Uterine prolapse happens when the uterus drops into or outside the vagina. It’s common after childbirth and during menopause. This issue is caused by weak pelvic floor muscles and ligaments. The Medical organization says it can lead to pain, discomfort, and trouble with urination or bowel movements. Guide to using a hysterectomy for prolapse (uterine) as a surgical solution for severe cases.
Dealing with a prolapsed uterus can be tough. Hysterectomy surgery, which removes the uterus, is a key solution for severe cases. At Liv Hospital, we focus on our patients, giving them the best care for uterine prolapse treatment. We aim to ease their pain and improve their life quality.
Key Takeaways
- Uterine prolapse is a common condition affecting women, specially after childbirth and during menopause.
- The condition is caused by weakening pelvic floor muscles and ligaments.
- Symptoms include pelvic pressure, discomfort, and urinary or bowel difficulties.
- Hysterectomy surgery is a definitive treatment for severe uterine prolapse.
- A patient-centered approach is key for complete care.
Understanding Uterine Prolapse
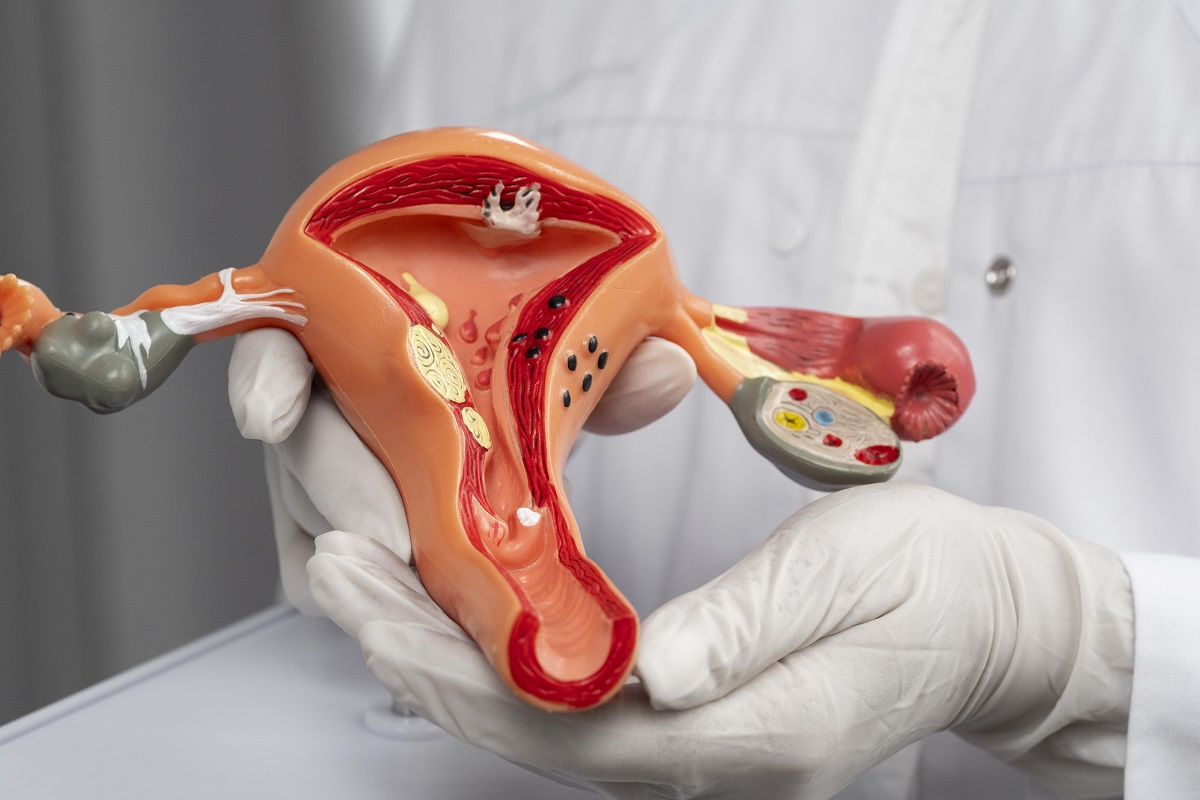
A prolapsed uterus happens when the uterus slips out of its normal spot. This can really affect a woman’s life. It causes symptoms and problems, so it’s key to know about it well.
What is a Dropped or Prolapsed Uterus?
A dropped or prolapsed uterus means the uterus falls into or comes out of the vagina. This happens when the muscles and ligaments that hold it up get weak. The prolapse can be mild or very severe.
Grades and Severity of Prolapse
Uterine prolapse is graded to show how bad it is. Doctors use this system to figure out how to treat it. The grades go from I to IV, with I being the least severe and IV being the worst, where the uterus is outside the vagina.
Grade | Description |
I | Mild prolapse, where the uterus is slightly displaced but is inside the vagina. |
II | Moderate prolapse, where the uterus is lower in the vagina. |
III | Severe prolapse, where the uterus is near or at the vaginal opening. |
IV | Complete prolapse, where the uterus is completely outside the vagina. |
Common Symptoms and Signs
The symptoms of uterine prolapse can differ based on how severe it is. Common signs include feeling heavy or uncomfortable in the lower belly or vagina. Women might also have trouble with urination or bowel movements. Sometimes, they might feel like something is “dropped” or sticking out from the vagina.
These symptoms can really affect a woman’s daily life and happiness. According to NHS, they can make life hard for many women.
“Women with uterine prolapse often experience a range of symptoms that can affect their quality of life, from physical discomfort to emotional distress.”
It’s important to know these symptoms and how severe the prolapse is to find the right treatment. By recognizing the signs and getting medical help, women can get better care and live better lives.
Causes and Risk Factors for Uterine Prolapse
Many things can make you more likely to get uterine prolapse. Weakened pelvic floor muscles and having had vaginal deliveries are big ones. Knowing what causes it helps in stopping it and treating it.
Weakening of Pelvic Floor Muscles
The pelvic floor muscles are key in keeping the uterus in place. If they get weak, a prolapse can happen. Things that make them weak include:
- Childbirth, mostly if you’ve had many vaginal deliveries
- Getting older
- Chronic coughing or straining
Pelvic floor muscle strength is key for keeping the uterus in its spot. Doing things that strain these muscles can up your risk of prolapse.
Pregnancy and Vaginal Delivery
Pregnancy and childbirth are big risks for uterine prolapse. The strain of pregnancy and vaginal delivery can make the pelvic floor muscles weak. The NCBI Bookshelf says vaginal delivery is a big reason for pelvic organ prolapse.
Age-Related Changes
As women get older, the muscles and ligaments that hold up the uterus get weaker. This makes prolapse more likely. Menopause also plays a part because estrogen levels drop.
Age Group | Risk Factors |
Young Women | Pregnancy, vaginal delivery |
Menopausal Women | Decreased estrogen, age-related muscle weakening |
Older Women | Cumulative effect of age and previous risk factors |
Other Contributing Factors
Other things can also lead to uterine prolapse. These include:
- Chronic constipation or straining during bowel movements
- Being overweight
- Having had pelvic surgery before
Knowing these risk factors helps in preventing and catching uterine prolapse early.
Diagnosing a Prolapsed Uterus
Doctors use a few ways to find out if you have a prolapsed uterus. They start by asking you about your health and symptoms. This helps them understand what might be causing your problem.
Physical Examination Process
A pelvic exam is key in finding out if you have a prolapsed uterus. Your doctor will check how your uterus is sitting and how strong your pelvic muscles are. They might ask you to cough or bear down to see how bad it is.
Key parts of the exam are:
- Looking at the vaginal area
- Feeling the uterus to see its size and position
- Checking how strong your pelvic muscles are
Imaging Tests and Procedures
Even with a physical exam, doctors might want to do more tests. These can help them see how bad the prolapse is or check for other problems. Tests might include:
- Ultrasound to look at the pelvic organs
- X-rays or MRI to see how far the prolapse has gone
- Dynamic MRI to see the prolapse in different positions
Grading Systems for Prolapse Severity
Doctors use grading systems to figure out how bad the prolapse is. The most common one is the Pelvic Organ Prolapse Quantification (POP-Q) system.
Stage | Description |
0 | No prolapse |
1 | The leading edge of the prolapse is above the hymen |
2 | The leading edge is at or within 1 cm of the hymen |
3 | The leading edge is more than 1 cm below the hymen but not complete |
4 | Complete procidentia or total vaginal vault prolapse |
Knowing how bad your prolapse is helps your doctor choose the best treatment. They will talk about what they found and suggest the best plan for you.
Non-Surgical Treatment Options
Uterine prolapse can often be managed without surgery. There are many non-surgical treatments available. These can help reduce symptoms and improve your quality of life.
Pelvic Floor Exercises
Pelvic floor exercises, or Kegel exercises, are key in treating uterine prolapse without surgery. They strengthen the muscles that support the uterus, bladder, and bowel. Doing these exercises can help tone the pelvic floor and lessen prolapse symptoms.
To perform Kegel exercises effectively:
- Identify the correct muscles by stopping the flow of urine mid-stream
- Contract these muscles for 5-10 seconds
- Release for the same duration
- Repeat this cycle 10-15 times, three times a day
Pessary Devices
A pessary is a removable device placed in the vagina to support the prolapsed uterus. There are different types of pessaries, and a healthcare provider can help choose the right one for you.
Benefits of pessary use include:
- Immediate symptom relief
- Non-invasive treatment option
- Reversibility if needed
Lifestyle Modifications
Changing your lifestyle can also help manage uterine prolapse. These changes can reduce symptoms and slow the prolapse’s progression.
Recommended lifestyle changes:
- Maintaining a healthy weight to reduce pressure on the pelvic floor
- Avoiding heavy lifting or bending
- Engaging in regular, gentle exercise to improve overall pelvic health
When Conservative Treatments Fail
Non-surgical treatments work well for many, but not all. If they don’t help, you should talk to your healthcare provider. They can discuss other options, like surgery.
“The decision to proceed with surgery should be made after thorough consideration of the severity of symptoms, overall health, and personal preferences.”
Hysterectomy for Prolapse: When It’s Recommended
When other treatments don’t work, hysterectomy might be an option for prolapse. Uterine prolapse happens when the uterus moves out of place. This can cause pain and other problems. Surgery is not always needed, but it might be if the prolapse is severe and affects daily life.
Indications for Surgical Intervention
Hysterectomy is usually suggested for women with severe prolapse who haven’t found relief elsewhere. The decision to have surgery depends on the person’s health and how bad their symptoms are. Surgery is considered when:
- Severe prolapse: The uterus is way out of place, causing a lot of pain or other issues.
- Failed conservative treatments: Treatments like pessaries or exercises haven’t helped enough.
- Significant impact on quality of life: The prolapse makes everyday tasks hard or causes ongoing pain.
Determining Candidacy for Surgery
Deciding if someone is right for hysterectomy involves a detailed check-up. We look at the patient’s health, how bad the prolapse is, and if there are other pelvic floor problems. We consider:
- The patient’s medical history and current health.
- How bad the prolapse is and how it affects daily life.
- If there are other pelvic floor issues that need to be fixed at the same time.
Discussing Options with Your Healthcare Provider
Talking openly with your doctor about hysterectomy is key. We discuss the benefits and risks based on your situation. This includes:
- What the surgery involves and what you can expect.
- The possible risks and complications of the surgery.
- Other treatments that might work for you.
By talking with your doctor, you can decide if hysterectomy is the best choice for you.
Types of Hysterectomy Procedures for Uterine Prolapse
The type of hysterectomy for uterine prolapse depends on several factors. These include the severity of the prolapse and the patient’s health. We will look at the different types of hysterectomies, their benefits, and considerations.
Total vs. Subtotal Hysterectomy
A total hysterectomy removes the whole uterus, including the cervix. On the other hand, a subtotal hysterectomy takes out the upper part of the uterus but keeps the cervix. The choice between these depends on the patient’s condition and the surgeon’s advice.
“The choice between total and subtotal hysterectomy should be based on a thorough evaluation of the patient’s anatomy and the severity of the prolapse,” according to medical guidelines.
Vaginal Hysterectomy Approach
Vaginal hysterectomy is often chosen for uterine prolapse. It’s less invasive and has a quicker recovery. This method removes the uterus through the vagina, avoiding big abdominal cuts.
Benefits of Vaginal Hysterectomy:
- Less post-operative pain
- Shorter hospital stay
- Quicker return to normal activities
Abdominal Hysterectomy Approach
Abdominal hysterectomy removes the uterus through an abdominal incision. It’s needed for more complex cases or when extra repairs are needed.
Considerations for Abdominal Hysterectomy:
- Longer recovery time compared to vaginal hysterectomy
- Potential for more post-operative pain
- May be necessary for severe or complex cases
Laparoscopic and Robotic Options
Laparoscopic and robotic-assisted hysterectomy are less invasive. They use small incisions, less blood loss, and quick recovery. These methods use advanced technology to help the surgeon.
“Laparoscopic and robotic hysterectomy represent significant advancements in surgical techniques, providing patients with less invasive options and better outcomes,” say medical professionals.
Preparing for Prolapse Surgery
Getting ready for prolapse surgery is a big step. It includes talking to doctors, doing tests, and changing your lifestyle. Knowing what to expect can make you feel less anxious and help your surgery go smoothly.
Pre-Surgical Consultations and Tests
You’ll have to see your doctor before surgery. These meetings are key to talk about your health, the surgery, and any worries. Your doctor might also do tests like blood work or imaging to check your health and find any risks.
Common pre-surgical tests include:
- Complete Blood Count (CBC)
- Electrocardiogram (ECG)
- Chest X-ray
- Pelvic ultrasound
Medication Adjustments
Your doctor might tell you to change or stop some medicines before surgery. This is to lower the chance of problems during and after surgery. For example, you might stop blood thinners or change your diabetes meds.
Medication Type | Pre-Surgical Instruction |
Blood Thinners | Stop 5-7 days before surgery |
Diabetes Medication | Adjust dosage as instructed |
Antihypertensive Drugs | Continue as usual unless instructed differently |
Practical Preparations for Hospital Stay
Getting ready for the hospital is important too. You’ll need to arrange for someone to be with you, get your home ready for recovery, and pack a bag with essentials. This includes comfy clothes, insurance info, and any medicines you take.
Tips for a comfortable hospital stay:
- Bring a list of your medications and dosages
- Pack comfortable, loose-fitting clothing
- Have a friend or family member accompany you
Mental and Emotional Preparation
Getting your mind and emotions ready is just as important as your body. Try relaxation techniques like deep breathing or meditation to calm your nerves. Talking about your feelings with your doctor or a mental health expert can also help.
By preparing well for your surgery, you can make your experience and recovery better. Always follow your doctor’s advice and don’t hesitate to ask questions.
The Hysterectomy Procedure Step-by-Step
Fixing a prolapsed uterus with hysterectomy is a detailed process. We know choosing this surgery is big. Knowing what happens can ease worries.
Anesthesia and Surgical Setup
The first step is giving general anesthesia for comfort. Then, our team gets ready with the right tools for the chosen method.
Surgical Techniques for Prolapse Correction
The method for fixing prolapse varies by patient and surgeon. We pick the best way to fix it safely and effectively.
Additional Repairs During Surgery
Sometimes, we fix other problems like vaginal wall prolapse or incontinence during the surgery. Our surgeons are experts at finding and fixing these issues at the same time. This means fewer surgeries later.
Closure and Immediate Post-Op Care
After the surgery and any extra repairs, we close the cuts. Then, we watch over the patient as they wake up. We manage pain to help them recover well.
Recovery After Prolapsed Uterus Surgery
Understanding the recovery process after prolapsed uterus surgery is key. It helps patients prepare and get the best results. The recovery includes hospital stay, managing pain, and slowly getting back to activities.
Duration of Hospital Stay
The time in the hospital after surgery varies. It depends on the surgery type and the patient’s health. Patients who have vaginal hysterectomy usually stay less than those with abdominal hysterectomy.
A study in the Journal of Minimally Invasive Gynecology found a difference in hospital stays. Vaginal hysterectomy patients stay about 1-2 days. Abdominal hysterectomy patients stay 2-4 days.
Pain Management Strategies
Managing pain is important for a smooth recovery. We use medicines and other methods to help with pain.
- Medications: We give pain relief medicines to help with discomfort.
- Non-pharmacological interventions: Deep breathing, relaxation, and gentle movement also help with pain.
The Medical organization says pain management is key. Patients should tell their doctors about their pain to adjust treatment.
Activity Restrictions and Guidelines
After surgery, it’s important to follow activity restrictions. This helps with healing and avoids complications.
Activity | Recommended Restriction Period |
Heavy lifting | 4-6 weeks |
Bending or straining | 4-6 weeks |
Driving | 1-2 weeks |
Return to work | 6-8 weeks |
Expected Timeline for Recovery
Recovery times vary, but most women return to normal activities in weeks.
Typical Recovery Milestones:
- 1-2 weeks: Start doing light activities.
- 4-6 weeks: Most normal activities can be resumed, with some limits.
- 8-12 weeks: Full recovery and all activities can be resumed.
Remember, every recovery is different. By following guidelines and talking with your doctor, you can improve your recovery and outcomes.
Potential Complications and Recurrence Risks
It’s important for patients with uterine prolapse to know about the risks after hysterectomy surgery. While it’s a common treatment, understanding the possible complications is key.
Short-Term Surgical Complications
After hysterectomy, patients might face infections, bleeding, or damage to nearby organs. We do our best to avoid these issues. But, it’s vital for patients to know the signs to look out for post-surgery.
Infection is a risk with any surgery. We use antibiotics to lower this chance. Bleeding might happen too, and sometimes, it needs more surgery to fix.
Statistical Data on Recurrent Prolapse
Some patients worry about prolapse coming back after hysterectomy. Research shows the rate of recurrence depends on several things. These include the surgery method and other pelvic issues.
- A study found about 10% of patients experience recurrent prolapse within 5 years after surgery.
- Another study showed that those with a history of many surgeries or weak pelvic floor are at higher risk.
Risk Factors for Complications
Several factors can up the risk of problems after hysterectomy. These include:
- Age and health status
- Other health issues like diabetes or heart disease
- History of pelvic surgeries or radiation
- The type of surgery (abdominal, vaginal, laparoscopic, or robotic)
Impact of Surgical Approach on Outcomes
The surgery method chosen can greatly affect outcomes and risks. We look at many factors to pick the best approach for each patient.
A vaginal hysterectomy usually means quicker recovery and fewer complications than abdominal surgery. But, the right choice depends on the patient and the surgeon’s skills.
Life After Hysterectomy for Prolapsed Uterus
Life after a hysterectomy for a prolapsed uterus brings many changes. Women will face physical, emotional, and sexual changes. Knowing about these can help manage expectations and improve recovery.
Physical Changes to Expect
Women may see physical changes after a hysterectomy. The pelvic area might change, and bladder or bowel habits could shift. If the ovaries are removed, surgical menopause might occur. Following post-operative instructions carefully is key to avoid complications.
Women might feel pain, swelling, or bruising at first. These symptoms usually go away in a few weeks. Not having periods anymore can be a big relief for many.
Impact on Sexual Function
Sexual function after a hysterectomy can differ for each woman. Some might feel better due to less discomfort, while others might see changes in libido or sexual response. Talking openly with healthcare providers about these changes is important.
What affects sexual function includes the type of hysterectomy, if the ovaries were kept, and individual differences. Many women start sexual activity again 6-8 weeks after surgery, with their doctor’s okay.
Hormonal Considerations
If the ovaries are removed, women might enter surgical menopause. Hormone replacement therapy (HRT) might be suggested to ease menopausal symptoms. Women who keep their ovaries might enter menopause earlier than expected.
Managing hormonal changes can involve lifestyle changes, HRT, or other treatments. Each woman’s needs are different.
Long-Term Pelvic Floor Health
Keeping the pelvic floor healthy is vital after a hysterectomy. Doing pelvic floor exercises, staying at a healthy weight, and avoiding heavy lifting are important. These steps can help prevent future pelvic floor issues.
Regular check-ups with healthcare providers are also key. They help monitor pelvic health and address any concerns or complications.
Conclusion
It’s important for women to know about uterine prolapse and its treatments. We’ve talked about what causes it, its symptoms, and how severe it can be. We’ve also looked at the different ways to treat it, including surgery.
Hysterectomy is a serious option for severe cases. It can greatly improve a woman’s quality of life. Knowing about the different types of hysterectomy helps women talk to their doctors about the best treatment.
Good treatment for uterine prolapse needs a full plan. This plan should consider the woman’s health and what she needs. We’ve stressed the need for accurate diagnosis, getting ready for surgery, and caring for oneself after surgery.
By understanding hysterectomy and uterine prolapse treatment, women can take charge of their health. This knowledge helps them make smart choices about their care. It leads to better health and well-being.
FAQ
What is uterine prolapse and how is it related to hysterectomy surgery?
Uterine prolapse happens when the uterus slips out of place. This is due to weak pelvic muscles and ligaments. Removing the uterus through surgery is a way to treat severe cases.
What are the common symptoms of uterine prolapse?
Symptoms include feeling pressure or heaviness in the pelvis. You might also have trouble with urination or bowel movements. In some cases, the uterus can even come out of the vagina.
How is uterine prolapse diagnosed?
Doctors start by asking about your medical history and doing a pelvic exam. They use different scales to measure how bad the prolapse is.
What are the non-surgical treatment options for uterine prolapse?
You can try pelvic floor exercises, like Kegels. There are also pessary devices for support. Keeping a healthy weight and avoiding heavy lifting can also help.
When is hysterectomy recommended for uterine prolapse?
If other treatments don’t work, surgery might be suggested. The decision depends on your health and how bad the symptoms are.
What are the different types of hysterectomy procedures used for uterine prolapse?
There are vaginal, abdominal, laparoscopic, and robotic hysterectomies. The choice depends on the severity of the prolapse and your health.
How should I prepare for hysterectomy surgery?
Start by going to pre-surgery meetings and getting any needed tests. Adjust your medications and make plans for your hospital stay. Getting mentally ready is also important.
What can I expect during the recovery process after hysterectomy surgery?
Recovery times vary, but most women can get back to normal in a few weeks. You’ll need to manage pain and follow activity rules set by your doctor.
What are the possible complications of hysterectomy surgery for uterine prolapse?
Complications can include short-term issues and the chance of prolapse coming back. Knowing these risks helps you make informed choices.
How will hysterectomy surgery affect my life afterward?
You might notice changes in your menstrual cycle or sexual function. Keeping your pelvic floor muscles strong is key for long-term health.
Can uterine prolapse recur after hysterectomy surgery?
Even with the uterus removed, other prolapse types can happen. Talk to your doctor about the risks and how surgery affects outcomes.
What is the role of pelvic floor exercises in managing uterine prolapse?
Kegel exercises strengthen the muscles that hold the uterus in place. They can help symptoms and might delay or prevent surgery.
How does age affect the risk of developing uterine prolapse?
As you get older, hormone levels drop, making muscles weaker. This increases the risk of uterine prolapse.
Can lifestyle changes help manage symptoms of uterine prolapse?
Yes, staying at a healthy weight and avoiding heavy lifting can help. These changes can reduce symptoms and possibly lessen the severity of prolapse.
References
https://my.clevelandclinic.org/health/diseases/16030-uterine-prolapse



































