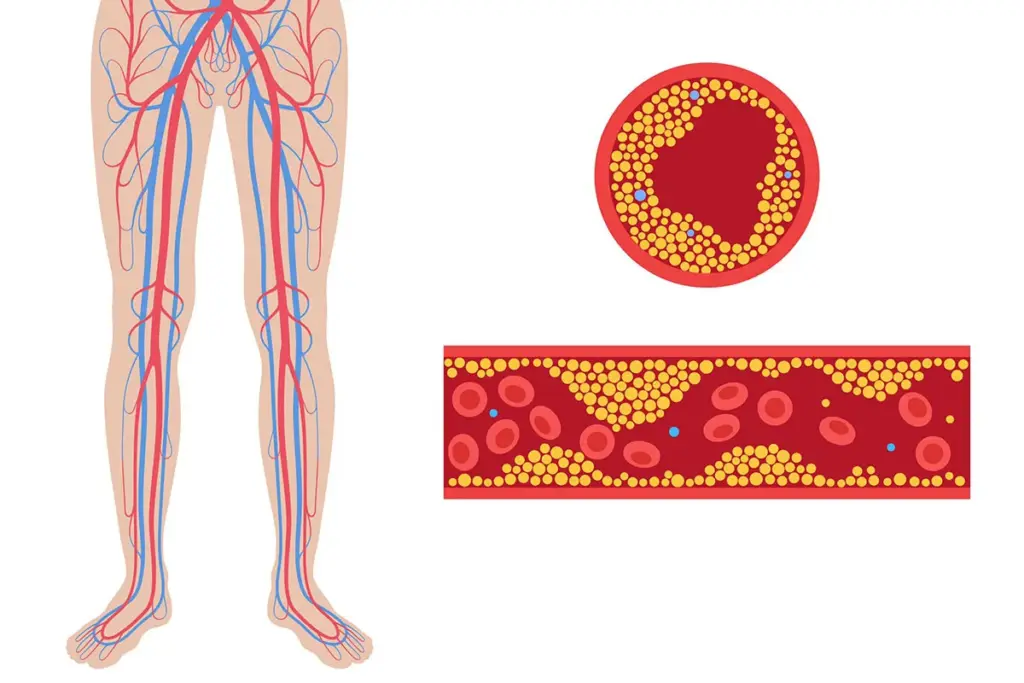
Can you Reverse Peripheral Arterial Disease? Discover key steps and lifestyle changes that may help improve your condition and restore health safely.
Peripheral artery disease (PAD) affects over 8 million Americans. Yet, it’s often not diagnosed or treated enough.
This condition happens when blood vessels outside the heart narrow or become blocked. This reduces blood flow to the limbs. PAD can make daily activities hard and cause a lot of pain.
It’s important to manage PAD to avoid serious problems and improve health. Knowing about PAD and its symptoms is the first step to managing it well.
Key Takeaways
- PAD is a common condition affecting millions of Americans.
- Reduced blood flow to the limbs can cause significant discomfort.
- Effective management of PAD is key to prevent complications.
- Understanding PAD symptoms is essential for managing the condition.
- Lifestyle changes can play a big role in managing PAD.
What Is Peripheral Arterial Disease?

Peripheral Arterial Disease (PAD) is a condition that affects the blood vessels outside the heart. It’s important to understand PAD’s definition, causes, and its impact on health in the United States.
Definition and Pathophysiology
PAD is when the blood vessels in the legs narrow or block. This is often due to atherosclerosis, where plaque builds up. This restricts blood flow to the limbs.
The pathophysiology of PAD involves inflammation, endothelial dysfunction, and smooth muscle cell proliferation. These factors interact in complex ways.
The reduced blood flow in PAD can cause pain when walking, cramping, and weakness in the legs. In severe cases, it can lead to critical limb ischemia. This can cause gangrene and amputation if not treated.
Prevalence and Impact in the United States
PAD is a big public health issue in the United States. The American Heart Association says PAD affects about 8.5 million Americans aged 40 and older. It’s more common with age and in people with risk factors like smoking, diabetes, high blood pressure, and high cholesterol.
The effects of PAD on public health are huge. It affects mobility and quality of life. It also shows a higher risk of heart attack, stroke, and death from heart disease.
Recognizing PAD Symptoms
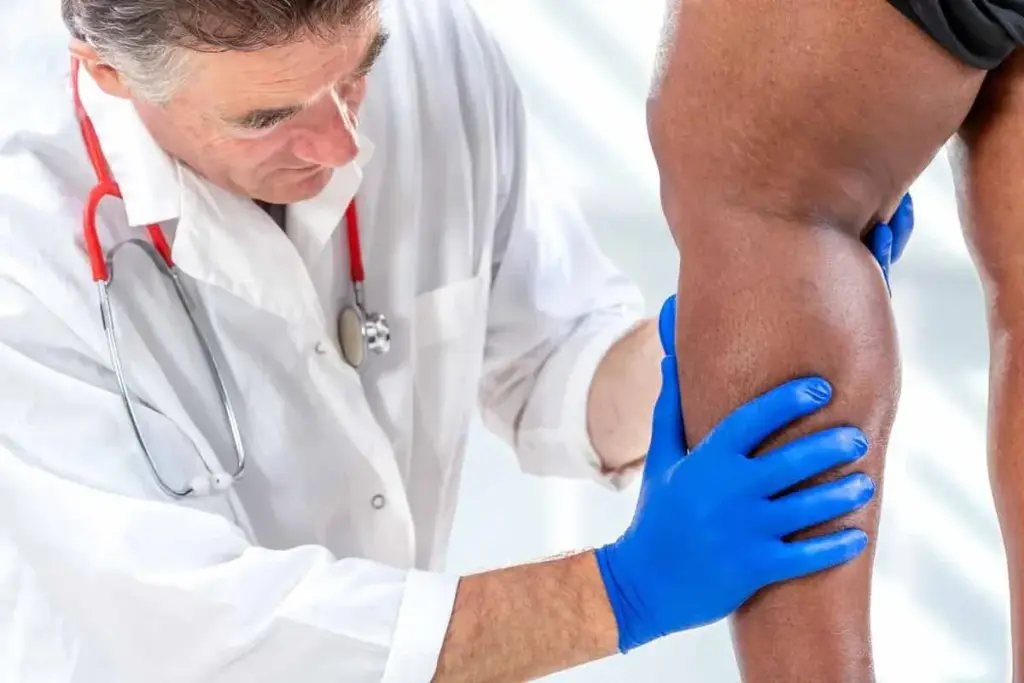
Knowing the symptoms of PAD is key to managing it well. Peripheral Artery Disease shows signs that patients should watch for. This helps them get medical help on time.
Classic Symptoms and Warning Signs
The main symptom of PAD is intermittent claudication. It’s pain or discomfort in the legs when you’re active, like walking. This pain goes away when you rest but comes back when you move again.
Other common symptoms include:
- Pain at rest, often in the toes or feet, which can mean severe PAD
- Numbness or weakness in the legs
- Coldness in the lower leg or foot, compared to the other leg
- Sores or wounds on the legs or feet that heal slowly
Silent PAD: When Symptoms Aren’t Obvious
Studies show up to 50% of PAD patients may not show symptoms, known as silent PAD. They might not have the usual PAD symptoms. This makes it hard to diagnose just by symptoms.
Even without obvious symptoms, PAD can get worse. Silent PAD can cause serious problems if not treated. So, it’s vital to check for risk factors and screen those at high risk of PAD.
Knowing about silent PAD is important. It shows the need to be aware and manage risk factors, even without symptoms.
Risk Factors for Developing PAD
Knowing the risk factors for Peripheral Arterial Disease (PAD) is key to preventing and managing it. Many factors can lead to PAD. Spotting these early can help in treatment.
Modifiable Risk Factors
Modifiable risk factors are things we can change to lower PAD risk. The top ones include:
- Smoking: Smoking harms artery linings and cuts blood flow.
- Diabetes: Diabetes damages blood vessels and nerves, raising PAD risk.
- Hypertension: High blood pressure damages arteries, making them more prone to PAD.
- High Cholesterol: High LDL cholesterol can cause artery plaque, increasing PAD risk.
By managing these risk factors through lifestyle changes and medical care, we can lower PAD risk.
Non-Modifiable Risk Factors
Non-modifiable risk factors are things we can’t change. These include:
- Age: PAD risk grows with age, more so after 50.
- Family History: A family history of PAD or heart disease raises risk.
- Genetics: Some genetic conditions make people more likely to get PAD.
Even though we can’t change non-modifiable risk factors, knowing them helps. It helps both individuals and healthcare providers watch for PAD and manage other risk factors better.
How Doctors Diagnose Peripheral Arterial Disease
Diagnosing Peripheral Arterial Disease (PAD) is a detailed process. It uses both physical checks and advanced tests. Accurate diagnosis is key to start the right treatment and help patients get better.
Physical Examination and Medical History
The first step is a detailed physical examination and looking at the patient’s medical history. Doctors search for signs like leg pain when walking, coldness, or weakness. They also check for risk factors like smoking, diabetes, and high blood pressure.
During the exam, doctors feel the pulses in the legs and feet. They look for signs of poor circulation, like hair loss, thickened toenails, or slow-healing sores.
Diagnostic Tests and Procedures
After the initial check, several diagnostic tests are done to confirm PAD and see how severe it is. The Ankle-Brachial Index (ABI) is a common test. It compares ankle and arm blood pressure. A lower ABI means PAD.
The Doppler ultrasound is another key tool. It uses sound waves to see blood flow and find blockages. Other tests include angiography and blood tests to check for risk factors.
These tests help doctors not just diagnose PAD but also plan the best treatment for each patient.
Complications of Untreated PAD
Untreated PAD can lead to serious problems, like critical limb ischemia and more heart issues. Peripheral Arterial Disease affects the arteries, causing severe issues if not treated.
Critical Limb Ischemia and Amputation Risk
Critical limb ischemia (CLI) is a severe blockage in the arteries. It cuts off blood flow to the legs, causing pain, tissue damage, and even amputation if not treated. The chance of losing a limb is much higher with CLI, making early treatment critical.
Key statistics related to CLI and amputation risk include:
|
Condition |
Risk Level |
Potential Outcome |
|---|---|---|
|
Critical Limb Ischemia |
High |
Amputation, Cardiovascular Events |
|
Untreated PAD |
Moderate to High |
Progression to CLI, Reduced Mobility |
Cardiovascular Complications
PAD is not just a problem for the limbs; it shows a bigger issue with heart health. It means a higher risk of heart attacks and strokes. This is because PAD is linked to widespread atherosclerosis.
The relationship between PAD and heart health is complex, involving factors such as:
- Shared risk factors (e.g., smoking, diabetes, hypertension)
- Atherosclerotic plaque instability
- Systemic inflammation
Impact on Mobility and Quality of Life
PAD can greatly affect how well you move and your overall happiness. Symptoms like intermittent claudication can make it hard to stay active. This can lead to a drop in health and happiness. It’s important to manage PAD well to keep moving and feeling good.
The impact on mobility can be summarized as follows:
- Reduced walking distance due to claudication
- Increased fatigue and decreased physical activity
- Potential for decreased independence
Medical Treatments for Peripheral Arterial Disease
Peripheral Arterial Disease (PAD) treatment includes many medical strategies. These aim to lower the risk of heart problems and improve life quality. Effective management of PAD involves lifestyle changes and medicines.
Antiplatelet and Anticoagulant Medications
Antiplatelet drugs like aspirin and clopidogrel prevent platelet clumping. This reduces the risk of blood clots in PAD patients. Anticoagulant drugs, such as warfarin, are used to stop blood clotting.
Guidelines recommend antiplatelet therapy for PAD management. It helps lower the risk of heart attacks and strokes.
Cholesterol-Lowering Drugs
Cholesterol-lowering drugs, like statins, are key in managing PAD. They lower LDL cholesterol, slowing atherosclerosis growth.
Statins not only lower cholesterol but also have anti-inflammatory effects. These effects help stabilize plaques and improve heart health.
Other Medications for PAD Management
Other drugs are used to manage PAD symptoms and improve walking. These include medications that enhance blood flow or reduce claudication symptoms.
Cilostazol is an example. It improves walking by increasing blood flow to the limbs.
|
Medication Type |
Primary Use in PAD |
Examples |
|---|---|---|
|
Antiplatelet |
Prevent thrombotic events |
Aspirin, Clopidogrel |
|
Anticoagulant |
Prevent blood clot formation |
Warfarin |
|
Cholesterol-Lowering |
Reduce LDL cholesterol |
Statins (e.g., Atorvastatin) |
|
Symptomatic Relief |
Improve walking distance |
Cilostazol |
Can You Reverse Peripheral Arterial Disease?
To understand if Peripheral Arterial Disease (PAD) can be reversed, we need to look at the latest research. PAD is not curable, but treatments and lifestyle changes can slow its progress and ease symptoms.
Current Medical Evidence on Reversibility
Medical studies show that PAD can’t be fully reversed. But, managing risk factors and using the right treatments can slow it down and make symptoms better. Lifestyle changes and medicines can help manage the condition.
Reversibility in PAD means improving symptoms and slowing the disease, not getting rid of it completely. Research shows that exercise, quitting smoking, and certain medicines can greatly improve life for PAD patients.
Factors That Influence Disease Progression
Many things affect how PAD progresses. Modifiable risk factors like smoking, high blood pressure, and high cholesterol are key. Non-modifiable factors like age and family history also play a role. It’s important to manage these risk factors to slow the disease.
|
Risk Factor |
Impact on PAD Progression |
Management Strategy |
|---|---|---|
|
Smoking |
Significantly accelerates PAD progression |
Smoking cessation programs |
|
High Blood Pressure |
Increases risk of PAD complications |
Antihypertensive medications, lifestyle changes |
|
High Cholesterol |
Contributes to plaque buildup in arteries |
Statins, dietary changes |
Setting Realistic Treatment Goals
Setting realistic goals is key to managing PAD well. Goals include better symptoms, more mobility, and lower heart disease risk. Doctors and patients work together to create plans that fit the patient’s needs and risk factors.
Realistic expectations help patients understand what their treatment can do. This makes them more likely to stick with the plan. Regular check-ups with doctors are important to keep the treatment on track.
Lifestyle Changes That Improve PAD Outcomes
Changing your lifestyle can greatly help if you have Peripheral Arterial Disease (PAD). Focus on quitting smoking, eating better, and managing your weight. These steps can boost your vascular health and lower PAD risks.
Smoking Cessation: The Single Most Important Step
Quitting smoking is key for PAD patients. Smoking harms blood vessels, cuts blood flow, and raises heart risks. Stopping can improve blood flow, lower heart attack and stroke risks, and slow PAD.
Nicotine replacement therapy (NRT) and certain meds can double your chances of quitting. Talk to your doctor to find the best way to quit for you.
Dietary Approaches for Arterial Health
Eating right is important for PAD management. A diet full of fruits, veggies, whole grains, and lean proteins helps. The DASH diet and Mediterranean diet are good for your heart.
- Eat more omega-3s from fish like salmon and sardines
- Add foods rich in antioxidants, like berries and leafy greens
- Lower intake of saturated fats, trans fats, and cholesterol
Weight Management Strategies
Keeping a healthy weight is critical for PAD patients. Extra weight strains the heart. Diet and exercise can help you stay at a good weight.
For weight control, aim for:
- Realistic weight loss goals
- Regular physical activity, like walking or swimming
- Watch your calorie intake and eat balanced
By making these lifestyle changes, PAD patients can see big improvements in their health and life quality.
Exercise Therapy: A Cornerstone of PAD Management
Exercise therapy is a key part of treating PAD. It helps patients live better lives and do more things. It’s known to help people walk farther and feel less pain.
Supervised Exercise Programs and Their Benefits
Supervised exercise programs are highly recommended for PAD. They happen in a clinic with doctors watching. The benefits include:
- Personalized plans that fit the patient’s needs
- Monitoring and adjusting the plan as needed
- More motivation to stick with the program
- Less chance of problems because of the supervision
Studies have shown these programs can make walking better and lessen symptoms.
Developing an Effective Home Exercise Routine
For those who can’t go to a clinic, a home routine is a good option. To make a good home plan:
- Begin with short, easy sessions and slowly get harder
- Do exercises that are good for your heart, like walking or biking
- Keep track of how you’re doing and change the plan if needed
- Use gadgets or apps to track your activity and stay motivated
Being consistent is important for home routines. Try to exercise at least three times a week.
Overcoming Pain and Exercise Limitations
One big challenge with PAD is dealing with pain and limits. Ways to handle this include:
- Begin slowly and slowly get more intense to avoid pain
- Choose exercises that are easy on your body
- Use pain relief methods, like medicine or relaxation, as your doctor suggests
Knowing the good and bad of exercise therapy helps PAD patients make better choices. This can lead to better health and quality of life.
Minimally Invasive Interventions for PAD
Minimally invasive treatments have changed how we treat Peripheral Arterial Disease (PAD). These methods are safer than open surgery. They offer quicker recovery times and fewer side effects.
Angioplasty and Stenting Procedures
Angioplasty uses a balloon to open blocked arteries. A stent is often placed to keep the artery open. Stenting has greatly improved angioplasty results by lowering the chance of the artery getting blocked again.
The process starts with a small incision in the groin or arm. A catheter is guided to the blocked area. The balloon is then inflated to push the plaque against the artery walls. If a stent is used, it’s placed to keep the artery open.
Atherectomy and Other Catheter-Based Treatments
Atherectomy removes plaque from arteries. There are different types, like laser and rotational atherectomy, each removing plaque in its own way.
Other treatments include thrombectomy (removing blood clots) and subintimal angioplasty (for total occlusions). The right treatment depends on the patient’s condition and the blockage.
Recovery and Long-Term Outcomes
Recovery from these treatments is faster than open surgery. Most patients can go back to normal activities in a few days. But, success over time depends on health, PAD severity, and following treatment plans.
|
Procedure |
Recovery Time |
Long-Term Success Factors |
|---|---|---|
|
Angioplasty and Stenting |
1-3 days |
Adherence to medication, lifestyle changes |
|
Atherectomy |
1-5 days |
Regular follow-up, management of risk factors |
|
Catheter-Based Treatments |
1-3 days |
Monitoring for restenosis, healthy lifestyle |
Knowing about these treatments helps patients make better choices. It’s important to talk to a doctor about the benefits and risks. This way, you can find the best treatment for you.
Surgical Treatments for Advanced PAD
Surgical options, like bypass surgery, are for those with advanced PAD who haven’t seen improvement with other treatments. These surgeries aim to improve blood flow, ease symptoms, and prevent serious problems.
Bypass Surgery Techniques and Approaches
Bypass surgery makes a new path around blocked or narrowed arteries using a graft. This graft can come from another part of the body or be synthetic. It helps increase blood flow to the affected limb.
Types of Bypass Grafts:
- Autogenous vein grafts (using the patient’s own veins)
- Synthetic grafts (made of materials like Dacron or PTFE)
- Composite grafts (combination of autogenous and synthetic materials)
The right graft depends on the patient’s health, the blockage’s location and size, and graft availability.
Determining Surgical Candidacy
Not everyone with advanced PAD is a good candidate for surgery. The choice to have surgery depends on symptom severity, disease extent, overall health, and other health issues.
|
Factor |
Description |
Importance in Surgical Candidacy |
|---|---|---|
|
Severity of Symptoms |
Presence and intensity of pain, claudication, and other symptoms |
High |
|
Extent of Arterial Disease |
Location and extent of arterial blockages or narrowing |
High |
|
Overall Health Status |
Presence of comorbid conditions like diabetes, hypertension, heart disease |
High |
|
Previous Surgical Interventions |
History of previous vascular surgeries or interventions |
Moderate |
Weighing Risks and Benefits of Surgery
Surgery for advanced PAD has both good and bad sides. Benefits include better blood flow, symptom relief, and lower risk of losing a limb. But, there are risks like infection, graft failure, and anesthesia complications.
It’s important for patients to talk to their healthcare provider about these points to make a well-informed choice.
Choosing surgery should be after a full evaluation of the patient’s situation and a detailed talk about possible outcomes.
Living With PAD: Daily Management Strategies
To manage PAD well, you need to take care of your feet, handle pain, and get emotional support. It’s not just about medical treatment. It’s also about changing your lifestyle to live better.
Foot Care and Wound Prevention
Foot care is key for PAD patients. The disease cuts off blood flow to your feet, raising the risk of wounds and infections. Here’s how to keep your feet healthy:
- Daily check your feet for cuts, sores, or swelling
- Keep your feet clean and dry
- Wear shoes that fit well and are comfy
- Avoid walking barefoot
- Trim your toenails carefully to avoid cuts
Table: Foot Care Tips for PAD Patients
|
Foot Care Activity |
Frequency |
Tips |
|---|---|---|
|
Inspect feet |
Daily |
Use good lighting and a mirror to check soles |
|
Wash feet |
Daily |
Use warm water, dry thoroughly, avoiding between toes |
|
Moisturize |
Daily |
Avoid lotion between toes |
Pain Management Approaches
Managing pain is vital for PAD patients. There are many ways to ease pain, including:
- Medications from your doctor
- Exercise to boost circulation
- Alternative methods like acupuncture or massage
Emotional and Psychological Support
Living with PAD affects your emotions and mind. Getting support is key for your well-being. You can find support from:
- Support groups for PAD patients
- Counseling or therapy
- Family and friends
Emotional support helps you deal with PAD’s challenges. It makes your life better.
Conclusion
Managing peripheral artery disease (PAD) needs a mix of lifestyle changes, medical treatments, and interventions. Knowing about PAD, its signs, and risk factors helps people manage it better. This way, they can take early steps to handle PAD.
A good treatment plan includes quitting smoking, eating right, and doing supervised exercises. These steps can greatly help PAD outcomes. Medications like antiplatelets and anticoagulants, and procedures like angioplasty and stenting, are also key in managing PAD.
In summary, a treatment plan for PAD should involve both healthcare providers and patients. Working together, people with PAD can lower their risk of serious problems. They can also improve their life quality and achieve better health results.
FAQ
What is Peripheral Arterial Disease (PAD)?
PAD is a condition where the arteries in the legs and arms get narrowed or blocked. This reduces blood flow. It can cause pain, cramping, and other symptoms.
What are the symptoms of PAD?
Symptoms of PAD include pain or cramping in the legs when walking. It can also cause pain at rest and numbness. Some people may not show symptoms, known as silent PAD.
What are the risk factors for developing PAD?
Risk factors for PAD include smoking, high blood pressure, and high cholesterol. Diabetes is also a risk. Non-modifiable factors include age, family history, and ethnicity.
How is PAD diagnosed?
PAD is diagnosed through physical exams, medical history, and tests. Tests include the ankle-brachial index (ABI), Doppler ultrasound, and angiography.
What are the complications of untreated PAD?
Untreated PAD can lead to serious problems. These include critical limb ischemia, amputation, and heart attack. It can also affect mobility and quality of life.
Can PAD be reversed?
PAD can’t be completely cured. But managing risk factors and making lifestyle changes can slow disease progression. This can improve symptoms.
What lifestyle changes can improve PAD outcomes?
Quitting smoking, eating right, and managing weight can help PAD outcomes. These changes promote arterial health.
What is the role of exercise therapy in PAD management?
Exercise therapy is key in managing PAD. It includes supervised programs and home exercises. It helps improve symptoms and mobility.
What are the treatment options for PAD?
PAD treatments include medications and minimally invasive procedures. Angioplasty and stenting are options. Surgical treatments like bypass surgery are also available.
How can I manage PAD on a daily basis?
Managing PAD daily involves foot care, pain management, and emotional support. Working with a healthcare provider is essential to create a personalized plan.
Are there any medications that can help manage PAD?
Yes, medications like antiplatelet and anticoagulant drugs can help. Cholesterol-lowering drugs and other medications also reduce cardiovascular risk.
What are the benefits and risks of surgical treatments for PAD?
Surgical treatments like bypass surgery can improve blood flow and symptoms. But they carry risks like infection and graft failure. Discussing benefits and risks with a healthcare provider is important.
References
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5182010/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























