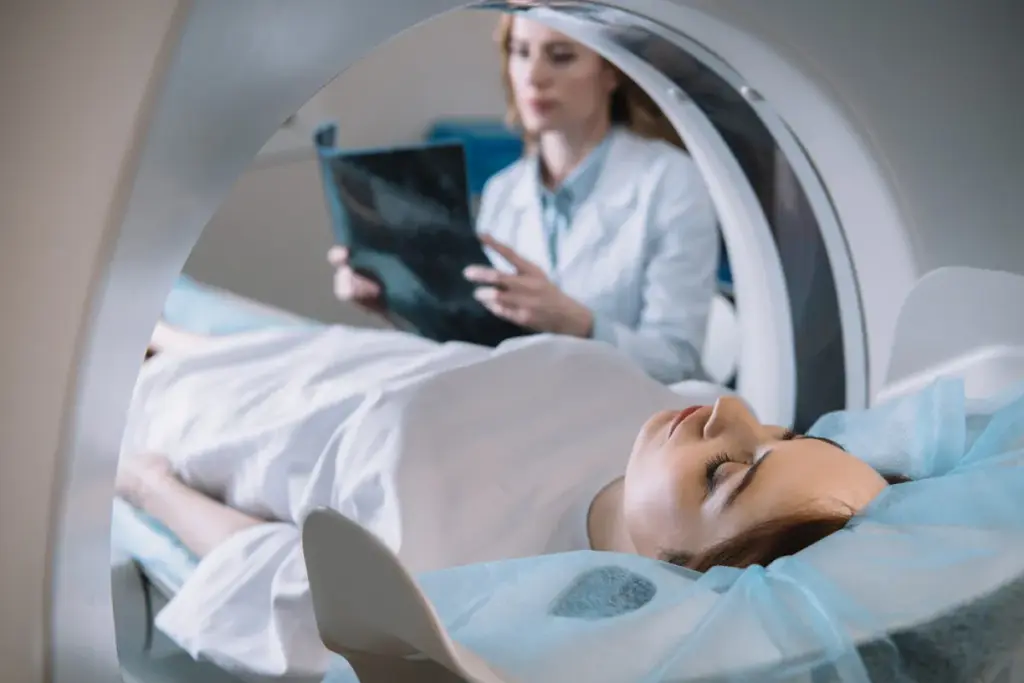
Interventional radiology (IR) has changed the medical world. It offers minimally invasive treatment options for many conditions. But, like any medical procedure, IR comes with risks that need to be understood and managed.
Recent data shows that major complications happen in 3-7% of IR procedures. These can include bleeding, infection, and vascular injury. We will explore these risks and how to reduce them. This ensures patient safety and quality care.
Key Takeaways
- Interventional radiology carries specific risks, including bleeding and infection.
- Major complications occur in 3-7% of IR procedures.
- Understanding these risks is key to ensuring patient safety.
- Minimizing complications requires careful management and planning.
- IR provides minimally invasive treatment options for various medical conditions.
Understanding Interventional Radiology
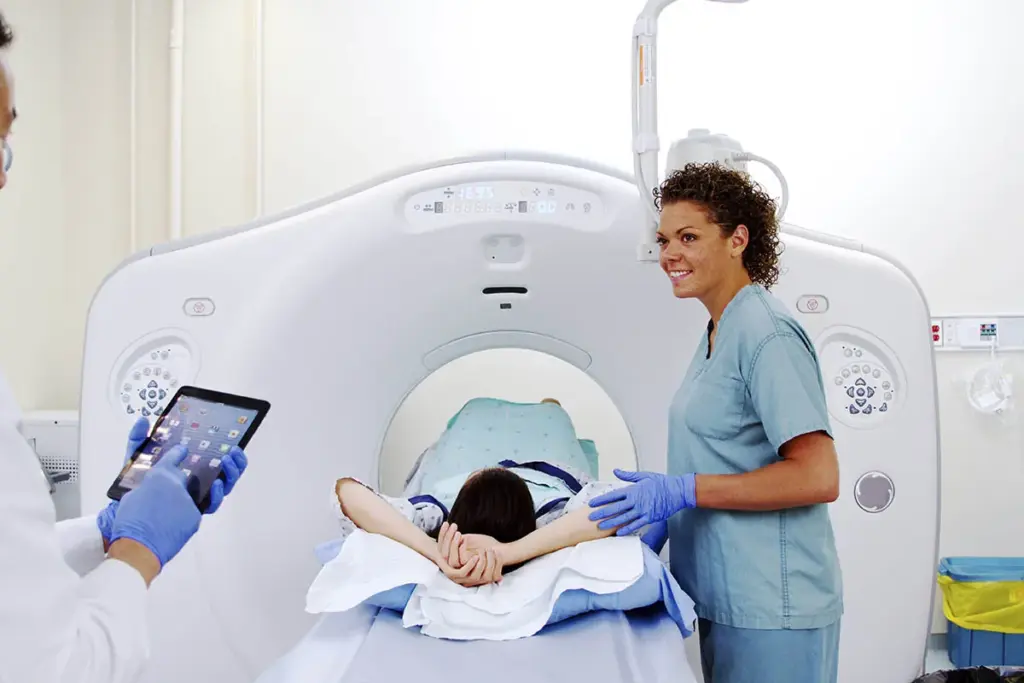
Interventional radiology is a key part of modern medicine. It uses imaging and small procedures to diagnose and treat many health issues. This field has changed patient care by giving new ways to treat diseases without big surgeries.
Definition and Scope of Interventional Radiology
Interventional radiology (IR) is a medical field that uses image-guided procedures to find and treat diseases. It covers many areas, from blood vessels to other parts of the body. IR is known for being less invasive, which means less pain and quicker recovery times compared to surgery.
The global market for interventional imaging is set to hit US$16.64 billion by 2033. It’s growing at a 6.8% CAGR. This shows more people are using IR and its importance in healthcare is growing.
Evolution of Minimally Invasive Techniques
The growth of minimally invasive procedures has boosted IR. Better imaging tech, like ultrasound and MRI, makes these procedures more precise. New devices, like stents, also help treat more conditions with IR.
Comparison to Traditional Surgical Approaches
IR and traditional surgery are different. IR is less invasive, causing less damage and quicker healing. It often uses local anesthesia, which is safer than general anesthesia. But, IR also has risks that need careful handling by experts.
Choosing between IR and surgery depends on the patient’s health and the disease. IR is often a good option or addition to surgery, giving patients more choices and possibly better results.
Common Radiology Interventional Procedures
Interventional radiology covers a wide range of procedures. These include vascular, non-vascular, and oncologic treatments. Each is designed to meet specific medical needs. They are key in modern medicine, providing less invasive options than traditional surgery.
Vascular Interventions
Vascular interventions deal with blood vessels, like arteries and veins. They are vital for diagnosing and treating vascular diseases. Some common procedures include:
- Angioplasty and stenting to open blocked or narrowed arteries
- Embolization to block blood flow to specific areas, such as tumors
- Thrombectomy to remove blood clots from vessels
Neurovascular devices, like stent retrievers and embolic coils, treat conditions like ischemic stroke and cerebral aneurysms. These devices have greatly improved treatment outcomes.
Non-vascular Interventions
Non-vascular interventions are not related to blood vessels. They include:
- Biopsies to diagnose various conditions, such as cancer
- Drainage procedures to remove fluid accumulations
- Ablation therapies to treat tumors
These procedures use imaging technologies like ultrasound, CT, or MRI. This ensures precision and safety.
Oncologic Interventions
Oncologic interventions are for cancer treatment. They include:
|
Procedure |
Description |
Benefits |
|---|---|---|
|
Chemoembolization |
Delivering chemotherapy directly to tumors and blocking their blood supply |
Reduces tumor size, minimizes systemic side effects |
|
Radioembolization |
Delivering radioactive particles directly to tumors |
Targets tumors with high doses of radiation while sparing healthy tissue |
|
Ablation Therapy |
Destroying tumors using heat, cold, or chemicals |
Minimally invasive, preserves organ function |
These oncologic interventions offer targeted treatments for cancer patients. They often improve outcomes and quality of life.
General Risk Profile of IR Procedures
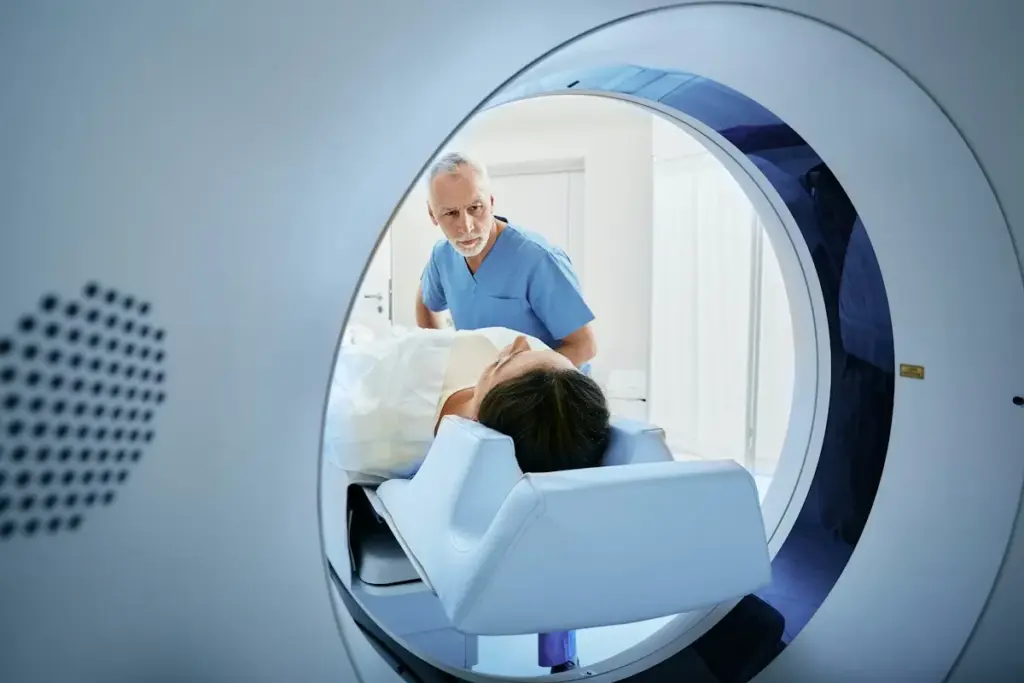
Interventional radiology (IR) offers many benefits, but it’s important to understand the risks. IR procedures are less invasive than traditional surgery. Yet, they come with risks that need to be managed.
Statistical Overview of Complication Rates
Major complications happen in 3-7% of IR procedures. This shows the need for careful risk management. The complication rates depend on the procedure type, patient factors, and the radiologist’s skill.
Risk-Benefit Analysis
Doing a thorough risk-benefit analysis is key for choosing IR procedures. This analysis weighs the procedure’s benefits against its risks. The patient’s medical history, current health, and condition severity are important in this analysis.
- IR procedures offer benefits like less recovery time, less pain, and lower complication risks compared to traditional surgery.
- Risks and complications can include bleeding, infection, vascular injury, and reaction to contrast media.
Factors Influencing Risk Assessment
Several factors affect the risk assessment of IR procedures. These include patient-related factors, procedural factors, and the operator’s expertise. Patient factors like age, comorbidities, and medication use are significant. The procedure type and equipment used also matter.
Key factors influencing risk assessment include:
- Patient comorbidities and overall health status
- Type and complexity of the IR procedure
- Expertise and experience of the interventional radiologist
- Quality of pre-procedural planning and post-procedural care
By evaluating these factors carefully, healthcare providers can reduce risks and improve outcomes for patients undergoing IR procedures.
Bleeding Complications
Bleeding is a common issue with interventional radiology procedures. It can be minor or serious and depends on the procedure, patient health, and how the procedure is done.
Mechanisms of Hemorrhage
Hemorrhage can happen during or after these procedures. It can be due to direct damage to blood vessels or because of medications that prevent blood clotting.
Risk Factors
Many things can increase the chance of bleeding. These include the patient’s age, health, and blood clotting status. The complexity of the procedure and how it’s done also play a role.
Management Strategies
To prevent bleeding, a few steps are important. First, choose the right patient and check their health before starting. Then, do the procedure carefully and watch the patient closely after it’s done. Using ultrasound for access and managing blood thinners are also key.
Knowing the risks and how to manage them is key to avoiding bleeding in interventional radiology.
|
Risk Factor |
Description |
Management Strategy |
|---|---|---|
|
Coagulopathy |
Pre-existing coagulation disorder |
Correct coagulopathy before procedure |
|
Vascular Calcification |
Hardening of arterial walls |
Use careful vascular access techniques |
|
Anticoagulation Therapy |
Use of blood-thinning medications |
Manage anticoagulation levels carefully |
In conclusion, bleeding is a big risk in interventional radiology. Knowing how it happens, the factors that increase it, and how to manage it is vital. This ensures patient safety.
Infection Risks in Interventional Radiology
Infections can complicate interventional radiology procedures, making infection control a top priority. As we explore minimally invasive procedures, it’s key to grasp the infection risks. We must also know how to lessen these risks.
Types of Infectious Complications
Infections in interventional radiology can vary. They can be localized, like abscesses or cellulitis, or systemic, like bacteremia or sepsis. The severity of these infections can vary, requiring quick recognition and treatment.
Some procedures carry a higher risk of infection. For example, biliary system interventions or drainage procedures are at higher risk. This is because of the chance of bacterial colonization.
Contributing Factors to Infection
Several factors increase the risk of infection in interventional radiology. Patient-related factors include health conditions like diabetes or immunosuppression. Procedure-related factors include the procedure’s complexity and duration, the use of sterile technique, and the equipment type.
The environment also plays a big role. Keeping the environment sterile and following strict infection control protocols are key to reducing infection risk.
Infection Control Protocols
To lower infection risk, we follow strict infection control protocols. These include proper hand hygiene, sterile gowns and gloves, and sterilized or disinfected equipment.
We also use antibiotic prophylaxis in high-risk cases. This is important for procedures involving foreign materials or potentially contaminated areas.
By understanding the types of infections, their causes, and implementing strong infection control, we can greatly reduce infection risks in interventional radiology.
Vascular Injuries and Complications
Vascular complications, like injuries and thrombotic events, are risks in IR procedures. These issues can happen during vascular interventions, key in interventional radiology. We’ll look at the types of vascular injuries, their effects, and how to manage and prevent them.
Vessel Perforation and Dissection
Vessel perforation and dissection are serious issues that can happen during vascular interventions. Vessel perforation means a hole forms in a blood vessel’s wall, leading to bleeding. Dissection is a tear in the vessel’s inner lining, causing it to narrow or block.
These problems can come from using the wrong catheter sizes, guidewire manipulation, or balloon angioplasty. They’re more likely in people with conditions like atherosclerosis or vasculitis.
Thrombotic Events
Thrombotic events, like thrombosis and embolism, are vascular complications of IR procedures. Thrombosis is a blood clot in a vessel, causing blockage. An embolism happens when a clot or material blocks a smaller vessel.
These events can be caused by catheter placement, contrast media, or procedural trauma. Managing them often involves anticoagulation or thrombolytic therapy.
Long-term Vascular Sequelae
The long-term effects of vascular injuries in IR procedures can be serious. Patients might face chronic conditions like stenosis or occlusion, leading to ischemia or organ dysfunction. Sometimes, these issues need more interventions or surgery.
We stress the need for careful patient selection, precise procedural technique, and thorough post-procedure care. This helps reduce the risk of vascular complications and their long-term effects.
Radiation Exposure Concerns
Interventional radiology uses ionizing radiation, which raises safety concerns. As we move forward, we must tackle the risks of radiation exposure.
Patient Radiation Dose in Common Procedures
Patients in interventional radiology face different radiation levels. The dose varies based on the procedure, its complexity, and the patient’s BMI.
|
Procedure |
Typical Radiation Dose (mSv) |
Equivalent Background Radiation |
|---|---|---|
|
Angiography |
5-10 |
2-4 years |
|
Embolization |
10-20 |
4-8 years |
|
Biopsy |
1-5 |
0.5-2 years |
Acute and Long-term Effects of Radiation
Radiation can cause immediate and long-term effects. Immediate effects like skin injuries are rare but can happen at high doses. Long-term effects, like cancer risk, are a major concern because they add up over time.
Acute Effects: High doses can lead to skin injuries like erythema and ulcers.
Long-term Effects: Cancer risk is a concern due to radiation. The risk is low but depends on the dose.
Dose Reduction Techniques
To lower radiation risks, several techniques are used. These include low-dose protocols, optimizing fluoroscopy settings, and monitoring doses in real-time.
- Low-dose protocols
- Fluoroscopy pulse rate reduction
- Collimation and filtration
- Real-time dose monitoring
By using these methods, we can reduce radiation exposure. This helps keep interventional radiology safe and effective.
Occupational Hazards for IR Professionals
IR professionals face many health risks at work. Their job involves complex procedures and equipment. We will look at these hazards and how to reduce them.
Radiation Exposure Among Staff
Radiation is a big worry for IR workers. Long-term exposure can harm their health. Radiation safety protocols are key to lower risks. They include wearing protective gear and tracking radiation doses.
A study in the shows the dangers of their job. It gives insights into the risks IR professionals face.
|
Radiation Safety Measure |
Description |
Benefits |
|---|---|---|
|
Lead Aprons |
Protective garment worn to shield against radiation |
Reduces radiation exposure to vital organs |
|
Thyroid Shields |
Protective shield worn around the neck |
Protects the thyroid gland from radiation |
|
Dose Monitoring Systems |
Systems used to track radiation exposure |
Helps in maintaining safe radiation levels |
Orthopedic Injuries from Protective Equipment
Protective gear is vital but can cause injuries. Lead aprons, for example, can strain muscles. Ergonomic practices and breaks can help prevent these injuries.
Cancer Risk Among Interventional Radiologists
There’s a worry about cancer risk for IR workers due to radiation. Ongoing studies aim to understand this better. For now, strict safety rules are essential.
By knowing these risks and taking safety steps, we can make IR work safer.
Contrast Media-Related Complications
Contrast media are important for making radiology images clearer. But, they can cause problems. We’ll look at issues like kidney damage and allergic reactions. We’ll also talk about how to reduce these risks.
Contrast-Induced Nephropathy
Contrast-induced nephropathy (CIN) is a big worry for those getting radiology tests with contrast. CIN is when kidney function suddenly gets worse after contrast media use. It’s important to spot who’s at risk, like those with kidney problems or diabetes.
“The risk of CIN can be lowered with the right steps,” say experts. We should check how well the kidneys work before the test. And we should think about other imaging options when we can.
Allergic Reactions to Contrast Agents
Allergic reactions to contrast media can be mild or serious. Anaphylaxis is a rare but deadly reaction that needs quick action. We must be ready to handle such reactions fast.
- Symptoms of allergic reactions include hives, itching, and trouble breathing.
- For those who’ve had allergic reactions before, we might give them corticosteroids and antihistamines.
Prevention and Management Approaches
Stopping contrast media problems means picking the right patients, checking them before the test, and using the right prevention steps. Drinking lots of water helps prevent CIN. The type of contrast agent used also affects the risk of problems.
“Low-osmolar contrast media are safer for the kidneys than high-osmolar ones.”
— Expert Opinion
Knowing the risks of contrast media and using the right prevention steps helps keep radiology tests safe. This way, we can lower the chance of bad outcomes.
Procedure-Specific Risks
Interventional radiology procedures come with unique risks. Each procedure has its own set of dangers. Knowing these risks is key to better patient care.
Risks in Arterial Interventions
Arterial interventions, like angioplasty and stenting, have their own set of risks. These include bleeding, vascular injury, and thrombotic events. Experts say careful patient selection is vital.
We use advanced imaging and special devices to reduce these risks. But, we must be ready for complications.
Complications in Biliary Procedures
Biliary interventions, like drainage and stenting, come with risks like infection and bleeding. Knowing the biliary anatomy well is important.
We follow strict sterile techniques and use antibiotics when needed. Careful planning and execution help avoid problems.
“The use of advanced imaging and navigation tools has significantly improved the safety and efficacy of biliary interventions,” according to a leading interventional radiologist.
Adverse Events in Neurointervention
Neurointerventions, such as aneurysm coiling and stroke thrombectomy, are complex and risky. Risks include stroke and vascular injury. These procedures need a lot of skill and precision.
We use advanced imaging and neuromonitoring to manage risks. A team approach is critical for these delicate procedures.
Understanding the risks of interventional radiology helps us prepare for complications. This knowledge lets us give better care and improve outcomes.
Patient-Related Risk Factors
It’s key to know about patient-related risk factors for better results in interventional radiology. These factors can greatly affect how safe and effective procedures are.
Comorbidities Increasing Procedural Risk
Comorbid conditions can make interventional radiology procedures more complicated. For example, diabetes can increase the risk of complications because of vascular changes and poor wound healing.
|
Comorbidity |
Potential Impact |
|---|---|
|
Diabetes |
Increased risk of vascular complications and impaired healing |
|
Hypertension |
Higher risk of bleeding complications |
|
Kidney Disease |
Risk of contrast-induced nephropathy |
The table shows how different comorbidities can affect procedural risks in various ways. This highlights the importance of thorough patient assessment.
Age-Related Considerations
Age is a big factor in the outcome of interventional radiology procedures. Older patients often have more health issues and less physical strength. This makes them more likely to face complications.
“The aging population presents unique challenges in interventional radiology, necessitating a tailored approach to risk assessment and management.”
Expert Opinion
For older patients, a detailed geriatric assessment can help spot risks. It guides how to prepare for the procedure better.
Medication Interactions and Concerns
Managing medications is vital in interventional radiology. Some drugs can raise the risk of bleeding or react with contrast agents. This can make procedures more complicated.
It’s important to carefully review a patient’s medications to lower these risks. Changes might be needed to ensure the procedure is safe.
Preventable Adverse Events in IR
Preventable adverse events in IR come from many sources. These include device misuse and communication problems. These issues can harm patients and make the IR suite less safe and efficient.
Device Misuse and Technical Errors
Device misuse is a big problem in IR. Technical mistakes can happen due to bad training, faulty equipment, or user mistakes. A study in showed that device misuse often causes problems in IR procedures.
To reduce these risks, it’s key to have strong training for IR staff. They need to learn how to use devices correctly. Also, keeping equipment in good shape and doing quality checks can prevent technical issues.
Positioning and Navigation Errors
Errors in positioning and navigation during IR procedures can cause serious issues. These include vascular injuries and bleeding. These mistakes often happen because of bad imaging or wrong understanding of body parts.
To lower these risks, using advanced imaging and real-time monitoring is important. IR teams should also get regular training on navigation systems and how to read images better.
|
Error Type |
Consequence |
Prevention Strategy |
|---|---|---|
|
Device Misuse |
Technical Errors, Adverse Events |
Robust Training, Equipment Maintenance |
|
Positioning and Navigation Errors |
Vascular Injuries, Bleeding |
Advanced Imaging, Real-time Monitoring |
|
Communication Failures |
Misunderstandings, Adverse Events |
Standardized Communication Protocols, Team Training |
Communication Failures in the IR Suite
Good communication is vital in the IR suite. It helps ensure procedures are done safely and well. Without clear communication, there can be misunderstandings, mistakes, and bad outcomes.
“Clear and consistent communication among the IR team is essential for preventing errors and ensuring patient safety.”
To fix this, IR teams should use standard communication methods and get training on how to communicate well. Holding regular team meetings can also help spot and solve problems, improving team performance.
Risk Mitigation Strategies
Risk mitigation in interventional radiology is about using many approaches to lower the chance of bad outcomes. It’s key to keep patients safe during IR procedures. This means we work hard to prevent problems and make sure patients do well.
Pre-procedural Planning and Assessment
Planning before a procedure is very important. We look at the patient’s health history, current state, and what the procedure needs. We check patient data, like lab results and images, to spot risks and plan how to avoid them.
Key elements of pre-procedural planning include:
- Review of patient medical history and current medications
- Assessment of renal function to determine the appropriate use of contrast media
- Evaluation of vascular access options
- Planning for possible complications and having the right tools and team ready
Intra-procedural Monitoring Techniques
Monitoring during the procedure is key to catching and handling problems right away. We use advanced methods, like live imaging and watching vital signs, to keep patients safe.
Effective intra-procedural monitoring involves:
- Keeping an eye on vital signs, like blood pressure and heart rate
- Using live imaging to guide the procedure and spot issues
- Applying sedation and anesthesia as needed, watching the patient’s awareness closely
Post-procedural Care Protocols
Aftercare is critical to avoid complications after the procedure. We have set protocols for aftercare. These include watching the patient closely, handling any issues that come up, and giving clear instructions for home care.
Post-procedural care protocols include:
- Watching for signs of bleeding or other problems
- Managing pain and discomfort
- Providing clear instructions for follow-up care and emergency contact info
By using these strategies, we greatly improve patient safety and results in interventional radiology.
Quality Improvement in Interventional Radiology
To keep patients safe and improve care, quality improvement is key in interventional radiology. As we grow in this field, we must focus on making care better and safer.
Improving quality in interventional radiology involves many steps. We’ll look at error reporting, ongoing learning, and using safety checklists.
Error Reporting Systems
Error reporting systems are vital for quality improvement. They help us find and learn from mistakes, making care safer for everyone.
With a strong error reporting system, we create a culture of openness and learning. This makes care better and safer for patients.
Continuous Education and Training
Keeping skills sharp is essential for interventional radiology professionals. As new tech and methods come along, training keeps us current.
Staying up-to-date with education boosts patient care and excellence in our field. It shows our commitment to top-notch care.
Implementation of Safety Checklists
Safety checklists are a big part of improving quality in interventional radiology. They make sure we follow important steps, reducing risks.
Checklists help standardize care, making it safer for patients. This careful approach is critical in the complex world of interventional radiology.
In summary, improving quality in interventional radiology is a big job that needs a wide range of efforts. By using error reports, training, and checklists, we can make care safer and better for everyone.
Conclusion: Balancing Risks and Benefits in Interventional Radiology
Interventional radiology has changed medicine a lot. It offers new ways to treat patients without big surgeries. But, like any treatment, it has risks that need to be watched closely.
Managing these risks is key. Doctors need to know the good and bad sides of IR treatments. This helps them choose the best options for patients and keep them safe.
By focusing on quality and learning more, we can make IR treatments better. This way, patients get the best care and have good results from these new treatments.
FAQ
What is interventional radiology and how does it differ from traditional surgery?
Interventional radiology (IR) is a medical field that uses small incisions for treatments. It’s different from traditional surgery because it’s less invasive. This means less recovery time and less scarring.
What are the benefits of vascular interventional radiology procedures?
Vascular IR procedures are safer and faster than traditional surgery. They can treat blocked arteries and varicose veins. Patients often have shorter hospital stays and quicker recovery times.
What are the risks associated with interventional radiology procedures?
IR procedures are generally safe but carry some risks. These include bleeding, infection, and radiation exposure. The risks depend on the procedure, the patient’s health, and the doctor’s skill.
How can bleeding complications be managed and prevented during IR procedures?
To prevent bleeding, doctors carefully choose patients and use special agents. They also plan the procedure well and monitor it closely. Good care after the procedure helps too.
What is contrast-induced nephropathy, and how can it be prevented?
Contrast-induced nephropathy is a risk for patients with kidney problems. It’s caused by contrast media used in IR. To prevent it, doctors use safer contrast agents and ensure patients are well-hydrated.
How can radiation exposure be minimized during IR procedures?
To reduce radiation, doctors use low-dose protocols and special techniques. They also follow safety rules to protect themselves and patients from radiation.
What are the occupational hazards faced by interventional radiologists and IR staff?
IR professionals face risks like radiation and injuries from protective gear. Safety protocols and regular breaks help reduce these risks.
How can patient outcomes be improved in interventional radiology?
Better patient outcomes come from managing risks and improving quality. Continuous education and careful planning are key. Good care before, during, and after the procedure also helps.
What role does quality improvement play in interventional radiology?
Quality improvement is vital in IR. It helps identify and reduce risks, leading to better patient care. Programs like error reporting and safety checklists are important.
How can patients prepare for an interventional radiology procedure?
Patients should follow instructions and disclose any health issues before the procedure. Asking questions about the procedure and risks ensures a safe experience.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK13463


































