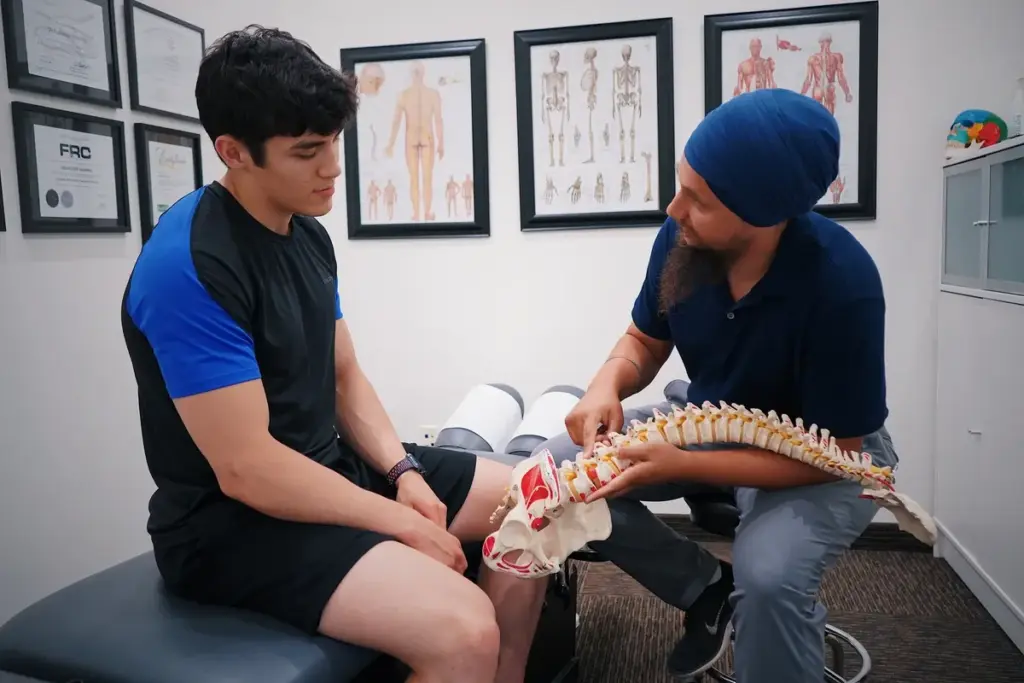
Minimally invasive surgery is a modern way to treat spinal stenosis. It helps reduce pain and discomfort. This method causes less damage and leads to quicker recovery times than old-school surgeries.
Spinal stenosis narrows the spinal canal, putting pressure on nerves. This can cause back and leg pain, numbness, and weakness. Minimally invasive surgery is a hopeful option for those dealing with this issue.
Key Takeaways
- Minimally invasive surgery is a less damaging alternative to traditional spinal stenosis treatment.
- This surgical approach can help alleviate pain and discomfort associated with spinal stenosis.
- Faster recovery times are a significant benefit of minimally invasive surgery.
- Spinal stenosis is a condition that can cause significant pain and discomfort.
- Minimally invasive surgery offers a promising solution for patients with spinal stenosis.
Understanding Spinal Stenosis
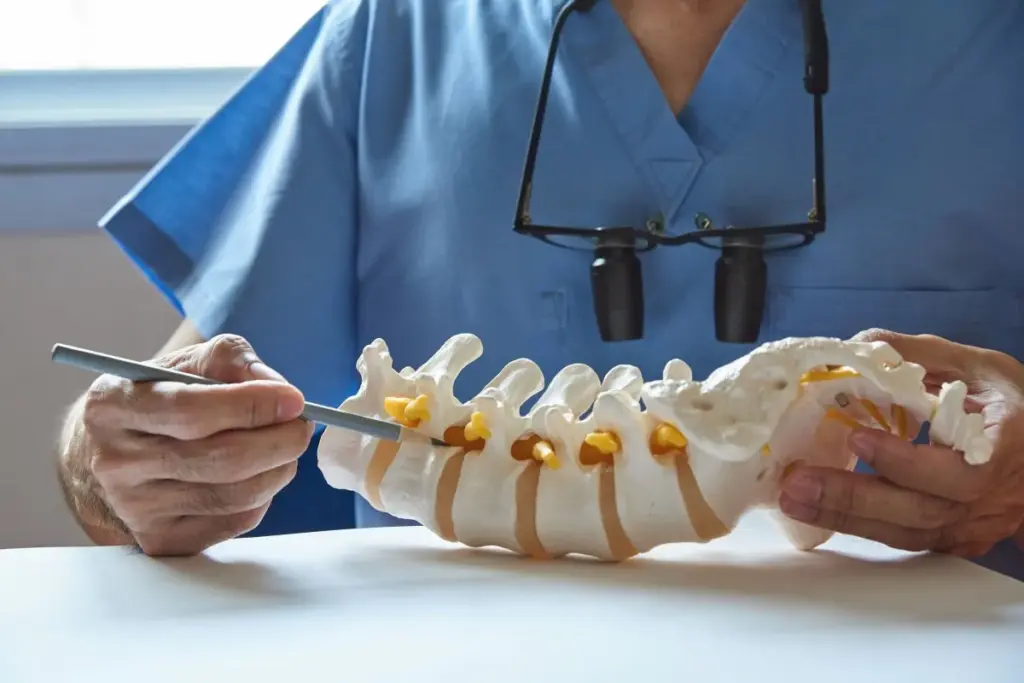
Spinal stenosis is when the spinal canal gets smaller. This puts pressure on the spinal cord and nerves. This can cause many symptoms, making life harder for those who have it.
Definition and Causes
Spinal stenosis happens when the space in the spinal canal shrinks. This can be due to wear and tear, birth defects, or injuries. Degenerative changes are the main reason, from the wear and tear on the spine over time.
The narrowing can happen anywhere in the spine. But it’s most common in the lumbar (lower back) and cervical (neck) areas. Knowing the causes helps find the right treatment. This might include spinal surgery or other spinal operations.
Symptoms and Progression
The symptoms of spinal stenosis vary from person to person. They depend on where and how much the narrowing is. Common symptoms are pain, numbness, tingling, and weakness in the back, legs, or arms. In severe cases, it can make daily activities very hard.
|
Symptom |
Description |
Progression |
|---|---|---|
|
Pain |
Often starts as mild and increases over time |
Can become chronic and debilitating |
|
Numbness/Tingling |
Typically affects the extremities |
May worsen with activity |
|
Weakness |
Can affect mobility and strength |
May lead to significant disability |
It’s important to understand how spinal stenosis gets worse. Some people’s condition gets worse slowly, while others’ gets worse fast. Before thinking about spinal surgery or other spinal operations, doctors usually try other treatments first.
Diagnosing Spinal Stenosis
To find out if you have spinal stenosis, doctors use a few methods. They do physical checks and use advanced imaging tests. This helps them understand how bad the condition is and what treatment you need.
Physical Examination
The first thing doctors do is a physical check-up. They look at your muscle strength, reflexes, and flexibility. They also check for numbness or tingling in your arms and legs.
Imaging Tests
Imaging tests are key to confirming spinal stenosis. The main tests are:
- Magnetic Resonance Imaging (MRI): MRI shows detailed pictures of the spinal cord and nerves.
- Computed Tomography (CT) scans: CT scans give clear views of the spinal canal and can spot bone spurs.
- X-rays: X-rays help see the spine’s alignment and any wear and tear.
The doctor picks the best test based on your symptoms and what they think might be causing your spinal stenosis.
Neurological Assessments
Neurological tests are important to see how spinal stenosis affects your nervous system. These tests check nerve function, like electromyography (EMG) and nerve conduction studies (NCS).
|
Diagnostic Method |
Purpose |
Key Findings |
|---|---|---|
|
Physical Examination |
Assess muscle strength, reflexes, and flexibility |
Identify limitations in mobility and pain triggers |
|
MRI |
Detailed imaging of spinal cord and nerves |
Reveals nerve compression and structural abnormalities |
|
Neurological Assessments |
Evaluate nerve function |
Identifies nerve damage or compression |
Doctors use the results from physical exams, imaging tests, and neurological tests to accurately diagnose spinal stenosis. This helps them create a treatment plan that might include spine surgery and other treatments.
Conservative Treatment Options
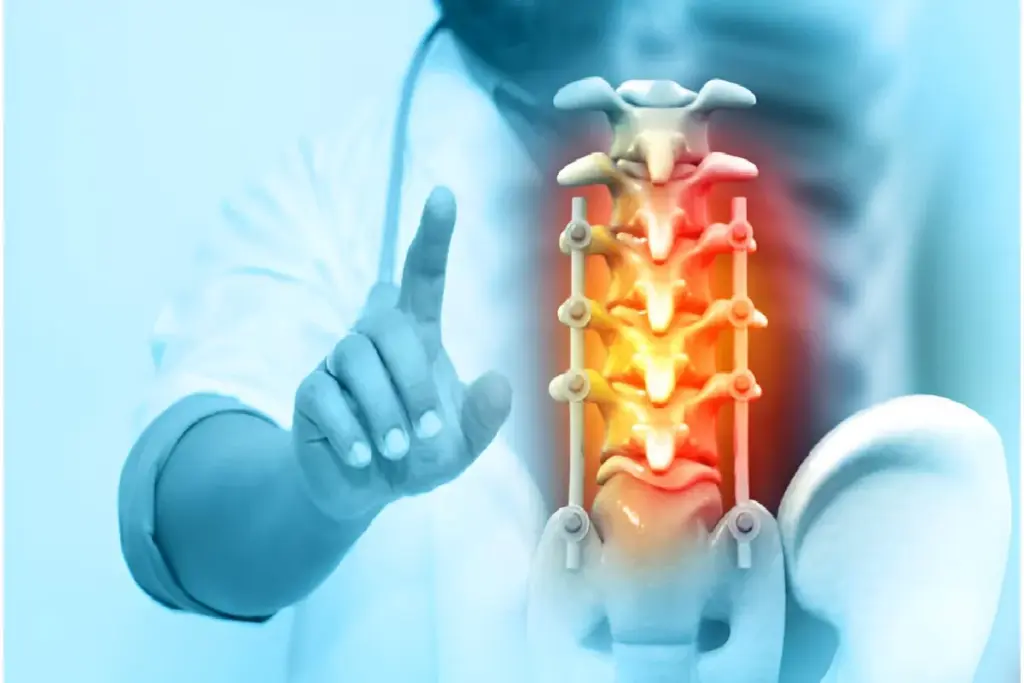
Many patients find relief in conservative treatments for spinal stenosis. These methods help manage pain, reduce swelling, and boost quality of life.
Medications
Medicines are key in treating spinal stenosis symptoms. Doctors often prescribe pain relievers, anti-inflammatory drugs, and muscle relaxants.
These medications can greatly enhance a patient’s life. They help reduce pain and make daily tasks easier.
Physical Therapy
Physical therapy is a vital part of conservative treatment. It’s designed to improve mobility, strengthen back muscles, and increase flexibility.
It’s great for reducing pain and boosting functional ability.
Steroid Injections
Steroid injections help cut down inflammation and pain. They offer significant relief, allowing patients to engage more in physical therapy and daily activities.
|
Treatment Option |
Primary Benefit |
Potential Drawbacks |
|---|---|---|
|
Medications |
Effective pain management |
Potential side effects, dependency risk |
|
Physical Therapy |
Improves mobility and strength |
Requires commitment to a therapy regimen |
|
Steroid Injections |
Significant pain relief |
Limited frequency of injections, possible side effects |
When Surgery Becomes Necessary
When other treatments don’t work, and life quality drops, surgery is considered. This is for minimally invasive spinal decompression surgery.
Choosing surgery for spinal stenosis is a big decision. It’s usually suggested when other treatments don’t help or symptoms get worse.
Failed Conservative Treatment
If treatments like meds, physical therapy, and steroid shots don’t help, surgery might be needed. Failed conservative treatment means ongoing pain, numbness, or weakness that hinders daily life.
Progressive Neurological Symptoms
Signs like growing numbness, weakness, or bladder issues are serious. Prompt surgical intervention can stop further damage.
Quality of Life Considerations
How spinal stenosis affects daily life is key in deciding on surgery. If symptoms greatly impact daily activities, mobility, or simple tasks, surgery is considered.
The choice to have minimally invasive spinal decompression surgery is made with a healthcare provider. It’s based on the person’s health, condition severity, and personal wishes.
Traditional Open Spine Surgery vs. Minimally Invasive Approaches
Minimally invasive surgery is now a good option instead of traditional open spine surgery for spinal stenosis. This section will look at the differences between these two methods. We’ll focus on their techniques, benefits, and how well patients recover.
Open Surgery Techniques
Traditional open spine surgery needs a big cut to see the spine. Surgeons can then directly work on the problem area. This method is used for complex cases or when spinal fusion is needed.
Key aspects of open surgery include:
- Larger incision to access the spine
- More tissue disruption and muscle detachment
- Direct visualization of the surgical site
- Potential for longer hospital stays and recovery times
Minimally Invasive Advantages
Minimally invasive surgery has many benefits. It uses smaller cuts, causes less damage, and helps patients recover faster. This is because special tools and techniques let surgeons work through small openings.
The advantages of minimally invasive surgery include:
- Smaller incisions, resulting in less scarring
- Reduced muscle damage and trauma
- Less post-operative pain
- Faster recovery and return to normal activities
Comparing Recovery Times and Outcomes
Recovery times and results differ a lot between open spine surgery and minimally invasive methods. Knowing these differences is key for patients and doctors when choosing the best surgery.
|
Criteria |
Traditional Open Spine Surgery |
Minimally Invasive Surgery |
|---|---|---|
|
Incision Size |
Larger (often 5-10 cm or more) |
Smaller (typically 1-2 cm) |
|
Recovery Time |
Generally longer (often 6-12 weeks or more) |
Typically shorter (often 2-6 weeks) |
|
Pain and Discomfort |
More post-operative pain |
Less post-operative pain |
|
Hospital Stay |
Often requires longer hospital stay |
Usually allows for shorter or outpatient procedures |
By looking at these points, patients can understand the choices they have for treating spinal stenosis.
Types of Minimally Invasive Procedures for Spinal Stenosis
Spinal stenosis is a condition where the spinal canal narrows. Now, there are many minimally invasive treatments for it. These treatments help ease the pressure on the spinal cord and nerves, giving relief to those affected.
Laminectomy and Laminotomy
Laminectomy and laminotomy are two main treatments for spinal stenosis. A laminectomy removes part or all of the lamina to relieve pressure. Laminotomy makes a smaller cut in the lamina to achieve the same goal. Both methods are good at opening up the spinal canal.
Foraminotomy
Foraminotomy is another treatment for spinal stenosis. It widens the foramina, the nerve exits, to ease nerve pressure. This is great for those with foraminal stenosis.
Interspinous Process Devices
Interspinous process devices are placed between vertebrae to keep them apart. This reduces pressure on the spinal cord and nerves. They are a less invasive option compared to traditional spinal fusion surgery.
Endoscopic Decompression
Endoscopic decompression is a modern, minimally invasive method. It uses an endoscope to see the spine during surgery. This allows for precise decompression with little tissue damage.
|
Procedure |
Description |
Benefits |
|---|---|---|
|
Laminectomy |
Removal of part or all of the lamina |
Relieves pressure on the spinal cord |
|
Laminotomy |
Smaller incision in the lamina |
Less invasive, preserves more bone structure |
|
Foraminotomy |
Widening of the foramina |
Relieves pressure on nerves exiting the spinal canal |
|
Interspinous Process Devices |
Implantation between spinous processes |
Maintains spacing, reduces pressure on spinal cord and nerves |
|
Endoscopic Decompression |
Utilizes an endoscope for precise decompression |
Minimal tissue damage, precise decompression |
Spinal Fusion Surgery: Minimally Invasive Techniques
Spinal fusion surgery can be done in a way that’s less invasive. This method helps avoid big risks and speeds up healing. It joins two or more vertebrae together to stabilize the spine. This helps relieve pain and improve function.
When Is Spinal Fusion Necessary
Spinal fusion is needed when other treatments don’t work. It’s also necessary when the spine becomes unstable or causes neurological symptoms. Doctors decide on surgery after checking with imaging tests and neurological exams.
Indications for Spinal Fusion:
- Severe spinal instability
- Significant deformity
- Failed conservative treatment
- Progressive neurological symptoms
Minimally Invasive Fusion Procedures
Minimally invasive spinal fusion uses new tech to reduce damage and speed up recovery. It involves smaller cuts, special tools, and bone grafts to help the spine fuse.
Key aspects of minimally invasive fusion include:
- Smaller incisions, reducing tissue trauma
- Less blood loss during surgery
- Shorter hospital stays and recovery times
Instrumentation and Materials Used
The tools and materials used in spinal fusion are key to its success. These include implants, bone grafts, and devices to support the spine while it heals.
|
Material/Type |
Description |
Use in Spinal Fusion |
|---|---|---|
|
Pedicle Screws |
Screws inserted into the vertebrae to stabilize the spine |
Provides immediate stability |
|
Bone Grafts |
Autografts (from the patient) or allografts (donor bone) |
Facilitates bone fusion |
|
Rods and Plates |
Metal devices used to stabilize the spine |
Supports the spine during healing |
Common Back Surgery Types for Spinal Stenosis
There are different surgeries for spinal stenosis, depending on how bad it is and where it is. It can happen in the neck, middle back, or lower back. Each area needs a special kind of surgery.
Cervical Procedures
Cervical spinal stenosis is in the neck and can hurt the spinal cord. This can cause serious problems. The surgeries for this include:
- Anterior cervical discectomy and fusion (ACDF)
- Cervical laminectomy
- Laminotomy
These surgeries try to take pressure off the spinal cord and nerves. ACDF removes a bad disc and fuses the vertebrae together to keep the spine stable.
Thoracic Approaches
Thoracic spinal stenosis is less common but harder to fix because of the spine’s shape and the rib cage. The surgeries might be:
- Thoracic laminectomy
- Costotransversectomy
- Thoracoscopic surgery
These surgeries need careful planning because of the complex anatomy of the thoracic spine.
Lumbar Surgeries
Lumbar spinal stenosis is the most common and affects the lower back. The surgeries for this include:
- Lumbar laminectomy
- Laminotomy
- Microdiscectomy
- Spinal fusion
Lumbar surgeries aim to take pressure off nerves and help you move better. Lumbar laminectomy is often used to remove part of a vertebra to make more space.
Here’s a comparison of the different surgical procedures for spinal stenosis:
|
Region |
Common Procedures |
Goals |
|---|---|---|
|
Cervical |
ACDF, Laminectomy, Laminotomy |
Relieve pressure on spinal cord and nerves |
|
Thoracic |
Laminectomy, Costotransversectomy, Thoracoscopic surgery |
Decompress spinal cord, stabilize spine |
|
Lumbar |
Laminectomy, Laminotomy, Microdiscectomy, Spinal fusion |
Relieve nerve pressure, improve mobility |
The right surgery depends on the patient’s health, how bad the spinal stenosis is, and where it is. Knowing these options helps make better treatment choices.
Advanced Technologies in Minimally Invasive Spine Surgery
The field of minimally invasive spine surgery has seen big changes with new technologies. These advancements make surgeries more precise, safe, and effective. This leads to better results for patients.
Endoscopic Techniques
Endoscopic techniques in spinal surgery use small endoscopes to see the surgery area. This method causes less damage to tissues. It also cuts down on pain and recovery time after surgery.
One common use is in treating spinal stenosis. Here, the surgeon removes parts that press on nerves. This relieves the pressure.
Robot-Assisted Surgery
Robot-assisted surgery is changing minimally invasive spine surgery a lot. It gives surgeons better views, precision, and control. Robots help with complex surgeries, making them safer.
Robotic systems are great for surgeries that need exact tools and stability.
Navigation and Imaging Systems
Advanced navigation and imaging systems are key in minimally invasive spine surgery. They give surgeons real-time feedback and views. These systems help find and work around spinal structures accurately.
They also make sure implants are placed right. This makes spinal surgeries safer and more effective.
The use of these advanced technologies in minimally invasive spine surgery is changing how we treat spinal problems. As these technologies get better, they will help even more. They will make surgeries better, shorter, and improve care for patients.
Preparing for Minimally Invasive Spinal Surgery
Getting ready for minimally invasive spinal surgery is key. This includes medical checks and lifestyle changes. These steps help the surgery go well and make recovery easier.
Medical Evaluation
A detailed medical check is vital before minimally invasive spinal surgery. Your doctor will look at your health history, medicines, and any health issues. They might also do tests like blood work or imaging to see if you’re a good fit for the surgery.
Talking to your healthcare team is important. You can ask questions and learn about the surgery’s risks and benefits. This includes understanding your decompression operation spine.
Lifestyle Adjustments
Changing your lifestyle can help a lot. Quitting smoking is a big plus, as it helps healing and lowers risks. Eating well and exercising can also make you healthier and reduce surgery risks.
Your doctor might tell you to stop some medicines before surgery. It’s important to listen to these instructions to stay safe.
What to Expect on Surgery Day
Knowing what to expect on surgery day can make you feel better. You’ll likely arrive at the hospital a few hours early. You’ll meet your surgical team, who will help you get ready for the surgery.
On surgery day, you’ll have the minimally invasive spinal surgery. This method is less invasive than traditional surgery. It uses new technologies to cause less damage, reduce pain, and help you heal faster.
Recovery After Minimally Invasive Spinal Surgery
The journey to recovery after minimally invasive spinal surgery is detailed and requires careful planning. It’s all about following the post-operative instructions closely. This ensures patients get the best results from their spinal decompression surgery.
Hospital Stay and Immediate Post-Op Care
After minimally invasive spinal surgery, hospital stays are often shorter than with traditional surgery. Most patients leave the hospital in less than 24 hours. The focus during this time is on managing pain, watching for complications, and starting to move around.
- Pain management through medication
- Monitoring for signs of infection or neurological issues
- Gradual mobilization to prevent blood clots and promote healing
Physical Therapy and Rehabilitation
Physical therapy is key in the recovery journey. It helps patients regain strength, flexibility, and mobility. A personalized rehabilitation plan is created based on the patient’s back surgery types and health.
The rehabilitation process includes:
- Gentle exercises to improve flexibility and strength
- Posture correction and body mechanics education
- Progressive resistance training to enhance muscle support around the spine
Timeline for Return to Activities
The time it takes to get back to normal activities varies. It depends on the patient’s health, the surgery’s extent, and the minimally invasive techniques used. Generally, patients can expect the following recovery timeline:
|
Activity Level |
Expected Timeline |
|---|---|
|
Light activities (e.g., walking, light housekeeping) |
1-4 weeks |
|
Moderate activities (e.g., bending, lifting light objects) |
4-8 weeks |
|
Strenuous activities (e.g., heavy lifting, contact sports) |
8-12 weeks or more |
It’s important to follow post-operative instructions and attend follow-up appointments. This helps ensure a smooth and effective recovery after minimally invasive spinal surgery.
Choosing the Right Surgeon and Medical Center
Choosing the right surgeon and medical center is key for minimally invasive spinal surgery. It’s important to consider several factors for the best care.
Surgeon Qualifications and Experience
The surgeon’s qualifications and experience are critical. A skilled surgeon can lower risks and speed up recovery. Choose a board-certified surgeon with a strong track record.
Ask about the surgeon’s experience with your specific procedure. For example, if it’s spinal fusion, find out when is spinal fusion necessary and how they decide the best approach for you.
|
Surgeon Qualifications |
Description |
Importance |
|---|---|---|
|
Board Certification |
Certification by a recognized medical board |
High |
|
Experience in Minimally Invasive Surgery |
Number of years and cases performed |
High |
|
Specialization in Spinal Surgery |
Focus on spinal conditions and surgeries |
High |
Hospital Facilities and Technology
The quality of the hospital and technology used can affect your surgery’s success. Modern technology, like robotic-assisted systems, can improve precision. Make sure the medical center has the latest facilities and technology.
“The right equipment and facilities can make a significant difference in the success of your surgery and your recovery.” – Expert in Orthopedic Surgery
Questions to Ask Your Surgical Team
It’s important to ask your surgical team the right questions before surgery. Ask about their experience with your condition, the techniques they’ll use, and what to expect during recovery. Key questions include:
- What experience do you have with backbone surgery?
- What are the possible risks and complications of the surgery?
- How will pain be managed during and after the surgery?
- What is the expected recovery time, and what rehabilitation will be required?
By carefully choosing your surgeon and medical center, you can greatly improve your surgery’s success. Research, ask questions, and make sure you’re in good hands.
Conclusion
Minimally invasive surgery is a safe and effective way to treat spinal stenosis. It offers many benefits over traditional open spine surgery. By understanding the causes, symptoms, and diagnosis of spinal stenosis, patients can make informed decisions about their treatment.
Minimally invasive spinal stenosis surgery has changed the field of spine surgery. It allows for a faster recovery, less tissue damage, and fewer complications. There are different types of minimally invasive procedures, like laminectomy, foraminotomy, and endoscopic decompression, to choose from.
When thinking about spinal stenosis surgery, it’s important to pick a qualified surgeon and medical center. They should have experience with minimally invasive techniques. This ensures the best possible outcomes and a smooth recovery.
If you’re experiencing symptoms of spinal stenosis, getting medical help is key. Thanks to advancements in minimally invasive surgery, there’s hope for those suffering. Talk to a healthcare professional to find the best treatment for your needs.
FAQ
What is spinal stenosis, and how is it diagnosed?
Spinal stenosis is when the spinal canal narrows. This can put pressure on the spinal cord and nerves. Doctors use physical exams, MRI or CT scans, and neurological tests to diagnose it.
What are the conservative treatment options for spinal stenosis?
Treatments include pain and inflammation medicines, physical therapy, and steroid injections. These help reduce swelling and relieve nerve pressure.
When is surgery necessary for spinal stenosis?
Surgery is needed when other treatments don’t work or symptoms get worse. It also depends on how much the condition affects your life.
What is the difference between traditional open spine surgery and minimally invasive approaches?
Open spine surgery uses a big incision and more tissue damage. Minimally invasive surgery uses small cuts and less damage. It often means less pain, shorter stays, and quicker recovery.
What are the different types of minimally invasive procedures available for spinal stenosis?
Procedures include laminectomy, foraminotomy, and endoscopic decompression. They aim to ease pressure on the spinal cord and nerves.
What is spinal fusion surgery, and when is it necessary?
Spinal fusion fuses vertebrae together to stabilize the spine. It’s needed for instability or deformity, or when other treatments don’t work.
What are the benefits of using advanced technologies in minimally invasive spine surgery?
Technologies like endoscopic techniques and robot-assisted surgery improve accuracy and safety. They lead to better results and faster recovery.
How do I prepare for minimally invasive spinal surgery?
You’ll need a medical check-up, quit smoking, and understand what to expect. This includes the surgery and post-care.
What is the recovery process like after minimally invasive spinal surgery?
Recovery includes a short hospital stay and physical therapy. You can usually get back to normal in a few weeks. The exact time depends on the procedure and individual.
How do I choose the right surgeon and medical center for minimally invasive spinal surgery?
Look for a surgeon’s experience and the hospital’s facilities. Ask about the surgical team and their approach to care for the best outcome.
What are the common back surgery types for spinal stenosis?
Common surgeries include cervical, thoracic, and lumbar procedures. Each targets different spine areas.
What is decompression operation spine, and how is it performed?
Decompression surgery relieves spinal cord and nerve pressure. It can be done with endoscopic techniques to minimize tissue damage.
When is backbone surgery necessary, and what does it involve?
Surgery is needed when other treatments fail or symptoms worsen. It includes decompression and fusion to stabilize and relieve pressure.
























