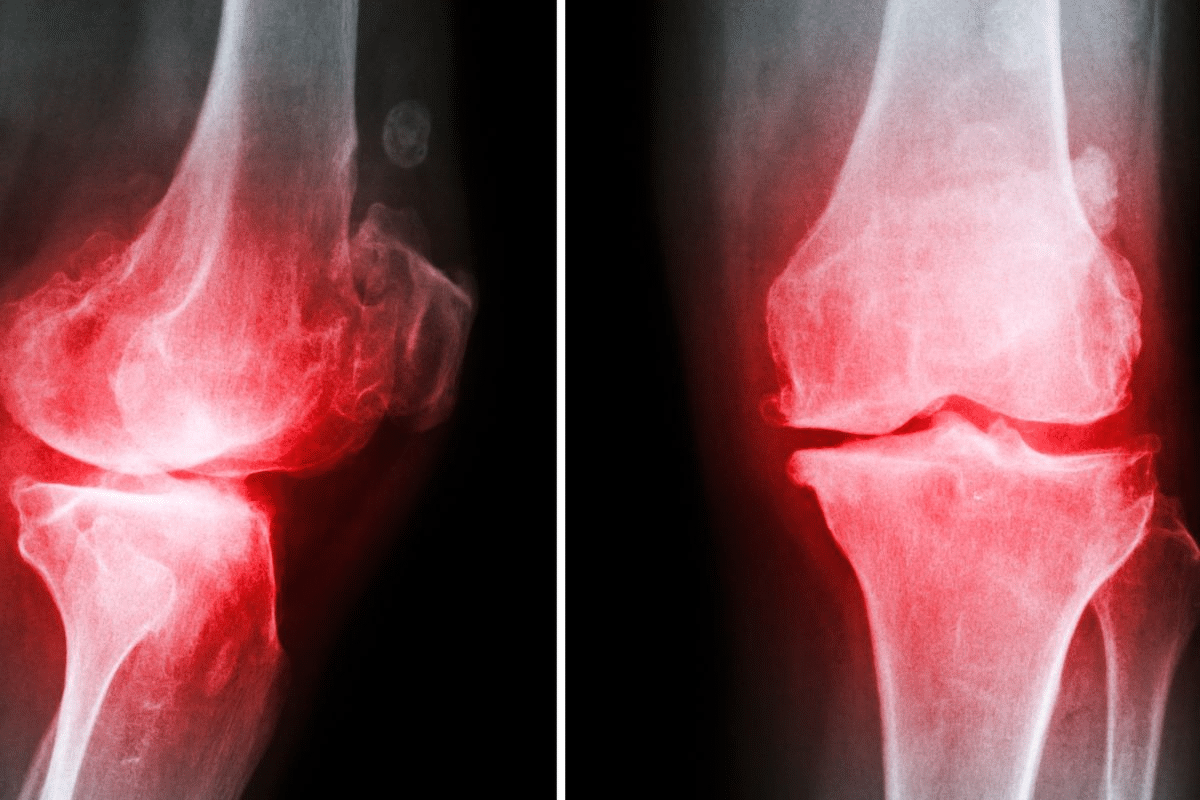
At Liv Hospital, we understand the importance of chondrocalcinosis of the knee. It’s a condition where calcium pyrophosphate dihydrate (CPPD) crystals build up in the knee cartilage chondrocalcinosis knee.
This condition, also called calcium pyrophosphate deposition (CPD) disease, can harm the cartilage and cause inflammation. Advanced imaging and clinical assessment are key to diagnosing it right.
Our team of experts uses the latest diagnostic methods to tackle this condition. By knowing its causes and symptoms, we offer full care to our patients.
Key Takeaways
- Chondrocalcinosis of the knee involves CPPD crystal deposition in the cartilage.
- Advanced imaging is essential for diagnosis.
- Proper diagnostic recognition is key for effective management.
- Our team at Liv Hospital uses state-of-the-art diagnostic protocols.
- Comprehensive care is provided based on the causes and symptoms identified.
Understanding Chondrocalcinosis of the Knee
Chondrocalcinosis of the knee is a condition where calcium pyrophosphate dihydrate (CPPD) crystals build up in the joint. This affects the menisci, which are key for the knee’s stability and function.
Definition and Basic Pathophysiology
Chondrocalcinosis is when CPPD crystals form in the knee’s cartilage and tissues. The meniscus, a cartilage in the knee, is often affected. This can lead to inflammation and damage in the joint over time.
The causes of chondrocalcinosis are complex. They include age, metabolic disorders, and genetics. CPPD crystals form when the balance of crystal formation and dissolution is off.
Prevalence and Demographics
Chondrocalcinosis is found in 5-15% of people, more in older adults. In Europe and the U.S., about 4-7% of adults have CPPD crystal deposition disease.
Age is a big risk factor, with more cases in older people. Metabolic disorders and genetics also play a part in who gets chondrocalcinosis.
Knowing who gets chondrocalcinosis helps doctors diagnose and treat it better. We’ll look into more details about this condition next.
The Anatomy of Knee Menisci and Cartilage
It’s important to know about the knee menisci and cartilage to understand chondrocalcinosis. The knee has bones, cartilage, and menisci. They all work together to help us move and absorb shock.
Structure of the Knee Joint
The knee is made up of three bones: the femur, tibia, and patella. The menisci, two cartilage pieces, sit between the femur and tibia. They are key to the knee’s function. The menisci are made of fibrocartilage, which is tough and elastic.
The knee also has ligaments for stability and to help it move. The cartilage on the bones’ ends reduces friction, making movement smooth.
Function of Menisci in the Knee
The menisci are essential for the knee’s proper working. They do several important things:
- Absorbing shock during weight-bearing activities
- Stabilizing the knee during movement
- Facilitating smooth movement by reducing friction between the bones
- Distributing load evenly across the joint
When the menisci get calcified, like in chondrocalcinosis, these roles can be affected. This can cause symptoms and harm the knee’s health.
Calcium Pyrophosphate Dihydrate (CPPD) Crystal Deposition
It’s key to know about CPPD crystal deposition to treat chondrocalcinosis well. CPPD disease makes calcium pyrophosphate dihydrate crystals build up in joint cartilage. This leads to inflammation and can cause long-term damage to joints.
The Nature of CPPD Crystals
CPPD crystals form when calcium pyrophosphate dihydrate abnormally deposits in joint cartilage. They can cause a lot of pain and swelling, making joints feel like those with arthritis.
Many things can lead to CPPD crystals, like getting older, metabolic issues, and genetics. Knowing the cause is important for managing it.
How CPPD Crystals Form in Joint Tissues
CPPD crystals form due to many factors, including changes in the joint’s chemistry. Important factors include:
- Abnormalities in calcium and pyrophosphate metabolism
- Degenerative changes in the joint cartilage
- Presence of certain metabolic disorders
CPPD crystals can settle in different parts of joints, like cartilage, synovium, and tendons. This can cause symptoms from no pain at all to sudden, severe inflammation, known as pseudogout.
Knowing these details helps in creating better treatment plans.
Common Locations for Chondrocalcinosis Knee
Chondrocalcinosis of the knee is caused by calcium pyrophosphate dihydrate (CPPD) crystals. These crystals often settle in the menisci. This condition can make knee joint symptoms worse and affect your quality of life.
Medial and Lateral Menisci
The menisci in the knee joint can get affected by chondrocalcinosis. Both the medial and lateral menisci are common places for CPPD crystals to form. The medial meniscus is often injured and can also have chondrocalcinosis.
The lateral meniscus can be affected too, but less often than the medial meniscus.
Other Cartilaginous Structures Affected
Other parts of the knee can also be affected by chondrocalcinosis. The articular cartilage on the ends of the bones in the knee can have CPPD crystals. This can cause degenerative changes and pain in the joint.
Chondrocalcinosis can affect many parts of the knee joint. Knowing where CPPD crystals usually form is key to diagnosing and treating the condition.
Causes and Risk Factors of Meniscal Calcification
It’s important to know what causes meniscal calcification. This helps us find who’s at risk and how to prevent it. Meniscal calcification often comes from metabolic disorders, injuries, or wear and tear.
Age-Related Factors
Age is a big risk factor for meniscal calcification. As we get older, our joints wear out more. This makes it more likely to get calcification in the menisci.
Studies show that more people over 60 get chondrocalcinosis. It’s a common problem in the elderly.
Metabolic Disorders
Some metabolic disorders raise the risk of meniscal calcification. Hemochromatosis and hyperparathyroidism are examples. These conditions can cause calcium pyrophosphate dihydrate (CPPD) crystals to build up in the joint.
Genetic Predisposition
Genetics also play a part in meniscal calcification. Some people are more likely to get chondrocalcinosis because of their genes. Research has found certain genetic markers that increase the risk of CPPD crystal deposition.
Trauma and Joint Degeneration
Knee injuries and degenerative changes can also cause meniscal calcification. Injuries or repetitive stress can lead to CPPD crystals and calcification. Degenerative diseases like osteoarthritis also raise the risk.
|
Risk Factor |
Description |
Impact on Meniscal Calcification |
|---|---|---|
|
Age |
Increased wear and tear on the joint |
Higher prevalence in elderly populations |
|
Metabolic Disorders |
Conditions like hemochromatosis and hyperparathyroidism |
Increased CPPD crystal deposition |
|
Genetic Predisposition |
Genetic markers associated with CPPD deposition |
Increased risk of chondrocalcinosis |
|
Trauma and Joint Degeneration |
Previous injuries or degenerative joint diseases |
Formation of CPPD crystals and calcification |
Knowing these risk factors helps doctors identify who’s at risk. They can then plan how to prevent and manage meniscal calcification.
Clinical Presentation and Symptoms
Knowing the symptoms of chondrocalcinosis is key for the right diagnosis and treatment. This condition can show up in different ways. It’s important to know how it can present itself.
Asymptomatic Presentation
Many people with chondrocalcinosis don’t show any symptoms. They might find out they have it by chance during tests for something else.
Acute Attacks (Pseudogout)
Some people with chondrocalcinosis get sudden, severe joint pain. This is called pseudogout. It can happen for many reasons, like an injury or surgery. Pseudogout episodes are marked by:
- Severe joint pain
- Swelling and redness around the affected joint
- Warmth to the touch
- Limited range of motion
These episodes can really hurt and often need doctor help to manage the pain and swelling.
Chronic Joint Inflammation
Some people with chondrocalcinosis also have ongoing joint inflammation. This can cause long-term pain and stiffness, mainly in the affected joints. This inflammation can also make joints worse over time.
The symptoms of chondrocalcinosis can really affect someone’s life. So, it’s important to see a doctor if symptoms don’t get better or get worse.
|
Symptom |
Acute Attack (Pseudogout) |
Chronic Joint Inflammation |
|---|---|---|
|
Joint Pain |
Severe, sudden onset |
Persistent, varying intensity |
|
Swelling |
Significant swelling |
Mild to moderate swelling |
|
Duration |
Typically resolves within days to weeks |
Can persist for months or longer |
Managing chondrocalcinosis symptoms needs a full plan, including medicine and lifestyle changes. Knowing how chondrocalcinosis can show up helps doctors give better care and support.
Diagnostic Methods for Chondrocalcinosis of the Menisci
Diagnosing chondrocalcinosis of the menisci requires a detailed approach. We use clinical assessment and advanced imaging techniques. This helps us accurately identify and manage the condition.
Clinical Assessment
The first step is a thorough clinical assessment. We look at the patient’s medical history for signs of joint pain, swelling, or limited mobility. A physical exam checks joint stability and detects abnormalities.
We also consider the patient’s age and any metabolic disorders. Older adults and those with hyperparathyroidism are more at risk.
Radiographic Evaluation
X-rays are key in diagnosing chondrocalcinosis. We look for calcifications in the menisci and other joint structures. X-rays show calcium pyrophosphate dihydrate (CPPD) crystals, a sign of chondrocalcinosis.
|
Radiographic Feature |
Description |
|---|---|
|
Calcification |
Presence of calcium deposits in the menisci or articular cartilage |
|
Joint Space Narrowing |
Reduction in the space between the bones, indicating joint degeneration |
|
Osteophytes |
Bony growths that can occur in response to joint degeneration |
Advanced Imaging Techniques
Ultrasound and MRI provide detailed information about chondrocalcinosis. Ultrasound detects CPPD crystals and assesses joint inflammation. MRI gives a detailed view of the joint structures, including the menisci and cartilage.
We often use MRI to evaluate the severity of chondrocalcinosis. It helps us plan the best treatment. MRI can also identify other conditions, like meniscal tears or osteoarthritis, which affect treatment.
By combining clinical assessment, radiographic evaluation, and advanced imaging, we can accurately diagnose chondrocalcinosis. This allows us to develop an effective treatment plan for each patient.
Laboratory Testing and Joint Fluid Analysis
To confirm chondrocalcinosis, healthcare providers use laboratory tests and joint fluid exams. These tools are key to identifying the condition and its causes.
Synovial Fluid Examination
Synovial fluid examination is a key diagnostic method for chondrocalcinosis. It involves analyzing fluid from the affected joint. This helps find calcium pyrophosphate dihydrate (CPPD) crystals, which are signs of the condition.
The process includes:
- Aspirating synovial fluid from the knee joint
- Examining the fluid under a microscope for CPPD crystals
- Using polarized light microscopy to identify the crystals’ characteristic birefringence
This test is vital. It confirms the presence of CPPD crystals, which sets chondrocalcinosis apart from other arthritis types.
Blood Tests for Associated Conditions
Blood tests are also important for diagnosing chondrocalcinosis. They help find metabolic disorders that may cause the condition.
Common blood tests include:
- Tests for serum calcium and phosphate levels
- Assessments of thyroid function
- Measurements of serum magnesium
- Tests for iron overload (e.g., ferritin levels)
These tests help doctors understand what’s causing chondrocalcinosis in a patient. This guides treatment choices.
A medical expert notes, “Laboratory testing, including joint fluid analysis, is essential for accurately diagnosing chondrocalcinosis and developing an effective treatment plan.”
Treatment Options for Knee Chondrocalcinosis
Managing knee chondrocalcinosis requires a mix of treatments. This includes handling acute attacks, long-term care, and sometimes surgery. The aim is to ease symptoms, enhance life quality, and slow disease growth.
Managing Acute Attacks
Acute chondrocalcinosis, or pseudogout, needs quick action to lessen pain and swelling. Nonsteroidal anti-inflammatory drugs (NSAIDs) are usually the first choice. For severe cases, corticosteroid injections into the joint can offer fast relief.
For those who can’t take NSAIDs or have reasons not to, colchicine is an option. It works best when started early in an attack.
Long-term Treatment Strategies
Long-term care aims to reduce attack frequency and joint damage. It includes lifestyle changes like staying at a healthy weight and doing gentle exercises to keep joints moving.
Medications like low-dose colchicine can prevent attacks. Also, drugs that lower uric acid, like allopurinol or febuxostat, can help, even though they’re mainly for gout.
Surgical Interventions
When chondrocalcinosis causes a lot of joint damage or fails to respond to other treatments, surgery might be needed. Arthroscopic surgery can remove crystals and fix cartilage. For severe cases, joint replacement surgery may be the best option to improve function and reduce pain.
It’s important for patients to talk to their healthcare provider to find the right treatment. Everyone’s needs and how they react to treatment can be different.
Conclusion: Prognosis and Living with Chondrocalcinosis
It’s key for patients to understand their prognosis and how to manage chondrocalcinosis. This chronic condition can be managed with the right approach. Making lifestyle changes and getting proper treatment can greatly improve life quality.
The outcome of chondrocalcinosis depends on its severity and any other health issues. A good management plan includes medication, lifestyle adjustments, and sometimes surgery. Working with healthcare providers helps create a tailored plan to control symptoms and slow the disease.
For those living with chondrocalcinosis, ongoing care is vital. Keeping joints mobile and preventing complications is important. This can be done by staying active, keeping a healthy weight, and managing other health conditions.
With the right care, people with chondrocalcinosis can live active and meaningful lives. It’s important for patients and healthcare providers to work together. This teamwork leads to the best outcomes.
FAQ
What is chondrocalcinosis of the knee?
Chondrocalcinosis of the knee is a condition where calcium pyrophosphate dihydrate (CPPD) crystals build up in the cartilage. This can cause inflammation and damage to the cartilage in the knee joint.
How is chondrocalcinosis diagnosed?
Doctors use X-rays, clinical exams, and lab tests to diagnose chondrocalcinosis. These tests include looking at the fluid in the joint and blood tests for related conditions.
What are the symptoms of chondrocalcinosis?
Symptoms can vary. Some people may not feel any pain, while others may have sudden, severe pain like gout. Others may have ongoing joint pain.
What are the common locations for chondrocalcinosis in the knee?
It often affects the menisci on the sides of the knee. It can also affect other cartilage in the joint.
What are the risk factors for developing meniscal calcification?
Risk factors include getting older, metabolic disorders, family history, and injuries or wear and tear on the joint.
How is chondrocalcinosis of the menisci treated?
Treatment depends on the severity. It can include managing sudden attacks, long-term care, and surgery if needed.
Can chondrocalcinosis be managed without surgery?
Yes, many cases are treated without surgery. This includes medication for sudden attacks and long-term plans to reduce symptoms and slow the disease.
What is the role of radiographic evaluation in diagnosing chondrocalcinosis?
X-rays are key to finding CPPD crystals in the cartilage. This is a main sign of chondrocalcinosis.
How does age affect the prevalence of chondrocalcinosis?
Chondrocalcinosis is more common with age. It’s more common in older people.
What is the significance of CPPD crystals in chondrocalcinosis?
CPPD crystals cause inflammation and damage to the cartilage. Their presence is a key part of the condition’s cause.
How does chondrocalcinosis affect the quality of life?
It can greatly affect quality of life, causing chronic pain and inflammation. But, with the right treatment plan, outcomes can improve.
References
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10040153/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News






























