements
After heart surgery like bypass or stent placement, patients need ongoing medicine. This helps manage their condition well.
Post-Bypass Medications
After coronary artery bypass grafting (CABG), patients get many medicines. These are to prevent problems and help them heal. Some of these include:
- Antiplatelet agents to stop blood clots
- Beta-blockers to slow heart rate and lower blood pressure
- Statins to lower cholesterol
- ACE inhibitors to control blood pressure and heart function
Post-Stent Medications
Patients with stents also need medicine to stop clots and prevent blockages. Their medicine list might include:
- Dual antiplatelet therapy (DAPT) with aspirin and a P2Y12 inhibitor to stop clots
- Statins to keep plaque stable and lower blockage risk
Duration of Medication Therapy
How long patients need these medicines varies. It depends on their health, the stent type, and more. Usually, those with drug-eluting stents need DAPT for 6 to 12 months. Patients with bare-metal stents might need it for less time.
To better understand the medication needs, let’s look at a comparison table:
|
Medication Type |
Post-Bypass |
Post-Stent |
|---|---|---|
|
Antiplatelet Agents |
Yes |
Yes (DAPT) |
|
Beta-blockers |
Yes |
Often Recommended |
|
Statins |
Yes |
Yes |
|
ACE Inhibitors |
Yes |
Often Recommended |
Knowing the medicines needed after heart surgery is key. It helps patients get better and lowers the chance of more problems. Taking the medicines as directed can greatly improve life quality and reduce the need for more treatments.
Cost Comparison and Insurance Considerations
Coronary artery blockage treatments like bypass surgery and stent placement have different costs. It’s important for patients and healthcare providers to understand these costs. This knowledge helps in making informed decisions about heart health.
Initial Procedure Costs
The costs of bypass surgery and stent placement vary. Bypass surgery is more expensive upfront because it’s a bigger procedure. It requires hospital stay, a surgical team, and post-operative care. Stent placement is cheaper at first because it’s less invasive and done in a lab.
Several factors affect the initial costs:
- Hospital Stay: Longer stays for bypass surgery increase costs.
- Surgical Team: The team’s expertise and fees for bypass surgery are higher.
- Equipment and Supplies: The cost of stents and materials can vary.
Long-term Follow-up Costs
Long-term costs are also important. Bypass surgery may need more rehabilitation and follow-up, raising long-term costs. Stent patients might need ongoing medication, adding to their expenses.
Key long-term costs include:
- Rehabilitation and physical therapy needs
- Costs of follow-up appointments and tests
- Ongoing medication costs
Insurance Coverage in the United States
Insurance for bypass surgery and stent placement varies in the U.S. Both are usually covered, but coverage can differ. Knowing your insurance is key to understanding your costs.
Insurance factors include:
- Policy Details: Deductibles, copays, and coinsurance matter.
- Pre-approval Requirements: Some procedures need approval.
- Network Providers: Using in-network providers can save money.
In conclusion, comparing bypass surgery and stent placement costs requires looking at both initial and long-term costs. Insurance coverage also plays a big role. This approach helps patients make better choices for their heart health.
Hybrid Approaches: Combining Bypass and Stents
In the world of heart care, new ways to treat heart disease are being explored. Hybrid methods mix bypass surgery and stent placement. This mix offers a custom plan for complex heart disease.
When Hybrid Procedures Are Recommended
Hybrid treatments are for patients with heart disease in many arteries. Some parts need bypass surgery, while others are better for stents. The choice of hybrid treatment depends on each patient’s health and disease complexity.
Several factors decide if a hybrid procedure is right. These include:
- The complexity of the heart’s blood vessels
- Previous heart surgeries or stent placements
- Risks of surgery or stent placement
- What the patient wants and values
Benefits of Combined Approaches
Hybrid treatments have many advantages. They include:
- Lower risk of complications: Hybrid treatments are less invasive, reducing risks.
- Shorter recovery times: Patients might leave the hospital sooner and recover faster.
- More tailored care: Doctors can mix the best of surgery and stents for each patient.
A leading cardiologist says, “Hybrid treatments are a big step forward. They offer a safer, more personalized way to treat heart disease.” This focus on the individual is a key part of modern heart care.
Future Directions in Hybrid Interventions
Hybrid heart treatments are getting better fast. Research is improving how to choose patients, making procedures better, and boosting long-term results. As technology improves, we’ll see more patients benefit from these treatments.
Future developments include:
- New stents and surgical methods
- Better imaging and diagnostic tools
- More use of minimally invasive surgery with stents
Decision-Making Factors for Doctors and Patients
Choosing between bypass surgery and stenting depends on many things. These include medical needs, lifestyle, and what the patient wants.
Medical Considerations
Doctors look at several things when deciding between surgery and stenting. They consider how bad the heart disease is, if the patient has diabetes, and their overall health.
For example, people with severe heart disease or diabetes might do better with bypass surgery. This is because it can lower the risk of serious heart problems in the long run.
|
Factor |
Bypass Surgery |
Stent Placement |
|---|---|---|
|
Complex Multi-Vessel Disease |
Often recommended |
May be considered in some cases |
|
Presence of Diabetes |
May offer long-term benefits |
Effective but may require closer monitoring |
|
Patient’s Overall Health |
Requires thorough evaluation |
Less invasive, suitable for some high-risk patients |
Lifestyle Factors
Lifestyle choices also matter. Things like how active the patient is, if they smoke, and if they take their medicine as told. For instance, a smoker might get different advice than a non-smoker.
Lifestyle changes are key for both surgery and stenting to work well. Patients should eat well, exercise, and manage stress to help their heart health.
Patient Preferences and Values
What the patient wants and values is also important. Some might choose bypass surgery for its long-term benefits. Others might prefer stenting because it’s less invasive.
Shared Decision-Making Process
The shared decision-making process is all about working together. Doctors and patients make decisions together. This way, patients know all about their options, including the good and bad sides.
We think this approach helps patients understand their situation better. It also lets them make choices that fit their own values and needs.
Quality of Life After Intervention
It’s important to understand how bypass and stent procedures affect quality of life. Both patients and healthcare providers need to look at the long-term effects. This includes how these treatments change daily life.
Physical Limitations
Patients may face physical challenges after bypass surgery or stent placement. Some regain strength quickly, while others take longer. Bypass surgery can lead to more initial limitations because it’s more invasive. But, new surgical methods have improved outcomes and recovery times.
Stent placement is less invasive, leading to shorter hospital stays and faster recovery. Yet, the choice between these options depends on the patient’s specific condition and coronary artery blockage extent.
Psychological Impact
The psychological effects of these interventions are also key to quality of life. Anxiety and depression are common. But, successful treatments can greatly improve mental health and overall well-being.
Support systems, like counseling and rehabilitation, are essential. They help patients deal with the emotional side of treatment. This way, healthcare providers can improve the heart health comparison between treatments.
Patient Satisfaction Surveys
Patient satisfaction surveys offer insights into the real effects of bypass surgery and stent placement. They cover the procedure, post-operative care, and long-term results.
By looking at patient satisfaction data, healthcare professionals can see what works best. This helps make decisions that meet each patient’s needs and preferences.
In summary, the quality of life after treatment depends on many factors. These include the procedure type, patient characteristics, and post-procedure care. By considering these, we can offer better care that enhances patients’ lives in meaningful ways.
Conclusion: Is Bypass Better Than Stents?
Our detailed look at bypass vs stent has shown the challenges in choosing between CABG surgery and stent placement. Both have their good points and downsides. The right choice depends on the patient’s specific needs and health.
Looking at stent vs bypass surgery results, CABG is often better for those with many blocked arteries. It gives longer-lasting benefits. But, stents are usually the go-to for single-blocked arteries or those who can’t handle surgery well.
In the end, picking between bypass surgery and stents needs careful thought. It’s about the disease’s severity, the patient’s health, and what they prefer. Knowing the differences helps patients make better choices for their care.
We think it’s key for patients, cardiologists, and surgeons to work together. This teamwork helps find the best treatment. Together, we can make life better for those with heart disease.
FAQ
What is the main difference between bypass surgery and stent placement?
Bypass surgery creates a new path around a blocked artery. Stent placement keeps the artery open with a small mesh tube.
Which procedure is more invasive, bypass surgery or stent placement?
Bypass surgery is more invasive, needing to open the chest. Stent placement is less invasive, done through a small leg or arm puncture.
How long does recovery take for bypass surgery compared to stent placement?
Bypass surgery recovery takes weeks to months. Stent placement recovery is faster, usually a few days to a week.
Are there different types of stents available?
Yes, there are bare-metal stents and drug-eluting stents. Each has its own benefits and risks.
What are the risks associated with bypass surgery?
Bypass surgery risks include infection, bleeding, stroke, and heart attack.
What are the risks associated with stent placement?
Stent placement risks include bleeding, clot formation, and restenosis (re-narrowing of the artery).
How do the costs of bypass surgery and stent placement compare?
Bypass surgery costs more due to longer hospital stays and recovery times.
Will I need to take medications after bypass surgery or stent placement?
Yes, you’ll need to take medications after both procedures. They help manage heart health and prevent clotting.
Can I undergo both bypass surgery and stent placement?
Sometimes, a hybrid approach combining both may be recommended. This depends on your condition and disease complexity.
How do lifestyle factors influence the choice between bypass surgery and stent placement?
Lifestyle factors, like health, activity level, and personal preferences, are important in choosing between the two.
What is the long-term effectiveness of bypass surgery compared to stent placement?
Bypass surgery is often more durable for complex cases. Stent placement is effective for less complex disease.
How does the type of coronary artery disease influence the choice between bypass surgery and stent placement?
The type and complexity of coronary artery disease affect the choice. Single vessel disease, multi-vessel disease, or left main disease are examples.
Reference
Centers for Disease Control and Prevention. Evidence-Based Medical Insight. Retrieved from https://www.cdc.gov/heart-disease/about/coronary-artery-disease.html




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News




























