Sleep apnea is more than just a sleep issue; it affects vital organs. It raises the risk of heart disease, brain decline, and damage to many organs. Obstructive Sleep Apnea (OSA) mainly hits the respiratory system by blocking the airway during sleep. This causes problems in many parts of the body. Sleep apnea affects your vital organs. Discover amazing ways to protect your health and learn critical safety tips from our expert team today.
The respiratory system is where sleep apnea starts, but it affects the whole body, like the heart. The blocked airway causes a chain reaction of problems. This makes it very important to find and treat sleep apnea quickly.
Key Takeaways
- The main problem in sleep apnea is the airway blockage that happens many times during sleep.
- This blockage causes problems that affect many organs.
- The heart is greatly affected by sleep apnea.
- It’s very important to diagnose and treat sleep apnea early to avoid organ damage.
- Obstructive Sleep Apnea (OSA) is a serious condition that needs medical help.
- Knowing the sleep apnea symptoms is key to catching it early.
The Systemic Nature of Sleep Apnea
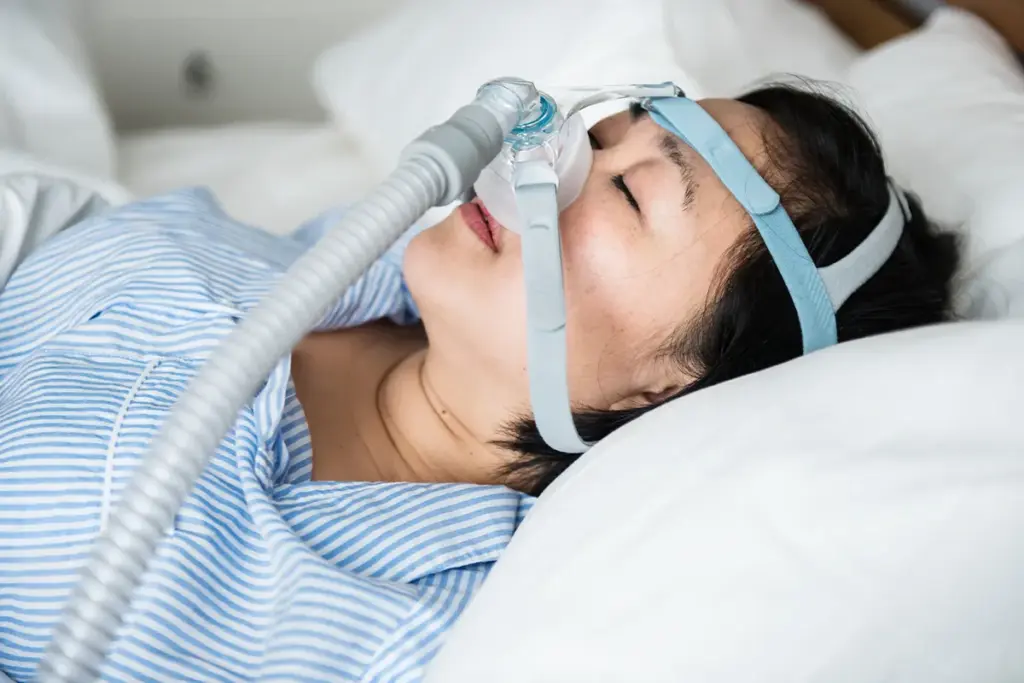
Sleep apnea is more than just a sleep disorder. It’s a condition that affects many parts of the body, causing various health problems.
Definition and Prevalence
Sleep apnea is a condition where breathing stops and starts during sleep. This can lead to poor sleep quality and low oxygen levels. It’s common, affecting millions globally.
About 4% to 7% of adults have sleep apnea, with most having the obstructive type. It’s often missed because its symptoms can be mild or mistaken for other issues. Yet, it has a big impact on health, making it a major public health issue.
The risk of sleep apnea grows with age. It’s also linked to obesity, a growing problem worldwide.
Types of Sleep Apnea Disorders
Sleep apnea isn’t just one condition. It includes several types, each with its own features. The main types are:
- Obstructive Sleep Apnea (OSA): The most common, caused by the upper airway getting blocked, usually because the throat muscles relax too much.
- Central Sleep Apnea: Happens when the brain doesn’t send the right signals to the breathing muscles.
- Complex Sleep Apnea Syndrome: A mix of OSA and central sleep apnea that starts during treatment.
Knowing the different types of sleep apnea is key for proper diagnosis and treatment. The cardiovascular system is most affected. OSA can lead to high blood pressure, heart rhythm problems, heart failure, and stroke.
Interestingly, up to 49% of patients with atrial fibrillation also have OSA. This is compared to 32% without AF. It shows how closely sleep apnea and heart health are connected.
Primary Mechanisms of Organ Damage in Sleep Apnea
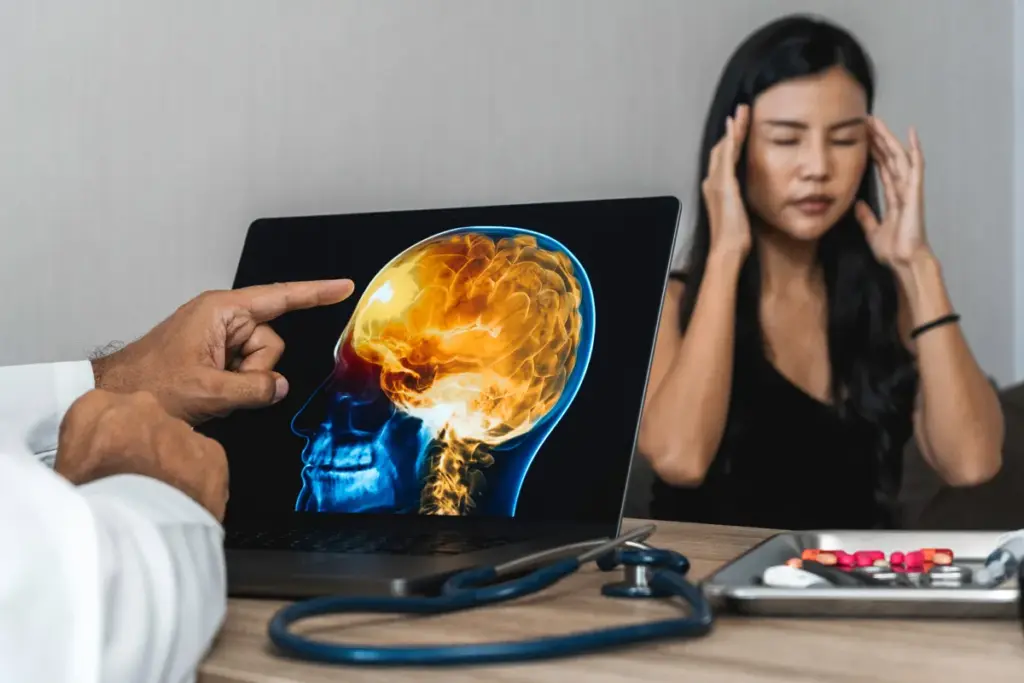
It’s important to understand how sleep apnea damages organs. This condition causes breathing to stop and start many times during sleep. It affects many parts of the body.
Chronic Intermittent Hypoxemia
Chronic intermittent hypoxemia (CIH) is a big problem in sleep apnea. It happens when the airway collapses during sleep. This leads to low oxygen levels and then high levels again.
This back-and-forth of oxygen levels hurts cells. It starts a chain reaction that damages organs.
Key effects of CIH include:
- Increased sympathetic nervous activity
- Enhanced oxidative stress
- Inflammation and cellular damage
Endothelial Dysfunction and Oxidative Stress
Endothelial dysfunction is a big problem caused by CIH. It happens when the endothelium, a layer of cells, doesn’t work right. This leads to blood vessels not working well.
Oxidative stress is another big issue. It happens when there’s too much damage from harmful compounds. These compounds can hurt cells, making organs work worse.
|
Organ/System |
Effect of CIH |
Consequence of Endothelial Dysfunction |
|---|---|---|
|
Cardiovascular System |
Hypertension, cardiac remodeling |
Atherosclerosis, increased risk of myocardial infarction |
|
Renal System |
Renal fibrosis, decreased renal function |
Reduced renal blood flow, increased risk of CKD |
|
Cerebrovascular System |
Increased risk of stroke |
Cerebral small vessel disease, cognitive decline |
The Respiratory System: Ground Zero for Sleep Apnea
Sleep apnea affects the respiratory system in many ways. It involves complex blockages in the upper airway. Obstructive sleep apnea (OSA) mainly causes these blockages during sleep.
This condition disrupts sleep and harms respiratory health. It leads to a series of problems that affect breathing.
Upper Airway Obstruction Pathophysiology
The causes of upper airway obstruction in sleep apnea are complex. They involve both the shape of the airway and how muscles work during sleep.
Key factors contributing to upper airway obstruction include:
- Anatomical characteristics: A narrow airway, big tonsils, or a large tongue can cause blockages.
- Neuromuscular factors: Muscle tone drops during sleep, leading to airway collapse.
Long-term Pulmonary Consequences
Recurring blockages in sleep apnea can harm the lungs over time. This includes chronic low oxygen levels, high blood pressure in the lungs, and lung damage.
|
Pulmonary Consequence |
Description |
Potential Impact |
|---|---|---|
|
Chronic Intermittent Hypoxemia |
Repeated episodes of low oxygen levels |
Can lead to oxidative stress and inflammation |
|
Increased Pulmonary Pressures |
Elevated blood pressure in the pulmonary arteries |
May result in pulmonary hypertension |
|
Long-term Lung Damage |
Potential for chronic lung injury |
Could exacerbate existing respiratory conditions |
Cardiovascular System: The Silent Victim of Sleep Apnea
<SEP-12124_image_4>
Sleep apnea has a big impact on the heart and blood vessels. It can cause serious problems that affect how well a patient does. This is why it’s so important to take action right away.
The link between sleep apnea and heart disease is complex. Knowing how sleep apnea affects the heart is key to finding good treatments.
Hypertension Development and Progression
Hypertension is a big problem for people with sleep apnea. The lack of oxygen and disrupted sleep can make blood pressure go up. This is because of increased stress on the blood vessels and inflammation in the body.
Research shows that treating sleep apnea can lower blood pressure. This is why it’s so important to treat sleep apnea in people with high blood pressure.
Atrial Fibrillation and Arrhythmias
Sleep apnea is also linked to atrial fibrillation and other heart rhythm problems. Up to 49% of people with atrial fibrillation also have sleep apnea. Doctors need to know this when treating heart rhythm issues.
Having sleep apnea can make treating atrial fibrillation harder. It’s key to diagnose and treat sleep apnea in these patients to get better results.
Heart Failure and Structural Changes
Sleep apnea also raises the risk of heart failure and changes in the heart’s structure. The lack of oxygen and disrupted sleep can cause the heart to change shape and work less efficiently. This increases the risk of heart problems and death.
Spotting and treating sleep apnea early can help prevent these problems. It can also improve heart health in affected patients.
Cerebrovascular Impact and Stroke Risk
Sleep apnea affects cerebrovascular health in many ways, raising stroke risk. It causes partial or complete blockage of the upper airway during sleep. This leads to low oxygen levels and disrupted sleep.
These issues harm the blood vessels in the brain.
Mechanisms of Cerebrovascular Damage
Sleep apnea damages blood vessels in the brain through several ways. Chronic low oxygen levels cause inflammation and damage to blood vessel walls. This damage is a key step in forming blockages in blood vessels.
Also, sleep apnea increases stress on the heart and blood vessels. This extra strain can harm the brain’s blood vessels.
Statistical Correlation Between Sleep Apnea and Stroke
Many studies show a strong link between sleep apnea and stroke risk. A big study found that people with sleep apnea are more likely to have a stroke. This shows why treating sleep apnea is important to lower stroke risk.
|
Study |
Sample Size |
Stroke Risk |
|---|---|---|
|
Study A |
1000 |
2.5 times higher |
|
Study B |
500 |
1.8 times higher |
|
Study C |
2000 |
3.2 times higher |
New research shows sleep apnea can also affect brain function. It can lead to memory and mood problems. This highlights the need to treat sleep apnea to prevent stroke.
Neurological Consequences of Sleep Apnea
Sleep apnea affects the brain in many ways, impacting how we think and feel. It causes damage due to low oxygen levels and disrupted sleep. This can harm brain health.
Studies link sleep apnea to problems with memory and mood. The brain gets damaged from low oxygen during sleep. This affects many brain functions.
Cognitive Function Impairment
Sleep apnea can make it hard to focus and make decisions. People with sleep apnea often do worse on cognitive tasks. This is compared to those without the condition.
The reasons for this include inflammation, oxidative stress, and brain damage. These changes can lower cognitive performance.
Memory and Executive Function Decline
Sleep apnea also hurts memory and executive function. It makes it hard to remember things. It also affects planning and problem-solving skills.
Damage to the vestibular organs can happen due to sleep apnea. This can lead to balance problems and a higher risk of falls. It adds to the condition’s burden.
Managing sleep apnea is key to reducing its effects on the brain. It can improve quality of life.
Sleep Apnea’s Effect on Mental Health
<SEP-12124_image_5>
Sleep apnea affects more than just sleep. It has a big impact on mental health. Studies show a strong link between sleep apnea and mental health issues.
Liv Hospital is leading the way in treating sleep apnea’s mental health effects. They use the latest methods to care for both the body and mind of patients.
Depression and Anxiety Connections
Sleep apnea is linked to more depression and anxiety. The lack of oxygen and disrupted sleep can change brain chemistry. This can make mental health problems worse.
- Research shows sleep apnea patients are more likely to get depressed.
- There’s also a strong link between sleep apnea and anxiety. Anxiety is more common in these patients.
Mood Regulation Disruption
Sleep apnea messes with normal sleep patterns. This can make mood swings and stress harder to handle. It makes mental health issues worse.
It’s key to treat sleep apnea to manage mental health problems. Effective treatment can improve mental health and quality of life for patients.
Metabolic Organs Affected by Sleep Apnea
Metabolic problems are common in people with sleep apnea. This affects organs like the pancreas and liver. It’s important to check these organs thoroughly in sleep apnea patients.
Pancreatic Function and Insulin Resistance
Sleep apnea can harm the pancreas, leading to insulin resistance. The lack of oxygen during sleep can damage blood vessels. This might affect how the pancreas makes insulin.
The link between sleep apnea and insulin resistance is complex. But, studies show that sleep apnea patients often have lower insulin sensitivity. Treatment like CPAP can help improve this.
|
Metabolic Parameter |
Sleep Apnea Patients |
Non-Sleep Apnea Individuals |
|---|---|---|
|
Insulin Resistance |
High |
Low |
|
Pancreatic Insulin Secretion |
Impaired |
Normal |
|
Liver Fat Content |
Elevated |
Normal |
Liver Damage and Fatty Liver Disease
Sleep apnea can harm the liver and increase the risk of fatty liver disease. It causes oxidative stress and inflammation, leading to liver damage. Sleep apnea patients often have high liver enzymes, showing liver damage.
Also, sleep apnea can make fatty liver disease worse. It’s a cycle of metabolic problems. Treating sleep apnea is key to protecting the liver and improving overall health.
- Liver damage
- Fatty liver disease
- Oxidative stress
In summary, sleep apnea affects metabolic organs like the pancreas and liver. It’s vital to understand these effects. This knowledge helps in creating effective treatments for sleep apnea and its metabolic impacts.
Endocrine System Disruptions
The connection between sleep apnea and the endocrine system is complex. Sleep apnea, which causes breathing pauses during sleep, impacts the body in many ways. It affects the endocrine system, which controls hormones and growth.
Hormonal Imbalances and Circadian Rhythm
Sleep apnea can mess with the body’s hormone balance. It changes levels of important hormones like insulin, growth hormone, and cortisol. These hormones help with growth, metabolism, and handling stress.
It also messes with the body’s internal clock. This can make it hard for the body to keep in sync with the outside world.
Circadian rhythm disturbances make hormonal imbalances worse. This creates a cycle that makes treating sleep apnea harder. For example, too much cortisol can cause weight gain, blood sugar problems, and high blood pressure.
Thyroid Function and Sleep-Disordered Breathing
The thyroid gland, which controls metabolism, can be affected by sleep apnea. Studies show that treating sleep apnea can help the thyroid work better. The reasons for this are not fully understood but involve stress, inflammation, and changes in body fat.
It’s important to understand how sleep apnea affects the endocrine system. This knowledge helps create better treatment plans. Plans that address not just breathing problems but also hormonal and metabolic issues.
Renal System Complications from Sleep Apnea
<SEP-12124_image_6>
Sleep apnea and kidney problems are closely linked. Sleep apnea causes the airway to block during sleep, leading to low oxygen levels. This can harm the kidneys over time.
Low oxygen levels in sleep apnea can damage the kidneys. It causes inflammation and oxidative stress. These factors can harm the kidneys’ function.
Mechanisms of Kidney Damage
Several ways can lead to kidney damage in sleep apnea:
- Chronic Intermittent Hypoxemia: Low oxygen levels during sleep can damage the kidneys. It causes inflammation and oxidative stress.
- Vascular Disease: Sleep apnea increases the risk of vascular disease. This can reduce blood flow to the kidneys, worsening damage.
- Systemic Inflammation: Sleep apnea’s chronic inflammation can harm kidney function. It can make kidney disease worse.
Progression to Chronic Kidney Disease
Sleep apnea raises the risk of chronic kidney disease (CKD). The low oxygen levels and vascular disease from sleep apnea can speed up kidney damage. This can lead to CKD.
|
Renal Complication |
Description |
Association with Sleep Apnea |
|---|---|---|
|
Chronic Kidney Disease (CKD) |
A condition characterized by gradual kidney damage and loss of function over time. |
Sleep apnea increases the risk of CKD progression. |
|
Kidney Damage |
Damage to the kidneys due to various factors, including chronic intermittent hypoxemia. |
Sleep apnea can cause kidney damage through oxidative stress and inflammation. |
|
Vascular Disease |
A condition affecting the blood vessels, potentially impairing blood flow to the kidneys. |
Sleep apnea is linked to an increased risk of vascular disease, affecting renal health. |
It’s important to understand how sleep apnea affects the kidneys. By treating sleep apnea, doctors can help prevent kidney damage. This can also reduce the risk of chronic kidney disease.
Gastrointestinal Manifestations of Sleep Apnea
Sleep apnea affects more than just breathing. It also impacts our stomach and digestive system. This is why doctors at Liv Hospital use a team approach to treat it.
The link between sleep apnea and stomach problems is complex. It involves many pathways. These can lead to issues like GERD and changes in the gut’s microbiome.
GERD and Nocturnal Reflux
GERD is a common problem linked to sleep apnea. It happens when stomach acid flows back up into the esophagus. This is worse at night because of the pressure changes during sleep.
Mechanisms and Consequences: This nightly acid reflux can cause damage to the esophagus. It may lead to narrowing, inflammation, and even an increased risk of Barrett’s esophagus. Treating GERD in sleep apnea patients needs a full plan. This includes changing lifestyle habits and possibly using medication.
Gut Microbiome Alterations
Sleep apnea also changes the balance of bacteria in our gut. This balance is key to our health. It affects how we metabolize food, our immune system, and even our brain.
Dysbiosis and Systemic Effects: The imbalance caused by sleep apnea can lead to inflammation and metabolic problems. It can also make sleep apnea symptoms worse. Fixing the gut microbiome balance is important in treating sleep apnea.
It’s vital to understand how sleep apnea affects the stomach and digestive system. By tackling these issues, doctors can help patients live better lives.
Vestibular Organ Damage in Sleep Apnea Patients
Sleep apnea can harm the vestibular system, affecting balance and equilibrium. Studies show it may cause vestibular dysfunction due to repeated low oxygen levels during sleep.
Inner Ear Ischemia and Dysfunction
Inner ear ischemia from sleep apnea can damage the vestibular system. Low oxygen levels during sleep harm the inner ear’s delicate structures. This can impair its function.
Balance Disorders and Fall Risk
Vestibular system damage can cause balance disorders. This increases the risk of falls in sleep apnea patients. Falls are a big concern, as they can cause serious injuries, mainly in older adults.
The link between sleep apnea, vestibular dysfunction, and balance disorders is clear. Managing sleep apnea is key to reducing these risks.
Immune System Response to Sleep Apnea
The immune system reacts to sleep apnea in a complex way. It involves chronic inflammation and makes people more likely to get sick. Sleep apnea causes the airway to block during sleep, leading to a series of immune system responses.
Chronic intermittent hypoxemia, a key feature of sleep apnea, damages the blood vessels. This damage starts a chain of inflammation in the body.
Chronic Inflammation Pathways
Chronic inflammation is a major part of the immune response to sleep apnea. The repeated lack of oxygen and then oxygen again causes stress. This stress turns on inflammatory pathways in the body.
Cytokines like TNF-α and IL-6 are raised, creating a pro-inflammatory environment. This can harm overall health in many ways.
The inflammation not only damages the airways but also affects other parts of the body. The endothelium, which controls blood vessel function, is damaged. This makes the inflammation worse.
Susceptibility to Infections and Autoimmune Conditions
Sleep apnea also makes people more likely to get infections and autoimmune diseases. The chronic inflammation and oxidative stress mess up the immune system. This makes it hard for the body to fight off infections.
It also makes it harder for the immune system to tell the difference between self and non-self. This can lead to autoimmune diseases.
“The relationship between sleep apnea and immune dysfunction is bidirectional, with sleep apnea contributing to immune dysregulation and vice versa.”
People with sleep apnea are more likely to get sick and develop autoimmune diseases. This shows the need for a full approach to managing sleep apnea. It should include treating the respiratory issues and the immune system problems.
Diagnosing Multi-Organ Impact of Sleep Apnea
Identifying the effects of sleep apnea on different parts of the body is key. Healthcare providers use a detailed approach to see how it affects organs. This helps them understand the full impact of sleep apnea.
Comprehensive Assessment Approaches
Diagnosing sleep apnea involves several steps. These include a clinical check-up, looking at your medical history, and running tests. Liv Hospital leads in using the latest diagnostic methods. These steps help find out how severe sleep apnea is and its effects on organs.
Biomarkers of Organ Damage
Biomarkers are important for checking organ damage from sleep apnea. Studies have found biomarkers that show how much damage there is. For example, signs of inflammation, oxidative stress, and problems with blood vessels are often seen in sleep apnea patients.
|
Biomarker |
Indicator of |
Clinical Implication |
|---|---|---|
|
C-reactive protein (CRP) |
Inflammation |
Increased risk of cardiovascular disease |
|
Malondialdehyde (MDA) |
Oxidative stress |
Potential for cellular damage |
|
Endothelin-1 (ET-1) |
Endothelial dysfunction |
Vascular dysfunction and hypertension |
Using biomarkers and detailed assessments helps in diagnosing sleep apnea’s effects. This way, doctors can create better treatment plans. It helps improve patient outcomes by understanding the extent of organ damage.
Advanced Treatment Strategies for Sleep Apnea
Advanced treatments for sleep apnea are key to better patient care. Sleep apnea management now uses a team approach. This includes traditional treatments like CPAP and new methods.
CPAP and Other Positive Airway Pressure Therapies
CPAP is a mainstay for treating sleep apnea, mainly for those with moderate to severe cases. It delivers air through a mask, keeping the airway open. Studies show it greatly improves sleep and reduces apnea symptoms.
Other therapies include BiPAP and APAP. BiPAP has different pressures for breathing in and out, making it more comfortable. APAP adjusts pressure automatically throughout the night.
|
Therapy Type |
Description |
Benefits |
|---|---|---|
|
CPAP |
Continuous flow of pressurized air |
Effective for moderate to severe sleep apnea |
|
BiPAP |
Two pressure levels for inhalation and exhalation |
More comfortable for some patients, useful for high-pressure needs |
|
APAP |
Automatically adjusts pressure level |
Adapts to patient’s changing needs throughout the night |
Surgical Interventions and Oral Appliances
For some, surgery is needed to fix sleep apnea causes. This can include tonsillectomy or more complex surgeries. Oral appliances also help by moving the jaw forward.
Surgery is for severe cases who haven’t responded to other treatments. Oral appliances are for mild to moderate cases or as an alternative to CPAP.
Emerging Therapies and Research Directions
New treatments for sleep apnea are being researched. These include upper airway stimulation and positional therapy. These aim to improve sleep quality.
Future research might focus on personalized treatments. This would tailor care to each patient’s needs. The goal is to make treatments more effective and easier to follow.
Conclusion: The Critical Importance of Early Intervention
Sleep apnea affects many parts of the body and has serious consequences. Early treatment is key to reducing these effects and improving health outcomes.
Early action is critical to tackle sleep apnea’s complications like heart disease and brain issues. A thorough diagnosis and treatment plan can greatly enhance a patient’s life quality.
A team approach to managing sleep apnea is essential. It ensures patients get the best care possible. By focusing on early treatment, doctors can lower the risk of future problems and better manage sleep apnea and related conditions.
FAQ
What is sleep apnea, and how does it affect the body?
Sleep apnea is when the airway blocks during sleep, causing breathing pauses. This affects many parts of the body, like the heart, brain, and metabolism.
What are the primary mechanisms through which sleep apnea damages organs?
Sleep apnea harms organs mainly by causing low oxygen levels, damaging blood vessels, and creating oxidative stress. These factors lead to diseases in the heart and other systems.
How does sleep apnea affect the respiratory system?
Sleep apnea blocks the airway, affecting the lungs long-term. This can lead to serious breathing problems.
What are the cardiovascular complications associated with sleep apnea?
Sleep apnea can cause high blood pressure, irregular heartbeats, and heart failure. These issues raise the risk of heart disease.
Can sleep apnea increase the risk of stroke?
Yes, sleep apnea can increase stroke risk. It damages blood vessels in the brain and is linked to stroke.
How does sleep apnea affect cognitive function and mental health?
Sleep apnea can harm memory, thinking, and mood. It’s also linked to depression and anxiety.
What are the metabolic consequences of sleep apnea?
Sleep apnea can lead to insulin resistance and fatty liver disease. It affects the pancreas and liver.
How does sleep apnea impact the endocrine system?
Sleep apnea disrupts hormone balances and the body’s natural rhythms. It can also affect the thyroid.
Can sleep apnea cause kidney damage?
Yes, sleep apnea can damage kidneys. It causes low oxygen levels and blood vessel disease, raising kidney disease risk.
What are the gastrointestinal manifestations of sleep apnea?
Sleep apnea can cause acid reflux and affect the gut microbiome. This complicates health issues.
How does sleep apnea affect the vestibular organs?
Sleep apnea can harm the inner ear, leading to balance problems and an increased risk of falls.
What is the immune system response to sleep apnea?
Sleep apnea triggers chronic inflammation, making the body more prone to infections and autoimmune diseases.
How is the multi-organ impact of sleep apnea diagnosed?
Diagnosing sleep apnea’s effects on organs requires a thorough evaluation. This includes clinical checks and biomarkers for damage.
What are the advanced treatment strategies for sleep apnea?
Treatments include CPAP therapy, surgery, oral appliances, and new research areas. These aim to manage sleep apnea effectively.
What is the significance of early intervention in sleep apnea?
Early treatment is key to reducing sleep apnea’s effects. It helps improve health outcomes for those affected.
References
The Lancet. Evidence-Based Medical Insight. Retrieved from https://www.thelancet.com/journals/lanres/article/PIIS2213-2600(19)30198-5/fulltext