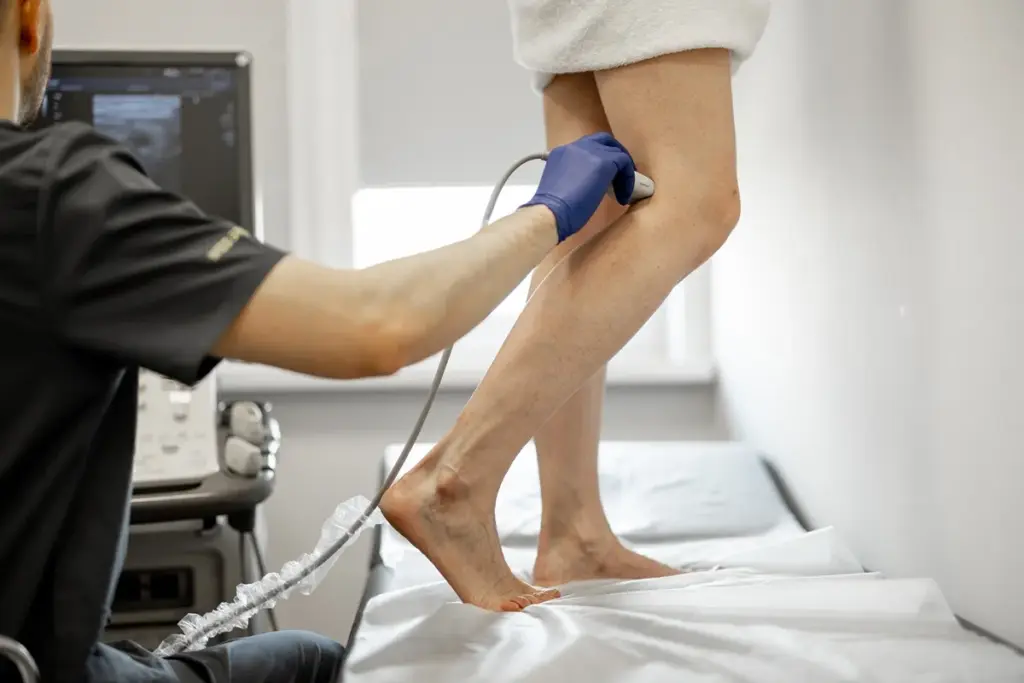
Every year, thousands of people face a serious condition. It’s called pulmonary embolism. This happens when a blood clot moves from the leg to the lungs. It blocks blood flow in the lungs.
Knowing how fast a blood clot moves is key. It’s important for quick treatment. A blood clot can quickly move from the leg to the lungs. This can happen without warning.
It’s a serious condition that needs immediate help. Without it, serious problems or even death can occur.
Key Takeaways
- A pulmonary embolism occurs when a blood clot travels from the leg to the lungs.
- This condition can be life-threatening and requires immediate medical attention.
- The speed of a blood clot’s travel can vary, but it often happens rapidly.
- Understanding the risks and symptoms is critical for timely diagnosis.
- Treatment options are available to prevent serious complications or death.
Understanding Blood Clots and Their Movement

It’s important to know how blood clots form and move in the body. Blood clots pose serious health risks. This is especially concerning when they migrate to vital areas such as the lungs.
What Are Blood Clots?
Blood clots are like gel-like clumps of blood. They form when blood coagulates. This can happen for many reasons, like injury, staying in one place for too long, or genetic factors.
When a clot forms, it might stay put or break loose. If it breaks loose, it can travel to other parts of the body.
How Blood Clots Form in the Legs
Blood clots often start in the legs, known as deep vein thrombosis (DVT). Things like staying in one place for a long time, injury, or surgery can cause DVT. It’s key to know the signs and risk factors of DVT early on.
The Journey from Leg to Lung
If a blood clot breaks loose from the leg, it can travel up the venous system. It goes through the heart and ends up in the pulmonary arteries. This can cause a pulmonary embolism (PE).
Symptoms of PE include shortness of breath, chest pain, and coughing up blood. Knowing how this happens helps doctors diagnose and treat PE right away.
The Speed of Blood Clot Travel
The speed of a blood clot moving from the leg to the lungs varies. This is because many factors can influence its journey.
Factors Affecting Travel Time
Several things can change how fast a blood clot moves. The size of the clot and the person’s health are key. Clot size matters a lot because bigger clots move faster.
Health conditions like deep vein thrombosis (DVT) also play a role. DVT is when clots form in deep veins, often in the legs. This can make it more likely for a clot to break loose and go to the lungs, causing a pulmonary embolism (PE).
Average Time for Clot Migration
Research shows clots can travel from the leg to the lungs in minutes to hours. The exact time varies. But, it’s important to know that clots can move fast, which is why quick medical help is needed.
|
Clot Size |
Average Travel Time |
Risk of Complications |
|---|---|---|
|
Small |
Several Hours |
Low to Moderate |
|
Medium |
1-2 Hours |
Moderate to High |
|
Large |
Minutes to 1 Hour |
High |
Scientific Studies on Clot Movement
Scientists have studied how clots move. They use imaging to track clots. This research helps us understand what affects clot travel time and how to prevent and treat it.
For example, a study might use ultrasound to watch clots form and move. This gives us important information about clot migration.
Deep Vein Thrombosis: The Starting Point
Deep vein thrombosis (DVT) is a serious condition. It happens when a blood clot forms in the deep veins, usually in the legs. This is a big risk for pulmonary embolism, a serious and potentially deadly problem.
Understanding DVT
DVT happens when a thrombus forms in the deep veins, often in the legs. This clot can be dangerous if it breaks loose and goes to the lungs, causing a pulmonary embolism.
Common Locations for DVT Formation
DVT most often happens in the legs, mainly in the calf and thigh. It can also happen in other deep veins, but the legs are the most common place.
Recognizing DVT Symptoms
It’s important to know the symptoms of DVT to get early treatment. Common signs include swelling, pain, warmth, and redness in the affected leg.
|
Symptom |
Description |
|---|---|
|
Swelling |
The affected leg may become swollen due to the clot obstructing blood flow. |
|
Pain |
Pain or tenderness in the leg, which can range from mild to severe. |
|
Warmth |
The area around the clot may feel warm to the touch. |
|
Redness |
The skin over the affected area may become red or discolored. |
Spotting DVT symptoms early can greatly lower the risk of serious problems like pulmonary embolism. If you notice any of these signs, get medical help right away.
What is Pulmonary Embolism?
Pulmonary embolism is a serious condition where a blood clot blocks a lung artery. It’s life-threatening if not treated quickly. We’ll look into what it is, its types, and how common it is to understand its effects.
Definition and Overview
A pulmonary embolism happens when a blood clot from the legs gets stuck in the lungs. This blocks blood flow and can harm lung tissue. It also stops oxygen from reaching the body.
Pulmonary embolism treatment usually includes medicines to stop more clots. In severe cases, doctors might use special medicines to break up the clot.
Types of Pulmonary Emboli
Pulmonary emboli can be different based on what they’re made of and where they are. The main kinds are:
- Thrombotic Emboli: These are blood clots.
- Non-Thrombotic Emboli: These can be from fat, air, or tumor cells.
Knowing the type of pulmonary embolism helps doctors choose the best treatment options.
Prevalence and Statistics
Pulmonary embolism is a big problem worldwide. Studies say it affects between 39 and 115 people per 100,000 each year.
|
Population |
Incidence Rate (per 100,000) |
|---|---|
|
General Population |
39-115 |
|
Hospitalized Patients |
Higher incidence due to risk factors like immobility |
These numbers show why we need to know about it and take steps to prevent it, mainly for those at higher risk.
The Mechanism of Pulmonary Embolism
Pulmonary embolism happens when a blood clot moves to the lungs. This is a serious issue that can be deadly. It often comes from deep vein thrombosis (DVT).
Clot Formation and Breakage
A blood clot forms in the deep veins of the legs first. Many risk factors make clotting more likely. These include staying in one place for too long, having a family history, and certain health issues.
When a clot breaks off, it turns into an embolus. This embolus then moves up the veins towards the heart and lungs.
The Path Through the Venous System
The embolus’s trip through the veins is key to understanding pulmonary embolism. It goes up the vena cava into the heart’s right side. Then, it’s pumped into the pulmonary arteries.
- The clot’s size and the person’s health decide how severe the embolism is.
- Knowing the risk factors for PE helps spot people at higher risk.
- Preventing measures can greatly lower the chance of pulmonary embolism.
Consequences in the Lungs
When the clot reaches the lungs, it can block arteries. This can cause serious symptoms and harm to the lung tissue. It also makes it hard for the blood to get enough oxygen.
It’s important to know the signs of pulmonary embolism to get help quickly. We’ll look at the symptoms in more detail later.
Recognizing Pulmonary Embolism Symptoms
It’s important to know the signs of pulmonary embolism to get timely help. This can greatly improve your chances of recovery. We’ll look at the symptoms and when they mean you need emergency care.
Immediate Symptoms
Pulmonary embolism can cause sudden and severe symptoms. These include:
- Shortness of breath or trouble breathing
- Chest pain that gets worse with deep breathing or coughing
- Coughing up blood
- Rapid heart rate or palpitations
- Lightheadedness or dizziness
These symptoms need quick medical attention. They can be signs of a serious condition.
Developing Symptoms Over Time
Sometimes, symptoms of pulmonary embolism come on slowly. These can be:
- Mild shortness of breath that gets worse over time
- Swelling or pain in one leg, which could mean deep vein thrombosis (DVT)
- Fatigue or feeling weak
Even though these symptoms are not as urgent, they also need medical check-up.
When Symptoms Indicate an Emergency
Knowing when symptoms mean you need emergency care is key. Severe trouble breathing, chest pain, or coughing up blood are emergencies. You should get help right away.
Let’s look at some important facts about pulmonary embolism:
|
Symptom Severity |
Common Symptoms |
Recommended Action |
|---|---|---|
|
Mild |
Mild shortness of breath, leg swelling |
Schedule a doctor’s appointment |
|
Moderate |
Increased shortness of breath, chest pain |
Visit the emergency room |
|
Severe |
Severe difficulty breathing, severe chest pain, coughing up blood |
Call emergency services immediately |
Preventing pulmonary embolism is also important. Using prevention tips like staying hydrated, moving often, and avoiding long periods of sitting can help lower your risk.
Diagnosing Pulmonary Embolism
Healthcare professionals use many tools to diagnose pulmonary embolism. It’s key to get the diagnosis right for good treatment and care. We use clinical checks, imaging tests, and blood tests together to do this.
Initial Assessment and Physical Examination
We start by checking the patient’s symptoms and medical history. We look for signs like shortness of breath, chest pain, and a fast heart rate. These are common in people with pulmonary embolism. A detailed physical exam also helps find deep vein thrombosis and checks the patient’s health.
|
Signs/Symptoms |
Description |
Clinical Implication |
|---|---|---|
|
Dyspnea |
Shortness of breath |
Common in PE patients |
|
Chest Pain |
Pain or discomfort in the chest |
May indicate PE or other conditions |
|
Tachycardia |
Rapid heart rate |
Often associated with PE |
Imaging Tests
Imaging tests are key for diagnosing pulmonary embolism. We often use computed tomography pulmonary angiography (CTPA) and ventilation-perfusion (V/Q) scans. CTPA is very good at showing PE, giving clear images of the lungs’ blood vessels.
Blood Tests and Other Diagnostic Tools
Blood tests, like D-dimer assays, help support the diagnosis. A negative D-dimer can help rule out PE in low-risk patients. Other tools, like electrocardiograms (ECG) and chest X-rays, help check the patient’s condition and rule out other causes.
By using these methods together, we can accurately diagnose pulmonary embolism. Then, we can create a good treatment plan.
Emergency Treatment for Pulmonary Embolism
When a pulmonary embolism happens, quick medical help is key to avoid serious complications. We know that fast treatment can greatly help patients and lower the chance of long-term health problems linked to PE complications.
Immediate Medical Interventions
The first thing we do is make sure the patient is stable. We give oxygen and medicines to help blood pressure. This helps keep the patient’s condition from getting worse.
Patients usually stay in an intensive care unit (ICU) for close watching. This lets us quickly change treatment if needed to tackle complications early.
Medication Options
Anticoagulant medicines are key in treating pulmonary embolism. They stop the clot from growing and prevent new ones. We start with heparin or low molecular weight heparin, then switch to oral anticoagulants like warfarin.
For severe cases, we might use thrombolytic therapy to break down the clot. But this can increase the risk of bleeding, so we use it carefully, considering the patient’s situation and risk of PE complications.
Surgical Procedures When Necessary
In some cases, surgery is needed to remove the clot. This is for patients at high risk of death from the embolism or those who can’t take anticoagulant medicines.
Another choice is putting in a vena cava filter. It stops new clots from reaching the lungs. We think about this for patients at high risk of another pulmonary embolism, even with anticoagulation therapy.
Effective emergency treatment for pulmonary embolism needs a full plan. This includes quick medical help, the right medicines, and sometimes surgery. Knowing these treatments helps us manage complications and improve patient results.
Long-term Treatment and Management
Managing pulmonary embolism long-term needs a full plan. This includes medical care, follow-ups, and lifestyle changes. We know it’s tough, but the right steps can lower the risk of it happening again and improve life quality.
Anticoagulation Therapy
Anticoagulation therapy is key in managing pulmonary embolism. It stops new blood clots from forming and prevents existing ones from growing. We usually prescribe these medicines for 3 to 6 months after diagnosis. But, the time can change based on the patient’s risk factors and the cause of the embolism.
Common anticoagulant medications include warfarin, apixaban, rivaroxaban, and dabigatran. Each has its own benefits and risks. We choose the best one for each patient based on their needs and medical history.
Follow-up Care
Regular check-ups are vital to see if the treatment is working and to manage side effects. We meet with patients often to check their condition, adjust medicines, and answer any questions.
Imaging tests, like ultrasound or CT scans, help us see if the clot is getting better or if new ones are forming. We also use blood tests to check if the medicine is working right.
Lifestyle Modifications
Changing your lifestyle is also important in managing pulmonary embolism. We suggest several changes to lower the risk of it happening again. These include:
- Staying active and exercising regularly to improve blood flow
- Keeping a healthy weight to reduce vein pressure
- Avoiding long periods of sitting, like on flights or car rides
- Quitting smoking to boost heart health
By using anticoagulation therapy, regular check-ups, and making lifestyle changes, patients can manage their pulmonary embolism well. We’re here to support our patients every step of the way and help them achieve the best health possible.
Preventing Blood Clots and Pulmonary Embolism
It’s important to take steps to prevent blood clots and pulmonary embolism. Knowing how to prevent these conditions can greatly lower your risk. This can help avoid a serious and potentially life-threatening situation.
Strategies During Long Periods of Immobility
Being immobile for a long time, like on a long trip or in bed, raises your risk of blood clots. To lower this risk, you should:
- Drink plenty of water to stay hydrated
- Get up and move around and stretch regularly
- Do simple exercises like ankle rotations and toe flexes while seated or in bed
These steps help keep your blood flowing well, making it less likely for clots to form.
Preventive Measures After Surgery
After surgery, the risk of blood clots goes up because you’re not moving much and the surgery itself can cause issues. To prevent this, you should:
- Take anticoagulant medications as your doctor tells you to
- Wear compression stockings or use intermittent pneumatic compression devices
- Start moving around early, as your healthcare team advises
These steps are key in lowering your risk of pulmonary embolism after surgery.
Daily Habits for Prevention
There are also daily habits that can help prevent blood clots and pe prevention. These include:
- Eating healthy and staying at a good weight through diet and exercise
- Being active with regular physical activity
- Not smoking and drinking alcohol in moderation
By making these habits part of your daily routine, you can lower your risk of blood clots even more.
In summary, preventing blood clots and pulmonary embolism needs a few different approaches. This includes being proactive when you’re not moving much, following steps after surgery, and living a healthy lifestyle. By doing these things, we can greatly reduce the risk of pulmonary embolism and keep our hearts healthy.
Complications of Untreated Pulmonary Embolism
Not treating pulmonary embolism quickly can cause serious health problems. It’s important to know these issues to see why quick medical help is key. We’ll look at the short and long-term effects and how they affect survival rates.
Short-term Complications
Untreated pulmonary embolism can lead to severe and dangerous conditions. Acute right ventricular failure is one, where the heart’s right side fails to pump due to the blockage. This can be fatal. Also, the blockage can cause hypoxemia, or low blood oxygen, making things worse.
Long-term Health Effects
Untreated pulmonary embolism can also cause long-term health issues. Some may get chronic thromboembolic pulmonary hypertension (CTEPH), where blood pressure in the lungs stays high. This can lead to right heart failure if not treated. Also, survivors might have post-PE syndrome, with symptoms like shortness of breath and less ability to exercise.
Mortality Rates and Statistics
The outlook for untreated pulmonary embolism is usually bad, with high death rates. Studies show that up to 30% of people might die within a month. Quick diagnosis and treatment can greatly improve survival chances, showing how urgent medical care is for suspected pulmonary embolism.
Understanding the dangers of untreated pulmonary embolism stresses the need for early detection and treatment. By knowing the risks, healthcare teams and patients can work together to better outcomes in pulmonary embolism cases.
Living with Pulmonary Embolism: Recovery and Beyond
Living with pulmonary embolism means a lot of work to get better. This includes medical treatment, making lifestyle changes, and getting emotional support. We know it’s a tough journey, full of challenges for patients and their families.
The Recovery Timeline
The time it takes to recover from pulmonary embolism varies. It depends on the clot size, any health issues, and how fast treatment started. Usually, people start feeling better in a few weeks. But, it can take months to fully recover.
It’s important to stick to the treatment plan. This often includes medicine to stop more clots. Also, regular check-ups with doctors are key to track progress and make any needed changes.
Physical and Emotional Challenges
Pulmonary embolism affects both body and mind. People might feel out of breath or tired for a long time. It can also cause anxiety or depression.
Dealing with these issues needs a broad approach. Doctors can guide on physical rehabilitation and lifestyle changes. For emotional issues, support from loved ones or mental health experts is very helpful.
Support Resources
Having the right support can greatly help in recovery. This includes medical care, educational materials, support groups, and counseling services.
|
Support Resource |
Description |
Benefit |
|---|---|---|
|
Medical Care |
Regular check-ups and monitoring by healthcare professionals. |
Ensures timely intervention for any complications. |
|
Educational Materials |
Information on managing PE, lifestyle changes, and medication. |
Empowers patients with knowledge for self-care. |
|
Support Groups |
Groups for sharing experiences and receiving support from peers. |
Provides emotional support and reduces feelings of isolation. |
By using these resources and staying proactive about health, people can overcome pulmonary embolism challenges. They can live a fulfilling life after their diagnosis.
Special Considerations for High-Risk Groups
It’s important to understand the unique challenges faced by high-risk groups when it comes to pulmonary embolism. Pregnant women, cancer patients, and the elderly are at a higher risk. Their care needs special attention.
Pregnant Women
Pregnant women face a higher risk of pulmonary embolism. This is due to changes in their body, like venous compression and increased blood clotting. The risk is even higher after giving birth, and more so after a cesarean section.
When treating PE in pregnant women, we must weigh the risks and benefits of blood thinners. We choose anticoagulants that are safe for both the mother and the baby.
Cancer Patients
Cancer patients are more likely to develop blood clots, including pulmonary embolism. This is because cancer and its treatment can make blood clot more easily. The risk varies by cancer type, with some cancers being higher risk.
Managing PE in cancer patients requires careful thought about blood thinners. We must consider drug interactions and the need for ongoing prevention of blood clots.
Elderly Individuals
The elderly are also at a higher risk of PE. This is due to decreased mobility, other health conditions, and changes in blood clotting with age. Diagnosing PE in older adults can be tricky because symptoms are often not clear and they may have other health issues.
When treating PE in older adults, we consider their overall health, kidney function, and risk of bleeding. We tailor blood thinner treatment to their specific needs.
|
High-Risk Group |
Risk Factors |
Management Considerations |
|---|---|---|
|
Pregnant Women |
Venous compression, increased coagulability |
Safe anticoagulation during pregnancy |
|
Cancer Patients |
Pro-coagulant effects of malignancy and treatment |
Anticoagulation therapy, possible drug interactions |
|
Elderly Individuals |
Decreased mobility, comorbid conditions, age-related coagulation changes |
Tailored anticoagulation, considering comorbidities and kidney function |
Advances in Pulmonary Embolism Treatment
The treatment for pulmonary embolism is changing fast. New treatments and technologies are coming out. Medical research is making treatments better and more tailored for patients.
New Medications and Therapies
New anticoagulant drugs are a big step forward. They help prevent clots and reduce bleeding risks. Direct oral anticoagulants (DOACs) are popular because they’re easy to use and don’t need constant monitoring.
Thrombolytic therapy has also improved. It now helps dissolve clots more effectively. New treatments aim to fix the root causes of pulmonary embolism, not just the symptoms.
Emerging Technologies
New technologies are helping diagnose and treat pulmonary embolism better. High-resolution CT scans make diagnoses more accurate and timely. Portable devices let doctors monitor patients outside hospitals.
Interventional radiology is also advancing. Techniques like catheter-directed thrombolysis are getting more precise. These advancements improve treatment outcomes and lower risks.
Future Directions in PE Management
The future of managing pulmonary embolism looks bright. Research into PE’s causes will lead to more tailored treatments. Artificial intelligence and machine learning will also improve diagnosis and treatment planning.
Guidelines will soon focus more on preventing PE. This means understanding and addressing risk factors better. Healthcare providers will keep up with these changes to give patients the best care.
Conclusion
Managing pulmonary embolism well is key to better health for those at risk or already affected. Knowing the causes, symptoms, and treatments helps a lot. It cuts down on complications and boosts life quality.
Preventing pulmonary embolism is vital. We must know the dangers of deep vein thrombosis. Spotting symptoms early and taking preventive steps, like when we’re not moving much or after surgery, is important.
It’s critical to keep up with new ways to treat pulmonary embolism. This way, doctors and patients can create plans that fit each person’s needs.
By raising awareness, preventing, and managing well, we can help those with pulmonary embolism get better care and outcomes.
FAQ
What is a pulmonary embolism?
A pulmonary embolism (PE) is a sudden blockage in one of the lung arteries, usually caused by a blood clot that breaks off from a deep‑vein thrombosis (DVT) in the leg and travels to the lungs, and it can be life‑threatening if not treated promptly.
How fast does a blood clot travel from the leg to the lungs?
A clot can travel from the leg to the lungs within minutes to a few hours after it breaks loose, and the speed depends on clot size, how heavily it stresses the heart and lungs, and how quickly circulation carries it.
What are the symptoms of pulmonary embolism?
Common symptoms include sudden shortness of breath, chest pain that worsens with breathing or coughing, rapid heartbeat, coughing (sometimes with blood), lightheadedness or fainting, and pale or bluish‑tinged skin. [web-47][web-48][web-55]
What is Deep Vein Thrombosis (DVT)?
DVT is a blood clot in a deep vein, usually in the leg, and it is a major risk factor for pulmonary embolism because part of this clot can detach and travel to the lungs. [web-54][web-55][web-50]
How is pulmonary embolism diagnosed?
Doctors first assess symptoms and risk factors, then use tests such as D‑dimer blood tests, CT pulmonary angiography, and sometimes lung perfusion scans or echocardiography to confirm a PE. [web-53][web-54][web-57]
What are the treatment options for pulmonary embolism?
Most people are treated with anticoagulant (“blood‑thinner”) medications; in severe cases, thrombolytic drugs, catheter‑directed clot removal, or surgery such as embolectomy may be used, and vena‑cava filters can be placed in selected high‑risk patients. [web-53][web-54][web-58]
How can pulmonary embolism be prevented?
Prevention includes staying active, using compression stockings, avoiding long‑term immobility, managing clotting risk factors, and—when appropriate—taking anticoagulant or mechanical prophylaxis around surgery or hospitalization. [web-54][web-50][web-56]
What are the complications of untreated pulmonary embolism?
Untreated PE can cause sudden cardiac arrest, shock, right‑heart failure, and chronic thromboembolic pulmonary hypertension, and it carries a high risk of death if not recognized and treated quickly. [web-53][web-54][web-58]
Who is at higher risk for pulmonary embolism?
High‑risk groups include people with cancer, heart or lung disease, recent surgery, prolonged immobility, pregnancy, those on estrogen‑based hormones, and older adults or individuals with inherited clotting disorders. [web-54][web-57][web-50]
What are the advances in pulmonary embolism treatment?
Advances include newer oral anticoagulants, catheter‑directed thrombolysis and clot‑removal devices, improved risk‑stratification scores, and protocols that safely allow some low‑risk patients to be treated as outpatients. [web-54][web-56][web-58]
What is the recovery process like for someone with pulmonary embolism?
Recovery typically involves several months or longer of anticoagulation, regular follow‑up, lifestyle changes, and sometimes rehabilitation to manage breathlessness or chronic pulmonary hypertension, alongside emotional support and close monitoring for recurrence. [web-54][web-58][web-50]
References
https://www.ncbi.nlm.nih.gov/books/NBK560551


































