
A ruptured eardrum is a serious condition. It happens when a tear or hole forms in the thin membrane between the outer ear and the middle ear. It needs immediate medical attention.
Is it burst? Stage 3 ear infection is a top critical sign. Learn if a rupture requires the ER or if it will heal on its own safely.
If you have a ruptured eardrum and a stage 3 ear infection, it’s a big deal. It can cause serious problems if not treated right away.
This article will cover symptoms, diagnosis, and treatment for a ruptured eardrum and severe ear infections. We’ll help you know when to get emergency care.
Key Takeaways
- A ruptured eardrum can lead to severe complications if not treated promptly.
- Understanding the symptoms is key to knowing how serious it is.
- Quick medical help is needed for the best treatment.
- Advanced ear infections can cause a ruptured eardrum.
- Emergency care is often needed for a ruptured eardrum.
Understanding Ear Anatomy and Function
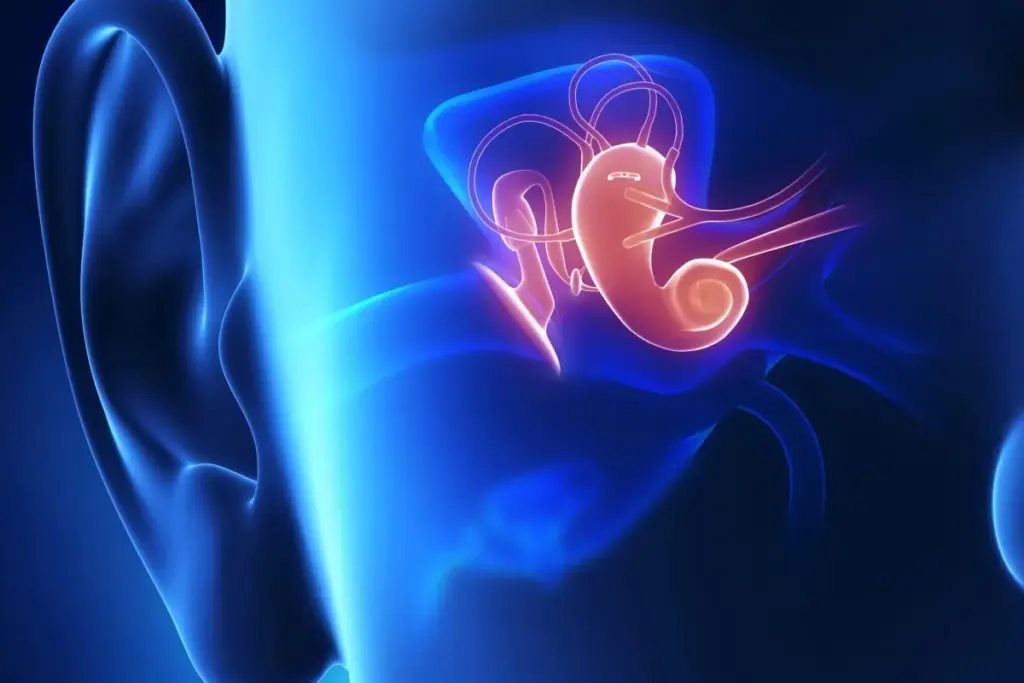
The human ear is a complex and fascinating organ. It plays a key role in our ability to hear and maintain balance. It is divided into three main parts: the outer ear, middle ear, and inner ear. Each part has distinct functions that work together to facilitate the hearing process.
The Structure of the Human Ear
The outer ear, or pinna, collects sound waves and directs them into the ear canal. The ear canal is lined with tiny hairs and glands that produce wax. This helps protect the eardrum by trapping dust and other foreign particles. The eardrum, or tympanic membrane, is a thin membrane that separates the outer ear canal from the middle ear.
The middle ear contains three small bones known as ossicles: the malleus, incus, and stapes. These bones transmit vibrations from the eardrum to the inner ear. The middle ear is also connected to the back of the throat by the Eustachian tube. This helps equalize pressure on both sides of the eardrum.
The inner ear is a complex structure that includes the cochlea and the vestibular system. The cochlea is responsible for converting sound vibrations into electrical signals that are sent to the brain. The vestibular system helps maintain balance and orientation.
How Sound Travels Through the Ear
Sound waves enter the ear through the outer ear and travel down the ear canal. This causes the eardrum to vibrate. These vibrations are then transmitted through the ossicles in the middle ear to the cochlea in the inner ear.
The cochlea converts these vibrations into electrical signals. These signals are interpreted by the brain as sound. This process is essential for our ability to hear and understand the world around us.
The Eardrum’s Role in Hearing
The eardrum plays a vital role in the hearing process. It acts as a barrier between the outer ear canal and the middle ear. When sound waves hit the eardrum, they cause it to vibrate. This initiates the process of sound transmission to the inner ear.
A healthy eardrum is essential for normal hearing. Damage to the eardrum, such as a rupture, can lead to hearing loss. It can also increase the risk of ear infections. Understanding the eardrum’s function and importance can help in appreciating the need for proper ear care and the prompt treatment of ear-related issues.
What Is a Ruptured Eardrum?
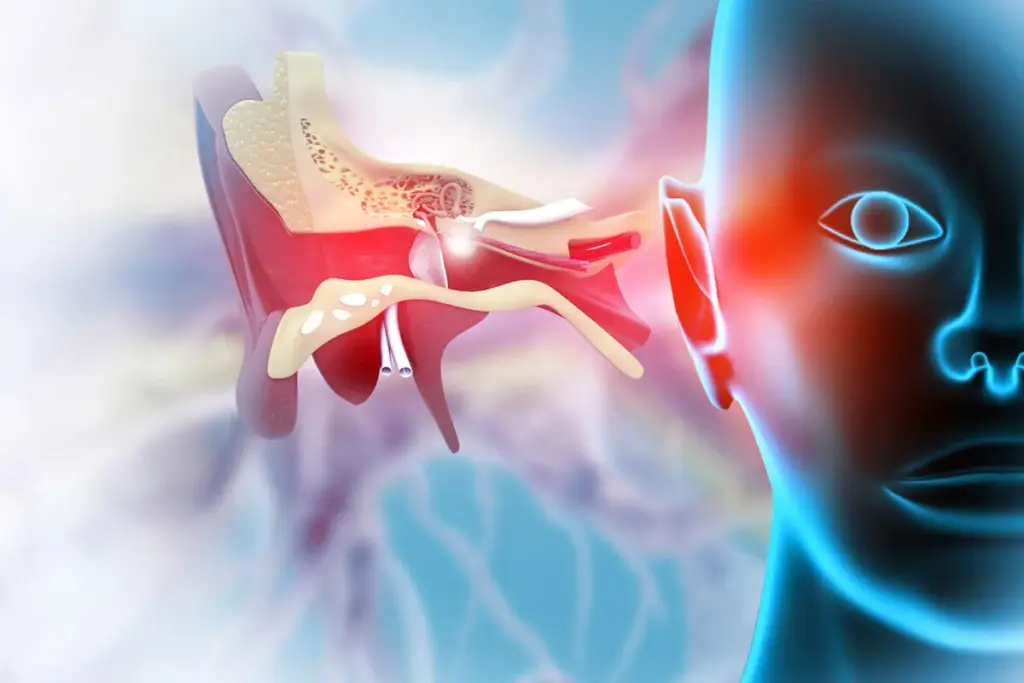
Knowing what a ruptured eardrum is can help you spot the signs and get help. A ruptured eardrum, or a perforated tympanic membrane, is when there’s a tear or hole in the eardrum.
Definition and Medical Terminology
The eardrum, or tympanic membrane, is a thin membrane. It separates the outer ear canal from the middle ear. When it’s whole, it helps us hear by vibrating with sound waves. A ruptured eardrum can mess with this, causing hearing problems and other issues.
The medical term for a ruptured eardrum is tympanic membrane perforation. This can happen from infections, injuries, or loud noises.
Common Causes of Eardrum Rupture
Many things can cause a ruptured eardrum. Medical sources say common causes include:
- Infections, like those that fill the middle ear with fluid or pus
- Trauma or injury to the ear, like from a slap or putting something in the ear canal
- Exposure to loud noises, like explosions or very loud music
- Pressure changes, such as during air travel or scuba diving
Risk Factors for Developing a Ruptured Eardrum
Some people are more likely to get a ruptured eardrum. These include:
|
Risk Factor |
Description |
|---|---|
|
History of Ear Infections |
Those with frequent ear infections are more at risk. |
|
Exposure to Loud Noises |
People often exposed to loud sounds are at higher risk. |
|
Inserting Objects into the Ear |
Using cotton swabs or other objects to clean the ear can push earwax deeper and potentially damage the eardrum. |
By knowing the causes and risk factors of a ruptured eardrum, you can prevent it and get medical help if you notice symptoms.
Stage3 Ear Infection: What You Need to Know
Stage 3 ear infections are serious and can lead to complications. It’s important to know how these infections progress and what symptoms to watch for. This knowledge helps in getting medical help quickly.
The Progression of Ear Infections
Ear infections start mild and can get worse. This happens if the infection isn’t fully treated or if the body can’t fight it off.
Factors Influencing Progression:
- Inadequate treatment
- Weakened immune system
- Recurring infections
Characteristics of Advanced Ear Infections
Stage 3 ear infections have more severe symptoms than earlier ones. Symptoms include more pain, fever, and sometimes discharge from the ear.
Common Characteristics:
- Increased severity of symptoms
- Potential for eardrum damage
- Risk of complications if left untreated
Relationship Between Severe Infections and Eardrum Rupture
Severe ear infections can cause eardrum rupture. The infection and pressure can make the eardrum perforate. This can lead to hearing loss and other problems.
|
Complication |
Description |
Potential Outcome |
|---|---|---|
|
Eardrum Rupture |
Perforation of the eardrum due to infection or pressure |
Hearing loss, infection spread |
|
Mastoiditis |
Infection of the mastoid bone |
Serious complications, including meningitis |
Knowing the risks of Stage 3 ear infections is key to effective treatment. Spotting the signs early and getting medical help can prevent serious problems.
Signs and Symptoms of a Ruptured Eardrum
It’s important to know the signs of a ruptured eardrum to avoid more problems. A ruptured eardrum, or perforated eardrum, shows symptoms that need quick medical check-up.
Common Symptoms to Watch For
The signs of a ruptured eardrum are clear. Look out for:
- Sudden sharp ear pain or discomfort that may be severe
- Fluid drainage from the ear, which may be bloody, clear, or pus-like
- Hearing loss or a feeling of fullness in the ear
- Tinnitus or ringing in the ear
- Vertigo or dizziness
Pain Levels and Characteristics
The pain from a ruptured eardrum can differ. Some feel a sharp pain, while others have a dull ache. The pain’s intensity depends on the perforation’s size and location.
Hearing Changes and Other Sensory Effects
A ruptured eardrum can change how you hear. Some might have temporary hearing loss, while others face ongoing issues. It can also affect balance, causing vertigo or dizziness.
|
Symptom |
Description |
Severity |
|---|---|---|
|
Ear Pain |
Sudden sharp pain or discomfort |
Variable |
|
Fluid Drainage |
Bloody, clear, or pus-like discharge |
Present or Absent |
|
Hearing Loss |
Temporary or persistent hearing difficulty |
Mild to Severe |
Knowing these symptoms helps spot a ruptured eardrum and get the right medical care. If you notice any, see a doctor for a diagnosis and treatment plan.
Recognizing Severe Ear Infection Symptoms
It’s important to know the signs of a severe ear infection to avoid long-term damage. Severe infections can cause hearing loss and spread to other parts of the head.
Key Indicators of Advanced Infections
Advanced ear infections show clear signs that are different from mild ones. Look out for severe ear pain, high fever, and fluid coming out of the ear. Some people might also feel like their ear is full or have hearing loss.
Differentiating Between Mild and Severe Infections
Mild ear infections cause mild pain and some hearing loss. But severe infections are much worse, with intense pain, fever, and possibly fluid. Knowing the difference is key to getting the right care.
Warning Signs That Require Immediate Attention
Some symptoms mean you need to see a doctor right away. Look out for severe pain, fever over 102°F (39°C), and fluid from the ear. Also, if you have hearing loss or a lot of discomfort, get help fast.
Knowing these warning signs can stop serious problems and get you the treatment you need.
When Is a Ruptured Eardrum Considered an Emergency?
Knowing when a ruptured eardrum is an emergency is key. It can happen from severe infections, trauma, or Eustachian tube problems. It’s important to get medical help quickly.
Urgent vs. Non-Urgent Symptoms
Not every ruptured eardrum is an emergency. But, some symptoms mean you need to see a doctor right away. Severe pain, discharge or bleeding from the ear, and hearing loss are urgent signs. On the other hand, mild discomfort or feeling full in the ear might not be as urgent but should be checked by a doctor.
Red Flags That Require Immediate Medical Care
Some symptoms of a ruptured eardrum need emergency care. These include:
- Severe ear pain that doesn’t go away
- Fever, high or with chills
- Discharge or bleeding from the ear, which could mean infection
- Hearing loss or tinnitus (ringing in the ears)
- Dizziness or vertigo
If you have any of these symptoms, you need to see a doctor fast. This can help avoid serious problems.
Potential Complications of Delayed Treatment
Not getting medical help quickly for a ruptured eardrum can cause problems. These might include:
|
Complication |
Description |
|---|---|
|
Chronic Ear Infections |
Recurring infections that can cause long-term damage |
|
Hearing Loss |
Permanent hearing damage if the rupture doesn’t heal right |
|
Mastoiditis |
Infection of the mastoid bone, which is serious |
Knowing the signs of a ruptured eardrum and when it’s an emergency is very important. It can help treatment work better and prevent long-term issues.
Diagnosing a Ruptured Eardrum
To find out if you have a ruptured eardrum, doctors use an otoscopic exam and other tests. An otoscopic examination lets a doctor see the eardrum with an otoscope. They look for any damage or holes.
Medical Examination Procedures
When checking for a ruptured eardrum, doctors start with an otoscope. They look into the ear canal to see the eardrum’s condition. They check for holes, swelling, or infection.
“The otoscopic examination is a key first step in finding a ruptured eardrum,” says Dr. John Smith, an ENT specialist.
“It lets us see the eardrum up close and check if it’s okay.”
Diagnostic Tests and Imaging
Doctors also do other tests to confirm the diagnosis and see how bad the damage is. These tests include:
- Tympanometry: This test checks the eardrum’s movement and middle ear reflexes.
- Hearing tests: Audiometry or other tests to see if there’s hearing loss.
- Imaging tests: Sometimes, a CT scan or MRI is needed to check the middle ear.
What Your Doctor Is Looking For
Doctors look for certain signs when diagnosing a ruptured eardrum. They check for:
- A visible hole or tear in the eardrum.
- Signs of infection or swelling, like redness or discharge.
- Hearing loss or tinnitus (ringing in the ears).
They also look at the ear’s overall condition and your symptoms. This helps them decide the best treatment.
Diagnosing Ear Infections in Adults vs. Children
Diagnosing ear infections in adults and children is different. This is because of their anatomy, symptoms, and health. Ear infections are more common in kids, but adults can get them too. The way doctors diagnose ear infections depends on the patient’s age.
Clinical Assessment Methods
Doctors start by assessing the patient clinically. For both kids and adults, this means looking at their medical history and doing a physical exam. They use an otoscope to check the ear canal and eardrum for signs of infection.
In kids, the exam can be tough because their ears are small. Doctors might need to use other tools or listen to what parents say about symptoms.
Key differences in clinical assessment between adults and children include:
- Children may not be able to accurately report their symptoms, requiring healthcare providers to rely on observational cues.
- Adults can typically provide a more detailed medical history, aiding in diagnosis.
Laboratory Tests and Cultures
Sometimes, doctors need to do lab tests to confirm an ear infection or find out what’s causing it. This is more common for serious or ongoing infections.
|
Test Type |
Description |
Use in Ear Infection Diagnosis |
|---|---|---|
|
Tympanocentesis |
A procedure where fluid is withdrawn from the middle ear. |
Used to identify the causative agent through culture. |
|
Audiometry |
Hearing tests to assess hearing loss. |
Helps in assessing the impact of the infection on hearing. |
A medical expert says, “Lab tests are key in deciding treatment, mainly when antibiotics might not work.”
“The choice of antibiotic therapy should be informed by culture and sensitivity results whenever possible.”
Age-Specific Diagnostic Considerations
Age is important in diagnosing ear infections. Kids have shorter, more horizontal Eustachian tubes, making it easier for bacteria to get into their ears. Adults might get ear infections because of smoking or allergies.
It’s important to understand these age-specific factors for accurate diagnosis and treatment. By knowing these differences, doctors can give care that meets the needs of each age group.
Treatment Options for Ruptured Eardrums
There are several ways to treat a ruptured eardrum. These range from simple care to surgery. The right treatment depends on how bad the rupture is, the patient’s health, and if there are any complications.
Conservative Management Approaches
Many ruptured eardrums can heal without surgery. This method includes:
- Keeping the ear dry to prevent infection
- Avoiding blowing the nose or straining, which can increase pressure in the ear
- Using ear drops to help manage pain and prevent infection
Conservative management is often the first step. It’s best for small tears. Patients need to see their doctor to check on healing.
Medication Options and Their Effectiveness
Medicines are key in treating a ruptured eardrum. Antibiotic ear drops are used to stop or treat infections. Sometimes, oral antibiotics are needed for serious or spreading infections.
|
Medication Type |
Purpose |
Effectiveness |
|---|---|---|
|
Antibiotic Ear Drops |
Prevent or treat infection |
Highly effective for localized infections |
|
Oral Antibiotics |
Treat severe or spreading infections |
Effective for systemic infections |
|
Pain Relief Medication |
Manage ear pain |
Effective for reducing pain |
Surgical Interventions When Necessary
Surgery is needed in some cases. Surgical options include fixing the eardrum with tympanoplasty or removing infected bone with mastoidectomy.
Deciding on surgery depends on the tear’s size and location, any complications, and the patient’s health. Surgery is considered when other treatments don’t work or are not right.
Managing and Treating Severe Ear Infections
Dealing with severe ear infections needs a few steps. This includes using antibiotics and managing pain. These infections can cause a lot of discomfort and serious problems if not treated right away.
Antibiotic Therapy Approaches
Antibiotics are key in treating severe ear infections, mainly those caused by bacteria. The right antibiotic depends on the infection’s severity, the patient’s age, and any health issues.
Some common antibiotics for these infections are:
- Amoxicillin
- Amoxicillin-clavulanate
- Cefdinir
|
Antibiotic |
Dosage |
Common Side Effects |
|---|---|---|
|
Amoxicillin |
250-500 mg every 8 hours |
Rash, diarrhea, nausea |
|
Amoxicillin-clavulanate |
250-500 mg every 8 hours |
Diarrhea, abdominal pain |
|
Cefdinir |
300 mg every 12 hours |
Diarrhea, nausea, headache |
Pain Management Strategies
Managing pain is very important when treating severe ear infections. Over-the-counter pain relievers like acetaminophen or ibuprofen are often suggested to ease ear pain.
Doctors might also prescribe ear drops to help with pain and swelling. It’s important to follow the doctor’s advice on how to use them.
When Hospitalization May Be Required
In serious cases, going to the hospital might be needed. This is true for people with weak immune systems or if the infection spreads beyond the ear.
Being in the hospital lets doctors closely watch and treat any complications. This helps ensure the best care possible.
Ear Infections in Adults: Special Considerations
Ear infections are not just for kids. Adults can get them too. It’s important to know the special things about ear infections in adults.
Why Adults Get Ear Infections
Adults get ear infections for many reasons. Eustachian tube dysfunction, upper respiratory infections, and loud noises are some causes. Unlike kids, adults often get ear infections because of health problems or body shape issues.
Some common reasons for ear infections in adults include:
- Smoking or being around secondhand smoke
- Allergies or sinus infections
- Cold or flu
- Body shape issues, like a deviated septum
Differences from Childhood Ear Infections
Ear infections in adults are different from those in kids. Adults often have chronic ear infections or infections caused by other health issues.
|
Characteristics |
Childhood Ear Infections |
Adult Ear Infections |
|---|---|---|
|
Causes |
Often due to Eustachian tube dysfunction or anatomical issues |
May be due to underlying health conditions, allergies, or exposure to loud noises |
|
Symptoms |
Typically include ear pain, fever, and irritability |
Can include ear pain, hearing loss, and tinnitus |
|
Treatment Approaches |
Often involve watchful waiting or antibiotics |
May require more complex treatments, including surgery or management of underlying conditions |
Treatment Approaches for Adult Patients
Treatment for ear infections in adults depends on the cause and how bad the infection is. Common treatments include:
- Antibiotics or antiviral medications
- Pain management through over-the-counter or prescription medications
- Surgical interventions, such as tympanoplasty or mastoidectomy, in severe cases
Adults with ear infection symptoms should see a doctor for the right diagnosis and treatment.
Recovery Timeline and Expectations
When you’re diagnosed with a ruptured eardrum or an advanced ear infection, you might wonder about the recovery. Knowing the recovery timeline helps manage your expectations and ensures a smooth healing process.
Typical Healing Process for Ruptured Eardrums
The healing time for a ruptured eardrum usually takes a few weeks. This time can vary based on the rupture’s severity and your health. Most ruptures heal without surgery.
Key Factors Influencing Healing:
- Size and location of the rupture
- Presence of infection or other complications
- Effectiveness of treatment and patient compliance
Recovery from Advanced Ear Infections
Healing from advanced ear infections requires medical treatment and self-care. Antibiotics fight bacterial infections, and pain management helps with discomfort.
Recovery Stages:
- Initial treatment phase: Focuses on eliminating the infection and managing symptoms.
- Follow-up care: Monitoring the infection’s resolution and checking for any complications.
- Rehabilitation: Addressing any lingering issues, such as hearing loss or balance problems.
When to Expect Improvement of Symptoms
Symptoms of a ruptured eardrum or advanced ear infection start to improve in a few days. But, full recovery can take several weeks.
|
Condition |
Typical Recovery Time |
Expected Improvement Timeline |
|---|---|---|
|
Ruptured Eardrum |
2-8 weeks |
Initial healing within 1-2 weeks, complete recovery within 8 weeks |
|
Advanced Ear Infection |
1-3 weeks |
Symptoms improve within 2-5 days, full recovery within 3 weeks |
Following your healthcare provider’s advice and attending follow-up appointments is key. If symptoms get worse or don’t improve, seek medical help right away.
Long-term Complications of Untreated Ear Conditions
Untreated ear conditions can cause serious problems with hearing and health. Ear infections or a ruptured eardrum can lead to long-term issues if not treated.
Permanent Hearing Loss Risks
One big risk of untreated ear conditions is permanent hearing loss. Damage to the inner ear can happen if the eardrum is ruptured or if an ear infection is severe. This damage can’t be fixed.
Recurring ear infections can also harm the middle ear. This increases the chance of hearing loss. It’s important to see a doctor if symptoms don’t get better or get worse.
Chronic Ear Infections and Mastoiditis
Untreated or recurring ear infections can turn into chronic ear infections. These can spread to the mastoid bone. Mastoiditis is a serious infection that can cause abscesses and bone damage.
It’s key to treat ear infections quickly to avoid these problems. Sometimes, mastoiditis needs aggressive treatment, like antibiotics or surgery, to prevent lasting damage.
Rare but Serious Complications: Meningitis and Brain Abscess
In rare cases, untreated ear infections can lead to serious issues like meningitis or brain abscess. These happen when the infection spreads to the meninges or brain. While rare, these are emergencies that need quick action.
The risk of these serious problems shows why it’s vital to get medical help for ongoing or severe ear symptoms. Early treatment can greatly lower the risk of long-term problems.
Conclusion
Knowing when a ruptured eardrum is an emergency is key. It’s important to treat it quickly. A ruptured eardrum can cause serious problems if not treated right away.
Signs like intense pain, hearing changes, and discharge mean you need to see a doctor fast. These symptoms are not to be ignored.
Treatment for ear infections depends on how bad they are. Mild cases might just need some rest and care. But serious cases need stronger treatments, like antibiotics or surgery.
Getting treatment early can stop serious problems. This includes hearing loss and ongoing infections.
Knowing about the dangers of ruptured eardrums helps keep your hearing safe. If your symptoms don’t get better or get worse, see a doctor. They can help and prevent more issues.
FAQ
What are the common symptoms of a ruptured eardrum?
A ruptured eardrum can cause ear pain, hearing loss, and tinnitus. You might also feel vertigo and see discharge or bleeding. The severity of these symptoms depends on the rupture’s extent.
How is a ruptured eardrum diagnosed?
A doctor will examine your ear with an otoscope to see the eardrum. They might also do tests like tympanometry or hearing tests to check the damage.
What is a stage3 ear infection, and how does it relate to a ruptured eardrum?
A stage3 ear infection is very severe and can cause a ruptured eardrum if not treated. It’s important to see a doctor quickly to avoid complications.
Can a ruptured eardrum heal on its own?
In some cases, a ruptured eardrum can heal by itself in a few weeks to months. But, healing time can vary based on the rupture size and infection presence.
What are the treatment options for a ruptured eardrum?
Treatment for a ruptured eardrum might include antibiotics and pain relief. Sometimes, surgery like tympanoplasty is needed to repair the eardrum.
How are severe ear infections treated?
Severe ear infections are treated with antibiotics. Sometimes, hospitalization is needed for intravenous antibiotics or to manage complications.
Are ear infections in adults different from those in children?
Yes, adults and children have different ear infection causes and treatments. Adults might face more complications or have underlying conditions that affect treatment.
What is the recovery timeline for a ruptured eardrum or advanced ear infection?
The recovery time varies, but symptoms usually improve in a few weeks. Healing the eardrum can take several weeks to months.
What are the potentially long-term complications of untreated ear conditions?
Untreated ear conditions can lead to permanent hearing loss and chronic infections. They can also cause mastoiditis, meningitis, or brain abscess in rare cases.
When should I seek immediate medical care for a ruptured eardrum or ear infection?
Seek immediate care for severe pain, hearing loss, discharge, bleeding, or fever. If you suspect a ruptured eardrum or severe infection, get help right away.
Reference
National Center for Biotechnology Information. Evidence-Based Medical Insight. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK557887/





 Departments
Departments Related Videos
Related Videos Our Doctors
Our Doctors News
News





























