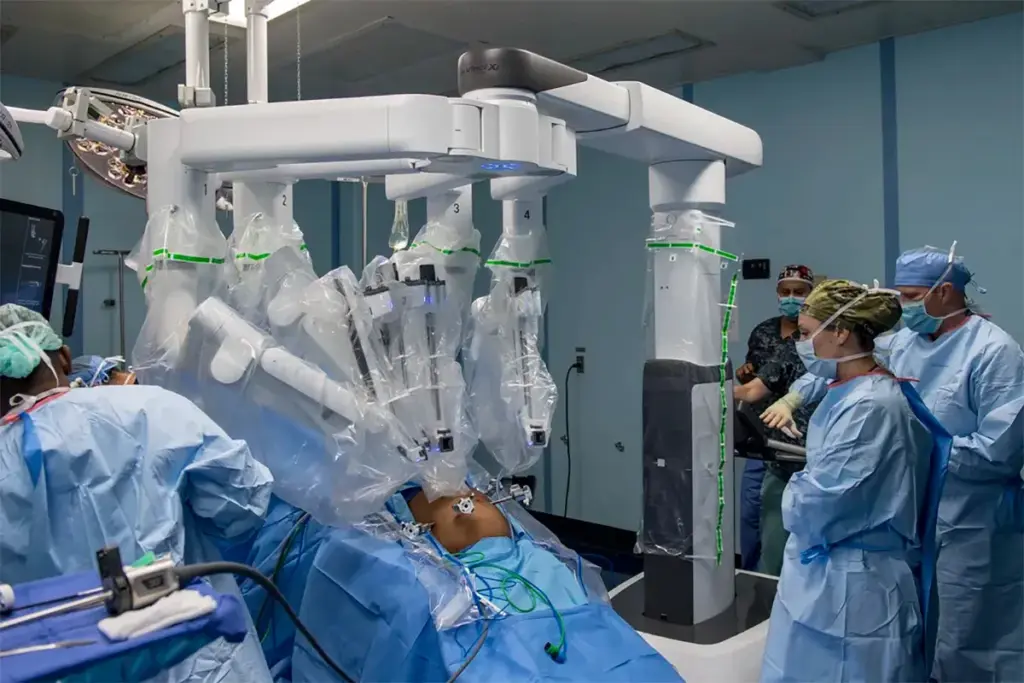
Robotic prostate surgery has changed how we treat prostate cancer. It’s a less invasive method that might lead to fewer complications. But, like any surgery, it has its own set of challenges. The Da Vinci system is a top choice for robotic surgery for prostate cancer. It’s known for its precision and the chance for better results.
It’s important to know the disadvantages of robotic surgery for both patients and doctors. We’ll look into the da vinci robotic surgery pros and cons. This will help everyone make better choices.
Key Takeaways
- Robotic prostate surgery is a type of minimally invasive surgery.
- The Da Vinci system is a leading technology used in robotic prostate surgery.
- Understanding the disadvantages is key for making informed decisions.
- Robotic surgery offers precision and may lead to fewer complications.
- It is essential to consider both the pros and cons before choosing robotic prostate surgery.
The Evolution of Prostatectomy Robotic Surgery
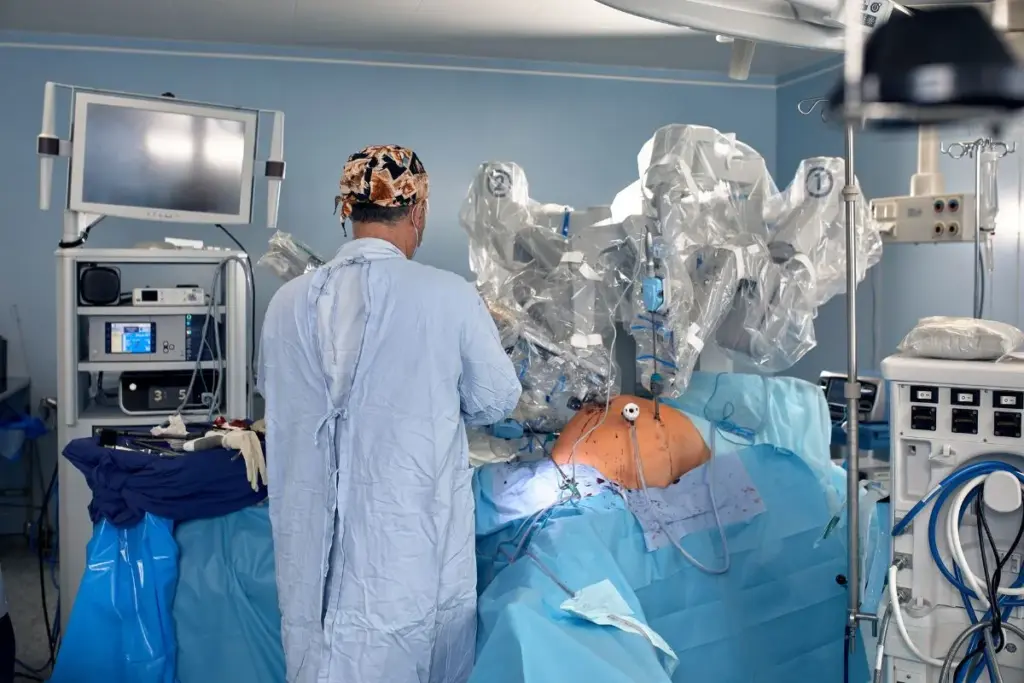
Robotic technology has improved prostatectomy outcomes, changing prostate cancer treatment. Robotic systems have made surgeries more precise and less invasive.
Development of Robotic Surgical Technology
The growth of robotic surgery technology is key in prostatectomy’s evolution. They allow surgeons to do complex surgeries with better precision and control.
These systems use advanced robotic technology for better vision, more dexterity, and less tremors. As technology advances, robotic systems are getting better. This leads to better results for patients.
Current Prevalence in Prostate Cancer Treatment
Robotic prostatectomy is now a common treatment for prostate cancer. It offers benefits over traditional surgery. The da Vinci prostatectomy is popular because it’s less invasive and can lead to quicker recovery.
Research shows robotic surgery for prostate cancer has fewer complications and less blood loss than open surgery. This makes robotic prostatectomy a top choice for many. Its growing use in prostate cancer treatment highlights its role in modern urology.
Understanding the Da Vinci Robotic Surgical System
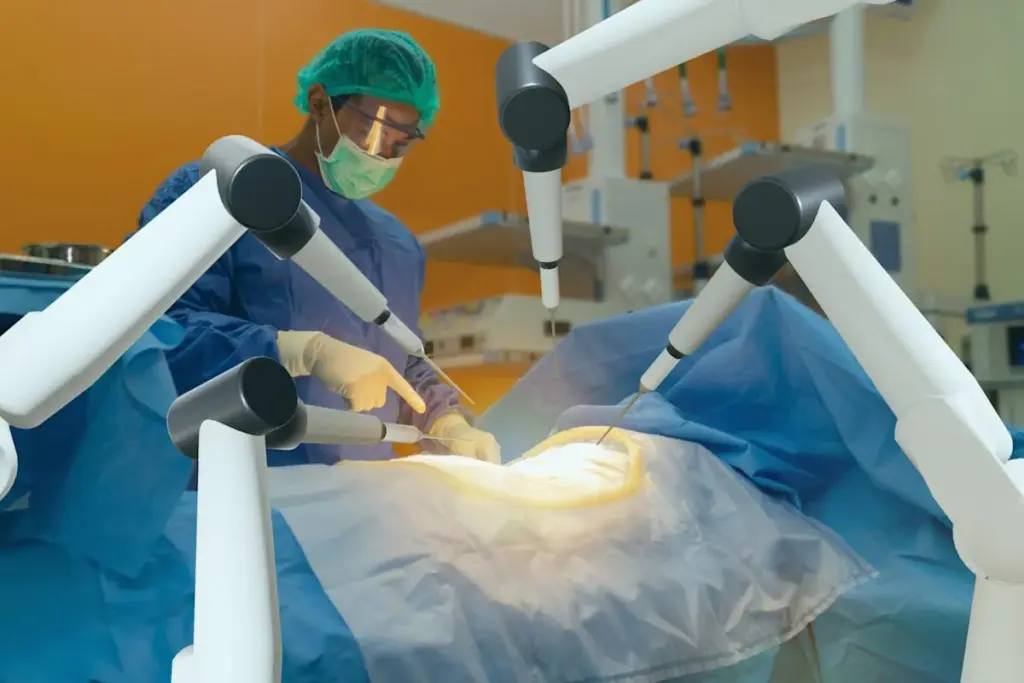
The Da Vinci Robotic Surgical System has changed surgery with its precision and new technology. It’s used for many surgeries, like robotic prostate surgery.
Components and Functionality
The Da Vinci system has several important parts that work together for complex surgeries. It has high-definition 3D visualization, precise robotic arms, and an ergonomic console for the surgeon. The high-definition 3D view helps surgeons see the surgical site clearly, making dissection and suturing more precise.
Precise Robotic Arms: The robotic arms mimic a surgeon’s hands, with great precision and control. This allows for detailed maneuvers during surgery, possibly lowering the risk of complications.
How the Surgeon Controls the Robotic System
A trained surgeon controls the robot arms from a console in the operating room. The console gives a 3D view of the surgical site. The surgeon’s hand movements are translated into precise robotic instrument movements. This design helps reduce surgeon fatigue during long surgeries.
“The Da Vinci system allows surgeons to perform complex procedures with enhanced precision, flexibility, and control compared to traditional methods.”
The Da Vinci Robotic Surgical System is a key tool in modern surgery. Its advanced technology and precise instruments make it valuable. Knowing its parts and how they work is important for understanding its role in surgeries like robotic prostate surgery.
Financial Disadvantages of Robotic Prostate Surgery
Robotic prostate surgery is becoming more common, but its high costs are a big issue. It has many benefits, but the cost of robotic systems is a big challenge for hospitals and patients.
Hospital Acquisition and Maintenance Costs
Buying a robotic surgical system is very expensive, costing millions of dollars. For example, the Da Vinci Surgical System can cost between $1 million to $2.5 million. Hospitals also have to pay for maintenance, which can cost $100,000 to $200,000 a year.
Studies show that healthcare systems worldwide face big challenges. The cost of robotic systems is one of these challenges. It can make it hard for places with less money to get this technology.
Higher Patient Out-of-Pocket Expenses
Patients who have robotic prostate surgery often have to pay more than those who have traditional surgery. The costs are higher because of the surgery fees, longer hospital stays, and more tests needed for robotic surgery.
A study showed that robotic prostatectomy can cost a lot more than traditional surgery. This can be a big problem for patients who don’t have much money or don’t have good insurance.
Insurance Coverage Limitations
Insurance for robotic prostate surgery can be limited, making things harder for patients. Some insurance companies might not cover all the costs, or they might have special rules for approval.
a well-known urologist, says, “The different ways insurance covers robotic surgery can be confusing for patients and doctors. It’s important for patients to know what their insurance covers and what they will have to pay before they decide.”
In summary, robotic prostate surgery has many good points, but the financial downsides are important. Hospitals and government officials need to work together to make sure this technology is available to those who need it.
The Surgeon Learning Curve Challenge
Robotic prostate surgery has changed urological oncology, but it’s tough for surgeons to learn. It takes time and practice to get good at using robotic systems. We need to look at the challenges of robotic prostatectomy, including training and how to measure skill.
Training Requirements and Proficiency Metrics
Surgeons must go through tough training to master robotic prostatectomy. This training includes learning, simulation, and guidance from experts. The goal is to make sure surgeons can do robotic surgeries safely and well. To check if they’re good, we look at how many surgeries they’ve done, how long they take, and if there are any problems.
A study found that doing at least 250 robotic surgeries makes a big difference. It lowers problems and improves results for patients.
“Building effective and trusted AI-augmented healthcare systems requires a multi-step, iterative approach.” This is true for adding robotic tech to surgery.
Volume-Outcome Relationship in Robotic Prostatectomy
The number of robotic surgeries a surgeon does affects patient results. Studies show that doing more surgeries leads to better outcomes. More experienced surgeons can handle tough cases better. This shows why training and experience are key in robotic surgery.
Impact on Patient Selection During Early Experience
Choosing the right patients is key when a surgeon is starting with robotic prostatectomy. They start with simpler cases and move to harder ones as they get better. Picking the right patients helps avoid risks and ensures the best care. As surgeons get more experience, they can take on more complex cases. This is important for getting the most out of robotic surgery while keeping risks low.
In summary, the challenge for surgeons learning robotic prostate surgery is complex. It involves tough training, a link between doing more surgeries and better results, and choosing the right patients. Understanding these points helps us see the challenges of new surgical tech and why ongoing learning and experience are key for the best patient care.
Operational Disadvantages: Time and Resource Utilization
Robotic prostate surgery has made big strides, but it also has some downsides. One major issue is how long it takes in the operating room. This is longer than traditional surgeries.
Extended Operating Room Time
Robotic systems need more setup and prep, which adds to the time spent in the OR. Research shows robotic prostatectomy takes longer than open or laparoscopic surgeries.
Comparison of Operating Room Times
|
Surgical Approach |
Average Operating Time (minutes) |
|---|---|
|
Robotic Prostatectomy |
180-240 |
|
Open Prostatectomy |
120-180 |
|
Laparoscopic Prostatectomy |
150-210 |
Setup and Docking Time Considerations
Setting up and docking the robotic system is a key step. It needs precision and takes time. This involves placing the robotic arms, attaching instruments, and calibrating the system.
Anesthesia Duration Implications
The longer surgery times mean patients need more anesthesia. This can raise the risk of complications and slow down recovery.
It’s important to weigh these challenges when looking at robotic prostate surgery. Understanding the time and resources needed helps healthcare providers manage better and improve patient care.
Technical Limitations of Prostatectomy Robotic Surgery
Robotic surgery is getting better, but we need to know its limits to make prostatectomy better. Even with its progress, robotic prostate surgery has technical hurdles. These can affect how well it works and the results it gets.
Absence of Haptic Feedback
One big problem is the lack of haptic feedback. This means surgeons can’t feel what they’re doing during surgery. They have to rely on what they see instead of feeling it.
This makes it hard to judge how tight tissues are and to handle small parts. Surgeons use the robotic system’s clear images to guide them.
Spatial Awareness Challenges
Another issue is spatial awareness. The design of the robotic system and the setup of the operating room can limit how well surgeons can see and move. This can make it hard to do the surgery right.
To get better at this, surgeons and their teams practice a lot. They work on understanding and moving well during robotic surgeries.
Instrument Range of Motion Constraints
The way robotic instruments move is also a problem. They are more precise than old laparoscopic tools but can’t move as freely. This makes it tough to reach some parts of the pelvic area.
|
Technical Limitation |
Description |
Impact on Surgery |
|---|---|---|
|
Absence of Haptic Feedback |
Lack of tactile sensation |
Difficulty in assessing tissue tension |
|
Spatial Awareness Challenges |
Restricted spatial understanding |
Potential for surgical complications |
|
Instrument Range of Motion Constraints |
Limited dexterity |
Difficulty accessing certain areas |
It’s key for surgeons and healthcare to know these limits to use robotic systems better in prostatectomy. By facing and solving these problems, we can improve surgery results and care for patients.
Potential Technical Failures and Complications
It’s important to know about the risks of technical failures in robotic prostate surgery. These failures are rare but can affect both the patient and the surgical team a lot.
System Malfunction Rates and Types
Robotic prostate surgery can face technical failures from different sources. This includes equipment, software, or integration problems with other equipment. Research shows that these failures happen in a small percentage of surgeries, from 0.3% to 4.6%.
The malfunctions can be:
- Instrument failure
- Problems with the robotic arms
- Vision system malfunctions
- Issues with the surgeon’s console
Conversion to Open Surgery: Frequency and Implications
If technical failures happen during robotic prostate surgery, a possible outcome is needing to switch to open surgery. This switch is not common but can happen.
Switching to open surgery can have big effects. It might lead to:
- More blood loss
- Longer recovery times
- Different complications after surgery
Emergency Protocols During System Failure
It’s key to have strong emergency plans for technical failures in robotic prostate surgery. These plans should include:
- Clear communication among the surgical team
- Quick access to backup equipment
- Steps for switching to other surgical methods
It’s vital for the surgical team to practice these emergency plans. This ensures they can work together well if a failure happens.
Functional Outcomes and Side Effects
Robotic prostate surgery is becoming more common. It’s important to look at how it affects urinary and sexual function. We’ll explore the good and bad sides of this surgery, helping both patients and doctors.
Urinary Incontinence Rates After Robotic Prostatectomy
Urinary incontinence is a big worry for those having prostate surgery. Research shows robotic surgery might help more people stay dry than traditional surgery. But, how well it works depends on the surgeon and the patient.
We looked at many studies to see how often people have trouble staying dry after robotic surgery. While some incontinence is common at first, most people do well in the long run.
Erectile Dysfunction: Expectations vs. Reality
Erectile dysfunction (ED) is a big concern after prostate surgery. Many patients hope to keep their ability to get an erection. But, the reality is not always the same. Robotic surgery tries to avoid nerve damage, but ED can happen.
Our comparison shows robotic surgery has some benefits like less blood loss and shorter hospital stays. Yet, the chance of ED is similar to open surgery. Things like age and how well you were doing before surgery affect your chances of ED after.
Comparative Data with Traditional Surgical Approaches
To understand robotic prostate surgery better, we need to compare it with traditional methods. The table below shows what studies have found.
|
Outcome |
Robotic Prostatectomy |
Open Prostatectomy |
|---|---|---|
|
Urinary Continence at 1 Year |
85-90% |
80-85% |
|
Erectile Function Preservation |
60-70% |
50-60% |
|
Positive Surgical Margins |
10-15% |
15-20% |
Our study found robotic surgery has some advantages. It might lead to less incontinence and better margins. But, ED is a big concern.
Knowing these facts helps patients and doctors make better choices about surgery.
Oncological Concerns in Robotic vs. Open Prostatectomy
Robotic prostatectomy has changed how we treat prostate cancer. But, there are worries about its effectiveness in fighting cancer. We need to look at the data on surgical margins, cancer control, and recurrence.
Positive Surgical Margin Rates
Positive surgical margin (PSM) rates show how well a prostate surgery works. Studies compare PSM rates between robotic and open surgery to see which is better.
The studies show robotic surgery might have slightly better PSM rates than open surgery. But, we must remember that different studies and techniques can affect the results.
Cancer Control and Recurrence Data
Keeping cancer under control and preventing it from coming back are key. Research shows robotic surgery can match open surgery in keeping cancer from coming back.
Limitations in Handling High-Risk or Advanced Cases
Robotic surgery is good for treating early prostate cancer. But, it’s not as clear for high-risk or advanced cases. These cases need a more detailed approach, which might not be as easy with robotic surgery.
Artificial intelligence (AI) and better imaging are helping plan and do prostate cancer treatments, including robotic surgery. AI can spot high-risk features and help plan the treatment.
In summary, robotic surgery has many benefits, like lower PSM rates and good cancer control. But, it’s not perfect for all cases, like high-risk or advanced prostate cancer. Choosing the right surgery for each patient is very important.
Healthcare Disparities and Access Issues
Robotic surgical systems are not spread evenly, causing unequal access to care. This issue is a big problem in healthcare, affecting how well patients do and the quality of care they get.
Geographic Distribution of Robotic Surgical Systems
Robotic prostate surgery is more common in cities, where big hospitals and specialized centers are found. But, rural areas often lack access to these advanced surgical tools.
Getting to the root of patient health and well-being is key. The spread of robotic surgical systems affects how patients can get these advanced treatments.
Socioeconomic Factors Limiting Patient Access
Income and insurance play big roles in who can get robotic prostate surgery. Those from lower income backgrounds may find it hard to get care at places with robotic systems.
The cost of robotic surgery is also a big issue. It’s more expensive than traditional surgery, making it hard for those without enough money to afford it.
Volume Requirements Creating Centralization of Care
Hospitals need to do a certain number of surgeries to stay good at robotic prostate surgery. This can make care more centralized, where only big centers offer robotic surgery. This limits access for those in less populated or remote areas.
As we move forward, we need to tackle these disparities to make sure everyone has equal access to advanced surgeries like robotic prostate surgery. By understanding what causes these disparities, we can work towards a more inclusive and accessible healthcare system.
Marketing Claims vs. Evidence-Based Outcomes
Robotic surgery is becoming more common, but it’s important to know the difference between what’s promised and what’s proven. The gap between what’s advertised and what really happens can be big. This can confuse both patients and doctors.
Analyzing Promotional Materials Against Clinical Data
Ads for robotic prostate surgery often talk about less blood loss, less pain, and faster recovery. But we need to check these claims against real studies. Research shows mixed results, like robotic surgery might mean shorter hospital stays and less blood loss. Yet, the long-term effects on cancer and how well the prostate works again are not as clear.
We should carefully look at ads and videos, beyond their shiny surface. For example, a study might show robotic surgery has short-term benefits. But it could also find that long-term cancer control is the same as traditional surgery.
Patient Perception Management
How patients see robotic surgery matters a lot. Ads often focus too much on the “robotic” part, setting up high hopes. Doctors need to manage these hopes, making sure patients know what robotic surgery can and can’t do.
Talking to patients about what robotic surgery really offers can help. This means sharing both the good and the bad, and what research says about long-term results.
Regulatory Oversight of Robotic Surgery Marketing
Groups like the Federal Trade Commission (FTC) in the U.S. help make sure ads for robotic surgery are honest. They watch over ads for medical devices and procedures.
|
Regulatory Aspect |
Current Practice |
Ideal Practice |
|---|---|---|
|
Claim Substantiation |
Often based on limited data or selective presentation of results |
Claims should be backed by robust, peer-reviewed evidence |
|
Comparative Advertising |
May compare robotic surgery favorably to traditional methods without clear evidence |
Comparisons should be based on complete, head-to-head studies |
|
Patient Testimonials |
May be used selectively to promote positive outcomes |
Testimonials should be typical of most patient experiences |
By improving how ads are watched over and making marketing clearer, we can help. This way, patients and doctors can make better choices about robotic prostate surgery.
Patient Selection: When Robotic Surgery May Not Be Ideal
The right fit for robotic prostate surgery depends on many things. This includes the patient’s health and their body’s specific conditions. Surgeons look at several important factors before deciding if robotic surgery is best.
Anatomical Considerations and Contraindications
Body shape and size are key in deciding if robotic surgery is right. The size of the prostate and any past surgeries also matter. For example, past surgeries can make it harder to use the robotic tools.
Some body types or past surgeries can make it hard for surgeons to work well. Being very overweight or having a narrow pelvis can be a problem. In these cases, other surgeries might be better.
Prior Abdominal Surgery Complications
People who have had surgery before might face extra challenges. Old scars can make it harder to cut through tissues. Surgeons need to look at past surgeries to plan better.
Old scars or other problems from past surgeries might mean a different surgery is needed. Planning before surgery helps find and solve these issues.
Medical Comorbidities Increasing Risk
Health problems like heart disease or diabetes can make surgery riskier. Patients with these issues need extra care before surgery. This helps lower the risks.
Doctors work together to manage these health issues. They make sure the patient is ready for surgery. This way, patients get the best results from robotic prostate surgery.
Ergonomic and Team Dynamics Challenges
Robotic prostate surgery is good for patients but has its challenges. The complex robotic systems need a well-coordinated team. This can sometimes cause operational problems.
Physical Strain on the Surgical Team
Robotic surgery can strain the surgical team physically. Surgeons often sit for long periods, leading to fatigue and back pain. The console design tries to be ergonomic but may not fully solve these issues.
Research shows surgeons face neck and back pain from robotic surgery. They need ergonomic adjustments and breaks to perform well.
Communication Barriers in the Robotic Operating Environment
Good communication is key in surgery, and robotic surgery is no different. The robotic setup can make communication hard. The surgeon and team are physically apart, which can cause misunderstandings.
To fix this, teams need clear communication strategies. They should use standard protocols and know their roles during surgery.
Training Requirements for the Entire Surgical Team
Robotic prostate surgery needs thorough training for the whole team. This includes the surgeon and support staff. Everyone must know their part and be skilled in their tasks.
Training should focus on team coordination and communication. Regular updates and practice help keep the team ready.
Future Innovations Addressing Current Limitations
In the future, robotic surgery will face new challenges. But, new technologies are coming to make it better. These advancements will make robotic prostate surgery more effective and easier to use.
Advancements in Tactile Feedback
One big problem with robotic surgery now is the lack of feeling. Scientists are working on fixing this. They want to add tactile feedback so surgeons can feel what they’re doing.
A study showed a new sensor that gives surgeons real-time feedback. This could lead to fewer mistakes and better results for patients.
Integration of Artificial Intelligence
Artificial intelligence (AI) is changing robotic surgery. AI can look at lots of data and help surgeons make better choices. This could make surgeries safer and more successful.
A report said AI could make surgeries shorter and help patients recover faster. Here are some benefits of AI in robotic prostate surgery:
|
Benefit |
Description |
Potential Impact |
|---|---|---|
|
Enhanced Precision |
AI algorithms assist in precise dissection and suturing |
Reduced risk of complications |
|
Predictive Analytics |
AI analyzes data to predict possible problems |
Improved patient outcomes |
|
Personalized Surgery |
AI helps tailor the surgical approach to individual patients |
Better recovery rates |
Cost Reduction and Accessibility
There’s also a push to make robotic surgery cheaper. Companies are making systems that cost less, and hospitals are finding ways to use them more efficiently.
A report said these efforts could make robotic prostate surgery available to more people. As technology gets better, we’ll see more hospitals using it.
A leading expert said, “AI is going to change medicine, bringing new tools that help doctors.” This change will likely make robotic surgery better and more available.
Conclusion
Robotic prostate surgery has both good and bad sides. Knowing these helps patients and doctors make smart choices. This is key when deciding on robotic surgery for prostate issues. We’ve looked at robotic surgery’s benefits and drawbacks. It’s evolved a lot and has great tech, but it’s not perfect. A caring and modern treatment setting is vital for patients. As we keep improving robotic surgery, weighing its pros and cons is critical. This way, we can give patients the care they need. It’s all about making sure each patient gets the best treatment for them.
FAQ
What are the main disadvantages of robotic prostate surgery?
The main downsides include high costs for the systems and training for surgeons. It also takes longer in the operating room. Plus, it lacks the feel of real surgery.
How does robotic prostate surgery compare to traditional open prostatectomy in terms of outcomes?
Robotic surgery often means less recovery time and less blood loss. But, it might have similar or slightly different rates of problems like incontinence and erectile issues.
What are the financial implications of choosing robotic prostate surgery?
It’s often pricier than traditional surgery, leading to higher costs for patients. Insurance might not cover it fully, making it even harder financially.
Are there any specific patient selection criteria for robotic prostate surgery?
Yes, picking the right patient is key. Doctors look at things like the patient’s body, past surgeries, and health issues to decide if robotic surgery is right.
How does the learning curve for surgeons impact robotic prostate surgery outcomes?
The learning curve can affect results, mainly in the beginning. Surgeons need a lot of training to get good at it. The more they do, the better they get.
What are the technical failures or complications during robotic prostate surgery?
Sometimes, technical issues or complications can happen. These are rare but might need a switch to open surgery. Knowing how to handle emergencies is very important.
How does robotic prostate surgery affect functional outcomes such as urinary continence and erectile function?
It can lead to different rates of incontinence and erectile problems. The results can be similar or a bit different than traditional surgery, depending on many factors.
Are there disparities in access to robotic prostate surgery, and what factors contribute to these disparities?
Yes, there are disparities due to where the systems are, money, and how often they’re used. This can make it hard for some to get the surgery.
What future innovations are expected to address the current limitations of robotic prostate surgery?
New tech might include better feel, AI, and ways to make it cheaper and more accessible. These could make robotic surgery even better.
How do marketing claims for robotic surgery compare to evidence-based outcomes?
Marketing claims need to be checked against real data to be sure they’re true. Rules are in place to stop false ads and help patients make informed choices.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC5600093/























