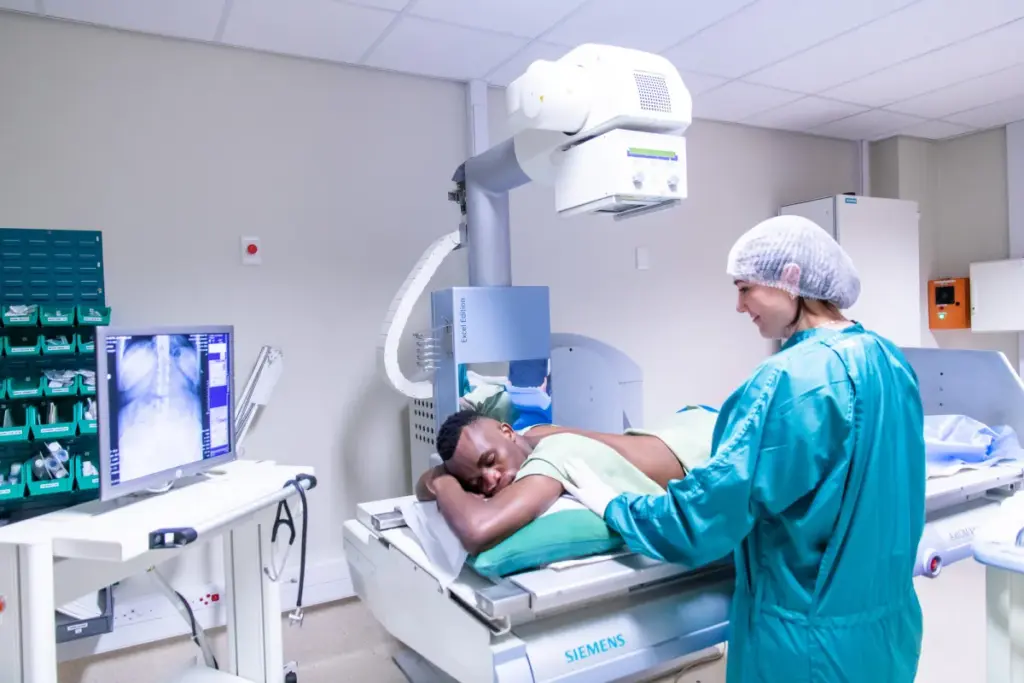
Medical interventions are often lifesaving. But, when used too much or without clear benefits, they have big downsides.
Worried about radiology interventional procedures ? Learn about scary complications and vital life-saving tips for a successful recovery.Studies reveal that up to 30% of healthcare costs worldwide are due to overuse.
At , we focus on top-notch, ethical, and new care. We aim to skipmedical interventions that aren’t needed. This way, our patients get the best treatment possible.
Key Takeaways
- Medical overuse accounts for up to 30% of global healthcare spending.
- Unnecessary interventions can undermine patient outcomes.
- Effective care requires a balanced approach to medical interventions.
- We prioritize delivering high-quality, ethical care.
- Avoiding unnecessary interventions is key for patient-centered care.
Understanding What Interventions Are in Healthcare and Beyond
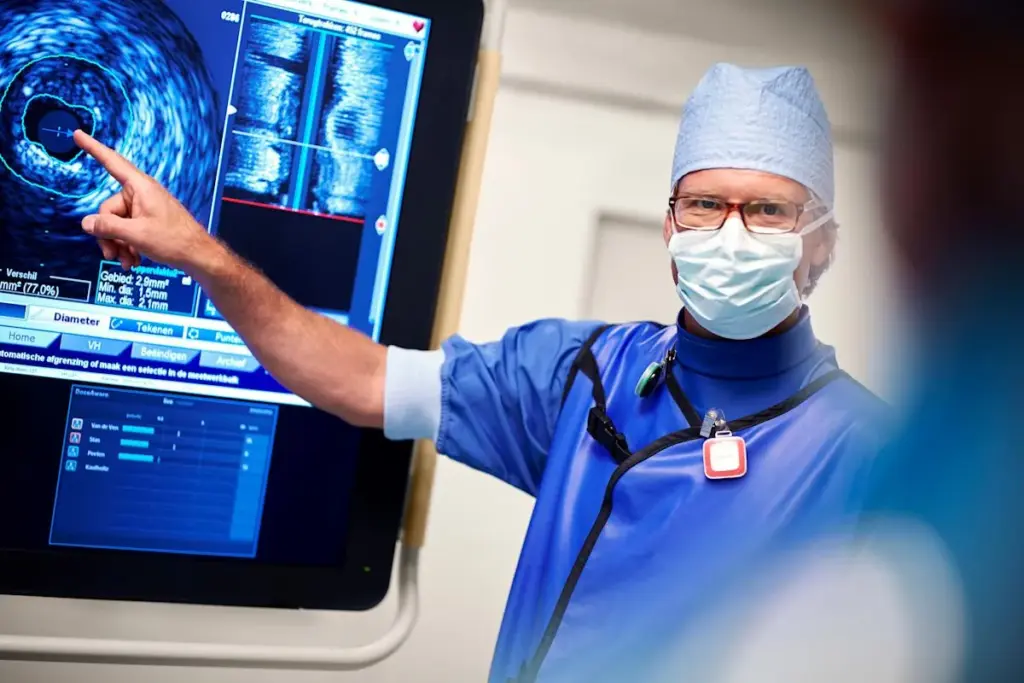
Interventions in healthcare come in many forms and uses. They are key in medical care, aimed at diagnosing, treating, or preventing health issues.
Medical Interventions Defined
Medical interventions are actions by healthcare pros to manage or treat health conditions. They include surgical procedures, pharmacological treatments, and behavioral therapies. The goal is to better patient outcomes, ease symptoms, and improve life quality.
Medical interventions aren’t just for physical health; they also cover mental health and prevention. For example, addiction treatments might include medication, counseling, and support groups.
Types of Interventions in Modern Healthcare
In today’s healthcare, interventions are categorized by their nature and purpose. These include:
- Diagnostic interventions, like imaging tests and biopsies, to find the cause of symptoms.
- Therapeutic interventions, including medications, surgeries, and physical therapy, to treat or manage health conditions.
- Preventive interventions, like vaccinations and screenings, to prevent illnesses or detect them early.
This variety of interventions lets healthcare providers tailor care to each patient’s needs, making care more effective.
|
Type of Intervention |
Purpose |
Examples |
|---|---|---|
|
Diagnostic |
Identify cause of symptoms |
Imaging tests, biopsies |
|
Therapeutic |
Treat or manage conditions |
Medications, surgeries, physical therapy |
|
Preventive |
Prevent illnesses or early detection |
Vaccinations, screenings |
Addiction and Behavioral Interventions
Addiction and behavioral interventions are key in healthcare, focusing on substance abuse and mental health. These interventions often combine medical treatment, counseling, and social support.
Professional interventions for addiction can be very effective when they match the individual’s needs. They might include medication-assisted treatment, cognitive-behavioral therapy, and support groups. It’s important to understand the cons of addiction treatment to provide full care.
By understanding the complexities of addiction and the available interventions, healthcare providers can offer better support to those struggling with substance abuse.
The Financial Burden: How Interventions Strain Healthcare Systems
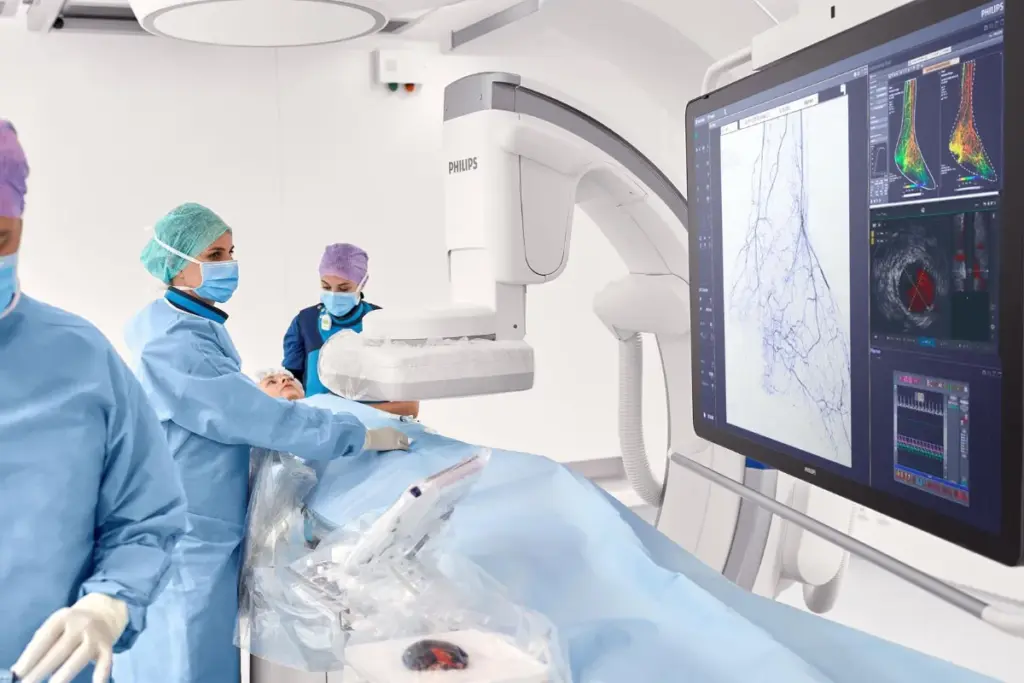
The cost of medical interventions is huge and affects many areas. It puts a strain on healthcare systems, patients, and their families. This issue is complex and needs careful attention.
The 30% Problem: Medical Overuse Statistics
Up to 30% of healthcare spending is due to overuse. This is a big problem for healthcare systems. It makes costs go up and takes away from more important needs.
Many medical interventions are not needed or are done twice. This adds to costs without helping patients much.
Medical overuse is a big issue worldwide. It affects healthcare systems and costs a lot. It also hurts patients’ finances and raises insurance prices. We need to look at research, like, to understand it better.
Impact on Patient Finances and Insurance Premiums
Medical interventions also hurt patients and their families. Unnecessary procedures can cause a lot of financial stress. Higher healthcare costs also mean higher insurance premiums for everyone.
While some medical interventions are vital, overuse is harmful. It affects healthcare systems and patients. By being more careful with medical interventions, we can make healthcare better and more fair for everyone.
Patient Safety Concerns: Physical Harm from Unnecessary Procedures
Patient safety is at risk when medical procedures are not justified. This can lead to physical harm. We must think about the dangers of unnecessary treatments, which can harm patients a lot.
Complications from Surgical Interventions
Surgeries are sometimes needed but can cause big problems. These include infections, bleeding, and bad reactions to anesthesia. Unnecessary surgeries put patients at risk and add to healthcare costs.
We know surgeries are key in healthcare. But, when they’re not needed, they can cause harm. It’s essential to carefully consider the benefits and risks associated with any surgical procedure.
Adverse Drug Reactions and Medication Errors
Bad drug reactions and mistakes with medication are big worries. Unnecessary medication can cause problems with other drugs or make health issues worse.
Interventions, like those for addiction, need careful handling to avoid bad outcomes. We must make sure any treatment is based on solid evidence and fits the patient’s needs.
To lower the risk of harm from unnecessary medical steps, we need to work together. Healthcare providers, patients, and policymakers must put patient safety first.
Hospital-Acquired Infections: A Direct Consequence of Interventional Care
Interventional care saves lives but comes with a cost. Hospital-acquired infections are a big worry in healthcare. They harm patients and put a strain on resources.
Prevalence of Hospital-Acquired Infections
About 7% of hospitalized patients worldwide get these infections. This shows we need strong infection control to fight this problem.
Long-term Health Consequences
Hospital-acquired infections can have serious long-term effects. They lead to longer hospital stays, higher costs, and more deaths. Patients often need more treatment, like extended antibiotic therapy.
It’s key to understand these risks to prevent infections. By focusing on prevention and better infection control, we can lower these infections. This improves patient care.
Interventions are vital for treating many conditions. But, they also come with risks, like infections. We must weigh the benefits against the risks.
By being careful and proactive, we can lessen the harm from interventions. This means treating patients well without causing more harm.
The Psychological Impact of Medical Interventions on Patients
Modern healthcare is complex, and understanding the mental effects of medical treatments is key. These treatments, though often necessary, can deeply affect a patient’s mental health.
Anxiety and Depression Following Major Interventions
Major medical treatments can cause a lot of anxiety and depression. The stress of the procedure and the uncertainty of the outcome can make patients feel scared and worried. Healthcare providers must recognize these effects and offer the right support.
Research shows that patients after big surgeries or treatments are more likely to get anxious or depressed. The emotional struggle can be as tough as the physical one during recovery.
Post-Traumatic Stress from Intensive Medical Procedures
Intensive medical procedures, like those in critical care or emergencies, can cause PTSD. Being in a life-threatening situation or going through a big procedure can be very traumatic. It can leave deep psychological scars.
Healthcare providers need to watch for early PTSD signs and offer the right psychological help. This can include counseling, therapy, and sometimes medication.
By understanding and addressing the mental effects of medical treatments, we can help patients recover better. This improves their quality of life.
Overdiagnosis and Overtreatment: When More Care Becomes Harmful
Modern healthcare faces big challenges like overdiagnosis and overtreatment. These issues harm patients and make healthcare systems less efficient.
Overdiagnosis means finding conditions that won’t cause problems or death. Then, treating these conditions can cause harm and cost a lot of money.
Excessive Imaging and Cancer Risk
Too much use of imaging like CT scans is a big problem. It can expose patients to harmful radiation and raise cancer risk.
A study in the Journal of the National Cancer Institute showed CT scans can increase cancer risk, mainly in kids. This shows we need to use imaging wisely, weighing its benefits against risks.
Cascade Effects: When One Intervention Leads to Many
Overtreatment can start a chain of more treatments, each with risks. For example, a false-positive test can lead to more tests and treatments.
Here’s a table showing how one treatment can lead to many others:
|
Intervention |
Potential Outcome |
Subsequent Action |
|---|---|---|
|
Initial Screening Test |
False-positive result |
Additional diagnostic testing |
|
Diagnostic Testing |
Inconclusive results |
Biopsy or invasive procedure |
|
Biopsy or Invasive Procedure |
Complications arise |
Corrective surgery or treatment |
Understanding these effects helps doctors make better choices. They can try to avoid unnecessary treatments.
To fix overdiagnosis and overtreatment, we need a few things. We must use medical care wisely, keep patients safe, and improve care quality. This way, medical help can be helpful, not harmful.
Antibiotic Resistance: A Growing Crisis Fueled by Interventional Approaches
Antibiotic resistance is growing worldwide, and healthcare’s use of antibiotics is a big reason. The more we use antibiotics, the more bacteria become resistant. This is a big danger to our health.
Factors Contributing to Resistance
Surgeries and tests often need antibiotics to prevent infections. But, this use makes bacteria stronger. Using too many antibiotics is a big problem.
Here are some reasons why antibiotic resistance grows:
- Using too many broad-spectrum antibiotics
- Not having good programs to manage antibiotics
- Not finding new antibiotics
- Poor infection control in hospitals
The Global Health Threat of Antimicrobial Resistance
Antimicrobial resistance (AMR) is a big problem worldwide. It affects not just hospitals but also our communities. It has many bad effects on society and the economy.
|
Impact Area |
Consequences of AMR |
|---|---|
|
Healthcare |
More sickness and death from resistant infections |
|
Economy |
Big costs from long treatments and lost work |
|
Society |
Higher risk of infections in everyday life, hurting the weak |
To fight AMR, we need many strategies. We must improve how we use antibiotics, better control infections, and find new medicines. By working together, we can lessen the danger of antimicrobial resistance.
Resource Allocation Problems: How Interventions Divert from Essential Services
Interventions are key in some medical cases but can cause big problems with resource use in healthcare. They can take a lot of money away from important health services.
Putting too much focus on interventions can mess up how health resources are spread out. This messes with the money for early disease prevention and makes health care harder to get for more people.
Impact on Preventive Care Funding
Preventive care is vital for catching and managing diseases early. But, money for interventions can take away from funds for prevention.
For example, a lot of health budgets go to advanced treatments. These treatments are key for some conditions, but they can leave less money for public health and prevention.
|
Healthcare Resource |
Intervention Focus |
Preventive Care Focus |
|---|---|---|
|
Funding Allocation |
High investment in advanced treatments |
Increased budget for public health initiatives |
|
Resource Distribution |
Concentrated on interventional procedures |
Balanced distribution for preventive measures |
|
Patient Outcomes |
Effective for specific medical conditions |
Improved overall population health |
Inequitable Access to Healthcare Resources
Putting interventions first can make health care unfair. Some groups get more access to treatments, while others miss out on prevention.
To fix this, health care needs to find a balance. We must think about both interventions and prevention. This way, everyone can get the health care they need.
So, we must think about if interventions are worth it when we look at how we use health care resources. By understanding our choices, we can make health care fairer and better for everyone.
Healthcare Provider Burnout: The Hidden Cost of Excessive Interventions
Modern healthcare faces a crisis due to too many interventions. Healthcare workers face more than just a heavy workload. They also deal with the moral and emotional impact of their actions.
Moral Injury Among Medical Professionals
Moral injury, once known mainly in veterans, now affects healthcare workers. It’s the distress from actions that go against their moral code. Healthcare workers may feel forced to do things they think are wrong for their patients.
Key factors contributing to moral injury include:
- Performing unnecessary procedures
- Feeling pressured by hospital or insurance policies
- Witnessing or being involved in adverse events due to interventions
This moral injury can cause burnout, lower job satisfaction, and make workers less committed to their jobs.
Workforce Shortages and Quality of Care Decline
Burnout and moral injury lead to a shortage of healthcare workers. As more leave or work less, those who stay have to do more. This makes burnout worse.
The consequences include:
- A decline in the quality of care due to fatigued staff
- Increased medical errors
- Reduced patient satisfaction
We need to rethink how we do medical interventions. We should focus on what’s necessary, care that puts patients first, and the well-being of healthcare workers.
By challenging the usual ways of healthcare, we can lessen the harm of too many interventions. This will help create a better environment for both patients and healthcare workers.
Addiction Interventions: Examining the Cons of Addiction Treatment Approaches
Interventions in addiction treatment are complex, with both good and bad sides. They can help people fight addiction, but they also carry risks.
When Professional Interventions Backfire
Professional interventions can sometimes harm those struggling with addiction. Confrontational approaches might make people defensive and less willing to get help. We need to think about how to make interventions work better for each person.
Confrontational Methods and Their Psychological Impact
Confrontational methods in interventions can deeply affect people’s minds. They can cause more anxiety, depression, and even PTSD. We must think about the benefits and risks and look for gentler ways to help.
Relapse Risks Following Forced Interventions
Forced interventions might make people more likely to relapse. Feeling pushed into treatment can make them less likely to stay in recovery. We should aim to create a supportive space where people want to get help.
In conclusion, interventions are valuable in fighting addiction, but we must know their downsides. By understanding these risks, we can make treatment more effective and caring.
Cultural and Social Considerations in Intervention Approaches
The success of intervention strategies often depends on understanding cultural and socioeconomic nuances. It’s key to consider the diverse backgrounds and social factors that affect patient outcomes.
Effective interventions need more than medical skills. They require a deep understanding of the cultural and social contexts. This includes recognizing cultural competency gaps and addressing socioeconomic factors.
Cultural Competency Gaps in Intervention Models
Cultural competency gaps happen when healthcare providers don’t understand diverse cultural backgrounds. These gaps can cause misunderstandings, misdiagnoses, and wrong treatment plans.
- Inadequate cultural training for healthcare providers
- Lack of culturally sensitive intervention materials
- Failure to incorporate cultural beliefs and practices into treatment plans
To close these gaps, healthcare organizations need to invest in cultural competency training. This means understanding different cultural beliefs about health and being aware of one’s own biases.
“Cultural competence is not just about being sensitive to different cultures; it’s about understanding how those cultures impact the way patients interact with the healthcare system.”
renowned expert in cultural competency
Socioeconomic Factors Affecting Intervention Outcomes
Socioeconomic factors like income, education, and access to resources greatly impact intervention outcomes. Patients from lower socioeconomic backgrounds often face barriers to care and achieving positive health outcomes.
|
Socioeconomic Factor |
Impact on Intervention Outcomes |
|---|---|
|
Low Income |
Limited access to healthcare resources and medications |
|
Limited Education |
Difficulty understanding treatment plans and health information |
|
Poor Access to Resources |
Inability to afford healthy lifestyle choices and preventive care |
To tackle these challenges, healthcare providers must take a holistic approach to care. This includes working with community organizations, providing patient education, and advocating for health equity policies.
By acknowledging and addressing cultural and social considerations, we can create more effective intervention strategies. These strategies are tailored to the unique needs of diverse patient populations. This improves health outcomes and enhances the quality of care.
The Prevention Paradox: How Focus on Intervention Undermines Preventive Care
The prevention paradox is a big problem in healthcare. It shows that focusing too much on treatments can hurt preventive care. This is a worrying trend where the push for treatments makes preventive care less important.
We look into this paradox and its effects on patient health. We compare the value of preventive care to treatment-focused approaches. Understanding the prevention paradox helps us see the need for a balanced healthcare approach. This approach should value both prevention and treatment when needed.
Increased Mortality Risk from Intervention-Centric Models
Models that focus on treatments can increase the risk of death. The says patient safety is key. They point out that unsafe care causes a lot of harm and death worldwide.
Surgeries, though lifesaving, can have fatal complications. Also, using too many antibiotics in treatments can lead to antibiotic resistance. This makes patient care even harder.
The Value of Preventive Medicine vs. Interventional Approaches
Preventive medicine aims to stop diseases before they start. This can lead to better health outcomes and lower healthcare costs. On the other hand, treatments are often used after diseases have developed.
We need to consider the benefits of preventive care against the need for treatments. For example, vaccines and screenings can greatly lower disease rates and improve health for many.
By focusing more on preventive care, we can lessen our need for treatments. This could also reduce some of the risks that come with treatments.
Balancing Act: Are Interventions Effective Despite Their Disadvantages?
Interventions have both good and bad sides. Healthcare providers must think about these carefully. This helps ensure patients get the best care.
Interventions work well when they follow the latest research. This means decisions are based on solid evidence, not just guesses. Following this approach helps avoid risks and boosts benefits.
Evidence-Based Criteria for Necessary Interventions
Deciding when to intervene needs careful thought. We look at the patient’s health, the latest research, and what the patient wants. This makes sure interventions are right for each person.
“The key to successful intervention is not just the intervention itself, but how it is tailored to the individual patient’s needs and circumstances.”
Healthcare Expert
Using evidence-based criteria helps interventions be precise and effective. This reduces risks and improves health outcomes for patients.
|
Criteria |
Description |
Benefits |
|---|---|---|
|
Clinical Guidelines |
Based on the latest research and clinical expertise |
Ensures interventions are evidence-based and effective |
|
Patient Assessment |
Comprehensive evaluation of the patient’s condition and needs |
Tailors interventions to individual patient needs |
|
Patient Preferences |
Takes into account the patient’s values and preferences |
Improves patient satisfaction and adherence to treatment |
Measuring Intervention Success Beyond Short-Term Outcomes
Success of interventions needs a long view. We look at more than just quick results. We consider how they affect health and happiness over time.
It’s important to see both the immediate and long-term effects of interventions. This way, we make sure they truly help in the long run.
In conclusion, interventions can be very effective. They work best when based on solid evidence and looked at over time. By balancing their good and bad sides, we can make them better for everyone.
Alternative Approaches to High-Intervention Healthcare Models
Healthcare is exploring new ways to tackle addiction and professional interventions. New models focus on value-based care, patient-centered decisions, and ethical care. These changes aim to improve care and reduce costs.
Value-Based Care as a Solution
Value-based care changes the game by focusing on patient results, not just services. It rewards providers for quality and efficiency. This means fewer unnecessary treatments.
Key Components of Value-Based Care:
- Pay-for-performance models
- Accountable care organizations (ACOs)
- Patient-centered medical homes
These models boost patient happiness and cut down on costs. They make healthcare more efficient and effective.
Patient-Centered Decision Making
Patient-centered care puts patients in charge of their health. It ensures treatments match their values and needs. This approach improves patient satisfaction and outcomes.
|
Benefits |
Challenges |
|---|---|
|
Improved patient satisfaction |
Increased patient responsibility |
|
Better health outcomes |
Potential for conflicting opinions |
|
Enhanced patient-provider communication |
Need for patient education |
Ethical and Innovative Care Delivery Systems
Ethical care systems focus on transparency and patient well-being. They use new tech like telemedicine and AI to improve care.
Telemedicine lets patients get care without hospital visits. AI-driven diagnostics spot conditions sooner and more accurately. This could mean fewer unnecessary treatments.
By adopting these new methods, healthcare can avoid the downsides of old models. It leads to better, more focused care for patients.
Conclusion
Interventions in healthcare have many downsides, like high costs and risks to patient safety. They can also affect a person’s mental health. It’s key to know when these treatments are really needed.
While some interventions help, others might not. Whether they work depends on many things. This includes the type of intervention and what the patient needs.
At , we focus on quality, ethics, and care that puts the patient first. We aim to give the best care, avoiding unnecessary risks. This way, we ensure our patients get the right treatment.
FAQ
What are the main disadvantages of medical interventions?
Medical interventions can cause physical harm and financial strain. They can also affect patients’ mental health. Issues like hospital infections, overdiagnosis, and antibiotic resistance are common problems.
Are interventions always effective in treating medical conditions?
Interventions can help with some medical conditions, but not all. Sometimes, they can even cause more harm. It’s important to think carefully before deciding on an intervention.
What are the financial implications of medical overuse?
Medical overuse can be very costly. It can strain healthcare systems and increase patient expenses. This can make healthcare less accessible and unfair for everyone.
How do interventions impact patient safety?
Interventions can harm patients in many ways. They can cause physical injuries, infections, and drug reactions. Ensuring patient safety is key, so we must evaluate interventions carefully.
What is the role of cultural competency in intervention approaches?
Cultural competency is very important in interventions. It affects how well interventions work. Without it, interventions might not be effective or could even harm patients.
Are professional interventions effective in treating addiction?
Professional interventions can help with addiction, but they’re not always successful. Sometimes, they can even make things worse. We need to think about other ways to help too.
What are the benefits of value-based care and patient-centered decision making?
Value-based care and patient-centered decision making are good. They focus on what patients need and want. This can lead to better care and happier patients.
How can healthcare systems balance the need for interventions with the risks associated with them?
Healthcare systems can manage intervention risks by using evidence-based criteria. They should also look at long-term outcomes and focus on preventing problems.
What is the prevention paradox, and how does it relate to interventions?
The prevention paradox is when focusing on interventions can hurt prevention efforts. This can increase risks and shows why prevention is key.
Are there alternative approaches to high-intervention healthcare models?
Yes, there are other ways to do healthcare, like value-based care and patient-centered care. These methods can reduce intervention risks and improve health outcomes.
How do interventions contribute to antibiotic resistance?
Interventions, like overusing antibiotics, can lead to antibiotic resistance. This is a big problem for global health. We need to use antibiotics wisely and find other ways to fight infections.
What are the psychological effects of medical interventions on patients?
Interventions can really affect patients’ mental health. They can cause anxiety, depression, and even PTSD. It’s important to consider these effects when deciding on interventions.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from



































