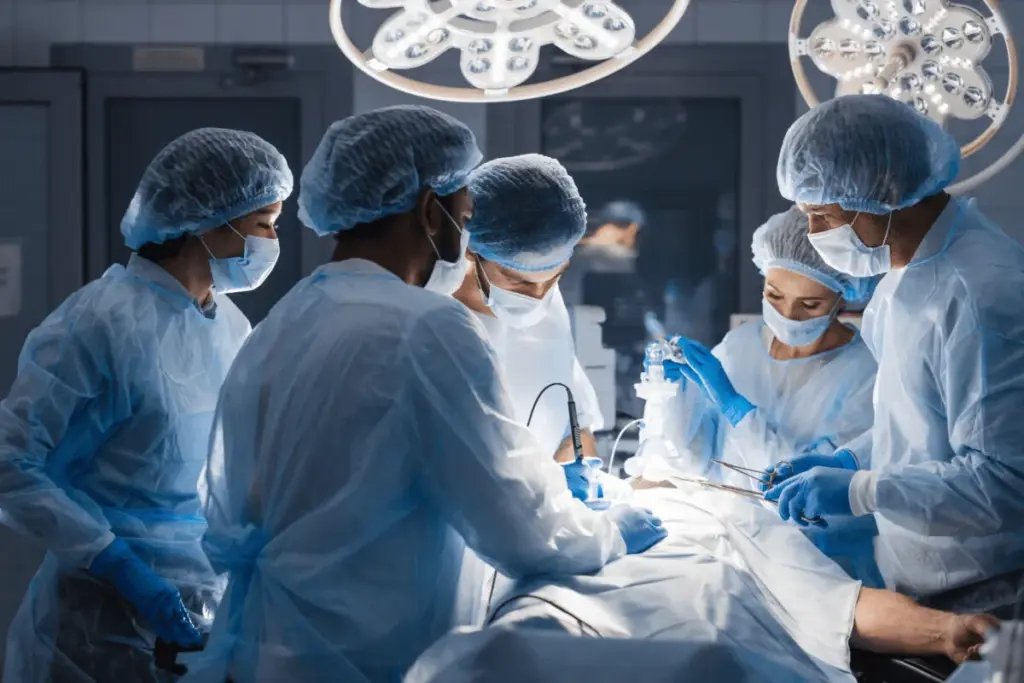
ENT surgery, while generally safe, carries certain risks that patients should be aware of. Advances in medical techniques and comprehensive care protocols have significantly improved the safety of these procedures. However, like all surgeries, ENT operations are not without risks. Understanding these risks and how they are assessed is crucial for patients considering surgery.
The RCRI score is a critical tool used in evaluating the risk associated with surgeries, including ENT procedures. It helps in assessing the patient’s risk of experiencing cardiac complications during surgery.
Key Takeaways
- ENT surgery carries certain risks despite being generally safe.
- The RCRI score is crucial for assessing surgical risk.
- Understanding the risks and benefits is vital for patients.
- ENT surgeries include procedures like ear tube placement and sinus surgery.
- Comprehensive care protocols have improved ENT surgery safety.
The Landscape of ENT Surgical Procedures
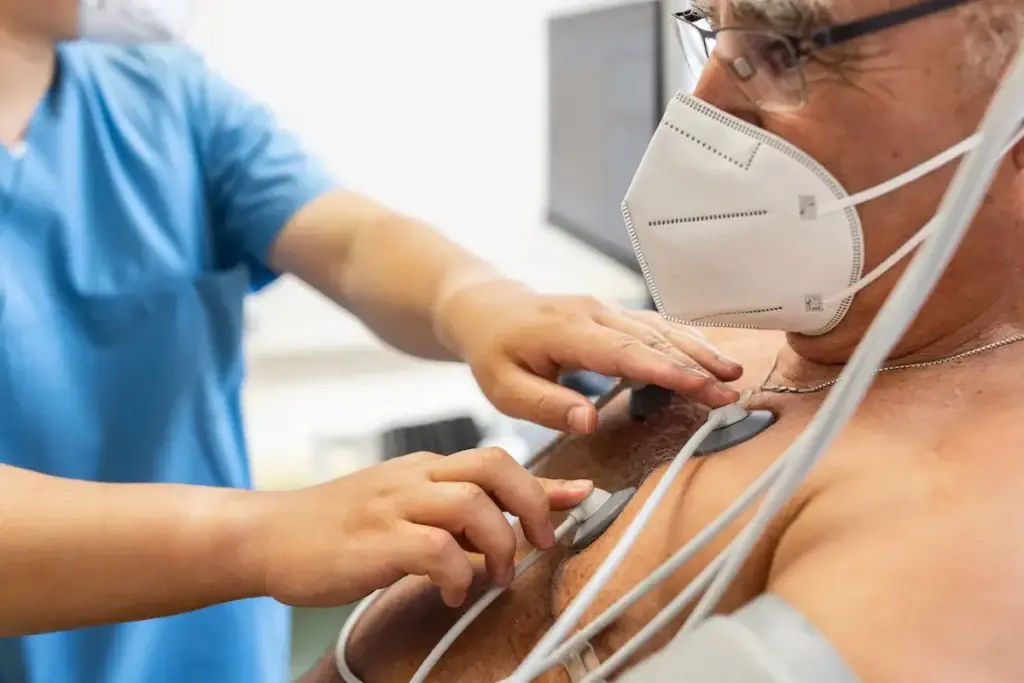
The landscape of ENT surgical procedures is broad, covering a multitude of operations that are critical for patient care. Ear, nose, and throat surgeries are performed to diagnose and treat a wide range of conditions, from hearing loss and sinus infections to tonsillitis and thyroid disorders.
ENT surgical procedures are diverse and include operations such as ear tube placement, nasal fracture repair, and endoscopic sinus surgery. These procedures are often performed to alleviate symptoms, improve quality of life, and in some cases, save lives.
Common Ear, Nose, and Throat Operations
Some of the most common ENT operations include:
- Tonsillectomy and adenoidectomy
- Myringotomy with tube insertion
- Septoplasty and turbinoplasty
- Endoscopic sinus surgery
- Thyroidectomy
These procedures are typically performed in a hospital or outpatient surgical center, depending on the complexity of the operation and the patient’s overall health.
General Safety Profile Compared to Other Surgeries
ENT surgeries are generally considered to have a good safety profile compared to other surgical specialties. According to various studies, the complication rates for ENT procedures are relatively low.
|
Procedure |
Complication Rate |
|---|---|
|
Tonsillectomy |
2-5% |
|
Endoscopic Sinus Surgery |
1-3% |
|
Thyroidectomy |
1-2% |
As shown in the table, the complication rates for common ENT procedures are relatively low, indicating a good safety profile. However, as with any surgery, there are risks involved, and patients should be thoroughly informed about the potential complications.
“The safety profile of ENT surgery is generally good, but it’s crucial to carefully evaluate each patient’s risk factors to minimize complications.” -ENT Specialist
To further enhance surgical safety, tools like the RCRI calculator are used to assess cardiac risk in patients undergoing surgery. This is particularly important for patients with pre-existing heart conditions.
Evaluating Surgical Risk: The Importance of Preoperative Assessment

ENT surgery requires a thorough preoperative assessment to identify potential risks. This critical step ensures that patients are adequately prepared for surgery, and it allows healthcare providers to mitigate risks whenever possible.
The preoperative assessment is multifaceted, involving a comprehensive review of the patient’s medical history, current health status, and the specific requirements of the surgical procedure. By evaluating these factors, surgeons can better understand the risks associated with the surgery and develop strategies to minimize them.
Key Risk Factors in ENT Surgery
Several key risk factors are commonly associated with ENT surgery. These include:
- Patient Age: Both pediatric and geriatric patients may have unique risks due to their age.
- Comorbid Conditions: Presence of other health conditions, such as heart disease or diabetes, can complicate surgery.
- Surgical Complexity: The nature and complexity of the ENT procedure can influence risk.
|
Risk Factor |
Description |
Mitigation Strategy |
|---|---|---|
|
Patient Age |
Age-related risks, such as reduced physiological reserve. |
Adjust anesthesia and surgical plans according to age. |
|
Comorbid Conditions |
Presence of other health issues that can complicate surgery. |
Optimize management of comorbid conditions before surgery. |
|
Surgical Complexity |
Complex procedures may have higher risks of complications. |
Use advanced surgical techniques and intraoperative monitoring. |
The Evolution of Risk Assessment Tools
Risk assessment tools have evolved significantly over time. The Revised Cardiac Risk Index (RCRI) is one such tool that has gained prominence in evaluating cardiac risk for non-cardiac surgeries, including ENT procedures.
Other risk assessment tools and indices have also been developed to address specific aspects of surgical risk. These tools help in stratifying patients according to their risk profile, thereby guiding preoperative preparation and intraoperative management.
<SEP-12025_image_4>
By understanding and applying these risk assessment tools, healthcare providers can enhance patient safety and improve outcomes in ENT surgery.
The RCRI Score: Essential Tool for Cardiac Risk Evaluation
The Revised Cardiac Risk Index (RCRI) score is a crucial tool for evaluating cardiac risk in patients undergoing surgery. This scoring system has gained widespread acceptance for its ability to predict major cardiac complications in non-cardiac surgeries, including ENT procedures.
Six Components of the Revised Cardiac Risk Index
The RCRI score is calculated based on six independent risk factors:
- High-risk surgery
- History of ischemic heart disease
- History of congestive heart failure
- History of cerebrovascular disease
- Preoperative treatment with insulin
- Preoperative serum creatinine > 2 mg/dL
Each of these factors contributes to the overall risk assessment, providing a comprehensive view of the patient’s cardiac risk profile.
How to Use the RCRI Calculator Effectively
To use the RCRI calculator effectively, healthcare providers must accurately identify and document the presence of the six risk factors. The total score is then calculated by summing the number of risk factors present. This score is used to stratify patients into different risk categories, ranging from low to high risk.
Effective use of the RCRI calculator involves:
- Accurate preoperative assessment
- Thorough patient history
- Appropriate laboratory testing
Clinical Significance of RCRI Risk Stratification
The RCRI risk stratification has significant clinical implications for managing patients undergoing surgery. It helps in:
- Identifying high-risk patients who may benefit from further cardiac evaluation or optimization
- Guiding perioperative management strategies
- Informing patient and family discussions about surgical risks
By understanding a patient’s RCRI score, healthcare providers can develop a more tailored approach to their care, potentially reducing the risk of cardiac complications during and after surgery.
Beyond RCRI: Additional Risk Assessment Methods
ENT surgery risk assessment isn’t limited to RCRI; other tools offer valuable information. While the Revised Cardiac Risk Index provides crucial insights into cardiac risks associated with surgery, other assessment methods can offer a more comprehensive view of surgical risks.
Goldman Risk Index Calculator for Surgical Patients
The Goldman Risk Index Calculator is another significant tool used to evaluate the risk of cardiac complications in surgical patients. Developed by Lee Goldman in 1977, this calculator considers various factors to predict cardiac risk.
Key components of the Goldman Risk Index include:
- History of heart disease
- Presence of jugular venous distension
- Type of surgery
- Age of the patient
- Other medical conditions
ASA Score in Anesthetics Planning
The American Society of Anesthesiologists (ASA) Physical Status classification system is widely used to assess a patient’s physical status before surgery. This scoring system helps anesthesiologists plan appropriate anesthesia care.
|
ASA Score |
Description |
|---|---|
|
ASA I |
Normal healthy patient |
|
ASA II |
Patients with mild systemic disease |
|
ASA III |
Patients with severe systemic disease |
|
ASA IV |
Patients with severe systemic disease that is a constant threat to life |
Specialty-Specific ENT Risk Tools
Specialty-specific risk tools are also available for ENT surgeries, providing surgeons with detailed insights into potential complications and risks associated with specific procedures.
Examples include:
- Risk calculators for tonsillectomy and adenoidectomy
- Thyroid surgery risk assessment tools
- Endoscopic sinus surgery risk evaluation guidelines
These tools help in making informed decisions and improving patient outcomes by identifying potential risks early.
Anesthesiology Risks in ENT Procedures
Understanding anesthesiology risks is essential for the success of ENT surgical interventions. Anesthesiology plays a critical role in managing patient care during these delicate procedures.
Airway Management Challenges
Airway management is a significant challenge in ENT surgery due to the proximity of the surgical site to the airway. Effective airway management is crucial to prevent complications such as respiratory distress or aspiration.
The complexity of airway management in ENT procedures often requires a multidisciplinary approach, involving both the surgeon and the anesthesiologist. Preoperative planning is vital to anticipate potential airway challenges.
Monitored Anesthesia Care vs. General Anesthesia
The choice between monitored anesthesia care (MAC) and general anesthesia (GA) in ENT procedures depends on several factors, including the type of surgery, patient health, and the anesthesiologist’s preference.
- MAC is often preferred for less invasive procedures, offering the benefit of reduced recovery time.
- GA is typically used for more complex surgeries or when patient cooperation is not expected.
Recovery Considerations Unique to ENT
Recovery from ENT surgery involves unique considerations, particularly regarding airway management and pain control. Postoperative care must be tailored to the specific needs of ENT patients to minimize complications.
Effective pain management strategies are crucial in the postoperative period to enhance patient comfort and reduce the risk of complications.
Specific Risks in Common ENT Surgeries
Understanding the risks associated with ENT surgeries is crucial for patient safety. While ENT procedures are generally safe, they carry specific risks that need to be understood for informed consent.
Tonsillectomy and Adenoidectomy Complications
Tonsillectomy and adenoidectomy are common ENT procedures, especially in children. Complications can include:
- Bleeding: Primary or secondary hemorrhage can occur.
- Respiratory complications: Airway obstruction or aspiration.
- Pain: Postoperative pain management is crucial.
Thyroidectomy and Nerve Injury Prevention
Thyroidectomy carries risks such as nerve injury. Measures to prevent nerve damage include:
- Intraoperative nerve monitoring.
- Careful surgical technique.
- Preoperative assessment of nerve function.
Endoscopic Sinus Surgery Risks
Endoscopic sinus surgery is used to treat sinusitis. Risks include:
- Ocular complications: Injury to the orbit or optic nerve.
- CSF leak: Potential for cerebrospinal fluid leakage.
- Infection: Postoperative infection.
Ear Surgery Complications
Ear surgery, such as tympanoplasty or mastoidectomy, carries risks including:
- Hearing loss: Temporary or permanent.
- Facial nerve injury: Rare but possible.
- Infection: Postoperative infection.
Understanding these risks is essential for managing patient expectations and improving outcomes in ENT surgery.
Pediatric ENT Surgery: Special Risk Considerations
When it comes to ENT surgery in children, understanding the special risk considerations is crucial for optimal outcomes. Pediatric ENT surgery presents unique challenges due to the anatomical and physiological differences between children and adults.
Age-Related Anatomical Challenges
Children’s smaller airways and developing structures pose significant challenges in ENT surgery. The anatomy of a child’s ear, nose, and throat is not a miniature version of an adult’s; it has distinct features that require specialized knowledge and techniques.
The size and delicacy of pediatric structures demand precision and gentleness during surgical procedures. Surgeons must be adept at handling these challenges to minimize risks.
Reported Complication Rates in Children
Complication rates in pediatric ENT surgery vary based on the procedure and the child’s overall health. Studies have shown that certain procedures have higher complication rates in children compared to adults.
|
Procedure |
Complication Rate in Children |
|---|---|
|
Tonsillectomy |
2-5% |
|
Adenoidectomy |
1-3% |
|
Myringotomy |
Less than 1% |
Parental Education and Preparation
Educating parents about the risks and benefits of pediatric ENT surgery is crucial. Parents should be informed about what to expect before, during, and after the surgery to reduce anxiety and ensure compliance with postoperative care instructions.
Clear communication between healthcare providers and parents is key to a successful surgical outcome. Parents should be encouraged to ask questions and express their concerns.
Surgical Clearance Protocols for ENT Procedures
Surgical clearance protocols play a crucial role in ensuring patient safety during ENT procedures. These protocols are designed to assess the patient’s overall health and identify potential risks that could complicate surgery or recovery.
Cardiac Clearance Requirements
Cardiac clearance is a critical component of surgical clearance, particularly for patients with a history of heart disease or those undergoing major ENT surgeries. The Revised Cardiac Risk Index (RCRI) is commonly used to stratify cardiac risk. Patients with a high RCRI score may require additional cardiac evaluation before surgery.
The process involves assessing the patient’s cardiac function through tests such as echocardiography or stress tests. Effective cardiac clearance requires collaboration between the otolaryngologist, anesthesiologist, and cardiologist to ensure that the patient is optimized for surgery.
Multidisciplinary Preoperative Assessment
A multidisciplinary preoperative assessment is essential for comprehensive risk evaluation. This involves a team of healthcare professionals, including surgeons, anesthesiologists, and other specialists as needed, who review the patient’s medical history, current health status, and surgical plans.
- Review of medical history and current medications
- Physical examination and assessment of overall health
- Discussion of surgical risks and benefits
- Development of a perioperative care plan
When to Delay or Cancel Surgery
Deciding when to delay or cancel surgery is a critical aspect of surgical clearance protocols. Uncontrolled hypertension, acute cardiac conditions, or severe respiratory infections are common reasons to postpone surgery.
The decision to delay or cancel surgery should be based on a thorough assessment of the patient’s condition and the potential risks associated with proceeding with surgery. Clear communication with the patient and their family is essential in these situations.
Procedure vs. Surgery: Risk Differences in ENT Practice
ENT procedures and surgeries have different risk profiles, influenced by factors like setting and invasiveness. Understanding these differences is crucial for optimizing patient outcomes and minimizing complications.
Office-Based vs. Operating Room Procedures
Office-based procedures in ENT practice are becoming increasingly common due to advancements in technology and the desire to reduce healthcare costs. These procedures are often less invasive and can be performed under local anesthesia, reducing the risks associated with general anesthesia and operating room complexities.
“The shift towards office-based procedures represents a significant change in how ENT care is delivered,” notes an ENT specialist. “It’s essential to carefully select patients and procedures suitable for an office setting.”
Minimally Invasive Approaches and Risk Reduction
Minimally invasive approaches in ENT surgery have revolutionized the field by reducing recovery times and minimizing scarring. Techniques such as endoscopic sinus surgery and transoral robotic surgery (TORS) have become staples in many ENT practices.
These approaches not only reduce the risk of complications but also improve patient outcomes by allowing for more precise surgery. As a doctor explains, “Minimally invasive techniques have significantly lowered the risk profile for many ENT procedures, making them safer for a wider range of patients.”
Patient Selection Criteria
Patient selection is critical when determining whether a procedure should be performed in an office setting or an operating room. Factors such as the patient’s overall health, the complexity of the procedure, and the patient’s preference play a significant role in this decision.
- Assessing the patient’s medical history and current health status.
- Evaluating the complexity and risks associated with the procedure.
- Considering patient preferences and anxiety levels.
By carefully considering these factors, ENT specialists can minimize risks and ensure the best possible outcomes for their patients.
Complication Rates: National Benchmarks vs. High-Volume Centers
The comparison between national benchmarks and high-volume centers reveals significant differences in ENT surgery complication rates. High-volume centers, which perform a large number of ENT surgeries, often report lower complication rates compared to national averages. This disparity highlights the importance of experience and specialized care in reducing surgical risks.
Tonsillectomy Reoperation Rates
Tonsillectomy is one of the most common ENT surgeries, and reoperation rates can serve as an indicator of initial surgery success. Studies have shown that high-volume centers tend to have lower tonsillectomy reoperation rates compared to national benchmarks. For instance, a study found that reoperation rates for tonsillectomy were significantly lower in hospitals performing more than 100 such surgeries annually.
- High-volume centers: 2.1% reoperation rate
- National benchmarks: 3.5% reoperation rate
This difference underscores the impact of surgical volume on outcomes.
Thyroidectomy Nerve Injury Statistics
Thyroidectomy, another common ENT surgery, carries the risk of nerve injury. High-volume centers have been shown to have lower rates of nerve injury during thyroidectomy compared to national benchmarks. A comparative study highlighted that the incidence of nerve injury in high-volume centers was 2.4%, significantly lower than the 4.2% reported in national benchmarks.
“The expertise and specialized care available at high-volume centers contribute to better outcomes in thyroidectomy surgeries.” ENT Specialist
Surgical Site Infection Monitoring
Surgical site infections (SSIs) are a significant concern in ENT surgeries. High-volume centers often implement rigorous SSI monitoring protocols, leading to lower infection rates. Data shows that SSIs occurred in 1.8% of ENT surgeries at high-volume centers, compared to 3.1% nationally.
|
Type of Surgery |
High-Volume Centers |
National Benchmarks |
|---|---|---|
|
Tonsillectomy |
2.1% |
3.5% |
|
Thyroidectomy |
2.4% |
4.2% |
|
ENT Surgeries (SSI) |
1.8% |
3.1% |
In conclusion, the data indicates that high-volume centers achieve better outcomes in terms of complication rates for ENT surgeries compared to national benchmarks. This information is crucial for patients and healthcare providers when making informed decisions about surgical care.
Socioeconomic Disparities in ENT Surgical Outcomes
The impact of socioeconomic disparities on ENT surgical outcomes is a critical area of concern. Socioeconomic factors, including access to care and income levels, significantly influence the outcomes of ENT surgical procedures.
Rural vs. Urban Access to Specialized Care
One of the primary socioeconomic disparities affecting ENT surgical outcomes is the difference in access to specialized care between rural and urban areas. Rural areas often face challenges such as limited access to ENT specialists, longer travel distances to reach healthcare facilities, and lower socioeconomic status, all of which can impact surgical outcomes.
A study published on the National Institutes of Health website highlights the disparities in access to ENT care, emphasizing the need for improved healthcare infrastructure in rural areas.
- Limited availability of ENT specialists in rural areas
- Longer travel times to access ENT care
- Lower socioeconomic status in rural populations
Income-Related Differences in Complication Rates
Income levels also play a significant role in determining ENT surgical outcomes. Patients from lower-income backgrounds may experience higher complication rates due to various factors, including delayed access to care, poorer overall health, and limited postoperative support.
Addressing these income-related differences requires a multifaceted approach, including improving access to healthcare, enhancing patient education, and providing adequate postoperative care.
- Improving access to healthcare for low-income populations
- Enhancing patient education on ENT conditions and postoperative care
- Providing adequate postoperative support
Addressing Healthcare Inequities
To address the socioeconomic disparities in ENT surgical outcomes, healthcare systems must adopt a comprehensive approach. This includes improving access to ENT care in rural and low-income areas, enhancing patient education, and implementing policies to reduce healthcare inequities.
By understanding and addressing these disparities, healthcare providers can work towards improving ENT surgical outcomes for all patients, regardless of their socioeconomic background.
Quality Measures and Safety Protocols in ENT Surgery
Quality measures and safety protocols are the backbone of ENT surgical practices, ensuring optimal patient outcomes. The implementation of these measures is crucial in minimizing risks and complications associated with ENT surgical procedures.
Tracking 30-Day Readmissions is a critical quality measure that helps in assessing the effectiveness of ENT surgical care. It involves monitoring patients’ progress after discharge to identify any potential complications or issues that may necessitate readmission. By analyzing 30-day readmission rates, healthcare providers can refine their care pathways and improve patient outcomes.
Tracking 30-Day Readmissions
Effective tracking of 30-day readmissions requires a systematic approach, involving both inpatient and outpatient care teams. This includes thorough patient education on post-operative care, follow-up appointments, and clear guidelines on when to seek immediate medical attention.
Unplanned Reoperation Prevention
Preventing unplanned reoperations is another vital aspect of ENT surgical quality. This involves meticulous pre-operative planning, precise surgical techniques, and comprehensive post-operative care. By minimizing the need for additional surgeries, healthcare providers can reduce patient morbidity and improve overall satisfaction.
Institutional Safety Standards
Institutional safety standards play a pivotal role in shaping ENT surgical practices. These standards encompass a wide range of protocols, from infection control to emergency preparedness. By adhering to these standards, healthcare institutions can ensure a safe environment for both patients and staff.
By focusing on these quality measures and safety protocols, ENT surgical practices can significantly enhance patient care and outcomes. Continuous monitoring and improvement of these measures are essential in maintaining high standards of care.
Advanced Techniques Reducing ENT Surgical Risk
Advanced techniques have transformed ENT surgery, enhancing precision and reducing complications. The integration of cutting-edge technologies has significantly improved patient outcomes and minimized risks associated with ENT procedures.
Image-Guided Surgery Benefits
Image-guided surgery has revolutionized the field of ENT by providing surgeons with real-time imaging and precise navigation. This technology enhances the accuracy of surgical interventions, reducing the risk of complications and improving patient safety.
Key Benefits of Image-Guided Surgery:
- Enhanced precision in surgical navigation
- Reduced risk of complications
- Improved patient outcomes
Image-guided surgery is particularly beneficial in complex ENT procedures, such as endoscopic sinus surgery, where precise navigation is crucial.
Robotic Applications in ENT
Robotic applications in ENT surgery have gained popularity due to their ability to enhance precision and dexterity. Robotic systems provide surgeons with improved visualization and control, allowing for more complex procedures to be performed with greater accuracy.
|
Robotic System |
Benefits |
ENT Applications |
|---|---|---|
|
da Vinci Surgical System |
Enhanced precision, improved visualization |
Tonsillectomy, thyroidectomy |
|
Robotic Endoscope |
Improved dexterity, reduced tremor |
Sinus surgery, skull base surgery |
Intraoperative Monitoring Technologies
Intraoperative monitoring technologies play a crucial role in enhancing patient safety during ENT surgical procedures. These technologies provide real-time feedback on critical structures, such as nerves, allowing surgeons to adjust their technique accordingly.
Examples of intraoperative monitoring technologies include:
- Electromyography (EMG) for nerve monitoring
- Electroencephalography (EEG) for brain activity monitoring
By utilizing these advanced techniques, ENT surgeons can significantly reduce the risks associated with surgical procedures, improving patient outcomes and enhancing the overall quality of care.
Case Study: LIV Hospital’s Approach to ENT Surgical Safety
A case study on LIV Hospital reveals its innovative approach to ensuring ENT surgical safety. LIV Hospital has established a comprehensive framework that integrates various disciplines to provide high-quality care.
Multidisciplinary Care Model
LIV Hospital’s multidisciplinary care model is a cornerstone of its ENT surgical safety protocol. This approach brings together specialists from various fields, including otolaryngology, anesthesiology, and nursing, to create a cohesive care team.
Key components of this model include:
- Preoperative assessment and planning
- Intraoperative care coordination
- Postoperative monitoring and support
A leading ENT surgeon at LIV Hospital notes, “Our multidisciplinary approach ensures that every patient receives comprehensive care, minimizing risks and optimizing outcomes.”
“The integration of different specialties has significantly improved our ENT surgical safety record,”
Reported Outcomes and Safety Metrics
LIV Hospital tracks and reports various safety metrics to continuously improve its ENT surgical services. Some of the key metrics include:
|
Safety Metric |
LIV Hospital Performance |
National Average |
|---|---|---|
|
Complication Rate |
2.5% |
4.2% |
|
Readmission Rate |
1.8% |
3.5% |
|
Infection Rate |
0.5% |
1.2% |
LIV Hospital’s performance in these areas demonstrates its commitment to ENT surgical safety.
Patient Selection and Preparation Protocols
Effective patient selection and preparation are critical to ENT surgical safety. LIV Hospital has developed rigorous protocols to ensure that patients are adequately prepared for surgery.
These protocols include:
- Comprehensive preoperative evaluation
- Personalized risk assessment
- Patient education on postoperative care
By following these protocols, LIV Hospital minimizes risks and enhances patient outcomes in ENT surgery.
Managing Expectations: Informed Consent in ENT Surgery
Effective informed consent in ENT surgery is about more than just legal compliance; it’s about patient-centered care. Informed consent is a critical process that ensures patients are well-informed about their treatment options, including the potential risks and benefits associated with their surgery.
Communicating Procedure-Specific Risks
One of the key elements of informed consent is communicating procedure-specific risks. This involves discussing the potential complications that can arise during or after the surgery. For ENT procedures, this might include risks such as bleeding, infection, or changes in voice or hearing. It’s essential to present this information in a clear and understandable manner.
- Discuss potential complications and their likelihood
- Explain the measures in place to mitigate these risks
- Provide information on what to expect during recovery
Documentation Best Practices
Proper documentation is vital in the informed consent process. This includes not only the consent form itself but also any discussions or materials provided to the patient. Best practices for documentation involve ensuring that all information is accurate, comprehensive, and accessible to the patient.
Key aspects of documentation include:
- Clear description of the procedure
- Details of potential risks and benefits
- Alternatives to the proposed surgery
- Patient’s questions and concerns addressed
Shared Decision-Making Approach
A shared decision-making approach involves collaboration between the healthcare provider and the patient to make informed decisions about care. This approach respects the patient’s autonomy while leveraging the clinician’s expertise.
The benefits of shared decision-making include:
- Improved patient satisfaction
- Better adherence to treatment plans
- More personalized care
By integrating informed consent, clear communication of risks, thorough documentation, and a shared decision-making approach, ENT surgeons can manage patient expectations effectively and ensure a positive surgical experience.
Conclusion: Balancing Risks and Benefits in ENT Surgery
ENT surgery involves a delicate balance of risks and benefits, and understanding these factors is crucial for making informed decisions. The Revised Cardiac Risk Index (RCRI) score and other risk assessment tools play a vital role in evaluating the potential risks associated with ENT surgical procedures.
By assessing the RCRI score and considering other risk factors, healthcare providers can identify patients who may be at higher risk for complications and take steps to mitigate these risks. This may involve optimizing preoperative care, selecting the most appropriate surgical approach, and ensuring that patients are adequately prepared for the procedure.
Ultimately, balancing risks and benefits in ENT surgery requires a comprehensive understanding of the potential risks and benefits associated with each procedure. By leveraging risk assessment tools and taking a patient-centered approach, healthcare providers can help ensure that patients receive the best possible outcomes.
Effective communication between healthcare providers and patients is also essential in balancing ent surgery risks and benefits. By clearly discussing the potential risks and benefits of ENT surgery, patients can make informed decisions about their care.
FAQ
What is the RCRI score and how is it used in ENT surgery?
The Revised Cardiac Risk Index (RCRI) score is a tool used to assess cardiac risk in patients undergoing surgery, including ENT procedures. It evaluates six components to predict the likelihood of cardiac complications.
What are the key risk factors in ENT surgery?
Key risk factors in ENT surgery include patient comorbidities, the type of surgical procedure, and anesthesiological risks. Preoperative assessment is crucial in identifying these factors.
How does the RCRI calculator work?
The RCRI calculator assesses six components: high-risk surgery, history of ischemic heart disease, history of congestive heart failure, history of cerebrovascular disease, diabetes requiring insulin, and preoperative serum creatinine level. It provides a score that stratifies the patient’s cardiac risk.
What is the difference between monitored anesthesia care and general anesthesia in ENT procedures?
Monitored anesthesia care involves sedation and monitoring, while general anesthesia induces a state of unconsciousness. The choice between the two depends on the procedure, patient factors, and anesthesiologist preference.
What are the specific risks associated with common ENT surgeries like tonsillectomy and thyroidectomy?
Tonsillectomy risks include bleeding and airway complications, while thyroidectomy risks include nerve injury and hypocalcemia. Understanding these risks is essential for informed consent and preoperative planning.
How do socioeconomic disparities affect ENT surgical outcomes?
Socioeconomic disparities can impact access to care, with rural areas and lower-income populations potentially facing barriers to specialized ENT care, leading to differences in complication rates and outcomes.
What advanced techniques are being used to reduce ENT surgical risk?
Techniques such as image-guided surgery, robotic applications, and intraoperative monitoring technologies are being used to enhance precision and reduce complications in ENT surgery.
What is the importance of informed consent in ENT surgery?
Informed consent is crucial as it involves communicating procedure-specific risks, benefits, and alternatives to patients, enabling them to make informed decisions about their care.
How do high-volume centers compare to national benchmarks in terms of ENT surgery complication rates?
High-volume centers often report lower complication rates compared to national benchmarks due to their experience, specialized care, and adherence to safety protocols.
What role does the Goldman Risk Index Calculator play in surgical risk assessment?
The Goldman Risk Index Calculator is another tool used to assess cardiac risk in surgical patients, providing an additional layer of risk stratification that can be used alongside the RCRI score.
How does patient selection impact the risk of ENT surgical procedures?
Patient selection criteria, including medical history and current health status, play a significant role in determining the risk associated with ENT surgical procedures.
What are the benefits of minimally invasive approaches in ENT surgery?
Minimally invasive approaches can reduce recovery time, minimize scarring, and decrease the risk of complications, making them an attractive option for many ENT procedures.
When should surgery be delayed or canceled based on preoperative assessment?
Surgery should be delayed or canceled if the preoperative assessment reveals significant risks that outweigh the benefits of proceeding with surgery, such as uncontrolled cardiac conditions.
Reference
Tonsillectomy complications (pediatrics) → https://pubmed.ncbi.nlm.nih.gov/26915058/



































