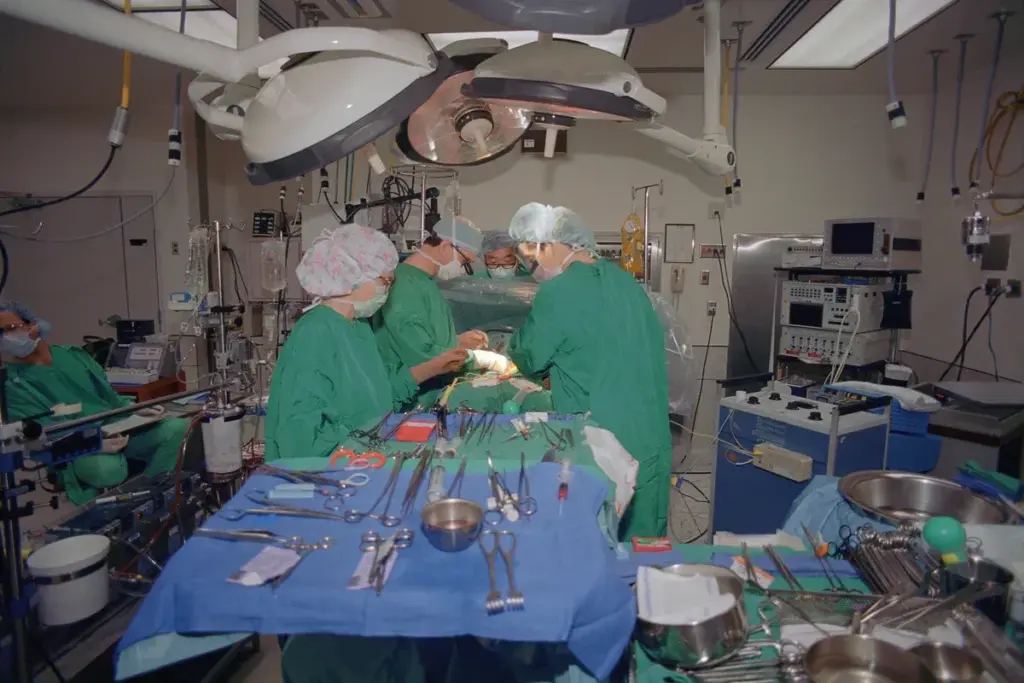
Open-heart surgery is a major medical step that saves many lives. It’s scary to think about, but most people bounce back well. They live longer and feel better, thanks to modern medicine and top hospitals.
People who get open-heart surgery often live as long as healthy folks their age. Studies show that most patients survive the surgery with a 97% success rate in top hospitals. This means a long, healthy life after surgery, if they stay healthy.
For more on how well open-heart surgery works, check out .
Key Takeaways
- Open-heart surgery can significantly improve life expectancy and quality of life.
- Survival rates for open-heart surgery exceed 97% in top hospitals.
- Patients can regain a lifespan similar to healthy individuals of their age group.
- A healthy lifestyle post-surgery is key for long-term survival.
- Advances in cardiac surgery have led to better patient outcomes.
What Happens During Open-Heart Surgery
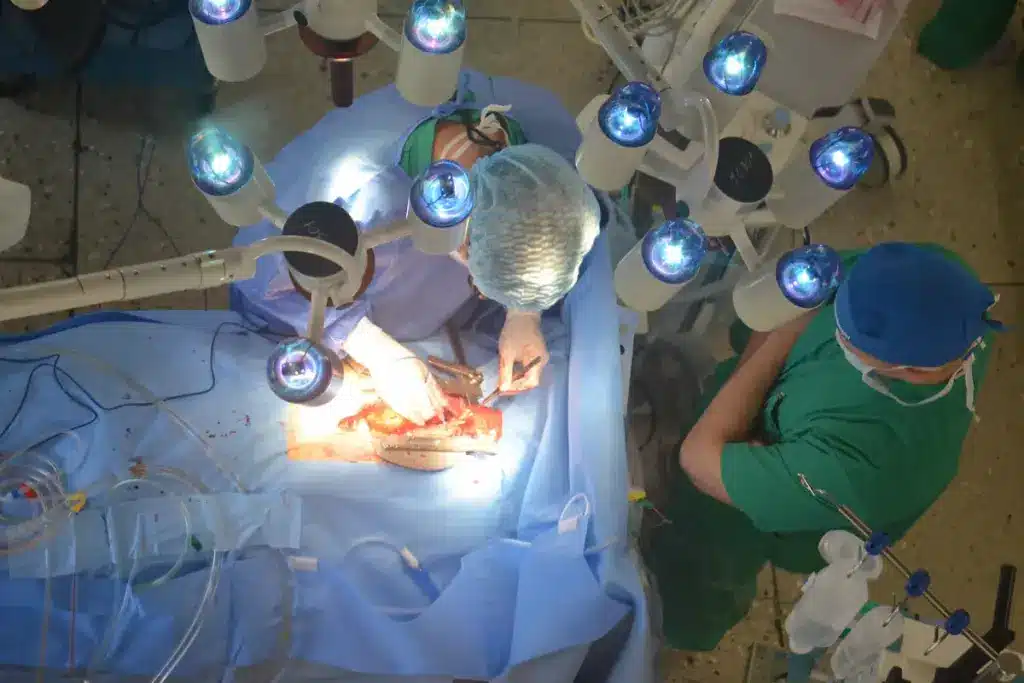
Open-heart surgery is a big deal. It involves cutting open the chest to work on the heart. Knowing what happens is key.
Types of Open-Heart Procedures
There are many open-heart surgeries. Two common ones are coronary artery bypass grafting (CABG) and fixing or replacing heart valves.
- Coronary Artery Bypass Grafting (CABG): This surgery fixes blocked arteries. It helps blood flow better to the heart.
- Valve Repair or Replacement: This fixes or swaps out faulty heart valves.
The Surgical Process
The surgery steps are clear:
- Preparation: The patient gets ready with anesthesia and a chest incision.
- Heart-Lung Machine: A machine takes over the heart and lungs’ jobs during surgery.
- Surgical Intervention: The surgery, like CABG or valve work, is done.
- Recovery: The patient is watched in the ICU then moves to a regular room to heal.
Understanding the details of open-heart surgery helps patients prepare more effectively. It’s important to listen to doctors during this time.
Survival Statistics for Open-Heart Surgery
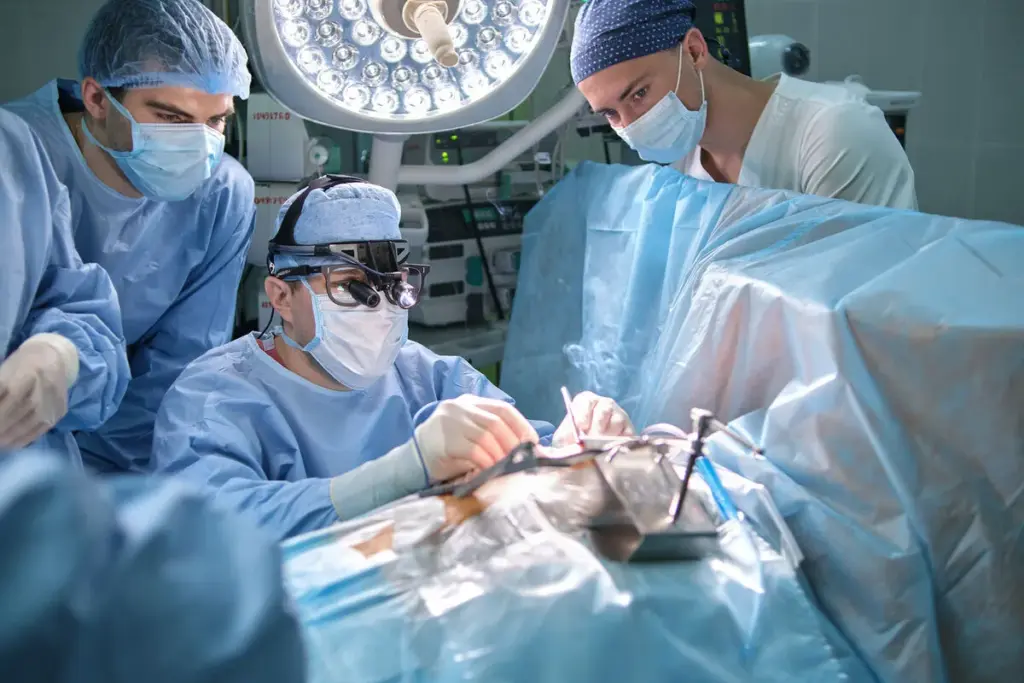
Recent studies have shed light on the survival rates of patients undergoing open-heart surgery. This offers hope for those needing cardiac care. Open-heart surgery has seen big improvements, leading to better survival rates.
In-Hospital Survival Rates
The in-hospital survival rates for open-heart surgery are key. Studies show that most patients survive their initial hospital stay. Survival rates often hit 95% in many cardiac centers. This shows the skill of cardiac surgeons and the progress in post-operative care.
Many factors affect in-hospital survival rates. These include the patient’s health before surgery, the surgery’s complexity, and the quality of care during the stay.
Five-Year Survival Statistics
Looking at long-term outcomes, five-year survival statistics are important. Studies show over 80% of people are alive five years after bypass surgery. This is a big win, showing the surgery’s success in improving long-term survival.
|
Time Frame |
Survival Rate |
|---|---|
|
In-Hospital |
>95% |
|
1 Year |
90-95% |
|
5 Years |
>80% |
|
10 Years |
60-70% |
Ten-Year and Beyond Outcomes
Survival statistics for open-heart surgery are encouraging beyond five years. While rates may drop over time, many patients live more than ten years after surgery.
Every patient’s journey is different. While statistics give a general view, individual results can vary. Yet, the data shows open-heart surgery can greatly extend life for many.
Coronary Artery Disease and Bypass Surgery
Coronary artery disease can cause severe heart blockages. This often requires bypass surgery to fix. The disease narrows or blocks the coronary arteries, which are vital for the heart.
This happens because of a buildup of plaque. Plaque is made of fat, cholesterol, and other substances. It forms on the artery walls.
Understanding Heart Blockages
Heart blockages happen when arteries get too narrow or blocked. This can cause angina, or chest pain, or even a myocardial infarction (heart attack). The blockage’s size and location decide the treatment.
We’ll look at tests like coronary angiography, stress tests, and cardiac CT scans. These help doctors figure out the best treatment.
When Surgery Becomes Necessary
Bypass surgery, or coronary artery bypass grafting (CABG), is needed for severe blockages. Doctors decide on surgery after careful evaluation. They consider the blockages, the patient’s health, and symptoms.
We’ll talk about the surgery’s benefits. It can improve survival rates and quality of life for those with severe disease. The surgery uses a healthy vessel to bypass the blockage, restoring blood flow.
Triple Bypass Surgery: Procedure and Life Expectancy
For many, triple bypass surgery greatly improves life expectancy and quality of life. This surgery grafts new blood vessels onto the heart. It bypasses three blocked arteries, restoring blood flow to the heart muscle.
The Triple Bypass Technique
The triple bypass technique is a complex surgery needing great skill. Surgeons use grafts from the patient’s leg or chest to bypass blocked arteries. This method relieves chest pain and boosts cardiac health.
During surgery, the patient is on a heart-lung machine. This machine takes over the heart and lungs’ functions. The grafts are then attached to the coronary arteries, bypassing blockages and ensuring the heart gets the oxygen and nutrients it needs.
Survival Rate by Age for Triple Bypass
The survival rate for triple bypass surgery varies by age. Younger patients generally have better outcomes than older ones, who may have more health issues. But, better surgical techniques and care have improved results for all ages.
- Patients under 60: High survival rate with significant improvement in life expectancy.
- Patients between 60-70: Good survival rate, with many experiencing a substantial increase in life expectancy.
- Patients over 70: While the risk is higher, many patients in this age group benefit from the surgery, with improved quality of life.
Quality of Life After Surgery
Successful triple bypass surgery and post-operative care can add 15-20 years of healthier life. Patients often see a big improvement in their quality of life. They experience less angina and can exercise more easily.
Lifestyle changes, like diet, exercise, and medication, are key to keeping the surgery’s benefits. Cardiac rehabilitation programs are highly recommended to help patients achieve the best outcomes.
Quadruple Bypass: Managing Severe Coronary Artery Disease
Severe coronary artery disease often needs aggressive treatment, like quadruple bypass surgery. This complex surgery is for those with blockages in four major arteries. We’ll look at when it’s needed, the surgery itself, and what recovery is like.
Indications for Quadruple Heart Bypass
Quadruple bypass surgery is for those with severe disease in four major arteries. This makes it hard for blood to reach the heart, causing symptoms like chest pain or shortness of breath. Doctors decide on surgery after checking with tests like angiography and looking at the patient’s health.
Surgical Complexity and Considerations
Quadruple bypass surgery is very complex because it involves many grafts. Surgeons plan carefully, choosing the best grafts and the right order for the bypasses. They might use advanced techniques, like off-pump surgery, to reduce risks.
Recovery Timeline and Expectations
Recovery from quadruple bypass surgery takes about 5 to 7 days in the hospital. Patients will slowly get better over weeks, with full recovery taking months. A good rehab program is key to getting back to normal.
Patients can expect to live 15-20 years longer after quadruple bypass surgery. The recovery includes watching your health closely, taking medicine, and making lifestyle changes. Here’s what to expect:
- Immediate Post-Surgery: Monitoring in ICU
- Short-Term Recovery (6-12 weeks): Gradual return to normal activities
- Long-Term Recovery (3-6 months): Full recovery and rehabilitation
|
Procedure |
Average Recovery Time |
Life Expectancy Gain |
|---|---|---|
|
Quadruple Bypass |
3-6 months |
15-20 years |
|
Triple Bypass |
2-5 months |
10-15 years |
|
Double Bypass |
1-3 months |
5-10 years |
We’ve covered the main points of quadruple bypass surgery, including when it’s needed, the surgery itself, and what to expect during recovery. Knowing these details helps patients prepare for this big surgery.
Quintuple Bypass Surgery: The Most Extensive Intervention
Quintuple bypass surgery is the most complex coronary artery bypass grafting (CABG) procedure. It involves five grafts to restore blood flow to the heart. This surgery is for patients with severe coronary artery disease, having multiple blockages in their coronary arteries.
When Five Grafts Are Required
Doctors decide on quintuple bypass surgery when a patient’s heart disease is very severe. They need multiple grafts to ensure enough blood flow to the heart. This decision is made after tests like angiograms and echocardiograms show the extent of the disease.
The reasons for quintuple bypass surgery include:
- Multiple blockages in the coronary arteries
- Significant reduction in heart function due to coronary artery disease
- Presence of symptoms such as angina or shortness of breath
- Failure of other treatments, such as angioplasty or medication, to manage the condition
Survival Outcomes for Complex Bypasses
Survival after quintuple bypass surgery depends on several factors. These include the patient’s health, any other health issues, and how complex the surgery is. Thanks to better surgical techniques and care, outcomes have improved.
Research shows that:
- The survival rate for quintuple bypass surgery is similar to other complex heart surgeries.
- Having to have the surgery again increases the risk of death in the short and long term.
- Patients with fewer health problems and better heart function before surgery tend to do better.
Long-Term Prognosis
The long-term outlook for patients after quintuple bypass surgery varies. It depends on lifestyle changes, sticking to medication, and other health conditions. Patients who make big lifestyle changes and follow their care plan tend to do better over time.
Important factors for long-term health include:
- Dietary changes and heart health
- Regular exercise and joining cardiac rehab programs
- Staying on medication and attending follow-up appointments
Understanding the complexities and outcomes of quintuple bypass surgery helps patients and doctors make better treatment choices.
Life Expectancy After a Widowmaker Heart Attack
The term ‘widowmaker heart attack’ means a blockage in the left main coronary artery. This is very dangerous and can be deadly if not treated quickly. The left main artery is key to the heart, and a blockage can cause a lot of damage.
Understanding the Left Main Coronary Artery Blockage
The left main coronary artery is vital. It splits into the left anterior descending and circumflex arteries. These arteries supply a big part of the heart with blood. A blockage here can cause serious heart damage.
Quick medical help is essential to fix the blockage and reduce damage. Studies show that fast treatment, like surgery or angioplasty, can greatly improve survival chances. The blockage’s complexity and the patient’s health are key in choosing the right treatment.
Immediate Survival Rates
Thanks to new medical tech and emergency systems, survival rates for widowmaker heart attacks have gone up. Quick treatment is vital for survival. Studies show that those who get help fast have a much better chance of living.
- Fast response and emergency care boost survival chances.
- Advanced cardiac life support during transport is key.
- In-hospital treatment, like surgery or angioplasty, is vital for survival.
Long-Term Life Expectancy
Long-term survival after a widowmaker heart attack depends on many things. These include the heart damage, the first treatment’s success, and sticking to post-treatment care and lifestyle changes. Staying healthy and taking medicine as directed are important for better long-term results.
“Survival after a widowmaker heart attack is significantly influenced by the patient’s ability to adopt a healthier lifestyle and comply with prescribed treatments.”
Patients who get through surgery or angioplasty and stick to rehab often live longer. It’s important to keep up with doctor visits to check on heart health and adjust treatments as needed.
Age as a Critical Factor in Cardiac Surgery Outcomes
Age is a key factor in how well patients do after cardiac surgery. As people get older, their bodies change in ways that affect their heart health.
Open-Heart Surgery Survival Rate by Age
Age affects how likely patients are to survive open-heart surgery. Even though older patients might face more risks, better surgery and care have helped improve results for everyone.
We see that:
- People under 60 usually have a lower risk of dying or facing complications.
- Those between 60 and 70 might face a bit higher risks, but they can often do well.
- Patients over 70 have higher risks, but many can have good outcomes with the right care.
Special Considerations for Patients Over 70
For those over 70, several things can affect how well they do after surgery. These include:
- Health problems like diabetes, high blood pressure, or COPD.
- Being frail, which can make recovery harder.
- How well they can follow doctor’s orders after surgery.
It’s vital to carefully check patients over 70 before surgery and tailor their care to their needs.
Outcomes for Younger Patients
Younger patients usually do better because they have fewer health problems. But, we must think about:
- How long the surgery will last.
- How their lifestyle might affect their heart in the future.
- The chance they might need more surgeries later.
Knowing these things helps us give care that meets their short-term and long-term needs.
Heart Function and Its Impact on Post-Surgical Outcomes
The heart’s ability to function before surgery is key to how well a patient does after surgery. We look at how heart function affects recovery and survival.
Ejection Fraction as a Predictor
Ejection fraction (EF) shows how well the heart pumps blood. A lower EF means the heart isn’t pumping as much. This can make recovery harder and affect long-term health.
Research shows patients with a higher EF do better after surgery. They have lower death rates and fewer problems. But, a low EF means patients need closer watch and more care after surgery.
Pre-Existing Heart Damage
Damage to the heart before surgery, like from heart attacks or high blood pressure, affects recovery. How much damage there is and how the heart adapts is important for predicting how well a patient will do.
Doctors can plan treatment better by knowing how much damage there is. This can help improve outcomes.
Recovery of Cardiac Function
How well the heart recovers after surgery varies. It depends on the heart condition, the surgery, and care after surgery. Some patients see big improvements, while others don’t.
Rehab and making healthy lifestyle choices can help the heart recover. This can lead to better results for patients.
|
Heart Function Measure |
Impact on Post-Surgical Outcomes |
Clinical Considerations |
|---|---|---|
|
Ejection Fraction (EF) |
Lower EF correlates with higher risk of complications and mortality |
Close monitoring and intensive post-operative care for low EF patients |
|
Pre-Existing Heart Damage |
Affects patient prognosis and recovery trajectory |
Tailored treatment plans based on extent of heart damage |
|
Recovery of Cardiac Function |
Variable among patients; influenced by condition and care |
Rehabilitation programs and lifestyle changes to support recovery |
Comorbidities Affecting Life Expectancy After Heart Surgery
Having other health conditions can change life expectancy after heart surgery. These conditions, or comorbidities, happen along with the main heart disease needing surgery.
Diabetes and Surgical Outcomes
Diabetes is a big comorbidity that can affect surgery results. Research shows that people with diabetes might live less long after heart surgery than those without it. This is because diabetes can harm heart health and increase surgery risks.
A study in the Journal of Thoracic and Cardiovascular Surgery found that diabetic patients had more risks and deaths after CABG than non-diabetic ones.
Kidney Function Considerations
Kidney health is also key for life expectancy after heart surgery. Those with poor kidney function or CKD face more risks after surgery.
Kidney issues can affect surgery in many ways. This includes managing fluids, how medicines are cleared, and the body’s stress response to surgery.
|
Kidney Function Status |
Impact on Life Expectancy |
|---|---|
|
Normal Kidney Function |
Less impact on life expectancy |
|
Mild CKD |
Moderate impact |
|
Severe CKD or Dialysis |
Significant impact, higher risk of complications |
Respiratory Conditions and Recovery
Respiratory issues, like COPD, can also impact recovery and life expectancy after heart surgery. Patients with COPD might face more respiratory problems after surgery, affecting their survival chances.
Improving respiratory health before surgery and careful care after it are key to reducing these risks.
How Long Can You Live With Blocked Arteries Without Surgery?
Living with blocked arteries without surgery is a serious health issue. It can lead to heart attacks and strokes if not treated right.
Medical Management Options
For those with blocked arteries, medical care is key. It includes changing your diet and being more active. It also involves taking medicine to control symptoms and slow the disease.
Medications are very important. They help lower cholesterol, control blood pressure, and stop blood clots.
|
Medication Type |
Purpose |
Examples |
|---|---|---|
|
Statins |
Lower cholesterol |
Atorvastatin, Simvastatin |
|
Beta-blockers |
Reduce blood pressure and heart rate |
Metoprolol, Atenolol |
|
Antiplatelet agents |
Prevent blood clots |
Aspirin, Clopidogrel |
Risks of Postponing Surgical Intervention
Medical care can be effective, but there are risks if you wait too long for surgery. Waiting can cause blockages to get worse, raising the risk of heart attack or stroke.
It’s important for patients to talk to their doctors. They need to decide the best treatment based on their health and medical history.
Quality of Life Considerations
Living with blocked arteries without surgery needs careful management to keep your quality of life good. You must follow your treatment plan, make lifestyle changes, and watch your health closely.
Understanding your treatment options and the risks of waiting for surgery helps you make better choices for your care.
Reoperative Cardiac Surgery: Increased Mortality Risk
Reoperative cardiac surgery is often needed but comes with a higher risk of death than the first surgery. This risk is due to the surgery’s complexity, the patient’s health, and past surgeries. We will look at the challenges of reoperative cardiac surgery and how to improve patient results.
First-Year Survival After Reoperation
Reoperative cardiac surgery has a high risk of death in the first year. About 21.2% of patients don’t make it past the first year. This shows the importance of choosing patients carefully and planning surgeries well.
The first year’s survival depends on the patient’s age, health, and the surgery’s complexity. Knowing these factors helps in finding ways to increase survival rates.
Technical Challenges of Repeat Procedures
Reoperative cardiac surgery faces big technical hurdles. These include adhesions, changed anatomy, and possible heart function issues. Such challenges require skilled surgeons and detailed planning for the best results.
Using advanced surgical methods and technology can help overcome these challenges. For example, custom cardiopulmonary bypass strategies can reduce complications.
Strategies to Improve Outcomes
To better outcomes in reoperative cardiac surgery, we need a multi-faceted approach. This includes better pre-op care, advanced surgery, and full post-op management.
One way to improve results is through multidisciplinary care teams. These teams include cardiologists, surgeons, and other experts. This teamwork ensures patients get care that fits their needs.
|
Time Frame |
Survival Rate |
|---|---|
|
1 Year |
78.8% |
|
5 Years |
55% |
|
10 Years |
35% |
Long-Term Side Effects of Open-Heart Surgery
The journey doesn’t end after open-heart surgery; patients often face various long-term challenges. While open-heart surgery can be lifesaving, understanding its long-term side effects is key for both patients and healthcare providers.
Physical Complications
Physical complications after open-heart surgery can be significant and varied. Some patients may experience chronic pain from the surgical incision or sternotomy. Others might have heart function issues like arrhythmias or irregular heartbeats.
Also, some individuals may develop adhesions or scar tissue that can cause future complications. In some cases, patients might get post-pericardiotomy syndrome, which is inflammation of the heart sac.
Cognitive and Psychological Effects
Open-heart surgery can also affect patients’ minds and emotions. Some may see cognitive decline, including memory, concentration, or processing issues. The surgery, anesthesia, and health conditions before surgery might play a role in these effects.
Psychologically, patients may struggle with depression or anxiety. The stress of major surgery and recovery can harm mental health. It’s vital for healthcare providers to offer support and resources to manage these effects.
We know every patient’s experience with open-heart surgery is different. Being aware of these possible long-term side effects can help manage and reduce them. Understanding these complications helps patients prepare for their journey and work with their healthcare team for the best outcomes.
Lifestyle Changes That Add Years After Cardiac Surgery
After cardiac surgery, making healthy lifestyle changes is key. It helps improve outcomes and adds years to life. We’ll look at important lifestyle changes that boost long-term health and well-being.
Dietary Modifications for Cardiovascular Health
Eating a heart-healthy diet is vital after surgery. Focus on fruits, vegetables, whole grains, and lean proteins. Limit saturated fats, cholesterol, and sodium too. The DASH diet and Mediterranean diet are great for heart health.
A healthy diet is a must for heart health. It lowers heart disease risk and boosts well-being.
“The Mediterranean diet has been shown to reduce cardiovascular events and improve survival in patients with heart disease.”
Exercise and Cardiac Rehabilitation Programs
Regular exercise is key for recovery and health after surgery. Cardiac rehabilitation programs offer safe exercise and education. They help lower death rates and improve life quality.
- Exercise training to improve cardiovascular function
- Education on risk factor modification
- Nutritional counseling
- Stress management techniques
Medication Adherence and Follow-Up Care
Following medication instructions is critical for heart health after surgery. Patients must understand their meds and take them as directed. Regular check-ups with healthcare providers are also vital for monitoring and adjusting treatment.
Smoking Cessation and Alcohol Moderation
For smokers, quitting is a major step for better heart health. Smoking cessation programs can help. Also, drinking alcohol in moderation is important to avoid heart harm.
By adopting these lifestyle changes, patients can greatly improve after surgery. It’s about diet, exercise, meds, and more. We urge patients to work with their healthcare team for a personalized plan. This promotes long-term heart health.
Conclusion: Open-Heart Surgery Often Extends Instead of Reduces Life Expectancy
Open-heart surgery is a big step in medical care. It can really improve life quality and length for many. We’ve looked at different parts of open-heart surgery, like types of surgeries, survival rates, and what affects results.
It’s clear that open-heart surgery usually doesn’t shorten life. Many patients live as long as healthy people of their age. Knowing how open-heart surgery works and what affects it helps patients make better choices about their health.
Choosing to have open-heart surgery depends on many things. These include how bad heart disease is, overall health, and lifestyle. With the right care, many can live a long and healthy life after surgery.
FAQ
What is the survival rate for open-heart surgery?
Open-heart surgery has a high survival rate. Most patients survive the surgery, with rates between 95% to 98%. Long-term survival depends on age, health, and the surgery type.
How long can you live after triple bypass surgery?
Life expectancy after triple bypass surgery varies. It depends on age and health. Studies suggest patients can live 10 to 15 years or more after surgery.
What is the life expectancy after a widowmaker heart attack?
Life expectancy after a widowmaker heart attack varies. It depends on the blockage’s severity, treatment success, and overall health. Prompt treatment can help many patients live active lives.
How long can you live with blocked arteries without surgery?
Living with blocked arteries without surgery varies. It depends on blockage severity, health, and medical management. Lifestyle changes and medication can manage symptoms, but surgery might be needed.
What are the long-term side effects of open-heart surgery?
Open-heart surgery can have long-term side effects. These include physical issues like infections or adhesions, and mental health effects like anxiety or depression. Yet, many patients see a big improvement in their life quality after surgery.
How does age impact the outcomes of cardiac surgery?
Age is a big factor in cardiac surgery outcomes. Older patients face higher risks but can have successful surgeries and better quality of life. Younger patients generally have better outcomes and longer life expectancy.
What is the role of ejection fraction in predicting post-surgical outcomes?
Ejection fraction is a heart function measure that predicts outcomes. Patients with lower ejection fractions may face higher risks. But, other factors like health and surgery type also matter.
How do comorbidities affect life expectancy after heart surgery?
Comorbidities like diabetes, kidney issues, and respiratory diseases can affect life expectancy after heart surgery. Managing these conditions is key to better outcomes and quality of life.
What lifestyle changes can improve outcomes after cardiac surgery?
Healthy lifestyle changes can greatly improve outcomes after cardiac surgery. This includes dietary changes, exercise, and sticking to medication. Cardiac rehabilitation programs also help in recovery and maintaining health.
What is the survival rate for quadruple bypass surgery?
Quadruple bypass surgery survival rates are generally good but may be lower than simpler procedures. Survival depends on age, health, and coronary artery disease severity.
What is quintuple bypass surgery, and when is it necessary?
Quintuple bypass surgery involves five grafts and is needed for severe coronary artery disease. It’s for patients with multiple blockages needing bypasses to restore heart blood flow.
References:
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://pubmed.ncbi.nlm.nih.gov/8670522/




 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























