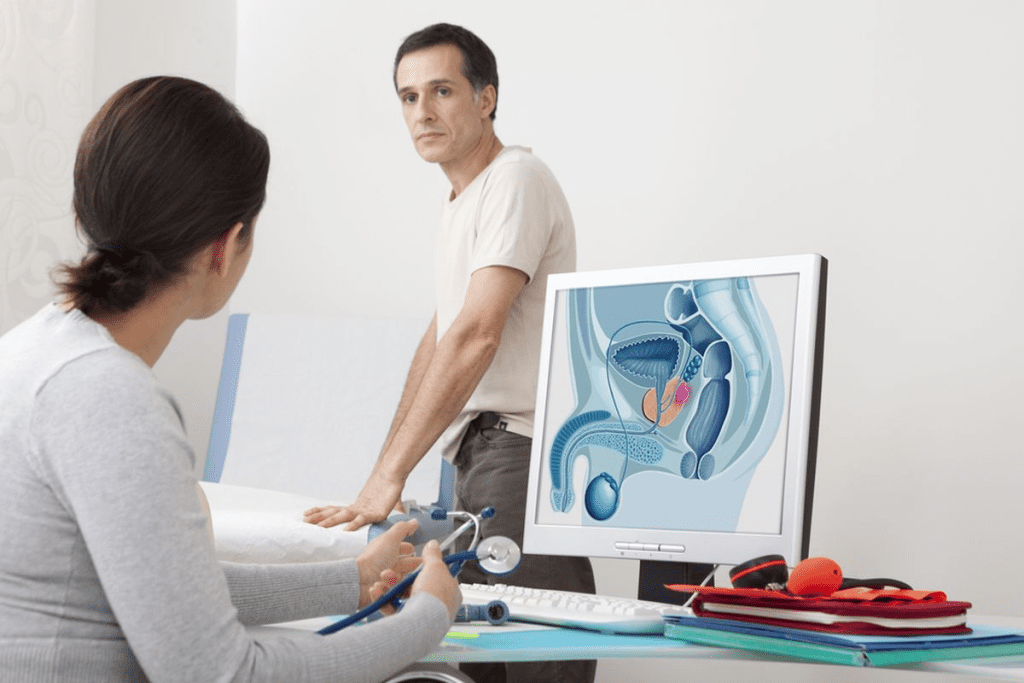
Did you know that nearly 1 in 8 men will be diagnosed with prostate cancer at some point in their lives? The decision to have prostate removal surgery is complex. It involves weighing the benefits against the risks.
When you’re diagnosed with prostate cancer, you might think removing the cancerous prostate right away is best. But, radical prostatectomy, the surgery to remove the prostate, has its own risks and complications.
It’s important to understand these risks before making a decision. While surgery can be effective, it’s not the only option. The chance of complications must be considered.
Key Takeaways
- Prostate cancer is a common diagnosis among men, affecting nearly 1 in 8.
- The decision to undergo surgery should be based on a thorough understanding of the risks and benefits.
- Radical prostatectomy is a major surgery with possible complications.
- Immediate removal of the prostate is not always necessary.
- Alternative treatment options should be considered.
The Nature of Prostate Cancer
Prostate cancer comes in many types, from slow-growing to aggressive. Knowing the exact type of cancer a person has is key to picking the right treatment.
Different Types and Grades of Prostate Cancer
Doctors use the Gleason score to classify prostate cancer. This score ranges from 2 to 10, with higher scores meaning a more aggressive cancer. Low-grade prostate cancers have a score of 6 or less. On the other hand, high-grade cancers score 8 or higher.
The type and grade of cancer affect treatment choices. For example, slow-growing prostate cancers might not need treatment right away. But, more aggressive cancers need quick and strong treatments.
The Natural Progression of Prostate Cancer
How prostate cancer grows can vary a lot. Some cancers grow slowly and don’t cause symptoms or affect life expectancy, while others grow fast and can spread to other parts of the body. Knowing how cancer progresses helps in making treatment decisions, as factors like age, overall health, and cancer stage all matter in choosing the best approach. For some men, active surveillance is a good option, meaning the cancer is watched closely with tests and exams without immediate treatment. However, when surgery is needed, understanding prostate removal surgery risks is crucial before deciding on the best course of action.
Why Immediate Removal Isn’t Always Necessary
Not every prostate cancer case needs the prostate gland removed right away. The choice to remove the prostate is complex. It depends on the cancer type, grade, and the patient’s health and life expectancy.
The Concept of Clinically Insignificant Cancer
The need for immediate prostate removal often hinges on clinically insignificant cancer. This means tumors that won’t cause symptoms or shorten a man’s life. Many men with prostate cancer have tumors that are clinically insignificant.
Spotting clinically insignificant cancer is key to avoiding unnecessary treatments. New tests like multiparametric MRI and genomic testing help doctors find men who can skip surgery.
Age and Life Expectancy Considerations
Age and life expectancy are big factors in treating prostate cancer. Older men or those with a short life span might not need aggressive treatment. Their cancer might not grow much before they pass away.
For men over 40, thinking about prostate health is more important. Research shows that men with less than 10-15 years to live might not need to treat low-risk prostate cancer right away. Instead, active surveillance or watchful waiting could be better options.
It’s vital to weigh the risks and benefits of prostate removal surgery. By looking at the cancer’s aggressiveness, the patient’s age, and health, men can make smart choices about their treatment.
Understanding Prostate Removal Surgery Risks

It’s important for patients with prostate cancer to know about the risks of prostate removal surgery. This surgery, also known as a prostatectomy, is a big deal. Like all surgeries, it can have complications.
Short-term Surgical Complications
Right after surgery, patients might face issues like infection, bleeding, or reactions to anesthesia. These problems are usually handled by doctors. But, they can change based on the patient’s health and the surgery details.
Common short-term complications:
- Infection
- Bleeding or hemorrhage
- Anesthesia reactions
- Blood clots
Long-term Health Implications
Long-term effects of prostate removal surgery can really impact a patient’s life. Issues like urinary incontinence and erectile dysfunction are common. These can affect how well a patient lives day to day.
| Complication | Description | Potential Impact |
| Urinary Incontinence | Involuntary leakage of urine | Affects daily activities and quality of life |
| Erectile Dysfunction | Inability to achieve or maintain an erection | Impacts sexual function and relationship dynamics |
Knowing about these risks helps patients make better choices about surgery. It’s key to talk to a doctor about these possible problems. This way, patients can understand how they might be affected.
Urinary Incontinence After Prostate Surgery
Urinary incontinence is a big worry for men after prostate surgery. It means they can’t control their bladder, leading to urine leaks. How much it affects someone can vary a lot.
Prevalence and Severity
Many studies show urinary incontinence is common after prostate surgery. How often it happens depends on the surgery type and what’s considered incontinence. Some men might just leak a little, while others could leak a lot. There are different kinds, like stress, urge, and mixed incontinence.
Impact on Daily Life
Urinary incontinence can really change a person’s life. It can cause emotional pain, make people feel alone, and lower their self-confidence. Even simple things like going out can be hard because of the fear of leaking. It can also hurt relationships and overall happiness.
Men dealing with incontinence might need to change their daily habits. They might do pelvic floor exercises, like Kegels, to help control their bladder. Sometimes, they might also need more treatments to manage it well.
Erectile Dysfunction After Prostatectomy
Prostatectomy can deeply affect a man’s sexual health, often causing erectile dysfunction. This is a big worry for many men facing prostate cancer surgery.
Erectile dysfunction (ED) after prostatectomy mainly comes from nerve and blood vessel damage. The nerves around the prostate, called the neurovascular bundles, are key for erections. During surgery, these nerves can get hurt or removed, causing ED.
Mechanism of Sexual Function Impairment
The cause of sexual function loss after prostatectomy is the damage to the nerves and blood vessels. The surgery can harm the nerves, causing them to not work right. It can also damage blood vessels, making it hard for blood to reach the penis, leading to ED.
Nerve-sparing techniques are used to lessen damage during surgery. These methods try to keep the nerves and blood vessels safe. But, how well they work depends on many things, like the patient’s age, cancer stage, and the surgeon’s skill.
Recovery Rates and Timeframes
How well men recover from erectile dysfunction after prostatectomy varies. Some men might get their erections back in a few months, while others might take longer or never fully recover.
Research shows that men who have nerve-sparing prostatectomy have a better chance of recovering. The time it takes to recover can be months to years. Things that affect recovery include how much nerve damage there is, the patient’s health, and the success of treatments like phosphodiesterase type 5 inhibitors (e.g., sildenafil).
It’s key for men having prostatectomy to talk about their risk of erectile dysfunction and recovery with their doctor. Knowing the risks and treatments can help manage hopes and improve results.
Other Physical Side Effects of Prostate Removal
Prostate removal can cause more than just urinary issues and erectile problems. Other complications can also affect a patient’s quality of life.
Bowel Function Changes
Changes in bowel habits are a less talked-about side effect. Some might face constipation or fecal incontinence. These issues can be upsetting and impact daily activities. It’s vital for patients to talk to their healthcare provider about these risks and how to prevent them.
Penile Shortening
Penile shortening is another possible side effect. The exact reasons are not fully known. It’s important for patients to know this is a known complication and to discuss it with their doctor.
Lymphedema Risks
Lymphedema is a swelling condition due to lymph node removal or damage. It can happen after prostate surgery. Watching for signs of lymphedema and acting early can help manage it.
Inguinal Hernia Development
There’s also a higher risk of inguinal hernias after prostate surgery. The exact cause is unclear, but it’s linked to pelvic floor changes. Patients should watch for a bulge in the groin and tell their doctor.
Knowing about these side effects is key to making informed treatment choices. By understanding the possible complications, patients can better prepare and talk to their healthcare team about any worries.
Psychological Impact of Prostate Removal
Prostate removal surgery is a lifesaving procedure for many. But, it can deeply affect a patient’s mind. It’s not just about removing cancer cells. It’s about making sure the patient feels whole again.
Depression and Anxiety
Men often feel sad and anxious after prostate surgery. The surgery and cancer diagnosis can make them feel hopeless. Many men deal with depression or anxiety after surgery.
Healthcare providers must watch for these feelings and offer help. This can include counseling or therapy. Early help can greatly improve a patient’s life and help them deal with their feelings.
Body Image and Masculinity Concerns
Prostate surgery can change how a man sees himself. Changes in sex life and bladder control can make him feel less manly. The emotional impact of these changes is huge, leading to feelings of not being good enough.
Support from doctors, family, and groups is key. By understanding these concerns, doctors can give better care. They can help with both physical and emotional needs.
Quality of Life After Prostate Removal
Men with prostate cancer face a big decision about surgery. This surgery can change their life in many ways. It affects their health and how they feel.
It’s important to know what to expect. This section will look at the good and bad sides of surgery. We’ll also check out what patients say to give a full picture.
Short-term vs. Long-term Quality of Life
Right after surgery, men might struggle with not being able to control their urine or have trouble with erections. These problems can make everyday life hard.
But, things often get better with time. Many men find their symptoms lessen and they feel more like themselves again. They might not be the same, but they can live well.
Table: Comparison of Short-term and Long-term Quality of Life After Prostate Removal
| Aspect | Short-term | Long-term |
| Urinary Continence | Often impaired | Generally improves |
| Erectile Function | Frequently affected | May recover partially |
| Overall Quality of Life | Significantly impacted | Improves over time |
Patient Satisfaction Studies
Many studies have looked at how happy patients are after surgery. Most men say they’re glad they had the surgery, even with the tough times.
“The majority of patients report a good quality of life after radical prostatectomy, though urinary and sexual problems are common.”
How happy a patient is can depend on many things. Things like how well they were told about the surgery, the care they got after, and their health before surgery.
Choosing to have prostate surgery is a big decision. Knowing what to expect and what others say can help men make the best choice for themselves.
Active Surveillance as a Viable Alternative
Men with low-risk prostate cancer might choose active surveillance over immediate surgery. This method involves regular check-ups and tests instead of immediate treatment.
Active surveillance is best for those with low-risk cancer. The choice depends on the cancer’s type, stage, and the patient’s health and life expectancy.
Eligibility Criteria for Active Surveillance
Not all prostate cancer patients can use active surveillance. Eligibility criteria include:
- Low-risk prostate cancer as defined by specific PSA levels, Gleason scores, and clinical staging.
- Patients with a life expectancy of 10-20 years or more, allowing for long-term monitoring.
- Those who are willing and able to adhere to a strict follow-up schedule.
Monitoring Protocols and Success Rates
Patients on active surveillance get regular tests. These include PSA tests, digital rectal exams (DRE), and prostate biopsies. The test frequency depends on the patient’s risk and the doctor’s advice.
Active surveillance has good success rates. Many patients stay on this path without needing aggressive treatments. The key is to catch those who might need more treatment due to cancer growth.
| Monitoring Protocol | Frequency | Purpose |
| PSA Tests | Every 3-6 months | Monitor PSA levels for changes |
| Digital Rectal Exam (DRE) | Every 6-12 months | Assess prostate for abnormalities |
| Prostate Biopsy | As recommended, typically annually or biennially | Evaluate prostate tissue for cancer progression |
Active surveillance balances cancer management. It avoids over-treatment but ensures timely action for those whose cancer grows. Understanding eligibility and following monitoring protocols helps patients make informed choices.
Radiation Therapy vs. Surgical Approaches
Radiation therapy and surgery are main treatments for prostate cancer. They have different effects and side effects. Knowing the differences is key when deciding on treatment.
External Beam Radiation
External Beam Radiation Therapy (EBRT) is a non-invasive method. It uses beams to kill cancer cells. It’s tailored to fit each person’s body, protecting healthy tissues. Advances in EBRT have made it more effective and reduced side effects.
- Types of EBRT include 3D Conformal Radiation Therapy, Intensity-Modulated Radiation Therapy (IMRT), and Stereotactic Body Radiation Therapy (SBRT).
- EBRT is often used for localized prostate cancer and can be combined with hormone therapy in more advanced cases.
Brachytherapy Options
Brachytherapy places radioactive material inside or near the tumor. It delivers a high dose of radiation to the cancer while protecting other tissues. Brachytherapy is very effective for patients with low-risk prostate cancer.
- Permanent brachytherapy involves implanting small radioactive seeds that remain in place.
- Temporary brachytherapy uses a high dose rate (HDR) source that is removed after treatment.
Comparing Outcomes with Surgery
When comparing radiation therapy to surgery, several factors are important. These include cancer control rates, side effects, and quality of life. Both treatments have their advantages and disadvantages.
- Studies have shown that, for many patients, the cancer control rates for radiation therapy are comparable to those of surgery.
- The choice between radiation therapy and surgery may depend on the patient’s overall health, the stage and grade of the cancer, and personal preferences.
The decision between radiation therapy and surgery should be made after talking to a healthcare provider. It should consider individual circumstances.
Other Treatment Alternatives
There are many treatment options for prostate cancer beyond surgery and radiation. These options are great for those who can’t have surgery or radiation, or who want to try something different.
Hormone Therapy Approaches
Hormone therapy, or androgen deprivation therapy (ADT), lowers male hormones in the body. This is often used when cancer has spread beyond the prostate. There are different types, like medications that lower testosterone and those that block testosterone’s effects on cancer cells.
This therapy can cause side effects like hot flashes and fatigue. It’s important for patients to talk to their doctors about these side effects to learn how to handle them.
Emerging Focal Therapies
Focal therapies target specific areas of the prostate with cancer. This can reduce side effects and keep more of the prostate working. Techniques include high-intensity focused ultrasound (HIFU) and cryotherapy. These are being studied in clinical trials to understand their benefits and risks.
Watchful Waiting for Older Patients
Watchful waiting is mainly for older patients or those with serious health issues. It means watching the condition without immediate treatment, focusing on symptom relief and quality of life. This is chosen when treatment risks are too high, like when cancer isn’t causing big symptoms.
Watchful waiting requires regular check-ups with a doctor to track the cancer. It’s a good choice for men with low-risk cancer or those who are older.
The Problem of Overtreatment in Prostate Cancer
Prostate cancer overtreatment is a big problem that needs careful thought. When prostate cancer is found, treatment often starts right away. But, this isn’t always the best choice for every man.
Overtreatment happens when men get treated for slow-growing cancer that wouldn’t harm them. This can cause unwanted side effects and lower their quality of life. It doesn’t offer much in terms of survival benefits.
Detecting Clinically Insignificant Cancers
Finding cancers that are not dangerous is a big challenge. These cancers grow slowly and won’t cause symptoms or death. New tests like genetic testing and MRI help tell the difference between dangerous and harmless tumors.
Some important things to know about these cancers include:
- PSA levels: Lower PSA levels mean less aggressive cancer.
- Gleason score: A lower score means the tumor is less aggressive.
- Tumor size and extent: Smaller tumors are more likely to be harmless.
Financial and Emotional Costs of Unnecessary Treatment
The costs of unnecessary treatment are high. It not only strains the healthcare system but also affects patients’ lives. Side effects like incontinence, impotence, and emotional distress can be severe.
The financial costs include:
- Direct medical costs for treatments and managing side effects.
- Indirect costs, such as lost productivity and travel expenses for treatment.
It’s important to understand the risks and benefits of treatments. Patients should talk to their doctors about their risks and the chance of overtreatment.
Decision-Making Process for Prostate Cancer Treatment
Choosing a prostate cancer treatment means looking at many things and working with doctors. This teamwork helps make care that fits each person’s needs and situation.
Shared Decision-Making with Healthcare Providers
Shared decision-making is key in treating prostate cancer. It’s when patients, their families, and doctors work together. They make choices based on what the patient wants, their values, and their lifestyle, along with the medical facts.
Benefits of Shared Decision-Making:
- Decisions are made with all the information
- Treatment plans are made just for the patient
- Patients are happier and do better
Important Factors to Consider
There are many things to think about when choosing a treatment. These include the cancer’s stage and how aggressive it is, the patient’s health, age, and how long they might live, and the side effects of treatments.
| Factor | Description | Considerations |
| Cancer Stage and Grade | The extent and aggressiveness of the cancer | Impacts treatment options and prognosis |
| Patient’s Overall Health | Presence of other medical conditions | Affects tolerance to certain treatments |
| Age and Life Expectancy | The patient’s age and expected lifespan | Influences the choice between aggressive treatment and watchful waiting |
Questions to Ask Your Doctor
To make good choices, patients should talk openly with their doctors. Asking the right questions helps understand treatment options and what they mean.
Key Questions to Consider:
- What are the available treatment options for my specific condition?
- What are the benefits and risks of each treatment?
- How will the treatment affect my quality of life?
- Are there any new or clinical trials I should look into?
By working together and thinking about important factors, patients can make smart choices about their treatment. It’s important to talk about all questions and worries with doctors to get the best results.
Advances in Surgical Techniques
New surgical techniques have changed prostate removal surgery a lot. These changes have made the surgery better and safer for patients.
Robotic vs. Traditional Prostatectomy
Robotic prostatectomy is a big step forward in treating prostate cancer. It uses small incisions, less blood, and quick recovery times. This method often leads to fewer problems and better results for patients.
On the other hand, traditional open surgery needs a bigger cut and takes longer to heal. But, it’s a good choice for some patients, like those with complex cases.
Nerve-Sparing Techniques
Nerve-sparing surgery is key to keeping sexual function and bladder control. It carefully avoids damaging nerves around the prostate. Nerve-sparing prostatectomy greatly improves life after surgery.
The success of this method depends on the surgeon and the patient’s health. Saving these nerves helps patients get back to how they were before surgery.
Do New Techniques Reduce Risks?
New surgical methods have made prostate removal surgery safer. Robotic surgery and nerve-sparing techniques have cut down on complications. These advancements have made the surgery safer and more effective.
As technology keeps getting better, we can expect even more improvements. This will lead to even better results for patients having prostate surgery.
Life Expectancy and Cancer-Specific Survival
It’s key to look at how different treatments affect survival rates and quality of life for prostate cancer patients. We need to know how each treatment impacts life expectancy and survival from cancer.
Impact of Treatment Choice on Survival
The treatment choice for prostate cancer greatly affects survival and life expectancy. Research shows that different treatments lead to different survival rates. For example, a study found that surgery can improve survival in some patients compared to active surveillance.
Treatment Outcomes Comparison
| Treatment | 5-Year Survival Rate | 10-Year Survival Rate |
| Radical Prostatectomy | 95% | 85% |
| Active Surveillance | 92% | 80% |
| Radiation Therapy | 90% | 78% |
Quality-Adjusted Life Years
Quality-adjusted life years (QALYs) give a deeper look at treatment results by looking at both life length and quality. QALYs are figured out by adjusting life years by the quality of life, from 0 (death) to 1 (perfect health).
For example, a patient living 10 years with a quality score of 0.8 would have 8 QALYs. This way, we can compare treatments better, considering side effects and complications that affect quality of life.
Knowing about QALYs is vital for choosing prostate cancer treatment. It helps patients and doctors make better choices by looking at the good and bad sides of each option.
Conclusion: Making an Informed Decision About Prostate Cancer Treatment
Choosing a prostate cancer treatment is a big decision. It involves knowing the different options and their risks and benefits. We’ve looked at prostate cancer, the risks of surgery, and other treatment choices.
Deciding on treatment needs careful thought. You must consider your cancer type, age, and health. Talking to doctors is key to finding the right treatment for you.
Knowing about treatment options helps patients make better choices. This knowledge lets them be more involved in their care. It helps them get the best results.
FAQ
What are the risks associated with prostate removal surgery?
Prostate removal surgery, also known as prostatectomy, carries risks. These include urinary incontinence and erectile dysfunction. Other side effects are bowel function changes, penile shortening, and lymphedema.
Why isn’t immediate removal of the prostate always necessary?
Immediate removal isn’t always necessary. This is because of the concept of clinically insignificant cancer. It’s slow-growing and may not affect life expectancy. Age and life expectancy also play a role in treatment decisions.
What is active surveillance, and is it a viable alternative to prostate removal?
Active surveillance involves closely monitoring the cancer. It’s a viable alternative to prostate removal for patients with low-risk prostate cancer.
How does radiation therapy compare to surgical approaches for treating prostate cancer?
Radiation therapy is an alternative to surgery. It includes external beam radiation and brachytherapy. Both have pros and cons. The choice depends on the cancer’s stage and grade, and the patient’s health.
What are the psychological impacts of prostate removal?
Prostate removal can affect mental health. It can lead to depression, anxiety, and concerns about body image and masculinity.
How does prostate removal affect quality of life?
Prostate removal can impact quality of life. Studies show varying results on patient satisfaction. It’s important to consider individual factors.
What are the advances in surgical techniques for prostate removal?
Advances include robotic prostatectomy and nerve-sparing techniques. These aim to reduce risks like urinary incontinence and erectile dysfunction.
How do treatment choices affect life expectancy and cancer-specific survival?
Treatment choices can impact life expectancy and cancer-specific survival. Quality-adjusted life years provide a nuanced understanding of treatment outcomes.
What is overtreatment in prostate cancer, and how can it be avoided?
Overtreatment occurs when clinically insignificant cancers are treated aggressively. It can be avoided by detecting cancers that are likely to progress. Choosing appropriate treatment options, like active surveillance, is key.
What factors should be considered when making a decision about prostate cancer treatment?
Important factors include the cancer’s stage and grade, overall health, life expectancy, and personal preferences. Shared decision-making with healthcare providers is essential.
What are the eligibility criteria for active surveillance?
Eligibility for active surveillance includes low-risk prostate cancer. This means a low PSA level, a low Gleason score, and a small amount of cancer in biopsy samples.
How does watchful waiting differ from active surveillance?
Watchful waiting is a more passive approach. It’s typically for older patients or those with significant comorbidities. It focuses on symptom management, not curative treatment.
What are the financial and emotional costs of unnecessary treatment?
Unnecessary treatment can be costly financially and emotionally. It can lead to decreased quality of life and long-term side effects.
What questions should I ask my doctor about prostate cancer treatment?
Important questions include the cancer’s stage and grade, treatment options, side effects, and the impact on quality of life and life expectancy.
References
- National Cancer Institute. (2025). Prostate cancer prevention (PDQ ®)“Patient version. National Institutes of Health. https://www.cancer.gov/types/prostate/patient/prostate-prevention-pdq




































